Abstract
This study aimed to assess the relationship between mental health, health behaviors, and food security in young adults in a university environment. Young adults (N = 536) at two United States universities completed a survey assessing health behaviors and characteristics. Logistic regression determined the odds of anxiety and/or depression based on gender identity, body mass index (BMI), food security status (FSS), and sleep restfulness. Over one-third of students were food insecure (36.7%), and almost all reported anxiety (57%) and/or depression (39.1%). Students who identified as female, reported very low FSS, poor sleep, and had higher BMI were at greater odds for the prevalence of depression. Students with poor sleep and low FSS were more likely to report mental health challenges. Universities should focus on priorities and interventions among at-risk students.
“Higher odds of anxiety and depression were found with those who identify as female vs male, reported higher rates of lack of sleep or rest, and very low food security.”
Introduction
Throughout the transitional period from a childhood home to emerging adulthood, approximately 62% of young adults enter college.1,2 As a result of immense change and the potential for new-found independence, these young adults entering college are responsible for their health, well-being, finances, educational engagement, and social activities. University living, particularly four-year institutions with a campus living environment, can bring a variety of pressures through the management of academics and lifestyles. 3 These competing interests can impact an individual’s performance toward their career path and thoughtful engagement with academic content. As such, this vulnerable development period in young adulthood can help improve knowledge of and instill healthful behaviors across the lifespan.
Due to emotional support changes and increased opportunities while in a campus environment, self-regulation of emotions can be difficult.4,5 The mental health status of college students is among the lowest compared to other age groups, with 33.7% of 18-25-year-olds reporting experiencing Any Mental Illness in 2021 compared to 28.1% among 26-49-year-olds and 15.0% among adults aged 50+. 6 Further, throughout the COVID-19 pandemic, mental health challenges significantly increased within college populations, with reported impacts on lifestyle, academics, and health.7,8 Several studies indicate the need to continue understanding the lasting mental health impacts of the pandemic on students returning to the classroom and early detection of mental health challenges among at-risk students.7-9 Recent research has shown several risk factors for mental health challenges among college student populations, including, but not limited to, female sex, sleep disturbances, low or high meal intake, stressful academic environments, and self-perceived health. 10 Unfortunately, those with clinical symptoms of anxiety and/or depression also tend to use unhealthy coping strategies. 11
Coping strategies to deal with negative mental health can include excessive social media use, insufficient or excess sleep, and fast food/sweets consumption.11,12 Additionally, some students may turn to substance use (e.g., alcohol, drugs) or engage in other risky behaviors as a means of coping with stress and mental health challenges. 13 Unhealthier coping mechanisms have the potential to consequently lead to unwanted weight gain, elevated body mass index (BMI), and an increased risk of chronic diseases. 14 Adequate sleep (e.g., 7.5-8.5 hours per night) is associated with a decreased risk of anxiety and depression among young adults. Yet in a sample by Dickinson and colleagues, the average sleep duration in a college population was 6.67 hours. 15 Likewise, irregular sleep durations in college students have additionally been associated with higher weight status. 16 Obesity (e.g., a BMI greater than 30) is coincidentally associated with poorer mental health due to multiple factors, including negative body image, bullying, and weight-biases. 17 Unfortunately, the college food environment exacerbates poor eating behaviors due to student time constraints, limited options, and limited student budget. As a way to budget funds for other expenses, university students may seek cheaper processed items through free or low-cost avenues such as fast-food, food pantries, or campus giveaways.18-20 Further, students may face additional barriers to preparing nutritious meals due to limited cooking skills or a lack of kitchen access, both of which can impact dietary quality and food security. 21 Alternatively, some students report incidents of food insecurity in an attempt to budget funds to pay rent, bills, and academic-related expenses.18,19
Food insecurity adds to the mental burden of United States college students. 22 A lack of financial resources has consequently led to 30-50% of young adult college students screening as food insecure. 23 Increased risk of food insecurity has also been associated with those who lack financial support from family and also suggests they may have come from a family with a history of food insecurity (e.g., free and reduced lunch; reported childhood food insecurity). 24 Studies reveal that if basic needs, such as food and housing, are met, then college students are likely to have higher grade point averages and be successful in attaining a degree. 25 Likewise, an inverse relationship has been identified among food security status and health outcomes. 26 In addition to poor focus and academic performance amid limited access to adequate and nutritious foods, food insecurity is associated with poor dietary quality and, consequently, correlated with overweight, obesity, and chronic diseases.27-29
With a myriad of stressors occurring in a young adult’s life during college, research is warranted to understand the intersections between food security, lifestyle well-being, and mental health. Protective factors, such as adequate sleep and maintaining a healthy weight, can decrease the severity of mental health disorders across the lifespan and throughout life experiences (e.g., occupation, athletic performance, pregnancy).15,30,31 Therefore, considering what are known influencers of mental health and the current state of mental health disorders among emerging adults and nationwide, the current study aimed to contribute to the existing body of literature on the topic. This formative study examines the current landscape relationships between mental health and/or higher body weight, sleep restfulness, and food security among young adults at two United States 4-year university institutions. It was hypothesized that those with a higher BMI, poor sleep and/or unrestful sleep, and food insecurity would have greater odds of reporting the prevalence of depression and anxiety in a college student population.
