Abstract
This paper is an literature evaluation of the treatments based on the 6 pillars of Lifestyle Medicine (nutrition, physical activity, restorative sleep, stress management, positive social connection, and avoidance of risky substances) to improve vasomotor symptoms. Main findings were: (1) the Mediterranean diet and other plant-forward approaches may effectively reduce vasomotor symptoms; (2) stress can directly impact menopausal symptoms by increasing the frequency and intensity of hot flashes and other symptoms; (3) the incidence of sleep disturbances are high during the menopause transition; (4) evidence on the impact of physical activity and exercise on vasomotor symptoms is mixed, although moderate activity and strength training may be better for vasomotor symptom optimization than vigorous exercise and part of a healthy aging process; (5) evidence on the impact of social support on VMS is mixed with some studies suggesting benefit; and (6) evidence on the impact of risky substances is mixed but appears stronger for the effects of tobacco cessation than for alcohol cessation. In summary, while there is a variety of quality of evidence depending on the pillar, lifestyle medicine may be generally considered to improve vasomotor symptoms for patients that cannot use or decline hormone therapy.
Keywords
“Evidence exists most strongly for stress reduction via cognitive-behavioral therapy, and clinical hypnosis, with mixed evidence for mindfulness-based stress reduction and other mind-body techniques.”
Introduction
While hormone therapy is the most effective treatment for vasomotor symptoms (VMS), 1 health care providers should still remain informed on evidence-based non-hormonal options to treat vasomotor symptoms in women that cannot use or may decline hormone therapy. The recent North American Menopause Society (NAMS) 2023 position statement covered non-hormonal therapies in detail; however, much of the review was focused on non-hormonal pharmaceuticals. This paper examines the evidence for the 6 pillars of Lifestyle Medicine—nutrition, physical activity, restorative sleep, stress management, positive social connection, and avoidance of risky substances—as a detailed analytic review on the topic of lifestyle elements and adjustments to improve vasomotor symptoms of menopause as a supplement to the recent NAMS position statement.
Methods
A comprehensive search was performed using PubMed, Auraria and Northwestern libraries’ website search function to search for articles pertaining to the pillars of Lifestyle Medicine and vasomotor symptoms. The search was conducted between 2021 and 2023, with articles from 2002-2023, and research published within the last 5 years prioritized for inclusion. Search words, including “vasomotor symptoms, menopause, menopausal, premenopausal, postmenopausal, hot flashes, night sweats, transition, flushes, and lifestyle medicine,” were used. In addition, words specific to each lifestyle medicine pillar helped narrow down the literature as follows. Nutrition: nutrition, diet, soy, isoflavones, healthy eating, nutrient, Mediterranean, whole food, plant-based, DASH, vegan, vegetarian Physical Activity: exercise, movement, yoga, aerobic, anaerobic, resistance, balance, sedentary, cardiometabolic, walking, moderate, vigorous Sleep: sleep disturbances, sleep problems, insomnia, sleep disorder, sleep apnea, sleep quality, sleep efficiency, fatigue Stress: psychological, oxidative stress, change, stressor, resilience, mindfulness, relaxation, perceived stress, cognitive-behavioral therapy, hypnotherapy Social Connection: partner, spouse, relationship, social support, interpersonal, friend, community Risky Substances: alcohol, tobacco, illicit drug
Mendeley reference management software was used to organize the literature. Paperpile was used to compile the reference list. Research articles published in the last 5 years were prioritized, unless there was a paucity of literature in the area of interest or if the study had a strong research cohort, prospective or randomized control trial, that was done prior to the five-year window. Randomized controlled trials, meta-analyses, and well-designed prospective studies were prioritized in the analytical review, although less robust studies were considered in the event of a paucity of available data.
Results
Each of six pillars of Lifestyle Medicine was examined for improvement in vasomotor symptoms in this analytic review.
Nutrition (Diet)
Recent studies have examined the potential benefits of specific dietary patterns and nutrients, as well as the impact of resultant weight change, in alleviating VMS. While many studies of natural products for VMS exist, this review focuses only on natural food sources.
Dietary Patterns
Studies on the Effect of Diet Patterns on VMS in Postmenopausal Women.
