Abstract
Surgical incision-induced nociception contributes to the occurrence of postoperative cognitive dysfunction. However, the exact mechanisms involved remain unclear. Brain-derived neurotrophic factor (BDNF) has been demonstrated to improve fear learning ability. In addition, BDNF expression is influenced by the peripheral nociceptive stimulation. Therefore, we hypothesized that surgical incision-induced nociception may cause learning impairment by inhibiting the BDNF/tropomyosin-related kinase B (TrkB) signaling pathway. The fear conditioning test, enzyme-linked immunosorbent assay, and Western blot analyses were used to confirm our hypothesis and determine the effect of a plantar incision on the fear learning and the BDNF/TrkB signaling pathway in the hippocampus and amygdala. The freezing times in the context test and the tone test were decreased after the plantar incision. A eutectic mixture of local anesthetics attenuated plantar incision-induced postoperative pain and fear learning impairment. ANA-12, a selective TrkB antagonist, abolished the improvement in fear learning and the activation of the BDNF signaling pathway induced by eutectic mixture of local anesthetics. Based on these results, surgical incision-induced postoperative pain, which was attenuated by postoperative analgesia, caused learning impairment in mice partially by inhibiting the BDNF signaling pathway. These findings provide insights into the mechanism underlying surgical incision-induced postoperative cognitive function impairment.
Keywords
Background
Postoperative cognitive dysfunction (POCD) is characterized by a decline in cognitive functions, such as cognitive flexibility, attention, and working memory, arising after anesthesia and surgery. 1 POCD has an adverse effect on daily life and is associated with increased mortality within one year after surgery. 2 According to previous clinical studies, postoperative pain, which is not uncommon in surgical patients, increases the occurrence of POCD. 3 The underlying mechanism of POCD is complex and largely remains unknown.
Brain-derived neurotrophic factor (BDNF) belongs to the neurotrophin family and is widely expressed in the central nervous system, such as the hippocampus, amygdala, cortex, and spinal cord nuclei. 4 BDNF plays pivotal roles in learning, memory, and pain processing.5–7 Deprivation of endogenous BDNF impairs axon regeneration and myelination, 8 whereas increased BDNF expression in the hippocampus or amygdala improves fear learning in rodents.9–11 Phosphorylation of the high-affinity receptor of BDNF, tropomyosin-related kinase B (TrkB), leads to activation of the Ras-extracellular signal-regulated kinase (ERK) signaling pathway and the phosphatidylinositol 3-kinase-protein kinase B (AKT) signaling pathway.11,12 The BDNF/TrkB signaling pathway is involved in regulating fear learning by modulating the transcription of specific genes that contribute to long-term potentiation, long-term depression, and short-term synaptic plasticity. 13 In vivo studies have also shown that the BDNF/TrkB signaling pathway modulates the fear learning process mainly by targeting the hippocampus and amygdala.14,15
Therefore, we hypothesized that the decrease in BDNF expression and impaired activation of the BDNF/TrkB signaling pathway induced by postoperative pain are involved in the occurrence of surgical incision-induced POCD. We investigated the effects of a surgical incision on postoperative pain and the performance of fear learning tasks to test this hypothesis. We tested the ability of a eutectic mixture of local anesthetics (EMLA, 2.5% lidocaine and 2.5% prilocaine) to mitigate the effects of postoperative pain on learning impairment as an additional method to further confirm the effect of postoperative pain on cognitive function. Furthermore, we examined whether the TrkB antagonist, ANA-12, prevented the effects of analgesia on postoperative learning ability to confirm whether the BDNF/TrkB signaling pathway was involved in pain-related learning impairment. Our study aimed to investigate the association between postoperative pain and surgical incision-related fear learning impairment.
Materials and methods
Animals
Nine-month-old male C57BL/6 mice weighing 32 to 38 g were purchased from the experimental animal center of Peking Union Medical College, Chinese Academy of Medical Science (Beijing, China) and randomly assigned to the surgical or control groups. The mice were housed under standardized barrier breeding conditions (20°C–22°C; 12 h) with free access to food and water. Adequate measures were taken to minimize the number of animals used and limit distress to the animals.
Plantar incision surgery
Surgical incisions in both the left and right hind paws of each mouse were performed under anesthesia (1.5% isoflurane anesthesia for 15 min). Briefly, a 0.5-cm longitudinal incision was initiated 0.2 cm from the proximal edge of the heel and extended toward the toes under sterile conditions, as described in a previous study. 16 The flexor digitorum brevis was separated and incised longitudinally. Transection of the muscle was avoided. The incision in the skin was closed with a 5-0 nylon monofilament suture and covered with a 10% povidone-iodine solution. The rectal temperature was maintained at 37 ± 0.5°C during the surgical procedure using a homoeothermic blanket. The mice were allowed to recover in cages with sterile bedding after surgery. Mice in the isoflurane group received anesthesia but did not receive plantar incisions. Neither anesthesia nor surgery was performed on mice in the control group.
