Abstract
Lifestyle medicine (LM) is a rapidly growing medical specialty that can be integrated into all aspects of care. LM is implemented across primary, specialty, inpatient, outpatient, community and home settings, with multiple modalities, including virtual, individual or group visits. This position paper outlines how LM achieves value, improves health outcomes, and meets the goals of the Quintuple Aim, thus providing a framework to guide LM stakeholders, including patients, providers, payers, employers, and community organizations. It is the position of the American College of Lifestyle Medicine (ACLM) that: (1) The LM care delivery model addresses the escalating chronic disease healthcare burden; (2) LM is a powerful catalyst for healthcare transformation that delivers the Quintuple Aim; (3) LM is whole-person care implemented for all populations, across various settings, intensities and modalities; (4) LM providers are trained, interdisciplinary experts in chronic disease care across the continuum, from prevention to treatment and remission of disease; (5) nine core elements are essential to an effective and evidence-based LM care framework.
“LM provides a framework to guide all healthcare stakeholders to implement a high-value solution that meets the goals of the Quintuple Aim.”
Background
Chronic conditions such as ischemic heart disease, stroke, and type 2 diabetes (T2D), are among the leading causes of disease burden and mortality worldwide.1-3 In the US, upwards of 30% of children have a chronic condition or functional limitation, 4 and 76% of adults have at least one chronic condition, and for those 65 years and older, this prevalence rises to above 90%. 5 Adding to the urgency is the fact that the prevalence of overweight and obesity among US adults 20 years and older is estimated to be over 70% 6 with a projected prevalence of over 80% by 2050 among US adults. 7 Estimated prevalence for T2D among US adults is 21%–33% by 2050. 8 Disability-adjusted life years (DALYs) due to diabetes increased by nearly 39% globally and by nearly 54% in the U.S. from 1990-2021, with over 1.3 billion individuals globally expected to be living with diabetes by 2050. 9 In addition to the impact on longevity and quality of life, chronic diseases drive an escalating annual healthcare expenditure burden reaching 4.9 trillion dollars in 2024 with an increase of 7.5% in 2023 alone.10-12 The US spends more per capita than other comparable nations, yet has the lowest performance on key population health metrics such as life expectancy and avoidable mortality. 13
The healthcare crisis has led to multiple reform attempts to control costs and improve outcomes such as managed care and, with an awareness of the need to improve care coordination and accountability, the concept of “value” emerged. Value-based care is described as better health outcomes for the cost of care. 14 It became part of the larger reform strategy to align payments with better patient and population health. Value-based financial incentives offer a range of alternative payment options, and CMS aims to have all Medicare and most Medicaid beneficiaries in value-based accountable care by 2030. 15 Yet, the adoption of value-based care is limited without incentives that align across all stakeholders and models that support a comprehensive, whole-person approach.16,17
Evidence shows about 80% of chronic diseases and premature deaths could be prevented by lifestyle-related behavior changes. 18 LM is one of the fastest growing medical specialties, and ACLM is an essential driver of high-value healthcare transformation with a focus on delivering evidence-based lifestyle interventions for the treatment, remission and prevention of these chronic conditions. 19 LM is grounded in 6 pillars and delivers comprehensive, team-based, integrated whole-person care that activates the patient in sustainable lifestyle change.19,20
Objectives
The objectives of this position paper are to: (1) present the position of the American College of Lifestyle Medicine on how LM is poised to provide high-value care; (2) support this position with evidence-based research, and (3) call for systematic alignment of chronic disease care using a framework of high-value care rooted in LM.
Methods
A task force was assembled with experts across a number of clinical fields including family medicine, internal medicine, emergency medicine, endocrinology, cardiology, pediatrics, oncology, preventive medicine, and psychiatry, all with substantial experience practicing LM. The task force met virtually on a monthly basis. Five statements were developed using a facilitated process involving iterative discussions. The process involved monthly 1-hour meetings for approximately 1 year facilitated by the task force chair (SM) and ACLM staff members (KLS, TAH). Post-meeting summaries were sent via email, and further discussion sometimes occurred over email. Position statement 5 was developed first with the task force identifying eleven core elements of effective and evidence-based LM care, mapping core elements to identified gaps in care. After further refinement, the task force voted to formally adopt 9 core elements (statement 5). Stemming from this facilitated process, other topics about lifestyle medicine care and delivery were identified and further developed into statements 1-4. The 5 statements developed by the task force were reviewed and approved by the ACLM Board of Directors Executive Committee. The Committee provided wording suggestions that were incorporated by the task force to finalize the statements.
