Abstract
Healthcare professionals recommending dietary changes to patients often find that institutional settings—businesses, universities, long-term care facilities, correctional institutions, among others—may not provide the healthful foods that healthcare professionals recommend. Moreover, such institutions encounter an increasing diversity of dietary restrictions, based on allergies, intolerances, religious mandates, or other reasons, that may be challenging to satisfy. To address these issues, experts in health, dietetics, culinary arts, religion, and ethics developed a simple set of guidelines that aim to meet the widest possible range of dietary needs. Three culinary teams then used these guidelines to create “Universal Meals”—simple recipes that were then adapted to larger production sizes for institutional use. The healthfulness of representative sets of meals drawn from these recipes was assessed using the Alternative Healthy Eating Index-2010 and found to be superior to that of a meal pattern based on National Health and Nutrition Examination Survey data.
Introduction
Clinical and nonclinical populations are becoming increasingly diverse. Along with this diversity of backgrounds comes a variety of dietary practices, needs, and expectations. Dietary practices are also influenced by medical conditions, food intolerances, and allergies. An increasing diversity of dietary needs may present challenges for healthcare personnel seeking to prescribe healthful diets, especially for individuals eating in institutional settings or traveling. This increasing diversity of needs may be similarly challenging for food service managers working to accommodate dietary demands.
One strategy is to accommodate differences in food choices with a wide range of food offerings in institutional settings. Another is to identify what various diet practices have in common. The need to provide meals for individuals from a wide variety of religious and cultural backgrounds led the Defense Logistics Agency of the U.S. Department of Defense to develop the Humanitarian Daily Ration in 1993. 1 The meals are based primarily on grains, legumes, and vegetables and generally avoid animal-derived products and alcohol. They prioritize simplicity and long shelf-life. Similarly, colleges and universities have long been exploring means of responding to the increasing diversity of nutritional needs in their communities.2,3
The goal of the present project was to build a set of recipes for “Universal Meals” that would be suitable for individuals across a range of health, religious, and cultural backgrounds that would provide healthful meals in institutional settings. A consortium of experts in dietetics, health, medicine, culinary arts, religion, and ethics identified food restrictions commonly observed in a wide variety of populations and developed a simple set of food guidelines that aimed to accommodate all of these restrictions. Their guidelines were then given to 3 culinary teams (The Culinary Institute of America, Spork Foods, Inc., and DC Vegan Catering) who used these guidelines to develop recipes that were to be (1) appealing to people with a variety of dietary restrictions and preferences, (2) familiar, favoring well-known foods, (3) flexible, with the ability to be tailored and enhanced as desired, and (4) adaptable to institutional settings. Recipes were to be as streamlined as possible for food service teams to navigate into daily production, using minimal ingredients that are already on hand or easy to obtain, and minimizing labor and production time.
To estimate the healthfulness of the Universal Meals, the Alternative Healthy Eating Index-2010 (AHEI) was used assess diet quality for a representative selection of these recipes as they would be used in meals. 4 The AHEI was developed to identify dietary patterns associated with lower risk of chronic disease. The index is comprised of 11 components representing foods to eat more often (eg, fruits and vegetables) and those to eat less often (eg, red and processed meat). The maximum score is 110 points; the higher the score, the lower the risk. Recipes were then tested for palatability and scaled to larger batch sizes for institutional use.
An additional set of recipes, called UM Thrifty, was developed for meals that are particularly easy to prepare and cost less than $1 per serving. The production cost for each recipe for institutional settings was estimated, drawing on ingredient costs listed by US Foods, Webrestaurant.com, and Amazon.com.5,6
Identification of Food Limitations
Dietary restrictions were examined in the context of health conditions, religious observances, and personal directives, as described in the sections below.
Health Conditions
Certain health conditions require avoidance of specific food products.
