Abstract
The incidence of type 2 diabetes (T2D) is increasing globally alongside poor diet quality, sedentary lifestyle, and obesity, outpacing the capacity and resources to effectively prevent and manage its impact. The glycemic benefits of lifestyle modification to prevent T2D and its downstream comorbidities and mortality are supported by numerous epidemiologic studies and randomized trials. However, despite lifestyle modification being the standard of care practice both for prevention and treatment of T2D, there has been limited success in curbing this pandemic, possibly due to environmental and socioeconomic barriers to the uptake and long-term adherence to healthy lifestyle programs. Therefore, mitigating the incidence and downstream health effects of T2D requires innovative clinical and population-based solutions for the implementation of sustainable lifestyle modification interventions. It is also important for public health stakeholders to address the numerous systemic and environmental barriers that persistently undermine the long-term success of adopting healthy diet and physical activity changes. Although interventions to improve diet, physical activity, and body weight are effective for preventing T2D and many of its downstream consequences, multi-pronged efforts to enhance the uptake of these programs and support long-term adherence are critically needed to reverse the current trends of this costly and debilitating chronic disease.
“Epidemiologic evidence indicates that the benefits of T2D prevention with sustaining healthy lifestyle patterns long-term are generalizable to the broader population.”
Introduction
Type 2 diabetes (T2D) affects nearly 10% of the population worldwide and is projected to increase from its current prevalence of 537 million adults to 784 million by 2045. 1 The global economic burden of T2D exceeded 900 billion US dollars in 2021, disproportionately affecting low- and middle-income countries with 80% of cases. 2 Genetics play a prominent role individual-level susceptibility to T2D and over 500 distinct polymorphisms have been identified, contributing to its estimated heritability of 25-72%. 3 Additionally, increasing prevalences of overweight and obesity, unhealthy lifestyle patterns, and aging populations have driven the recent pandemic surge in T2D. 4 Of the 75.6 million life-years lost globally due to T2D in 2021, an estimated 45% is attributed to habitually poor diet, low physical activity, and cigarette smoking, with another 52% due to high body mass index (BMI). 4 Thus, the widespread availability of sustainable and cost-effective population- and individual-level interventions to improve lifestyle is of major public health importance.
Clinically, referral and support to adopt and maintain a healthy lifestyle has been the cornerstone of T2D prevention among high-risk patients, supported by landmark randomized controlled trials (RCTs) such as the Da Qing T2D and Diabetes Prevention Program trials conducted more than 20 years ago.5,6 The prevention of T2D with healthy diet and physical activity interventions, alone or in combination, is also supported by several shorter-term clinical trials investigating effects of lifestyle on improvements in intermediate glycemic traits.7,8 Among patients already diagnosed with T2D, RCTs establishing the effectiveness of lifestyle for the prevention of progression to the microvascular and macrovascular complications of T2D and cardiovascular disease outcomes are sparse due to the need for relatively longer durations of follow-up to observe the development of clinical endpoints. However, there is a large body of evidence that diet quality, physical activity, and weight loss through a variety of interventions have beneficial effects on intermediate biomarkers of T2D morbidity and mortality, such as improved glycemic control and insulin sensitivity.8,9 Additionally, there is robust evidence for the effects of lifestyle on non-glycemic comorbidities conducted among T2D patients, such as reductions in blood pressure, chronic inflammation, and improved blood lipid levels, indicating a cardiovascular benefit. 9
The underlying causes of T2D are complex and multifactorial, underscoring the need to consider prevention and treatment interventions that have broad-spectrum effects, such as the modification of diet and physical activity, for reversing global trends in T2D incidence and burden. In this narrative review, we summarize the state of the evidence supporting the efficacy of lifestyle interventions across the continuum of T2D, from the prevention of T2D onset among individuals at high risk, to mitigating the risk of microvascular and macrovascular morbidity and mortality among patients already diagnosed (Figure 1).