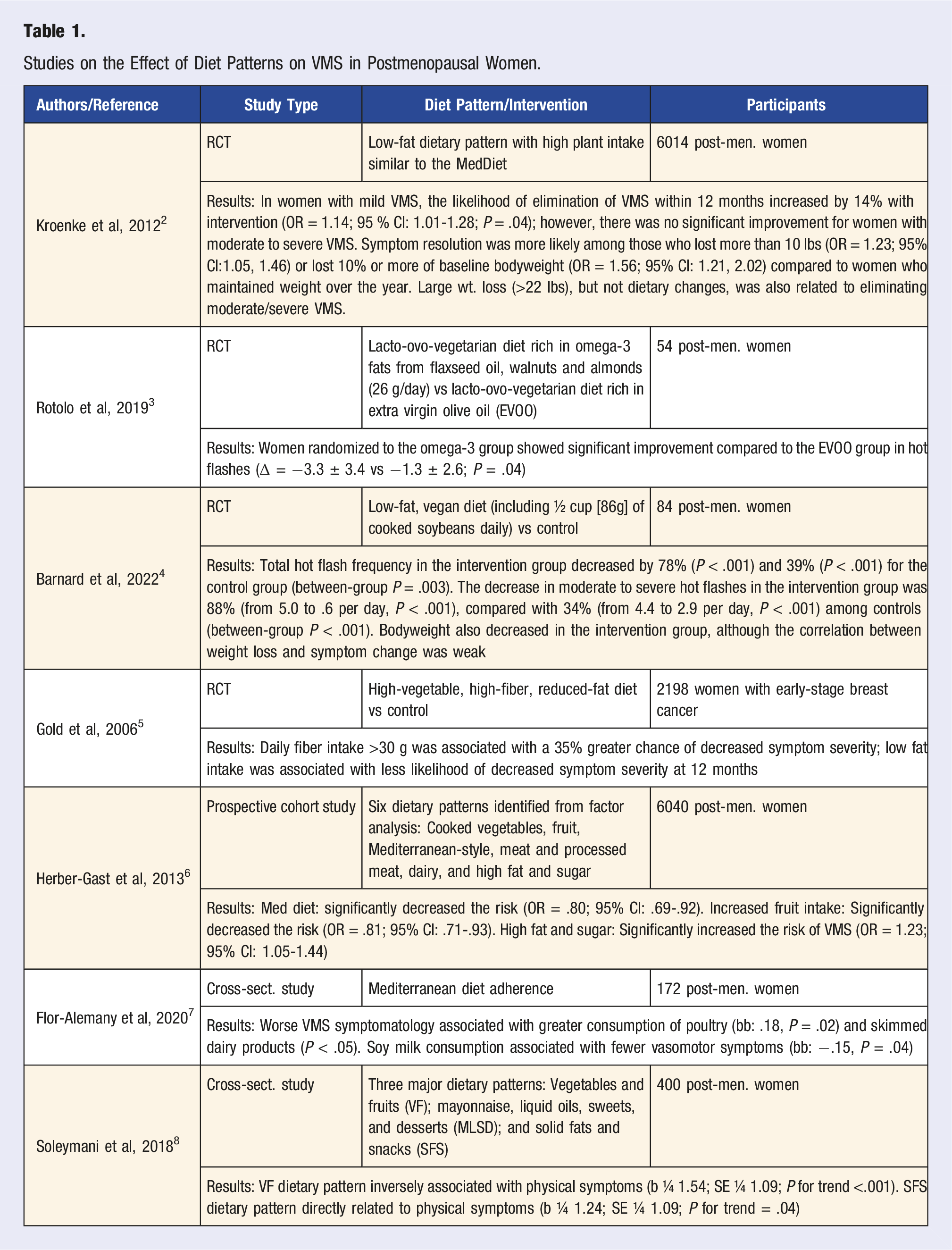
Insulin resistance (IR) and metabolic syndrome have been correlated with VMS.9,10 Dietary strategies such as low carbohydrate diets, intermittent fasting, and fasting mimicking diets may counter IR, 11 and theoretically relieve VMS; however, only anecdotal data for this indication exists. A study comparing 4 dietary patterns from the Women’s Health Initiative Observational Study: low-fat; reduced-carbohydrate; Mediterranean-style; and a diet consistent with the USDA’s Dietary Guidelines for Americans found that a reduced-carbohydrate diet, with moderate fat and high protein intake, may decrease the risk of weight gain in postmenopausal women, whereas a low-fat diet was associated with increased risk of weight gain. 12 While this study did not examine VMS, the link between weight, metabolic syndrome, and VMS postmenopause suggests a plausible benefit to lower carbohydrate diets.
Specific Dietary Components
Studies on the Effect of Dietary Phytoestrogens on Vasomotor Symptoms (VMS).
