Abstract
In an era of ever-increasing healthcare expenditures, yet simultaneously worsening outcomes, many of our patients choose between traditional medical care or often unproven alternative therapies. While the recognition of lifestyle change in addressing cardiovascular and metabolic disease grows, there is less understanding of the impact of lifestyle change on issues facing women every day. Millions of women around the globe struggle with infertility, cancer, sexual dysfunction, and dermatologic needs. Yet, research on the benefits of lifestyle change on these conditions is scarce, and gaps exist both in our understanding of evidence-based approaches to address these issues, as well as adequate provider education when evidence exists. The Women’s Health Member Interest Group convened medical experts in these areas that affect women’s lives to provide insights and meaningful education applicable not only for our patients, but also in our own lives.
Introduction
Lifestyle medicine recognizes that healthy behaviors, starting with self-care, eating a high-fiber diet rich in plant-based foods, getting adequate movement, avoiding risky substances, attending to sleep and stress, and engaging with others, are the foundations of health: improving the prevention and management of disease, as well as benefiting overall wellbeing and vitality. Despite rising healthcare expenditures, for the first time in American history (even before the current pandemic), life expectancy is falling.
Frustrated by worsening outcomes at higher costs, our patients' search for alternative approaches to health is understandable. In 2012, Americans spent over $30 billion out of pocket on visits to complementary healthcare practitioners and on purchases of products related to this care. 1 Many of these treatments are of questionable benefit and may even cause harm. Despite this understandable quest for improved health, a recent study found that only 2.7% of Americans met the 4 core lifestyle-related characteristics associated with low risk of chronic disease (healthy diet, recommended body fat percentage, non-smoking status, and recommended exercise). 2 As we continue to have both an unhealthy lifestyle and an ever-expanding array of lifesaving medical care, the number of Americans surviving with chronic conditions continues to increase.
In 2019, 16.9 million individuals with a history of cancer resided within the United States. 3 Cancer survivors may benefit greatly from lifestyle change that may both lower risk of recurrence and also improve overall wellbeing, yet all too often, patients and providers are not well informed of the foundational importance of lifestyle medicine and instead focus on traditional medical approaches. Frustrated patients may then turn to unproven and potentially harmful alternative approaches, and healthcare providers are ill equipped to answer patients’ inquiries of both lifestyle and integrative approaches.
Infertility is another common concern, affecting millions of couples, with global spending on infertility projected to rise to $45 billion by 2027. 4 While lifestyle factors impact fertility for both men and women, the focus in medicine has primarily been on costly treatments, which not only have potential risks, but also lead to profound disparities in access to care for individuals and couples with fewer financial resources.
In addition, the global wellness economy is now valued at 4.5 trillion dollars, with the largest expenditure in the personal care, beauty, and anti-aging sector. 5 A recent survey estimated that the average American woman spends $225,360 on skin care products over a lifetime, far in excess of the average American’s total retirement savings. 6 Sexual health concerns for women are highly prevalent, with 43% of American women reporting sexual problems in a 2008 survey. 7 Increasing evidence supports the importance of lifestyle factors on both skin and sexual health, which may be motivators for patients to engage in behavior change that can have long reaching benefits on other health risks as well.
To address this lifestyle medicine knowledge gap, we highlight specific research findings that demonstrate the positive impact of healthy lifestyle recommendations on fertility, hormonal health, sexual health, and dermatological conditions. The purpose of congregating lifestyle-focused medical experts’ opinions and work is to better equip practitioners with credible scientific evidence for future patient education dialog and increase leverage amongst colleagues and health administrators in various healthcare systems.
Fertility and Preconception Health
Within the realm of reproductive and sexual health, the positive potential of lifestyle medicine (LM) and its 6 pillars of health—healthful eating, social connectedness, avoidance of toxic substances, and sufficient sleep, physical activity, and stress management—as a primary modality, delivered by trained clinicians occurs at the physiological level generating positive health outcomes. 8 There is a need for robust research to demonstrate a dose relationship of lifestyle medicine factors on preconception health and fertility.
