Abstract
Preeclampsia is a syndrome that consists of hypertension (blood pressure ⩾ 140/⩾ 90 mm Hg) and proteinuria (⩾ 0.3 g/24 h). It occurs after 20 weeks of gestation. Preeclampsia and eclampsia are the causes of maternal mortality in Indonesia. Hypertension is the second cause of maternal mortality in Indonesia after hemorrhage. The mechanism of preeclampsia might occur through inflammation process that would cause endothelial dysfunction. Preeclampsia leads to complications both in the mother and the fetus. The effective management for preeclampsia is prevention, including mild regular exercise since early pregnancy. This research objective was to analyze the inflammation process and endothelial dysfunction in an endothelial dysfunction model using mice who had mild regular exercise since early pregnancy. There were three treatment groups with 14 mice each, namely, normal pregnancy group (K1), endothelial dysfunction group (K2), and endothelial dysfunction group with mild regular exercise since early pregnancy (K3). The mice in K3 group had mild regular exercise by doing a treadmill for 18 min once every 2 days. The results showed that the placental interleukin 10 (IL-10) level in K3 was lower than that in K2 (599.86 vs 636.36, P = 0.001), the placental interferon gamma (IFN-γ) level in K3 was higher than that in K2 (322.36 vs 299.50, P = 0.002), and the placental vascular cell adhesion molecule 1 (VCAM-1) expression in K3 was higher than that in K2 (5.33 vs 1.67, P = 0.000). It can be concluded that mild regular exercise since early pregnancy did not decrease the inflammation process and the expression of placental VCAM-1 in endothelial dysfunction model using mice.
Introduction
Preeclampsia is a syndrome that consists of hypertension (blood pressure ⩾ 140/⩾ 90 mm Hg) and proteinuria (⩾0.3 g/24 h). It occurs after 20 weeks of gestation. Preeclampsia might occur in women who have normal blood pressure before pregnancy. 1
Data from the Indonesian Health Ministry in 2010–2013 showed that hypertension was the second cause of maternal mortality in Indonesia after hemorrhage. The incidence of hemorrhage was 30.3% and hypertension was 27.1%. 2 Data in Ulin Hospital Banjarmasin, South Kalimantan, showed that preeclampsia was included in the top 10 major diseases. In 2011, mild preeclampsia was diagnosed in 32 patients, severe preeclampsia in 278 patients, and eclampsia in 56 patients. In 2012, mild preeclampsia was found in 76 patients, severe preeclampsia in 391 patients, and eclampsia in 41 patients. 3
Preeclampsia leads to complications both in the mother and the fetus. For the mother, it causes the HELLP (Hemolysis, elevated liver enzyme, low platelet count) syndrome, cerebral dysfunction, renal disturbance, and maternal mortality. For the fetus, it causes low birth weight, fetal growth retardation, and intrauterine fetal death. 4
One of the mechanisms of preeclampsia is through inflammation process. 5 Szarka et al. 6 and Vitoratos et al. 1 suggested that preeclampsia causes increased levels of proinflammatory cytokines like tumor necrosis factor α (TNF-α) and interferon gamma (IFN-γ), as well as a decreased level of interleukin 10 (IL-10). The levels of IFN-γ and IL-10 are not in balance, so that they inhibit trophoblastic invasion. Inhibition of trophoblastic invasion causes inadequate placentation, and it induces placental ischemia. Ischemic placenta induces anti-angiogenic factor, which in turn inhibits proangiogenic factor and causes endothelial dysfunction. 7 The indicator of endothelial dysfunction is vascular cell adhesion molecule 1 (VCAM-1). 8
The management of preeclampsia still depends on symptoms and complications. The effective management should be the prevention of preeclampsia since early pregnancy. One of the prevention methods is by mild regular exercise. 9 Mild regular exercise might increase interleukin 6 (IL-6) level, which could increase IL-10 level. 10
Hopps et al. showed that regular exercise or exercise plus anti-inflammation would decrease proinflammatory cytokines like TNF-α and interleukin 1 beta (IL-1β). Exercise also increases anti-inflammatory cytokines like IL-10 and interleukin 6 (IL-4). Those cytokines are also found in preeclampsia, so exercise is assumed to influence cytokine level. 11
Sulistyowati et al. developed an endothelial dysfunction model as an early induction of preeclampsia model. It could be created by giving an injection of anti-QA2 to block placental QA2 expression, which is homologous with placental human leukocyte antigen G (HLA-G) expression in human. Low HLA-G expression is a predictor for endothelial dysfunction in preeclampsia.
