Abstract
Objective
Chronic lower extremity arterial occlusive disease (LEAO) presents significant diagnostic and management challenges, often requiring effective perioperative pain management to enhance patient outcomes. This study evaluated the efficacy of ultrasound-guided popliteal sciatic nerve block (PSNB) compared to traditional analgesia in managing early perioperative pain and improving microcirculation in patients with severe LEAO.
Methods
This retrospective, exploratory study involved 92 patients with Fontaine classification III and IV LEAO, treated from January 2021 to December 2022. Patients were divided into two groups: those receiving traditional analgesia with fentanyl patches and those undergoing PSNB. Clinical outcomes assessed included early perioperative pain intensity using the Visual Analogue Scale (VAS), Toe-Brachial Index (TBI), foot temperature (FT), and feet transcutaneous oxygen pressure (FTpO2). Data on tramadol usage and results from lower limb ultrasound post-analgesia were also collected.
Results
PSNB was associated with significantly lower VAS scores and higher TBI, foot temperature, and transcutaneous oxygen pressure compared to traditional analgesia, indicating enhanced pain management and microcirculation. Furthermore, PSNB patients showed a significantly reduced consumption of tramadol and improved collateral circulation in the lower limbs as evaluated on the fifth day post-analgesia.
Conclusion
PSNB provides superior pain control and enhances microcirculatory outcomes in the early perioperative period for patients with severe LEAO, presenting a promising alternative to traditional analgesic methods. These findings suggest that PSNB has the potential to improve early perioperative management in LEAO, although further research is needed to confirm these results across broader populations.
Keywords
Introduction
Chronic lower extremity arterial occlusive disease (LEAO) is commonly induced by the accumulation of lipid plaques within arterial vessels, causing their narrowing or obstruction. 1 Globally, LEAO has a high incidence and mortality rate, significantly contributing to various cardiovascular diseases. 2 More than 10.6% of the population, and approximately 20% of the elderly, are affected by LEAO. 3 LEAO’s atypical and elusive initial symptoms often escape patients’ notice, complicating diagnosis and early intervention. 4 Patients often seek treatment only when experiencing severe symptoms such as unbearable lower limb pain, foot ulcers, or gangrene. Typically, these cases are classified as stages III or IV according to the Fontaine classification. 5 Treatment primarily aims to relieve symptoms, preserve limbs, and reduce the necessity for amputation. Methods mainly comprise traditional vascular bypass surgery and the rapidly developing endovascular treatment techniques in recent years. 1
Pain, a primary symptom of LEAO, is crucial for reducing patient discomfort, alleviating anxiety, and improving quality of life. 6 Studies indicate that enhancing perioperative pain management and stress response reduction can lead to better post-operative outcomes. 7 Traditional analgesia (TA) methods include intravenous paracetamol, non-steroidal anti-inflammatory drugs (NSAIDs), tramadol, and patient-controlled opioids. In this study, patients receiving fentanyl transdermal patches were designated as the traditional analgesic group. We propose that fentanyl patches, due to their sustained and potent analgesic effects compared to other methods, are representative of traditional analgesic approaches. This is based on the established use of fentanyl patches in clinical practice as a reliable and effective form of pain management, often considered a standard treatment option for persistent pain. Regional analgesia primarily involves epidural analgesia and peripheral nerve blocks. Compared to TA, regional analgesia significantly enhances pain management, lowers morphine use, and reduces symptoms like vomiting. 8 Currently, research on regional analgesia for LEAO is limited. Although some case reports suggest that ultrasound-guided peripheral nerve blocks can maintain cardiovascular stability and manage pain effectively, this technique has not yet been clinically evaluated as a perioperative analgesic method for LEAO. 9 This retrospective study collected clinical data from stages III and IV LEAO patients treated with different analgesic methods. It aims to evaluate the differences between TA (using fentanyl patches) and ultrasound-guided popliteal sciatic nerve block (PSNB) in early perioperative pain relief and microcirculation improvement, offering new perspectives for clinical decision-making.