A literature search was simultaneously performed in Medline focused on identifying literature from the past full year at the time of the search (all of 2023-June 2024). The search strategy is included in Supplemental File 1. A total of n = 346 results were returned, and these were single-screened for relevance by three members of the team (SM, KLS, TAH), guided by input from team discussions during meetings. Seventy-five abstracts were identified as highly relevant, n = 54 as potentially relevant, and the remaining n = 217 as not relevant. Studies were excluded if they were not in English or were not human studies. Relevant abstracts were grouped into the following categories, identified based on themes after an initial review of the included abstracts: bariatric surgery vs LM intervention; barriers to LM; community LM interventions; LM in employee populations; health equity; LM education; LM pertaining to the following health outcomes: aging, brain health/cognition, cardiovascular outcomes, cancer, chronic kidney disease, type 2 diabetes, liver disease, and osteoarthritis/rheumatoid arthritis; sleep interventions; LM and GLP1 receptor agonists; pediatric LM intervention; provider-patient alliance; whole health implementation; and whole health and the veteran’s health administration. Nine additional sources identified via hand-search were deemed relevant. This final set of abstracts was shared with the task force to consider throughout the process of both developing the position statements as well as, later, writing the accompanying text.
Supporting Research for Position
(1) The LM Care Delivery Model Addresses the Escalating Chronic Disease Healthcare Burden
Currently in the US, reimbursement is largely fee-for-service, with care that is often reactive and fragmented by managing symptoms and complications rather than proactively addressing root causes. Payment incentives are for quantity of services rather than quality of care, contributing to the rise in chronic conditions. 21 Fragmented care is not person-centered care as the patient must navigate a labyrinth of providers, referrals, and technology, resulting in greater adverse outcomes (ED visits, healthcare costs, etc.). 22 Providers experience a lack of coordinated, collaborative care contributing to their own burnout, while the health systems and payers have misaligned incentives for care and utilization. The resulting burden is escalating cost, a shortage of healthcare providers affecting access to care, unengaged patients, poor quality of care, poor patient outcomes, and an inefficient model of care. 23
LM offers an alternative to this model and takes an evidence-based approach to using therapeutic lifestyle interventions as a primary modality to treat chronic disease, rooted in 6 pillars: whole-food, plant-predominant nutrition; regular physical activity; restorative sleep; stress management; avoidance of risky substances; and social connectedness. 19 LM-trained professionals assess a patient’s current health behaviors and offer person-centered interventions in varying levels of intensity to prevent and treat the root causes of chronic disease. 24 The professional works together with the patient to empower them to identify achievable steps toward optimizing those lifestyle behaviors. Standard care does not allow adequate time and training for detailed discussion surrounding behavior change. While standard care is fragmented and monitors worsening chronic disease, LM care is coordinated, team-based, outcomes-driven, and focused on continuous improvement. Many clinical practice guidelines for chronic conditions recommend lifestyle change as first-line or adjuvant treatment, with one study highlighting that 83% of clinical practice guidelines from 2010-2021 made food group recommendations. 25 Thus, implementing lifestyle change into clinical practice needs better reimbursement to sustain the growing interest in LM provider and team training.
(2) LM is a Powerful Catalyst for Healthcare Transformation that Delivers the Quintuple Aim
An approach to deliver value-based care was outlined in the National Academy of Sciences, Engineering, and Medicine (NASEM) landmark report, “Implementing High-Quality Primary Care: Rebuilding the Foundation of Health Care.” 26 The NASEM report offers a vision for transforming primary care in the United States, recognizing that a strong primary care system is foundational to achieving better population health, equity, and sustainable health care systems. High-quality care is described as a patient-centered, holistic, coordinated and integrated, comprehensive, team-based approach with aligned payment incentives as in value-based care models.
By fully integrating the patient’s physical, behavioral and health-related social needs (HRSN), LM care delivers high-quality, high-value care that addresses each aspect of the Quintuple Aim as outlined below. 27 Patients are activated, motivated, and empowered with lifestyle change. 24 LM professionals develop person-centered care plans using comprehensive assessments rooted in personal goals and cultural competency. This approach of engaging patients shows promise for improving healthcare 28 and may lead to higher patient satisfaction, improved clinical outcomes, and a better overall experience. By focusing on lifestyle changes that patients can control, such as diet and exercise, lifestyle medicine empowers patients to take an active role in their health, improving engagement and satisfaction.