Drug treatment
EMLA (2.5% lidocaine and 2.5% prilocaine) was applied to the wounds of the EMLA treatment group every 8 h for seven consecutive days after surgery. Mice were placed in a plastic cage on a mesh platform. EMLA was smeared onto the wounds using a cotton swab. The mice were observed for 5 min in the plastic cage before they were put back to the rearing cage. Mice in the surgery group underwent handling and observation, but their wounds were not treated with EMLA after surgery. ANA-12 (Sigma-Aldrich, St. Louis, MO), a TrkB antagonist, was dissolved in corn oil (Sigma-Aldrich) containing 1% dimethyl sulfoxide (Sigma-Aldrich). In the ANA-12 group, mice received an intraperitoneal injection of 0.5 mg/kg ANA-12 every 12 h for three days after surgery. The dose of ANA-12 used in our study was 0.5 mg/kg which was determined according to the previous studies.10,17,18 In the vehicle group, mice received an intraperitoneal injection of 0.5 mg/kg vehicle every 12 h for three days after surgery.
Behavioral assessment of pain
Behavioral assessments were performed by an experimenter who was blinded to the experimental schedule. The nociception threshold was measured using von Frey filaments as described in previous studies.3,19 Mice were placed in a plastic cage (8 cm diameter × 20 cm high) on a mesh platform (5 mm long × 5 mm wide grid) 20 min before the test. An ascending series of von Frey filaments, starting with 0.07 g and ending with 4.0 g as the cutoff value (North Coast Medical, Elmont, NY), were applied on the wound edge for 5 s, with a 10 s interval between stimulations. The other hind paw was subjected to the same testing procedure at 5 min intervals. Each monofilament was applied to the hind paw five times. Brisk withdrawal of the hind paw, or paw flinching, was defined as a positive response. If the mouse withdrew its paw three times among the five stimulations, the force (in grams) was recorded as the nociception threshold.
Open-field test
Spontaneous locomotor activity was measured in the open field by an experimenter blinded to the experimental schedule. Animals were placed in the same corner of a white open arena (50 cm long × 50 cm wide × 30 cm high) and allowed to move freely for 5 min during the recordings. The open field was cleaned with 70% ethanol after each test. The distance traveled and time spent in the center zone were recorded and analyzed with the Ethovision XT software (Noldus Information Technology, the Netherlands).
Fear conditioning test
The fear conditioning test was performed as described in a previous report by an experimenter blinded to the experimental schedule. 3 Training for the fear conditioning test was performed 24 h after surgery. Mice were placed in a test chamber that had been wiped with 70% ethanol. After being allowed to freely explore the chamber for 180 s, mice were subjected to the tone-foot shock pairing (tone 1500 Hz, 80 dB, 60 s; foot shock 0.8 mA, 0.5 s). Context and tone learning were examined three days after surgery. In the context test, mice were placed in a new chamber with a different scent and context than those of the training chamber. The mice were allowed to explore freely in the chamber for 180 s, followed by another 180 s without a tone and, finally, 30 s for recovery. In the tone test, mice were placed in a chamber with the same scent and context as that used during training. The mice were allowed to explore freely in the chamber for 180 s, followed by another 180 s with a tone (1500 Hz, 80 dB), and, finally, 30 s for recovery. Freezing behavior was defined as complete immobility except for respiration. Freezing time was recorded by a camera and analyzed with the SuperMaze software (Xinruan Information Technology, Shanghai, China) during the second 180 s period.
Western blot analysis
The hippocampus and amygdala were harvested from anesthetized mice and frozen in liquid nitrogen. Tissues were homogenized on ice for total protein analysis with a radioimmunoprecipitation assay (0.1% sodium dodecyl sulfate (SDS), 0.5% Na deoxycholate, 1% NP40, 1 mM EDTA, 20 mM Tris-HCl, and 150 mM NaCl) in the presence of a protease inhibitor cocktail and phosphatase inhibitors (Sigma-Aldrich). Supernatants were collected and denatured with SDS-polyacrylamide gel electrophoresis (SDS-PAGE) loading buffer (0.25 M Tris-HCl, 0.1% bromophenol blue, 5% β-mercaptoethanol, 6% SDS, and 52% glycerol). The proteins were separated via SDS-PAGE and then transferred to polyvinylidene difluoride membranes (GE, Fairfield, CT). The membranes were blocked with 5% bovine serum albumin in Tris-buffered saline with 0.1% Tween 20 (TBST) for 1 h at room temperature and then incubated with primary antibodies at 4°C overnight. Next, the membranes were washed with TBST and incubated with secondary antibodies for 1 h at room temperature (antibodies used for Western blot analysis are listed in Table 1). Bands were detected with enhanced chemiluminescence reagents (CWBio, Beijing, China) and visualized using the GE ImageQuant LAS4000 mini chemiluminescence imaging analysis system (GE). The results were analyzed with ImageJ Software (National Institutes of Health, Bethesda, MD).
