Abstract
Limited research exists examining self-perceived vision and driving ability among individuals with glaucoma, and this study assessed the relationship between glaucoma, visual field, and visual acuity with driving capability.
137 individuals with glaucoma and 75 healthy controls were asked to evaluate self-rated vision, self-perceived driving ability, and self-perceived distracted driving. Visual acuity and visual field measurements were also obtained. Multivariable linear regressions were run to test each visual measure with driving outcomes.
The average age was 72.2 years, 57.3% were male, and 72.5% were White. There were significant associations for a one-point increase in visual field and quality of corrected vision (RR = 1.06; 95% CI = 1.03–1.10), day vision (RR = 1.05; 95% CI = 1.03–1.08), night vision (RR = 1.08; 95% CI = 1.05–1.13), visual acuity score and higher quality of corrected of vision (RR = .41; 95% CI = .22-.77), day vision (RR = .39; 95% CI=.22–.71), and night vision (RR = .41; 95% CI = .18–.94); visual acuity score and ability to drive safely compared to other drivers your age (RR = .53; 95% CI = .29–.96).
Individuals with poorer visual acuity and visual fields rate their vision and ability to drive lower than those with better vision, and this information will allow clinicians to understand where to target interventions to enhance safe driving practices.
“...complete cessation may not be appropriate for all drivers with glaucoma...”
Background
By 2060, the number of Americans aged 65 and older is expected to nearly double from 52 million in 2018, to 95 million. 1 This group will comprise 23% of the total population. As of 2017, there were 44 million licensed drivers over the age of 65. There are 20 older adults killed and 700 injured in motor vehicle crashes every day. 2 Distracted driving is a major cause of crashes across age groups, though less prevalent in older drivers. In our studies and others, drivers feel that the distracted driving of other drivers is more problematic than their own distracted behaviors.3-5 Additionally, glaucoma is one of the leading causes of visual field loss and irreversible blindness worldwide and if left untreated results in loss of contrast sensitivity (CS), visual acuity (VA), and depth perception. 6 Contrast sensitivity is the ability to distinguish the foreground from the background, visual acuity is the finest level of detail that one can detect, and depth perception is the ability to detect distance between elements within an environment.7,8 Currently, 3.4 million individuals have glaucoma in the United States, and this will increase to 5.5 million by 2050. 9 Eye diseases have been shown to increase the risk of motor vehicle crashes. 10 Driving is incredibly important for older adults to maintain a high quality of life as it provides them the opportunity to stay mobile, independent, and socially engaged. Newly diagnosed glaucoma patients report difficulty with glare and peripheral vision at baseline, and over time, visual field loss increases the risk of night driving difficulty, while decreasing visual search and processing speeds. 11 Previous studies have shown that older adults with either impaired vision or newly diagnosed glaucoma are at increased risk of getting a citation, car crashes, at fault errors, and at fault crashes. 12 Due to decreased visual acuity, contrast sensitivity, and depth perception, drivers are often unable to see other vehicles or pedestrians, have difficulties with object recognition, and trouble driving in reduced-light conditions. Drivers with glaucoma have almost double the rate of critical errors related to lane positioning, planning, approach, traffic lights, and yield/give-way intersections compared to those without glaucoma. 13 Other studies have shown an increased avoidance of higher risk driving conditions and higher cessation rates among older adults with glaucoma. Glaucoma is one of the primary reasons that older adults stop driving altogether.14-18
Although it is well established that the effects of glaucoma and additional visual defects increase the risk of injury to older adults, it is unclear why only some individuals choose to modify their driving habits in order to accommodate their condition. The disease may not have impacts on vision that are easy to detect, which may lead individuals to continue driving as they were prior the diagnosis. 19 Additionally, if proper counseling does not occur at the time of diagnosis, individuals may not understand the effects of the disease and will continue to drive while not meeting visual standards. 20 Based on visual field loss, Gramer and Gramer estimated that up to 50% of patients with glaucoma were determined to require counseling on driving. 21 Finally, patients may overestimate their vision and driving capabilities and underestimate their distracted driving, which significantly increases their risk for an error while driving. 13
The aim of this article was to assess the relationship between glaucoma, visual field, and visual acuity with self-rated vision, self-perceived driving ability, and self-perceived distracted driving. This study will provide additional information to clinicians about self-perception in driving ability among drivers with visual impairments. Knowing how vital driving is for older adults’ happiness and overall well-being, it is important to have older adults practice safe driving.
