Abstract
Objective
To assess the association between the Mannose-binding lectin (MBL) gene polymorphism and the susceptibility to sepsis using a meta-analysis.
Methods
The publications were searched on PubMed, Embase, and Web of Science databases up to December 1, 2019 for relevant literature.
Results
A total of 32 studies (21 adult and 11 pediatric studies) were selected for analysis. Overall, in the three models of MBL +54 A/B gene polymorphisms, namely the dominant model BB + AB vs. AA (p = 0.03), the recessive model BB vs. AB + AA (p < 0.00001), and the allele model B vs. A (p = 0.04), MBL +54 A/B was significantly related to the risk of sepsis. In the adult group, the MBL A/O gene polymorphism was associated with the risk of sepsis in the dominant model AO + OO vs. AA (p = 0.006) as well as in the allele model O vs. A (p = 0.04). The MBL +54 A/B gene polymorphism was significantly related to the risk of sepsis in the recessive model and, therefore, may increase the risk of sepsis. In the pediatric group, no polymorphic loci were significantly associated with sepsis in any of the three models. The results of the publication bias test demonstrated no publication bias in an unadjusted estimate of the relationship between MBL A/O and −211Y/X gene polymorphism and sepsis.
Conclusions
The polymorphisms of MBL that are related to the occurrence of sepsis are primarily A/O and +54 A/B, while −221Y/X and −550H/L have no clear relationship with the susceptibility of sepsis in various age groups or different models.
Introduction
Sepsis is one of the most common serious complications following trauma, burns, shock, infections, and other clinically critical illnesses in patients and is also a primary cause of death in intensive care unit (ICU) patients. 1 The condition of sepsis is complex and can progress quickly. If not diagnosed and treated in time, it can easily develop into severe sepsis or even septic shock. Latest data in Highlights of the Report on Global Burden of Disease showed that nearly 50 million cases developed sepsis every year in the world.2,3 Sepsis had an estimated mortality of 11 million in 2017, which represented nearly 20% of all deaths globally. 2 Each year, at least 1.7 million adults in the United States developed sepsis, resulting in nearly 270,000 deaths. 4 Even when using the same intervention method, the clinical outcomes may be quite different among patients with sepsis. The international expert consensus is that the heterogeneity in host hereditary susceptibility might be in part responsible for the failure of clinical trials of treatments for patients with sepsis.5-7
Mannose-binding lectin (MBL) is one of the component glycoproteins of the complement system and is a first-line anti-infective molecule, playing a critical role in the body’s natural immunity and prevention of infection. MBL can affect the secretion of a series of cytokines, which influences the balance of inflammation in the mice and may mediate the progress of sepsis. 8 It was reported that MBL2 concentration, but not genotype, was a determinant of bacterial infection recurrence, low serum MBL concentrations may act as a predictor of bacterial infection recurrence. 9 In the study of Frakking FN, almost half of there NICU patients, especially the premature ones, were MBL deficient (MBL plasma concentrations ≤0.7 μg/ml) at birth. These infants may be at increased risk of neonatal infections. 10 MBL production is controlled by the MBL gene and its polymorphisms. 11 The close relationship between MBL polymorphic variants and plasma MBL concentration persists during sepsis, MBL genetic polymorphisms resulting in MBL deficiency are associated with increased susceptibility to sepsis. 12 And in intensive care unit, the patients with MBL polymorphisms and low levels of serum were easily to develop sepsis and fatal outcome.13,14 MBL gene mutations can cause a decrease in the level of MBL in the serum, hindering the activation of the complement system and affecting the body’s immune response.15,16
Current research on the MBL gene polymorphism primarily focuses on six polymorphic sites, including three mutation sites in the promoter region (−550H/L, −221X/Y, and +4P/Q) and three sites in the exon 1 region. Single-base mutations in codons 52, 54, and 57 in the exon 1 region results in the substitution of cysteine (Cys) for arginine (Arg), aspartic acid (Asp) for glycine (Gly), and glutamic acid (Glu) for glycine (Gly) in the encoded collagen amino acids. The alleles corresponding to the mutations at these three sites are named D, B, and C and are collectively referred to as O, with the wild type referred to as A. 17 The variants rs1800451 (C), rs1800450 (B), rs5030737 (D), rs7096206 (X/Y) and rs11003125 (H/L) were used for haplotype determination. 9 And the corresponding rs denominations of A/O,+54 A/B, - 221 YX and - 550H/L were marked respectively, for example: A/O (rs1800451, rs1800450, rs5030737), +54 A/B (rs1800450), - 221 YX (rs7096206), and - 550H/L (rs11003125). The above MBL gene polymorphic site mutations impact the protective effect of MBL on the body and can increase the susceptibility to infectious diseases. 18