Lactose intolerance is an inability to digest lactose, the sugar found in milk products, due to the lack of the lactase enzyme. Without sufficient lactase, milk ingestion can cause abdominal pain, bloating, flatulence, nausea, and diarrhea. Congenital lactase deficiency is a rare condition in which a mutation of the lactase-phlorizin hydrolase gene prevents lactase production.7,8 Much more common is the gradual loss of lactase starting in mid- to late childhood or early adulthood. Lactose intolerance was typically described as an uncommon condition prior to 1965, when tests in 60 adult hospital patients in Maryland identified the condition in 70% of Black participants, compared with 15% of White participants, 9 a finding soon confirmed in subsequent studies. 10 Since then, it has become clear that lactase non-persistence is the norm in human populations (as for all mammals) overall. In individuals who tolerate lactose, the persistence of lactase into adulthood appears to be due to a genetic mutation occurring in dairying communities in Europe some 7500 years ago. 11
A gluten-free diet is essential for the roughly 1% of the world’s population that has celiac disease 12 and is of interest to a far larger population. A gluten-free diet omits wheat, rye, barley, triticale, malted grains, and brewer’s yeast (which contains gluten from barley). 13 Foods that work well on healthful gluten-free diets include fruits, vegetables, beans, legumes, rice, quinoa, millet, flax, chia, gluten-free oats, and nuts. 14
Food allergies are common in children and adults.15-17 Approximately 90% of food allergies
18
are attributable to the following 8 products: 1. Milk 2. Eggs 3. Fish 4. Crustaceans and shellfish 5. Tree nuts 6. Peanuts 7. Wheat 8. Soybeans
Pursuant to the Food Allergen Labeling and Consumer Protection Act of 2004, the U.S. Food and Drug Administration requires that these potential allergens be listed on product labels. 19 Despite labeling, allergic reactions are a continuing threat. A 2018 survey of 246 school nurses found that 32% of respondents reported at least one severe reaction taking place in the preceding year, and only 31% reported proper labeling of allergens on food items served. Limited staff and resources were noted as barriers. 20
Religion
According to the Pew Research Center, Christianity is the world’s leading religion, with 2.2 billion adherents in 2010, followed by Islam (1.6 billion), Hinduism (1.0 billion), Buddhism (488 million), and Judaism (14 million); 463 million were described as adhering to other religions, and 1.1 billion people were described as unaffiliated. 21 Among Christians, dietary restrictions are uncommon, with certain notable exceptions. An emphasis on health has led many Seventh-day Adventists to limit or avoid animal products. 22 The Ethiopian Orthodox Church requires that people over age 13 “fast” during many days of the year, omitting meat, eggs, and dairy products on those days.23,24 Suitable meals for these fast days typically emphasize grains, vegetables, and legumes. 25
Muslims make up 24% of the global population. 26 The Qur’an uses the terms halal and haram for foods and lifestyle practices deemed lawful and unlawful, respectively. 27 Foods considered haram include pork products, alcohol, carnivorous animals, birds of prey, blood and blood byproducts, and products that have been contaminated by any of these sources. The status of some foods can vary depending on their origin, preparation, or ingredients. If a food’s status is unclear, it is typically referred to as mashbooh (doubtful). Food products can receive halal certification through programs that evaluate methods of food sourcing and preparation. However, foods that have not gone through this process will be acceptable to most Muslims, provided they fit within the standards of acceptable foods. Among Muslims who do not strictly follow halal standards, avoidance of pork and alcohol is nonetheless very common. 28
Of the world’s approximately 14 million Jewish people, 5.7 million live in the United States. 29 Jewish dietary traditions are embodied in kashrut, a set of dietary laws outlined in the Torah. The term “kosher” refers to being fit or proper, with certain foods deemed acceptable for consumption, while others are prohibited. 30 In the former category are products from cows, sheep, goats, and deer. In the latter category are pork products, shellfish and other aquatic species lacking fins and scales, and meat from several other species. 27 Kosher guidelines also extend to food preparation methods (eg, meat and milk are not combined in cooking), 27 packaging, and processing equipment. A kosher symbol ensures that there are no non-kosher ingredients or non-kosher methods used in production. For Passover, additional rules apply.