Method
Patients
This retrospective, exploratory study focused on early perioperative pain management and outcomes in patients who are preparing for surgical intervention for severe chronic lower extremity arterial occlusive disease. We collected clinical data from 92 LEAO patients classified as Fontaine stages III and IV, from January 2021 to December 2022. Inclusion criteria were a Toe-Brachial Index (TBI) < 0.9, limb rest pain or gangrene, and age above 18. Exclusion criteria included absence of informed consent, diagnosis of vascular malformations, history of reperfusion surgery (bypass and/or arterial stent placement), allergy to analgesic drugs, severe coagulopathy, and inability to perform nerve blocks due to concurrent psychiatric or neurological disorders. Before and during the study, all patients were allowed to choose tramadol extended-release tablets (0.1 g) as a temporary analgesic when necessary, with a maximum usage frequency of three times per day. Patients included in the study routinely received antiplatelet therapy with aspirin at a dose of 75 mg/day. Non-opioid analgesics, such as gabapentin, were not used. None of the patients included in the study received anticoagulant therapy. The surgical procedures for study patients were consistent between groups, with all patients undergoing endovascular treatment. Depending on the severity and extent of the lesions, either plain balloon angioplasty or stent placement was appropriately selected.
Analgesic techniques and data collection
Before receiving endovascular treatment, all patients underwent different analgesic method for 5 days. 42 patients were treated with traditional analgesia method using fentanyl patches (with a dosage of 4.2 mg per patch, administered every 72 hours (q72h)), and 50 patients underwent ultrasound-guided PSNB. The standard procedure for PSNB is as follows: The patient is positioned supine, followed by routine disinfection and draping. Ultrasound is used to clearly identify the popliteal artery and the course of the sciatic nerve. A needle is inserted from lateral to medial, between the lateral head of the gastrocnemius and the biceps femoris. The needle is advanced toward the sciatic nerve, and continuous ropivacaine infusion (100 mg in 50 mL saline, infused at 20 mg/hour) is carried out for nerve blockade. An epidural catheter is then placed using a 22 G Quincke needle (Type B), and the site is secured before the patient is returned to the ward. The position of the catheter was confirmed to be accurate through ultrasound imaging. The sciatic catheter will be discontinued before the surgery. The primary endpoint of this study was the assessment of pain relief, measured by the Visual Analogue Scale (VAS), on the third day following analgesic intervention. Secondary endpoints included: 1. the evaluation of microcirculation, assessed by the TBI, foot temperature, and feet transcutaneous oxygen pressure (FTpO2) on the third post-analgesic day (PAD). 2. Collateral circulation formation was assessed on the fifth post-analgesic day using lower extremity ultrasound. A scoring system (collateral vessel score, CVS) was implemented, awarding 0 points for the absence of collateral formation and 1 point for the presence of collateral in each separate arterial region. 3. The cumulative frequency of tramadol consumption, an analgesic, was recorded from the first to the third day post-analgesia. 4. The post-operative effects on pain were also assessed using the VAS on the third post-operation day.
Statistical analysis
Data is mainly presented as mean ± standard deviations. To assess differences in categorical variables, Pearson’s χ2 test or Fisher’s exact test was employed. Continuous variables were compared using the t test or Mann–Whitney U test, based on the distribution’s normality. The correlation between the frequency of tramadol administration and the elapsed time post-analgesia was evaluated using Spearman’s rank correlation coefficient. All statistical tests were two-sided, setting the significance level at p < .05. SPSS software was used for all statistical analyses (SPSS Inc., ver. 26.0, Chicago, IL, USA).
Result
Demographic and baseline characteristics.