Methods
The study was conducted at two land-grant universities in the United States. The study was designed and implemented in accordance with the Declaration of Helenski, and the protocol received expedited review and approval at both universities’ Institutional Review Boards; University of Kentucky Institutional Review Board (#61400; 5/18/2021) and the University of Maine (2020-07-14).
The current study was a sub-project from a larger, overarching program that utilized community-based participatory research (CBPR) approaches to partner with students in the community to identify health-related issues on campus. 32 In collaboration with the students, a survey was developed to identify the needs of their peers on each college campus.
Study participants were college students at the two participating universities and were recruited for an online cross-sectional health survey via college-wide informational announcements and emails. Total university enrollment of the two universities were 32,710 in Kentucky and 8,021 in Maine. Students were sent the survey link invitation in January 2023 to complete baseline data collection after completing informed consent into the study. Inclusion criteria to participate included being between the ages of 18-26 years, currently enrolled as an undergraduate student at one of the two participating universities, and able to read and understand the English language. Following the survey, participants were entered into a raffle to win one of ten $50 Amazon gift cards as an incentive for their time.
Survey items included demographics (age, race and ethnicity, gender identity, sexual identity, year in school), self-reported anthropometrics, and lifestyle and behavioral based surveys. BMI was calculated from self-reported height and weight, which has been used as a valid measure of weight status for young adults. 33 Chronic disease was measured by a single self-reported item asking individuals to report if a health professional has ever diagnosed them with a series of 15 options of conditions (e.g., depression, anxiety, obesity, type 2 diabetes). For the current sub-study, mental health challenges were the only focus of chronic conditions due to interest of our student community partners. Food security status (FSS) was assessed using the 10-item USDA Household Food Security Screener. 34 Scores were calculated for each of the 10 items and summed for a total score. FSS of 0 were classified as high food security, scores 1-2 classified as marginal food security, scores 3-5 classified as low food security, and scores of 6-10 as very low food security. Finally, sleep behaviors were assessed through the Center for Disease Control’s Healthy Days Module. 35 The single item from the CDC’s Module for sleep included “for the past 30 days, about how many days have you felt you did not get enough rest or sleep?”
Continuous variables were analyzed for measures of central tendencies and categorical variables were assessed using frequencies. Demographic and behavioral characteristics are reported separately for those who reported “yes” or “no” for anxiety and those who reported “yes” or “no” for depression. Independent t-tests were used to assess differences between groups for gender, BMI, sleep, and food security.
