Abstract
“Intentional weight loss, achieved through exercise and diet, in chronic stroke survivors may offer benefits for physical function and psychosocial outcomes.”
Introduction
With a surviving cohort of nearly 7 million individuals, stroke is the leading cause of long-term disability in the United States.1,2 Of the ∼795 000 new strokes occurring in the U.S. each year, 3 approximately two thirds of survivors will have some degree of long-term disability, and less than half will progress to independent community ambulation. 4 Even among those who do achieve independent ambulation, significant residual deficits persist, with more than 60% of persons post-stroke reporting limitations in mobility related to walking.3,4
Contemporaneously, obesity is highly prevalent in stroke survivors (∼30%-45% of stroke survivors have a BMI
In addition to the physical function impairments experienced by many stroke survivors, which can be compounded by obesity, this population also exhibits higher rates of depression and anxiety, with up to 50% experiencing depression and 33% experiencing anxiety post-stroke.21-23 These higher rates may be further increased in stroke survivors with obesity, as obesity is also associated with increased rates of depression and anxiety. 14 Weight loss achieved through multicomponent exercise and nutrition interventions promote improvements in depression, as well as physical function, in otherwise healthy individuals and clinical populations, including those with other neurological conditions.24-26 Still, the impact of weight loss on post-stroke psychosocial outcomes, as well as physical function, is largely unexplored.
With obese stroke survivors being such a large population at risk for long-term disability in the U.S., 1 establishing the efficacy of weight management to improve their mobility, independence, and quality of life is imperative to guide future directions of cardiovascular and stroke research and funding agencies and organizations. Therefore, the aim of this scoping review is to comprehensively review the available literature on the influence of intentional weight loss on physical function and psychosocial outcomes during rehabilitation of chronic stroke survivors.