10
Comprehensive research supporting these benefits and the plausible underlying mechanisms stem from large-scale epidemiologic studies with long-term follow-up, randomized pragmatic interventions, and traditional experimental studies. There is also increasing recognition of the need to improve the implementation of behavioral and lifestyle interventions to maximize patient uptake and long-term adherence. Importantly, there also needs to be change at the environmental and population level to facilitate, rather than undermine, the adoption of healthier diets and physical activity. Finally, we discuss the role of newer medications for weight loss and diabetes management as potential complements to lifestyle strategies. Research supports lifestyle modifications for maintenance of glycemic control, preventing progression to type 2 diabetes among those at high risk, and glycemic control in patients with typ2 diabetes to mitigate vascular complications.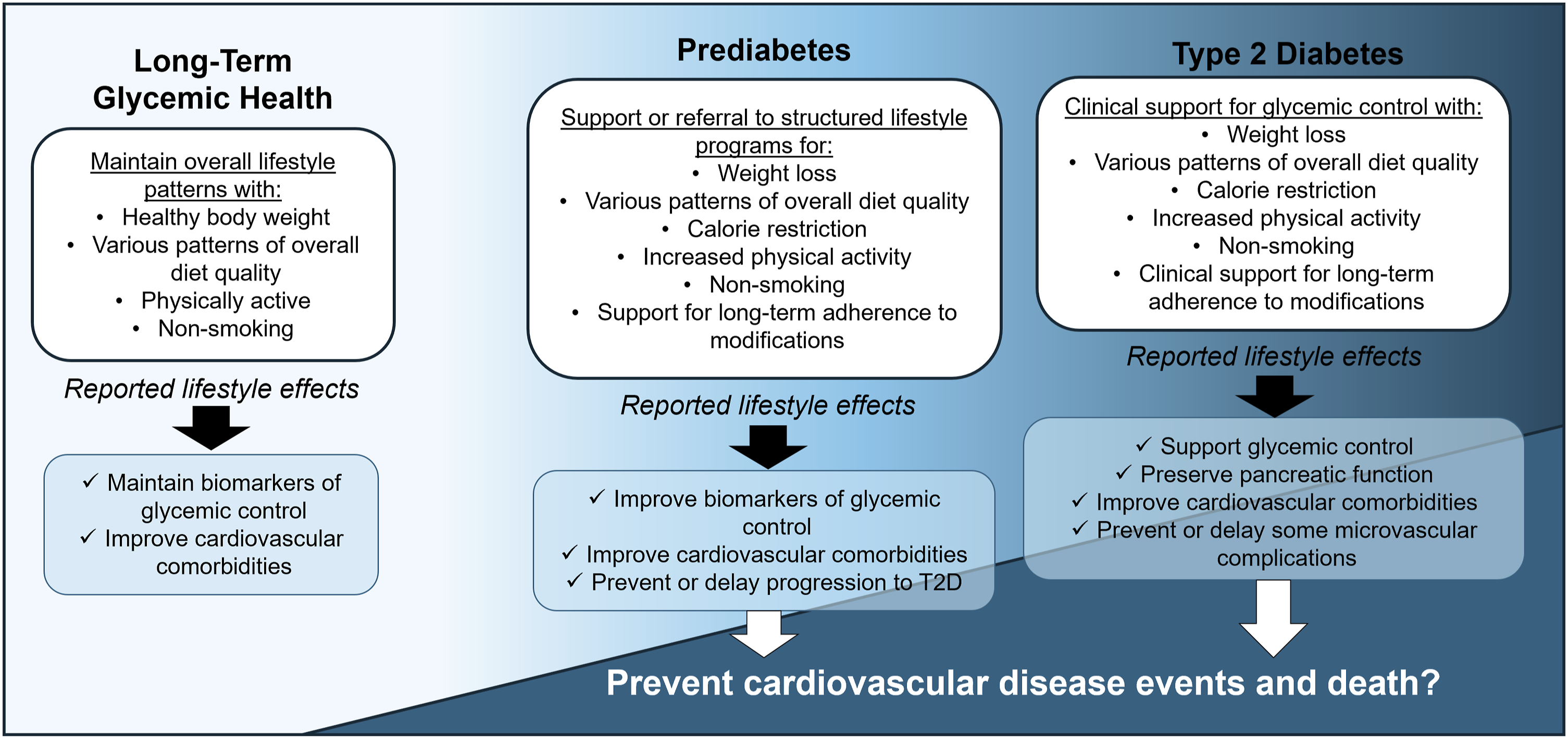
Lifestyle Strategies for T2D Prevention
Lifestyle-based prevention programs have been predominantly evaluated among target populations of adults at high T2D risk, including those with impaired fasting glucose or insulin, glucose intolerance, family history, or history of gestational diabetes mellitus in a prior pregnancy, with the goal of delaying the trajectory towards a T2D diagnosis. The World Health Organization (WHO) defines impaired fasting glucose as plasma glucose levels of 100 to 125 mg/dl (5.6 to 6.9 mmol/L) and impaired glucose tolerance as plasma glucose levels of 140 to 199 mg/dL (7.8 to 11.0 mmol/L) 2 h after a 75g oral glucose tolerance test challenge. 11 The American Diabetes Association (ADA) implements a threshold for preventive action at prediabetes defined as 5.6 mmol/l (100 mg/dl) in 2003, and broadened to also consider HbA1c ≥ 5.7% in 2010. 12 In observational follow-up of patients with impaired fasting glucose, the 5- and 10-year cumulative incidences of conversion to T2D were 18% and 23%, respectively. 13 Predictors of progression among those at high risk include low diet quality, sedentary lifestyle, older age, overweight or obesity, family history of T2D, a history of gestational diabetes mellitus, and some race/ethnicity groups. 14 However, in this same population, 34% of patients had reverted to normoglycemia at 5 years; thus, there is potential for preventing and even reversing the course towards T2D.
Upon clinical recognition of impaired glucose tolerance or other high risk indicators for T2D, the ADA and the European Association for the Study of Diabetes (EASD) recommend a combination of intensive diet and physical activity lifestyle changes including 5-7% body weight loss, and in some instances pharmacological therapy, to prevent further impairment.15,16 A series of landmark research trials from the 1990s and 2000s underscored the pivotal role of lifestyle modification in clinical prevention of T2D. 17 For example, the DaQing T2D prevention trial conducted in China randomized 577 patients with impaired glucose tolerance to one of three lifestyle interventions for up to 6 years. 