Three logistic regressions determined if college students were more likely to report prevalence of anxiety, depression, and anxiety and depression (“yes” or “no”) based on demographic characteristics and behaviors (e.g., sleep, food insecurity, BMI, and gender identity (male or female)). For gender, only individuals who identified as female or male were included in the logistic regression models to control for small sample sizes of gender minority groups. For categorical variables, male and high food security were set as the referent values. Both models excluded participants with missing data for any of the variables. The X2 was evaluated to determine overall model significance, effect size was reported as an average of the R2 results provided by Cox & Snell R2 and Nagelkerke R2 values. 36 Effect size results were interpreted following Cohen’s guidelines for small (0.02), medium (.13), and large (.26) effect sizes. 37 Micro-level indices were examined to determine which variables were most strongly linked with the outcome. It was predicted that college students who identify as female, have higher BMIs, report less restful sleep, and higher food insecurity would be more likely to report prevalence of anxiety or depression. Significance was set at P < 0.05.
Results
Characteristics of the Sample Stratified by Prevalence of Anxiety and Depression (“Yes” or “No”) (N = 536).
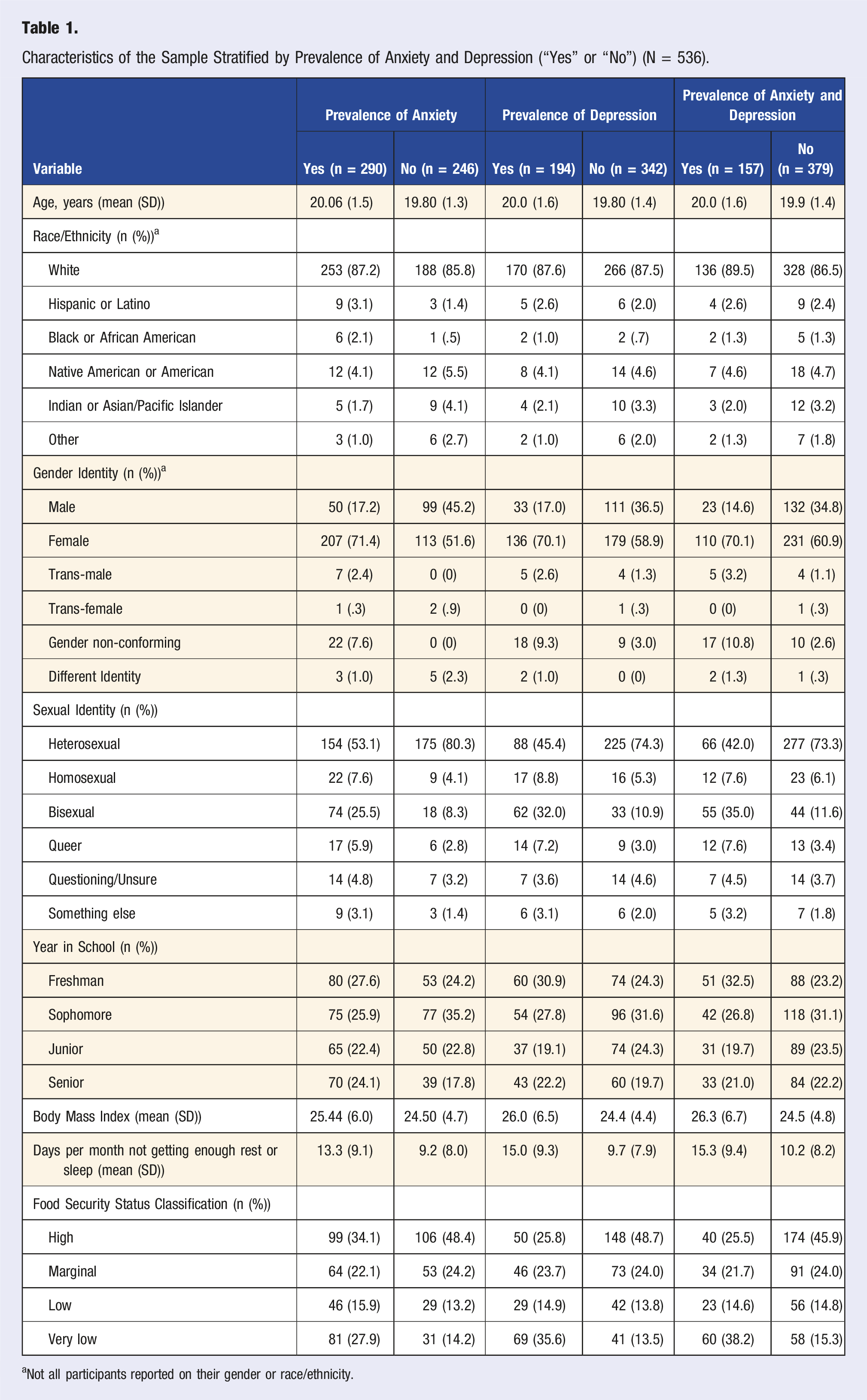
aNot all participants reported on their gender or race/ethnicity.