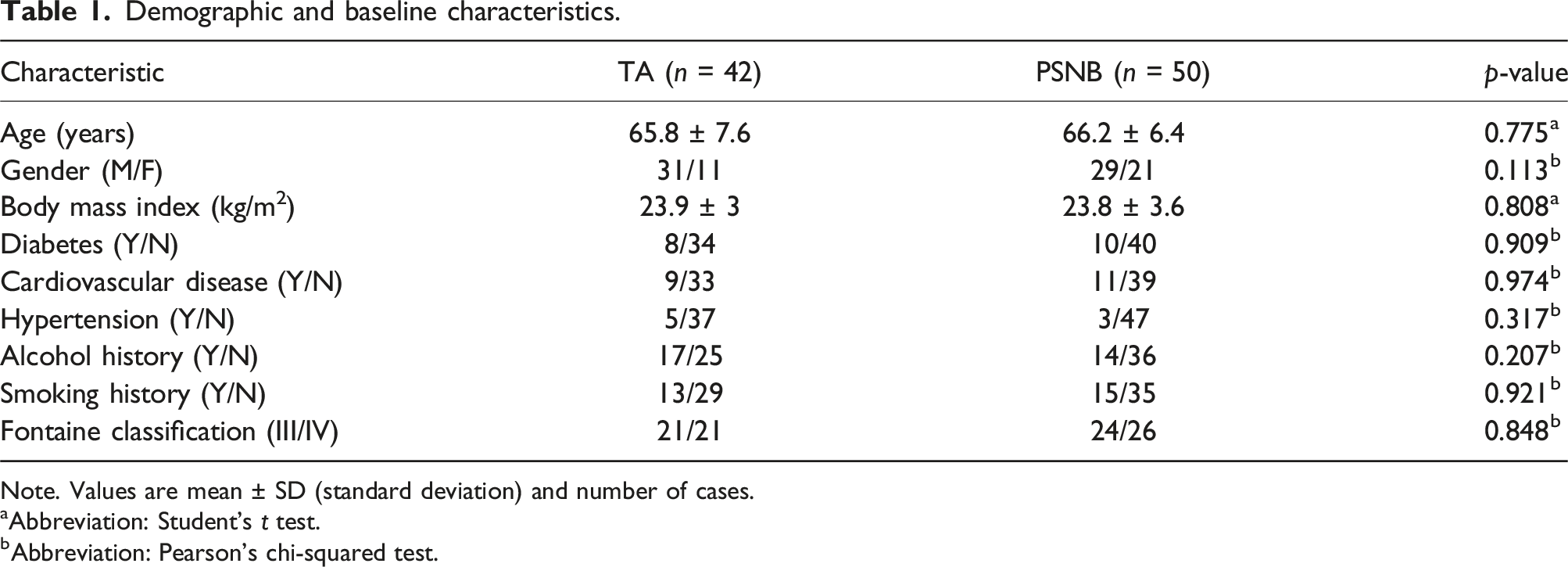
Note. Values are mean ± SD (standard deviation) and number of cases.
aAbbreviation: Student’s t test.
bAbbreviation: Pearson’s chi-squared test.
Access the efficacy of different analgesic method in severe LEAO
Comparison of post-analgesia outcomes in Fontaine stage III patients.
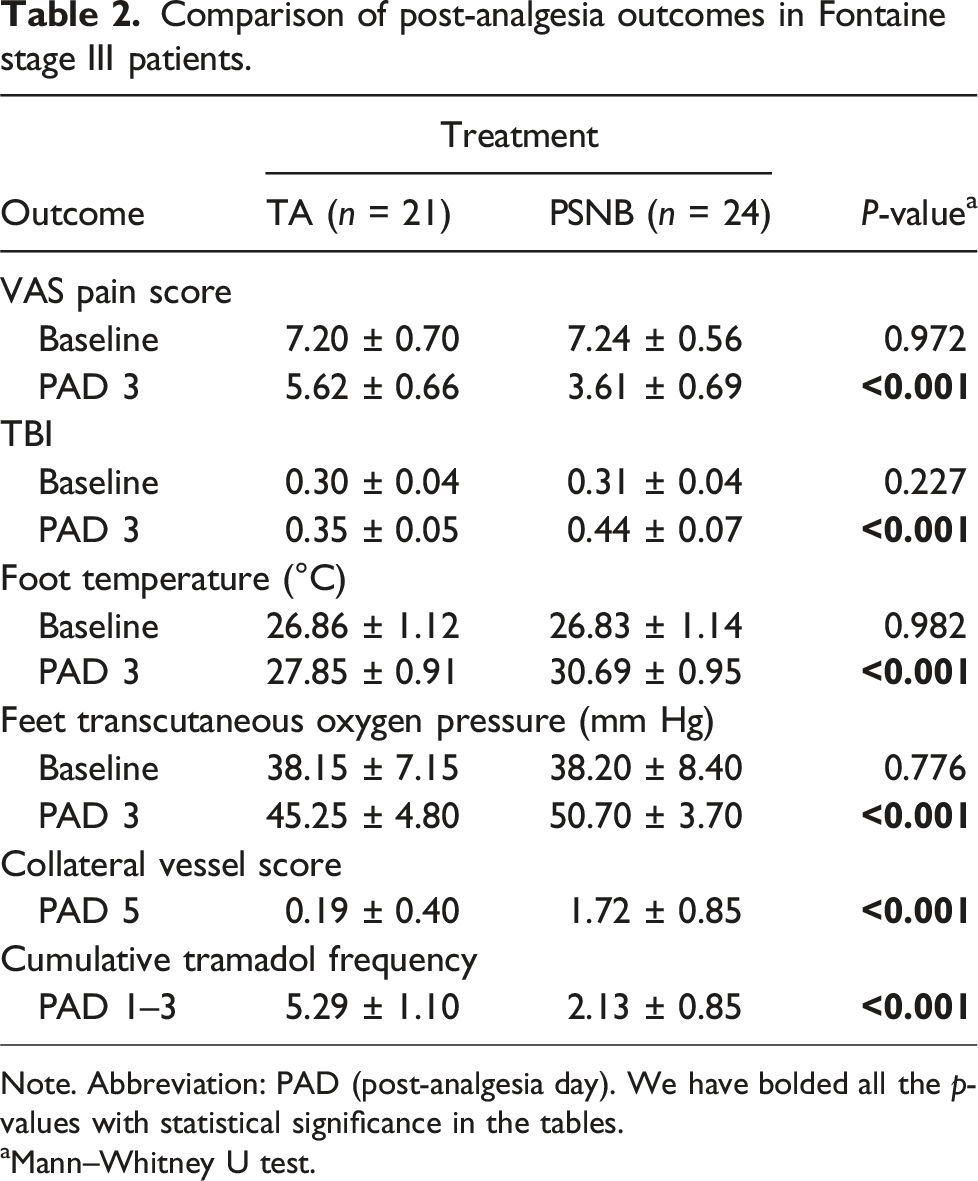