Garred et al. 19 used blood samples from 272 patients with systemic inflammatory response syndrome (SIRS) to demonstrate that MBL mutant alleles primarily exist in patients with a high risk of sepsis. Furthermore, patients with low serum MBL levels are more likely to experience sepsis. Another study found that the blood MBL level of neonates and preterm infants with sepsis was significantly lower than that of children without sepsis and that preterm infants with MBL exon 1 allele B were more likely to develop neonatal sepsis and lung infections.17,18,20 Therefore, MBL expression level, activity changes, and genetic polymorphisms have a certain reference value for predicting the illness changes and the prognosis of patients with sepsis and are important candidate genes to study for early warning signs and diagnostic methods for sepsis. Dzwonek et al. 21 performed MBL phenotype and genotype analyses (A/O, A/A, and O/O) on 120 newborn samples the third day after birth and suggested that the risk of developing sepsis was not significantly related to the MBL genotype. Hartz et al. 18 recently conducted a large-scale study that collected samples from 6,878 extremely low birth weight infants, then genotyped MBL2 and divided the plasma levels into normal (A/A) and low (A/O or O/O), ultimately demonstrating no association between the MBL level based on genotype. However, there seemed to be an association between O/O MBL levels and the risk of gram-negative sepsis in babies born between 32 and 36 weeks gestation.
An increasing number of studies being reported on the association between the MBL gene polymorphism and the risk of sepsis, but the results obtained for different populations, regions, research design types, genotyping methods and sample sizes have varied greatly, to the point of being contradictory. Not all studies could provide and extract the genotype distribution data of case and control populations in detail, resulting in that some studies were only applicable to the analysis of a certain genetic model, which might also affect the authenticity and bias of the results.
Therefore, the current study used a comprehensive and systematic literature review to evaluate the published genetic association studies between MBL gene polymorphism and the risk of sepsis using a meta-analysis.
Materials and methods
Literature search
The three major medical literature databases of PubMed, Embase, and Web of Science were selected for the literature search; articles on the association between the MBL gene polymorphism and sepsis published before December 1, 2019 were selected. The search keywords used were “mannose binding lectin or MBL” and “sepsis or severe sepsis or septic shock or septicemia or bacteraemia” and “polymorphism or variant or mutation”. Studies that fulfilled the following criteria were selected: (1) The original article on the association between the MBL gene polymorphism and sepsis was published in a peer-reviewed journal; (2) the study design used cross-sectional observation or was a case-control, nested case-control, or cohort study; (3) the language of publication was English; (4) the paper provided statistical data on the association between various genotypes of the MBL gene polymorphism and the risk of sepsis, which could be used for the meta-analysis.
Literature quality assessment
Two investigators independently extracted data and cross-checked one another. After reviewing all the relevant data, EndNote X8 (Clarivate Analytics, PA, USA) was used to exclude overlapping documents between the databases. The two researchers then independently reviewed the titles and abstracts of every article, screening out relevant research documents according to unified standards, cross-checking the screening results, then discussing any inconsistencies until they reached a consistent conclusion. In addition, the original articles, reviews, and meta-analysis references that met the inclusion criteria were reviewed and the missing articles were supplemented, and finally, the summary analysis was performed.
Statistical analysis
All statistical analyses were performed using Review Manager 5.2 (The Cochrane Collaboration, Oxford, UK) and STATA 11.0 (StataCorp LP, College Station, Texas, USA). The included studies were first tested for heterogeneity. A p > 0.1 was used to indicate that the heterogeneity between the results of each study was not statistically significant, suggesting that the fixed effects model could be used for analysis, otherwise, the random-effects model was used. The heterogeneity analysis was conducted by using Cochran Q statistics and the I2 test to qualitatively and quantitatively evaluate the heterogeneity between the different studies of polymorphic sites of the same gene. The combined effect size, OR value, and its 95% CI were reported and a forest map was then drawn. The funnel plots, Begg’s test, and Egger’s test were used to assess the possibility of publication bias. Egger’s test p < 0.1 was considered a significant publication bias.