Predicting Prevalence of Anxiety in College Students (n = 483).
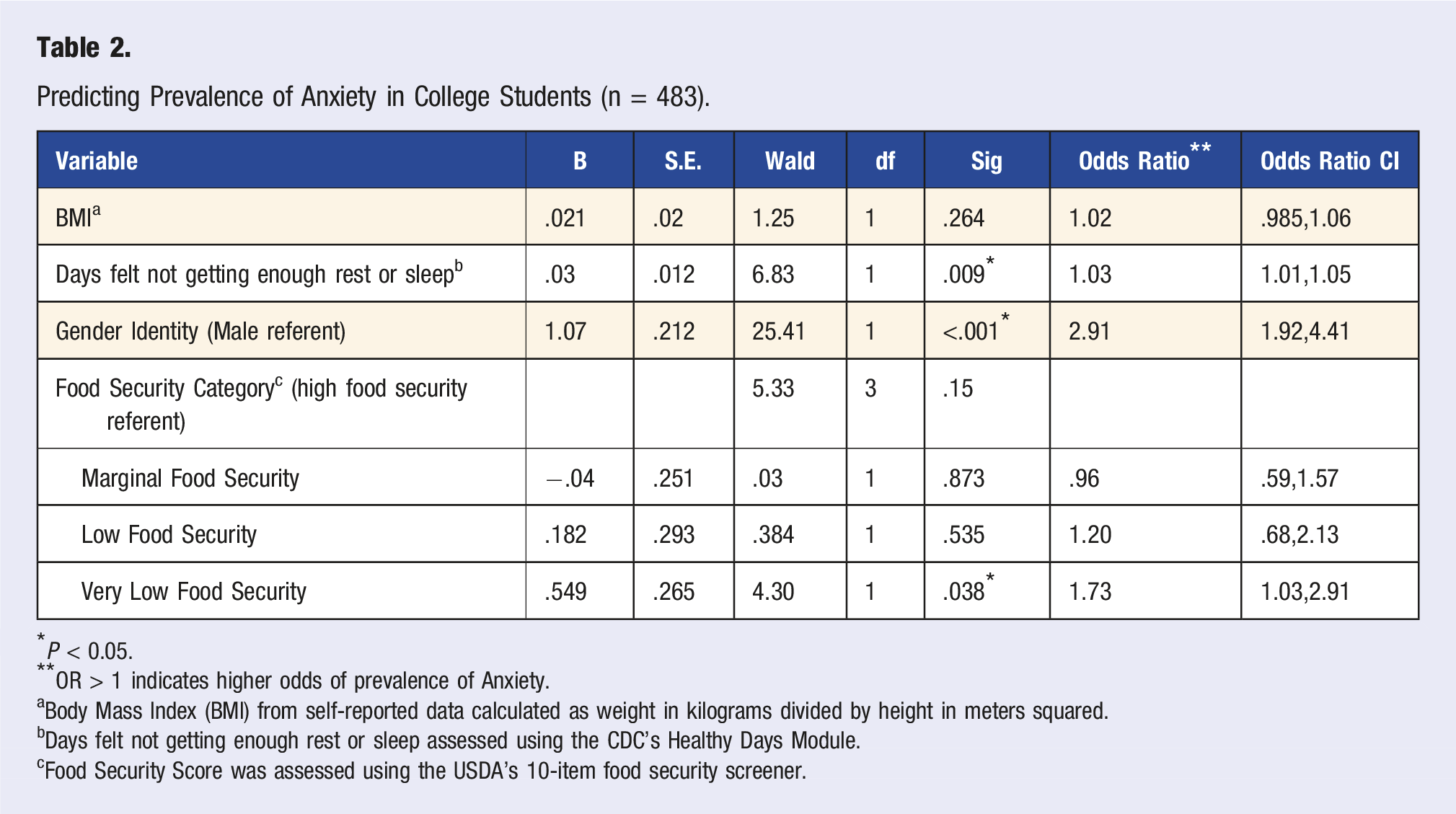
*P < 0.05.