Antibodies used for Western blot analysis.

Abbreviations: AKT: protein kinase B; ERK: extracellular signal-regulated kinase; GAPDH: glyceraldehyde 3-phosphate dehydrogenase; IgG: immunoglobulin G; IL: interleukin; pERK: phosphorylated ERK; pAKT: phosphorylated AKT; pTrkB; phosphorylated TrkB; TrkB: tropomyosin-related kinase B.
apTrkB antibody (Abcam, catalog #ab109684) was used for Western blot in one research article (PubMed ID: 27297627).
bTrkB antibody (Abcam, catalog #ab18987) was used for Western blot in seven research article (PubMed ID: 28394765, 27297627, 26192455, 24465591, 25132263, 25239601, and 22232032).
Enzyme-linked immunosorbent assay
The hippocampus and amygdala were collected at three days or seven days after surgery. BDNF levels were quantified using enzyme-linked immunosorbent assay kits (Promega, Madison, WI) according to the manufacturer’s instructions. Each sample was measured in duplicate. The absorbance of each microwell was determined at a 450 nm wavelength with a microplate reader (Bio-Rad iMark, Hercules, CA). BDNF levels were normalized to the total protein content. The total protein concentration was measured using a Bicinchoninic Acid Protein Assay Kit (CWBio, Beijing, China).
Statistical analysis
Normally distributed data were presented as the mean ± standard deviation and analyzed using one-way analysis of variance or Student’s t test. Nonnormally distributed data were presented as the median and interquartile range and analyzed with the Mann–Whitney test or the Kruskal–Wallis test. Statistical analyses were performed using SPSS 20 (IBM, Armonk, NY). A significant difference was defined as P < 0.05 (two-sided).
Results
Plantar incision-induced pain and learning impairment
The plantar incision induced significant mechanical hyperalgesia in the right and left hind paws of mice. Compared with the control group, mice in the surgery group showed a decrease in the mechanical withdrawal threshold of both the right (Figure 1a) and left hind paws (Figure 1b) from one to five days after surgery. Similar to the results from the nociceptive behavioral tests, we further found that the plantar incision surgery reduced the freezing times in the context and tone tests of the fear conditioning assessment at three days (context test: 14.4 (5.6) vs. 34.6 (21.5) s; tone test: 18.3 (20.3) vs. 96.9 (40.9) s) but not seven days (context test: 9.9 (8.5) vs. 14.6 (5.9) s; tone test: 19.0 (8.8) vs. 18.7 (9.3) s) after surgery compared to those in the control group (Figure 1c, 1d). The isoflurane group displayed similar mechanical withdrawal thresholds and freezing times as the control group in both the context and tone tests of the fear conditioning assessments (Figure 1).
