Abstract
Background:
Health visitors have a key role in supporting and protecting adults and children affected by domestic abuse.
Aims:
The study aimed to examine the experiences and perceptions of student health visitors recognising and responding to domestic abuse in practice placement settings.
Methods:
Semi-structured interviews were conducted with five student health visitors in the United Kingdom. Interviews were transcribed and analysed using interpretive phenomenological analysis.
Results:
Four superordinate themes were identified: ‘part and parcel of health visiting practice’; ‘challenges in identifying domestic abuse’; ‘uncertainty and apprehension’; ‘strengthening knowledge and confidence’. All participants had engaged in practice activities related to domestic abuse within SCPHN placements, commonly expressing a sense of disbelief at the scale of the issue in practice. Difficulties and unease regarding identification and management of domestic abuse were reported. Access to support and opportunities to reflect and ‘talk things through’ were found to be important for students regarding this sphere of practice.
Conclusions:
The findings contribute to the body of knowledge about domestic abuse-related practice within nursing. Recommendations made may contribute to practice development and help inform future teaching and educational strategies within SCPHN programmes.
Keywords
Introduction
Domestic abuse (DA) is a significant public health issue. An estimated 2.4 million adults aged 16 years and over experienced DA in England and Wales in the year ending March 2022, and during this period, 1,500,369 DA-related crimes were recorded by the police in these nations (Office for National Statistics (ONS), 2022). Defined as either a single act or a pattern of conduct occurring between those aged 16 years and over with a personal connection, DA incorporates a range of behaviours, including, but not limited to, physical, controlling, coercive, economic, psychological and emotional abuse (Domestic Abuse Act, 2021). The impacts of DA on individuals and wider society are well documented, encompassing physical and mental health harms to individuals, as well as harms to national economic costs through productivity loss, and healthcare and criminal justice system spending associated with DA (SafeLives, 2023). Of particular significance, 470 DA-related deaths were recorded in England and Wales between April 2020 and March 2022 resulting from intimate partner homicide, victim suicide, adult family homicide, including DA-associated child death (Bates et al., 2022). Furthermore, in the UK children exposed to DA are legally considered victims (Domestic Abuse Act, 2021), recognising the substantial risks posed to children.
This paper reports on a study examining an aspect of UK community nursing practice related to DA management, focusing on the experiences of student health visitors identifying and responding to DA while working in practice placements. Health visitors are registered nurses or midwives who have completed further studies leading to the qualification of Specialist Community Public Health Nurse (SCPHN), and as such, they work in local communities, seeking to improve population health and well-being (Nursing and Midwifery Council (NMC), 2022). In October 2022, 5671 full-time equivalent (FTE) health visitors were employed by the National Health Service (NHS) in England (NHS Digital, 2023), leading teams which include community staff nurses and nursery nurses. Those undertaking the SCPHN course, referred to in this paper as student health visitors, complete community placements under the supervision of Practice Supervisors (PSs) and Practice Assessors (PAs) who aim to ensure safe and effective learning experiences (NMC, 2023) and to facilitate achievement of defined proficiencies leading to SCPHN registration (NMC, 2022).
Recognition of DA, supported by effective responses, is imperative in ensuring the safety and protection of adults and children experiencing abuse, forming an important part of health visiting practice. Indeed, embedded within professional standards is the need for SCPHNs to proactively identify vulnerable people, and lead coordinated action to support and safeguard those at risk of harm (NMC, 2022). With a specific focus on promoting health and well-being of children aged 0–5 years through implementation of the Healthy Child Programme (Office for Health Improvement & Disparities, 2023), health visitor assessment of DA within families is integral to practice (Department of Health & Social Care (DHSC), 2009). Practitioners are guided to ask women during health visiting contact, if they are experiencing DA. This practice is known as ‘routine enquiry’ (DHSC, 2013, 2017). Health visiting services resulted in more than 1.96 million children in England receiving mandated health reviews in the year ending November 2023 (Institute of Health Visiting (iHV), 2024), evidencing the significant opportunities for identifying DA that the service offers.
It is within this context that student health visitors develop knowledge and skills in assessing and responding to DA in practice settings. Although those undertaking SCPHN programmes are NMC registrants, DA is a challenging and emotive topic, and not all student health visitors will have had prior professional experience of managing DA. Supporting this, Bradbury-Jones and Broadhurst’s (2015) qualitative study investigating student nurses’ and midwives’ educational needs regarding DA found that student practice experiences varied, with some students reporting no exposure to DA in clinical placements, and most feeling removed from situations where DA did exist, which reduced confidence in responding to DA in practice. Similarly, Alshammari et al. (2018) in reviewing literature, identified that nurses receive insufficient training on DA in pre-registration nursing education to equip them with the requisite skills, knowledge and attitudes to effectively facilitate and manage DA disclosure.