**OR > 1 indicates higher odds of prevalence of Anxiety.
aBody Mass Index (BMI) from self-reported data calculated as weight in kilograms divided by height in meters squared.
bDays felt not getting enough rest or sleep assessed using the CDC’s Healthy Days Module.
cFood Security Score was assessed using the USDA’s 10-item food security screener.
Predicting Prevalence of Depression in College Students (n = 448).
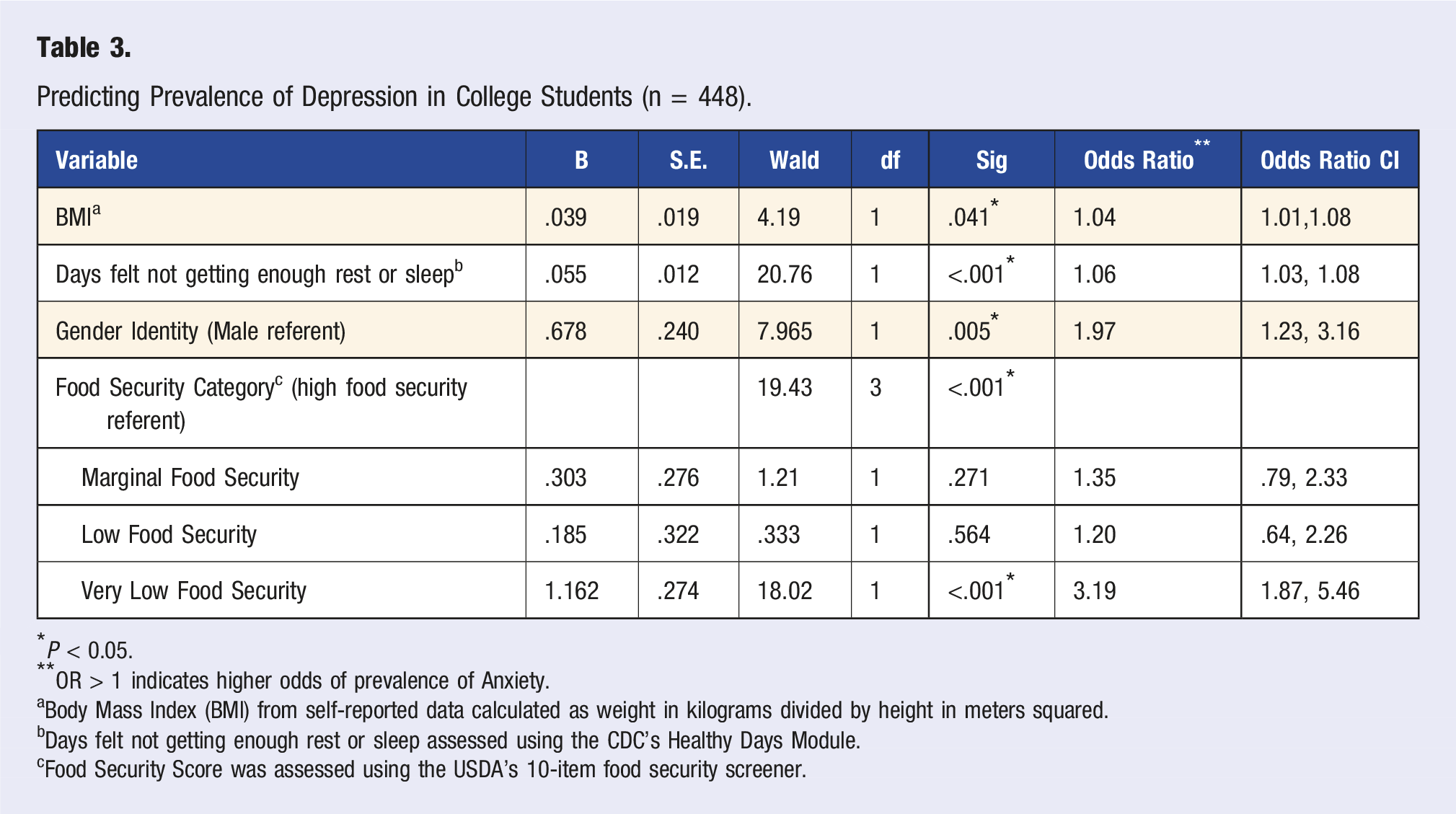
*P < 0.05.