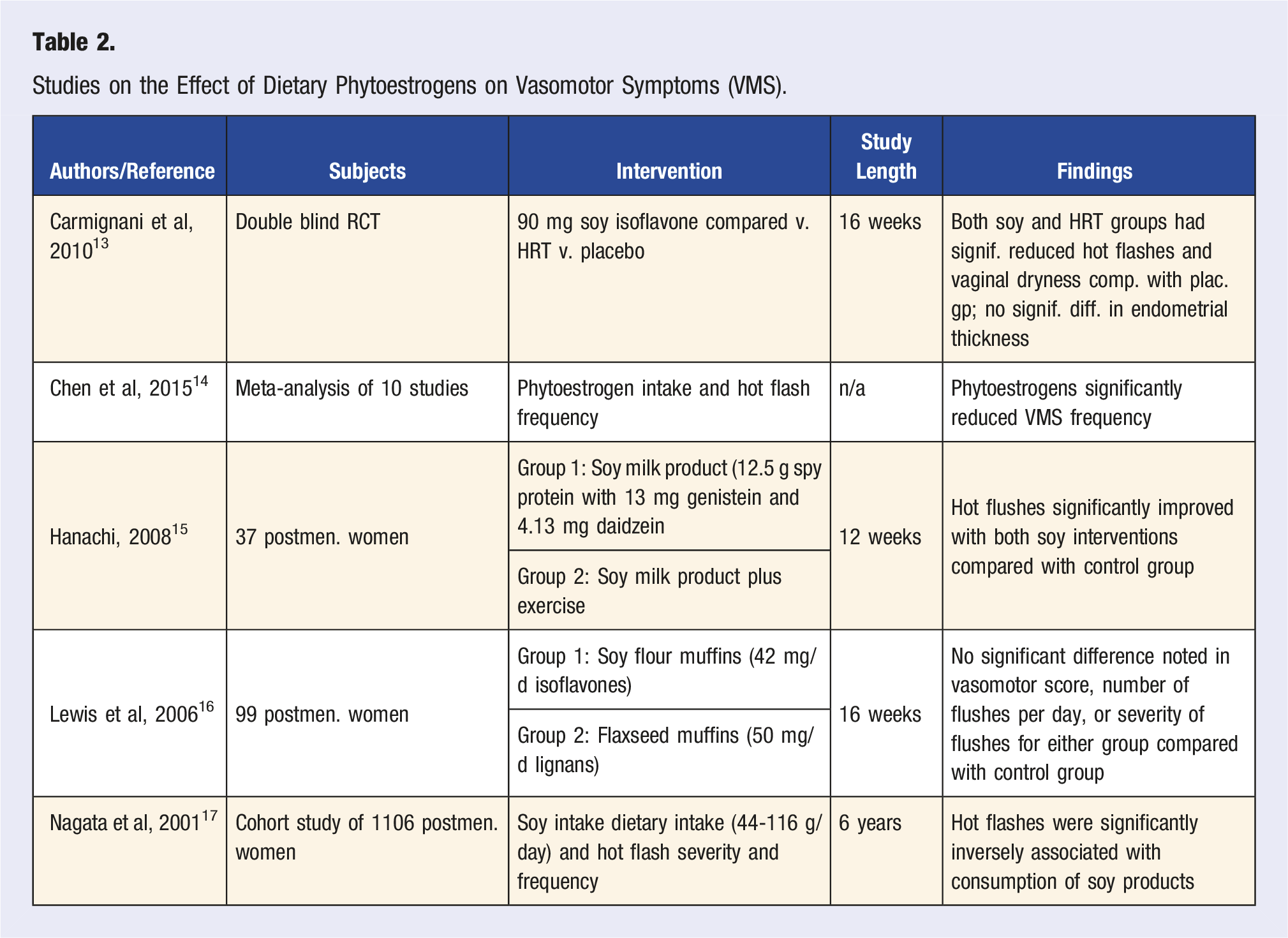
Summary
Many potential mechanisms of diet on VMS exist, including the role of the gut microbiome in estrogen metabolism, insulin resistance, estrogen production in adipose tissue, hormone receptor modulation, and vasodilation. Given the correlation of VMS with cardiovascular disease risk, 21 a plant-based diet is an appropriate option to both improve quality of life for women with VMS and prevent CVD, with consideration of reduced-carbohydrate diets in women at risk for weight gain and metabolic syndrome.
Avoidance of Risky Substances
Studies on the Effect of Alcohol and Cigarette Smoking (Risky Substances) on Vasomotor Symptoms (VMS).