Methods
Data Collection—Survey
Study participants were from a longitudinal study of visual function in glaucoma at the Hamilton Glaucoma Center, University of California, San Diego. 22 The study was approved by the University of California, San Diego Human Subjects Committee. A total of 260 letters were sent to patients that were actively being followed at the center and 212 were mailed back. 75 individuals with a glaucoma diagnosis from a longitudinal study of visual function in glaucoma were recruited to take a driving behavior survey.
137 healthy controls were recruited from the general population, employees, and university staff. Inclusion criteria for controls were as follows: (1) intraocular pressure below 22 mm Hg and no history of elevated intraocular pressure; (2) normal ophthalmologic examination results; (3) at least two reliable normal visual fields in both eyes defined as a pattern SD within the 95% confidence interval and a glaucoma-hemifield test result within normal limits; and (4) a normal appearance of the optic disc on masked grading of stereophotographs.
Glaucoma diagnosis at baseline was assessed using repeatable (≥3 consecutive) abnormal standard automated perimetry (pattern standard deviation P<.05 and/or had glaucoma hemifield test results outside normal limits). If visual field loss was present in at least one eye, a patient was considered to have glaucoma. If patients had any ocular or systemic disease with potential to affect the optic nerve or visual field, they were excluded. Binocular summation of the visual field was calculated by summing the sensitivities of the monocular standard automated perimetry tests of the right and left eyes to calculate an integrated binocular visual field using the binocular summation model as described by Nelson-Quigg et. al. 23 The eye that had better visual acuity was used for the visual acuity measurement in this analysis.
Questions to Assess Self-Rated Vision, Self-Perceived Ability, and Self-Perceived Distracted Driving from the Older Adult Cell Phone Survey.

Statistical Analysis
Baseline demographics, visual measures, and survey responses were reported overall and by glaucoma status. Multivariable linear regression models were applied to investigate the associations between glaucoma, binocular summation of the visual field, and visual acuity with self-rated vision, self-perceived driving ability, and self-perceived distracted driving. Glaucoma, binocular summation of the visual field, and visual acuity were tested independently with each outcome. Models were adjusted for sex and age. All statistical analyses were performed using SAS University Edition. A two-sided alpha level was set at .05.
