Abstract
Objective/Background
Older people with dementia often show behavioural and psychological symptoms of dementia such as agitation, aggression, and depression that affect their activities of daily living, and hence reduce the quality of life of their caregivers. The aim of this study was to investigate the effects of a new technological intervention—a parametric speaker, creating a narrow personal acoustic environment, which may reduce the manifestation of behavioural and psychological symptoms of dementia symptoms.
Methods
A parametric speaker was placed on the ceiling of a large day room, and personally selected pieces of music were provided in a narrow space just under the speaker during the intervention. Two older residents with behavioural and psychological symptoms of dementia participated in the experiment.
Results
Playing pieces of favorite music via the parametric speaker decreased their behavioural and psychological symptoms of dementia during the intervention. In addition, this intervention reduced the burden on caregivers. One of the advantages of using parametric speaker was being able to create a personal space in a common room.
Conclusion
We considered that the parametric speaker might be useful to reduce behavioural and psychological symptoms of dementia and the burden on caregivers, providing individualized rehabilitation for the improved quality of life of residents.
Keywords
Introduction
The number of older people with dementia has rapidly increased all over the world, and it is estimated to reach 65.7 million in 2030 and 115.4 million in 2050 (WHO and Alzheimer’s Disease International, 2012). Limited services in rehabilitation and care for older people with dementia in care facilities, as well as at home, are major issues.
It is not unusual for residents with dementia to show behavioural and psychological symptoms of dementia (BPSD), such as agitation, aggressiveness, and depression (Finkel, 2000), in a care facility as often as at home. The BPSDs are associated with declines in the cognitive function, activities of daily living, and quality of life (QOL) of patients (González-Salvador et al., 2000; Lyketsos et al., 1997). The BPSDs adversely affect both residents and caregivers (Buhr & White, 2006; Melo, Maroco, & de Mendonça, 2011), especially the neighbor residents in a shared room in the care facility. Nonpharmacological interventions such as music therapy, reminiscence therapy, and relaxation, have been reported to be effective in order to reduce the BPSD and improve QOL (Gitlin, Winter, Dennis, & Hauck, 2007). For instance, music therapy and individualized music listening were reported to be effective on reducing some BPSD such as anxiety, inhibition, and some behavioural problems (Thomas et al., 2017; Ueda, Suzukamo, Sato, & Izumi, 2013) though Raglio et al. (2015) reported that music therapy had no significant effect on BPSD. However, it is not practical in general to increase the number of occupational therapists, music therapists, and/or caregivers for individual care in many countries.
In almost all care facilities in Japan, a resident often spends the daytime with other residents together in a large common room. Because of limited number of staff in the facilities, residents usually stay in a large common space so they can be observed together. In such scenario, it will be difficult to provide personal space and time for each resident during daytime.
Parametric speakers, which have been experimentally developed since the early 1960s, are high-directional loudspeakers based on a parametric array, which allows sound transmission within a narrow range of acoustic space as a “spotlight” (Croft & Norris, 2001; Westervelt, 1963) (Figure 1). Parametric speakers have been used in various situations, such as for information provision in a public space, for instance, they are utilized as an information tool in a museum, and a traffic information apparatus for people with visual impairments (Lee, Katsuura, & Shimomura, 2011b). It is believed that the sound delivered from the parametric speaker will direct to particular people in the limited space without disturbing others (Ju & Kim, 2010). In addition, people’s reaction to audible cues from the parametric speakers are much faster than those given out from a general speaker (Lee, Shimomura, & Katsura, 2012). Parametric speakers can create a personal space with auditory stimulation such as individualized listening music; however, to the best of our knowledge, there has been no study before regarding the use of parametric speaker for music providing in the field of health care, although music might have some effects on improving the BPSD. We considered that a personal acoustic environment could be effective in providing an individualized intervention in a common room for a resident with BPSD.
