Abstract
The digestive system is involved in providing both regulatory and biochemical signaling to the nervous system via the gut–brain axis. Major brain neurotransmitters within the enteric nervous system include acetylcholine, serotonin, and norepinephrine, which are triggered by various stimuli within the digestive system, including the microbiota. Associations between the gut microbiome and activation of neuroreceptors and neurotransmitters are related to factors such as appetite control, mood, and memory. This column presents the results of a brief review of recently published clinical trials related to gut microbiome interventions (n = 11) that aimed to address a variety of mental health outcomes. The impacts of probiotics on mental health and other clinical outcomes vary by the health of study participants. Continuing research on the mental health benefits of probiotics in healthy individuals is necessary.
“... health care providers aiming to provide tools to address mental health issues may consider probiotics...”
Body
Whole-person treatment and intervention strategies are imperative to optimizing outcomes for individuals suffering from mental health and psychologic conditions. Nutrition plays a key role in maintaining optimal physiologic function that is foundational to optimal mental health. Even prior to the manifestation of physical signs of poor nutrition, psychologic consequences occur, which can be observed in irregular eating habits and unhealthy food choices. Additionally, the digestive system is involved in providing both regulatory and biochemical signaling to the nervous system via the gut–brain axis. 1 There are nearly 100 million neurons that function autonomously in what is called the enteric nervous system (ENS). 2 Major brain neurotransmitters within the ENS include acetylcholine, serotonin, and norepinephrine, which are triggered by various stimuli within the digestive system, including the microbiota. 3 Associations between the gut microbiome and activation of neuroreceptors and neurotransmitters are related to factors such as appetite control, mood, and memory.4,5
These observations warrant further exploration on the influence of the gut microbiome and mental health. There are more bacteria colonized in the digestive system than there are cells in the body. 6 These bacteria can influence brain function and subsequently behavior. Alterations in the composition and quantities of microflora in the gut microbiome can directly and indirectly influence physical and mental health status. A wide array of diseases have been linked to changes in the gut microbiome such as functional gastrointestinal disease, intestinal infection, inflammatory bowel disease, liver disease, gastrointestinal malignancies, obesity, metabolic syndrome, diabetes mellitus, allergies, and autism. 6
Because the gut microbiome is influenced by both genetic and environmental factors, there is a large degree of diversity among individuals. The gut microbiome is made up primarily of Firmicutes, Bacteroidetes, Actinobacteria, Proteobacteria, Fusobacteria, and Verrucomicrobia. The composition of the gut microbiome is influenced by factors such as birth gestational age, delivery type, methods of infant feeding and weaning, age, antibiotic use, and factors such as body mass index (BMI), dietary habits, exercise, and ethnicity. Many studies are exploring the effects of various dietary manipulations through food, diet, and supplements on both gut health and mental health. 7 This column presents a brief review of recently published clinical trials related to gut microbiome interventions that aimed to address a variety of mental health outcomes.
Search Criteria
A PubMed search on “gut health and mental health” with the filters for full text, clinical trial, published in the last 5 years, including adults, human subjects, and written in English, resulted in 25 articles. Upon review of the abstracts, an additional 14 articles were removed (4 were protocols only, 7 did not include a diet or supplement intervention, one was a pilot study, one included children only, and one did not address a mental health outcome), resulting in 11 articles presented here.
Study Subjects and Interventions
Summary of Recently Published Clinical Trials Related to Gut Microbiome Interventions and Mental Health (n = 11).