Materials and Methods
This review protocol adheres to guidelines outlined within the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) guidelines. 27
Search Strategy
A comprehensive review of English-language literature published between January 2000 and April 2022, in peer-reviewed journals, was conducted using electronic medical databases (PubMed, EMBASE, and CINAHL). Articles were searched utilizing the following search syntax: ((“Body Composition” [Mesh] OR BMI) AND (Obese OR Obesity OR Overweight) AND ((“Stroke” [Mesh] OR (Ischem* AND Stroke)). Filters were applied to include only adult (18+ yrs old) and human research articles. The Cochrane library was explored for reviews utilizing the same key terms.
Study Inclusion Criteria
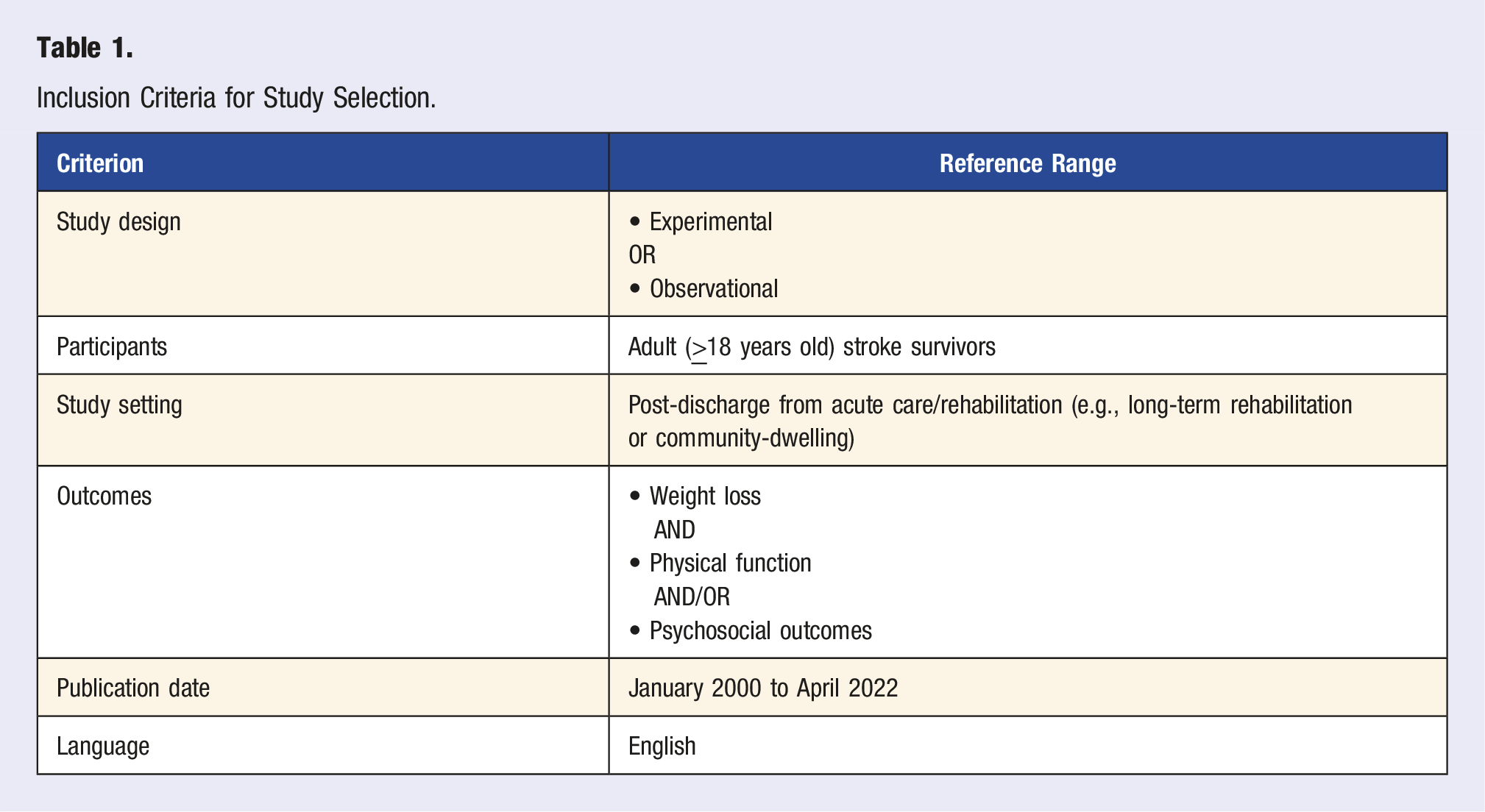
Inclusion Criteria for Study Selection.
Study Design
All experimental (randomized controlled trial, quasi experimental study, pre-post study, etc.) and observational (cross-sectional, longitudinal) study designs that met the other inclusion criteria below were included, due to the limited number of studies available on the present topic.
Participants
Studies with sample populations of stroke survivors ages 18 and above post-discharge from acute/subacute care and rehabilitation were included in the present study.
Study Setting
Given that the aim of this scoping review is to review the influence of intentional weight loss on outcomes in individuals with chronic stroke survivors, studies conducted in the acute setting were excluded.
Outcomes
Only studies that reported participant weight loss and at least one outcome measure of physical function (6-minute walk test, 1-minute sit-to-stand test, etc.) and/or psychosocial outcomes (depression, anxiety, quality of life) were included in the present study. Studies that reported weight loss that was unintentional (e.g., weight loss during acute hospitalization post-stroke) were excluded.