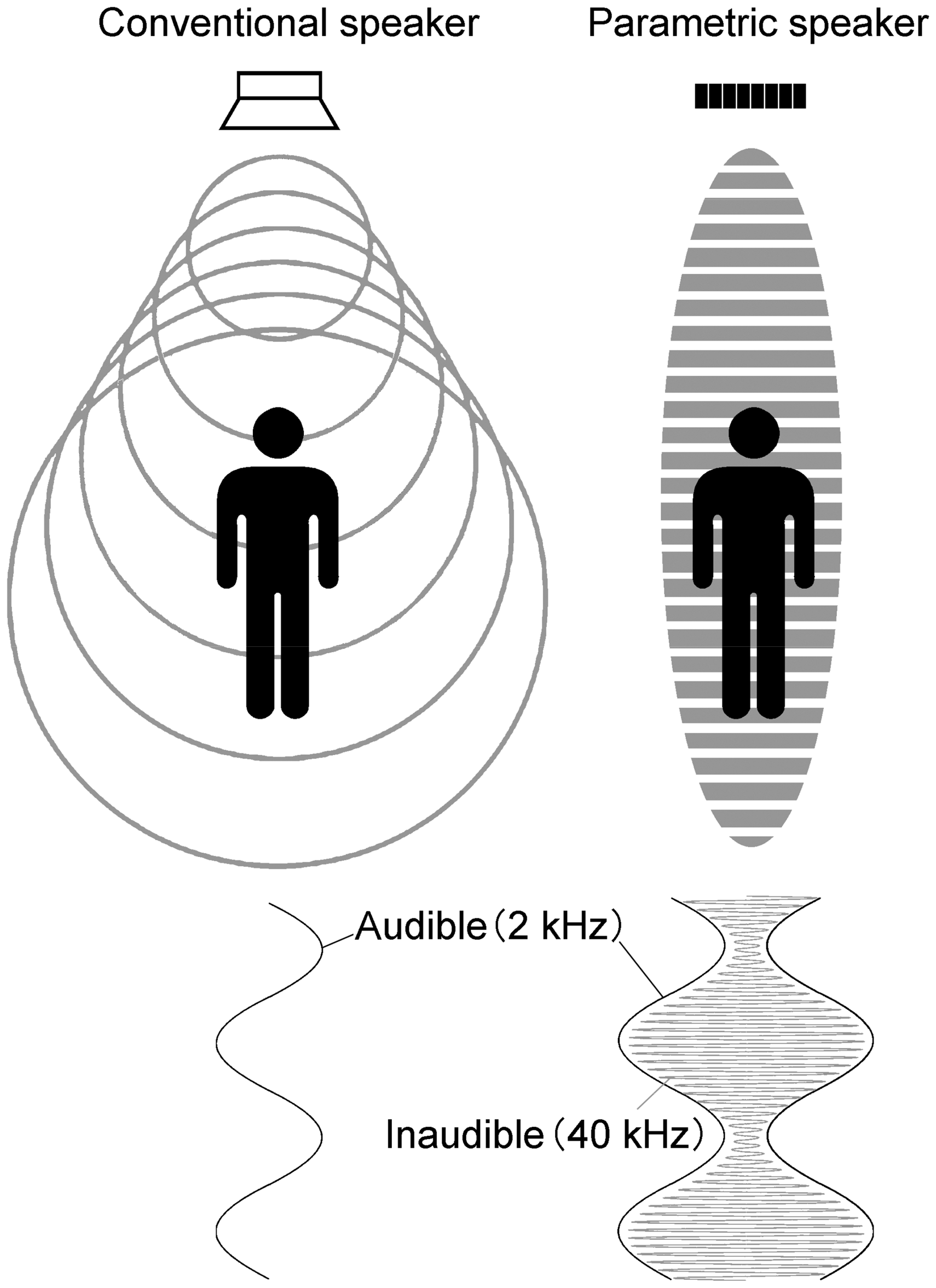
Schematic explanation of the parametric speaker. The parametric speaker (right) provides inaudible ultrasonic sound (40 kHz, gray line) with a frequency of waxing and waning, which corresponds to the frequency of audible sounds (2 kHz, black lines). Ultrasonic sound is transmitted within a narrow range of space relative to the sound produced by a conventional speaker (left).
In the present study, we created a personal acoustic space with a parametric speaker in a common room to provide an individualized intervention for two successful cases with BPSD and investigate the effectiveness of this new technological intervention.
Methods
Study design
It was the first trial to create a personal acoustic space and confirm its effectiveness in decreasing BPSD in older people with dementia. We focused on behaviours like wandering and agitation, which are often observed in people with severe dementia. We observed these symptoms in a multiple case study used as a preliminary investigation into whether intervention with parametric speakers is useful in decreasing the number of instances of wandering and agitation.
Experimental setting
The study was conducted in a large common living room at a community care facility for older people in Japan. The room was 20 m × 15 m and contained a television, four tables, 10 chairs, some washstands, and other furniture. The room also contained modified washrooms and was accessible through a staff room so that the staff members could observe and approach the residents in the room (Figure 2). The mean noise level in the room was approximately 60 dB.