Note. Abbreviation: PAD (post-analgesia day). We have bolded all the p-values with statistical significance in the tables.
aMann–Whitney U test.
Comparison of post-analgesia outcomes in Fontaine stage IV patients.
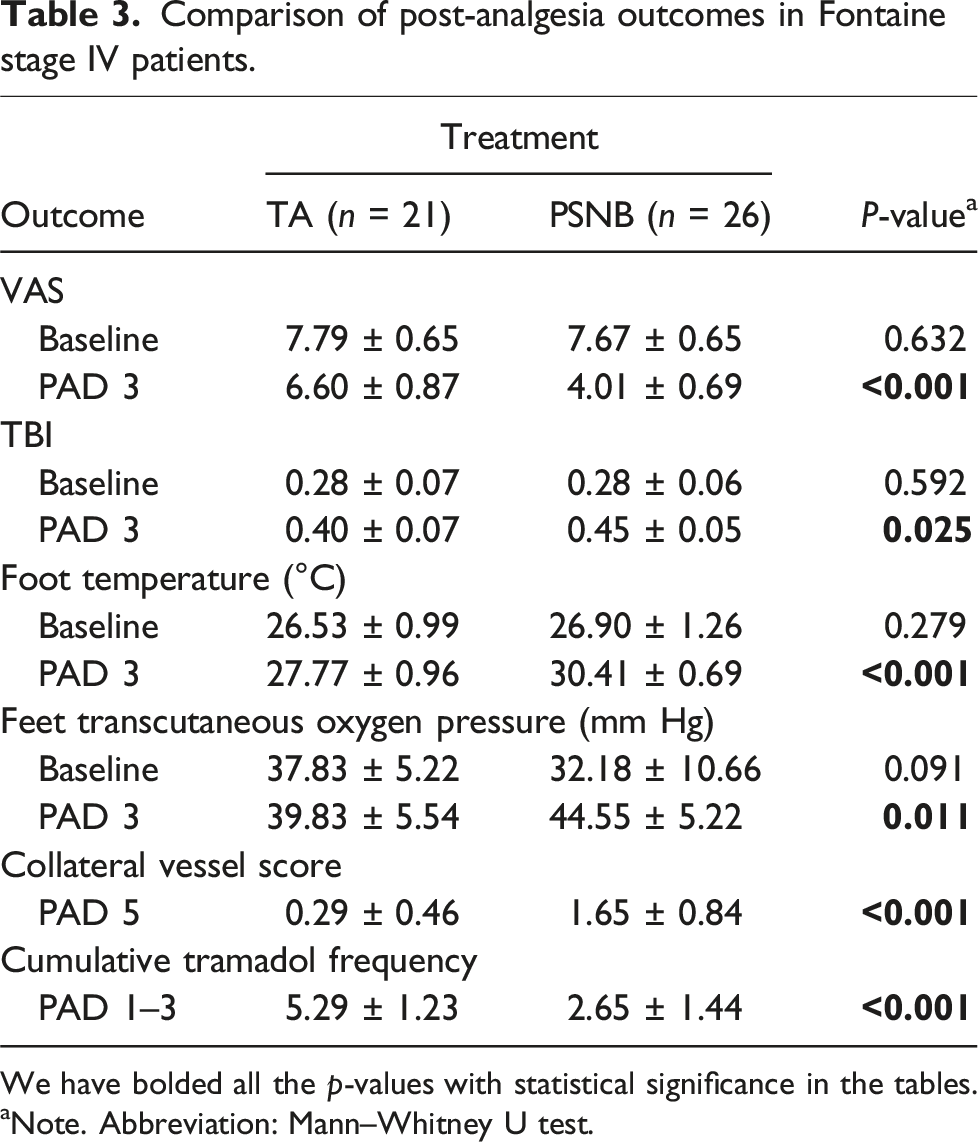
We have bolded all the p-values with statistical significance in the tables.
aNote. Abbreviation: Mann–Whitney U test.