Results
Characteristics of studies included in the meta-analysis for paediatric.

A/O (rs1800451, rs1800450, rs5030737), +54 A/B (rs1800450), - 221 YX (rs7096206), and - 550H/L (rs11003125).
Characteristics of studies included in the meta-analysis for adult.
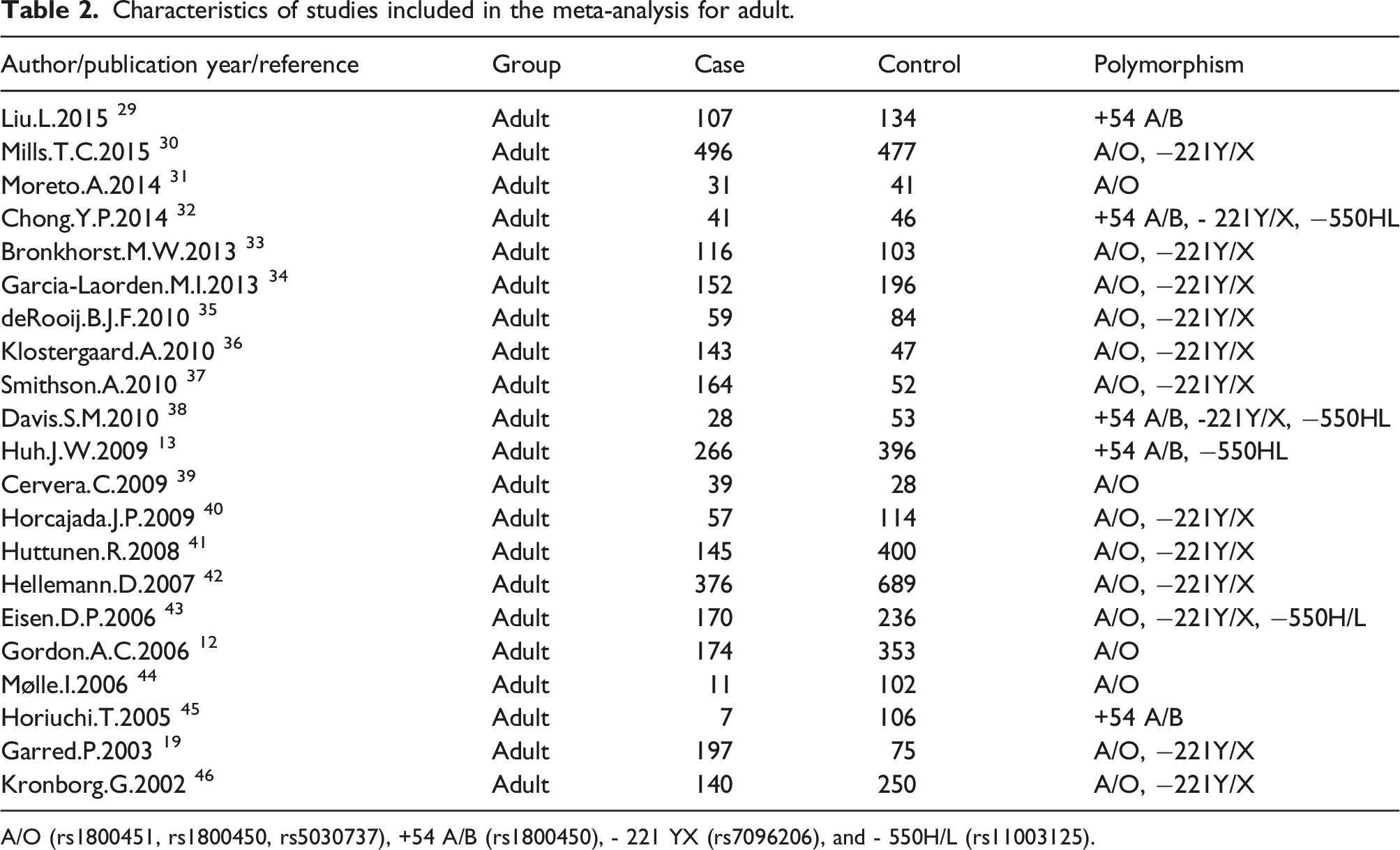
A/O (rs1800451, rs1800450, rs5030737), +54 A/B (rs1800450), - 221 YX (rs7096206), and - 550H/L (rs11003125).

Flow chart of literature search and selection process.