Observance of kosher guidelines varies widely. The approximately 10% of the American Jewish population who follow orthodox Judaism are the most adherent, 31 compared with roughly one-third of conservative Jews and 7% of reform Jews. 28 Many individuals, while not strictly kosher, avoid pork and shellfish products and avoid mixing meat and milk. 32 Some may follow kosher standards generally but will eat some products without kosher certification, particularly nonmeat items.
Hindus make up 15% of the global population, living principally in India, Nepal, and Mauritius, 33 with 2.2 million living in North America. 34 Under the principles of karma, samsara (reincarnation), and ahimsa (non-violence), an estimated 30% of the Indian population opts for a vegetarian diet; this percentage varies widely across regions. 35 A Hindu vegetarian diet typically omits meat and eggs, but allows dairy products and honey. 32
Personal Directives
Many individuals avoid animal-derived products for ethical, health, or environmental reasons. A vegetarian diet omits meat products and may or may not include dairy products, eggs, or honey. Vegan diets omit all animal-derived products. 36 An estimated 8 million American adults follow vegetarian diets, including 3.7 million who follow vegan diets. 37 According to Google Trends, a website that tracks the popularity of search queries across various regions and languages, there has been a global increase in the interest in vegan diets since 2004, especially in Israel, Australia, Canada, Austria, and New Zealand. 