Beyond pre-registration experiences, research evidence reports commonly shared barriers to the identification and responses to DA in healthcare settings, nationally and internationally. Midwives, in an Australian qualitative study (Eustace et al., 2016) reported feeling unprepared and lacking in confidence in conducting routine enquiry for DA, accompanied by feelings of anxiety and fear regarding managing disclosure. In reviewing community nurse-led interventions during the post-natal period, a lack of knowledge, skills and confidence were found as barriers to identifying and responding to DA (Boyle and Murphy-Tighe, 2022), and similarly, Ahmad et al. (2016) in a literature review examining DA screening in emergency departments, found that knowledge, training, confidence and comfort in undertaking enquiry affected the abilities of healthcare professionals to identify DA. Such findings are significant as women feel that it is the responsibility of health professionals to ask about abuse (Bradbury-Jones et al., 2014), and yet inappropriate handling of disclosures may re-traumatise or re-stigmatise victim-survivors of DA (Melendez-Torres et al., 2022).
Such studies, although providing insight, do not specifically relate to SCPHN programmes, and although a core area of practice, very limited data are available on the experiences of student health visitors working with DA. Acknowledging gaps in knowledge, a small qualitative study was conducted seeking to answer the following research question: What are the experiences of student health visitors regarding the identification and responses to domestic abuse in practice placement settings?
Methodology
Aim
The study aimed to examine the experiences of student health visitors regarding DA during community practice placements, increasing knowledge and understanding of this phenomenon. It is intended that learning will help inform and strengthen related curriculum strategies for student health visitors undertaking the SCPHN programmes, and in doing so, it will contribute to improved care outcomes for families and children experiencing DA.
Design
To gain in-depth information and detailed exploration of participant experience, a qualitative methodology was adopted. Recognising the sensitive nature of the research topic, an interpretive phenomenological analysis (IPA) was used, enabling meaning and understanding of the participant lived experience to be achieved. IPA acknowledges the interpretive nature of participant experience, and engages in the researcher interpretation of the data, thus encouraging reflection and examination of self (Smith and Shinebourne, 2012). This double hermeneutic process was deemed pertinent, with the assumption that both participant and researcher would be actively attempting to make sense of the reported realities. IPA recognises that researcher interpretation of data is influenced by personal knowledge and history (Smith, 2004), this being relevant and supporting the rationale for study design choice, as the researcher is an NMC registrant previously employed as a health visitor, and a university lecturer.
Participants
Purposive recruitment in accordance with IPA methodology (Smith and Shinebourne, 2012) was undertaken. Participants were registered nurses or midwives undertaking a 1-year SCPHN health visiting programme, studying at the higher educational organisation in South-East England where the researcher was based. Due to the detailed nature of analysis in IPA studies, a small sample was advocated (Smith and Shinebourne, 2012) and therefore a maximum of eight participants was proposed.
Recruitment processes involved the delivery of an explanatory briefing to the group of potential participants, and the provision of an information sheet. Subsequently, the researcher met individually with those expressing interest in participation to discuss information further, prior to obtaining consent for inclusion in the study.
Five (N = 5) student health visitors participated in the study, all recruited from the same SCPHN cohort. Adhering to research ethics principles, it was important to ensure that participation remained voluntary, and so beyond the recruitment strategies identified above, no further interventions were made by the researcher to increase the sample size. Supporting this decision, Alase (2017) identifies that the number of participants can be as low as two in an IPA study.
Although all five students were studying the same academic curriculum in one university, they were employed by different organisations and undertook practice placements in different geographical locations. Prior to commencing the SCPHN programme, all participants had worked for varying periods as registered nurses or midwives in acute or community settings.
Data collection
Data were collected through semi-structured interviews conducted online via Microsoft Teams. An interview schedule was developed in advance (see Appendix One) containing open, explorative questions and prompts to facilitate dialogue. Smith and Shinebourne (2012) identified the importance of promoting comfort and minimising participant distress during interviews, and accordingly, consideration was given to the order of questions, aiming to create ease and a non-threatening environment. As suggested by Smith and Shinebourne (2012), the semi-structured approach to interviewing allowed flexibility to extend understanding of participant reporting. The average length of interviews was 40 minutes, and all interviews were audio and video recorded, and transcripts documented verbatim.