5 At 6 years, the cumulative incidence of T2D onset was 67.7% in the control group, while the diet, exercise, and diet-plus-exercise programs reduced 6-year incidence to 43.8%, 41.1%, and 46.0%, respectively. Shortly after, findings from the US Diabetes Prevention Program (DPP) replicated the efficacy of randomization to an intensive lifestyle change. Investigators randomized 3234 high-risk adults with prediabetes to daily metformin, placebo, or to participate in an intensive lifestyle intervention program, including a reduced calorie diet and physical activity goals to induce and sustain weight loss. The lifestyle group had a 58% reduction in T2D incidence vs control group over 2.8 years follow-up. 6 By the end of follow-up, 38% of participants in the intensive lifestyle intervention arm maintained their weight loss goal of 7% body weight and 74% reported that they continued to achieve the physical activity goals. Although both the metformin and lifestyle intervention arms had comparatively lower risk of T2D than the placebo group, 31% and 58% respectively, the lifestyle intervention arm saw a 39% lower risk of diabetes compared with metformin. 6 These findings have been replicated in diverse populations with varying diet and physical activity regimens. A meta-analysis of 11 RCTs summarized a 64% lower risk of progression from prediabetes to T2D under these interventions vs comparator groups. 18 Further, while the benefits of lifestyle vs control groups for T2D prevention waned over post-trial observational follow-up periods when the intensive programming ended, there was evidence that a benefit for T2D persisted for ∼15 years in the DPP and over 23 years in the DaQing study populations. 19 However, extended observational follow-up of the DPP did not show this translated to long-term effects on cardiovascular disease risk. 20
Effects of diet and exercise, alone and in combination, are also supported by RCTs comparing effects of interventions on glycemic traits as intermediate endpoints of T2D. For example, a recent meta-analysis confirmed that interval training, resistance training, and aerobic training were all related to reduced fasting plasma glucose levels and HbA1C among participants in trials lasting at least 12 weeks duration, 21 providing evidence of the benefits of physical activity independently from other lifestyle changes. The PREvencion con DIeta MEDiterranean (PREDIMED) trial conducted a dietary intervention in a population not selected necessarily for having impaired glycemia, although they were enrolled for their high cardiovascular risk. Participants randomized to the Mediterranean dietary pattern had a 53% lower risk of incident T2D compared with the low-fat dietary pattern after 4 years, 22 suggesting an even greater benefit for dietary goals aiming to improve overall quality.