For overall meta-analysis of A/O polymorphism in the allele model O vs. A (OR = 1.14, 95% CI: 1.00–1.29, p = 0.04), allele O is related to the risk of sepsis and can increase the risk of sepsis (Figure 2). Also, significant correlation between +54 A/B polymorphism and the risk of sepsis was found in a dominant model (OR = 2.01, 95% CI: 1.08–3.75, p = 0.03), recessive model (OR = 6.32, 95% CI: 3.89–10.27, p < 0.00001) and allelic model (OR = 2.09, 95% CI: 1.03–4.24, p = 0.04) in overall comparison (Figure 3), while −221Y/X and −550H/L polymorphism have no obvious association with the susceptibility of sepsis in any models. Analysis of MBL A/O gene polymorphism and sepsis susceptibility in the allele model O vs. A. Analysis of MBL +54 A/B gene polymorphism and sepsis susceptibility in dominant model, recessive model and allelic model.

The results of the meta-analysis in the adult group suggest that the A/O gene polymorphisms in the dominant model (OR = 1.37, 95% CI: 1.10–1.72, p = 0.006) and the allelic model (OR = 1.19, 95% CI: 1.00–1.41, p = 0.04) are related to the susceptibility of sepsis (Figure 4). The +54 A/B gene polymorphism was associated with sepsis in the recessive model, demonstrating an increase in the risk of sepsis (OR = 6.32, 95% CI: 3.89–10.27, p < 0.00001, Figure 5). No positive association of the −221Y/X polymorphism was demonstrated with the susceptibility of sepsis. The analysis of MBL A/O gene polymorphism and sepsis susceptibility in adult dominant and allelic models. The analysis of MBL +54 A/B gene polymorphism and sepsis susceptibility in adult recessive models.

In the pediatric group, there was no positive association of A/O polymorphism observed with the risk of sepsis.
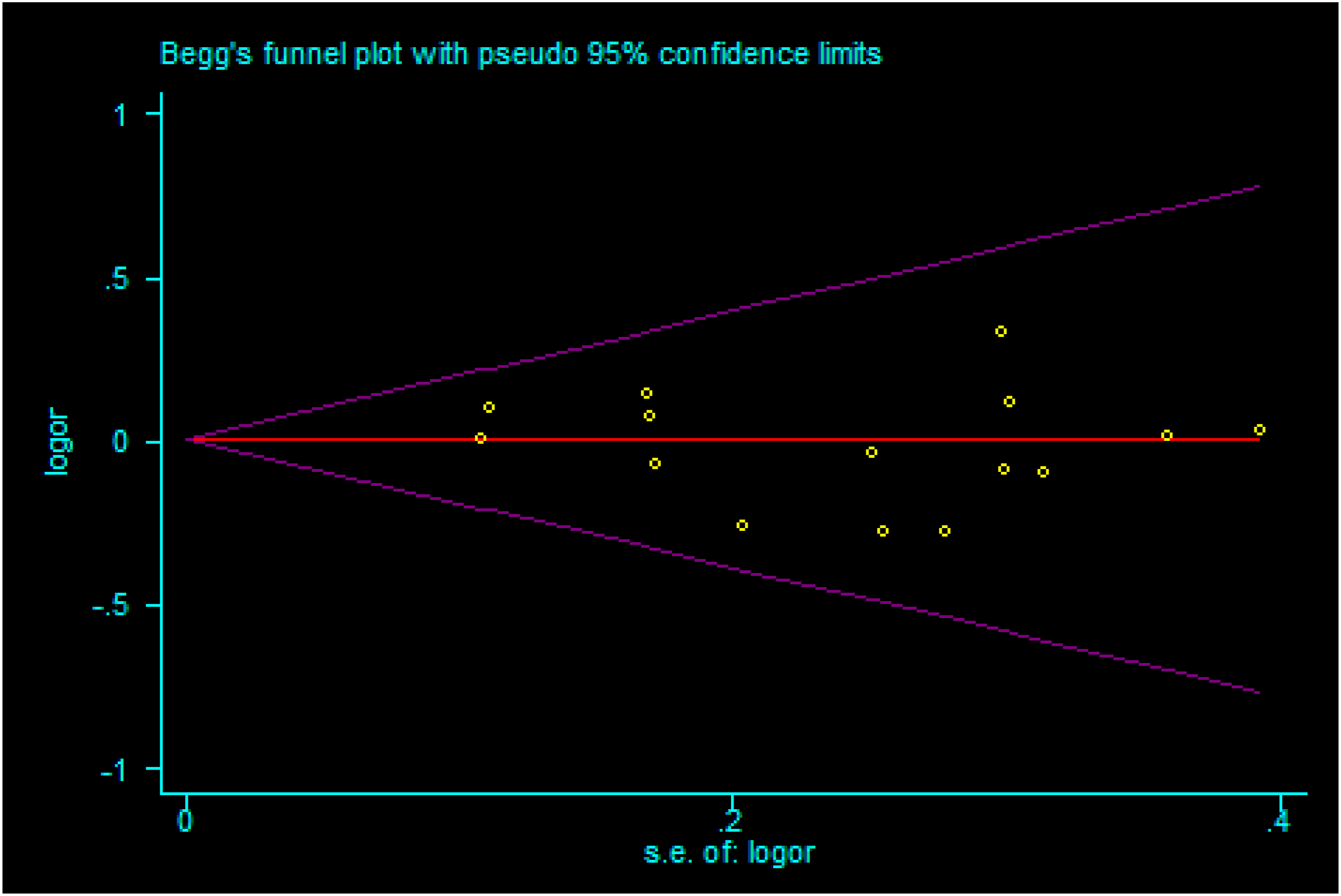
The funnel plots, Begg’s test, and Egger’s test were used to assess the possibility of publication bias. For the total and adult groups, the results demonstrated there was no publication bias in the unadjusted estimate of the association between MBL A/O and the −211Y/X gene polymorphism and sepsis; Egger’s test p = 0.270 and Begg’s test p = 0.266 in the allelic model O vs. A for the total group (Figure 6); Egger’s test p = 0.334 and Begg’s test p = 0.767 in the allelic model X vs. Y for the total group (Figure 7); Egger’s test p = 0.117 and Begg’s test p = 0.244 in the allelic model O vs. A in adults (Figure 8); Egger’s test p = 0.137, Begg’s test p = 0.304 in the allelic model X vs. Y in adults (Figure 9). The Begg funnel chart of the allelic model O vs. A in total, and no publication bias was found (Egger’s test p = 0.270 and Begg’s test p = 0.266). The Begg funnel chart of the allelic model X vs. Y in total, and no publication bias was found (Egger’s test p = 0.334 and Begg’s test p = 0.767). The Begg funnel chart of the allelic model O vs. A in adult, and no publication bias was found (Egger’s test p = 0.117 and Begg’s test p = 0.244). The Begg funnel chart of the allelic model X vs. Y in adult, and no publication bias was found (Egger’s test p = 0.137, Begg’s test p = 0.304).


Discussion