Results
The study included 212 participants who had mailed back complete surveys and copies of their consent forms. The average age of participants was 72.2 years (SD=10.8 years), and 57.3% were male. The majority of participants were White (72.5%) followed by Black (18.8%) and Other (8.7%).
Baseline Demographics, Clinical, and Self-Reported Driving Characteristics.
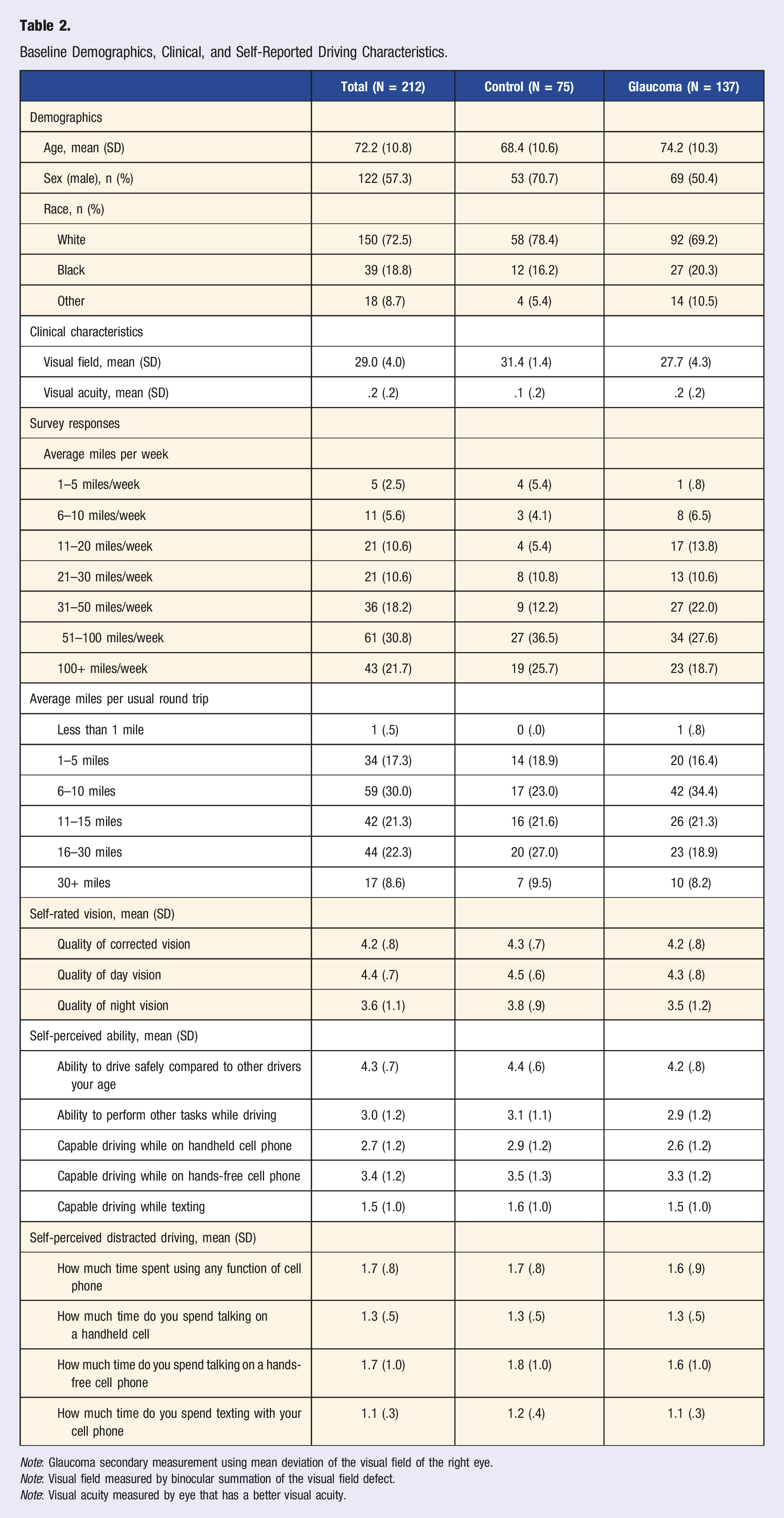
Note: Glaucoma secondary measurement using mean deviation of the visual field of the right eye.
Note: Visual field measured by binocular summation of the visual field defect.
Note: Visual acuity measured by eye that has a better visual acuity.
The average self-rated quality of corrected vision (1 = Poor; 5 = Excellent) was 4.2 (SD = .8), the self-rated quality of day vision was 4.4 (SD = .7), and self-rated quality of night vision was 3.6 (SD = 1.1). Although the self-perceived ability to drive was high, the self-perceived ability to drive while talking on a handheld cell-phone or texting was much lower. For self-perceived ability to drive, higher scores indicate higher self-confidence. The average scores were as follows: ability to drive safely compared to other drivers your age: 4.3 (SD = .7), ability to perform other tasks while driving: 3.0 (SD = 1.2), capable driving while on handheld cell phone: 2.1 (SD = 1.2), capable driving while on hands-free cell phone: 3.4 (SD = 1.2), and capable driving while texting: 1.5 (SD = 1.0). Distracted driving behaviors (1 = Never and 5 = Frequently) were not highly reported in this population. The average responses were as follows: how much time spent using any function of cell phone: 1.7 (SD = .8), how much time do you spend talking on a handheld cell phone: 1.3 (SD = .5), how much time do you spend talking on a hand-free cell phone: 1.7 (SD = 1.0), and how much time to do you spend texting with your cell phone: 1.1 (SD = .3) (Table 2).
The Association of Glaucoma Status With Self-Rated Vision, Self-Perceived Driving Ability, and Self-Perceived Distracted Driving Comparing Patients With Glaucoma to Controls.
