Abstract
Purpose: Physical activity and sedentary behavior have significant prognostic importance in survivors of breast cancer. However, not much is known about physical activity and sedentary behavior in the midwestern United States for patients who have breast cancer. This study provides patient-reported physical activity and sedentary behavior from a cohort of patients from the midwestern United States. Methods: A survey assessed physical activity and sedentary behavior from patients with all types of local or invasive breast cancer and ductal carcinoma in situ (DCIS). Demographic information and characteristics of participants’ breast cancer, including time since diagnosis, type of cancer, and remission status were gathered. Results: Data from 108 patients reveal diverse physical activity and sedentary behavior patterns. Seventeen individuals (15.9%) report not engaging in any form of physical activity and only 15.9% report meeting national guideline recommendations of greater than 150 minutes of moderate intensity-equivalent physical activity per week. A wide range of physical activity in minutes was reported across age, time since diagnosis, type of cancer and remission status, none of which was statistically significant. Participants report sitting or reclining an average of 6.1 hours (SD = 3.9) per day during a typical workday and 5.8 hours (SD = 3.8) on a typical non-workday. Conclusions: Our study provides information about physical activity and sedentary behavior in a cohort of midwestern patients with breast cancer and indicates that the majority of the patients could be at high risk for long-term adverse prognosis. Tailored lifestyle programs to enhance physical activity and decrease sedentary behavior are critical to improve outcomes. Our results indicate that clinicians should incorporate healthy lifestyle medicine recommendations for all patients living with breast cancer at any age or time since diagnosis, independent of cancer type or remission status.
“Physical activity and sedentary behavior in patients who have been diagnosed with cancer can have key effects on overall outcomes.”
Background and Introduction
With advancements in breast cancer diagnoses and treatment, more women are surviving breast cancer. Currently, there are over 3.1 million breast cancer survivors in the United States, the largest among all cancer survivor groups.1,2 This group has been a focal point for research aiming to identify the lifestyle choices that ensure the highest quality of life while reducing cancer-specific and all-cause mortality.1,3,4 Lifestyle changes involving physical activity have a well-known impact on improving the quality of life of patients with cancer.5-7 Physical activity reduces the risk of breast cancer recurrence and mortality, cancer-related fatigue, and depressive symptoms. Moreover, physical activity can minimize treatment-related side effects and the risk of developing chronic disease.8-10 The biological benefits of physical activity include improved energy utilization, angiogenesis, neurogenesis, enhanced endothelial and immune function, increased skeletal muscle mass and mitochondria, and modulation of inflammation. 11
There are various national guidelines for physical activity from organizations such as the American College of Lifestyle Medicine, 12 Exercise is Medicine Moving Through Cancer Initiative, 13 the American College of Sports Medicine,14,15 the World Cancer Research Fund/American Institute for Cancer Research, 16 the American Cancer Society 17 and the U.S. Department of Health and Human Services. 18 These guidelines are generally similar with minor variations and emphasize that individuals, including patients living with cancer or in remission from cancer, should be as physically active as their abilities and conditions allow, with an explicit recommendation to avoid inactivity as any physical activity is better than none. The key aerobic activity guidelines suggest 150 minutes of moderate-intensity activity, 75 minutes of vigorous-intensity activity, or an equivalent combination of both, per week.8,19
Conversely, the lack of regular and vigorous physical activity in industrialized populations today is known to be a major risk factor for cardiometabolic disease (i.e., unhealthy weight gain, heart disease, and diabetes) and decreased longevity.19,20 Reducing levels of sedentary behavior can improve cancer outcomes. 21 The increase in occupational sedentary behavior and leisure inactivity can reduce lipoprotein lipase activity, muscle glucose, and protein transporter activities and impairs lipid metabolism while simultaneously diminishing carbohydrate metabolism, ultimately impacting insulin sensitivity and vascular function, increasing the risk of hormone-related cancer. 22 Emerging data also indicates that sitting time can have independent adverse impacts on oncology and cardiovascular outcomes independent of whether the person is meeting minimal physical activity guidelines. As a result, the World Health Organization released updated guidelines in 2020 that combine physical activity and sedentary behavior. However, there are no specific U.S. guidelines for sedentary behavior besides general recommendations to reduce sitting time and that “adults should aim to do more than the recommended levels of moderate-to-vigorous physical activity.” 23
Despite the well-recognized benefits of increasing physical activity and decreasing sedentary behavior, observational studies reveal that the majority of patients with cancer do not meet current physical activity guidelines and are mostly sedentary.4,24 Moreover, longitudinal studies demonstrate a decline in physical activity levels as time since diagnosis increases, with notable reductions observed over extended follow-up periods.25,26 There are few studies of patient-reported physical activity that have been conducted in a clinical setting. Many have limitations such as not including sedentary behavior or patients across all types or stages of breast cancer. Many only included patients in approximately the first 5 years since diagnosis. A 2014 systematic review and meta-analysis of population-based studies investigating the association between physical activity and mortality among breast and colorectal cancer survivors did not include studies from the clinical setting, nor did it investigate sedentary behavior. 27 A 2016 study reported a dose-response relationship between increasing levels of physical activity and decreasing risk of overall mortality but did not note the complete absence of moderate to vigorous physical activity, time since diagnosis, or sedentary behavior. 28 Hence sedentary behavior for patients with breast cancer is not addressed in the majority of studies, affirming the need for studies to strengthen the evidence and further improve the health status of survivors of cancer. 4
Our study addresses the gaps in the current knowledge of physical activity and sedentary behavior in patients with breast cancer in the midwestern United States in the clinical setting. Our primary aim is to assess physical activity and sedentary behavior across the breast cancer disease continuum, from shortly after diagnosis to a decade or more from diagnosis. This descriptive analysis will also meet our secondary aim of assessing how many patients with breast cancer meet national physical activity recommendations. Our goal is to provide information that clinicians can use to tailor interventions at the point of care for promoting physical activity and decreasing sedentary behavior. Such recommendations can extend the reach of lifestyle medicine into oncology care, expanding on an emerging collaboration between these two fields of expertise.3,29
Methods
Study Population
The study took place in a midwestern state. The study population consisted of all patients over 19 years of age who have a diagnosis of breast cancer and who presented for their routine oncology visits. Patients with all types of local or invasive breast cancer and ductal carcinoma in situ (DCIS) were included. Patients in various treatment stages, including those in active treatment and those in remission, were included.