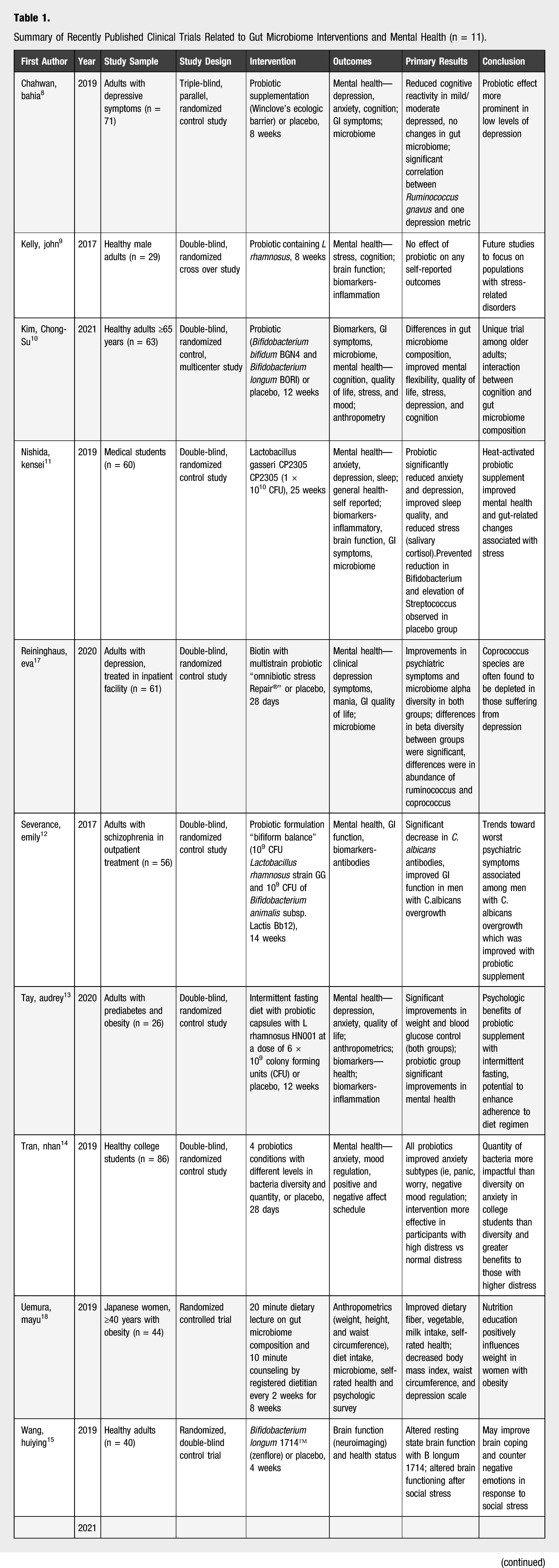
Outcomes Assessed in Studies
A number of mental and physical outcomes were also assessed across studies. These included depression symptoms,8,13,16,17 anxiety,8,11,13,14 cognitive function,8,9 sleep, 11 brain function,9,11,15 self-rated health/quality of life,10,11,13,18 microbiome composition,8,10,12,16-18 GI symptoms,10-12,16,17 inflammatory biomarkers,9,11,13,16 anthropometry,13,18 dietary intake, 18 and chronic disease-related biomarkers (ie, blood glucose, HbgA1c, and blood lipids). 13 Tools for assessing depression, mental health, and anxiety varied across studies but included primarily self-reported methods that utilized assessment types validated for the research setting and participants.
Study Results
Mental Health Outcomes
All ten studies collected self-reported at least one measure of mental health of which two showed improvements in both intervention and control groups16,17 and six showed improvements in self-reported depression, anxiety, and cognition that were significantly greater in the probiotic group.8,10,11,13,14,18 Two studies found no improvement in any mental health outcomes.9,12 One of the two studies that included a measure of sleep found improved sleep latency in the probiotics group, measured objectively with an EEG. 15 Brain function was significantly improved in one study as a result of a social stress situation, also assessed with brain imaging.
Microbiome Composition
Six studies showed positive impacts on gut microbiome composition, with these interventions yielding improvements in composition that were theoretically or statistically linked to positive mental health or cognitive health improvements.8,10,12,16-18
GI Symptoms
Probiotic supplementation’s effect on GI symptoms was mixed. In the five studies that included a measure of digestive health, bowel habits, or symptoms, four found no improvement10,11,16,17 and 1 study, Severence, 12 found significant improvements in self-reported gastrointestinal symptoms. Among the four studies that did not identify any improvement, the study populations were healthy,10,16 stressed, 11 or depressed. 17 In the one study that did observe statistically significant improvements in GI symptoms, the study population that most benefited from probiotic supplementation was men with schizophrenia and overgrowth of yeast, C albicans, where probiotic supplementation aided in attenuating overgrowth of the undesirable yeast. 12
Inflammatory Markers
Four studies included outcomes related to inflammation such as interleukin 6, interleukin 8, tumor necrosis factor, and salivary cortisol.9,11,13,16 Two of these four studies saw significant changes in inflammation through interleukin 6 16 and salivary cortisol 11 in depressed and stressed individuals, respectively. The other two studies that saw no change in inflammatory markers included populations with obesity and prediabetes 13 and healthy individuals. 9
Anthropometry and Dietary Intake
Two studies included anthropometric measures as outcomes, as assessed by body mass index and waist circumference.13,18 Both studies were unique, in that, one focused on nutrition education and counseling on gut health, not probiotic supplementation, for women with obesity and prediabetes. 18 The other study included a probiotic supplement regimen with intermittent fasting for the treatment of obesity and prediabetes. Uemura et al 18 found that the nutrition education led to significantly improved body mass index and waist circumference, largely attributed to improvements in dietary habits. In the study that included intermittent fasting and probiotic supplementation, all participants had significant improvements in weight loss, where the probiotic group also experienced improved social and mental health outcomes. 13
Chronic Disease-Related Biomarkers
One study 13 included blood lipids, hemoglobin A1c, insulin concentration, and insulin sensitivity. There was no significant effect of probiotic supplementation on the observed improvements of these biomarkers.