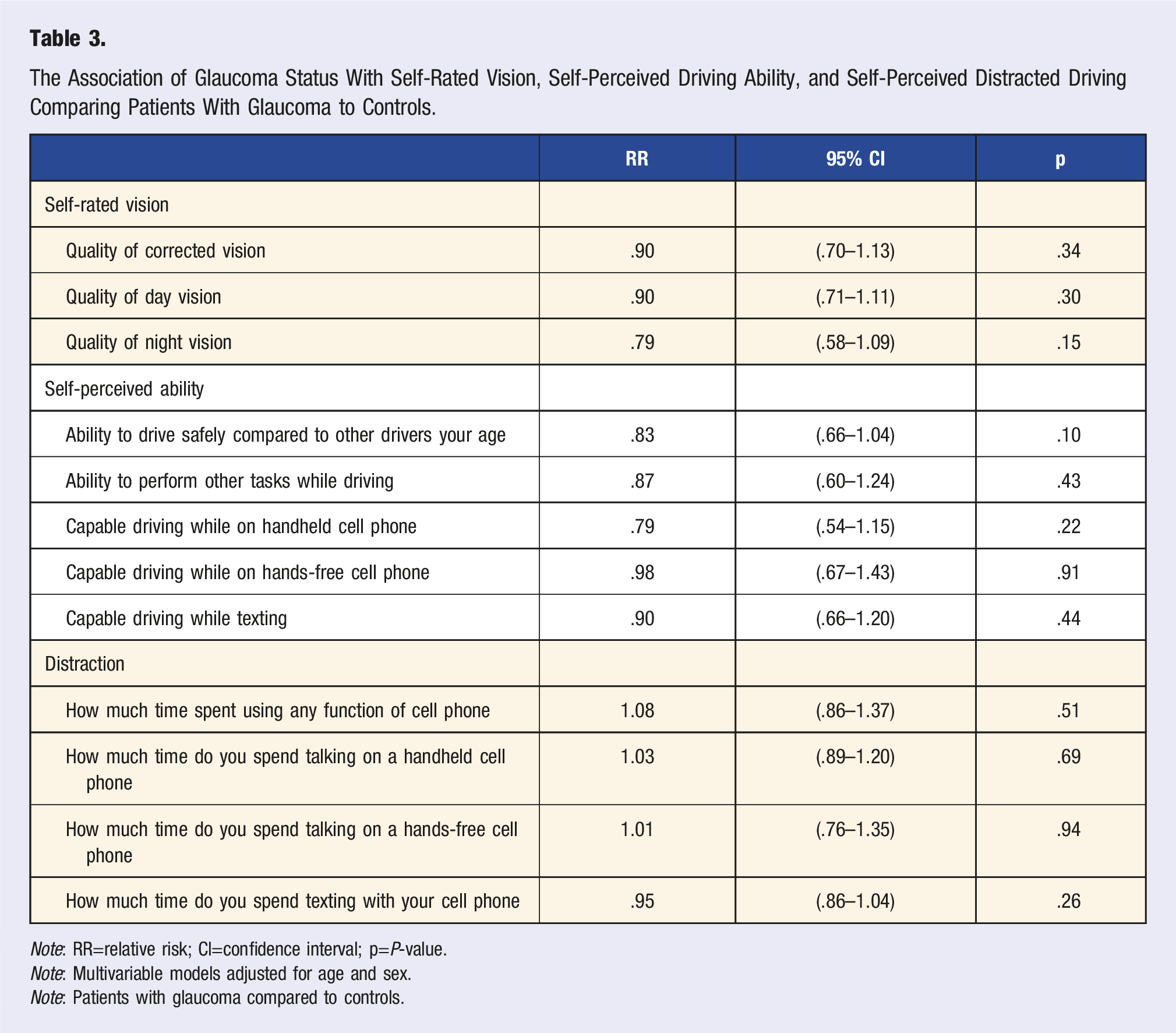
Note: RR=relative risk; CI=confidence interval; p=P-value.
Note: Multivariable models adjusted for age and sex.
Note: Patients with glaucoma compared to controls.