Improving Population Health
Lifestyle medicine delivers better population health outcomes by directly addressing the root causes of many chronic diseases, such as heart disease, diabetes, and obesity to treat, prevent and, often, reverse chronic conditions as demonstrated by several landmark studies.20,29-34 LM care improves population health with greater access for all populations to multiple modalities of care. 20 LM care can be offered individually or in group settings such as shared medical appointments (SMAs), in a clinic or virtually, or in a school, workplace, community or home setting.35-38 LM care uniquely positions objective measurement of health behaviors as a leading outcomes metric. Objective measurement of health behaviors and patient-reported outcomes measures (PROMs) drives upstream population health goals. This allows LM clinicians to mitigate health risk from suboptimal health behaviors and reduce the impact of previously diagnosed chronic diseases.
Enhancing Patient Experience and Outcomes
Lifestyle medicine takes a person-centered approach, where healthcare providers collaborate closely with patients to establish and achieve health goals related to their lifestyles. Specifically, LM professionals develop person-centered care plans accounting for unique circumstances, preferences, and goals based on comprehensive assessments and screening tools. This can improve patient satisfaction and provide a better overall experience. 24 By focusing on lifestyle changes that patients can control, LM empowers patients to take an active role in their health, improving engagement and satisfaction. In addition, LM fosters a more meaningful patient-provider therapeutic alliance that enhances communication and promotes shared decision-making to improve the patient experience. This strong patient-provider therapeutic alliance is a key driver for patient engagement that can help facilitate behavior change. 28
Lowering the Cost of Care
By prioritizing preventive measures and lifestyle modifications, lifestyle interventions can significantly lower healthcare costs by reducing the need for expensive procedures, pharmaceuticals, avoidable ED visits, hospitalizations and readmissions—particularly for individuals with chronic diseases, who are often among the costliest patients to treat.39-42 LM aims to achieve both clinical and cost-effectiveness as foundational to care. Participants in an employer-sponsored disease management program which included medication optimization and care coordination achieved improvements while yielding an impressive return on investment (ROI) of $9.64 for every $1 invested. 43
The concept of lifestyle modification to reduce costs is not new. In 1998, the Ornish Intensive Cardiac Rehabilitation (ICR) program delivered an average savings of $29,000 per patient over a three-year period by avoiding costly revascularization procedures. 44 These examples illustrate how lifestyle medicine delivers high-value care by improving health outcomes while significantly reducing the cost burden on healthcare systems, making it an essential component in the future of value-based care. ACLM is highly committed to the adoption of LM care models that deliver results on cost and quality. Since the implementation of LM is relatively recent, studies on cost-effectiveness are limited. Objective measurement of health outcomes, behaviors, provider well-being, and PROMs will allow for future comparative effectiveness research on this topic.
Health Professional Well-being
A recent study showed that providers who integrate lifestyle medicine more deeply into their clinical practice report lower likelihood of burnout. 45 Remarkably, 90% of those surveyed reported that lifestyle medicine positively impacted their professional satisfaction. 45 By empowering providers with the knowledge and tools to embrace healthy lifestyle behaviors themselves, lifestyle medicine can serve as a vital antidote to the growing issue of burnout in healthcare providers. In addition, by moving from simply treating symptoms to addressing the root causes of illness, clinicians can find deeper satisfaction in their work. This model fosters stronger patient-provider relationships, leading to enhanced outcomes and more gratifying patient interactions—ultimately enriching the professional lives and well-being of healthcare providers.
Addressing Health Disparities and Promoting Health Equity
LM addresses health disparities by advancing health equity with accessible, culturally relevant interventions and shared decision-making for patient-empowered lifestyle behavior change. Community-engaged lifestyle medicine (CELM) is an evidence-based framework that prevents chronic disease and promotes healthy lifestyle behaviors with a collaborative, community-engaged, and culturally relevant delivery of LM across multiple stakeholders. 37 LM considers health-related social needs (HRSN) such as access to healthy food, safe, walkable environments, and educational resources.20,46
(3) LM is Whole-Person Care Implemented for all Populations, Across Various Settings, Intensities, and Modalities
LM is whole-person care integrating comprehensive physical, behavioral, and culturally competent social needs assessments and interventions that are person-centered, across the continuum of care from treatment, remission, and prevention, when applicable.