Data on lifestyle during the preconception phase have repeatedly demonstrated inconsistent folic acid supplementation, uneven access to preconception counseling, and ongoing consumption of cigarettes, marijuana, or excessive alcohol. 9 On a national level, rates of unhealthy eating patterns, overweight and obese BMI or sedentary behavior, as well as of poor sleep, anxiety, and depression, continue to rise.10-13 Each of these habits or diagnoses raises the risk of infertility or obstetric and post-partum complications. A large systematic review and meta-analysis demonstrated that preconception lifestyle interventions, ranging from individual counseling from a physician to comprehensive multidisciplinary interventions, can significantly increase the natural pregnancy rate. 14
Polycystic ovary syndrome (PCOS) is a specific diagnosis frequently characterized by ovulatory dysfunction causing infertility, and it is a risk factor for insulin resistance, gestational diabetes, and type 2 diabetes. Those with PCOS who have not undergone appropriate preconception counseling often miss a critical window for evaluation of glycemic control and, therefore, are at risk for metabolic dysfunction and have increased risk of obstetric complications that can result in lifelong metabolic sequelae for the child.
The Reproductive Medicine Network has demonstrated that a comprehensive lifestyle evaluation can result in a significantly higher ovulation and live birth rate than oral contraceptive pills, and even that delaying pregnancy to improve preconception lifestyle can result in the same for obese women with PCOS, when compared to proceeding straight to treatment.15,16 As such, PCOS offers a clear example of how an LM approach to preconception care can enhance fertility as well as improve obstetric, pediatric, and public health outcomes.
However, even with infertility secondary to other underlying chronic medical conditions preconception health optimization can improve treatment success rates. Multiple studies have demonstrated the negative impact of overweight and obese BMI, and the value of healthy eating patterns over excessive consumption of processed foods.17-20 Further, given the epigenetic impact of poor diet, high stress levels, and other lifestyle choices, emphasizing healthy habits in the preconception phase has the potential for multigenerational positive impact. 21
Yet another role of LM in the arena of reproductive health is in improving the mental health of infertility patients. Receiving an infertility diagnosis is an inherently stressful phenomenon; however, studies have demonstrated that lifestyle or mind–body approaches, such as mindfulness and meditation practices, can help improve quality of life for those pursuing infertility evaluation and treatment. 22 Enhancing social connectedness through in-person and virtual support groups or more frequent touch points with clinical staff members has similarly shown a positive impact on infertility patient wellbeing.23,24 Thus, shared social experiences can help to support patient mental health during the journey of navigating infertility treatment.
Given the many ways in which comprehensively addressing lifestyle in the preconception phase can benefit mental and physical health on an individual and population level, it appears a reasonable conclusion that stakeholders within the healthcare system should work to improve access to preconception health counseling. Though the American College of Obstetricians & Gynecologists and the American Academy of Family Practice both strongly espouse reproductive life-planning and preconception counseling, many reproductive-aged individuals remain unaware of the relevance or availability of such visits.25,26 Addressing uneven access to care and public health messaging may help these deficiencies. Destigmatizing factual and comprehensive sexual and reproductive education for young people may help establish early knowledge around the best ways to safeguard reproductive and general health. 27 Further, providing physicians and other healthcare providers with specific training and tools (such as these resources prepared by the American College of Lifestyle Medicine (ACLM) 28 to fully offer LM-based recommendations and resources during the preconception and fertility journey would also be likely to yield positive impact. The risks of emphasizing and supporting a healthy lifestyle among those seeking pregnancy are essentially null, while the potential windfall seems too beneficial to miss: now is the right time to work toward enhancing awareness and accessibility of lifestyle medicine in the context of reproductive health. 29
Healthy Skin
Research in the realm of lifestyle medicine and skin health is still in its infancy, with more data being gathered at a rapid pace. Likewise, the relationships between skin health, anti-aging, exercise, sleep, stress, and environmental toxins are all being investigated. Epigenetic factors likely play as much of a role in skin health and external anti-aging as it does in the rest of our health and wellbeing. Growing evidence suggests that our food choices, exercise, sleep, stress management, social networks, and environmental exposures all contribute to a healthy glow from the inside out. What is powerful about the role of lifestyle medicine in dermatology and skin health is that when we optimize evidence-based factors that help to keep skin clear and to reduce skin disease burden, we are also positively impacting cardiometabolic health, cognitive and emotional health, and overall wellbeing.
Both research and empiric evidence show that diet affects skin health. A brief overview of embryology points to the fascinating link between our skin, digestive tract, and food. During gastrulation of the embryo, when the GI and spinal tracts form, an indentation in the spherical blastula gradually pinches down and all the way through the embryo, creating the donut-shaped gastrula. 30 This donut or olive shape, known as a torus, has a single surface, the inside portion of which eventually becomes the GI tract, and the outside of which becomes our skin surface. This intimate relationship shows up in several ways: our GI tracts and our skin both contain our bodies’ largest immune systems; are complex living barriers built for selective absorption of desirable nutrients and substances, while keeping out unwanted or harmful substances; and contain complex microbiomes increasingly recognized as crucial to our health and functioning. What happens in the gut shows up on the skin and, to some degree, vice versa. This relationship is known as the gut–skin axis.