The Association of Visual Field With Self-Rated Vision, Self-Perceived Driving Ability, and Self-Perceived Distracted Driving Comparing Patients With Glaucoma to Controls.
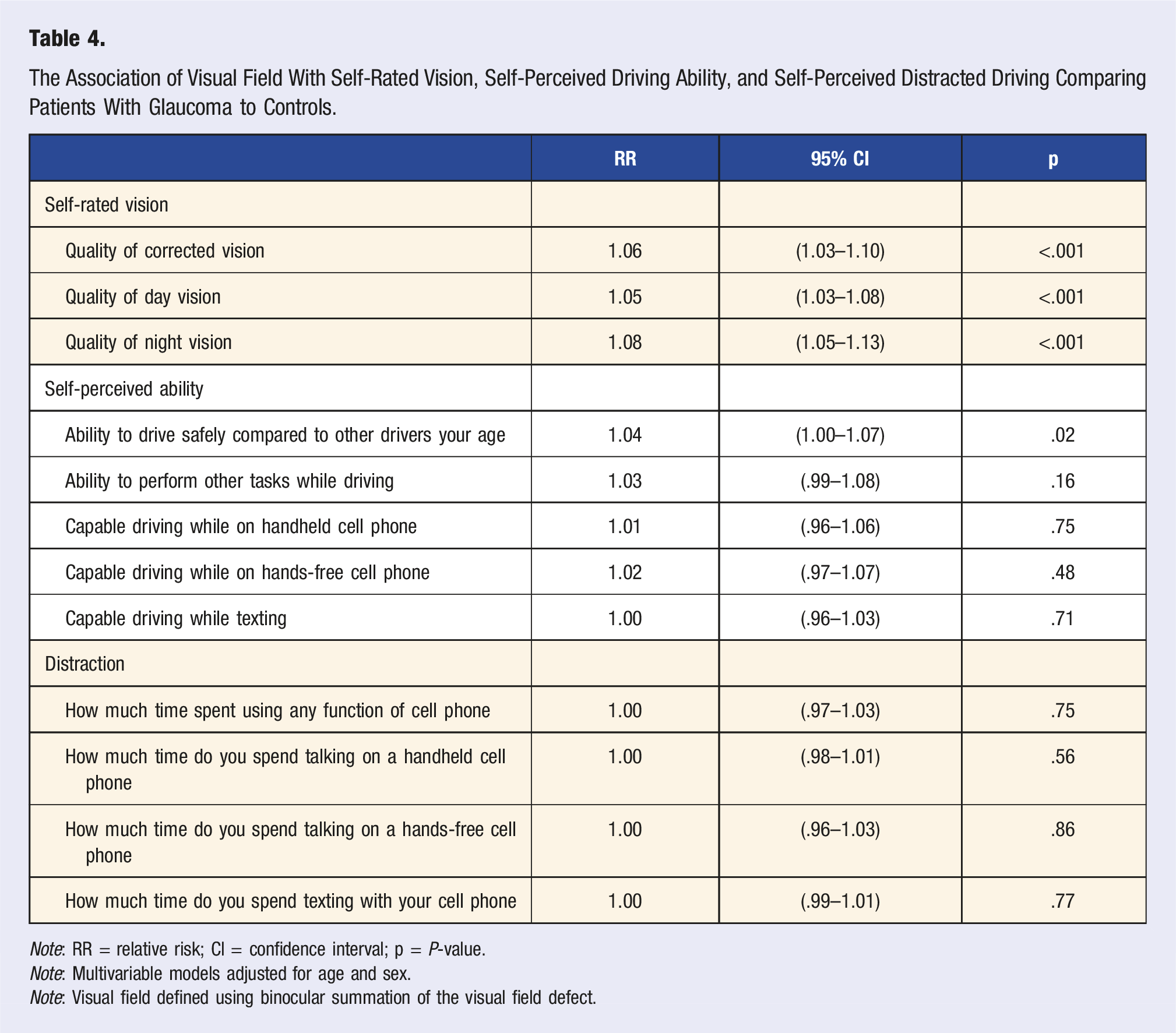
Note: RR = relative risk; CI = confidence interval; p = P-value.
Note: Multivariable models adjusted for age and sex.