27
LM is accessible within a variety of care settings, including primary care organizations, integrated health systems, other clinical networks, schools, the workplace, community organizations and within the home. Just as adherence to medication therapies is reinforced at every stage of medical care, therapeutic lifestyle intervention is delivered by LM-certified clinicians and is accessible at
Primary Care
LM successfully delivers the continuum of care by implementing the level of intensity and intervention needed. (1) Comprehensive Assessments: LM vital signs, comprehensive health behavior, patient readiness for change, PROMs assessments, and LM prescriptions as part of annual wellness and health promotion visits (2) Therapeutic lifestyle change (TLC): low-to-medium level of intervention dosing to support incremental changes during regular office visits (3) Intensive therapeutic lifestyle change (ITLC): higher, intensive dosing; reaches maximum effort with the goal of supporting disease remission
Pediatrics
Lifestyle medicine interventions in pediatric populations (ages 0-18 years) are critical for the treatment, remission and prevention of diseases at an age where it can have a large impact on life and health span. The range of diseases that lifestyle medicine can apply to in the pediatric population is vast and includes some of the more obvious, such as overweight and obesity, hypertension, diabetes, and heart disease; as well as less obvious, such as asthma, ADHD, mental health disorders, and autoimmune diseases. In addition, the LM care model of collaborative, interprofessional teams, family engagement and care coordination are essential for children with special health care needs.47,48
Endocrinology and Diabetes Care
LM, with its emphasis on interprofessional, team-based, comprehensive care, low overall costs, sustainability, and high rates of patient and provider engagement, is an optimal solution for high-value endocrine care and fostering health equity and access. Previous work has demonstrated that intensive dietary change can achieve remission of type 2 diabetes,49,50 and ACLM’s clinical practice guideline on lifestyle intervention for treatment of prediabetes and T2D offers a roadmap for delivering therapeutic lifestyle change. 51
According to the American Diabetes Association (ADA), “high-quality diabetes care” is a patient-centered approach that prioritizes individual needs, considers social determinants of health, and focuses on “optimizing” diabetes management, essentially providing the
Perhaps the domain facing the most revolutionary change in all of modern endocrinology is the realm of newer anti-obesity medications (AOMs) such as the glucagon-like peptide agonists. Yet with barriers such as low adherence rates,53,54 cost and side effects, LM programs are vital to support high-value outcomes as they are implemented at a fraction of the drug costs with more sustainable long-term outcomes. 55
Cancer Care
LM is increasingly recognized as essential at each stage of the cancer journey from risk reduction through treatment, including advanced cancer.56-61 LM significantly reduces colorectal cancer (CRC) risk, the leading cancer-related cause of death in men under 50, 62 and healthier lifestyle behaviors can reduce the risk of breast cancer. 63 Benefits of lifestyle extend beyond just risk reduction and include cancer treatment. 64 In addition, lifestyle is highlighted in guidelines for cancer survivorship to reduce risk of recurrence.65,66
Hospital Settings
In addition to LM implementation in outpatient and primary care settings, the impact and value of LM in hospital-based settings (emergency department, inpatient, post-acute care, transition care), including rehabilitation hospitals, is gaining attention and provides value by reducing readmissions, avoidable ED visits and post-acute complications. LM in the acute-care setting and rehabilitation facilities improved patient outcomes among the sickest patients, particularly for patients with conditions such as cardiovascular disease, diabetes, and obesity.
A recent CMS report outlined a readmission prevention strategy that describes the LM care model: identifying root causes, including health-related social needs, patient education/empowerment, use of an interprofessional team, and community partnerships to support post-acute/transition care. 67
There are emerging proven models of healthcare systems providing lifestyle interventions in these contexts, such as the Loma Linda University Health inpatient consult service, which provides LM care in the adult inpatient and post-acute rehabilitation settings. 68 Service provision was expanded stepwise to include all major clinical teams (hospitalist, cardiology, general surgery, obstetrics/gynecology, and neurology services) and locations (patient rooms, emergency department, as well as the intensive care unit and peri-operative areas). 69
(4) LM Providers are Trained, Interdisciplinary Experts in Chronic Disease Care Across the Continuum, Including Prevention, Treatment, and Remission of Disease
A fundamental element of LM’s high-value care framework is its emphasis on delivering comprehensive care across the continuum of health: from prevention (health promotion) to treatment (therapeutic lifestyle change, or TLC) and, when feasible, the remission (intensive therapeutic lifestyle change, or ITLC) of chronic disease. This approach requires integrating evidence-based lifestyle interventions and health-promoting behavior changes into all phases of patient care to reduce disease risk, halt progression, and potentially restore health.51,70
The American Board of Lifestyle Medicine used a consensus-based process to identify 88 core competencies to define the knowledge and skills required for healthcare professionals to “provide high quality lifestyle interventions that optimize chronic disease outcomes with effective, efficient, and accessible care.” 70 One theme reflected throughout these competencies is the importance of LM professionals being able to describe the evidence around how lifestyle interventions can improve health and behaviors. Additionally, practical skills are highlighted, such as writing lifestyle prescriptions and referrals to other appropriate, trained professionals with expertise in LM pillars such as nutrition, physical activity, and sleep.