In that study, mice were injected with 40 ng anti-QA2. HSP-10 and VCAM-1 expression were assessed on day 6, 12, and 18 using immunohistochemical methods. There was no QA2 expression in placenta after 40 ng dose of anti-QA2 injection. The study concluded that HSP-10 and VCAM-1 expressions were higher in low or lack of expression of QA2 in trophoblast tissues, might be associated with endothelial dysfunction in preeclampsia. 8
Until recently, the changes in placental IL-10 level, placental IFN-γ level, and placental VCAM-1 expression in endothelial dysfunction model using Mus musculus who had mild regular exercise have not been evaluated yet. Therefore, this research is important to provide information on the biological mechanism of the effect of mild regular exercise on preeclampsia.
Materials and methods
This research used a true experimental post-test only with control group design. The experimental units were pregnant mice (Mus musculus), who were healthy, aged 3 months old, with body weight of 15–25 g. The total number of mice were 14 per group.
There were three treatment groups, namely, normal pregnant mice (K1), endothelial dysfunction model (K2), and endothelial dysfunction model with mild regular exercise since early pregnancy (K3). The measured variables were placental IL-10 level, placental IFN-γ level, and placental VCAM-1 expression.
Preliminary research was conducted to estimate the anti-QA2 dose. The dose used was 50 ng, and it could block placental QA2 expression. Anti-QA2 10 ng (0.1 mL) was injected intraperitoneally to pregnant mice every day, from day 1 until day 5. Mild regular exercise was given from day 1 for 2 weeks.
Mild regular exercise was conducted in the form of non-angular treadmill. The speed was 14 cm/s for 15 min. It started from 7 cm/s for 1 min, 11 cm/s for 2 min, and then 14 cm/s for 15 min. The exercise was given once every 2 days for 2 weeks.
All mice were terminated on day 19 of pregnancy. Placenta was taken and crushed with phosphate buffer saline (PBS) solution. The placental samples were examined with Elisa to estimate the level of IL-10 and IFN-γ. The other placenta was kept in formalin, and it was examined to estimate the expression of placental VCAM-1. Each variable needed one placenta, so three placentas were taken from one mouse.
The immunohistochemistry assessment of placental VCAM-1 expression was semi-quantitative, based on the modification of Remmele’s method. Immunoreactive score (IRS) was calculated by multiplying the immunoreactive cell presentation score with the color intensity score on immunoreactive cell. The IRS data were examined in five fields of view, with 400× and 1000× magnification. All of the assessments were conducted with Nikon H600 L microscope equipped with digital camera DS-Fi2 300 megapixel and Nikon Image System software.
We could not examine the blood pressure in this research to confirm the sign of preeclampsia because we did not have the device to examine the blood pressure in mice.
Data were analyzed with Kruskal–Wallis test with the confidence interval of 95%. To further analyze the difference between groups, we used Mann–Whitney U test with the confidence interval of 95%.
Results
Placental IL-10 level
The data for placental IL-10 level were not normally distributed (P < 0.05), therefore the data were analyzed with Kruskal–Wallis test with confidence interval of 95%. The comparison between groups was analyzed with Mann–Whitney U test. The results are shown in Table 1.
Placental IL-10 level in all the treatment groups.