In recent years, there has been an increase in association studies between MBL gene polymorphism and sepsis in the world. Liu. et al. 29 performed genotyping (GG, GA, AA, G, A) on the MBL2 gene rs1800450 polymorphism (codon 54 A/B, G230 A) in patients with sepsis and found that allele genes can significantly increase the risk of sepsis. The GA genotype is closely related to the onset of sepsis, while the AA genotype is not significantly related to the occurrence of sepsis. Furthermore, the frequency of the GA genotype and the A allele based on the MBL2 gene rs1800450 polymorphism was significantly increased and further ELISA testing demonstrated that the serum MBL level of the sepsis group was significantly lower than that of the control group, as was the MBL level of the rs1800450 genotype. There was also a significant downward trend, so it is inferred that the rs1800450 A allele increases the risk of sepsis by reducing MBL levels. A study showed that the B allele of the A/B polymorphism is a risk factor for sepsis in Turks . 14 Huh et al. 13 included a total of 266 sepsis patients and 398 healthy patients and detected three single nucleotide polymorphisms (54, −550, +4) in the MBL2 gene related to sepsis in a Korean population. Seemingly, a single nucleotide polymorphism has nothing to do with the occurrence of sepsis, but the homozygosity of promoter 54 (A/A) and promoter −550 (H/H) is associated with the degree of severity of sepsis, but is not related to the outcome of sepsis. Mills et al. 30 genotyped and analyzed four MBL2 mononucleotide polymorphisms (rs5030737, rs1800450, rs1800451, rs7096206) in 1,839 European patients with community-acquired pneumonia and peritonitis sepsis and found that, in this large cohort of adult patients, there was no obvious association between the MBL2 gene polymorphism and the susceptibility to sepsis. The conclusions of these studies were not completely consistent, or even opposite, which might result from small quantity of samples, different geographic regions and ethnicities, etc. When the MBL gene polymorphism is inconsistent with the research results of sepsis susceptibility, a meta-analysis is the best analysis method. Compared with traditional descriptive literature reviews, a meta-analysis is a quantitative analysis method with better accuracy and higher testing power. 47 Meta-analysis is a means of augmenting the effective sample size by pooling data from individual association studies, thus enhancing the statistical power of the analysis for the estimation of genetic effects. 11
The current study summarized the research articles on the association between MBL gene polymorphism and sepsis published before December 1, 2019, then conducted a meta-analysis to analyze the association between the MBL gene polymorphism and the risk of sepsis. The results suggested that allele O may increase the risk of sepsis overall and that, among the three models of the MBL +54 A/B gene polymorphism, the MBL +54 A/B gene polymorphism had a significant association with the risk of sepsis. In the adult group, the MBL A/O gene polymorphism was related to the risk of sepsis in the dominant and allele model, while the MBL+54 A/B gene polymorphism was significantly related to the risk of sepsis in the recessive model. In the children group, none of the polymorphic sites were found to be significantly related to the occurrence of sepsis in any of the three models.