The SCPHN programme from which the participants were recruited is classified into three study periods with the final phase focusing on clinical practice. To allow time for student health visitors to acquire practice experience of the research topic, participant interviews occurred in the final study period of the course. This helped increase homogeneity, a common aim in IPA research involving small sample groups (Smith and Shinebourne, 2012), although it is acknowledged that the varied professional backgrounds of the participants prior to the SCPHN course made it difficult to achieve a truly homogenous sample.
Ethical considerations
Ethical Guidelines for Educational Research (British Educational Research Association (BERA), 2018) underpinned the approaches adopted; ethical approval for this study was granted by the Research Ethics Panel of the university through which the research was conducted.
DA is an emotive issue which the participants may have personal experience of as well as professional involvement, and discussion of the issue may evoke emotionally painful thoughts and feelings. To minimise potential harm to participants, care was taken during all stages of the research process, including the provision of debrief and post-interview support material. Written consent was obtained from all participants, and the opportunity to withdraw consent was offered until initiation of data analysis. All the collected data were stored securely in accordance with university policy on data security; and pseudonyms were used in reporting results to preserve participant anonymity.
A further ethical consideration was presented through the position of the researcher as a university lecturer teaching on the SCPHN programme from which participants were recruited. Steps were taken to minimise the possible effects of power imbalance with the cooperation of the SCPHN programme leader. The researcher did not undertake an Academic Assessor role for the programme during the research period, and only assessed academic work in the capacity of a second marker.
Data analysis
Analysis of data reflected IPA methodology involving researcher immersion in data by reviewing recorded interviews, close reading of transcripts and initial note-making, transforming initial notes to emerging themes, examining emerging themes for connections, clustering to form superordinate and finally subordinate themes (Smith and Shinebourne, 2012). This involved a systematic and methodical approach which began at commencement of data collection, accompanied by reflective and abstract thinking in identifying patterns and concepts emerging from the data.
Rigour
The degree of trustworthiness and authenticity are argued to indicate the quality of research within a constructivism paradigm, with indicators of credibility, transferability, dependability and confirmability used to reflect validity and reliability in qualitative research (Guba and Lincoln, 1994). As a novice, sole researcher, prior to development of the study two educational sessions on IPA, led by academic researchers, were attended.
A diary recording thoughts, ideas and reflections was maintained by the researcher which aided bracketing, a technique used in phenomenology (Creswell, 2007), whereby the researcher strove to separate personal assumptions and preconceptions about the phenomenon from participant data.
Adherence to IPA methodology, including referral to the research question, revisiting, and reviewing data, accompanied by detailed documentation, was maintained throughout the research process. To strengthen credibility and confirmability, final transcripts of interviews were shared with individual participants. In addition, the quality of the study processes was checked by using a qualitative research appraisal tool (Critical Appraisal Skills Programme (CASP), 2018).
Results
Four superordinate themes were identified, each containing one to two subordinate themes (see Appendix Two: Table One: Themes). Findings from all five participants contributed to each theme. Although perceptions and individual practice realities differed, significant commonalities and shared experiences existed in all themes.
Superordinate theme 1: ‘Part and parcel of health visiting practice’
During interviews all participants were asked about previous clinical experiences of DA to provide context and to help in the interpretation of their experiences as student health visitors.
Experience of DA in clinical practice prior to commencing the SCPHN course varied among participants, and for most it was limited. As Maja expressed I actually don’t think I had any experience with domestic abuse
Similarly, Amira reported having had ‘really minimal experience of it’ and Zuri that ‘it was quite rare’.
Of those who had encountered DA in previous practice, there was little direct engagement with the issue of DA, and a focus on delivering other aspects of clinical care. Elan discussed her awareness of patients in her former work area experiencing DA but nothing that I dealt with myself.
Echoing that, but with perhaps greater involvement, Nia, discussed prior working experiences of DA as part of a team approach.
In contrast, all participants reported direct experience of DA as a practice component since commencing the SCPHN course, including identification of abuse and the associated safeguarding and child protection implications and work practices. Significantly, a sense of disbelief was commonly conveyed indicating that participants had not realised the scale of DA before working in practice placements as student health visitors: (It’s) ‘massive, big, very big. A lot of children on Child in Need plans, a lot of Child Protection plans because of it’ (Elan) It just sort of seems that its rife really . . . I sort of like (sic) had never been aware that it was so prevalent (Zuri)
Normalisation
While observing health visitor colleagues, a perception that DA is a routine practice issue in health visiting was reported.