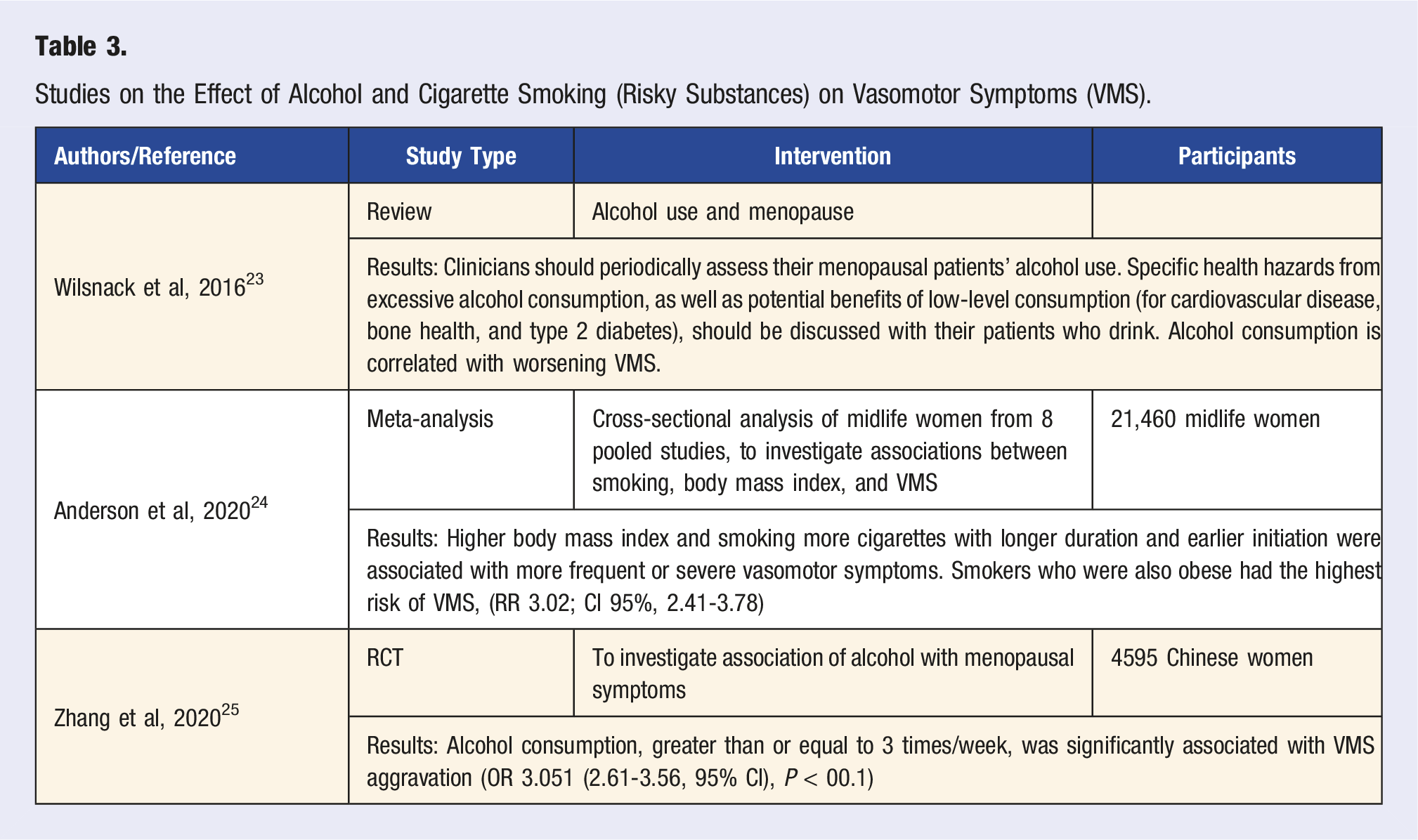
There are conflicting studies regarding positive, negative, or no association between the effects of alcohol and vasomotor symptoms. 23 Avoiding alcohol, along with other environmental triggers, is one lifestyle recommendation that may be helpful in the management of mild hot flashes. 26 However, the 2023 Non-hormonal Therapy position statement of the North American Menopause Society cites a 2020 Clinical Interventions in Aging study, which showed that menopausal women had a significant increase in vasomotor symptoms with alcohol consumption,24,25 but also observed that other studies did not show this association. 1 For those who do not drink alcohol, there is no recommendation to start, especially due to other health risks associated with excessive alcohol. 23
Current smoking and past smoking are associated with an increased risk of vasomotor symptoms, possibly due to the anti-estrogenic effects of smoking.
27
Smoking has been associated consistently with an increased incidence of hot flashes.