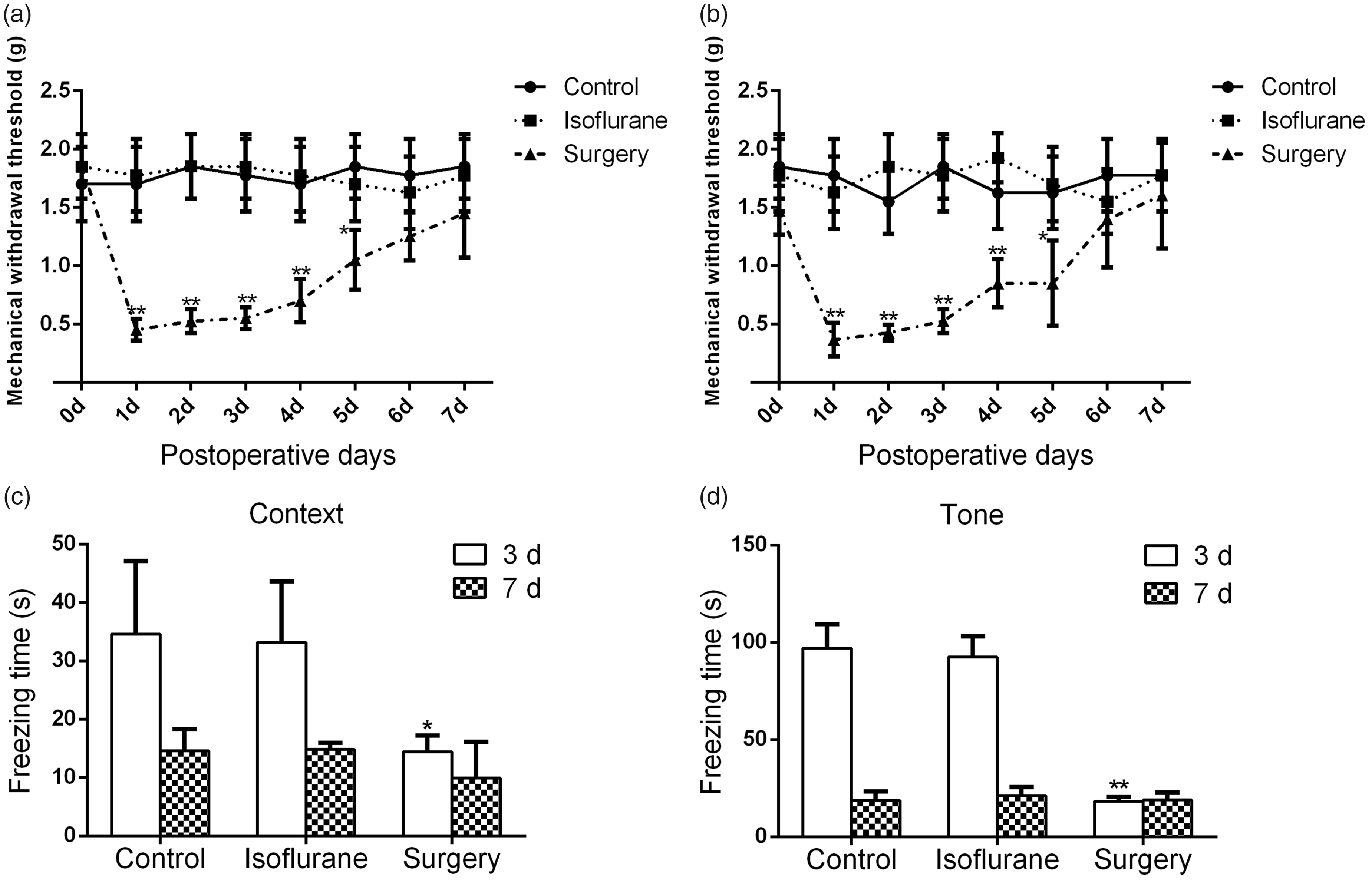
Decreased nociceptive threshold and freezing time after plantar incision. Plantar incision induced mechanical allodynia in both right hind paw (a) and left hind paw (b) at one to five days after surgery. Plantar incision decreased freezing time in the context test (c) and tone test (d) of the fear conditioning test at three days after surgery. N = 8 in each group, *P < 0.05 versus control or isoflurane, **P < 0.01 versus control or isoflurane.
EMLA attenuated the plantar incision-induced pain
The mechanical withdrawal thresholds of both the right (Figure 2a) and left hind paws (Figure 2b) were significantly increased in the EMLA group from one to five days after plantar incision compared with the surgery group. The mechanical withdrawal threshold returned to the preoperative levels at five days after surgery. No significant differences in the mechanical withdrawal threshold were observed among the EMLA group, the surgery group, and the isoflurane group at five days after surgery.

Attenuated pain and increased freezing time after EMLA treatment. EMLA treatment increased nociceptive threshold in right hind paw (a) and left hind paw (b) after plantar incision. Plantar incision-induced reduction in freezing time in the context test (c) and tone test (d) of the fear conditioning test were attenuated by EMLA treatment at three days after surgery. Plantar incision had no effect on the travel distance (e) and time spent in the center zone (f) in the open-field test at three days after surgery. N = 8 in each group, *P < 0.05 versus isoflurane, **P < 0.01 versus isoflurane, #P < 0.05 versus EMLA, and ##P < 0.01 versus EMLA. EMLA: eutectic mixture of local anesthetics.
Our results also revealed that mice in the surgery group had no significant difference with the mice in the isoflurane group in the travel distance (Figure 2e) and the time spent in the center zone (Figure 2f) in the open-field test at three days after surgery (travel distance: 26.1 ± 4.2 vs. 26.3 ± 3.9 m; time spent in the center zone: 2.8% (1.8%) vs. 3.4% (1.7%)).
EMLA attenuated the plantar incision-induced fear learning impairment and increased the activation of the BDNF/TrkB signaling pathway in the hippocampus
The results obtained from the fear conditioning system showed that EMLA treatment significantly attenuated the plantar incision-induced decrease in freezing time in both the context test (Figure 2c) and tone test (Figure 2d) compared to that in the surgical group at three days after surgery (context test: 32.5 (14.2) vs. 14.4 (5.6) s; tone test: 67.3 (27.1) vs. 18.3 (20.3) s).