Survey Instrument
Questions addressed in the current study were part of a larger survey assessing lifestyle and diet in patients with breast cancer. 1) Demographic and breast cancer information: The participant demographic questions consisted of age, gender, pregnancy status, ethnicity, and race. The questions regarding participants’ breast cancer included time since diagnosis, type of breast cancer (local or invasive), and remission status. 2) Physical activity and sedentary behavior: The researchers reviewed the current national guidelines and other published resources for pre-existing questionnaires of physical activity and sedentary behavior in patients with breast cancer that could be used in a busy breast cancer clinic setting. However, the existing surveys were found to be too lengthy for rapid use in the clinic, needed additional researcher training, were associated with complicated scoring systems, were confusing or inaccurate, or were limited by age cutoffs.13,30-34
We developed a brief survey for the clinical setting that assessed: a) Minutes of moderate to vigorous physical activity, which increases breathing or heart rate, during a typical week, including activities like brisk walking, carrying loads, running, digging, and bicycling. The amount of time was categorized into 30-minute intervals up to 2½ hours. (For the purpose of this study, unless otherwise specified, all references to physical activity will imply moderate to vigorous physical activity.) b) Sedentary behavior, as measured by workday and non-workday sitting or reclining time in hours.
35
The survey was available in paper form and electronically via QR code access.
Procedures
Patients were recruited after they checked in for their appointment. A medical student researcher (SC) explained the study to patients and answered questions. Each participant who gave verbal informed consent was given the survey to fill out while they waited for their appointment with their oncologist. Completed paper surveys were placed in a dropbox at the front desk or were returned via a postage-paid return envelope. Due to clinic workflow, not all patients presenting for care during a given clinic session were approached.
As an incentive to complete the survey and a token of appreciation for participating in our study, a handmade greeting card was given to each participant upon their consent to complete the survey.
This study was approved by the University of Nebraska Medical Center IRB (IRB protocol # 0333-23-EX).
Statistical Analyses
All analyses were conducted using SPSS v29.0. Descriptive statistics are used to summarize the characteristics of our sample. Differences across groups were examined using analyses of variance for continuous outcomes and chi square tests of independence or Fisher’s exact tests for categorical outcomes. The relationship between sedentary behavior and age was examined using Pearson’s correlation coefficient. The alpha level was set at 0.05.
Results
One hundred and nine patients with breast cancer were approached by the medical student researcher with only one refusal to participate in the survey, resulting in 108 participants (99% response rate). No participants opted to complete the survey electronically.
Demographic and Sample Characteristics of Patients With Breast Cancer.
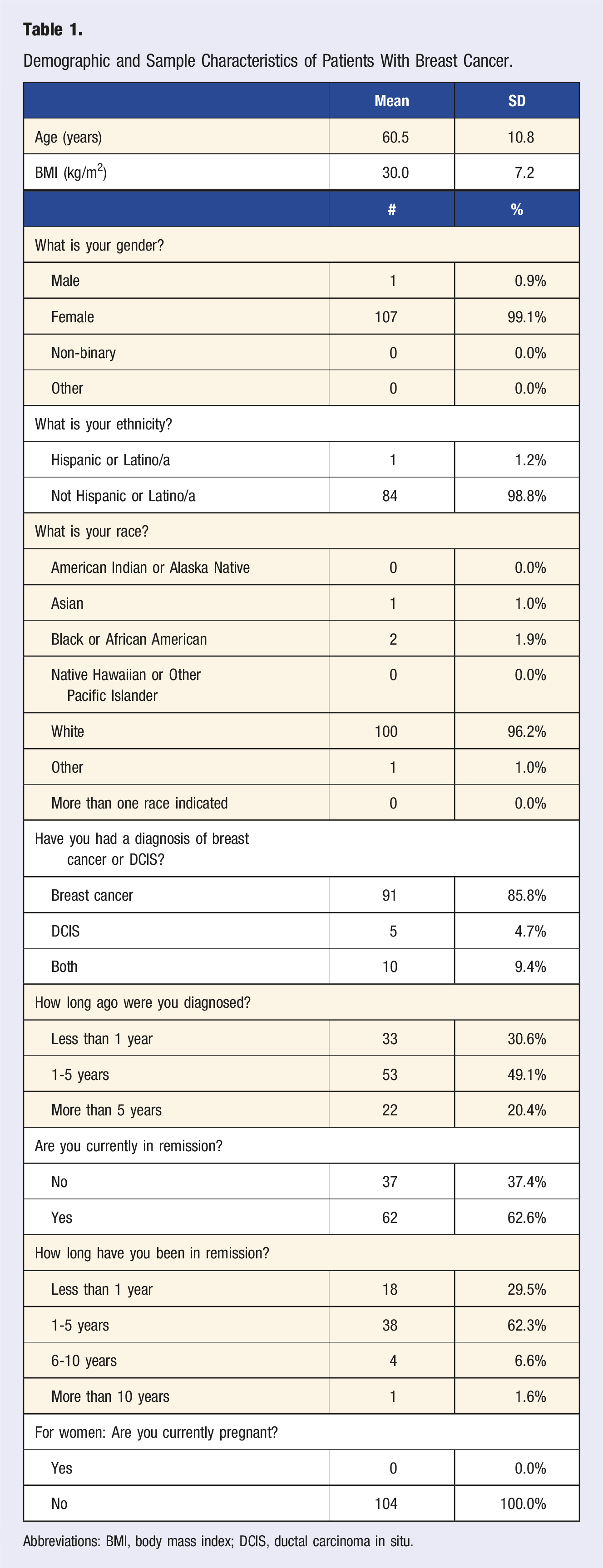
Abbreviations: BMI, body mass index; DCIS, ductal carcinoma in situ.