26
A pooled analysis of eight observational studies looking at the associations between body mass index, smoking, and potential effects on vasomotor symptoms noted significant interactions between BMI and smoking status for increased risk of vasomotor symptoms (
Restorative Sleep
The incidence of sleep disturbances (SD) a high during the menopause transition, around 43%-47%. 28 Poor sleep can lead to dysfunction both in the short term resulting in memory loss, attention deficits and decreased quality of life; and long term with more serious effects including a higher prevalence of diabetes, obesity, depression and increased mortality due to cardiovascular disease. 29 The causes of SD in menopause are still not fully known; however, a five-year retrospective follow-up study found risk factors including but not limited to vasomotor symptoms (80%), CNS medications, personal crises, anxiety, and depression. 30 Women who experienced surgical menopause compared to those who develop naturally were found to be more affected. 31
Hormone replacement therapy is the standard of care for evidence-based improvement of vasomotor symptoms, which can impair sleep quality; however, there is no direct evidence for treatment of sleep disorders. 32 Sleep apnea and sleep-disordered breathing increases in the perimenopause transition.
It is important for patients to work with their clinical team to exclude underlying sleep pathology, including treatment of associated anxiety, depression, or psychosis.33,34 Sleep hygiene is important which includes consistent bedtimes, early light exposure, and cooling bedding. 35 In addition, high fiber intake, especially in morning, 36 regular exercise, 37 and stress and mood management 38 have been shown to improve vasomotor symptoms and sleep in the menopausal transition, although causation should not be inferred. The addition of cognitive-behavioral therapy and maintaining healthy relationships also has a positive impact on quality sleep. In addition, avoidance of late-night meals, eating less processed foods, 39 and minimizing overall alcohol consumption has been shown to decrease sleep disturbances, but not VMS per se.40,41