IL-10: interleukin 10; SD: standard deviation.
P < 0.05 means there was a significant difference. In each variable, the groups with different letters were significantly different (K1: normal pregnant mice, K2: endothelial dysfunction model, K3: endothelial dysfunction model with mild regular exercise).
a, b, c, d: Group that has same letter code with other groups means there is no significant different between those groups. Group that has different letter code with other groups means there is significant different between those groups.
Placental IFN-γ level
The data of placental IFN-γ level were analyzed with Kruskal–Wallis test with confidence interval of 95% (Table 2).
Placental IFN-γ level in all the treatment groups.

IFN-γ: interferon gamma; SD: standard deviation.
P < 0.05 means there was a significant difference. In each variable, the groups with different letters were significantly different (K1: normal pregnant mice, K2: endothelial dysfunction model, K3: endothelial dysfunction model with mild regular exercise).
a, b, c, d: Group that has same letter code with other groups means there is no significant different between those groups. Group that has different letter code with other groups means there is significant different between those groups.
Placental VCAM-1 expression
Placental VCAM-1 expression was identified to find out whether endothelial dysfunction had occurred. Placental VCAM-1 expression is shown in Figure 1. The data for placental VCAM-1 expression are shown in Table 3.

The comparison of placental VCAM-1 expression in capillary wall and trophoblast cells (arrow) between all groups (immunohistochemistry, 1000× magnification; Nikon microscope H600 L; camera DS-Fi2 300 megapixel): (a) K1, (b) K2, and (c) K3.
Placental VCAM-1 expression in all the treatment groups.
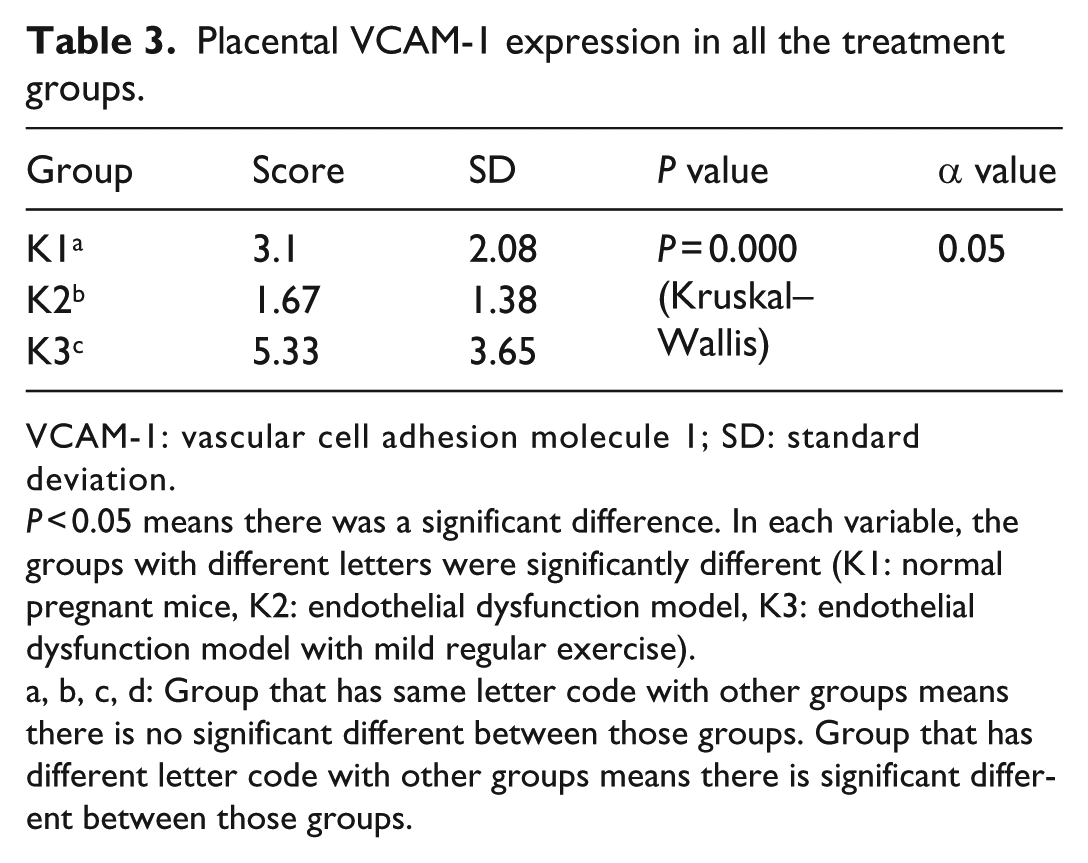
VCAM-1: vascular cell adhesion molecule 1; SD: standard deviation.