Physical Activity Duration.
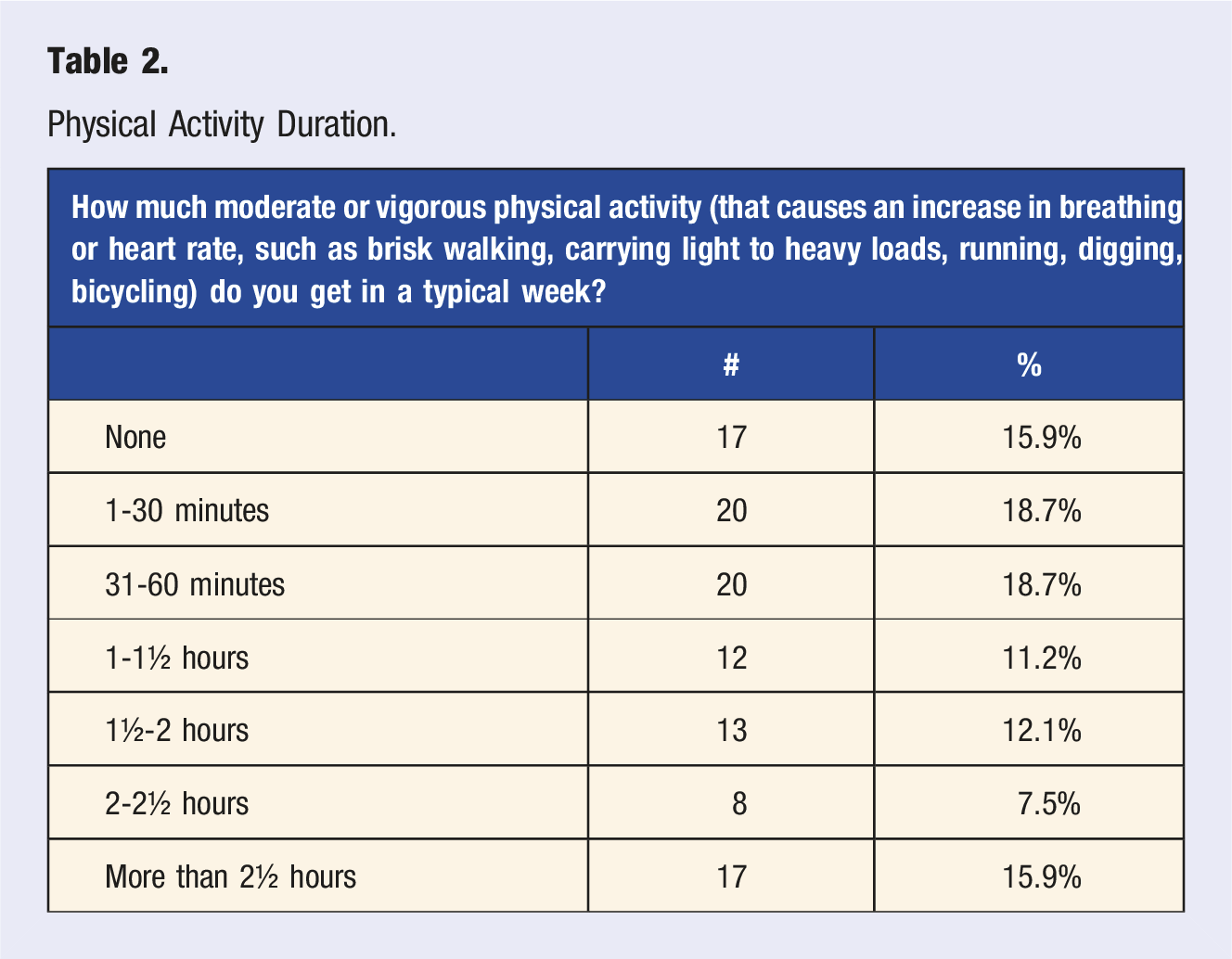
Percent of Respondents Meeting National Guidelines for Recommended for Moderate or Vigorous Physical Activity Per Week.