Stress Management
Stress can directly impact menopausal symptoms by increasing the frequency and intensity of hot flashes and other symptoms, making the menopausal transition more challenging. 42 Managing stress is crucial as part of a comprehensive approach to menopausal symptom management, and many stress management techniques are available to help women cope with the physical and emotional challenges of menopause.
Studies on Stress Management and Vasomotor Symptoms (VMS).
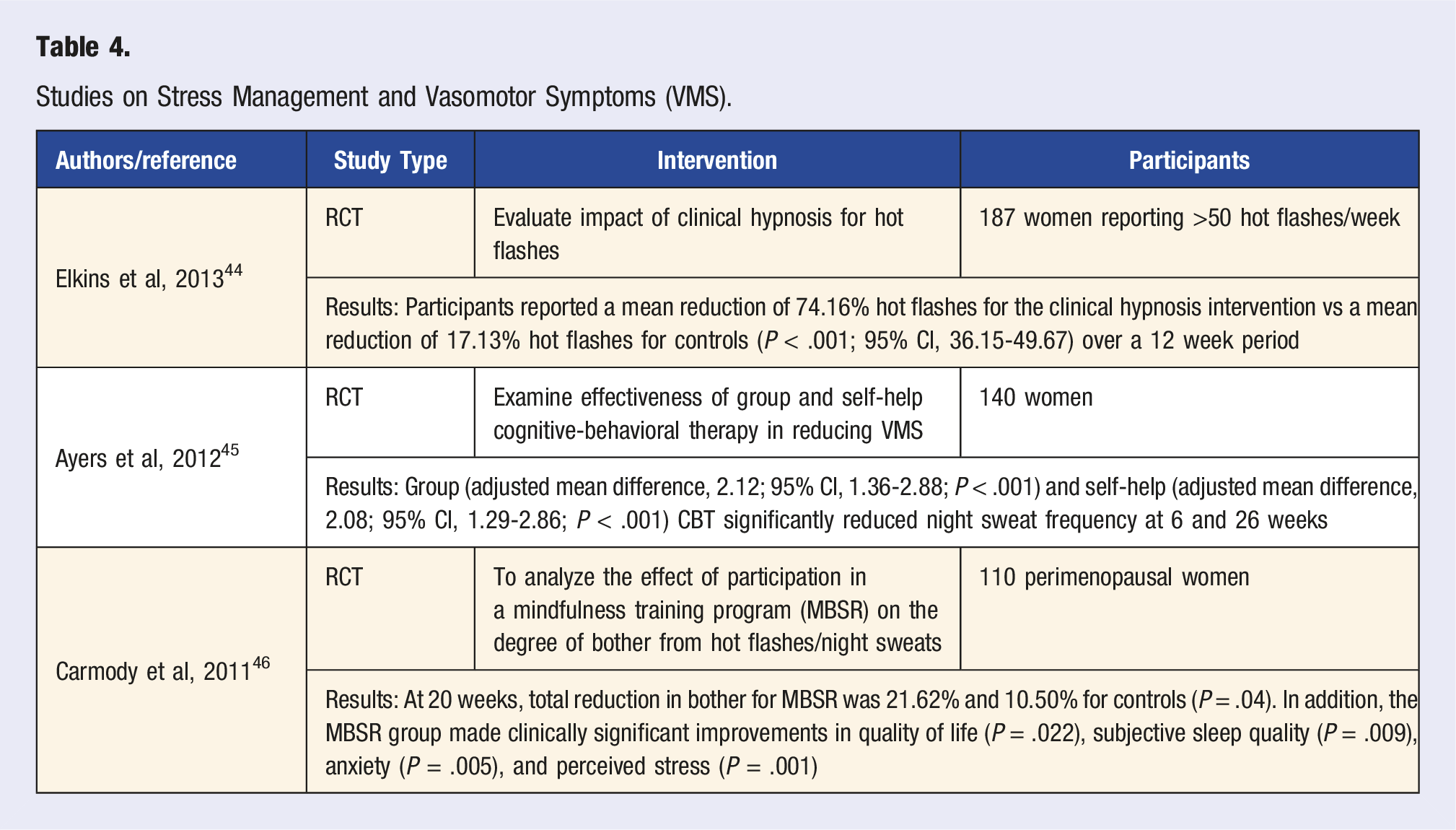
Structured stress management programs, which can effectively reduce stress and menopausal symptoms, should also be considered when creating a menopause management plan. While the NAMS 2023 position statement did not recommend yoga, relaxation, or mindfulness-based interventions, limited evidence exists for supporting mind-body therapies such as these overall during the menopause transition. One study found that a program combining mindfulness meditation, relaxation techniques, cognitive-behavioral therapy, and social support was effective in reducing perceived stress and menopausal symptoms in peri- and postmenopausal women. 45 In addition, a study examining the effect of mindfulness-based stress reduction for VMS demonstrated a 21.6% reduction in bothersome VMS vs 10.50% for controls. In addition, the MBSR group made clinically significant improvements in quality of life, subjective sleep quality, anxiety, and perceived stress. 46 These results suggest that a comprehensive approach to menopausal symptom management that includes structured stress management programs may significantly improve women’s well-being and quality of life during the menopausal transition beyond vasomotor symptoms alone.
Social Connection