Study Selection
Two reviewers independently screened all titles (n = 376). Upon determination of potential eligible articles, subsequent abstracts (n = 37) were assessed for inclusion. Disagreements during abstract screening were resolved through unanimity conversation, resulting in n = 11 included for full-text review. Upon full-text review, n = 4 were included in the final review (Figure 1). Study Selection Flowchart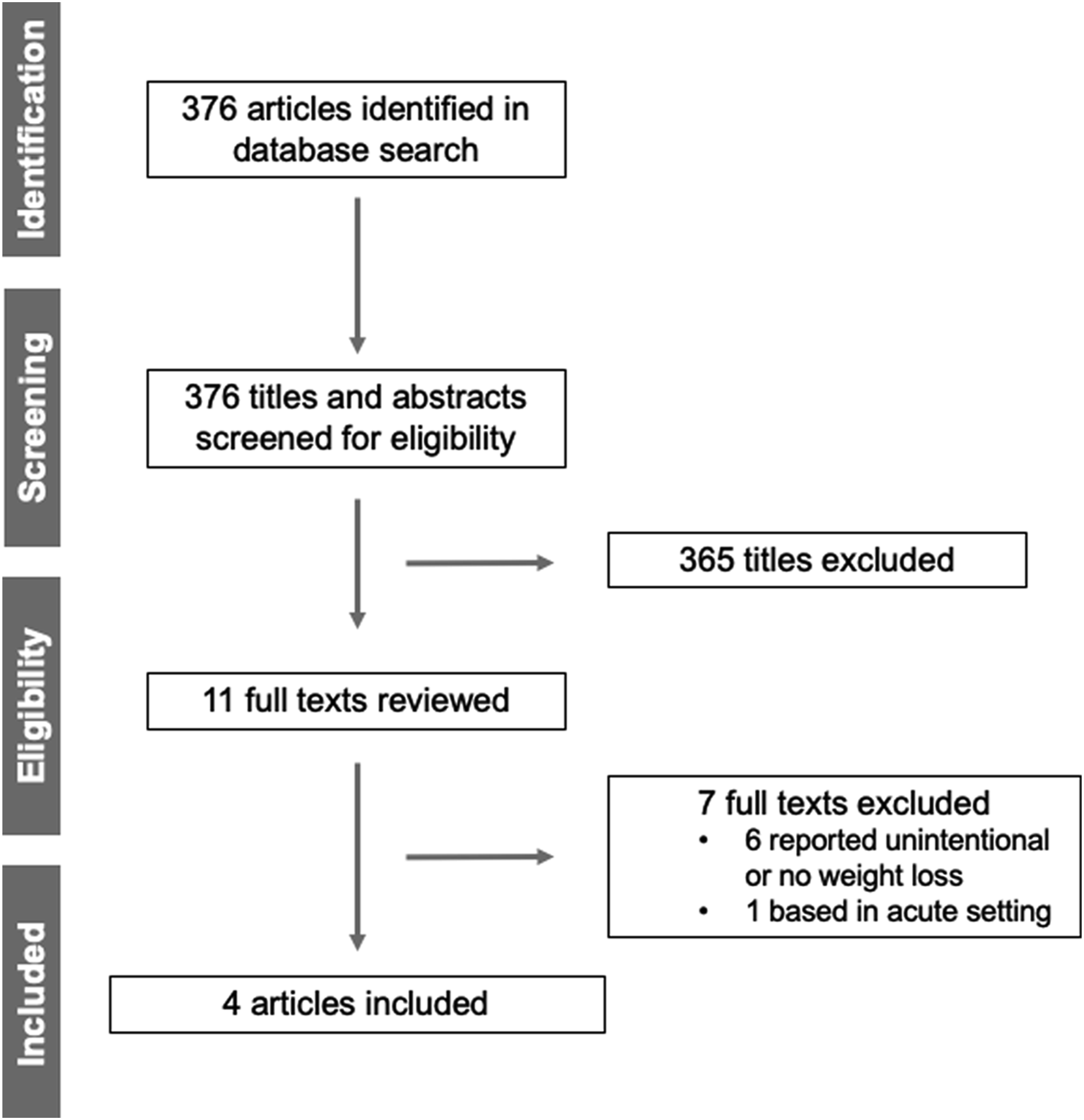
Data Extraction/Charting
A data extraction form was used to extract key information from the 4 articles included in the review (available upon request). The information extracted from each article included the sample size; mean age of the study sample, as well as age range if provided; baseline mean BMI; study design; study setting; intervention characteristics; outcome measures; and relevant results.
Collating, Summarizing, and Reporting the Results
Results of the included studies were grouped as (1) weight loss outcomes, (2) physical function outcomes, and (3) psychosocial outcomes.
Results
Study Characteristics
Characteristics of Included Studies.