Publication bias is one of the main factors affecting the validity of the analysis results in meta analysis. The main reasons for publication bias are: the included studies of meta analysis are missed, the bias of small sample studies and the negative results are not easy to publish. Funnel plots are the most common method to identify publication bias in the process of meta analysis, which reflects the estimated intervention effect of a single study under a certain sample size or accuracy. In the absence of bias, the points in the image should be clustered into an inverted funnel. If there is bias, the appearance of the funnel map is asymmetric. Both Begg test and Egger test are quantitative publication bias tests, which can detect the symmetry of funnel plots. p value represents the significance of bias, and p < 0.1 indicates that there is significant publication bias. If the number of included studies was small, it was unnecessary to perform publication bias analysis.For data sets with ≥10 articles, funnel plots, Begg’s tests, and Egger’s tests were used to evaluate the possibility of publication bias in this study. For the total and adult groups, the results demonstrated no publication bias in the unadjusted estimate of the association between the MBL A/O and −211Y/X gene polymorphism and sepsis. Although the Begg’s tests and Egger’s tests did not show any obvious publication bias, the influence of bias in the present analysis could not be completely excluded as studies with positive results are more easily published than those with negative results.
There are still some limitations to the current study. First, as the diagnostic criteria for sepsis are constantly updated, the diagnostic criteria for sepsis reported in the literature in different years are not unified, which may affect the results of systematic analysis. In addition, there were disparities in the detection methods of the genotypes in the studies, the sources of specimens were also different, and the control group settings were inconsistent, all of which might affect the association between the genetic polymorphism and the risk of sepsis. Finally, the current study only collected the English documents from the three major databases; documents in other languages or other databases would inevitably be missed, which would affect the results.
Conclusions
In summary, the MBL gene polymorphisms that are closely related to the occurrence of sepsis are primarily A/O and +54 A/B, although not every model or population has consistent results; MBL -221Y/X and −550H/L have no obvious association with the occurrence of sepsis in different age groups or different models.
Supplemental Material
Supplemental Material - Mannose-binding lectin gene polymorphism and the susceptibility of sepsis: A meta-analysis
Supplemental Material for Mannose-binding lectin gene polymorphism and the susceptibility of sepsis: A meta-analysis by Shaowen Cheng, Rong Wang, Hengjie Zhu, Jian Yang, Jiangling Yao, Yunfu Zeng, Hongwang Cui and Binwen Huang in European Journal of Inflammation.
Footnotes
Acknowledgments
SC, RW and HZ are the guarantees of the integrity of the entire study and all authors (SC, RW, HZ, JY, YZ, HC, BH and J Yao) contributed to the study concept and the design and definition of the intellectual content of this study. SC, RW and BH contributed to finding papers and analysing statistics. SC, HC and HZ contributed to the preparation of the manuscript. JY and J Yao contributed to the manuscript review. All authors read and approved the final manuscript.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported by the Hainan Province Clinical Medical Center, Academician Workstation in Hainan Province, National Natural Science Foundation of China (81860347, 81871611), Hainan Provincial Natural Science Foundation of China (822MS174), Hainan Province Science and Technology Special Fund (ZDYF2021SHFZ238, ZDKJ2021038).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