A substantial amount of evidence for the benefits of individual lifestyle factors and overall patterns for T2D prevention also comes from observational studies. Observational cohorts can benefit from long-term follow-up and therefore span a larger window of the etiologic time course even years before participants are considered at high T2D risk. In these studies, high quality epidemiologic evidence for individual dietary factors consistently implicates reductions in sugar sweetened beverages, 23 replacement of red and processed meat with nuts and other plant proteins, 24 and substitution of refined grains with whole grains and higher fiber 25 can meaningfully improve overall diet quality for long-term reduction in T2D risk. A recent meta-analysis of 30 prospective cohort studies comprising ∼1.7 million individuals reported that those sustaining a healthy diet, maintaining physical activity, having healthy body weight, not smoking, and with light alcohol intake, had incrementally lower risk of developing T2D, collectively preventing a striking 80% of cases. 26 However, confirming epidemiologic findings through RCTs of lifestyle interventions for T2D prevention in the general population are sparse owing to the sample size and follow-up duration needed. For example, the Women’s Health Initiative (WHI) Dietary Modification Trial randomized 48,835 postmenopausal women not selected for their baseline risk to follow a healthy low-fat pattern vs maintain their usual diet for 8.1 years. Among women without diabetes at baseline, the cumulative incidence of initiating T2D medication or insulin use was similar between the low-fat and usual diets (7.1% vs 7.4%, respectively) 27 ; however, when requiring insulin was analyzed alone, risk was 26% lower for the low-fat group. 28
There are important considerations for translation of lifestyle’s efficacy for T2D prevention from RCTs to population settings. Given the evidence from RCTs like the DPP conducted among motivated clinical trial populations, there have been numerous replication trials conducted globally. 29 In a meta-analysis across RCTs and non-randomized interventions, lifestyle programs of various content and intensities were collectively related to lower risks of developing T2D among eligible high-risk program participants, explained in large part by the degree of participants’ weight loss. 29 In a large national implementation of the UK Diabetes Prevention Program, T2D prevention was also predicted by participant retention in the program. 30 There are challenges in maintaining healthy lifestyles in the absence of continuous program availability and ongoing patient engagement, emphasizing the importance of addressing the societal and environmental barriers to long-term sustainability. 31
Lifestyle Strategies for T2D Treatment and Vascular Risk Reduction
Early treatment following T2D diagnosis is critical for the preservation of pancreatic islet β-cells and to reduce the risk of downstream micro- and macrovascular complications. The risk of T2D-related retinopathy, vision loss, and blindness is highest in patients with long-term poor glycemic control.32,33 Patients with T2D are at 2 to 4-fold higher risk of fatal and non-fatal cardiovascular disease compared with adults without T2D, 34 and risk of these outcomes is incrementally worse with higher fasting plasma glucose levels (e.g., ≥7 mmol/L). Even among T2D patients without additional cardiometabolic risk factors such as obesity, a history of smoking, and elevated blood pressure, coronary events occur ∼2 times more frequently than in those without T2D.33,35 As such, the World Health Organization (WHO) 36 and US Centers for Disease Control (CDC) guidelines for clinical treatment of T2D center around long-term management of glycemic control, specifically targeting lower fasting blood glucose and Hba1c levels, for the prevention of retinopathy, microalbuminuria, and other vascular complications. 37 However, despite its established importance, optimal HbA1c targets for long-term reduction in cardiovascular outcomes and mortality remain controversial. 38 A 2022 updated consensus report from the ADA and the EASD proposes tailoring glycemic treatment goals based on age, presence of other comorbidities, and risk of hypoglycemia, with a general guidance for maintaining HbA1c ≤ 7%. 39