The gut–skin axis has an impact on all skin conditions, but we have the most evidence for its impact on rarer skin conditions such as dermatitis herpetiformis (celiac disease) and hidradenitis suppurativa, as well as the more common psoriasis, acne, and rosacea. A traditional Western diet higher in processed foods, animal products, and saturated fats reduces AMP-activated protein kinase (AMPK), increases insulin signaling, and activates mTORC1, all of which contribute to acne. 31 Growing evidence strengthens the relationships between obesity, insulin resistance, and various aspects of skin disease, such as acne, skin tags, unwanted hair, and acanthosis nigricans. Rosacea, while highly complex, has been shown to be linked not only to small intestine bacterial overgrowth (SIBO), but also to the broader gut–brain–skin axis, imbalances of both the skin and gut microbiomes, and emotional stressors. 32
A second hot area of research with growing evidence is the impact of diet on skin cancer risk. Data show the benefits of eating a rainbow of brightly colored plants in increasing antioxidant value and reducing the harmful effects of ultraviolet rays, but no conclusive evidence yet exists on the exact statistical impact on reducing skin cancer itself. 33 Finally, food has benefits in reducing the outward signs of aging, which may be motivating for patients. An anti-aging diet consists of 3 goals. First: fighting cellular oxidation by eating plenty of brightly colored plants and spices. Second: fighting glycation (reducing advanced glycation end products, or AGEs) by reducing not only sugar and processed food intake, but also reducing intake of foods cooked and scorched at high heats. Third: fighting inflammation, known as “inflammaging,” by eating anti-inflammatory foods and spices such as turmeric, garlic, fiber, and more.34,35
Like food, the exact role of exercise in skin health and anti-aging is still being identified. There may be a direct impact of exercise on reducing aging in our skin cells. One group has shown through various measures that mitochondria play a role in maintaining a younger-acting metabolism in skin cells (again via AMPK, as with diet, but this time stimulated by IL-15). 36
Sleep is a complex biological process: sleep quality, quantity, and timing impact brain health, heart health, and cancer risk. 37 There is less evidence about the direct impact of sleep on skin health, but because of the effect of poor sleep on factors such as diet, stress, and hormone levels, it is likely that sleep affects the health and appearance of our skin as well. One study linked poor quality reported sleep with worsening acne. 38 Another linked poor quality sleep with increased inflammatory signaling and increased tendency for rosacea flares. 39 Another group found evidence that late night blue light exposure and screen use affected skin hydration and skin quality. 40 Finally, the idea of “beauty sleep” is prevalent in the wellness industry, but data is still sparse. One study used a blinded rating comparison of photos taken after good sleep vs poor sleep, where researchers concluded that poor sleep negatively affected attractiveness and appearance of health in the short-term. 41
Psychological stress has been so well linked to skin health that there is a subspecialty for it known as psychodermatology. The brain–skin axis, like the gut–skin axis, is bidirectional. Chronic skin disease can be emotionally debilitating, and emotional or mental stress can have direct impacts on skin disease and skin health. Unfortunately, a vicious cycle can also be created, which is difficult for patients to break out of on their own. Stress triggers inflammation, which has also been shown to lead to increased aging. An excellent review of this topic was published in 2014, 42 and more recent research has corroborated and elucidated many complex factors relating acute and chronic stress with skin quality, skin disease, and skin aging. 43
The benefit of healthy relationships and healthy social networks on skin health is likely 2-fold. First, healthy intimate and personal relationships are less stressful and contribute more joy to life. Since we know stress directly debilitates our health and our skin, it stands to reason that there is a connection that might be found here. Second, we are impacted most highly by the personal habits of those closest to us. If we surround ourselves with people who aim for health, eat well, care about sleep, and stay active, we are more likely to engage in healthful behaviors ourselves, which may also impact our skin and keep us youthful.
