Abstract
“The majority of epidemiological evidence supports that RT is associated with a lower risk of all-cause mortality.”
Introduction
National and international physical activity (PA) guidelines recognize the health benefits of muscle-strengthening activities also referred to as resistance training (RT; which will be used for this current study).1-3 RT promotes hypertrophy, which has a dose-response association with improvements in blood pressure, lipids, and glycemic markers.4-8 Additionally, RT may improve insulin sensitivity independently of hypertrophy by increasing perfusion surface within the muscle and improving vasodilator response. 9 However, approximately 72% of adults in the United States (US) achieve less than the US Department of Health and Human Services recommended 2 days of moderate or greater RT per week involving the major muscle groups of the body.2,10
While the current guidelines provide recommendations based only quantifiably on RT frequency (at least 2 days per week of moderate or greater intensity involving all major muscle groups), evidence from interventional and randomized control trials suggests that RT volume—the product of frequency, intensity, and duration—is the primary metric associated with markers of cardiometabolic health.1,11-13 A meta-analysis found no association between hypertrophy and weekly RT frequencies (1 day/week, 2 days/week, 3 days/week, and 4-6 days/week) when holding total RT volume fixed. 14 The component studies examined changes in hypertrophy directly rather than the downstream markers of cardiometabolic morbidity or mortality. Experimental studies generally have more control over RT volume dose and measurement compared to observational studies, which often measure RT via self-reported recall. However, large population-based cohorts can examine the association between RT and all-cause mortality in a representative sample of people who engage in RT, which can be challenging to recruit in a trial. Some large population-based and cohort studies have investigated the association between RT and mortality,15-17 but to our knowledge, no studies have examined these associations using RT volume.
There is discordance between the RT frequency recommendations in the guidelines and the empirical evidence that supports measuring RT volume to study health benefits that may be due in part to the heterogeneity in the conduct of experimental vs observational studies. Our objective was to examine the associations of meeting the RT guidelines and greater RT volume with all-cause mortality rates in a nationally representative sample of US adults.
Methodology
Data were from the four National Health and Nutrition Examination Survey (NHANES) cycles spanning 1999-2006. NHANES is a nationally representative cross-sectional survey of the civilian, noninstitutionalized population of the US. The National Center for Health Statistics Ethics Review Board approved all NHANES protocols, and all participants provided written informed consent. The NHANES uses a complex, multistage, probability sampling design and provides the corresponding sampling weights. 18 Exclusions were enforced after consideration of the sampling design and weights to maintain proper population-level estimates.
NHANES participants self-reported the past 30 days of PA. For the present study, we used the individual PAs questionnaire which inquired about detailed information specific to moderate and vigorous leisure-time activities. Participants who reported any PA also reported specifics about each type of movement including the number of sessions and average session duration (minutes). Activity intensity was measured in metabolic equivalents (METs). 19 Total monthly volume of each activity was calculated as the product of the number of sessions of the activity, average session duration, and intensity. Push-ups, sit-ups, and weightlifting were categorized as RT. A participant met the RT guidelines if they reported 8 or more sessions of RT in the past 30 days. The total monthly RT volume was calculated as the sum of the total monthly volume for push-ups, sit-ups, and weightlifting. 15 All other activities were categorized as aerobic PA. Total monthly aerobic PA volume was calculated analogously.
Vital status was determined using the NHANES-National Death Index linked file through December 31, 2019. Follow-up time was calculated as person-months between the date of the NHANES interview and the sooner of the date of death and December 31, 2019. Vital status is not publicly available for individuals under 18 years of age (n = 18,850). Individuals missing vital, follow-up time, PA, or covariates were excluded.