Note: Visual field defined using binocular summation of the visual field defect.
The Association of Visual Acuity With Self-Rated Vision, Self-Perceived Driving Ability, and Self-Perceived Distracted Driving Comparing Patients With Glaucoma to Controls.
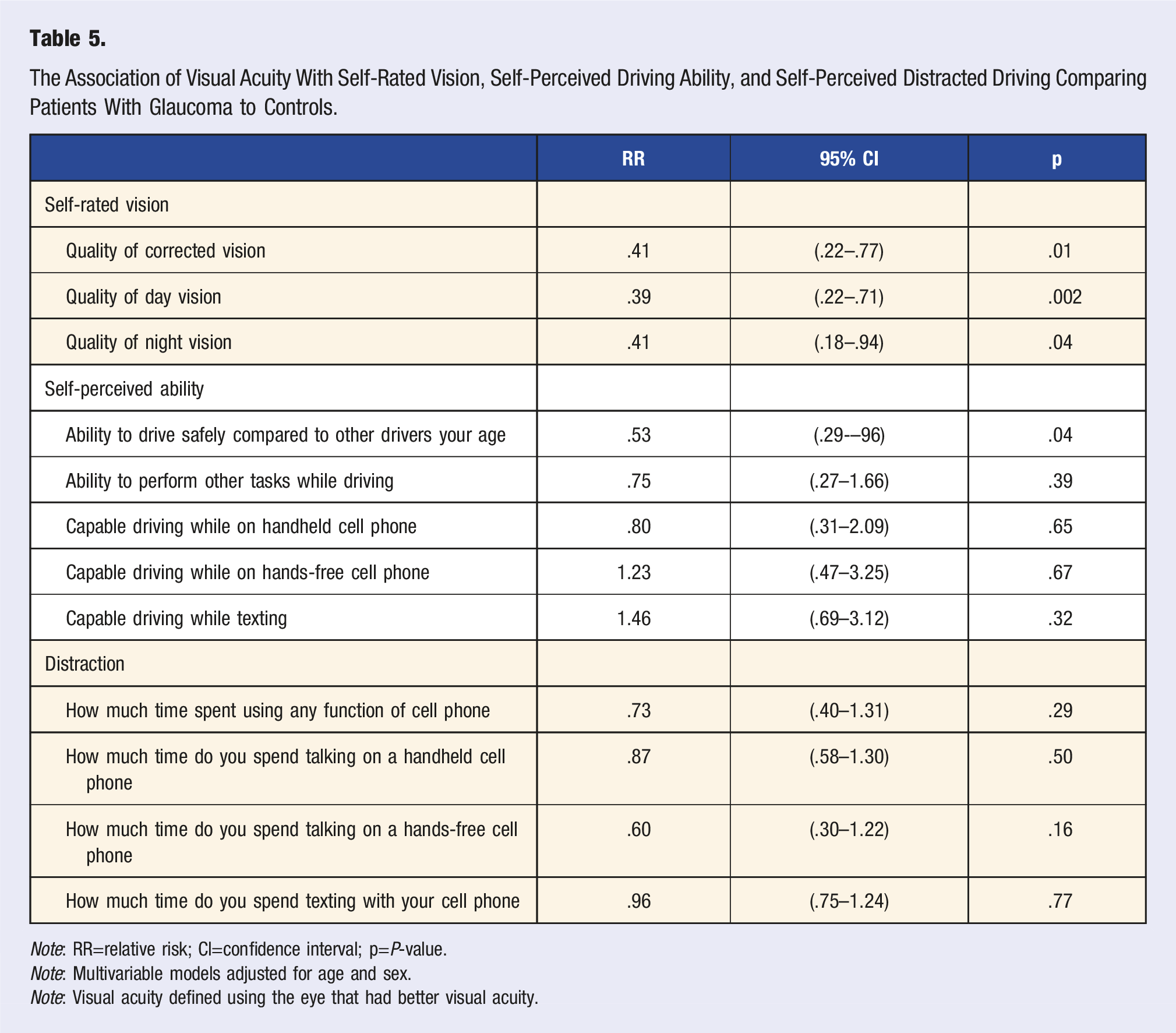
Note: RR=relative risk; CI=confidence interval; p=P-value.