Alcohol and smoking have well documented negative impacts not only on skin diseases such as psoriasis but also negative impacts on aging, as noted in famous twin studies. Environmental exposures such as air pollution also affect skin health. One broad-ranging study reviewed the impact of these factors, plus sun damage and nutrition, on the skin and concluded that all have a provable deleterious effect. 44
While solar ultraviolet radiation can both accelerate aging as well as increase the risk of skin cancer, newer research supports the importance of direct sun exposure on our skin. Previous wisdom has suggested that if we get adequate vitamin D through diet and supplementation, this should be enough to balance the reduced sun exposure. But, more recently, the effects of too little sun on many aspects of our physical and mental health have been elucidated, 45 and one researcher has become well known for pointing out that measuring blood vitamin D levels may not be enough, and it may in fact just act as a poor proxy for the sum total of the complement of benefits we receive via the direct impact of ultraviolet radiation in reasonable amounts upon our skin, especially the impact on our immune system known as photoimmunology. 46
Every lifestyle choice we make every day affects our health from the inside out, including the clarity and glow of our skin as well as the quality of our aging.
Breast Cancer Survivorship
Breast cancer is the most commonly diagnosed cancer in women in the United States (excluding skin cancers). Due to advances in early detection and treatment, breast cancer mortality rates have declined by 40% since the 1980s. Long-term survival after a diagnosis of breast cancer is common, and survival rates at 5 years are > 90%. Currently, there are 3.8 million breast cancer survivors in the United States. 47 By 2030, this number is predicted to increase to 4.9 million. 47 Breast cancer survivors have unique medical and psychosocial issues that must be addressed as part of survivorship care. Key areas of breast cancer survivorship care include monitoring for disease recurrence, screening for second primary cancers, addressing medical and psychosocial consequences of treatment, and counseling on health promotion. 48 There is increasing data which demonstrates the importance of lifestyle interventions, which may decrease risk of recurrence, improve quality of life, and ultimately improve outcome after a diagnosis of breast cancer.
The American Cancer Society and the American Society of Clinical Oncology have outlined specific guidelines for health promotion for breast cancer survivors. These health-promotion guidelines recommend that the healthcare team: (1) assess body weight, specifically breast cancer survivors who are overweight/obese should be counseled to achieve and maintain a healthy weight; (2) counsel about physical activity, specifically breast cancer survivors should be encouraged to engage in regular exercise, including at least 150 minutes of moderate physical activity or 75 minutes of vigorous aerobic activity each week, along with strength training 2 days per week; (3) counsel about the importance of a healthy diet pattern; and finally, (4) counsel about the role of smoking cessation. 48
Although these recommendations for health promotion have been incorporated into the guidelines described above, there are significant barriers for oncologists to address these issues. In 2018, the American Society of Clinical Oncology launched a survey to assess oncologists’ understanding and practice behaviors related to counseling cancer survivors about diet, weight management, and physical activity. 49 The majority of respondents agreed that there was a strong link between obesity/overweight and cancer outcomes, and that nutrition, weight, and physical activity should be addressed as part of cancer treatment. However, 83% of the respondents indicated that additional training was needed to address these issues adequately in cancer patients. A number of barriers to addressing these lifestyle behaviors were identified, to include (1) oncologists’ lack of education on these topics, (2) not enough time during a clinic visit, and (3) the need for weight management and physical activity programs for cancer survivors. 49
Thus, healthcare providers with expertise in lifestyle medicine have an opportunity to contribute in a meaningful way to improve the care of breast cancer survivors. By using evidence-based tools from lifestyle medicine, clinicians with expertise in lifestyle medicine have an opportunity to educate and empower cancer survivors to make sustainable lifestyle changes to improve their physical and mental wellbeing after a diagnosis of cancer, and ultimately to lower risk of disease recurrence and improve overall outcomes from cancer. The 6 pillars of lifestyle medicine, physical activity, nutrition, sleep, stress management, avoidance of risky substances, and social connections, play an important role in breast cancer survivorship.
Physical activity has been shown to improve multiple clinical outcomes in breast cancer survivors. There have been numerous randomized trials which have assessed the feasibility and benefits of increasing exercise activity after a breast cancer diagnosis. Physical activity after a breast cancer diagnosis has been associated with improvements in mental health (anxiety and depression), cancer-related fatigue, body image, body size and body composition, aerobic fitness, strength, cognitive function, and quality of life.50,51 Exercise has also been shown to reduce risk for development of lymphedema. A recent meta-analysis of 16 prospective observational studies in breast cancer survivors demonstrated that when comparing the most vs least active breast cancer survivors, there was a 48% reduction in overall mortality, and a 28% reduction in breast cancer–specific mortality. 52 Furthermore, for those individuals who increased their physical activity levels relative to their pre-diagnosis levels, those individuals had a lower risk of mortality compared to survivors who decreased their physical activity levels or were inactive at both time points. 52
There are many resources which provide education on the role of physical activity for cancer survivors. Through the American College of Sports Medicine, the “Moving Through Cancer” initiative has many helpful resources for both healthcare providers and for patients. 51
The World Cancer Research Fund/American Institute of Cancer Research (WCRF/AICR) provides updated analyses on the latest evidence regarding the role of nutrition, physical activity, and weight, in terms of cancer risk reduction, and the role of these lifestyle interventions for cancer survivors. With regard to nutrition recommendations, guidelines from the WCRF/AICR and American Cancer Society are consistent and focus on 3 key areas: (1) the role of diet quality, (2) the importance of weight control, and (3) the importance of obtaining nutrients from food sources, rather than dietary supplements. 53 There are a number of excellent resources which provide education regarding nutrition for breast cancer survivors. In addition to comprehensive resources from the WCRF/AICR, materials from ACLM are practical resources for cancer survivors.