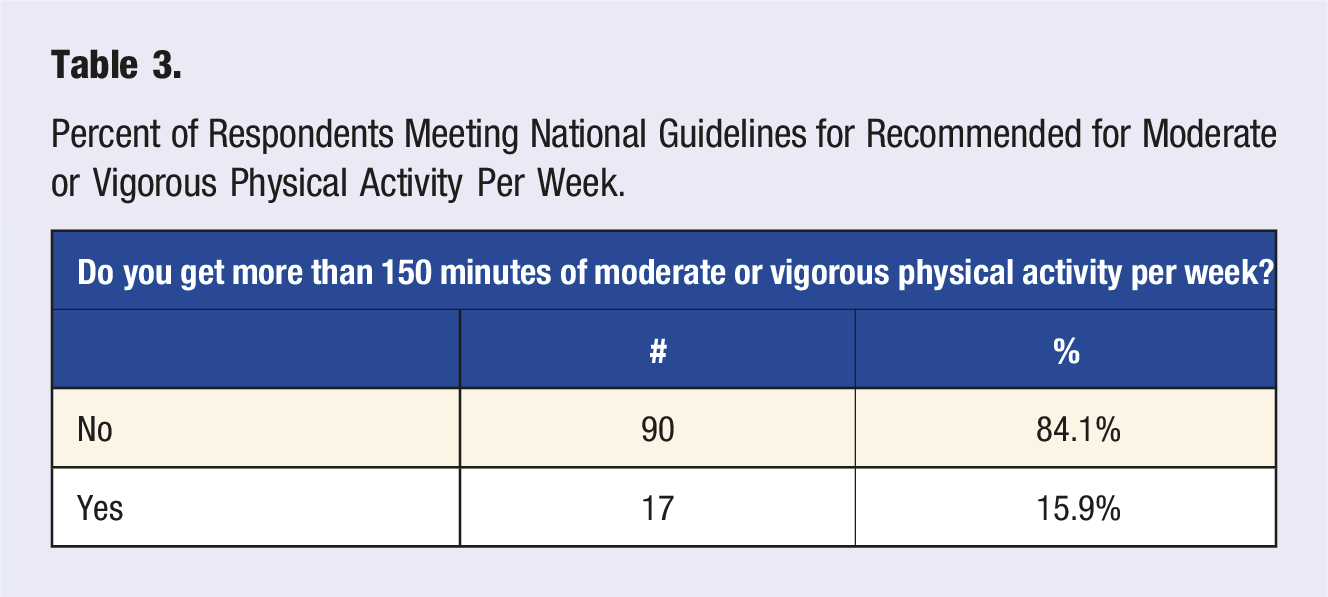
Figure 1 depicts the breakdown of physical activity by time since diagnosis. There was not a clear pattern of physical activity. Among those with a recent diagnosis, only 9.4% report more than 150 minutes of physical activity, while 13.2% of those who were within 1-5 years of diagnosis and 31.8% of those diagnosed more than 5 ago achieved the recommended amount of physical activity. There is not a statistically significant difference in the amount of physical activity based on the time since diagnosis (P = .839). Overall, across the three “time since diagnosis” groups, none had more than 50% of their patients meeting national guidelines of 150 minutes or more of physical activity per week. Amount of weekly moderate to vigorous physical activity by time since diagnosis of breast cancer in years.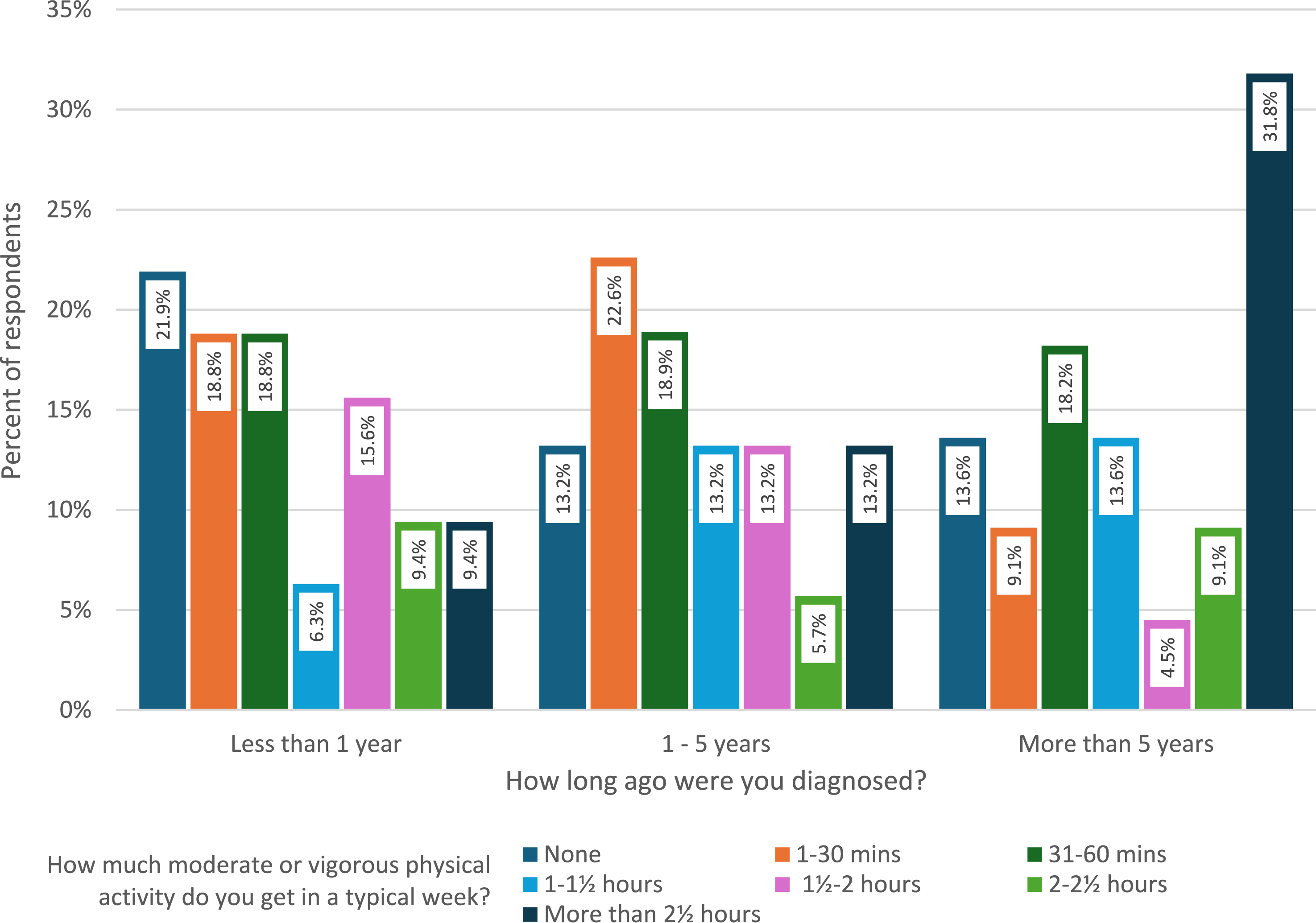
Levels of Physical Activity by Age at Time of Diagnosis, Breast Cancer Diagnosis, and Remission Status.