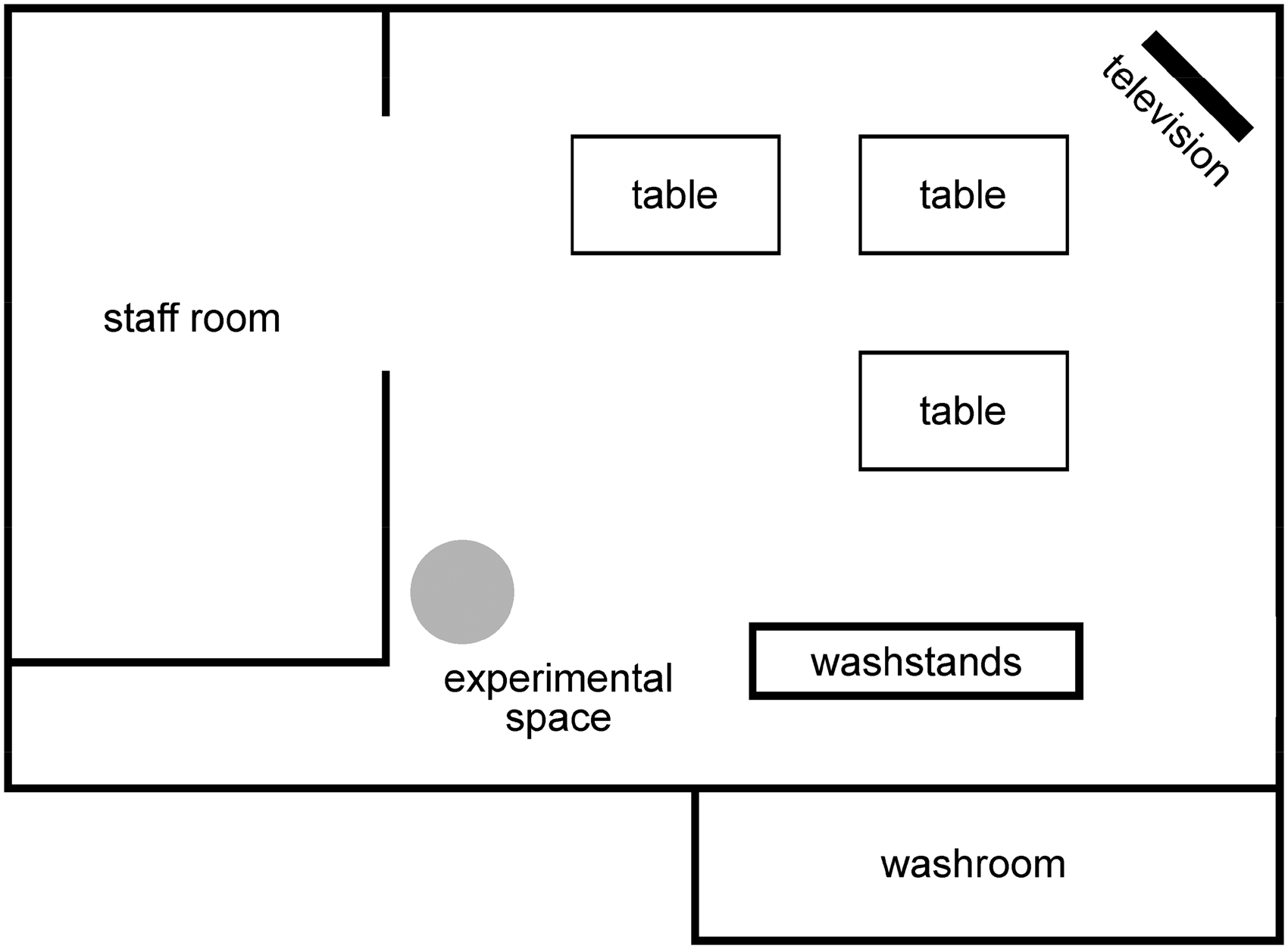
Experimental setting of the personal acoustic space in the common day room. The gray area indicates the space below the parametric speaker, which provided personally arranged music.
The present study used the experimental parametric speaker K-02617 (Akizuki-denshi), which utilizes an array of 100 piezo ultrasonic transducers to produce a 40.3 kHz sound carrier wave. The speaker was a square (98 mm × 98 mm) with a thickness of 20 mm. The speaker was attached to the ceiling 2.5 m above the floor and played pieces of music, which were received as input from a personal computer in the staff room via wires. The mean intensity of audible sound at the point below the center of the speaker was adjusted to be 80 dB. The sound intensity 1 m from the center point was 60 dB, which was similar to the mean noise level of the room.