38 In addition, many people who routinely consume animal products nonetheless often choose vegan or vegetarian products at home or at restaurants. In 2018, plant-based product sales increased by 20% over the previous year, with total sales exceeding $3.3 billion. 39 These included increased sales of meat alternatives (24%) and plant-based versions of milks (9%), cheeses (43%), yogurts (55%), and creamers (131%). 35
From Limitations to Meal Guidelines
The wide range of restrictions described above was used by the consortium of experts to create the following set of guidelines, based on necessary exclusions. Universal Meals will: 1. Omit animal-derived ingredients. 2. Omit gluten-containing grains (wheat, rye, barley, triticale, malted grains, and brewer’s yeast). 3. Be prepared without common allergens: milk, eggs, fish, crustaceans and shellfish, tree nuts, peanuts, wheat, soybeans. 4. Avoid the use of alcohol.
Following these guidelines, most health, religious, and personal choice frameworks can be readily satisfied. Vegetables, fruits, legumes, and non-gluten grains are broadly acceptable to virtually all groups.
Universal Meals Nutrition Information and Cost Per Serving
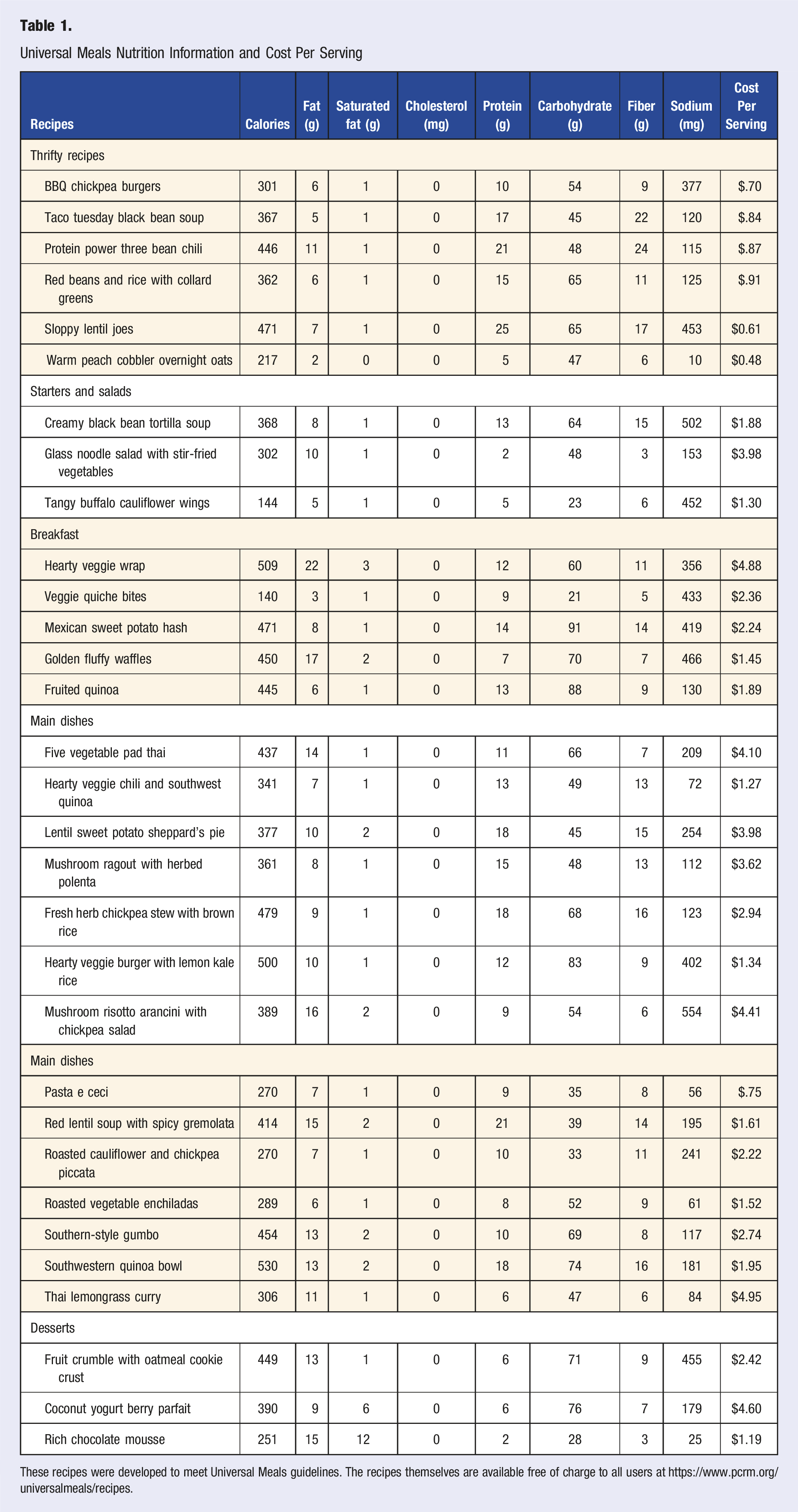
These recipes were developed to meet Universal Meals guidelines. The recipes themselves are available free of charge to all users at https://www.pcrm.org/universalmeals/recipes.
Diet Quality
Alternative Healthy Eating Index for Selected Universal Meals.