Two sets of analyses were conducted to examine the associations between meeting the RT guidelines and greater RT volume with all-cause mortality rates. All analyses accounted for the complex, stratified, multistage probability sampling design in the NHANES by using analytical methods for weighted survey samples. Each set of analyses included unadjusted and covariate-adjusted models. The adjusted models were adjusted for aerobic PA volume (categorized into empirical quartiles), sex (male or female), race/ethnicity (Mexican American, Other Hispanic, Non-Hispanic White, Non-Hispanic Black, and Other Race—Including Multi-Racial), age (years), education (less than high school, some college or associate degree, college graduate or above), tobacco use (ever or never), alcohol use (average number of drinks per day over the last 12 months), comorbidities (sum of self-reported prevalence of arthritis, diabetes, emphysema, heart attack, hypertension, osteoporosis, diabetes, and stroke) and BMI (kg·m−2) at the time of the survey.
The first set of analyses used a Cox proportional hazards model to estimate hazard ratios for all-cause mortality for those who met the RT guidelines vs those who did not among the full sample. The second set of analyses used Cox proportional hazards regression to estimate hazard ratios for all-cause mortality for every 1000 MET-minute increase in monthly RT volume. A monthly RT volume of 1000 MET-minutes is equivalent to engaging in approximately two 45-minute RT sessions at moderate intensity (3.0 METs) per week. The second set of analyses was repeated in the subsample of participants who reported at least one RT session.