Sleep disturbance and insomnia are highly prevalent among breast cancer survivors, with rates as high as 30–50%. 54 Multiple factors contribute to insomnia, including side effects from endocrine therapy, discomfort from local therapy, anxiety, and fear of recurrence. Cancer-related insomnia is associated with worsening daytime functioning and quality of life. There are a number of treatment options for management of cancer-related insomnia, including psychosocial interventions, behavioral treatments such as cognitive behavioral therapy for insomnia (CBT-I), and pharmacologic therapies.
Psychological distress is unfortunately quite common among breast cancer survivors. 55 Per guidelines outlined by the National Comprehensive Cancer Network, all cancer survivors should be assessed for distress, depression, and anxiety. 56 Individuals should be offered counseling or referrals to mental health resources, if needed.
Consumption of alcoholic beverages of all types increases the risk for development of cancer, and consumption should be limited in breast cancer survivors. 53 The WCRF/AICR and American Cancer Society have made the recommendation that it is best for cancer survivors not to drink alcohol. There are a number of mechanisms by which alcohol may increase risk for development of cancer, or risk for recurrence, which include direct damage to cellular DNA, decreased breakdown of estrogen, impaired absorption of nutrients, and weight gain.
Finally, studies have shown that poor social support is associated with an increased risk of cancer mortality. 57 Breast cancer survivors derive great benefit from social support from virtual groups as well, such as PAVING the Path to Wellness, a breast cancer survivorship program in which participants pursue positive lifestyle changes in a supportive environment. 58
Sexual Health
Sexual function and sexual health are key elements of wellbeing, serving both as a marker of general health and a component of quality of life for many individuals.59,60 Sexual health concerns are common, with 43% of women experiencing problems with desire, arousal, lubrication, orgasm, pain, and/or satisfaction.7,61,62 The prevalence is higher in women with chronic health problems, such as cardiometabolic disease, obesity, and mental health disorders.59,63-69 These same health problems are effectively addressed by lifestyle medicine, making sexual health a logical extension of its application. In fact, lifestyle behaviors are extensively tied to positive sexual function (Figure 1). Healthcare providers can fill an important gap by understanding these connections and empowering patients to utilize lifestyle medicine techniques to prevent and address female sexual dysfunction.
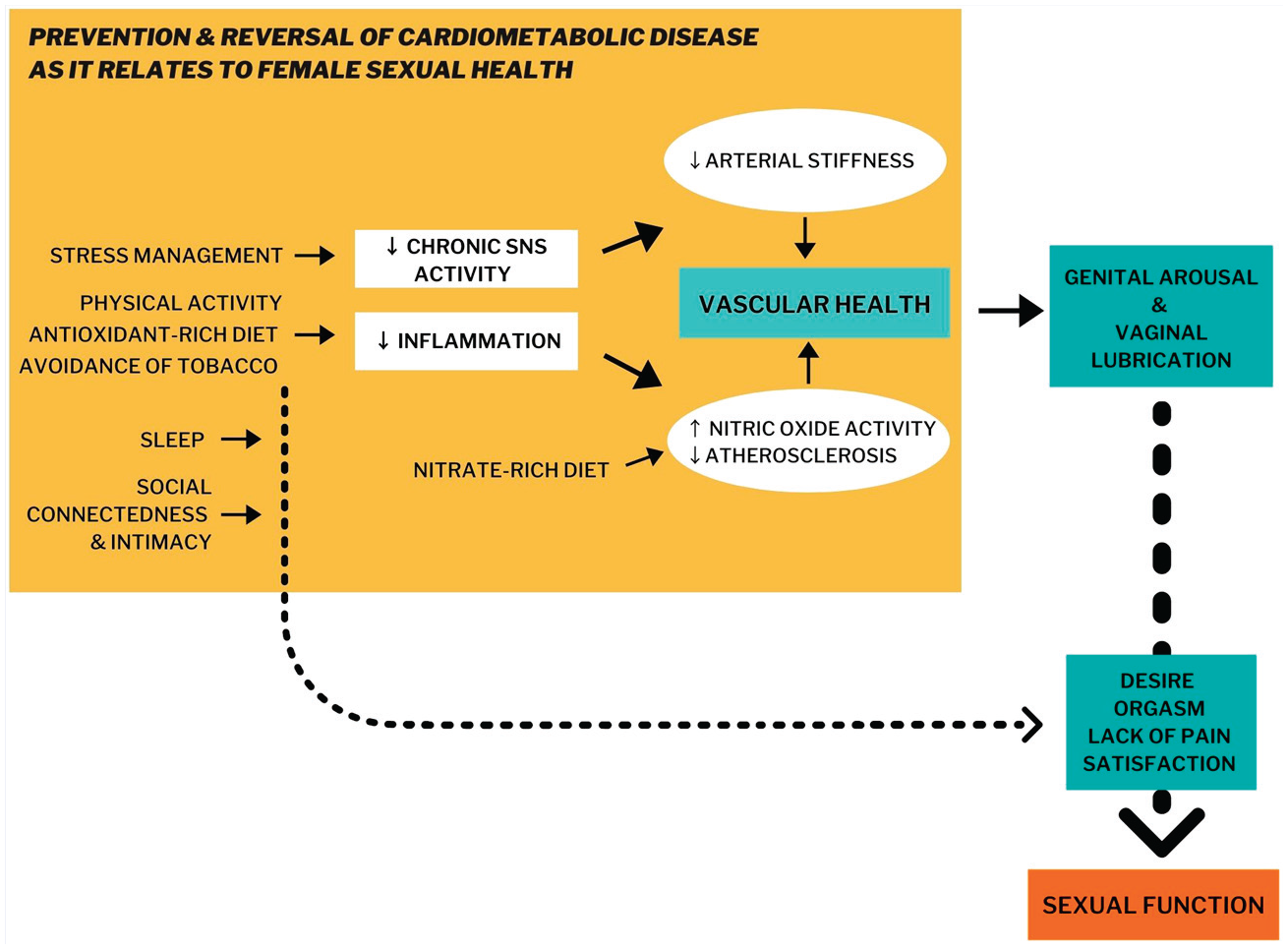
Healthy lifestyle behaviors can support female sexual function From: Improving Women’s Health Across the Lifespan, 1st Edition, Edited By Michelle Tollefson, Nancy Eriksen, Neha Pathak Copyright (2022) by CRC Press. Reproduced by permission of Taylor & Francis Group.