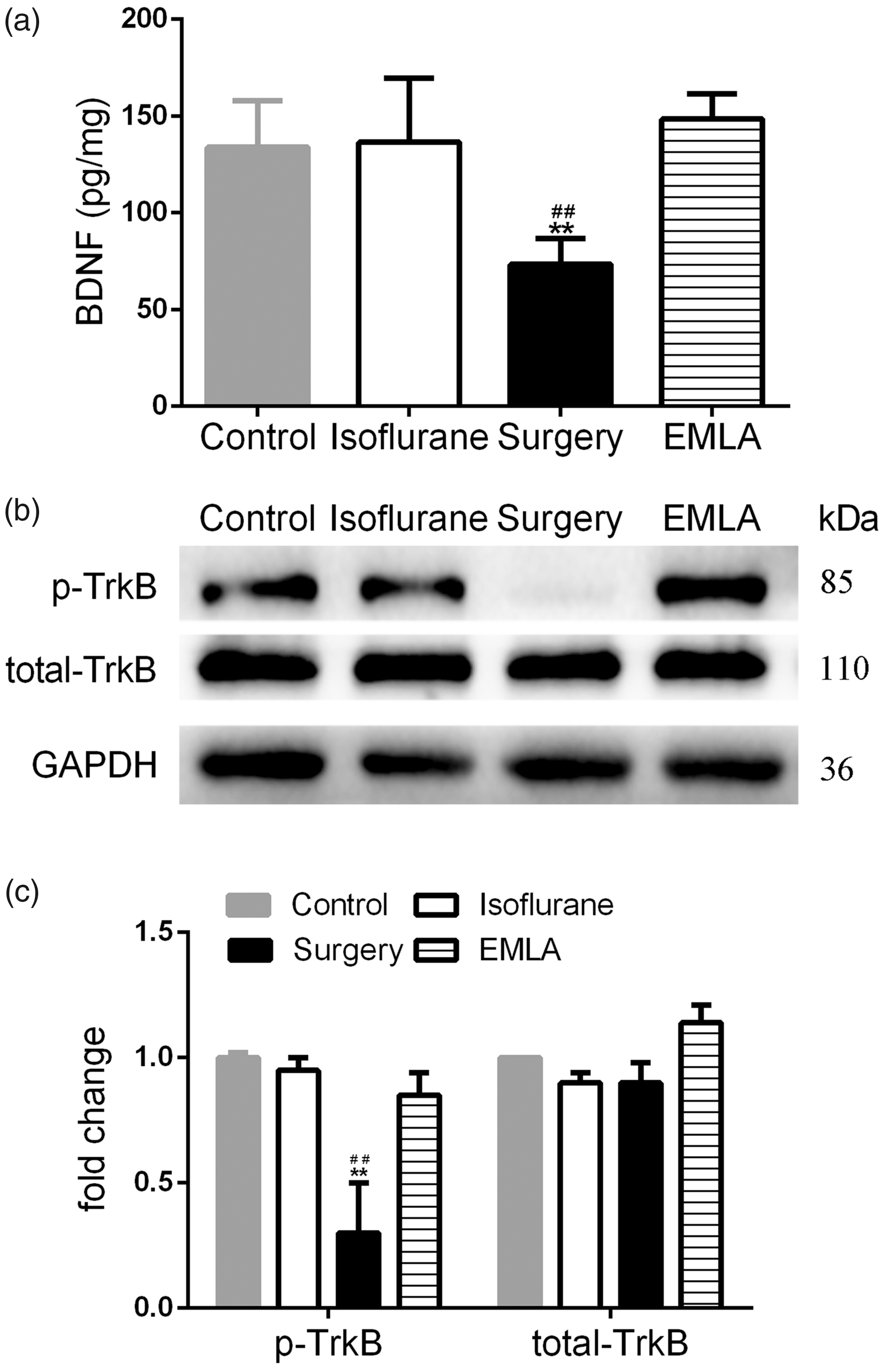
EMLA treatment attenuated plantar incision-induced decrease in BDNF expression and TrkB activation in the hippocampus. (a) Plantar incision-induced decrease in BDNF expression is attenuated by EMLA treatment at three days after surgery. (b) Western blot analysis shows the expression of total TrkB and activated pTrkB in hippocampus. (c) Data summary of panel b. N = 5 in each group, *P < 0.05 versus control or isoflurane, **P < 0.01 versus control or isoflurane, #P < 0.05 versus EMLA, and ##P < 0.01 versus EMLA. BDNF: brain-derived neurotrophic factor; EMLA: eutectic mixture of local anesthetics; TrkB: tropomyosin-related kinase B; GAPDH: glyceraldehyde 3-phosphate dehydrogenase; pTrkB: phosphorylation of TrkB.
The expression of BDNF in the hippocampus in the surgery group (73.3 ± 13.5 pg/mg) was significantly decreased at three days after plantar incision compared to the isoflurane group (136.4 ± 33.0 pg/mg) and the control group (133.8 ± 24.2 pg/mg) (Figure 3a). Phosphorylation of TrkB (pTrkB), a receptor for BDNF, was significantly reduced in the surgery group compared with that in the isoflurane and control groups at three days after surgery (Figure 3b).