Given the paucity of epidemiological work examining the various components of RT, sensitivity analyses examined duration, session, and intensity of RT, bodyweight only (i.e., push-ups and sit-ups), and weightlifting only.
The proportional hazards assumption was assessed using scaled Schoenfeld residuals. All statistical analyses were conducted using R (version 4.2.1, R Program for Statistical Computing). A 95% confidence interval that did not contain one was considered statistically significant.
Results
Of the 41,474 individuals from the 1999-2006 NHANES cycles, individuals missing vital status (n = 18,871; n = 18,850 being under 18 years of age and n = 21 eligible, but missing), follow-up time (n = 1419), PA (n = 8949), or covariates (n = 6367) were excluded. Additionally, individuals whose RT volume was greater than three standard deviations from the mean were considered outliers and excluded (n = 13) for a final analytic sample of 5855. The RT-only analysis included 813 participants who reported any RT.
Participant Characteristics by Engaging in Any or No Resistance Training.
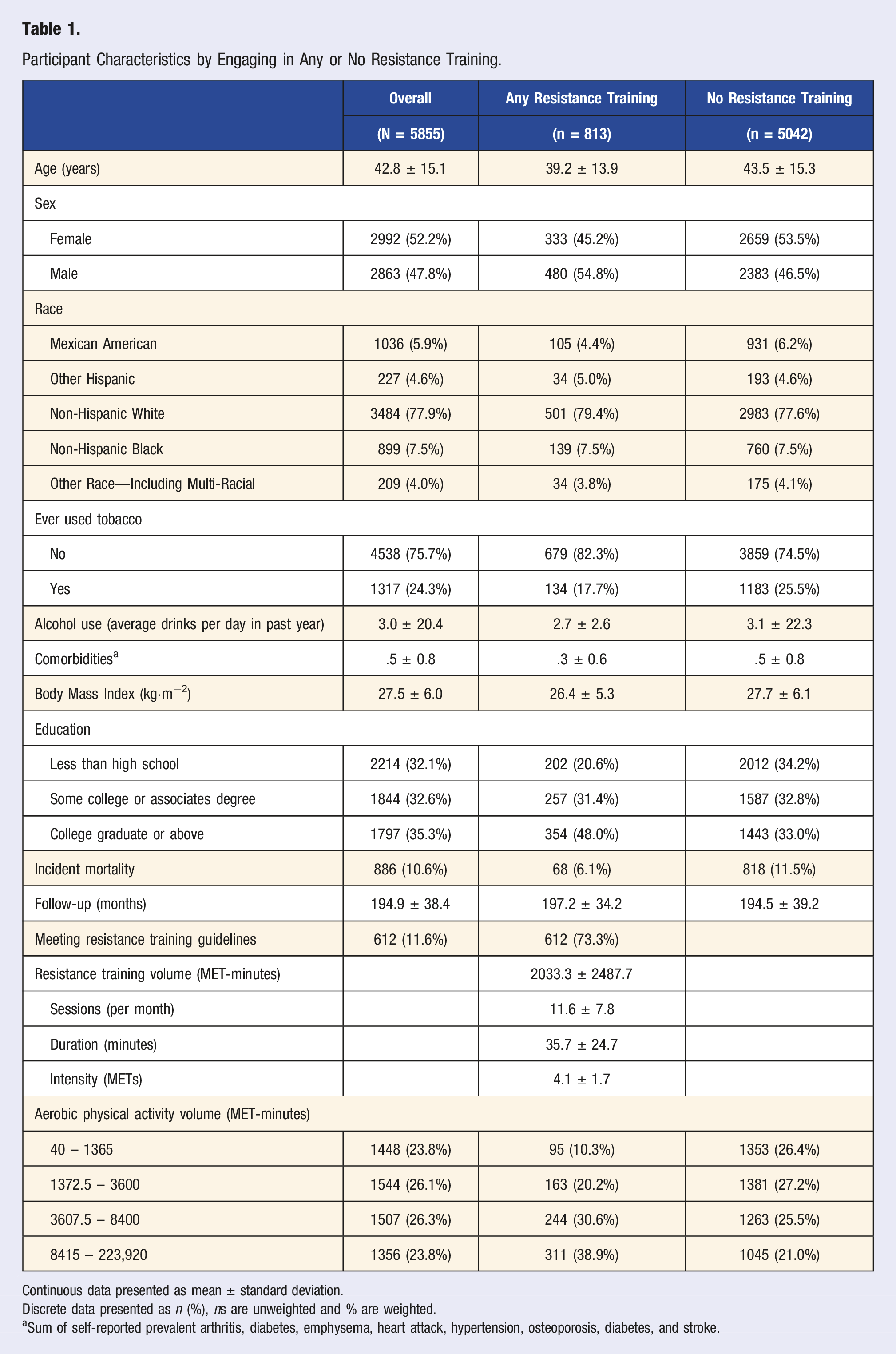
Continuous data presented as mean ± standard deviation.
Discrete data presented as n (%), ns are unweighted and % are weighted.
aSum of self-reported prevalent arthritis, diabetes, emphysema, heart attack, hypertension, osteoporosis, diabetes, and stroke.
Among those with any RT (n = 813), participants were 39.2 ± 13.9 years old, equally split by sex (female: n = 333; 45.2%), and 48.0% were at least a college graduate. The average monthly RT volume was 2033.3 ± 2487.7 MET-minutes across 11.6 ± 7.8 sessions lasting 35.7 ± 24.7 minutes at an intensity of 4.1 ± 1.7 METs.
Cox Regressions of Resistance Training Measures and All-Cause Mortality.