**OR > 1 indicates higher odds of prevalence of Anxiety.
aBody Mass Index (BMI) from self-reported data calculated as weight in kilograms divided by height in meters squared.
bDays felt not getting enough rest or sleep assessed using the CDC’s Healthy Days Module.
cFood Security Score was assessed using the USDA’s 10-item food security screener.
Predicting Prevalence of Depression and Anxiety in College Students (n = 448).
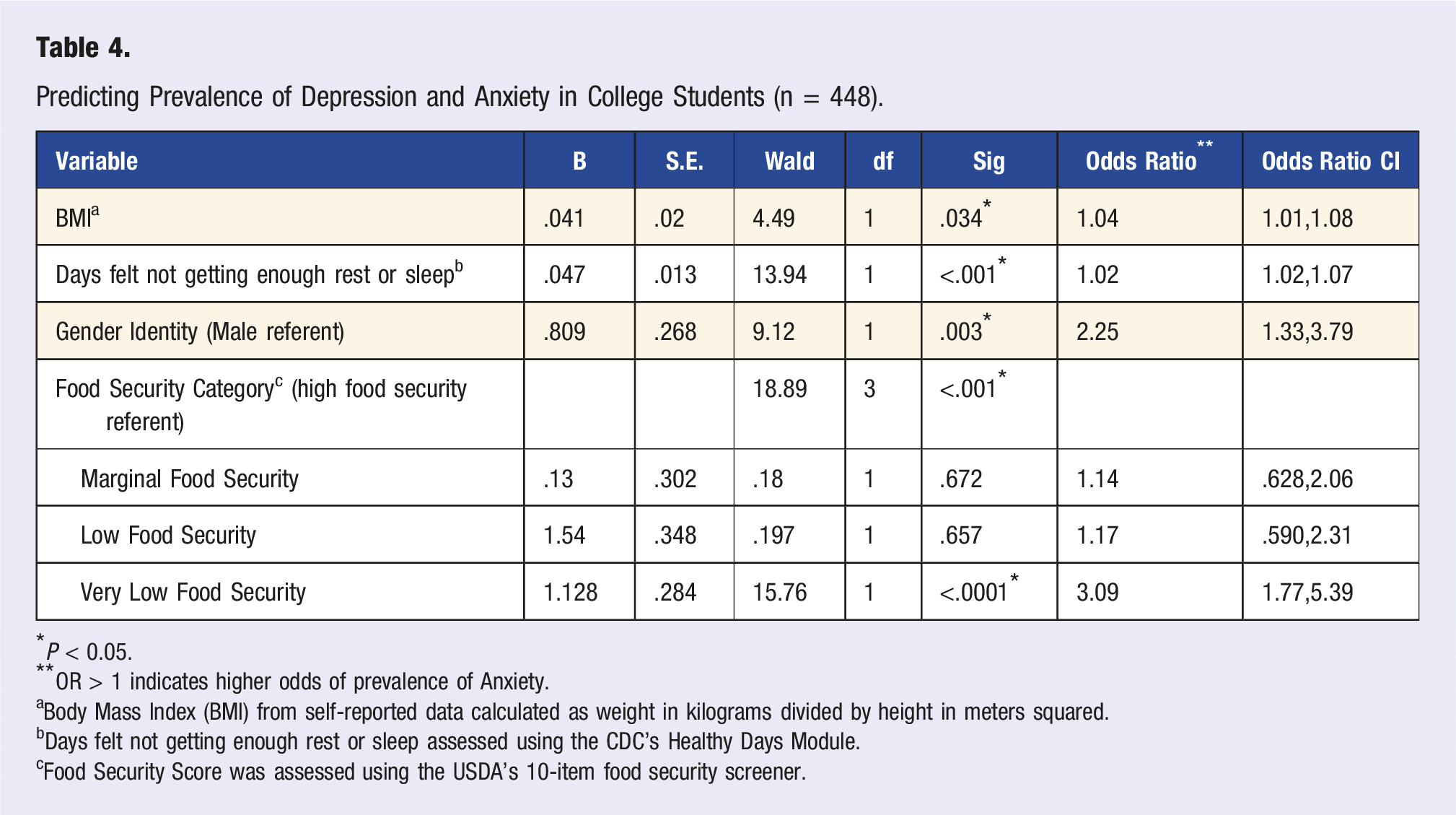
*P < 0.05.