Participants
The participants were two residents who fit the criteria for dementia presented in the Diagnostic and Statistical Manual of Mental Disorders (Fourth Edition; DSM-IV). They had no hearing difficulty in their daily lives, and they could talk to their caregivers.
Participants were excluded if they exhibited hearing impairment, unwillingness to listen to the music, or loss of consciousness. The participants chosen for the study were therefore those who were willing to listen to the music and who tentatively agreed to participate in the study. Study protocol was explained to the participants and their families using a written document, and a member from each of the two families signed an informed consent form. This study was approved by the Ethical Committee of Obu Dementia Care Research and Training Center prior to commencement.
Case 1
The first participant was a 78-year-old man diagnosed with vascular dementia. He had left hemiparesis of the upper and lower limbs.
He needed a handheld walker to walk, but was still unstable while using it. He often wandered around the day room, especially in the morning and early evening, when his family did not stay with him. To prevent him from falling, a caregiver had to accompany him during this wandering. He exhibited depression, agitation, and would take off his clothes; these behaviours were recognized as BPSD. He had enjoyed listening to classical music at home, but there was little opportunity to listen to this music in the facility.
Case 2
The second participant was a 90-year-old female with a history of vascular dementia and had experienced a left hemisphere brain hemorrhage. She had severe mixed aphasia, but her auditory function was relatively well preserved, and she was able to communicate with others. Due to right hemiparesis, she needed a wheelchair. She often shouted loudly while hitting a table and would also push herself up on her wheelchair while holding a table with her left hand. These behaviours were repeated, and her loud shouting often disturbed other residents in the room. A caregiver often needed to stay with her for more than half an hour to calm her down. She also experienced hallucinations that continued throughout the day and exhibited agitation, disinhibition, and depression at various times during the day. Her favorite songs were Japanese popular ballads, and she would stay calm while she listened to them.
Procedure
Each participant’s favorite pieces of music was selected according to advice from their families. One trial of the intervention consisted of three sessions of 30 min, a listening session (LS), and one nonlistening session before (NLS-1) and after (NLS-2) the LS (ABA design). The ABA design was chosen owing to its single-subject design and ability to demonstrate individual changes as a result of treatment. The extended effects of LS (B) to NLS-2 (A) must be considered. The NLS-1, LS, and NLS-2 sessions were sequentially applied twice a day: in the morning (10:00–11:30) and afternoon (15:30–17:00), because cognitive function and behaviours generally change over the course of the day (Mazzucco et al., 2017). Since both participants usually spent their time sitting in chairs in the day room, they were simply moved below the parametric speaker during the trials. The series of sessions was conducted biweekly for four weeks. During the experiment, the number of BPSD instances was recorded; these were instances of wandering for Case 1 and agitation, such as shouting, for Case 2.
Statistical analysis
An instance of BPSD was defined as a behavioural event during which caregivers were needed to provide care. These instances were counted, and their frequencies were compared among the sessions using a one-way factorial analysis of variance (ANOVA) for each subject. Bonferroni–Dunn’s test was applied for multiple comparisons. A p-value of less than 0.05 was considered significant.
Initial and final assessments were made by an occupational therapist. The assessments included the Global Deterioration Scale (GDS) (Reisberg, Ferris, de Leon, & Crook, 1982), the Mini-Mental State Examination (MMSE) (Folstein, Folstein, & McHugh, 1975), and the neuropsychiatric inventory (NPI) (Cummings et al., 1994), conducted before and after the intervention period, although those scores were not statistically analyzed.
The GDS was used to assess the stage of dementia using a scale ranging from 1 (no cognitive decline) to 7 (very severe cognitive decline). The MMSE was used to evaluate the cognitive function using a scale ranging from 0 to 30, with lower scores indicating severe impairment. The NPI was used to rate the presence, severity, and level of caregiver distress for 12 behaviours: delusion, hallucination, agitation/aggression, depression/dysphoria, anxiety, euphoria/elation, apathy, disinhibition, irritability/lability, aberrant motor behaviour, sleeping, and eating.
Results
The pieces of music were successfully presented via the parametric speaker, and they did not cause any problems to the participants, other residents, or caregivers. The sound from the parametric speaker could be clearly heard below the speaker, but its volume was quite low at a point 1.5 m away from the subject; thus, the sound did not disturb any activity of the other residents or caregivers in the room.
