Abstract
In looking for solutions to the COVID-19 pandemic, important lessons come from the H1N1 influenza pandemic of 1918–1919. During the H1N1 influenza pandemic, the soldiers had better outcomes than the civilian populations, but the best outcomes were reported by a Seventh-day Adventist seminary, where a plant-based diet was provided. The diet has been described as including grains, fruits, nuts, and vegetables. A few clinical trials have also assessed the role of nutrition in COVID-19. One study with almost six hundred thousand participants showed that those with a high consumption of fruits and vegetables had a reduced risk of COVID-19 of any severity by 9% and a reduced risk of severe COVID-19 by 41%. Another study in healthcare workers who were frequently exposed to COVID-19 in their clinical practice has demonstrated that those who reported being on a plant-based diet had a 73% lower risk of moderate-to-severe COVID-19. Based on the lessons from 1918 and the recent nutrition research in COVID-19, it seems plausible that a healthful plant-based diet may be a powerful tool to decrease the risk of severe COVID-19 and should be promoted as one of the public health safety measures.
Evidence supports the possibility that good nutrition can support immune function and may play an important role in resistance to the sequelae of infection.
Background
In looking for solutions to the COVID-19 pandemic, important lessons come from the H1N1 influenza pandemic of 1918–1919. Although COVID-19 appears to spread more rapidly and to have a lower fatality rate compared with H1N1 influenza, 1 both are viral respiratory infections for which human populations had no pre-existing immunity.
The H1N1 Pandemic and the Potential Role of Nutrition
The H1N1 influenza (“Spanish flu”) pandemic started in March 1918 and led to serious challenges in military personnel mobilized for World War I. Many soldiers reported acute symptoms, including cough, respiratory distress, chills, body aches, and high fever. About 20–40% of soldiers in the U.S. Army camps developed the infection. 2 In the fall of 1918, the disease started spreading to the civilian population. 3 It is estimated that about 500 million people or one-third of the world’s population became infected with this virus. Deaths were estimated at more than 50 million worldwide, 4 with about 675 000 in the United States.
Comparing figures from the Army and civilian populations, it appears that soldiers had better outcomes. Of those infected, 17% developed pneumonia. Of those with pneumonia, 40% died. The fatality rate was 6.7%, well below the worldwide average, presumably due to younger age, better overall fitness, better access to medical equipment, and higher standards of care in the military.2,3,5
A curious report of particularly good outcomes came from a seminary in Minnesota, housing 120 faculty and students, of whom 90 developed influenza symptoms. Surprisingly, none progressed to pneumonia and none died, despite the fact that there were no effective pharmacologic treatments at the time (Figure 1). Cases of H1N1, Pneumonia, and Deaths in the U.S. Army, Adventist Sanitarium Outpatient, and Inpatient Clinic.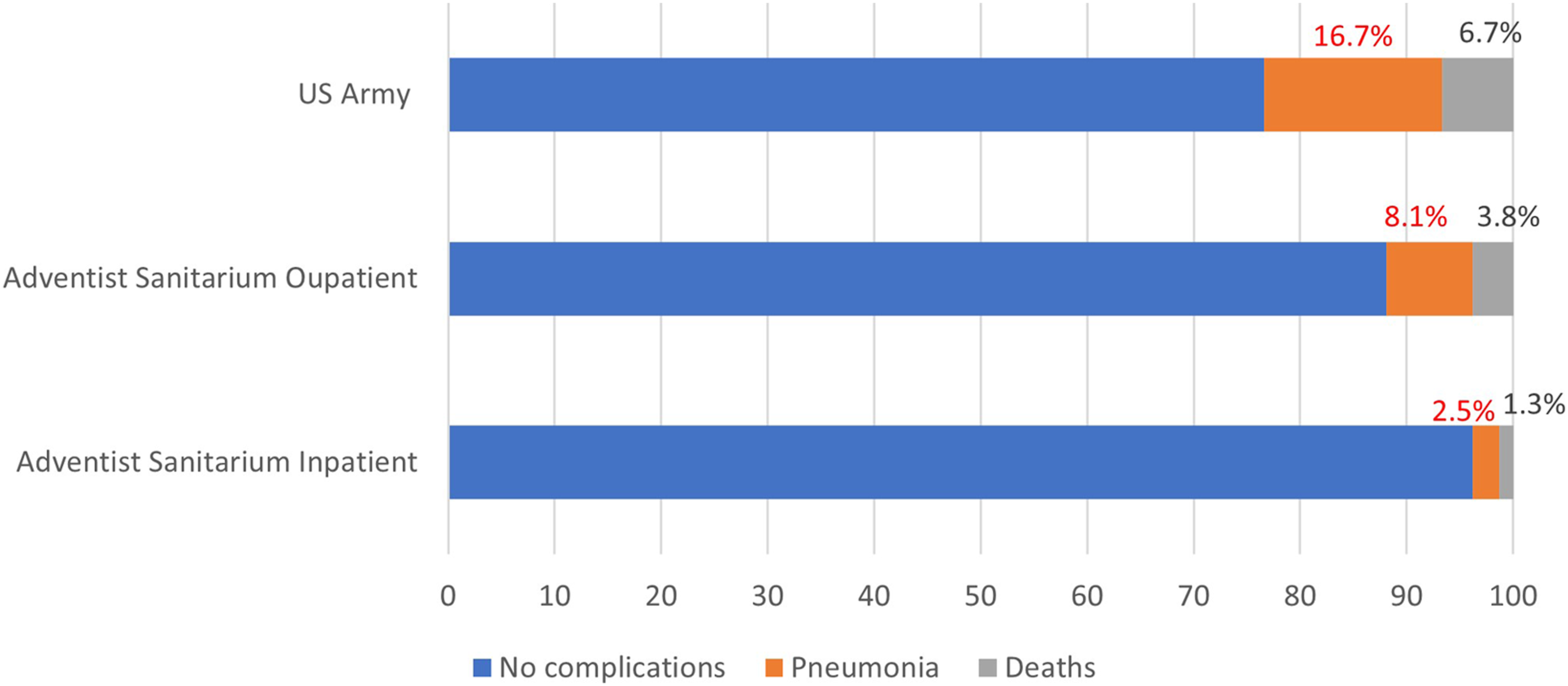
According to a newspaper account published December 17, 1918, the seminary asked infected patients to rest in bed and apply warm soaks to the throat and chest. It seems plausible that the habitual dietary practices at the seminary may have contributed to better influenza outcomes. As a Seventh-day Adventist seminary, a plant-based diet was provided. 6 The diet has been described as including grains, fruits, nuts, and vegetables, which are foods rich in fiber and antioxidants. It was particularly rich in vegetables and fruits, which may influence immunity. The report from the Adventist seminary concluded: “… there has not been one case that could have been called serious or a single death in the Seminary although there were more than 90 persons affected. The record is remarkable. It makes the ordinary methods of dealing with the flu appear irrational.” 6