Recommended therapies for maintaining glycemic control after diagnosis of T2D include lifestyle interventions to reduce body weight, improve diet quality, and increase physical activity, with the consideration for glucose-lowering medications (e.g., metformin, sulfonylureas, glucagon-like peptide 1 [GLP-1] agonists, sodium-glucose co-transporters type 2 [SGLT-2] inhibitors) and insulin when warranted. 40 Numerous RCTs demonstrate the efficacy of these approaches, independently or in combination, for glycemic control, in turn lowering risk of microvascular complications. Meaningful reductions in fasting blood glucose levels and Hba1c can be achieved with a variety of overall dietary patterns that emphasize diet quality, such as Mediterranean and health vegetarian patterns.41,42 The evidence for the effectiveness of macronutrient-focused diets is less consistent, particularly due to few RCTs with follow-up beyond 6 and 12 months.42,43 Improved glycemic control with low-carbohydrate diets is comparable to comparator diets when matched for intervention intensity and engagement, and the benefits are comparable to low-fat and low glycemic index/glycemic load diets.41,44 Collectively, the body of evidence from short-term RCTs underscores that restriction of carbohydrate or fat can be integrated into a healthy dietary pattern, but that the macronutrient composition alone is not uniquely beneficial for glycemic control in T2D. For example, in a head-to-head comparison of randomization to very low carbohydrate vs low-fat high-carbohydrate diets for 1 year, both diets conferred an average 9.1% weight loss with significant reductions in HbA1c of 1.0% for both and fasting glucose of −1.3 mmol/L and −1.5 mmol/L for low-carb and low-fat, respectively. 45 In contrast, evidence for high protein diets does not indicate there is a consistent reduction in HbA1c or fasting glucose levels but they have been shown to modestly improve insulin resistance. 41
Most interventions evaluating efficacy of lifestyle interventions among T2D patients have relied on evaluating short-term changes in intermediate glycemic traits and other biomarkers as surrogate endpoints of long-term T2D complications, morbidity, and mortality. However, RCTs of glucose-lowering medications have not consistently supported the hypothesis that more intensive glycemic control (e.g., HbA1c <7.0%) confers even greater reductions in morbidity and mortality and highlight safety concerns due to an increased risk of hypoglycemia. 46 For example, the Veterans Affairs Diabetes Trial (VADT) achieved significant reductions in Hba1c with intensive glycemic control goals vs standard care (HbA1c at 5.6 years follow-up: 6.9% vs 8.4%, respectively), and yet observed no difference between groups in microvascular complications, incident cardiovascular disease events, or all-cause mortality. 47 Additionally, the Action in Diabetes and Vascular Disease: Preterax and Diamicron Modified Release Controlled Evaluation (ADVANCE) RCT sustained an HbA1c of 6.5% with intensive therapy vs 7.3% with standard therapy after 5 years, and intensive therapy prevented increases in albuminuria and nephropathy, but had no effect on ophthalmologic complications, neuropathy, or CVD incidence and mortality.48,49 Thus, although poorly controlled blood glucose levels reflect underlying pathology of T2D, the use of medications to intensively target their reduction appears to mitigate some, but not all, vascular complications.