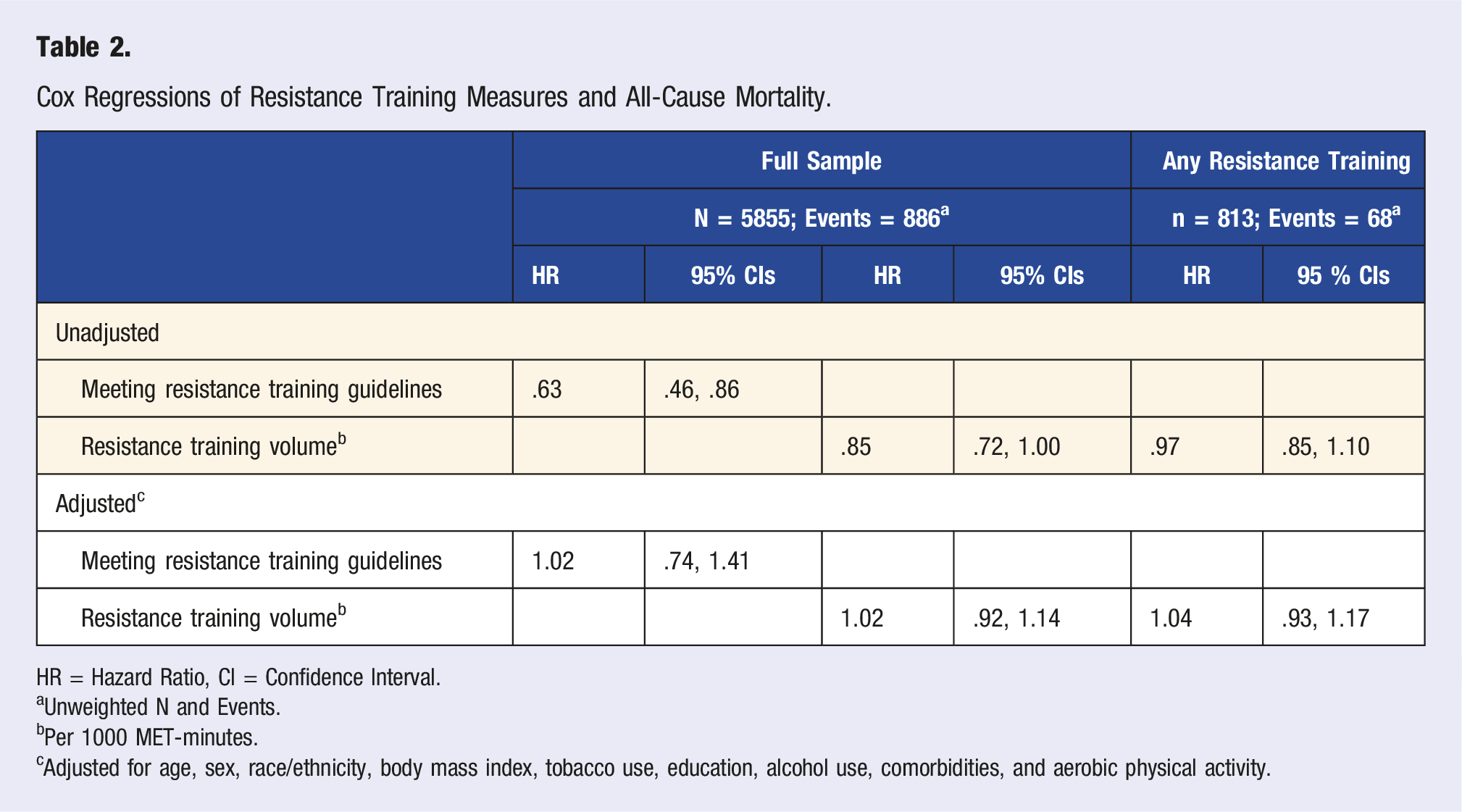
HR = Hazard Ratio, CI = Confidence Interval.
aUnweighted N and Events.
bPer 1000 MET-minutes.
cAdjusted for age, sex, race/ethnicity, body mass index, tobacco use, education, alcohol use, comorbidities, and aerobic physical activity.
In the adjusted Cox proportional hazards models (Table 2), neither meeting the RT guidelines (HR [95% CIs]; 1.02 [.74, 1.41]) nor monthly RT volume (1.02 [.92, 1.14]) were associated with all-cause mortality. There was no effect modification by sex or age for meeting the RT Guidelines (P = .15 and P = .95, respectively) nor RT volume (P = .34 and P = .22, respectively). Among participants with any RT, the volume of RT was not associated with all-cause mortality (1.03 [.94, 1.13]) with no effect modification between RT volume with sex (P = .35) or age (P = .22).