VAS in POD 3 for patients in Fontaine III and IV stages.
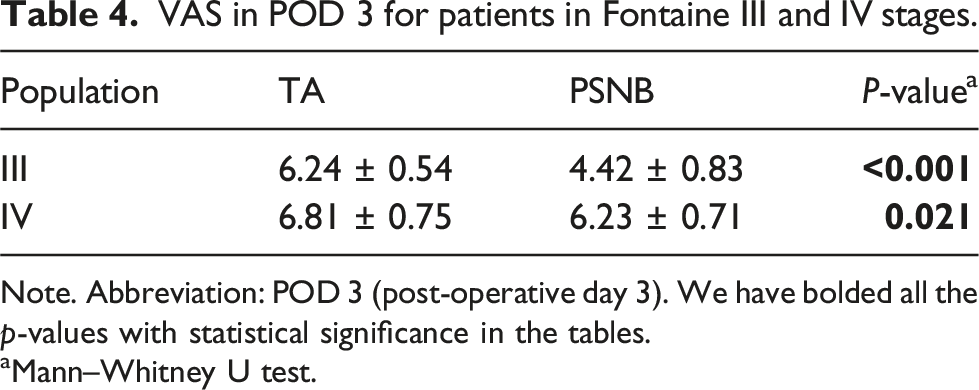
Note. Abbreviation: POD 3 (post-operative day 3). We have bolded all the p-values with statistical significance in the tables.
aMann–Whitney U test.
Access the tramadol consumption of different analgesic method in severe LEAO
Tramadol usage in post-analgesia periods for patients in Fontaine III and IV stages.