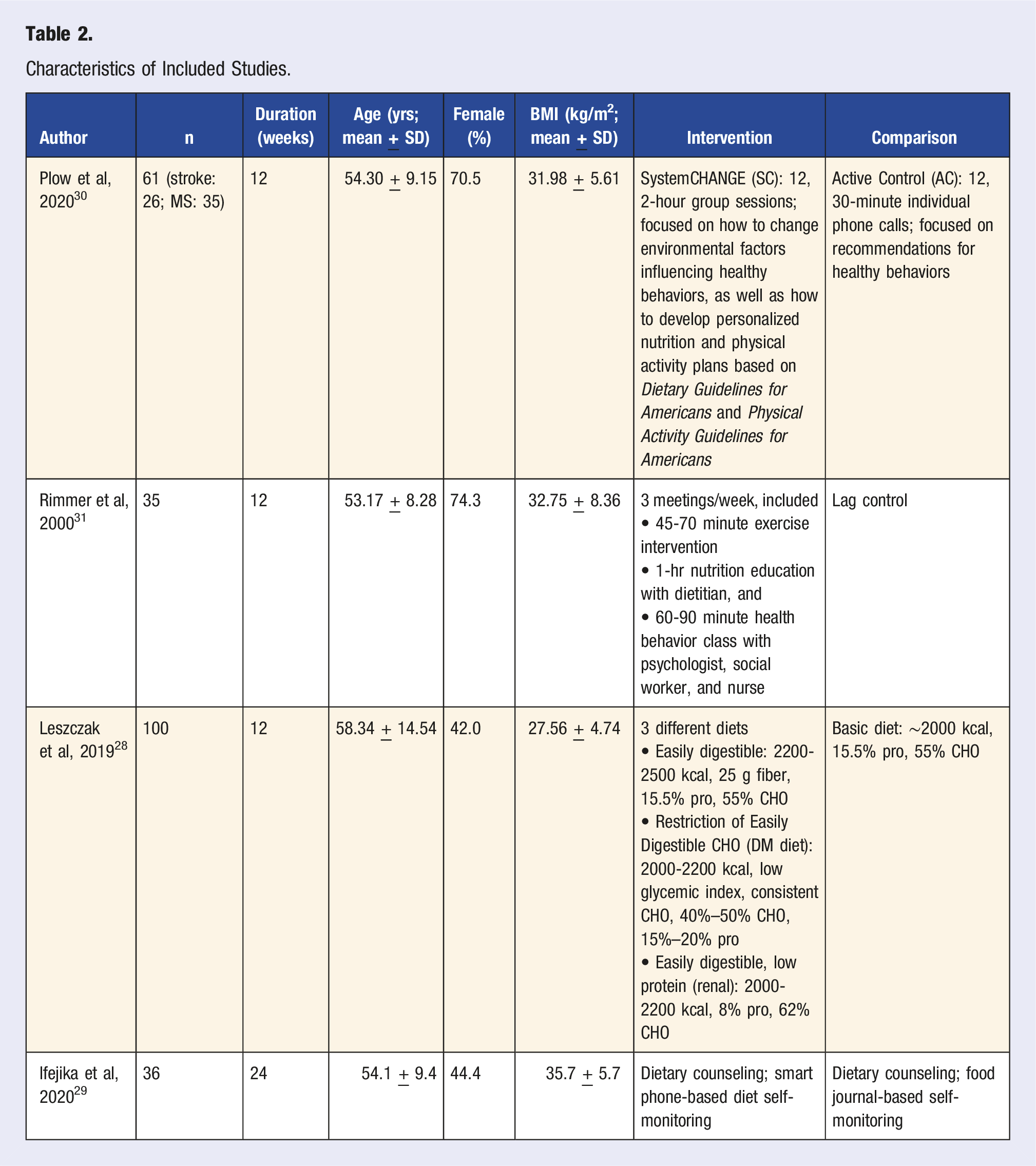
Nutrition, exercise, and behavior change strategies utilized in the interventions varied significantly. The duration of a majority of the interventions was 12 weeks,28,30,31 with only one intervention lasting 24 weeks. 29 Two interventions included both nutrition education/counseling and exercise classes/education,30,31 while two primarily focused on nutrition.28,29 Varying opportunities for social support and self-monitoring were offered to participants, including group classes and smart phone-based tracking with feedback and reminders.28-31 Only one study explicitly stated inclusion of education/counseling by registered dietitians, exercise physiologists, and other health professionals including psychologists. 31 Each intervention is detailed further in the sections below and in Table 2.