In the full sample, the average monthly body weight-only RT volume was 58.8 ± 501.7 MET-minutes across .4 ± 3.6 sessions lasting .4 ± 3.0 minutes at an intensity of .2 ± 1.1 METs. The average monthly weightlifting-only RT volume was 273.1 ± 1088.5 MET-minutes across 1.6 ± 4.9 sessions lasting 5.9 ± 17.1 minutes at an intensity of .5 ± 1.4 METs. Sensitivity analyses demonstrated similar non-significant associations as the primary analyses. In the full sample compared with no bodyweight or weightlifting, there was no association with all-cause mortality when examining either any bodyweight exercise (.79 [.39, 1.58]) or any weightlifting (.99 [.70, 1.38]). Among participants with any RT compared with no bodyweight or weightlifting, there was no association with all-cause mortality when examining either any bodyweight exercise (.90 [.44, 1.87]) or any weightlifting (.98 [.37, 2.65]). Among participants with any RT, the duration, number of sessions, or intensity of RT was not associated with all-cause mortality (1.00 [.99, 1.01], 1.00 [.99, 1.01], and .98 [.92, 1.05], respectively). Additionally, among the full sample, compared with 0-1 RT sessions, 2-3, 4-6, and 7 or more RT sessions were not associated with all-cause mortality (.83 [.19, 3.55], .76 [.31, 1.91] and 1.01 [.73, 1.39], respectively).
Discussion
In this study of a nationally representative sample of adults in the United States, neither meeting the RT guidelines nor RT volume in the past 30 days was associated with all-cause mortality in covariate-adjusted models. These results add to the mixed literature on RT and mortality.15-17,20,21 Corroborating the present results, using data from the 1999-2004 NHANES, researchers observed meeting the RT guidelines (≥2 times per week in response to “How often do you do physical activities specifically designed to strengthen your muscles, such as lifting weights or doing calisthenics?”) was not associated with all-cause mortality after controlling for aerobic PA (hazard ratio [95% CIs]; .97 [.61, 1.54]). 17 Boyer et al., using 1999-2006 NHANES data, observed that meeting the RT guidelines (≥2 times per week) was not associated with all-cause mortality (.86 [.69, 1.07]). 15
However, the majority of epidemiological evidence supports that RT is associated with a lower risk of all-cause mortality. Gorzelitz and colleagues found weightlifting, a specific type of RT, to have independent and joint associations with aerobic PA in reducing the risk of all-cause mortality. 16 Among adults who reported no aerobic moderate-to-vigorous PA, there was a dose-response association with weightlifting and a lower risk of all-cause mortality ranging from 9% to 20%. 16 Webber and collaborators used 1997-2018 National Health Interview Survey data on RT (“How often do you do leisure-time physical activities specifically designed to strengthen your muscles such as lifting weights or doing calisthenics?”) to examine possible thresholds or nonlinearities in the association of RT with all-cause mortality. 22 When compared with 0-1 RT sessions and less than 10 minutes of aerobic moderate-to-vigorous PA weekly, achieving 150-300 minutes of aerobic moderate-to-vigorous PA and 0-1, 2-3, or 4-6 RT sessions per week to be associated with lower risk of all-cause mortality (.76 [.73, .79], .66 [.59, .73], and .58 [.49, .68], respectively) although the authors did not assess if these risks were significantly different from one another. 22 Additionally, researchers conducted a systematic review and meta-analysis of 16 studies of the relation between RT (calisthenics and RT) and health outcomes in adults without severe health conditions. 20 Six studies examined the dose-response relation between RT, per 10 minutes per week increase, with all-cause mortality in which the lowest relative risk was observed at 40 minutes per week of RT (.83 [.79, .86), and the relative risk estimate for up to nearly 140 minutes per week was less than 1.00. 20 The overall quality of the evidence supporting the association between RT and all-cause mortality was rated as “very low.” 20
From the same systematic review by Momma et al., 20 seven of the 16 studies examined the relation between any RT and all-cause mortality and found that any RT was associated with a 15% lower risk of all-cause mortality (relative risk [95% CIs]; .85 [.79, .93]). 20 Zhao and colleagues using the National Health Interview Survey data from 1997-2014 with vital status assessed through the end of 2015 observed that the risk of all-cause mortality was lower among participants meeting the RT Guidelines (≥2 times per week in response to “How often do you do physical activities specifically designed to strengthen your muscles, such as lifting weights or doing calisthenics?”) compared with those not meeting the RT Guidelines (hazard ratio [95% CIs]; .89 [.85, .94]). 21