The broad-spectrum effects of diet and physical activity in patients with T2D may reduce vascular complications and cardiovascular disease benefits through mechanisms other than glycemic control, including weight management, blood pressure reduction, and improved dyslipidemia.50-52 However, evidence from longer-term RCTs of clinical outcomes to support this is sparse. Among the largest and longest term studies to date, the Look Action for Health for Diabetes (Look AHEAD) was a US-based RCT in adults with a mean baseline BMI of 35.8 kg/m2 and within a median 5 years from T2D diagnosis to test a lifestyle weight loss intervention on glycemic control as well as the prevention of cardiovascular complications. 53 The 4-year behavioral and social support program emphasized a calorie-restricted low-fat diet, physical activity, and fitness goals, which facilitated sustained mean percent body weight loss of −4.7% and HbA1c reduction of 0.36% at year 4. The lifestyle intervention group was significantly less likely to initiate the use of diabetes medications (42% vs 67%, respectively) or insulin (7% vs 12%) than the control group. 54 For cardiovascular risk factors, lifestyle significantly improved blood pressure, fitness levels, and triglycerides, but not LDL-cholesterol, and these effects waned over follow-up. Ultimately, despite effects on intermediate risk factors, there was no effect of lifestyle cardiovascular disease events and deaths at the 9.6 years median follow-up vs control group.55,56 Although the trial researchers attribute this lack of effect to innate risk within the sample, the fact that weight regain was greatest after 5 years of intervention, coinciding with the greatest number of remission cases, could offer an explanation of the lack of effect. Interventions may need to support sustained lifestyle modifications for at least a decade to adequately capture the long-term effects of intensive lifestyle improvements on cardiovascular outcomes. However, RCTs are unlikely to be conducted and replicated with external validation studied across various settings and populations, highlighting the limitations of relying on RCT evidence and the need to support of rigorous epidemiological research and post-trial surveillance to determine long-term efficacy and safety.
Sustainability and Scalability of Lifestyle Modifications
Long-term adherence to a variety of multifactorial healthy lifestyle patterns prevents ∼80% of T2D, as indicated by numerous observational cohort studies with decades of follow-up. Rigorously conducted RCTs have contributed to further defining the benefits of improving diet quality and increasing physical activity levels with weight loss and have elucidated the plausible biological mechanisms through not only improved glycemic control, but also improvements to body weight and composition, fitness, blood pressure, and dyslipidemia. However, corroboration of benefits for long-term outcomes in general populations and for major T2D-related morbidity and mortality after T2D onset and diagnosis has proven difficult. This is in part due to the difficulties in sustaining lifestyle changes over the long-term even among motivated clinical trial participants.19,55 Thus, pragmatic research to address and overcome implementation challenges in the scalability and sustainability of lifestyle challenges is critically needed.
One option to improve the sustainability of major lifestyle changes is to innovate cost-effective interventions that individuals can affordably interact with long-term. Such advances could address declines in adherence and engagement following the tapering or cessation of more intensive programs, such as the 12-month-long US Diabetes Prevention Program and similar programs worldwide for patients with prediabetes or T2D. Cost-effective health care system infrastructure has already been developed, tested, and scaled for patient monitoring of medication efficacy and compliance in various settings.57,58 A second objective for implementation research is to consider implementing lifestyle interventions through modalities or platforms that are more broadly accessible or tailored to individuals’ preferences. Having a variety of effective options for lifestyle program delivery can serve to increase participant enrollment, engagement, and retention, 59 and can be adapted across socioeconomic and geographic settings, cultural audiences, and personal preferences. 60 Third, it may be possible to further improve the standard of care for patient lifestyle recommendations by re-tooling specific aspects of the diet and physical activity guidance for even greater efficacy and durability. For example, many of the early landmark T2D prevention and treatment trials featured low-fat diets, which in subsequent decades have been shown in some cases to be inferior for glycemic control and cardiometabolic health, when compared with overall diet quality patterns such as the Mediterranean or healthy plant-based eating patterns.22,41 Insertion of lifestyle programs for T2D prevention and treatment in local and national health care systems and increasing the awareness and importance of these programs by health professionals to increase program referral has translated into improved cost-effectiveness in some settings. 61 Alternatively, personalized and precision medicine approaches have the potential to eventually optimize diet and physical activity recommendations to the individual to inform the most effective, safe, and sustainable combination of therapies.62,63
Finally, it is important to acknowledge that the available approaches for T2D prevention and treatment rely heavily on individual behavior change at all stages, from the initial enrollment into a lifestyle program to initiate change, to the long-term engagement and maintenance. Therefore, although effective diet and physical activity interventions may be innovated to improve their sustainability and scalability, even modest population-level approaches may be just as impactful at addressing the T2D epidemic given its massive scale. 31 There are many levels of intensity for population-level lifestyle changes that have been reviewed in detail,64,65 including taxation, subsidization, and other policies to improve the availability and affordability of healthier foods and physical activity to promote these to being the opt-out default, instead of a burden. However, individual-level behavioral interventions and options are not mutually exclusive, and both should be prioritized.