The interaction between menopausal vasomotor symptoms and social connectedness is difficult to study and has little data, but is likely bidirectional. Menopause can be a time of social isolation for some women; moreover, negative attitudes towards menopause can lead to underreporting. In one study, 25% of women reported that vasomotor symptoms impacted quality of life through social embarrassment, physical discomfort, and disturbed sleep. 47 Not only can menopause lead to social disconnection, but lack or presence of social connectedness may also shape a woman’s experience of this period. For example, Asian women living in the UK attributed more symptoms to menopause compared with Asian women living in Delhi. In cultures where older women are held in high respect, generally fewer symptoms are reported. 48 There is evidence that strong social networks and higher social support may reduce symptom severity and frequency.49,50 Exactly how this happens is not well understood but may be hypothesized to be secondary to better health behaviors, less depression, and less stress. Conversely, other studies have not found that increased social support leads to reduced VMS or moderates the relationship between stress and its impact on such symptoms. 51
Physical Activity
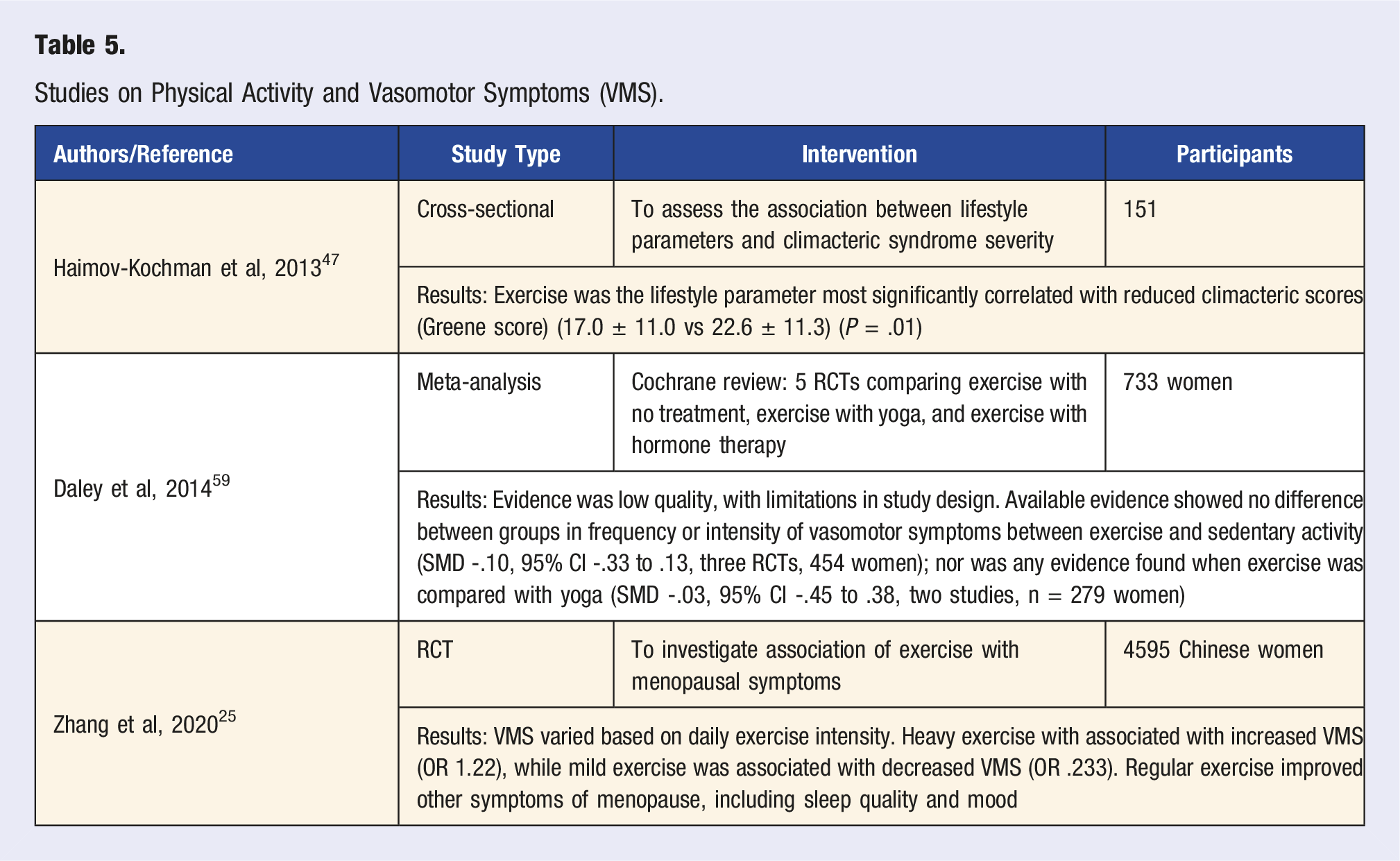
Physical activity and exercise are part of a healthy lifestyle and have accepted benefits for many menopausal concerns including cardiovascular risk, blood pressure control, osteoporosis, and mood. 52 Evidence on physical activity and exercise for vasomotor symptoms, however, is mixed.53–55 While there are some trials showing that aerobic and strength training exercise programs can decrease the frequency of hot flashes, other studies have linked higher levels of vigorous physical activity to a greater risk of hot flashes.52,54–56
Studies on Physical Activity and Vasomotor Symptoms (VMS).
Discussion
Lifestyle Pillars and Effects on Vasomotor Symptoms Recommendations.