P < 0.05 means there was a significant difference. In each variable, the groups with different letters were significantly different (K1: normal pregnant mice, K2: endothelial dysfunction model, K3: endothelial dysfunction model with mild regular exercise).
a, b, c, d: Group that has same letter code with other groups means there is no significant different between those groups. Group that has different letter code with other groups means there is significant different between those groups.
Placental VCAM-1 expression data were not in normal distribution; therefore, they were analyzed with Kruskal–Wallis test with confidence interval of 95%. The comparison between groups was analyzed with Mann–Whitney U test.
Discussion
Placental IL-10 level
Table 1 shows that placental IL-10 level in K2 was higher than that in K3, but they were not significantly different. K2 was the endothelial dysfunction model. Its placental IL-10 level was higher than K1’s and K3’s levels because the mice experienced inflammation process due to endothelial dysfunction induction. The endothelial dysfunction was induced by anti-QA2 injection. 8 The induction used 50 ng of anti-QA2. Anti-QA2 blocks trophoblast QA2 expression, and it induces immune response. To ensure balance, the body also produces anti-inflammation such as IL-10. Higher placenta IL-10 level in K2 was different from the results in the study by Laresgoiti-Servitje et al., 7 which showed that IL-10 level in preeclampsia was lower than that in normal pregnancy.
These different results might be caused by the fact that K2 had presented positive response by increasing IL-10 level to inhibit the inflammation as body mechanism. The effect of anti-QA2 injection lasted from day 1 until day 5 of pregnancy-induced inflammation, but we did not know if it still occurred until day 19 of pregnancy. The interval time between day 6 and day 19 might be an opportunity for the body to develop defense mechanism and to balance the inflammation and anti-inflammation (Figure 2).

Normal and abnormal placental development. 4
The body had a mechanism to balance the inflammation and anti-inflammation. It was assumed that this occurred in K2. But we did not examine placental inflammation and anti-inflammation levels on day 6 and day 19. The IL-10 levels in K2 and K3 were not significantly different; therefore, mild regular exercise since early pregnancy did not lead to a significant increase in placental IL-10 level.
Placental IFN-γ level
IFN-γ is an inflammatory cytokine induced by anti-QA2. Placental IFN-γ level in K3 was higher than that in K2. K3 was an endothelial dysfunction model with mild regular exercise since early pregnancy. Endothelial dysfunction causes a high level of placental IFN-γ. Anti-QA2 injection blocks placental QA2 expression. It leads the body to recognize the fetus as non-self, and it activates natural killer (NK) cell and produces immune response by increasing placental IFN-γ. 7
Placental IFN-γ levels in K2 and K3 were not significantly different because mild regular exercise since early pregnancy in this research did not decrease the inflammation yet. This might be caused by the different model and exercise type used by this research compared with the previous studies.
A study by Gilbert et al. showed that exercise could prevent preeclampsia. The model used the binding of uterine artery to produce ischemia. The exercise used was a voluntary type, running in spinning wheel. 12 Different methods influence the results.