In practice environments, the participants witnessed a high volume of interagency communications, mostly through police notifications to health visiting teams, with assigned ‘duty’ health visitors managing referrals. As Zuri described: On the safeguarding duty line, it’s just almost constant . . . a sort of stream of notifications of DV (domestic violence) incidents.
Recognising the responsibilities, and potential personal impacts on health visiting colleagues of assessment and decision-making relating to DA, Nia observed: I think it can be quite overwhelming to screen such a large quantity and work out who actually needs health visiting input
Although the impact of responding to and managing DA on health visitors in terms of workload was acknowledged, participants did not detect overt signs of associated distress or difficulty, but they interpreted a normalisation among qualified SCPHNs in this sphere of practice: I think it’s just normal for them. It’s just part of the role (Elan)
Supporting this perception, and identifying the influence of practice familiarity on behaviours, Maja observed the following about health visitor colleagues: They’re probably so experienced with it now that I don’t think necessarily . . . that there’s a shock factor or ‘oh my goodness’ . . .. I think it’s . . .. just part and parcel of health visiting.
While recognising the familiarity of DA-related workload, a sense of distinction between the roles of qualified SCPHNs and student health visitors emerged, with students only partially involved in this aspect of practice: I have been sort of involved a bit but more as an observer in this role (Zuri)
This appears to be a shielding strategy adopted by PSs and PAs in a supportive learning environment, as conveyed by Elan: There is a lot of domestic abuse, but I feel I’m protected a little bit from it . . . they wouldn’t put me in a situation where I had to deal with anything myself.
Superordinate theme 2: Challenges in identifying DA
Several challenges were reported regarding the identification of domestic abuse. These clustered around the following areas:
Asking the question
All participants demonstrated sound theoretical and procedural knowledge of routine enquiry, recognising when to conduct and when not to, as illustrated by Amira: I always ask the question . . . if it is obviously safe to do so.
Safety appeared at the forefront of decision-making with participants describing steps taken to ascertain if the situation was appropriate for DA enquiry. For example, Maja reported checking if: anybody else (is at) home
when conducting routine enquiry during home visits.
Circumstantial factors were a source of frustration, with a realisation that opportunities to identify DA were reduced: You can’t ask it if the partner is in the house . . . and you can’t ask if there is a child aged two years and over. . . . You can’t really assess it . . . because obviously you don’t want to put the mum at risk, but then you can’t really make sure she is safe either. I just find that quite frustrating. (Elan)
Barriers to conducting routine enquiry were consistently reported. They included environmental constraints, such as working in a community facility where privacy could not be ensured: As a student, I’ve been in a clinic . . . and there’s been two . . . nursery nurses seeing two women at the same time, so one’s on one side of the room, and one’s on the other side, with no sort of like barrier in between, and at the 6–8 week check obviously you like to talk about domestic abuse . . . but because there’s like (sic) three other people in the room within earshot . . . I think it’s almost pointless (Zuri)
Similarly, shared observations were made on infrequencies of universal contact and a lack of continuity of care which were felt to reduce the likelihood of abuse disclosure. Amira captures this expressing: I think it’s very unlikely mums are going to disclose it (DA) at a first meeting. Where I’m based . . . unless you target the family, they go to clinic for the 6–8 week, so actually there’s not that continuity . . . If they’re (then) with somebody completely different, a different member of staff, it’s kinda like they’ve gone back to the beginning again.
Feelings related to conducting routine enquiry varied. Some displayed confidence, while others found it an uncomfortable experience: To be honest, I don’t like asking it . . . I never say it outright. (Amira)
Though the use of abuse-specific terminology was sometimes avoided, adaptations to practice to improve techniques occurred: I used to ask it . . . in a not very direct way . . . I used to say ‘do you feel safe at home?’ and that could be interpreted quite widely by many different people . . . so I have changed that slightly now. (Maja)
As reported by Nia, wider assessment skills, involving observing the home environment and family interactions and dynamics, were also used to identify DA: Even if I’m unable to ask I tend to make observations about the interactions between parents . . . I think you can always get a bit of the sense of the atmosphere.