Dietary patterns, including some specific dietary components, are linked to sexual health, with vascular and other mechanisms at play. Healthy pelvic and genital tissue vasculature is needed for the female peripheral sexual response, such as genital engorgement and vaginal lubrication.70,71 A diet rich in diverse, colorful plants with antioxidants and flavanols, with minimal processed foods and saturated fat, is protective of endothelial health, and is associated with more regular sexual activity and less dysfunction. The Mediterranean diet is the most extensively studied pattern in relation to sexual health and is associated with better sexual function in both observational and interventional studies.72,73 Specific foods such as apples, cacao beans, beets, watermelon, and nuts provide antioxidants and/or the nitric oxide precursor arginine that can improve endothelial function.74-79 Finally, deficiencies in Vitamin D and iron are linked to sexual dysfunction, with improvement seen after repletion.80-83
Sedentary lifestyle increases the risk of sexual dysfunction through its impact on lifestyle-related chronic disease risk, mood, and body image.84-90 Conversely, regular physical activity is associated with higher sexual desire, more frequent sexual activity, and lower risk of sexual dysfunction in women.68,91-95 Aerobic activity, in particular, is beneficial for vascular health, such as through increasing nitric oxide availability, important for the female peripheral sexual response. 96 Yoga, Pilates, and other mind–body movement therapies are shown to improve all domains of sexual function.97-100 Some women may benefit from pelvic floor muscle exercises, shown to increase sexual desire, arousal, orgasm, and satisfaction.101-103 Acute sympathetic nervous system (SNS) activation, such as through exercise, is found to increase sexual desire and objective genital arousal, positively impacting orgasm. 96 Of note, chronic SNS activation, as seen in chronic stress, can negatively affect sexual health. 104 Physical activity is shown to positively impact body image, which, in turn, is positively correlated with feeling more sexually desirable, more frequent engagement in a diverse range of sexual experiences, and less sexual dysfunction.90,105
Quality and quantity of sleep are also important predictors of female sexual function. Women who experience insomnia or frequent sleep disturbances report increased difficulty with sexual arousal, decreased frequency of sexual activity, and increased dyspareunia.106-109 Conversely, engagement in partnered sex and/or self-genital stimulation are linked to improved sleep onset and quality. 110 This may relate to post-orgasm oxytocin and prolactin release, which can reduce cortisol release and have a calming effect. 111
Chronic stress has a significant negative impact on female sexual health. Chronic stress is associated with decreased sexual thoughts, desire, and physiologic genital arousal. Stress-related distraction from sexual stimuli, low mood, and anxiety all play a role.61,104,112 Conversely, orgasm is found to coincide with the release of prolactin, which may reduce stress. 111 Stress also impairs vascular health through multiple mechanisms. 113 Mindfulness-based stress reduction for sexuality (MBSR-S) is associated with increased sexual desire, arousal, and satisfaction. 114