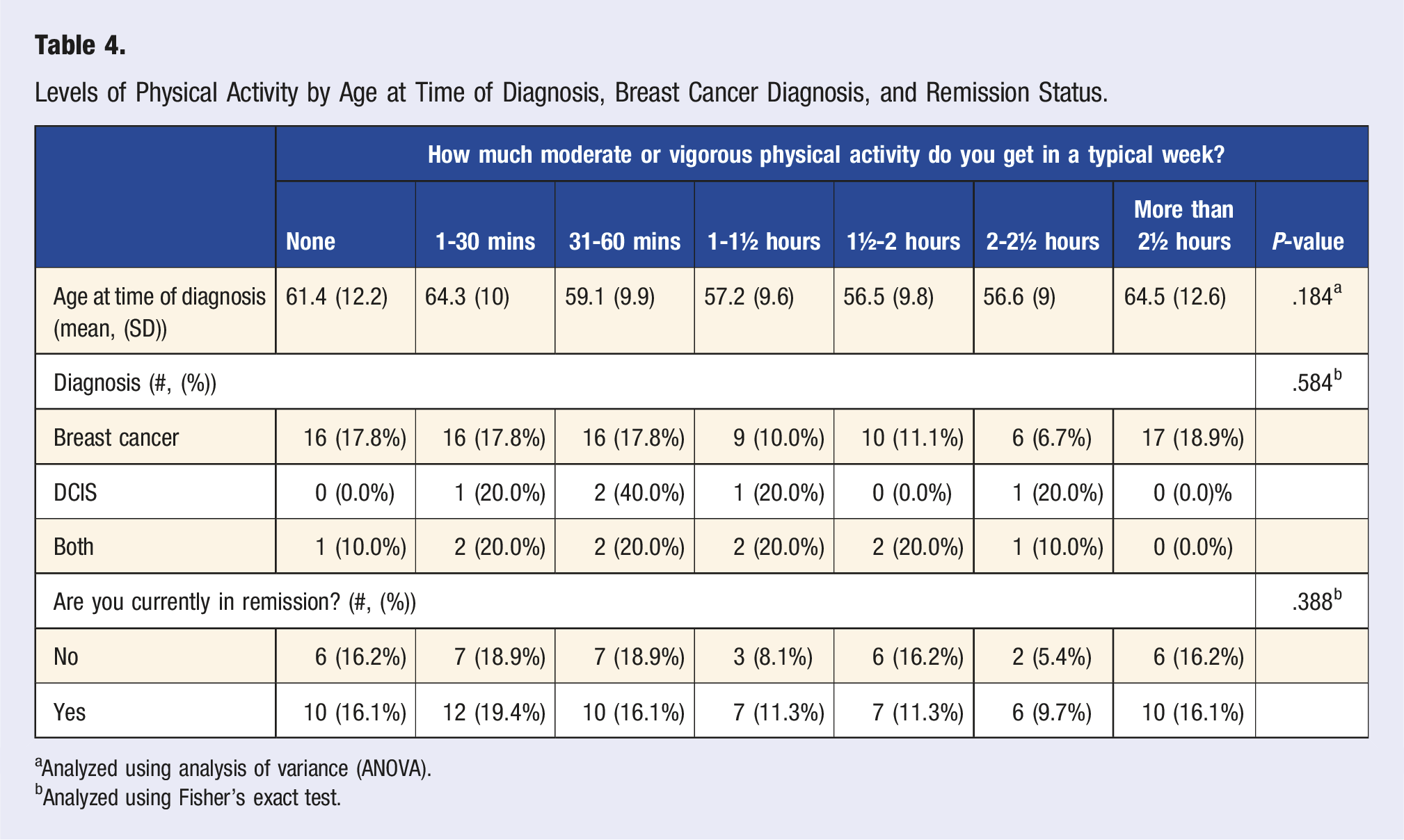
aAnalyzed using analysis of variance (ANOVA).
bAnalyzed using Fisher’s exact test.
Participant-Reported Time in Hours Spent Sitting or Reclining Per Day.