Weight Loss
Plow et al.’s single-blinded randomized controlled trial evaluated the influence of a weight management intervention on weight, physical function, and psychosocial outcomes in stroke survivors (n = 26) and individuals living with multiple sclerosis (MS; n = 35). 30 Participants (mean age 54.30 ≤ 9.15 yrs; mean BMI 31.98 ≤ 5.61 kg/m2) were randomized to two groups, a SystemCHANGE (SC) group or an active control (AC) group. 30 SC participants received twelve, weekly 2-hour group sessions that focused on changing environmental factors influencing their health behaviors. 30 SC participants also received education and training on developing personalized nutrition and physical activity plans based on U.S. guidelines (Dietary Guidelines for Americans and Physical Activity Guidelines for Americans). 30 The AC group received twelve, weekly 30-minute individual phone calls with study staff that provided brief education on U.S. nutrition and physical activity guidelines. 30 Weight significantly decreased in the SC group (SC: pre = 87.19 ≤ 14.93 kg, post = 84.78 ≤ 14.39 kg; AC: pre = 93.26 ≤ 16.50 kg, post = 94.02 ≤ 15.73 kg), though there was no difference between groups. 30 Unfortunately, results of this study were not stratified by stroke/MS, limiting interpretation of the following results. Still, due to the limited number of relevant studies on the present topic, the authors felt this study worth including.
Rimmer et al utilized a crossover trial to evaluate the effect of a 12-week health promotion intervention on weight loss, physical fitness and function, and psychosocial outcomes in stroke survivors (n = 35). 31 Participants (mean age 53.17 ≤ 8.28 yrs; mean BMI 32.75 ≤≤ 8.36 kg/m2) were randomized to two groups, the intervention or control group. 31 Stroke survivors in the intervention group participated in 3 meetings per week for 12 weeks, with each meeting including 45-70 minutes of structured exercises, as well as nutrition education and health behavior change strategies. 31 Participants randomized to the control group were enrolled in the intervention following completion of the control period. 31 Stroke survivors in the intervention group lost a small but significant amount of weight over the course of the intervention (mean weight loss = 2.8 lbs, P < .01), while stroke survivors in the control group did not lose a significant amount of weight. 31
Leszczak et al evaluated changes in BMI, fat mass, visceral fat mass, muscle mass, activities of daily living (ADLs), upper and lower limb movement (as measured by the Brunnstrom Scale), and muscle tone (as measured by the Ashworth Scale) in stroke survivors (n = 100) placed on four different diets for disease management. Results were collected at three timepoints: (1) at the time of admission to subacute inpatient rehabilitation, (2) at the time of discharge from subacute inpatient rehabilitation, and (3) 3 months post-discharge from subacute inpatient rehabilitation. 28 Participants (mean age 58.34 ≤ 14.54 yrs; mean BMI 27.56 ≤ 4.74 kg/m2) were placed on one of four diets, (1) basic diet (∼2000 kcal, 15.5% protein [PRO], 55% carbohydrate [CHO]), (2) easily digestible diet (2200-2500 kcal, 15.5% PRO, 55% CHO, 25 g fiber), (3) restriction of easily digestible CHO diet for diabetes (2000-2200 kcal, 15%-20% PRO, 40%-50% CHO [consistent CHO], low glycemic index), and (4) easily digestible, low protein diet for renal disease (2000-2200 kcal, 8% PRO, 62% CHO). 28 No between-group differences were observed, likely due to the similar total caloric and macronutrient content of the different diets. 28 However, when groups were combined, BMI, fat mass, and visceral fat mass significantly decreased over time. 28
Ifejika et al evaluated changes in weight, BMI, and depression, as measured by the Patient Health Questionnaire-9 (PHQ-9), among stroke survivors (n = 36; mean age 54.1 ≤ 9.4 yrs; mean BMI 35.7 ≤ 5.7 kg/m2) randomized to either a smart phone-based self-monitoring intervention or a food journal-based self-monitoring intervention. 29 Both groups received nutrition counseling. 29 Both groups lost a significant amount of weight over time (smart phone group: 2.1% weight loss; food journal group: 2.9% weight loss), though there was no significant difference in weight loss between groups. 29
Physical Function Outcomes