However, uncertainties regarding interpretation of such observations were voiced indicating complexity and illustrating difficulties in DA recognition: Is it domestic abuse . . . what is normal for that family? (Zuri)
Adding a further dimension, two respondents spoke of ambiguities in DA enquiry posed through possible cultural differences whereby individual interpretations and acceptances of abuse vary.
Gendered experiences
During each interview, an open question was asked regarding identification of DA, with all participants discussing experiences relating to the discovery of only female victims of DA. Participants were then asked of their experiences regarding recognition of male victimisation of abuse, with all describing a service focus on women and children and reporting it unlikely that men experiencing DA would be identified: I think it is really difficult because generally we don’t ask dads about domestic abuse (Nia)
Reiterating this, Zuri expressed: health visiting is so focused on the mum and child . . . it would be such a big thing for a man to open up about something like that . . . I’d be absolutely shocked if a man did feel that they could tell me.
Conveying some uncertainty about DA enquiry, and a sense of inequity, Maja described a conversation with colleagues following a time when she had asked a father about relational safety: It was such an interesting conversation because they were saying we shouldn’t ask dads, and I was saying ‘oh why not, because they could be at risk?’, and they were saying . . . in case they were the abuser
Superordinate theme 3: Uncertainty and apprehension
Regarding broader responses to DA, feelings of trepidation were commonly shared.
What if they say yes?
Although all participants conducted routine enquiry, none of the student health visitors had experienced a disclosure of DA, and the prospect of managing a disclosure-created unease, with this powerfully conveyed by Amira: I’m always a bit apprehensive asking the question because if they turn round and say . . . ‘yes’, I just think, what would I say next? What would I do next?
Similarly, reflecting on how she may feel and react in the event of DA disclosure, Nia stated: I’d probably find it quite daunting . . . I’m not sure how confident I’d be . . . I think it is a lot of responsibility. I’d probably be quite overwhelmed if somebody did disclose.
Inexperience was consistently acknowledged, with recognition that the application of theoretical knowledge to practice situations may be challenging: I do have all the knowledge, but then when . . . it comes to the time of dealing with it, it’s different isn’t it (Elan)
Raising the issue
Other elements involved in management of DA also caused worry, including perceived impact on the relationship between client and health professional. This particularly related to child safeguarding practice, centring on difficulties in discussing the impact of DA on children, with parents. In recalling a conversation with a mother, Maja likened it to breaking bad news
with concerns that in raising the issue, the woman may perceive herself as a bad mother.
Where child protection concerns existed, explanation of the effects of DA exposure on children was considered a necessary, but uncomfortable part of the health visiting role, presenting tensions in working relationships with families and potential conflict between supporting victims of abuse while protecting children. Words such as ‘difficult’ and ‘challenging’ were repeated in respondent descriptions of such situations as illustrated by Maja: I don’t want to upset any parents . . . on a personal level . . . I find it challenging because it’s a difficult conversation at the end of the day.
A common thread throughout participant accounts was the uncomfortable emotional consequences evoked in seeking to identify and respond to DA. In part, this appeared to relate to uncertainty over practice, but physical engagement in placement settings also brought stark realisations regarding the effects of abuse on families. Zuri, in visiting a woman living in temporary accommodation as a result of fleeing abuse, empathised: Her life was turned upside down . . . it was horrendous. I felt for her
Although responses varied, stress and unease were reported, with this appearing to be experienced privately and managed personally. Maja, in referring to conversations with clients about DA, mirrors this: In terms of how it makes me feel . . . I’d say uncomfortable . . . but I wouldn’t try to show that I was uncomfortable
Superordinate theme 4: Strengthening knowledge and confidence
An active approach to learning was apparent as participants described strategies undertaken to improve knowledge and skills related to DA. Keeping ‘up-to-date’ through accessing educational events and local training and reading and researching the topic contributed to knowledge development. Observation of qualified staff was valued and actively sought: I’m going to try and observe as many health visitors as I can . . . even when I’m qualified. If there’s an opportunity I will do so still. (Nia)
Reflection was a meaningful technique reported by one participant in helping process difficult occurrences: I find reflecting so helpful . . . Those written reflections can help sometimes . . . to really think in depth about conversations you’ve had and how they make you feel. (Maja)
Consistently, the significance of personal practice and experience in strengthening confidence was acknowledged, as conveyed by Amira in reference to routine enquiry: I think the more I ask it, the more comfortable I am asking it
Talking it through
Discussing DA-related issues, and being able to talk to more experienced staff, were important in supporting knowledge and confidence growth. This included direct contact with PSs and PAs and the wider health visiting team, and access to specialised expertise such as Safeguarding Leads in health and social care: Just talking through with colleagues helps . . . the more you talk about stuff, the more it kind of makes it less of a dauting prospect (Zuri)
Maintaining dialogue with others was reassuring and a strong support mechanism, as articulated by Elan: I’ve got really good support from (my Practice Assessor). I can discuss anything with her. If ever I’m worried or not sure, I feel like I can go and ask her anything. I think that’s good.