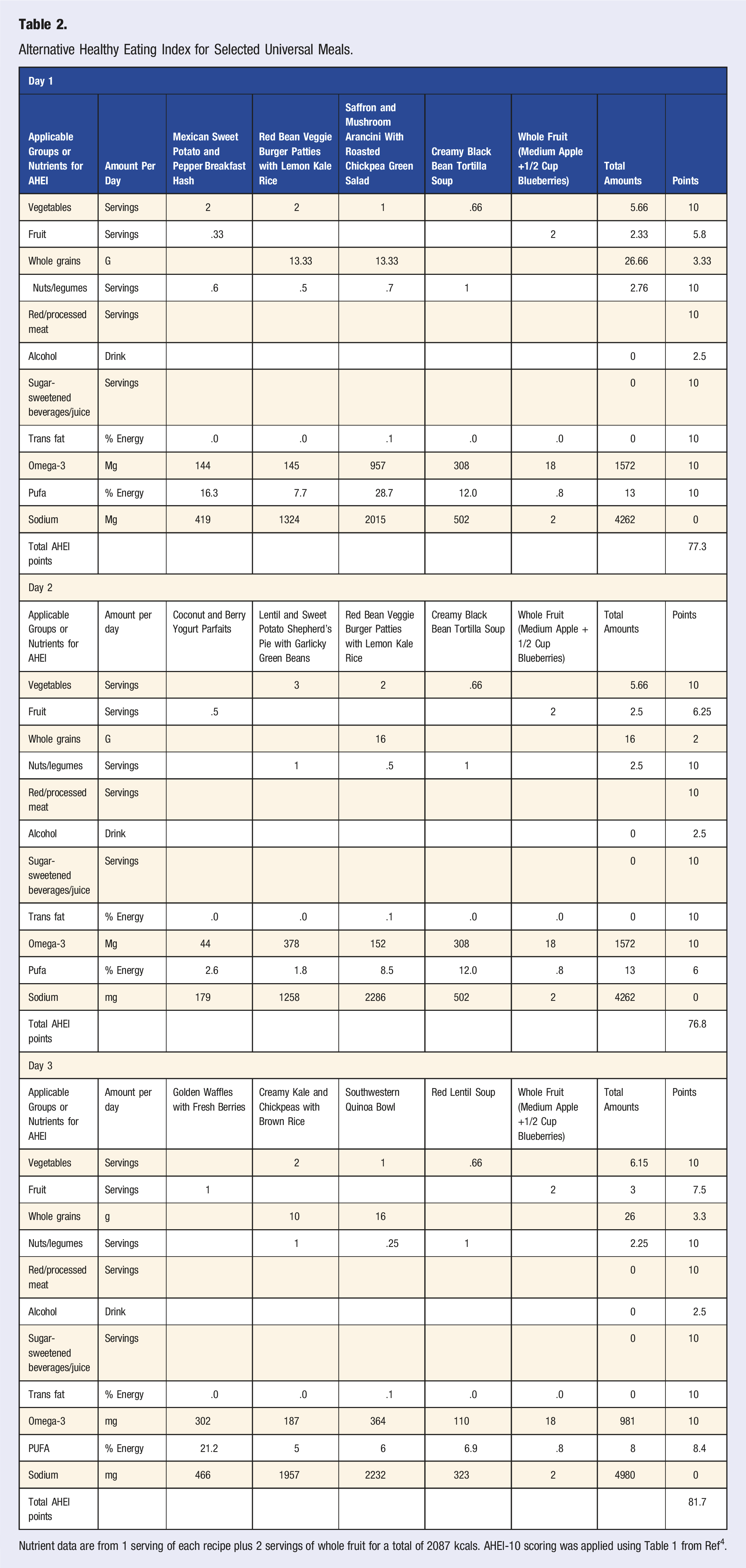
Nutrient data are from 1 serving of each recipe plus 2 servings of whole fruit for a total of 2087 kcals. AHEI-10 scoring was applied using Table 1 from Ref 4 .
Day 1
Breakfast: Mexican Sweet Potato and Pepper Breakfast HashLunch: Red Bean Veggie Burger Patties with Lemon Kale Rice Dinner: Creamy Black Bean Tortilla Soup and Saffron and Mushroom Arancini with Roasted Chickpea Green Salad.
Snacks: Apple (1 medium) and blueberries (1/2 cup).
Day 2
Breakfast: Coconut and Berry Yogurt Parfaits.
Lunch: Lentil and Sweet Potato Shepherd’s Pie with Garlicky Green Beans.
Dinner: Red Bean Veggie Burger Patties with Lemon Kale Rice with Creamy Black Bean Tortilla Soup.
Snacks: Apple (1 medium) and blueberries (1/2 cup).
Day 3
Breakfast: Golden Waffles with Fresh Berries.
Lunch: Creamy Kale and Chickpeas with Brown Rice.