Change in behaviours of participants during intervention
Over the course of four weeks, Patients 1 and 2 completed 14 and 16 sessions, respectively. Two sessions were omitted in Case 1 because his physical condition was not favorable. Both participants listened to the music provided by the parametric speaker during the LS sessions.
The sessions had a significant effect on the mean number of BPSD (wandering in Case 1 and agitation in Case 2) that necessitated care by caregivers in Case 1 (F [2, 42] = 12.47, p < .001) and Case 2 (F [2, 42] = 8.92, p < .001). Multiple comparisons showed that the number of behaviours was significantly lower during the LS session than during the NLS sessions in both cases during the intervention period (Figure 3). Neither an extended effect after LS (during NLS-2) nor an effect of time of day was found.
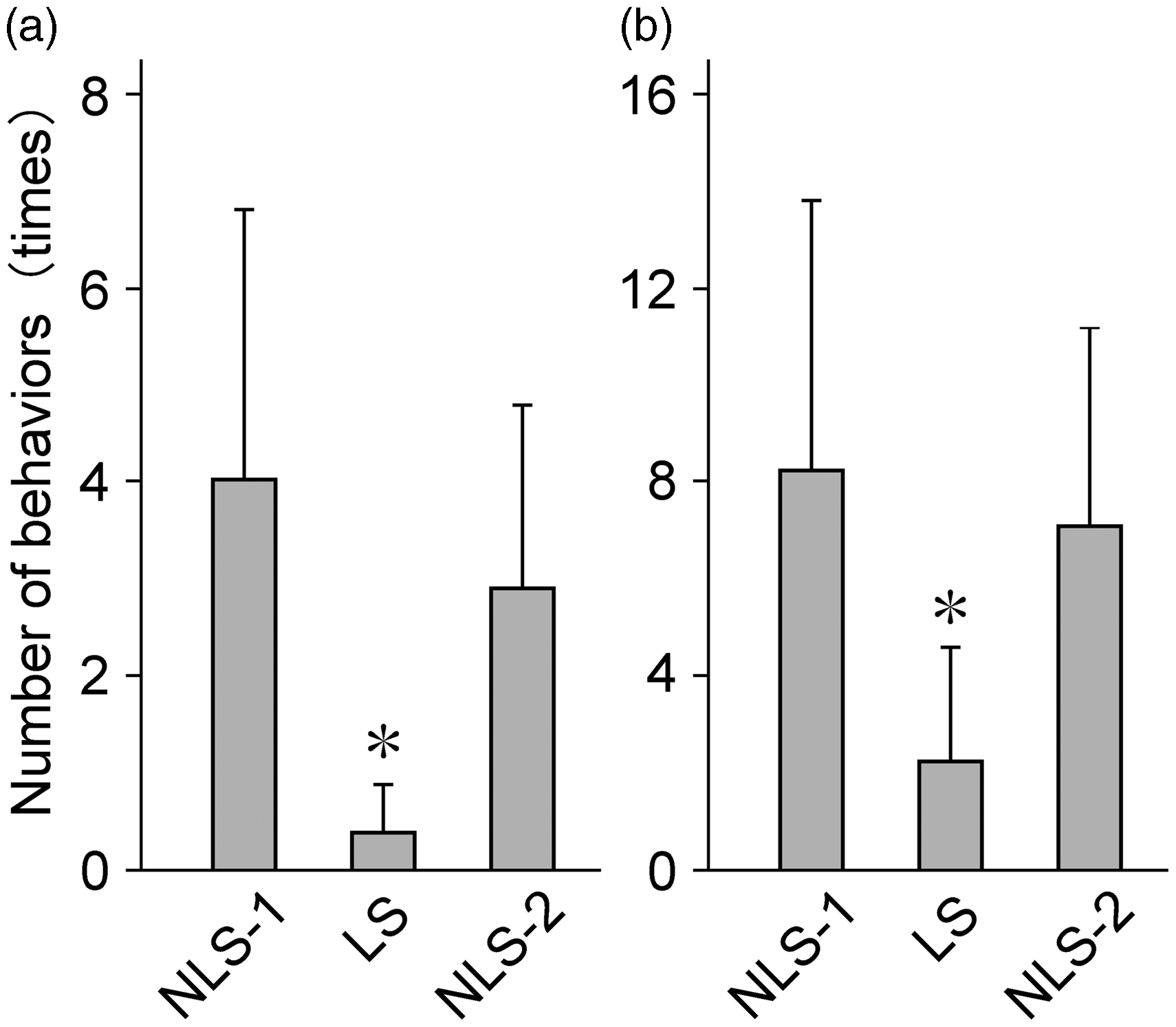
The mean number of behaviours which necessitated care by caregivers. The values were significantly lower during the LSs than sessions before (NLS-1) and after (NSL-2) LS in both cases (p < 0.01, ANOVA, Bonferroni–Dunn’s test). (a) Case 1 and (b) Case 2. LS: listening session; NLS: nonlistening session.