Similarly, knowing that colleagues or senior practitioners were accessible and could be contacted for advice if needed, seemed comforting and important in enhancing confidence, as reflected by Nia: I just know who to go to for support; I know who to go to.
Within the health visiting team, a willingness to share practice concerns and to openly seek advice from one another, appeared reassuring, modelling an acceptance of enquiry and help-seeking: Just to talk it through with someone could be really helpful . . . I observe them doing it as well when they’re on their team meetings, so it makes me feel I’m not the only one asking all these questions, because they use each other as support, so I think that’s really helpful. (Maja)
Discussion
The significance and scale of DA as a practice issue within health visiting were evident in the study findings. Although all participants had undertaken previous nursing or midwifery roles, similar to research evidence on pre-registration experiences (Bradbury-Jones and Broadhurst, 2015), direct responsibility for identifying and responding to DA prior to commencing SCPHN practice was limited. The sense of surprise at the extent of DA encountered by the student health visitor participants in practice placements confirms the specialist nature of health visiting, and related to this, a perception of DA management as being a ‘normal’ part of practice, indicates the need for focused student support in preparation for this aspect of the professional role, acknowledging that unfamiliarity with this sphere of clinical care is likely.
Routine enquiry for DA is part of health and social care policy, and yet the challenges reported in this study in conducting enquiry, including discomfort in asking the question, environmental and service constraints, and concerns over managing disclosure of DA, mirror difficulties reported in wider research. Bradbury-Jones et al. (2016) found that some health visitors felt uneasy and lacked confidence in conducting conversations with women about DA, with such experiences shared by nurses and midwives in different fields, and more broadly by other health professionals (Ahmad et al., 2016; Boyle and Murphy-Tighe, 2022; Eustace et al., 2016). Yet, female survivors of DA report that they expect health professionals to ask women about domestic abuse, and to be equipped to address the issue (Bradbury-Jones et al., 2014). Arguably, inadequate health professional responses may reduce future help-seeking attempts, inadvertently increasing risk for those experiencing DA, thus indicating a need to address knowledge and skill shortfalls.
In this study, although responses varied, it is of significance that student health visitors articulated uncertainty and apprehension over broaching the subject of DA and responding to disclosure, with a sense of associated internal personal distress. ‘Emotional labour’ describes the phenomenon whereby individuals in the workplace suppress their feelings or emotions to maintain a professional demeanour, which reflects socially expected behaviours, when interacting with clients (Hochschild, 1983), but this can have negative effects on the employee. Data collected from a study of Australian community nurses found that high levels of emotional labour were associated with increased job stress and lower well-being (Karimi et al., 2013). Regarding student health visitors, such effects may impact on learning and individual health, and in the context of DA, they may compromise client and family safety.
Acknowledging the above, it is important to explore possible approaches to strengthening preparedness for DA-related practice. Morgan et al. (2023) propose use of a flowchart for health visitors providing a practical framework in screening for DA and responding to disclosure. While the authors recognise the need for further research, such tools offer potential for increasing student confidence, particularly in knowing ‘what to do next’. Offering further insight, a practice evaluation examining preparation for DA enquiry found that health visitors favoured interactive learning over didactic methods (Johnson, 2020), with this being of relevance to SCPHN education. Simulation techniques enable learners to interact and engage in scenarios which imitate real-life, aiding the development of problem-solving skills while avoiding the anxiety that can accompany practising skills in actual settings (Hughes and Quinn, 2016). Indeed, a simulation-based learning event designed for a SCPHN student group was evaluated positively by student participants (Hatt, 2018). Similarly, Coates (2021) demonstrated effectiveness in using a simulation-based intervention to improve confidence in acute care nurse practitioner students in conducting difficult conversations related to clinical practice. Although long-term gains are unknown, such evidence supports the use of simulation in SCPHN curricula in preparing students to address DA in practice settings.