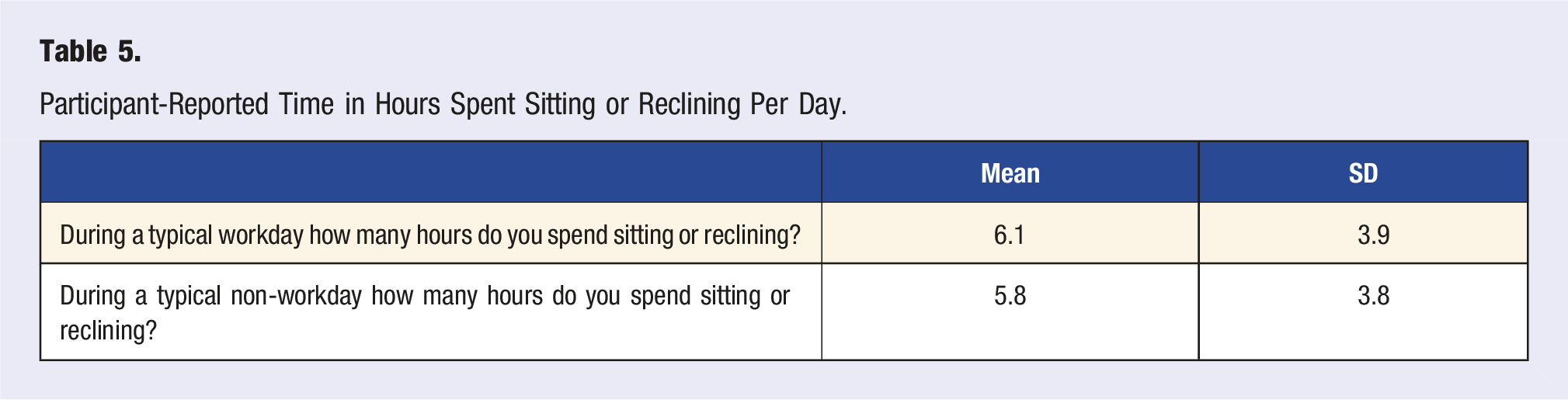
Figure 2 depicts the average number of hours sitting or reclining based on time since breast cancer diagnosis. Although the average number of hours of sedentary behavior declines as the time since breast cancer diagnosis increases, this trend is not statistically significant (P = .355). Sedentary behavior in number of hours spent sitting or reclining by time since breast cancer diagnosis.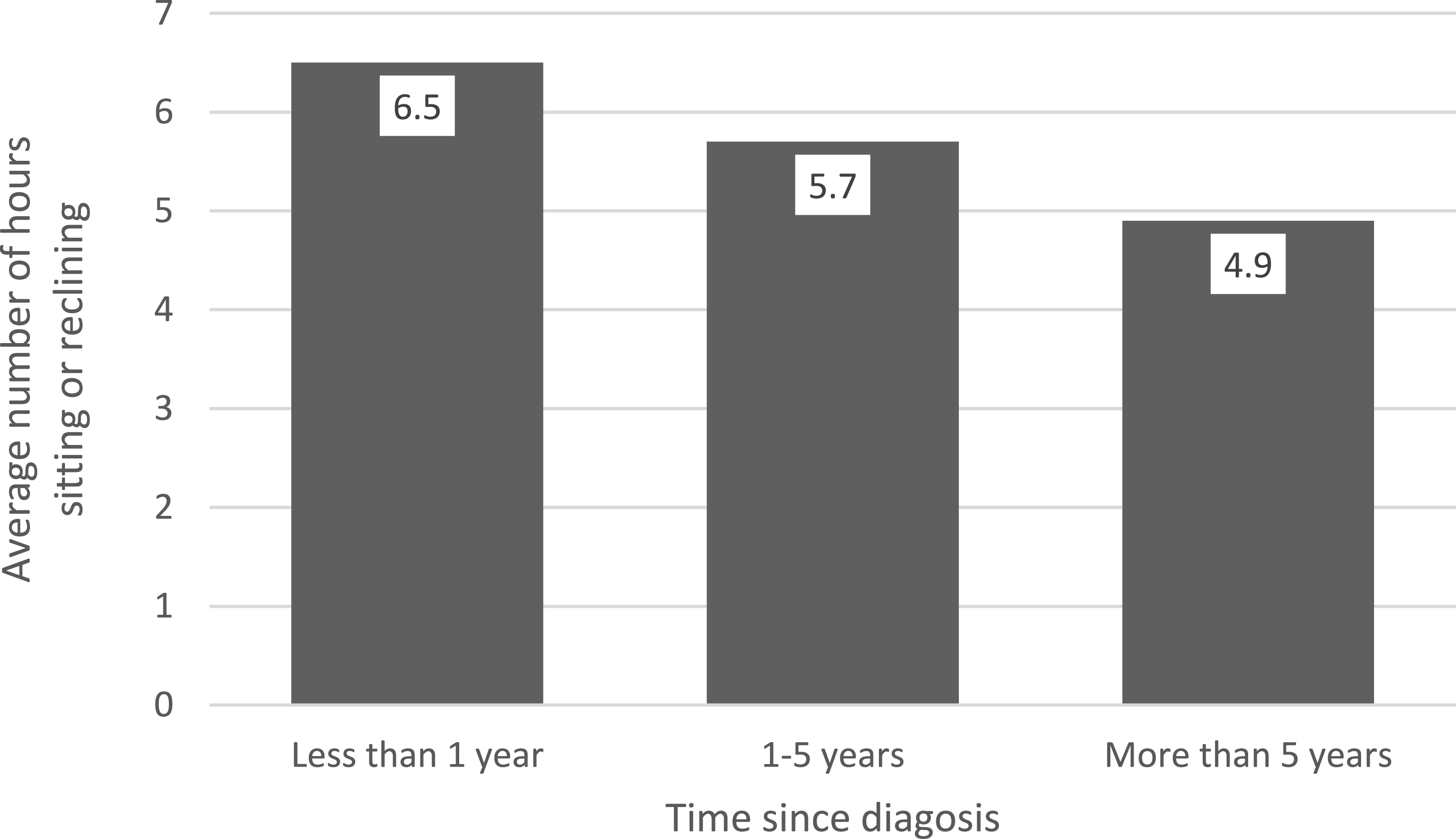
Although there is a slight positive relationship between age and sedentary behavior (r = 0.115), this relationship is not statistically significant (P = .261).
Sedentary Behavior by Breast Cancer Diagnosis and Remission Status.