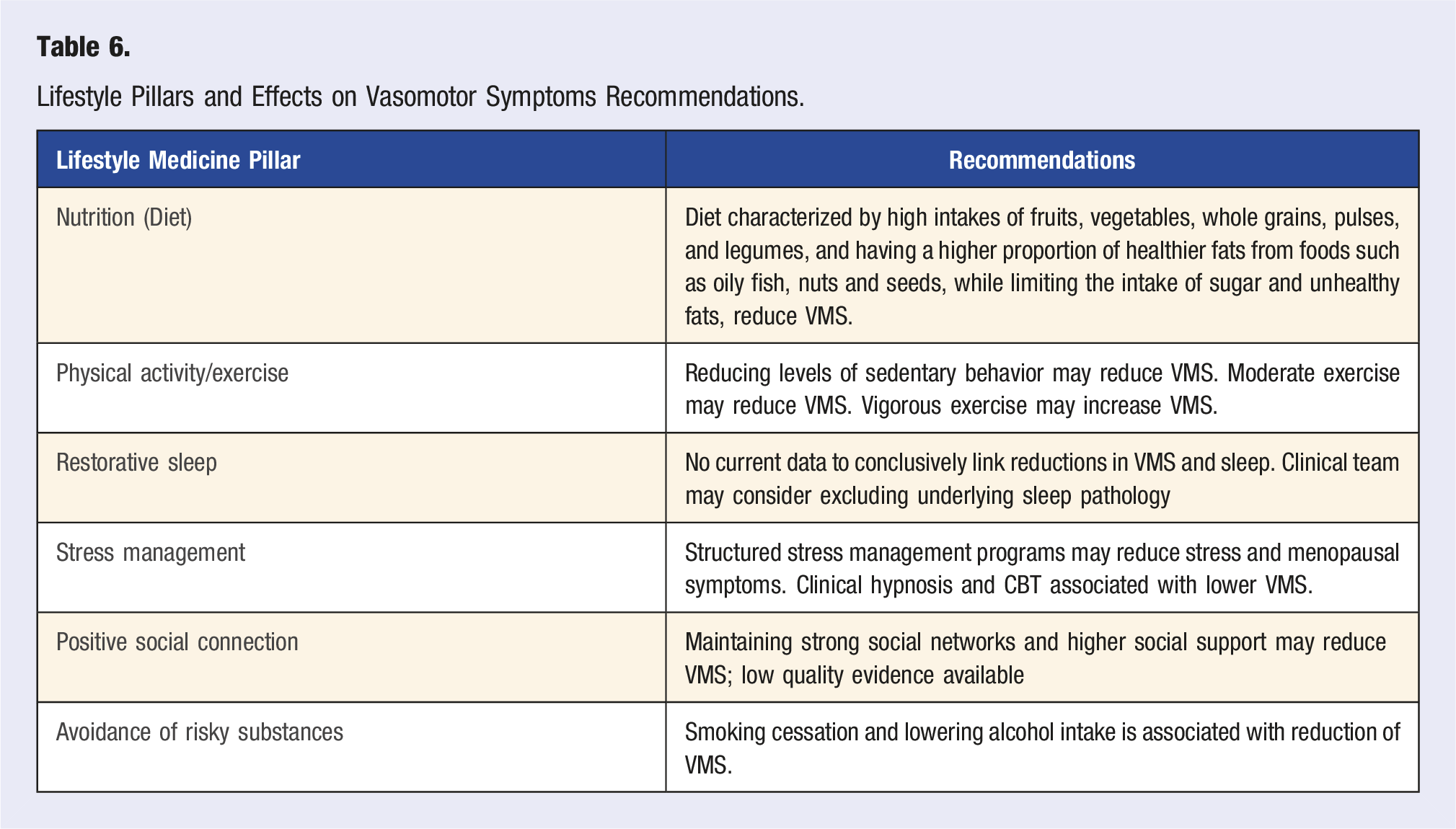
There was strong support for the reduction and/or avoidance of risky substances, particularly tobacco products, in reducing VMS. There was evidence that a Mediterranean-style plant-forward dietary pattern may effectively reduce vasomotor symptoms, specifically as it relates to weight loss (Table 1). There was a linear correlation observed for an increasing fiber and reduction in VMS, with the best results observed for a WFPB diet. Hot flushes were significantly inversely associated with consumption of soy products, and phytoestrogens reduced hot flash frequency compared to placebo (Table 2).14,17,60–62 Evidence exists most strongly for stress reduction via cognitive-behavioral therapy, and clinical hypnosis, with mixed evidence for mindfulness-based stress reduction and other mind-body techniques. While restorative sleep and positive social connections have been associated with longevity and successful aging, the evidence could not support specific recommendations regarding vasomotor symptom relief.
Conclusion
Vasomotor symptoms are a common feature of the menopause transition, and while hormone therapy is the first-line recommendation, women may not utilize this form of treatment due to medical contraindications or personal preference. This review found evidence that utilizing the pillars of Lifestyle Medicine may be an effective strategy to improving vasomotor symptoms in a nonpharmacologic approach. It should be explicitly stated that the scope of this paper is for vasomotor symptoms alone; all pillars of Lifestyle Medicine should be re-evaluated for other elements of menopause, including cardiovascular health, bone health, and longevity. Follow-up systematic reviews on a broader scope of health after the menopause transition using the pillars of Lifestyle Medicine would be an area of future interest for clinical practice and patient education. 63
Footnotes
Acknowledgments
The authors wish to thank Metropolitan State University of Denver students (now graduates) Andrea Musick and Olivia Till, who assisted with the initial literature searches, and Dr Martin Bonsangue, for proofreading and editing the manuscript.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