Student health visitors in this study utilised various learning strategies, including observing and talking through practice experiences. Social learning (Bandura, 1977) whereby learning occurs through observing the behaviours of others is argued to be a powerful technique in nurse education. Similarly, the relationship between student and teacher can be instrumental in learning (Hughes and Quinn, 2016). Significantly, teaching within the practice environment aims to orientate student health visitors to their professional role, encompassing the values and attributes necessary for health visiting practice (Cowley et al., 2015; Fanner et al., 2022), suggesting that modelling, and protected supervision time, are valuable components in SCPHN education. These factors place emphasis on the accessibility and quality of PS and PA support. However, of concern, numbers of full-time qualified health visitors in England have significantly reduced in recent years (NHS Digital, 2023), and service demands are high (Institute of Health Visiting (iHV), 2024). This potentially may not only impact negatively on student learning within practice settings but could also reduce support and opportunity for ongoing education and support of qualified practitioners.
Possibly linked with service constraints, this study identifies gendered differences in professional recognition of DA, with participants describing their experiences of conducting routine enquiry with women, and a practice focus on mother and child. Yet, men too experience victimisation of DA (ONS, 2022), although often remaining invisible to services (Hine et al., 2022). Supporting this, the Healthy Child Programme (DHSC, 2009) recognises a familiarity in working with mothers within maternity and child health services, which can result in fathers’ needs being poorly understood. This may partially explain the experiences reported by study participants. However, since health professionals are responsible for promoting and maintaining equality (Equality and Human Rights Commission, 2023), and recognising the commitment to address inequalities in the SCPHN standards (NMC, 2022), gender-inclusive practice remains a vital component in the SCPHN curriculum. Although influenced by policy and commissioning commitments, such approaches serve to expand student understanding of DA, aiding preparedness for future health visiting practice.
Limitations
Using IPA methodology, findings from this study contribute to the knowledge base on DA-related care in nursing. However, limitations exist. A small sample, recruited during a defined period was used, and therefore the experiences and views reported may not be representative of wider and current student health visitor populations. Obtaining further demographic details of participants could have enhanced understanding and interpretation of findings, and although rigorous steps were taken in research processes, the influences of researcher knowledge and their relationship with participants, and the complexities of IPA analysis, may limit dependability and confirmability of the results.
Conclusion
As an under-explored phenomenon, this study sought to examine the experiences of student health visitors in identifying and responding to DA while working in practice placements. All participants reported direct involvement in this sphere of practice with varied experiences and perceptions described. This study not only identifies the commitment of the participants to furthering personal professional development and competence but also finds the demands addressing DA often uncomfortable and stressful, particularly regarding disclosure management. This paper confirms the significance of practice support for learners and drawing on study findings and the wider evidence base, and makes recommendations for practice (see Appendix Three: Table Two: Implications for Practice). Acknowledging the importance of ongoing clinician support related to the issue of DA, it is suggested that practice implications also extend to qualified health visitors.
DA is recognised as a substantial public health issue, with legislation and policy guiding healthcare practice. Understanding of the realities of nursing practice regarding this phenomenon is strengthened through this study, and it is hoped that learning from the results may help inform related educational strategies within SCPHN curricula, contributing to increased safety for those affected by DA.
Key points for policy, practice and/or research
Routine enquiry for domestic abuse (DA) is included in health visiting practice and yet challenges in conducting this are experienced by student health visitors.
Uncertainties regarding the management of DA disclosure are reported by student health visitors, with associated anxieties experienced.
Practice support and guidance in managing DA is highly valued by student health visitors.
Further research into the effectiveness of educational interventions regarding DA practice within nursing is recommended.
Implementation of gender-neutral practice within health visiting may increase equity of service for all individuals experiencing DA.
Footnotes
Appendix
Table Two: Implications for Practice.