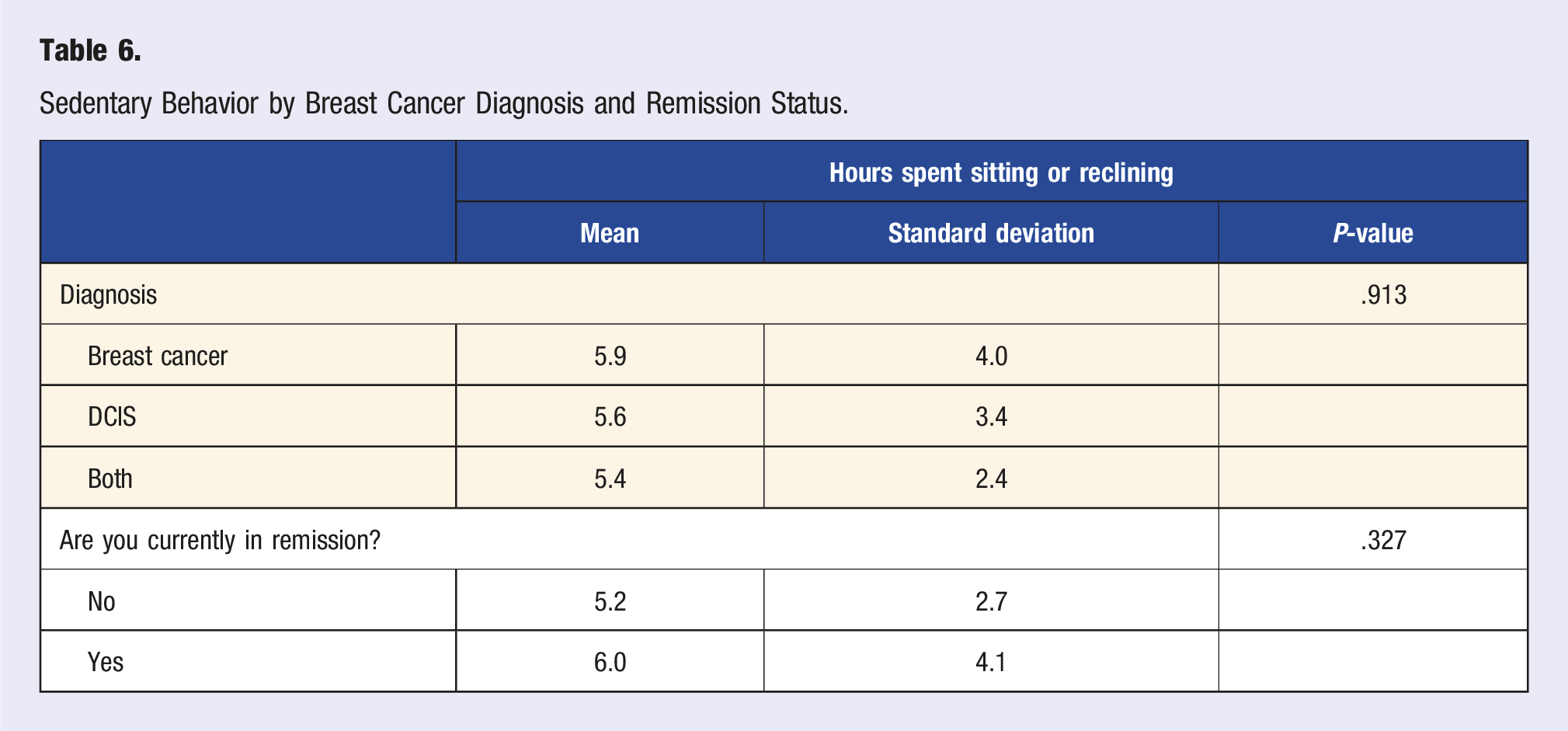
Discussion
Our study of a single cohort of midwestern U.S. patients with breast cancer provides valuable insights into their physical activity levels and sedentary behavior. The majority of our study participants, independent of age, type of breast cancer diagnosis, remission status, or time since diagnosis had suboptimal physical activity and did not achieve the recommended minimum of 150 minutes of moderate or vigorous activity weekly. Additionally, the survey participants report a high level of sedentary behavior, sitting or reclining an average of about 6 hours a day. Only in the small group of patients who are at least 5 years from diagnosis is there a more favorable trend of reduced sitting time and increased physical activity.
Lack of physical activity in these patients is similar to that reported in the general population of this midwestern state, where nearly one-fifth of adults report no physical activity. 36 While 62.6% of our sample reported being in remission, indicating a stage where they may have more energy and ability to engage in physical activity, a notable portion of these individuals reported no engagement in any form of physical activity. This could be due to several factors. The Health Belief Model posits that the intention to engage in physical activity post-cancer-diagnosis is multifaceted, influenced by perceived susceptibility and severity of the diagnosis, belief in benefits vs barriers, and self-efficacy. 37 Many patients who have cancer recognize the benefits of physical activity; however, there are a number of cancer and non-cancer-related barriers. These barriers include treatment-related side effects such as fatigue and gastrointestinal issues,38-40 physical pain and movement issues,38,41 clinical depression or anxiety,42,43 lack of motivation,38,43,44 limited access to suitable facilities and programs, 38 knowledge gaps, 39 and time pressures. 39 Lack of activity prior to breast cancer diagnosis was also related to physical inactivity after the diagnosis of breast cancer. 38 Lower adherence to recommendations has been noted in women compared to men. 44
Our study indicates that trends in physical activity from the time of diagnosis are similar to the overall trends over time reported recently in a study of 171 participants in the Mayo Clinic disease registry. In this study, a decrease in total physical activity over time was noted, and nearly one-third of the participants did not meet recommended guidelines at any time point. This study was stopped at 4 years post-diagnosis. A decline with age and physical activity was noted. 45
The levels of physical inactivity and sedentary behavior in our study were slightly better than those of a more recent study that found that 56.8% of cancer survivors reported no leisure time physical activity and 24.6% were sedentary for more than 8 hours per day. 46 Survivors of all types of cancer were significantly more likely to sit for 8 or more hours per day compared to a healthy population. 47
Physical activity and sedentary behavior in patients who have been diagnosed with cancer can have key effects on overall outcomes. Sitting 10 hours per day or more increased the risk of all-cause mortality in cancer survivors by 62%. 48 Overall and cancer-specific mortality risks were higher in breast cancer survivors who had a combination of physical inactivity and were highly sedentary. 46 Given these findings, the results of our study would indicate that our study cohort would also experience higher overall and cancer-specific mortality compared to those who meet the physical activity guidelines.