Placental VCAM-1 expression
Placental VCAM-1 expression in K3 was higher than that in K2, and they were significantly different. This showed that there was endothelial dysfunction in K3. This was different from the results by Gilbert et al. which showed that regular exercise could prevent preeclampsia. This was caused by the different models used. Preeclampsia model in Gilbert et al. 12 study used the binding of uterine artery to induce ischemia. This research used anti-QA2 injection to block placental QA2 expression, which is homologous with HLA-G in human. Its inhibition induced the mothers’ immune response.
This difference was also caused by the type of exercise. Gilbert et al. study used voluntary exercise with spinning wheel, but this research used involuntary exercise with treadmill.
Endothelial dysfunction occurred in K3 was induced by anti-QA2. The dose given induced endothelial dysfunction, and the exercise given had not decreased the inflammation yet. This condition was showed by the placental IL-10 and IFN-γ levels in K3. These values still showed inflammation process.
The other causes of endothelial dysfunction could be from a local inflammation. The source of local inflammation might be from the musculosceletal system, digestive system, skin, or the other systems. Local inflammation induces circulating inflammation by increasing inflammation products like reactive oxygen species (ROS), or the other substances from liver or spleen. Those substances induce endothelium dysfunction by increasing VCAM-1 level. 13
Possibility of fungal infection was prevented by keeping the pellet in dry place and far away from the water, as well as cleaning the cages and replacing the husk every 2 days. Possibility of infection from wounds was prevented by excluding the mice who had wounds. Therefore, this research had prevented the potential source of infection.
The other factors that might cause high expression of placental VCAM-1 consist of the risk factors for blood vessel disturbances such as diabetes mellitus, hypercholesterolemia, hypertension, smoking, obesity, heart failure, inflammation, and coronary diseases. 14 These conditions were difficult to identify in this research, but the researcher had chosen healthy mice for this research.
Higher expression of placental VCAM-1 in K3 is caused by the inflammation process after QA2 injection. This injection blocked QA2 expression in trophoblast cell. Low expression of QA2 induces NK cell to produce inflammation cytokine. NK cell is the source of IFN-γ. Therefore, the inflammation was higher and induces endothelial dysfunction. 7
While the QA2 injection was given, the exercise was also conducted. Acute response after exercise could be due to increasing inflammation. 10 Therefore, it probably increases inflammation and induces higher endothelial dysfunction.
K2 was also injected with anti-QA2, but VCAM-1 expression was lower than K3. After QA2 injection, this group might also had showed an increase in proinflammation, but there was no effect of acute exercise, so immune response probably produced anti-inflammation to create a balance in cytokines. 4 Therefore, the inflammation probably decreased, and endothelial dysfunction also decreased.
The weakness of placental VCAM-1 expression examination is that the description is influenced by the color absorption and the cutting of preparation. Color absorption could influence cell expression. The more colors that are absorbed, the higher the expression that is shown. The cutting of preparation also has influence. If the cutting of preparation was accumulated, the cells would accumulate too, and the accumulation of cells would lead to a higher expression.
Although this study had not given significant results for exercise in endothelial dysfunction model, it does not mean there was no positive input. We still need further research about exercise and endothelial dysfunction that induces preeclampsia. We still need upcoming research to understand the other mechanisms of exercise that might potentially prevent preeclampsia and research about the other models of preeclampsia that could describe the types of preeclampsia (early and late preeclampsia). We also need to assess the type, frequency, and duration of exercise.
We concluded that mild regular exercise since early pregnancy did not increase placental IL-10 level and did not decreased placental IFN-γ level and placental VCAM-1 expression yet.
Footnotes
Acknowledgements
The authors would like to extend considerable gratitude to the whole team in the Embryology Department, Faculty of Veterinary Medicine, Airlangga University, Surabaya, Indonesia, who had helped the running of this research. The authors would also like to extend considerable gratitude to the Ministry of Research, Technology and Higher Education, Indonesia who supported the funding of this research.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