**OR > 1 indicates higher odds of prevalence of Anxiety.
aBody Mass Index (BMI) from self-reported data calculated as weight in kilograms divided by height in meters squared.
bDays felt not getting enough rest or sleep assessed using the CDC’s Healthy Days Module.
cFood Security Score was assessed using the USDA’s 10-item food security screener.
Discussion
The current study aimed to add to the literature a formative exploration of mental health and food insecurity among young adults. Overall, this study reveals mental health disorders remain high in college students with modifiable (e.g., sleep, BMI, FSS) and nonmodifiable (e.g., gender) risk factors that should be considered when developing programming to improve mental health in this vulnerable population. Higher odds of anxiety and depression were found with those who identify as female vs male, reported higher rates of lack of sleep or rest, and very low food security. Likewise, though not associated with anxiety, a higher BMI was associated with higher odds of depression.
While this study identifies significant associations, it is essential to acknowledge that the relationship between anxiety, depression, BMI, sleep, and food insecurity are likely bidirectional. Anxiety and depression may exacerbate poor sleep, increased BMI, and food insecurity, while these factors may also act as predictors for mental health conditions, such as anxiety and depression. In addition to bidirectionality, it is critical to explore underlying reasons for key variables such as lack of sleep. Students may experience sleep disturbances for a multitude of reasons in addition to poor mental health, including employment, academic pressure, and social activities. These nuances, which were not captured in the study, could inform targeted interventions addressing sleep.
The connection between mental health, sleep, and FSS was showcased by Nagata and colleagues 38 in 2008, revealing that a sample of approximately 15,000 young adults screened as food insecure also reported poor sleep habits and mental health challenges. 38 With approximately 15 years between Nagata and colleagues’ study and the current one, it is alarming to note that the prevalence of poor mental health, sleep, and food insecurity are not improving among young adults. Corroborating our results, Becker and colleagues also found that in a large sample of over 7,000 college students, poor sleep was a predictor of anxiety and depression and students who identified as female reported the worst sleep and mental health. 39 However, it is crucial to emphasize that poor sleep may serve as both a predictor and consequence of anxiety and depression, further underscoring the bidirectional nature of these relationships. Addressing one component may have cascading effects on others, highlighting the need for policy change, student support interventions, and bolstering of resources on college campuses to attenuate and improve these prominent issues on college campuses.