Given that EMLA significantly increased the mechanical threshold in the paw after surgery, we examined whether inhibition of the BDNF-TrkB signaling pathway could also be attenuated by EMLA. Levels of the BDNF and pTrkB proteins were significantly increased in the EMLA group compared with the surgery group (0.85 ± 0.09 vs. 0.31 ± 0.21).
EMLA attenuated the plantar incision-induced activation of AKT and ERK in the hippocampus
The plantar incision induced marked increases in the levels of phosphorylation of ERK (pERK) (Figure 4a) and phosphorylation of AKT (pAKT) (Figure 4b) at three days after surgery in the surgery group. Compared with the surgery group, the EMLA group exhibited decreased levels of pAKT (2.53 ± 0.21 vs. 1.38 ± 0.18) and ERK (2.35 ± 0.20 vs. 1.20 ± 0.16).
EMLA attenuated the plantar incision-induced interleukin (IL)-1β and IL-6 levels in the hippocampus
IL-1β and IL-6 have been shown to regulate BDNF expression and are involved in the ERK and AKT signaling pathways. 20 We therefore determined the effects of the plantar incision on the IL-1β and IL-6 levels in the hippocampus (Figure 5a). The levels of IL-6 and IL-1β were significantly increased in the surgery group compared with the isoflurane group at three days after surgery (IL-6: 2.69 ± 0.15 vs. 1.20 ± 0.08; IL-1β: 3.89 ± 0.19 vs. 0.95 ± 0.07). Furthermore, the high levels of IL-6 and IL-1β observed in the mouse hippocampus after surgery were mitigated by the EMLA treatment. The expression of IL-6 and IL-1β was significantly decreased in the EMLA group (IL-6: 1.32 ± 0.14; IL-1β: 1.30 ± 0.17) compared with the surgery group at three days after surgery.
EMLA attenuated the plantar incision-induced decrease in BDNF expression and activation of ERK and AKT in the amygdala
The plantar incision significantly decreased the levels of BDNF (124.4 ± 23.6 pg/mg) (Figure 6a) and pTrkB (0.48 ± 0.23) (Figure 6b, 6c) but increased the levels of pAKT (2.28 ± 0.25) (Figure 6d, 6e) and pERK (2.58 ± 0.22) (Figure 6f, 6g). Similar to the changes in the hippocampus, the levels of BDNF (183.8 ± 32.1) (Figure 6a) and pTrkB (0.95 ± 0.11) (Figure 6b, 6c) but not the levels of pAKT (1.25 ± 0.17) (Figure 6d, 6e) and pERK (1.35 ± 0.15) (Figure 6f, 6g) in the amygdala were also increased by EMLA treatment compared to those in the surgery group.
ANA-12 blocked the EMLA-induced amelioration of learning impairment
We used ANA-12 to inhibit the BDNF-TrkB signaling pathway and determine its role in plantar incision-induced learning impairment. The freezing times in both the context test (Figure 7a) and the tone test (Figure 7b) were significantly decreased in the ANA-12 group compared with the vehicle group (context test: 6.9 (6.6) vs. 25.1 (9.4) s; tone test: 14.9 (8.3) vs. 67.3 (17.9) s).

Plantar incision increased pAKT and pERK levels in the hippocampus. (a) Western blot analysis shows the expression of total ERK and activated pERK in the hippocampus. (b) Western blot analysis shows the expression of total AKT and activated pAKT in the hippocampus. (c) Data summary of panel (a). (d) Data summary of panel (b). N = 5 in each group. **P < 0.01 versus control or isoflurane and ##P < 0.01 versus EMLA. EMLA: eutectic mixture of local anesthetics; GAPDH: glyceraldehyde 3-phosphate dehydrogenase; ERK: extracellular signal-regulated kinase; pERK: phosphorylated ERK; AKT: protein kinase B; pAKT: phosphorylation of AKT.

EMLA treatment attenuated plantar incision-induced increase in IL-1β and IL-6 expression in the hippocampus. (a) Western blot analysis shows the expression of pro-IL-1β, IL-1β, and IL-6 in the hippocampus. (b) Data summary of panel (a). N = 5 in each group. **P < 0.01 versus control or isoflurane and ##P < 0.01 versus EMLA. EMLA: eutectic mixture of local anesthetics; GAPDH: glyceraldehyde 3-phosphate dehydrogenase; IL: interleukin.