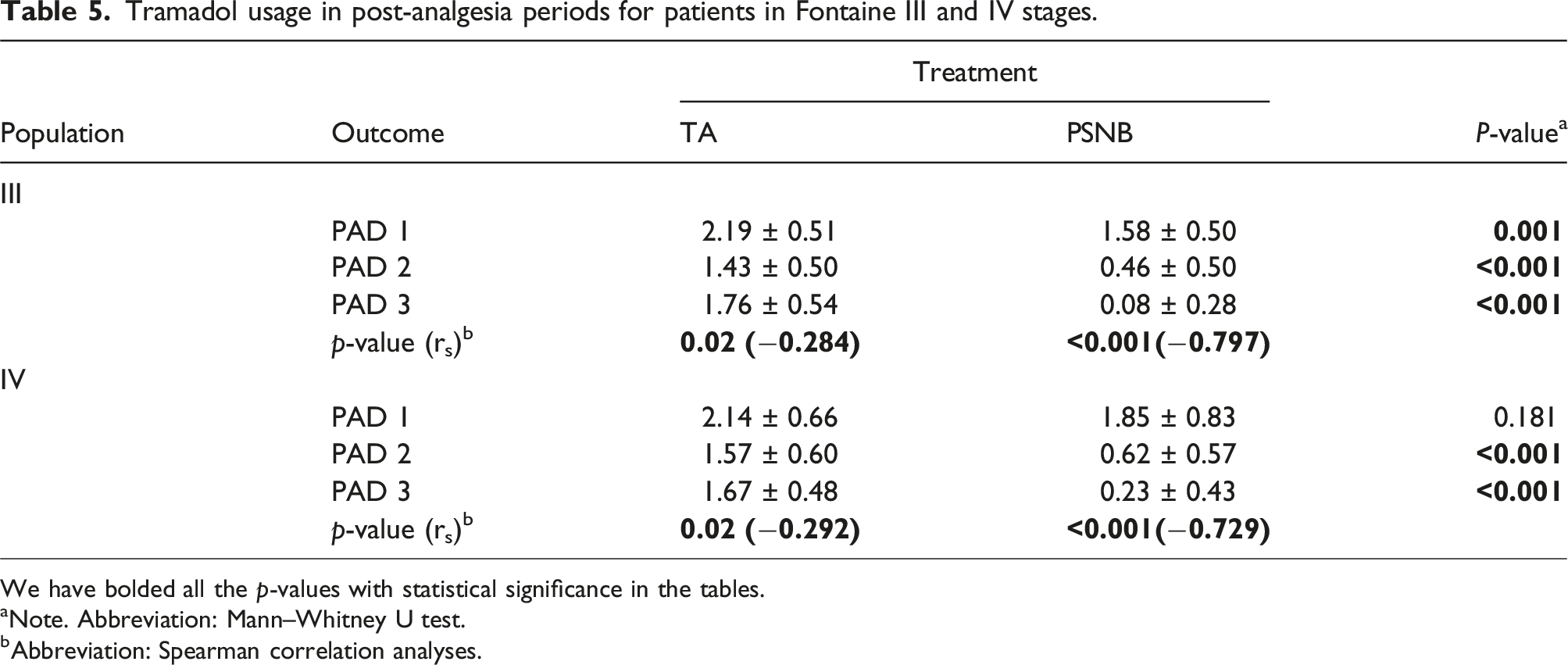
We have bolded all the p-values with statistical significance in the tables.
Note. Abbreviation: Mann–Whitney U test.
bAbbreviation: Spearman correlation analyses.
Discussion
In this retrospective observational study, PSNB demonstrated superior clinical pain control over traditional analgesia in patients with Fontaine stages III or IV. PSNB significantly reduced the intake of tramadol post-analgesia. Moreover, PSNB more effectively enhanced collateral circulation development in the lower limbs.