A new clinical practice guideline on LM for treatment and remission of T2D and prediabetes in adults demonstrates how guidance for practicing LM continues to expand. 51 This guideline was endorsed by the American Association of Clinical Endocrinology, American Academy of Physician Associates, American Association of Nurse Practitioners, American College of Clinical Pharmacology, Obesity Medicine Association, American Academy of Sleep Medicine, Association of Diabetes Care & Education Specialists, and National Board of Health and Wellness Coaches. It was also designated with an “Affirmation of Value” from the American Academy of Family Physicians and is supported by the Academy of Nutrition and Dietetics. The guideline provides pragmatic, evidence-based recommendations in the form of 14 key action statements to further guide clinicians and healthcare providers in treating patients and improving quality of care. The guideline also includes a number of practical tools to help in assessing and educating patients, as well as prescribing lifestyle as treatment. Complementing the guideline is ACLM’s CME/CE course on remission of T2D and the Lifestyle Empowerment for Diabetes Remission (LEADR) Curriculum to support healthcare professionals in delivering sustainable behavior change for patients with diabetes.
As noted in the 2022 core competency update, as LM grows, LM high-value care is best provided by a team of LM-trained clinicians and other healthcare providers, as depicted in Figure 1, who are organized and supported to meet the needs of the people and the communities they serve.
70
Team-based care improves health care quality, use, and costs among chronically ill patients, and can also lead to reduced burnout among healthcare professionals.71-74 Well-designed teams deliver nurturing, longitudinal, person-centered care with multiple modalities such as shared medical appointments (SMAs) either in an inpatient/outpatient facility, community setting, home, or virtually. LM treatment can be efficiently delivered in group settings, in the form of SMAs, which are a cornerstone of LM as their benefits are well-documented in a variety of contexts.36,38 These visits offer The lifestyle medicine interprofessional care team.
There are multiple pathways for interdisciplinary healthcare professionals to obtain lifestyle medicine CME/CE/MOC, including educational and experiential pathways to board certification as depicted in Figure 2. ACLM also offers training for community health workers to provide education, tools, and resources to improve patient health. Pathways for interdisciplinary healthcare professionals to obtain lifestyle medicine CME/CE/MOC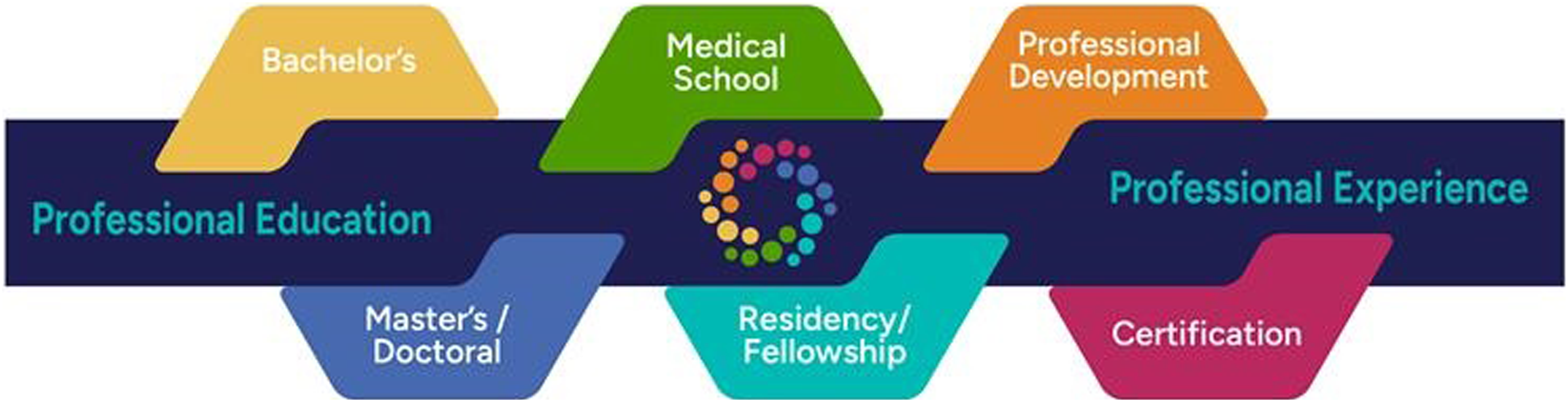
Interdisciplinary healthcare professionals implement lifestyle medicine with comprehensive assessments and screening tools, including the Lifestyle Medicine Assessment, 75 to evaluate the patient’s current health behaviors in the six domains of LM. Treatment is provided through lifestyle medicine prescriptions or interventions that are co-created with patients using a SMART (specific, measurable, achievable, relevant, time-bound) goal-setting approach, and applied by giving the patient a concrete action plan. Reassessments occur during follow-up visits, and LM prescriptions are adjusted accordingly. In addition, ACLM has developed multiple practice support resources, such as guides to LM SMA, reimbursement roadmap and provider toolkits to advance the implementation of LM care.