ANA-12 suppressed the pTrkB, pAKT, and pERK in the hippocampus and amygdala
The Western blot results showed a significant decrease in the level of pTrkB in the hippocampus and amygdala following ANA-12 treatment (hippocampus: 0.58 ± 0.07; amygdala: 0.70 ± 0.08) compared with the EMLA group (hippocampus: 0.85 ± 0.09; amygdala: 1.01 ± 0.02). Moreover, compared with the EMLA group, ANA-12 treatment decreased the pAKT (hippocampus: 0.63 ± 0.09 vs. 1.38 ± 0.18; amygdala: 0.61 ± 0.10 vs. 1.03 ± 0.05) and pERK (hippocampus: 0.55 ± 0.08 vs. 1.20 ± 0.16; amygdala: 0.55 ± 0.07 vs. 1.05 ± 0.06) levels in the hippocampus (Figure 8a, 8c) and amygdala (Figure 8b, 8d).
Discussion
In the present study, the nociceptive stimulation induced by the plantar incision impaired fear learning ability in mice. In addition, the blockade of pain stimulation by EMLA improved the fear learning ability after surgery. The plantar incision decreased the expression of BDNF and inhibited the activation of the BDNF/TrkB signaling pathway in the hippocampus and amygdala. A TrkB receptor antagonist, ANA-12, inhibited the activation of the BDNF signaling pathway and the improvement in fear learning induced by the EMLA treatment. Based on these results, the surgical incision itself might induce learning impairment, and these impairments were partially mediated by BDNF and its downstream signaling pathway.
A decrease in the nociceptive threshold was observed after surgery, which confirmed the effects of the surgical stimulation after the operation. In addition, the freezing times in both the conditioning test and the tone test were significantly decreased in the surgery group compared with the control group. Because a shorter freezing time reflects a disruption of the fear learning function, 21 this result suggested that the surgery group exhibited an impaired fear learning ability compared with the control group, and the learning impairment observed after surgery might be caused by the plantar incision. The surgical incision was a strong nociceptive stimulus both during and after surgery. In terms of neural signaling, the signal from the unblocked nociceptive stimulus was transduced to the spinal cord and brain, leading to the release of excitatory neurotransmitters 22 and alterations in neuronal firing activity patterns, 23 which ultimately resulted in cognitive changes. In addition, we used EMLA to inhibit the surgical stimuli to clarify whether the cognitive dysfunction observed in this study was induced by the nociceptive stimulus. The results showed that EMLA treatment could increase the nociceptive threshold after surgery, which suggested that EMLA partially inhibited the transduction of peripheral nociceptive stimuli caused by the plantar incision. Meanwhile, a prolonged freezing time, which indicated a better fear learning ability, was observed after the plantar incision in the EMLA group compared with the surgery group. Based on these findings, the impairment in fear learning function was related to the transmission of nociceptive stimulation after surgery.

EMLA treatment attenuated plantar incision-induced decrease in BDNF expression and activation of TrkB signaling pathway in the amygdala. (a) Plantar incision-induced decrease in BDNF expression is attenuated by EMLA treatment at three days after surgery. (b) Western blot analysis shows the expression of total TrkB and activated pTrkB. (c) Data summary of panel (b). (d) Western blot analysis shows the expression of total AKT and activated pAKT. (e) Data summary of panel (d). (f) Western blot analysis shows the expression of total ERK and activated pERK. (g) Data summary of panel (f). N = 5 in each group, *P < 0.05 versus control or isoflurane, **P < 0.01 versus control or isoflurane, #P < 0.05 versus EMLA, and ##P < 0.01 versus EMLA.EMLA: eutectic mixture of local anesthetics; GAPDH: glyceraldehyde 3-phosphate dehydrogenase; ERK: extracellular signal-regulated kinase; pERK: phosphorylation of ERK; AKT: protein kinase B; pAKT: phosphorylation of AKT; TrkB: tropomyosin-related kinase B; pTrkB: phosphorylation of TrkB; BDNF: brain-derived neurotrophic factor.

Decreased freezing time after ANA-12 treatment. ANA-12 treatment induced reduction in freezing time in the context test (a) and tone test (b) of the fear conditioning test at three days after surgery. N = 8 in each group, *P < 0.05 versus isoflurane or vehicle and **P < 0.01 versus isoflurane or vehicle.
The plantar incision model was used in our study. To strengthen the nociceptive effect of plantar incision, an incision was made in both hind paws in our study. Accordingly, both sides of the hippocampus and the amygdala were acquired and examined in this study. Open-field test was used to evaluate the locomotor activity levels which can affect the freezing time in the fear conditioning test in our study. The results suggested plantar incision had no significant effect on the locomotor activity ability at three days after surgery. In this study, the open-field test was done after a three days recovery from the plantar incision. In order to decrease the effect of surgery on locomotor activity, the flexor digitorum brevis was incised longitudinally, and the tendon was kept intact. Increased anxiety also resulted in less locomotion. 24 The time spent in the center zone in the open-field test was examined to assess the degree of anxiety after surgery. Our results shown that no significant difference of the time spent in the center zone was found in the open-field test. These results excluded the effect of anxiety on the exploratory activity at three days after surgery.