Discussion
This brief review of recently published clinical trials related to gut and mental health contributes to the knowledge that health care providers can use to determine when probiotic regimens may benefit their patients. Three of the 11 studies included subjects that were free of health conditions, either healthy adults or healthy college students.9,14,16 In one of those studies, social stress was introduced which showed evidence of improved brain functioning when probiotics were supplemented. 16 In the other study of healthy subjects, college students, who are seen as at risk for anxiety and stress, probiotic supplementation improved all mental health outcomes (anxiety, worry, and negative mood regulation). 14 In the last study that included healthy adults, there was no beneficial effect of probiotic supplementation on mental health outcomes such as self-reported stress, cognitive assessments, brain function, or inflammation. 9 This trend suggests that healthy adults without mental health or other health conditions may experience minimal improvement in mental health outcomes such as stress, anxiety, or cognitive function.
Additionally, when considering individuals with existing depression, the effects of probiotic interventions differed across severity of illness. For example, in a study that included adults with depressive symptoms, the impact of the probiotics was found to be more prominent in those with low vs high levels of depression. 8 And going back to the study of college students, the probiotic intervention was more effective in individuals who had higher distress compared with normal distress. 14 Future studies and meta-analysis can help to uncover patterns of effectiveness across the spectrum of mental health disorders.
Poor gut health is associated with gastrointestinal conditions such as irritable bowel syndrome (IBS). There are upwards of 3.5 million physician visits in the United States each year for IBS. 19 The pathophysiology of this condition is poorly understood, but includes abnormalities in the gut microbiome as well as psychosocial stress. The linkage between digestive diseases and mental health warranted the inclusion of GI outcomes in some of the studies identified in this review. Only one 12 of the five10,11,16,17 studies that included GI outcomes identified significant and beneficial impacts of probiotic supplementation. Healthy subjects were the primary populations of interest in two of the four studies that found no impact of probiotics on GI symptoms.10,11 No studies sought to associate GI conditions with mental health outcomes, which is a limitation. The one study that found significant improvements in GI symptoms focused on the use of probiotics in correcting the overgrowth of undesirable gut bacteria in patients with schizophrenia. 12
A notable finding in this review was the observed improvements in mental health in all study participants, regardless of intervention group. For example, in one of the studies that included depressed individuals, depressive symptoms were significantly improved for all study participants, regardless of intervention or control group. 17 This observation was attributed to the effect of interaction with study staff and health care providers treating the patients for intervention. This reinforces the importance of quality patient–provider interactions when providing care for patients with depression, regardless of probiotic use.
Implications for Lifestyle Medicine Practice
Whole-person treatment and intervention strategies are imperative to optimizing outcomes for individuals suffering from mental health and psychologic conditions, as well as those with sub-clinical mental health issues. Mental health is an especially important health issue to address, especially given the COVID-19 pandemic, where lock downs, changes in employment, challenges in providing distance education, and more have taken a toll on the psychologic well-being of individuals globally. 20 Health care providers aiming to provide tools to address mental health issues may consider probiotics in some situations. Providers should be mindful of managing expected outcomes of utilizing probiotics, the benefits of which may be minimal, weigh the cost-benefit ratio of additional medications/supplements to the patients’ treatment regimens. Continuing research on the mental health benefits of probiotics in healthy individuals is necessary.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