Perioperative analgesia for LEAO is often considered a critical component of clinical management. Advancements in imaging technologies have highlighted the advantages of ultrasound-guided peripheral nerve blocks in perioperative pain management. Numerous research consistently demonstrates that ultrasound-guided peripheral nerve blocks surpass traditional analgesic methods such as intravenous injections, oral medications, and local infiltration anesthesia in effectiveness.10,11 Recent studies have highlighted PSNB as an emerging analgesic method. In a 2006 study, 12 Marcus et al. found that PSNB in lower limb angioplasty achieved pain control comparable to that of epidural or general anesthesia, while reducing complications like nausea and vomiting post-analgesia. In 2017, Tureli et al. preliminarily evaluated the potential of PSNB in the acute endovascular treatment of LEAO. 13 The study involved 30 patients, with 26 reporting a drop in VAS pain scores to 0 and the remaining four scoring between 1 and 3. Similarly, a prospective study by Discalzi et al. found that PSNB significantly improved patient comfort and compliance during endovascular treatment. 14 Oguslu et al. further analyzed the analgesic differences between PSNB and traditional methods in endovascular treatments. 15 In their study, 252 patients undergoing endovascular treatment received either PSNB (n = 69) or traditional analgesia (n = 183). Results showed a significantly lower median VAS score in the PSNB group compared to the traditional analgesia group (0 vs 3; ***p < 0.001). Post-operatively, the PSNB group also displayed significantly higher satisfaction rates among both patients and operators.
Studies mentioned above primarily evaluated the analgesic effects of PSNB during the middle and later stages of perioperative care. This study extends these evaluations by assessing PSNB’s analgesic outcomes in the early perioperative period. To comprehensively assess PSNB’s analgesic effects, we utilized a combination of subjective and objective measures, including the VAS, TBI, FT, FTpO2, and CVS. For patients in Fontaine stages III and IV, the PSNB group demonstrated lower VAS scores and superior objective outcomes. Additionally, the study examined the supplementary tramadol use post-analgesia. The findings suggest that PSNB reduces tramadol consumption, which continues to decrease over the post-analgesia period. Notably, for stage IV patients, tramadol use on the first post-analgesia day did not differ significantly between the two methods. This could be attributed to the more severe ischemic symptoms in stage IV patients’ lower limbs, which obscure immediate differences in analgesic effectiveness. This thorough assessment not only confirms the comprehensive analgesic effects of PSNB but also underscores its value in early perioperative pain management. This further supports previous findings that PSNB has advantages over traditional pain management methods.
In PSNB, we select ropivacaine as analgesia due to its prevalent use. Ropivacaine provides greater safety, enhanced selectivity for sensory nerves, and reduced cardiovascular toxicity compared to other amide local anesthetics. 16 Ropivacaine can inhibit sympathetic nerve activity and promotes smooth muscle vasodilation, enhancing perfusion in distal vessels. 17 Although the drugs used in traditional analgesia also have similar effects, there may be differences in drug absorption efficiency. This could explain the observed significant improvement in collateral circulation in the PSNB group.
Limitations
This study has several limitations, including its retrospective design, which inherently lacks randomness and may introduce confounding factors and selection bias. Secondly, the short duration of the early perioperative period poses challenges for conducting long-term follow-ups to obtain exact outcomes; however, we attempted to enhance the evaluation by including additional clinical indicators. Thirdly, the TA group primarily used fentanyl transdermal patches. While we noted supplementary oral analgesic use post-analgesia, a comprehensive summary of other methods, such as local infiltration and intravenous injection, was beyond the scope of this study.
Conclusion
In conclusion, PSNB provides safe and effective analgesia in the early perioperative period for patients with severe LEAO, while also partially alleviating symptoms of lower limb ischemia. This offers clinicians valuable insights for developing future analgesic strategies. Although further high-level research is necessary, the substantial relief of subjective pain and improvement in objective indicators confirm PSNB as a viable analgesia option for patients with severe LEAO.
Footnotes
Acknowledgments
The authors would like to thank the patient for his willingness to give his consent and approval for publication of this report.
Author contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Zeyi Zhao. The first draft of the manuscript was written by Jie Zhang. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript. Jie Zhang and Zeyi Zhao contributed equally to the work.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: this work was supported by the Medical Science and Technology Project of Zhejiang Province (2021449255).
Ethical statement
Data Availability Statement
The datasets generated during and/or analyzed during this study are available from the corresponding author on a reasonable request.