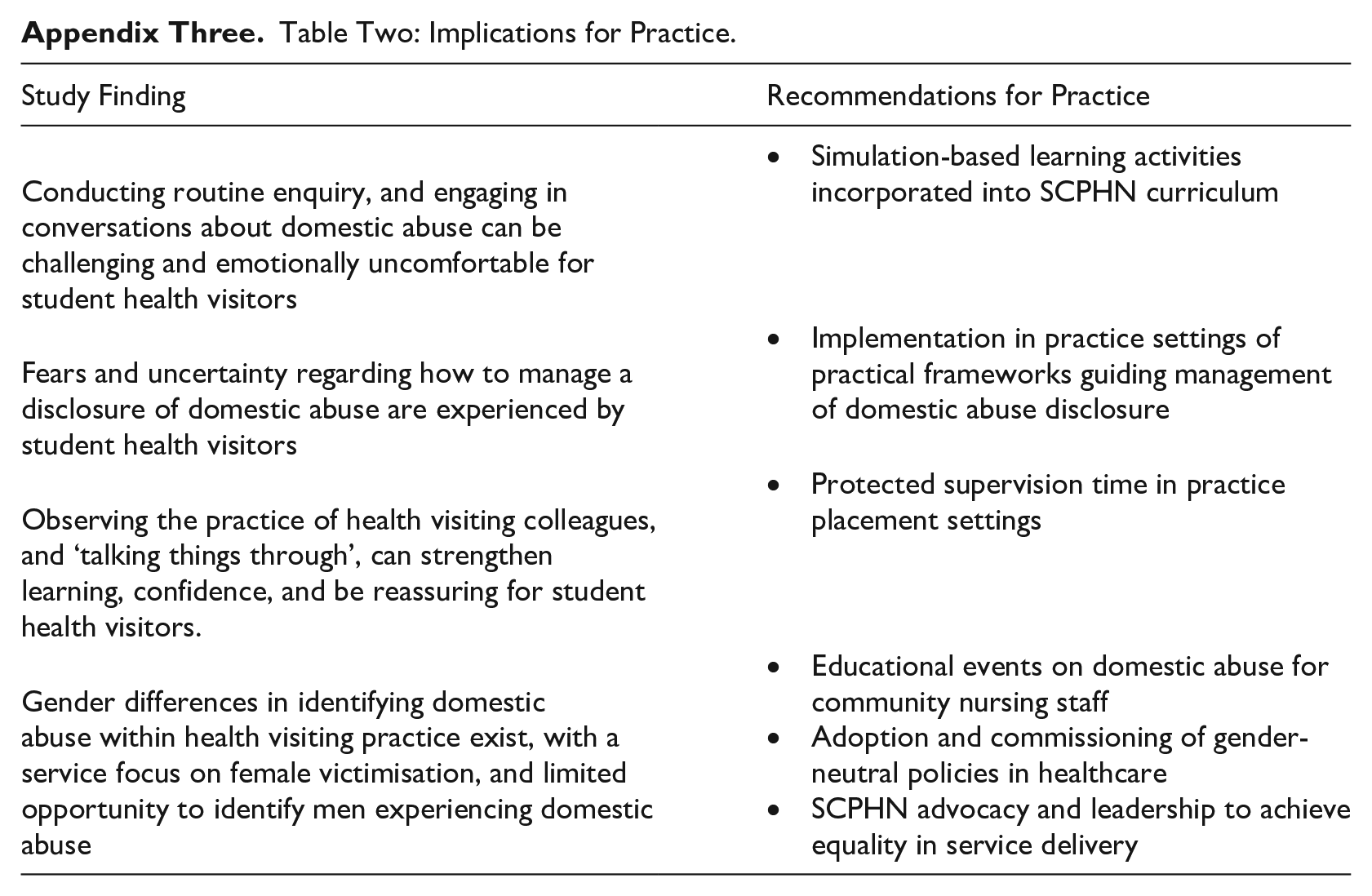
| Study Finding | Recommendations for Practice |
|---|---|
Conducting routine enquiry, and engaging in conversations about domestic abuse can be challenging and emotionally uncomfortable for student health visitors |
• Simulation-based learning activities incorporated into SCPHN curriculum |
Fears and uncertainty regarding how to manage a disclosure of domestic abuse are experienced by student health visitors |
• Implementation in practice settings of practical frameworks guiding management of domestic abuse disclosure |
Observing the practice of health visiting colleagues, and ‘talking things through’, can strengthen learning, confidence, and be reassuring for student health visitors. |
• Protected supervision time in practice placement settings |
Gender differences in identifying domestic abuse within health visiting practice exist, with a service focus on female victimisation, and limited opportunity to identify men experiencing domestic abuse |
• Educational events on domestic abuse for community nursing staff • Adoption and commissioning of gender- neutral policies in healthcare • SCPHN advocacy and leadership to achieve equality in service delivery |
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical approval
Ethical approval for the study was granted by the Research Ethics Panel at Buckinghamshire New University (Reference: UEP2021 May01 Perryman; Date of approval: 15 June 2021). Verbal and written informed consent were obtained from all study participants.