The contradictory results could be due to differences in how RT and aerobic PA were captured, participant characteristics including age at inclusion/assessment, follow-up duration, and covariates. While the novelty of using RT volume has been highlighted already, the average age of our study was substantially younger than the studies by Gorzelitz 16 and Webber 22 (42.8, 71.3, and over 65 years old, respectively). While the present study had a longer average follow-up time than the Gorzelitz and Webber studies (16.2, 9.6, and 7.9 years, respectively), the event rate was lower (10.6%, 28.6%, and 38.8%, respectively). Further, while Zhao and colleagues had comparable follow-up (8.75 years) and proportion of events (12.5%), the overall sample was approximately 40 times larger. 21
The lack of comparable guideline recommendations between RT and aerobic PA may stem from the crude and varied tools used to measure RT. Shakespear-Druery and colleagues conducted a systematic review of epidemiological assessments of muscle-strengthening exercise and identified 58 unique surveys spanning 17 countries. 23 Not only are existing instruments varied, but none are validated against a criterion measure (i.e., direct observation) and none, including NHANES, collected all three domains required to calculate RT volume as defined by the National Strength and Conditioning Association (NSCA; the product of sets, repetitions, and resistance).3,23-25 Notably, of the 58 unique epidemiological tools for assessing RT only 23.7% assessed duration, 85.3% frequency, and 1.3% intensity (e.g., perceived intensity and not resistance). 23 In the current PA guidelines and more generally among PA instruments, three dimensions of aerobic PA are captured, which more precisely describes each activity. By contrast, RT instruments usually omit or improperly measure all three dimensions required to calculate RT volume. These issues in measuring RT volume are echoed in the 2020 World Health Organization’s PA Guidelines, which recommend refining the monitoring systems that track RT. 1
Limitations of this study include the possibility of reporting bias in self-reported 30-day PA recall (a universally acknowledged limitation of survey-based PA research 26 ), and the use of METs to characterize RT intensity to calculate RT volume. METs are a measure of the metabolic cost (i.e., energy expenditure) above resting to perform an activity, and are used to quantify activity intensity under the assumption that the activity is aerobic and performed at a steady state for at least 3 minutes. 19 RT is often discontinuous and typically anaerobic, 19 and therefore violates the fundamental assumption that links METs to intensity, although the use of METs for RT has been used before.27-29 Additionally, RT may improve health and longevity through mechanisms other than energy expenditure, including adaptation to the neuromuscular system (e.g., strength, power, and endurance), muscle quality, body composition, and vasoactive properties through sympathetic activation that are not captured by METs.25,30-33 Lastly, RT volume was derived but not measured by NHANES. Strengths of this study include the use of the nationally representative NHANES sample, which allows findings to be generalized to the national population.
Participation in RT has known benefits on cardiometabolic health. However, there is conflicting evidence in population-based studies on whether RT is associated with a lower risk of all-cause mortality. The absence of an association between monthly RT volume and all-cause mortality in the present study warrants further investigation using a criterion-measure-validated instrument for assessing RT volume.
Footnotes
Acknowledgments
The authors would like to thank the participants of the 1999-2006 NHANES cycles.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: RB was supported by grant funding from the National Heart, Lung, and Blood Institute (K99HL168338 and T32HL069771).
Data Availability Statement
NHANES is a publicly available dataset and is available for download at https://www.cdc.gov/nchs/nhanes/index.htm. The NDI is a publicly available dataset and is available for download at ![]() .
.