Three studies reported physical function outcomes. Plow et al evaluated physical function changes with the 1-minute sit-to-stand test and the 6-minute walk test. 30 Some changes in 1-minute sit-to-stand (SC: pre = 11.02 ≤ 5.50, post = 11.05 ≤ 4.72; AC: pre = 10.98 ≤ 3.08, post = 11.78 ≤ 2.66) and 6-minute walk tests (SC: pre = 970.96 ≤ 415.31, post = 1006.24 ≤ 575.43; AC: pre = 844.48 ≤ 450.10, post = 998.68 ≤ 408.97) occurred in the two groups. However, the AC group had significantly greater improvements than the SC group over time (P = .010), with Cohen’s d effect size of the AC compared to SC intervention being -.37 and -.20 for the 1-minute sit-to-stand and 6-minute walk tests, respectively. 30 In addition, time spent in physical activity significantly improved following the intervention in both groups (P = .004), with the SC group having significantly greater improvements than the AC group (P = .002). 30
Rimmer et al.’s intervention group significantly improved in several measures of physical fitness and function, including bench press (pre = 26.92 ≤ 17.25 lbs, post = 39.80 ≤ 24.44 lbs, P < .001), leg press (pre = 152.15 ≤ 74.11 lbs, post = 240.50 ≤ 73.32 lbs, P < .001), and flexibility as measured by the sit and reach test (pre = 9.22 ≤ 12.36 in, post = 17.20 ≤ 9.75 in, P < .001). 31 The control group did not make significant improvements in any of these measures. 31 While both groups improved their time to exhaustion (intervention: pre = 320.13 ≤ 159.23 sec, post = 431.35 ≤ 182.24 sec, P < .001; control: pre = 258.53 ≤ 128.17 sec, post = 311.76 ≤ 130.15 sec, P < .03), stroke survivors in the intervention group improved their time to exhaustion significantly more than stroke survivors in the control group. 31
While Leszczak et al observed significant decreases in BMI, fat mass, and visceral fat mass when their diet groups were combined, muscle mass also significantly increased. 28 It is important to note that these changes primarily occurred while patients were in subacute, inpatient rehab; and the changes were at least partially maintained 3 months post-discharge. 28 Significant improvements in function fitness of the upper limb (P = .0145), as well as hand (P = .0292) and upper limb (P = .0099) muscle tone, occurred. 28
Psychosocial Outcomes
Three studies reported psychosocial outcomes. Plow et al reported depression, anxiety, fatigue, and positive affect and well-being scores using the Neuro-QOL short-form measure, in addition to weight loss and physical function outcomes. 30 Participants in the SC group reported significant improvement in depression (P < .001) and anxiety (P = .023) symptoms following the SC intervention, compared to participants in the AC group. 30 Significant differences between groups or over time were not observed in fatigue or positive affect and well-being scores, however. 30
Rimmer et al reported life satisfaction, as measured by the Life Satisfaction Questionnaire (LSQ), and depression as measured by the depression subscale of the Symptom Check List-90 Revised (SLC-90R). 31 Stroke survivors in the intervention group significantly improved on six of the nine measures in the LSQ, including life as a whole, ability to manage self-are, leisure situation, sexual life, relations with significant other, and friends/social relations. 31 Stroke survivors in the control group improved in only one of the nine LSQ measures (sexual life). 31 Intervention participants also significantly improved in five of the thirteen measures in the SLC-90R, including feeling low in energy or being slowed down, feeling trapped or caught, feeling blue, feeling no interest in things, and feeling everything is an effort. 31 The control group did not significantly improve in any SLC-90R measures. 31
Interestingly, in Ifejika’s RCT, stroke survivors that screened positive for depression at baseline lost less weight (3.9 lbs) than those who screened negative for depression (6.4 lbs), though this difference was not significant. 29 The smart phone group reported significantly lower depression scores on the PHQ-9 after 30 days of the intervention compared to the food journal group (P = .03). 29
Discussion