Other religious facilities using the same approach had remarkably good outcomes in treating influenza. In the article “Sanitarium Treatment of Influenza,” published in the journal Life & Health in May 1919, the outcomes from 1123 influenza patients treated by 10 Adventist sanitariums were compared with the outcomes reported by the US Army. Of 677 people in the adjacent communities who came to the sanitariums on an outpatient basis, 8.1% developed pneumonia and the fatality rate was 3.8%. Among 446 nurses, employees, and regular patients of the sanitariums, 2.5% contracted pneumonia, and the fatality rate was 1.3%—one-fifth of that in the U.S. Army. 5 The treatment outcomes are summarized in the chart.
Nutrition and COVID-19
A few observational studies have assessed the role of nutrition in COVID-19. One study with almost six hundred thousand participants showed that those with a high consumption of fruits and vegetables had a reduced risk of COVID-19 of any severity by 9% and a reduced risk of severe COVID-19 by 41%. 7 Another study in healthcare workers who were frequently exposed to COVID-19 in their clinical practice has demonstrated that those who reported being on a plant-based diet had a 73% lower risk of moderate-to-severe COVID-19. 8
Potential Mechanisms
Several potential mechanisms may explain beneficial effects of a plant-based diet rich in fruits and vegetables on infectious diseases, including the H1N1 influenza or COVID-19. A 2012 randomized clinical trial in 83 healthy volunteers (age 65–85 years) showed that eating 5 or more servings of fruits and vegetables a day for 16 weeks led to almost 2 times higher titers of antibodies against the pneumovax II vaccine compared with eating 2 or fewer daily portions of fruits and vegetables. 9
Plant foods rich in nitrates, particularly dark green leafy vegetables, increase the production of nitric oxide, 10 which plays a key role in cardiovascular health and cellular defense mechanisms. 11 Nitric oxide has inhibitory effects on the replication of the influenza virus 12 and also on the SARS coronavirus. 13 Several studies have suggested that diets rich in antioxidants and phytochemicals may improve immune defenses and aid in the prevention and treatment of respiratory tract infections.14–16
Summary
Based on the lessons from 1918 and the recent nutrition research in COVID-19, evidence supports the possibility that good nutrition can support immune function and may play an important role in resistance to the sequelae of infection. Adopting a healthful plant-based diet may be a powerful tool to decrease the risk of severe COVID-19 and should be promoted as one of the public health safety measures.
Footnotes
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr. Kahleova works at the Physicians Committee for Responsible Medicine. Dr. Barnard serves without financial compensation as president of the Physicians Committee for Responsible Medicine and Barnard Medical Center, nonprofit organizations providing education, research, and medical care related to nutrition. He writes books and gives lectures related to nutrition and health and has received royalties and honoraria from these sources.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was funded by the Physicians Committee for Responsible Medicine.