The 99% response rate in our cohort reflects a strong willingness among patients with breast cancer to participate in research related to their condition. Proponents of lifestyle medicine should be aware that breast cancer survivors may have increased motivation to improve their health, and that healthy lifestyle recommendations from their providers can be a powerful tool to motivate and change behavior.13,29 Although previous research has found that as many as 47% of cancer patients expressed interest in a physical activity program, 49 only 13% of cancer survivors received counseling on such from health care providers, and just 46% of oncologists actively encouraged physical activity in their patients. 50
Our study suggests that there may be “teachable moments” in which health care professionals can promote lifestyle modification. Such moments can occur anytime following a breast cancer diagnosis but may be particularly useful in the early years following diagnosis. 51 We found that the gaps in physical activity appear to be more profound closer to their diagnosis compared to those who were diagnosed 5 years or more prior to our study. Early physical activity engagement can prevent muscle mass loss, reduce recurrence, and improve overall physical functioning.52,53 Although health care professionals possessed knowledge about the benefits of physical activity for cancer patients, their advice was often general, lacking specific details such as frequency, intensity, time, and type (FITT principles) to effectively encourage patient adherence to recommendations. 54 The research underscores the importance of providing patients with specific and understandable instructions for improved adherence. 55 Understanding physical activity and sedentary behavior patterns can be valuable to health care providers in designing tailored interventions that consider individual preferences, capabilities, and treatment trajectories.
Evidence supports the integration of physical activity interventions throughout all stages of cancer treatment, necessitating sensitive framing to accommodate patients’ evolving needs and challenges.56-58 Interventions should consider the timing and nature of support, especially during critical periods like during chemotherapy or post-surgery recovery. Special considerations for the projected prevalence of long-term arm and shoulder complications among breast cancer survivors should be undertaken.59,60 The development of flexible and patient-centered physical activity resources, leveraging digital platforms and telehealth to reach a wider audience, will be needed with the growing population of patients surviving breast cancer. 61 Physical therapists who specialize in prescribing physical activity for chronic conditions can be integrated into cancer care teams, providing education and translating knowledge on activity-related topics.52,53
Unfortunately, specific interventions for reducing sedentary behavior have not yet been effective and have mainly focused on increasing physical activity rather than decreasing sedentary behavior. Ongoing quality research is recommended to develop strategies that target sedentary behavior reduction. 4
Notably, our cohort was slightly younger than most breast cancer patients. In the United States, the median age of breast cancer diagnosis is 62 years. 62 The mean age of our study participants was 60.3 years, the median was 60.5, and most patients in our study were diagnosed more than a year before, suggesting an even younger age at diagnosis. Nationally, the average age of diagnosis of colon cancer has been trending downward, and the lower age of diagnosis in our cohort implies that this trend may be also evident in breast cancer. 63 One contributing factor to this trend toward earlier onset of cancer may be the decrease in physical activity and increase in sedentary behavior in younger people. 64
Our study has the benefit of recording even small amounts of physical activity. Emerging evidence indicates that participants who move from no physical activity to minimal amounts may see meaningful benefits.18,23,65 Health care professionals in the clinical setting can align their recommendations with more updated guidance, personalizing their approach if necessary by encouraging smaller amounts than the traditional 150 minutes of aerobic physical activity.
Collecting information from patients in a clinical setting strengthens our study in that it facilitates translation into clinical practice. Additionally, it serves as a model for future research with patients who have been diagnosed with breast cancer, utilizing a brief survey instrument that can be administered easily by clinic staff or student volunteers. Future studies could use similar methodology to better understand barriers and facilitators to physical activity and sedentary behavior.
The limitations of this study are those inherent to any self-reported survey, including a small convenience sample and cross-sectional design. Responses may have been biased due to inaccurate recall or reporting. The necessarily brief survey administered in a busy oncology clinic could not delve into all of the factors that impact physical activity and sedentary behavior or assess the cancer-specific details that may have impacted the results, such as grade, stage, treatment phase or treatments. Our survey did not distinguish between moderate- and vigorous-intensity physical activity and may have therefore underrepresented those who met the U.S. aerobic activity guidelines. Furthermore, because we designed our own survey, direct comparisons between our findings and other clinic-based studies cannot be made. Our sample consisted of predominantly white, older women and results may not be reflective of a more diverse U.S. population. Both physical activity and sedentary behavior are difficult to precisely quantify without technology, such as an accelerometer, or detailed monitoring, as demonstrated in a recent study and study participants are well-known to overestimate physical activity and underestimate sedentary behavior; hence overall physical inactivity and sedentary behavior are likely higher than the self-reported results. 66 However, such studies may not be feasible in the clinical setting.
Future studies should incorporate an assessment of muscle-strengthening activity, compare mild, moderate and vigorous levels of physical activity and account for all daily movement in examining physical activity. The use of accelerometers is recommended to obtain objective, accurate measures of activity. If accelerometers are not available, to allow for direct comparisons across studies, we suggest using published measures of physical activity, such as the questions found in the National Health Interview Survey. 67 An in-depth exploration of targeted and personalized interventions, particularly closer to time of diagnosis, along with strategies to enhance adherence to physical activity recommendations, could lead to improved patient outcomes.
Conclusion
Our study provides patient-reported information at the point of clinical care from a cohort of participants with breast cancer in a midwestern U.S. city. Findings reveal profound physical inactivity leading to a potentially increased adverse impact on overall health and prognosis. Key recommendations to remain as physically active as possible after breast cancer diagnosis are not being currently achieved. Tailored lifestyle programs to enhance physical activity and decrease sedentary behavior are critical to improve outcomes and our results indicate that clinicians should incorporate healthy lifestyle medicine recommendations for all patients living with breast cancer, at any age or time since diagnosis independent of cancer type or remission status.
Footnotes
Acknowledgments
Dr Amulya Yellala for patient access. Frauke Wilcox and Mary Beth Steele for administrative support and manuscript preparation.
Declaration of conflicting interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