Further, new financial responsibilities and lifestyle management stressors within the college environment contribute to food insecurity and mental health challenges in college students.18,28,29 Of our 536 students, 36.7% screened as food insecure, coinciding with the average rates for college food insecurity (between 30-50%). 23 Whether food insecurity takes place across all four years of college or a few months, health behaviors, and academic performance can be irreversibly impacted and lead to continued poor behaviors long-term. 26 Both anxiety and depression have been historically linked to food insecurity rates. In our study, over 50% of the cohort reported anxiety and 37% reported depression, as diagnosed by a health professional. These findings have been reflected in other studies focused on young adult mental health.39,40 As reported in the current study, very low food insecurity almost doubled students’ odds of reporting anxiety and/or depression. While other studies have focused on documenting prevalence of food insecurity and mental health separately in this population, our results showcase the strong connection between the two issues. 41
Efforts should be made to improve student health-related quality of life and basic needs. Setting young adults up for success when they enter college can help improve the education they earn and provide them with healthy habits as they become the next generation of the workforce. A recent Society for Nutrition Education and Behavior position paper also indicates the lack of literature surrounding the implications of food insecurity on educational and career attainment following university. 23 It has been documented that academic attainment and knowledge are associated with positive health outcomes and key social determinants of health. 23 Health of the student body largely relies on resources, policies, and access throughout the campus environment and student’s social networks.42,43
Our current study aimed to update the literature on the state of mental health and food insecurity among college students. The population was recruited from two land-grant institutions in the United States and has the potential to serve as an updated time point for continued investigation. We were also able to equally recruit a sample from each grade level, which serves as a strong representation of students throughout the universities. However, we are not without limitations. The data was taken from a singular cross-sectional examination at the beginning of a new academic semester. Timing for research in academic settings can be difficult to manage since stress, finances, educational requirements, and social events can fluctuate. The financial status of college students varies throughout different time points in a semester (e.g., beginning, end, holiday breaks, tax season). Therefore, when investigating the food security status of college students, data collection and intervention dosage should be adjusted to reflect these time points. 44 Likewise, programming intended to improve food security and encourage healthy lifestyle changes could benefit from prioritizing money management. This focus would ensure students budget their finances effectively throughout the semester, accommodating fluctuations in income.18,19
Additionally, regarding recruitment efforts, the sample self-selected to participate in the study, which was advertised as being health-related. Wording of the program could have influenced student participation based on interest in health programming. Our sample was also predominantly white, female, and heterosexual individuals leaving out gender and sexual minority college students who may face even worse mental health and food insecurity rates. 45 Voluntary research in college settings often attracts a homogenous demographic. Future studies should prioritize purposeful sampling to ensure a more diverse participant group. Finally, care should be taken when developing surveys to analyze particular behaviors and conditions. Survey items utilized for sleep and mental health diagnoses in the study were single item, self-reported measures. However, these items have been used in similar studies to capture a broad picture of sleep and mental health status in various populations.45,46
Implication for Research and Practice
The current works aim to update the college student health data and bring a call for effective preventative programming. As universities continue to operate through the enrollment of students and employers continue to stay in business with a healthy workforce, the health and well-being of young adults is an imperative area of focus. Evidence-based lifestyle interventions in this young adult population are warranted as health and chronic disease rates of adults are far from lowering.
In our cohort at two land-grant institutions in the United States, rates of mental health challenges, food insecurity, and poor sleep behaviors were elevated. There is a critical need for interventions that provide education, support, and resources for engaging in healthy lifestyle behaviors, accessing adequate healthy food, and supporting heightened mental health crises. Future works should consider developing and implementing lifestyle-based interventions, such as hands-on, in-person, or support-based diet and mental health approaches. Though there have been programs implemented for these areas separately, particularly in down-stream mechanisms (e.g., emergency food programs, mental health therapy as a treatment), there is a void in the literature when targeting the nexus of health behaviors and challenges in an up-stream, or preventative manner (e.g., increase knowledge, financial literacy).
In university environments where young adults spend their formative years, developing and sustaining evidence-based interventions targeting interconnected challenges such as mental health, sleep, BMI, and food insecurity is essential. Future research should prioritize low-burden interventions for at-risk students supported by university financial and staffing resources. A holistic approach addressing these factors simultaneously is critical, given their bidirectional relationships. Additionally, longitudinal studies can provide valuable insights by documenting pre-existing conditions and changes over time. Qualitative methods could further enhance understanding of contextual factors, such as employment, social or academic demands, and poor mental health, which influence variables such as sleep and food insecurity. This deeper understanding can guide the development of more tailored and impactful interventions.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by University of Kentucky Department of Dietetics and Human Nutrition and USDA NIFA AFRI SEED (grant no. 2021-68015-33432).