Lifestyle in the Era of Effective T2D and Weight Loss Medicines
In recent years, additional classes of diabetes medications have emerged to prevent and treat diabetes, including the sodium-glucose cotransporter 2 (SGLT2) inhibitors and the glucagon-like peptide 1 (GLP-1) agonists. Moreover, these medications have been shown to result not only in improved glycemic control but also in short-term benefits to other cardiometabolic risk factors. SGLT2 inhibitors lead to significant weight loss in patients with overweight and obesity and reduce biomarkers of chronic inflammation. Moreover, they also promote ketone metabolism to replace glucose as the main source of energy and improve systemic blood pressure and arterial stiffness. 66 GLP-1 agonists promote insulin secretion and overall postprandial glucose metabolism, but these also regulate satiety which results in weight loss and reducing overnutrition. 67 The approval of these treatments in T2D provides an opportunity to promote broader cardiometabolic health. Used in isolation GLP-1 agonists reduce major adverse cardiovascular events by 14%, and heart failure by at least 12%. However, a recent trial reported that the combination of GLP-1 agonists plus a lifestyle intervention promoted weight loss as well as improvements to glycemic markers, and these were significantly better than groups receiving either the lifestyle or medication alone. 68 Indeed, even in the setting of effective T2D and weight loss medications, concomitant lifestyle interventions remain highly relevant and provide additional broad-spectrum benefits.
Summary & Conclusions
The causes and underlying pathology of T2D are complex and multifactorial, and comprehensive changes in lifestyle have pleiotropic benefits on multiple risk factors, underscoring their role in standard of care for high-risk patients. Randomized controlled trials of intensive lifestyle programs incorporating a variety of healthy dietary patterns than emphasize overall quality, physical activity recommendations, and weight loss, can delay T2D onset in patients at elevated risk and improve glycemic control in clinical populations with T2D. Epidemiologic evidence indicates that the benefits of T2D prevention with sustaining healthy lifestyle patterns long-term are generalizable to the broader population. Long-term observational studies among patients with T2D indicates that in addition to its effects on improved glycemic control, modifying diet and physical activity is also related to lower risks of cardiovascular morbidity and mortality.
However, the persistent prevalence of T2D and its cardiometabolic consequences highlight significant shortcomings in the translation of effective lifestyle interventions at the population level. Further, clinical and public health recommendations that target modifying individuals’ behaviors are often undermined by an environment that promotes poor diet quality and a sedentary lifestyle and other socioeconomic obstacles to sustaining a healthy lifestyle. Therefore, prioritizing implementation research to innovate accessible, effective, and affordable strategies, with parallel efforts from public health stakeholders to improve the healthfulness of the broader food and built environment, are needed to maximize the effectiveness of lifestyle interventions for T2D prevention and treatment.
Footnotes
Acknowledgments
Dr Tobias is PI of research funded by the American Diabetes Association and the NIH/NIDDK for research related to diet and T2D prevention. Dr Pano is supported by a research project funded by the American Diabetes Association. Dr Manson has no relevant conflicts of interest.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article. DT and JM report research outside of this manuscript related to type 2 diabetes funded by the NIH (DT, JM) and the American Diabetes Association (DT).