Available research on the influence of intentional weight loss on physical function and psychosocial outcomes during rehabilitation of obese chronic stroke survivors is limited and variable in nature. Still, this review suggests physical function and psychosocial benefits of weight loss with participation in weight management lifestyle programs in chronic stroke survivors.28-31 All studies reported significant weight loss and/or improvement in body composition among chronic stroke survivors that participated in a lifestyle intervention.28-31 In addition, all studies reported significant improvements in at least one measure of physical function, psychosocial outcomes, or both.28-31
An obesity paradox has been observed in stroke survivors, in which individuals with obesity have lower mortality rates in the acute phase following stroke; yet, obesity is a known risk factor for stroke incidence.32,33 This observation may have contributed to the limited exploration of the efficacy of obesity treatment in stroke survivors to date. Yet, it is important to consider the limitations surrounding the obesity paradox, including its observation in the acute phase only, reliance on BMI as the measure of obesity, and the observational nature of the studies on which the paradox is based. 33 Furthermore, while unintentional weight loss during acute stroke rehabilitation seems to be associated with negative health-related outcomes, including decreased independent ambulation,34-36 these results cannot be extrapolated to chronic stroke survivors participating in intentional weight loss interventions that may incorporate nutrition and physical activity components. Unintentional weight loss during acute rehabilitation is an indicator of muscle mass loss and protein-energy malnutrition,37,38 potentially explaining the negative effects of this form of weight loss in stroke survivors. Conversely, intentional weight loss achieved through evidence-based nutrition and physical activity guidelines typically does not result in the significant decreases in muscle mass and may even result in increased muscle mass.11-13,20
Notably, the suggested negative influence of obesity on physical function and psychosocial factors of chronic stroke survivors is consistent with findings in acute and subacute populations.39-41 Kalichman et al observed BMI to be negatively associated with improvement in physical function in subacute rehabilitation of stroke survivors, with obese stroke survivors having poorer rehabilitation outcomes than normal weight or even overweight patients.18,19 In addition, Zhu et al reported a significant association between abdominal obesity and post-stroke anxiety in stroke survivors during the acute phase. 42 Importantly, the finding that weight loss, though modest, was associated with changes in physical and psychosocial function among stroke survivors in the studies included in this review are encouraging. Still, the magnitude of weight loss reported in these studies (e.g., 1%-2%) is much less than is typically targeted in weight loss studies in other populations (e.g., 5%-10%).11-13,20 It is possible that the observed improvements in physical function and psychosocial outcomes of the included studies were not due to the minimal weight loss achieved during the interventions. This limitation again highlights the need for more research to determine the role of intentional weight loss, achieved through effective exercise and nutrition interventions, on long-term stroke rehabilitation outcomes.
As part of future research endeavors, intensive multicomponent lifestyle interventions that are more consistent with weight management intervention guidelines11-13 are needed to elucidate the relationship between weight loss, physical function, and psychosocial factors of stroke survivors. Among the studies included in this review, significant variation was present in the included self-management strategies, such as weight, physical activity/exercise, and diet self-monitoring; problem solving; and social support. In addition, the duration of each included study was significantly shorter than the minimum 6-month duration recommended for intensive lifestyle interventions.11-13 The degree of education and training participants received by registered dietitians and exercise physiologists also varied significantly among the included studies. While the aim of this review was simply to establish the current evidence on the relationship between intentional weight loss, physical function, and psychosocial outcomes, these considerations are important for the design of future research initiatives, funding opportunities, and studies investigating weight loss in chronic stroke survivors.