Contrary to depictions in popular media, many commonly used substances, including tobacco, cannabis, and alcohol, have deleterious or mixed effects on sexual function. Smoking tobacco products causes endothelial damage, which can result in decreased pelvic blood flow and subsequent blunting of genital arousal and vaginal lubrication.115,116 The literature concerning cannabis consumption is mixed and limited. While some studies show that use closely before sexual activity increases pleasure and satisfaction, others show decreased orgasm and increased pain.92,117,118 The effects of alcohol consumption on sexual activity also appear to be mixed. In the short-term, alcohol consumption preceding sexual activity may increase reported pleasure and arousal, although orgasm and objectively measured genital arousal are blunted.117,119 In the long-term, moderate alcohol consumption is linked to increased coital frequency and lower rates of sexual dysfunction, though heavy use is linked to sexual dysfunction.92,117
Additional education and awareness around sexual health, including female anatomy as it relates to sexual activity and pleasure, as well as strategies to improve communication, complement the benefits of lifestyle medicine pillars in improving sexual satisfaction for women. For those engaging in partnered intimacy, open communication about sexual needs and concerns can be emphasized, opening the door to healthy relational negotiation. Many prescribed and over-the-counter tools are available to help with sexual dysfunction. For those with vaginal dryness or genitourinary syndrome, vaginal estrogen, vaginal moisturizers, lubricants, and vaginal dilators can be considered, depending on the underlying diagnosis and healthcare provider recommendations. Genital vibratory stimulation can assist with genital arousal and orgasm through increasing pelvic floor and genital blood flow. 120 Genital vibratory devices may be particularly helpful for postmenopausal women, for whom clitoral sensitivity often persists, despite decreased clitoral tissue and vaginal sensitivity.120,121 Experimentation with sexual health tools should be normalized and women encouraged to identify what works best for them.
Given the connections between sexual health, general health, and quality of life, healthcare providers should become comfortable initiating conversations about sexual health. First, ensure an appropriate setting for the conversation, with the patient fully clothed and the provider seated. An established positive rapport is important. The provider should be aware of the possibility of a history of sexual trauma and its potential impact. Then, simple conversational models can be used. The Permission, Limited Information, Specific Suggestions, Intensive Therapy (PLISSIT) model is one such approach. 122 Additionally, the Ask–Tell–Ask model is easy to remember and in line with patient-centered communication (Table 1). 123 Importantly, a provider need not be a sexual health expert or necessarily block off longer appointment times to initiate a conversation. Simply starting a dialogue can begin to dispel stigma, provide hope, and serve to point a patient in the right direction. Building and utilizing a referral base of local gynecologists with expertise in sexual health, pelvic floor physical therapists, and sex or other mental health therapists is important, as not all sexual dysfunction can be managed through lifestyle modifications.
Useful Models for Providers When Discussing Sexual Health.