Dinner: Southwestern Quinoa Bowl with Red Lentil Soup.
Snacks: Apple (1 medium) and blueberries (1/2 cup).
For the above menus, which provided approximately 1775–2000 calories per day, the AHEI-2010 scores were 77.3, 76.8, and 81.7, respectively (out of 110 points possible).
Costs
The median ingredient cost for Universal Meals was $1.89 per serving, with a range from $.48 for Warm Peach Cobbler Overnight Oats to 4.95 for Thai Lemongrass Curry. For UM Thrifty meals, the median ingredient cost was $.77 per serving, with a range from $.48 for Warm Peach Cobbler Overnight Oats to $.91 for Red Beans and Dirty Rice with Collard Greens.
Conclusions and Applications
Universal Meals were developed to provide healthful meals meeting the requirements of the vast majority of people dining in institutional settings. The availability of Universal Meals will make it easier for individuals with a wide variety of needs based on medical conditions, religious restrictions, or personal choices to find suitable foods, and for healthcare providers to recommend foods that meet the needs of their clients.
Several limitations should be acknowledged. While the 8 most common food allergens were omitted, other allergens affect individuals in rare cases. Meals will be kosher or halal only when catering companies have made the necessary arrangements. Some religious mandates may not have been accounted for. The current project developed a finite number of suitable recipes, recognizing that an infinite number of other recipes could meet these guidelines. Universal Meals were not designed to be low in sodium or vitamin-fortified but could easily be modified in these ways if desired.
Footnotes
Acknowledgments
Chefs Dave Kamen, Paul Dellerose, Mark Ainsworth, and George Shannon, and Registered Dietitian Suki Hertz of The Culinary Institute of America, Jenny Engel and Heather Bell of Spork Foods, Inc., and DC Vegan Catering developed recipes. Walle Engedayehu, PhD, and Wondyefraw Mekonen, PhD, reviewed the manuscript for critical content. Neal Barnard, MD, FACC; Aarti Batavia, MS, RDN, CLT, CFSP, IFMCP; Mayim Bialik, PhD; Sherene Chou, MS, RD; Jeffrey Spitz Cohan; Lilian Correa RDN, MPH, DipACLM; Evelyn F. Crayton, EdD, RDN, LDN, FAND; Anthony Dissen, MPH, MA, RDN, CPH; Kristi Grim; Natalie Hardcastle; Bawa Jain; Pietro Leemann; YaQutullah Ibraheem Muhammad MS, RDN, LD; Sailesh Rao, PhD; Rojean Williams, MS, RD, LD; and Rabbi Dr Shmuly Yanklowitz helped set-up program guidelines. Permission was received to include those named in the acknowledgments.
Author Contributions
N. Barnard, N. Hardcastle, L. Correa, Y. Muhammad, A. Batavia, and S. Levin wrote the manuscript. A. Lenthall and D Harder provided recipe analyses on nutrients and costs. V. Rahman, S. Yanklowitz, and H. Kahleova reviewed the manuscript for critical content. S. Levin calculated the Alternate Healthy Eating Index. The Culinary Institute of American Consulting, Spork Foods, Inc., and DC Vegan developed the recipes.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Dr Barnard is an Adjunct Professor of Medicine at the George Washington University School of Medicine. He serves without compensation as president of the Physicians Committee for Responsible Medicine and Barnard Medical Center in Washington, DC, nonprofit organizations providing educational, research, and medical services related to nutrition. He writes books and articles and gives lectures related to nutrition and health and has received royalties and honoraria from these sources. Ms Hardcastle, Ms Levin, Ms Lenthall, Mr Harder, Dr Kahleova, and Dr Rahman received compensation from the Physicians Committee for Responsible Medicine for their work on this manuscript. Ms Correa, Ms Muhammad, Ms Batavia, and Dr Yanklowitz declare no conflicts of interest related to the manuscript.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article: This work was funded by the Physicians Committee for Responsible Medicine.