Though not an aim of this scoping review, weight loss interventions are likely to influence other disease risk factors in addition to weight alone, and these factors are important to consider in addition to weight to provide clinicians with a more complete picture of stroke survivors’ health status and disease risk. Rimmer et al observed a significant decrease in total cholesterol (TC) in weight loss intervention participants, while the control group experienced a significant increase in TC. 31 Plow et al and Ifejika et al did not report significant changes in any biochemical markers, possibly due to the small sample size of these studies.29,30 Interestingly, none of the included studies reported blood glucose levels, which would provide further insight on the influence of the weight management interventions on risk of chronic conditions like T2DM. Still, considering that as little as 2% weight loss can result in clinically meaningful reductions in blood glucose, it is possible that participants that achieved this level of weight loss experienced blood sugar management benefits. 11 Future research on weight loss in stroke survivors should evaluate the influence on biochemical disease risk factors, in addition to physical function and psychosocial outcomes.
Limitations
The primary limitation of this scoping review is the extremely limited number of studies (only four) available to be included, and the significant variability in their methods, aims, and reported outcomes. In addition, the studies available did not associate the weight loss achieved with the physical function or psychosocial outcomes measured. Furthermore, the weight loss achieved in the included studies was very minimal; and, it is possible that the physical function and psychosocial improvements observed were not due to weight loss. While the limited number of studies may suggest a positive influence of weight loss achieved through exercise and/or nutrition, it is possible that other studies have shown no influence or a negative influence of weight loss on physical function and psychosocial factors of stroke survivors yet are not available due to publication bias. Further research is needed to understand the influence of weight loss on physical and psychosocial function in stroke survivors, as well as what intervention components (exercise, nutrition counseling/dietary factors, behavioral strategies) are necessary to achieve positive outcomes.
Clinical Implications
Unlike in the acute rehabilitation phase, weight management interventions in obese stroke survivors may offer benefits for physical function and independent living, as well as psychosocial factors and quality of life. As in other populations with obesity, incorporation of both exercise and nutritional programming led by trained exercise physiologists and registered dietitian nutritionists are likely key components to optimize outcomes of weight management interventions in long-term rehabilitation of stroke survivors. Due to the varying abilities of stroke survivors for different exercise intensities, further investigation into exercise protocols based on functional ability is likely warranted. In addition, following weight management guidelines12,13 for intervention length (i.e., 6 months or longer) and behavior change strategies, including social support, goal setting, and self-monitoring of weight, diet, and physical activity, may result in more clinically meaningful weight loss than was achieved in the included studies.
In light of the strikingly few studies published on the topic of weight loss in obese stroke survivors, an undeniable clinical implication of this review is to bring attention to this gap in the care of stroke survivors. While there is extensive attention on obesity treatment interventions among the general population, little attention by research organizations and funding agencies is currently placed on this topic in stroke survivors. With a large cohort of stroke survivors in the U.S. and obesity rates being potentially higher (up to 45%) 5 in this population compared to the general population (approximately 42%), 13 efforts to address obesity will be limited without attending to this population. Furthermore, as discussed throughout this review, weight loss in stroke survivors requires additional considerations to prevent loss in physical function observed with unintentional weight loss in this population. Thus, we cannot assume that the evidence base for effective weight management interventions in the general population can be extrapolated to the clinical population of stroke survivors, again calling for further exploration into this topic by researchers and clinicians.
Conclusion
Intentional weight loss, achieved through exercise and diet, in chronic stroke survivors may offer benefits for physical function and psychosocial outcomes. However, current research is highly limited and variable in design; and, further research is imperative to determine the efficacy of weight loss interventions for physical and psychosocial function in chronic stroke survivors. Until this issue is prioritized on the agendas of health agencies and organizations, the quality of conclusions that can be derived from disconnected, individual research studies on weight management for physical function, psychosocial, and other health benefits will likely remain inconclusive.
Footnotes
Declaration of Conflicting Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