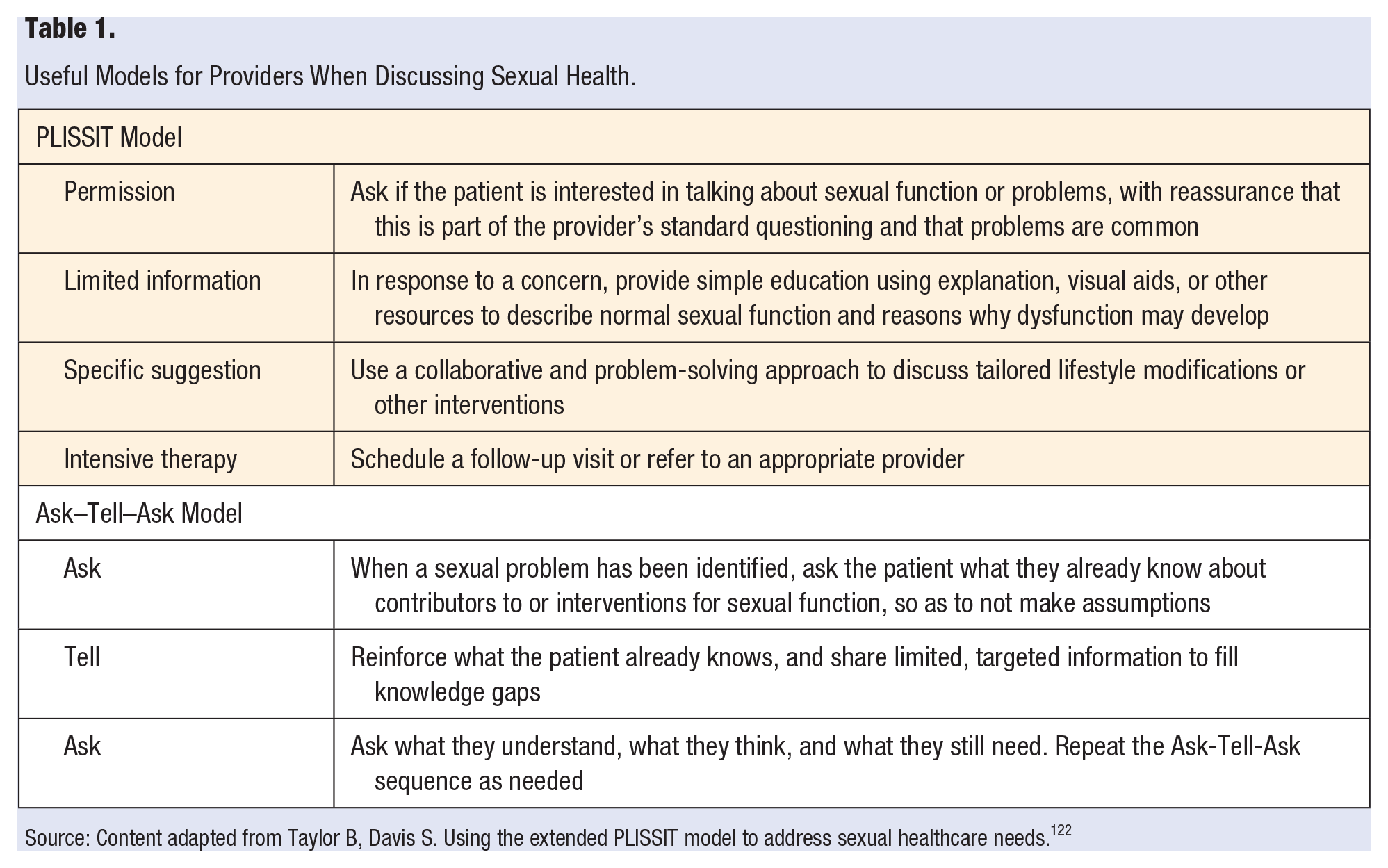
Source: Content adapted from Taylor B, Davis S. Using the extended PLISSIT model to address sexual healthcare needs. 122
Many women experience sexual health concerns or dysfunction, many of which are closely related to lifestyle medicine factors. Providers have an opportunity to engage patients around healthy lifestyle behaviors in the context of conversations about improving sexual health and satisfaction, ultimately contributing to a spectrum of benefits for both sexual health and overall wellbeing.
Conclusion
We live in an era in which research advances and lifestyle medicine education have the potential to transform women’s healthcare. Our patients are in search of safe and effective options to address the challenges they face every day. As lifestyle medicine practitioners we see the potential for benefit as well as the risks of both traditional and alternative therapies. With further research and greater education, we can unify both traditional and lifestyle medicine under the banner of safe, effective, evidence-based care for women. Within ACLM, The Womens’ Health Member Interest Group, brings together health professionals working to understand and apply the foundational pillars of lifestyle medicine to help women realize optimal health and live their best life.
Footnotes
Author’s Note
This workshop was presented virtually at Lifestyle Medicine 2021 on November 6th, 2021.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