By addressing lifestyle factors, the interprofessional team delivering primary and specialty care can meet their patients’ needs, promoting health while simultaneously addressing chronic conditions.
(5) Nine Core Elements are Essential to an Effective and Evidence-Based LM Care Framework
As a multidisciplinary and growing specialty that can be implemented across a variety of settings, LM is delivered in diverse ways. Some LM-trained clinicians may focus on prevention while others deliver more intensive lifestyle programs to treat and reverse chronic conditions, in either virtual or in-person groups, in clinical, workplace, or community settings. Given the broad scope, impact and relevance of LM, there emerged recognition that delineating LM as a framework for high-value care is essential in communication with all stakeholders such as patients, providers, healthcare administrators, community partners, payers and government agencies.
The Nine Core Elements of LM Care are as follows:
The Core Elements of the LM High-Value Care Framework to Drive Healthcare Transformation.
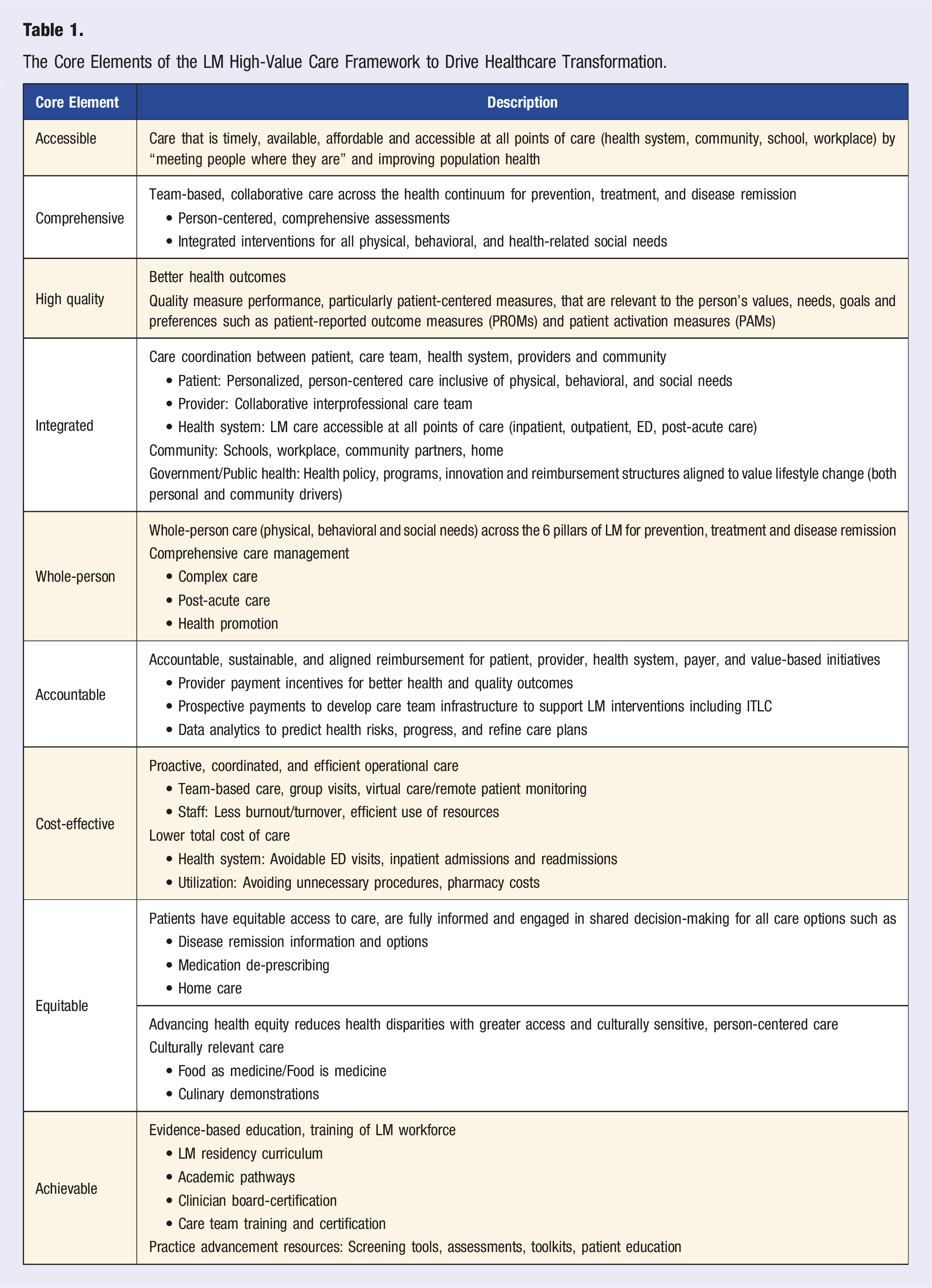
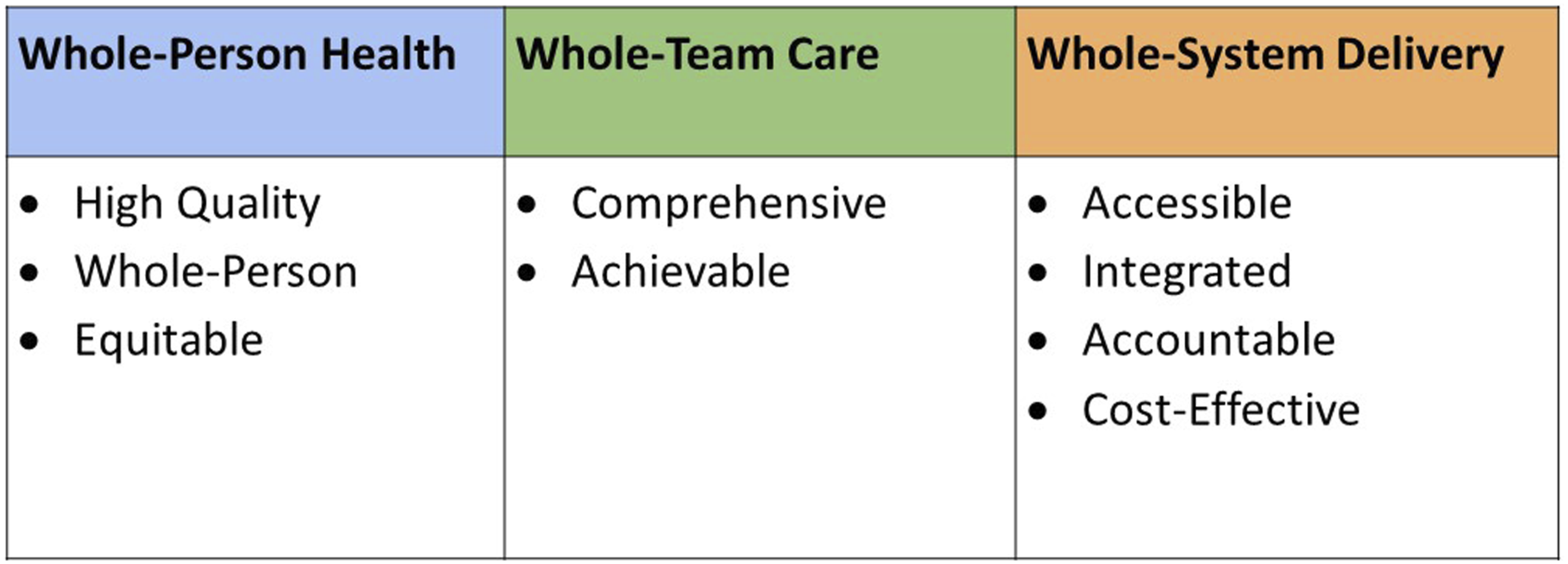
Nine core elements categorized into three care domains.