GDS, MMSE, and NPI scores
The GDS score did not change after the intervention, remaining at stage 6 and 7 in Cases 1 and 2, respectively. The MMSE score in Case 1 increased from 13 to 17 after intervention, but there was no change in Case 2, where the score remained 0.
The NPI score improved in both cases. In Case 1, the total NPI score was 21 points out of 120, indicating that agitation, depression, and aberrant motor behaviour were observed before the intervention. After the intervention period, agitation and depression were reduced, with the NPI item points for both reducing from 3 points before the intervention to 1 point after the intervention. However, the patient still took off his clothes in public. In Case 2, the total NPI score prior to intervention was 22 points, with the item points of hallucination, agitation, depression, and disinhibition at 8, 3, 2, and 3 points, respectively. The frequencies of hallucination and disinhibition diminished after the intervention, and their new NPI item points were 6 and 1, respectively. However, agitation and depression persisted. The total NPI score after intervention was 18 points.
Discussion
The results showed that creating a personal acoustic space with a parametric speaker was effective in decreasing BPSD. The advantages of the speaker were as follows: (1) it provided a personal acoustic environment in a common room, (2) the sound did not disturb other residents and caregivers in the room, (3) the residents did not need to wear a device (e.g. headphones or earphones), and (4) caregivers could observe residents as they usually would.
The present study showed that the numbers of wandering and agitation behaviours were significantly reduced during the LS. We selected subjects for whom the present intervention might be applicable, and therefore, we cannot report that it may be generally effective for all residents with dementia. However, the equipment was clearly effective in decreasing BPSD in the participants. A resident could also listen to his/her favorite songs without disturbing other residents in a common room, where they might feel relief owing to the presence of other residents and caregivers.
Long-term effects of the present intervention on BPSD were not observed. The numbers of wandering and agitation in Case 1 and Case 2, respectively, decreased during the LS session, but they increased again during the NLS-2 session. In both cases, some BPSD disappeared after the intervention, but others remained unchanged. We did not observe that the present intervention changed the basic pathophysiology for BPSD, but it temporarily decreased the symptoms during the LS sessions.
Future studies could confirm whether the same setting used in this study could reduce other types of BPSD and should use a larger sample size so that more significant results might be obtained.
We propose that this equipment could be used for individualized rehabilitation in a care facility. Individualized care has reportedly had positive effects on older residents as well as on caregivers’ job satisfaction (van den Pol-Grevelink, Jukema, & Smits, 2012), but it sometimes exacerbates manpower shortage, one of the crucial problems in residual care facilities (Zeller, Dassen, Kok, Needham, & Halfens, 2011). This problem is now at a critical stage in Japan, and the latest techniques to provide individualized care should be applied.
The safety of the parametric speaker has been studied in the field of technology. It has been found that there is no adverse effect of the parametric speaker, at least in the ultrasonic wave range of 40 kHz, on either physical or mental conditions (Lee et al., 2011, 2012). However, the quality of sound produced by the experimental parametric speaker was not high. The sounds from the experimental speaker contained some high-frequency noise, which might not be suitable to provide music with high-quality sound. Parametric speakers available commercially might provide high-quality sounds, but they are still expensive.
In conclusion, we report that the use of a parametric speaker is effective in cases with specific BPSD in a residual care facility. The parametric speaker could be used in various situations in a care facility; for example, a sound could indicate the location of a toilet or another area for residents with visual disabilities or dementia (Lee et al., 2011). One of the main advantages of using the parametric speaker was being able to create a personal space in a common room. We believe that this equipment could be useful in providing individualized care for a better residential QOL.
Footnotes
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was partially supported by the Japan Society for the Promotion of Science (Grant-in-Aid for Scientific Research C: 24591292), Ministry of Health, Labour and Welfare (Kenko-zoshin 25).