In the present study, we also found that the expression of BDNF was decreased after the plantar incision. The hippocampus and the amygdala were the brain regions involved in regulating context-related fear learning and tone-related fear learning, respectively. 25 Our results showed that the BDNF levels in the hippocampus and amygdala were decreased at three days after the plantar incision. However, BDNF expression was significantly increased in the EMLA group after blocking the nociceptive stimulation by the EMLA treatment. These results further indicated that the transduction of signals induced by surgical stimuli decreased the expression of BDNF. BDNF is an important neurotrophic factor that participated in cognitive function. 5 Consistent with the previous studies, impaired fear learning was observed in the group displaying decreased BDNF expression in the present study. As the high-affinity receptor for BDNF, TrkB was phosphorylated following its binding to BDNF. 10 Consistent with our results regarding BDNF expression, decreased pTrkB was observed in the surgery group, and this change was attenuated by the EMLA treatment. To confirm the effect of surgical incision-induced nociception on BDNF signaling pathway activation, ANA-12 was used to block the combination of BDNF and TrkB. 26 ANA-12 attenuated the increase in pTrkB and improvement in fear learning ability induced by surgical stimuli blockade. These data suggested that plantar incision-induced nociception decreased fear learning function by inhibiting the BDNF signaling pathway.

ANA-12 treatment decreased the pTrkB, pAKT, and pERK in the hippocampus and amygdala. (a) Western blot analysis shows the expression of pTrkB, pAKT, and pERK in the hippocampus. (b) Western blot analysis shows the expression of pTrkB, pAKT, and pERK in the amygdala. (c) Data summary of panel (a). (d) Data summary of panel (b). N = 5 in each group, ##P < 0.01 versus EMLA. EMLA: eutectic mixture of local anesthetics; GAPDH: glyceraldehyde 3-phosphate dehydrogenase; ERK: extracellular signal-regulated kinase; pERK: phosphorylation of ERK; AKT: protein kinase B; pAKT: phosphorylation of AKT; TrkB: tropomyosin-related kinase B; pTrkB: phosphorylation of Trkb.
Our results showed that the expression of pERK and pAKT were increased in the surgery group compared with the isoflurane group. However, BDNF was not the only factor that resulted in increased expression of pERK and pAKT.27–29 Our results also suggested that the expression of IL-6 and IL-1β was increased in the surgery group compared with the isoflurane group. Increased expression of pERK and pAKT was the result of inflammatory cytokines and BDNF. Combined with the previous studies,30,31 it could be inferred from our results that both the decrease in BDNF caused by neural transduction of nociceptive stimulation and increase in inflammation caused by surgical injury were participated in the occurrence of POCD. To confirm the role of BDNF signaling pathway in plantar incision-induced learning impairment, the BDNF signaling pathway was blocked by ANA-12. The expression of pERK and pAKT significantly decreased in the ANA-12 group comparison with the EMLA group. These findings suggested the expression of pERK and pAKT was partially determined by the BDNF signaling pathway. Our results indicated that blocking surgical stimuli increased the activation of BDNF/TrkB signaling pathway. The current findings further suggested that plantar incision induced fear learning impairment by inhibiting the BDNF/TrkB signaling pathway.
Our study has several limitations. First, in this study, we explored the effect of surgical incision-induced nociception on the fear learning ability after surgery. Other cognitive functions and emotional changes related to POCD, such as memory loss and depression, were not examined in this study. Further studies are still needed to illuminate the role of surgical incision-induced nociception on other aspects of cognitive function. Second, we focused on the effect of the BDNF/TrkB signaling pathway on surgical incision-induced learning impairment. The interactions of BDNF with other well-documented receptors that participate in cognitive function, such as NMDA receptors and cholinergic receptors, will be investigated in our future studies.
Conclusions
The present study demonstrated that plantar incision decreased the levels of BDNF in the hippocampus and amygdala and impaired fear learning ability in mice which can be attenuated by blocking the transduction of surgical stimuli. Our results indicated that the BDNF/TrkB signaling pathway participated in surgical incision-induced POCD. These findings helped us understand the influence of nociceptive stimulation on the nervous system after surgery.
Footnotes
Author Contributions
JZ, CM, and ZL conceived and designed the experiment, supervised research, and wrote the manuscript. XL, FL, and ZL performed the experiments, analyzed the data, and helped write the manuscript. All authors have read and approved the final manuscript.
Declarations of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethics Approval
All animal experiments complied with the Ethics and Animal Welfare Committee guidelines for the care and use of laboratory animals and were approved by the Ethics Committee of Peking Union Medical College Hospital (XHDW-2015–0041).
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Scientific Research Fund of China-Japan Friendship Hospital (2017-RC-3), a nonfinancial foundation. The funding body has not participated in the design of the study, the collection, analysis, and interpretation of data or the writing of the manuscript.