Conclusion
This position paper describes LM as a framework for high-value, whole-person care. This care is comprehensive and integrated with highly engaged patients empowered in a therapeutic alliance with an interprofessional team delivering care across the continuum from prevention and treatment to remission. ACLM, as the medical and professional society for LM, provides a roadmap with training, board certification, clinical practice toolkits, and numerous other resources to implement LM care. LM provides a framework to guide all healthcare stakeholders to implement a high-value solution that meets the goals of the Quintuple Aim: better health outcomes, patient satisfaction, provider well-being, and advancing health equity at a lower cost of care (Figure 4). Lifestyle medicine high-value care framework.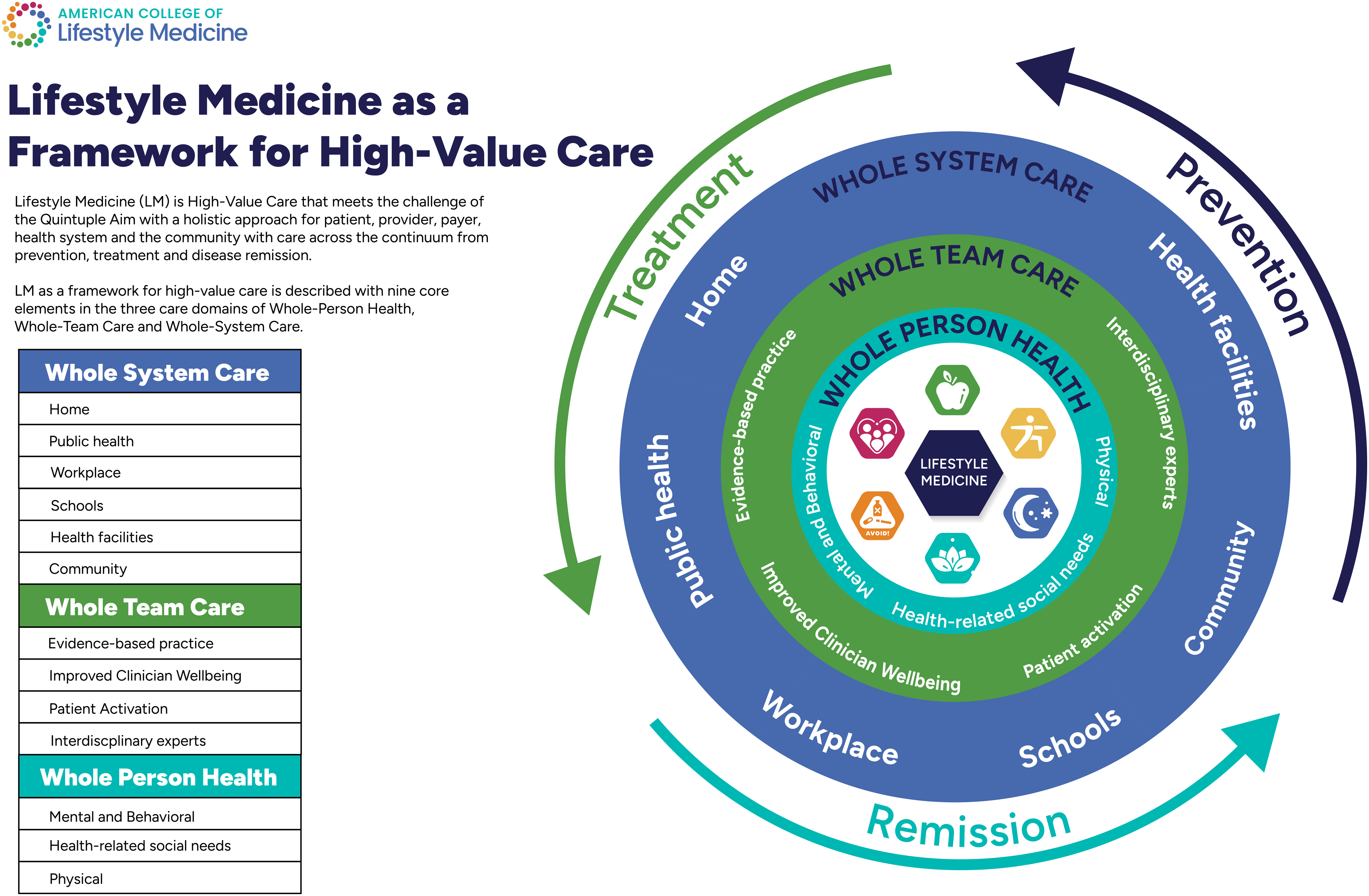
Supplemental Material
Supplemental Material - Lifestyle Medicine as a Framework for High-Value Care: A Position Statement From the American College of Lifestyle Medicine
Supplemental Material for Lifestyle Medicine as a Framework for High-Value Care: A Position Statement From the American College of Lifestyle Medicine by Samrina Marshall, Padmaja Patel, Rahul Anand, Kristi Artz, Allison Collins, Meagan Grega, Mahima Gulati, Tyler A Hemmingson, Sami Mansfield, Aruna Nathan, Kaitlyn Pauly, Steven G. Sugden, Valeria Tivnan, April Wilson and Kara L. Staffier in American Journal of Lifestyle Medicine.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Samrina Marshall is a healthcare advisor for the American College of Lifestyle Medicine (ACLM); Kristi Artz has stock options with Nudj Health; Kara Staffier and Kaitlyn Pauly are ACLM staff; Tyler Hemmingson was an ACLM staff member at the time of writing; Padmaja Patel is President of ACLM and CMO of Nudj Health.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the American College of Lifestyle Medicine.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