Note: Multivariable models adjusted for age and sex.
Note: Visual acuity defined using the eye that had better visual acuity.
Discussion
This study assessed self-rated vision, self-perceived driving ability, and self-perceived distracted driving among older adults. We did not find that patients diagnosed with glaucoma had any significant differences in self-related driving measures compared to controls. Higher objectively measured visual field (better) was associated with higher self-rated vision, while higher objectively measured visual acuity score (worse) was associated with lower self-rated vision. We did not observe a relationship with either visual acuity or visual field and self-perceived ability to drive or self-perceived distracted driving. It was interesting to find that while glaucoma status did not predict self-rated vision, worse visual field and visual acuity measurements did. Additionally, while worse visual acuity and visual field were associated with worse self-rated vision, these objective measures were not associated with differences in self-perceived ability to drive or the amount of time spent driving distracted.
These findings are concerning considering that those with glaucoma or worse visual outcomes do not have significant differences in perceptions on their ability to drive and how much time they spend driving distracted. Another study found that most older drivers rated themselves as good or excellent drivers regardless of their citation or crash rate. Self-rated driving was not found to be associated with actual driving proficiency as indicated by previous crash involvement in older adults. 24 Despite evidence of the risk of driving distracted, individuals in general tend to overestimate their distracted driving capabilities. When drivers in one study were asked if talking on the phone or sending messages made a difference in their driving ability, 54% of participants said that talking on a handheld device made no difference, and 25% said texting or sending messages made no difference to their driving performance. 25 Although a 2014 study found that many distracted drivers engaged in that behavior despite knowing the risks, many older adult participants perceived their own driving ability as good or excellent while driving distracted, suggesting that they failed to recognize the impact that distracted driving had on their driving safety. 26
Drivers that experience glaucoma-related visual field loss or have worse visual acuity, contrast sensitivity, or lower peripheral visual fields have been found to be more likely to stop driving. 17 One study did not find any demographic or clinical factors that were associated with older drivers’ self-awareness of changes in driving ability over time. However, two studies found a marginal effect in self-awareness of changes in driving ability over time associated with changes in visuo-motor processing speed and executive functioning measured by the Trail Making Test. 27 There is very limited research on when people with glaucoma decide to change their driving habits, what factors are associated with those changes, and if those changes are sufficient in reducing their risk of injury and death due to driving with lower quality vision. 18 Older drivers would benefit from recommendations from physicians and family members through physician counseling, driver evaluations, and advanced driving directives in order to introduce and implement driving cessation in their lives if deemed appropriate. 28
The benefits of driving cessation including fewer injuries and potential deaths should be weighed in the face of the potential downsides related to overall health, happiness, and quality of life. Driving is a primary factor in the maintenance of independence in the lives of older adults, and a large majority of older drivers rate driving as “completely important regardless of their residence in an urban, suburban, or rural area.” 29 When older adults stop driving, they may face many issues including a decline in overall health, physical, social, and cognitive function with an increased risk of depression and social isolation. 27 These related outcomes may result in transitioning from the community to long-term care facilities or increased risk of mortality. 30 Any strategies to reduce or stop older adults driving must be accompanied with strategies that provide accessibility to frequented destinations through alternative transportation methods in order to optimize well-being and quality of life.
While driving cessation may be appropriate for those individuals who experience significant declines in visual functions required for safe driving, complete cessation may not be appropriate for all drivers with glaucoma. It may be safe for some patients to continue driving with specific modifications to ensure safety such as avoiding highways and nighttime driving. 31 The use of an occupational therapist can often be useful to identify and guide an individual with glaucoma on driving and community mobility based on their new limitations and to enroll them in appropriate patient education programs. Finally, vision rehabilitation by therapists using low vision training can be an integral part of a team to maximize the usable vision that prioritizes individuals’ health and well-being through participation in everyday activities. 32
There are a few limitations in this study. This study included self-reported driving behaviors, including distracted ability and distracted driving rather than objective measures. However, older adults are likely to overreport their ability to drive safely and underreport their distracted driving; thus, making the results presented in this study conservative. Additionally, this study included participants that were still driving and thus may also be a group of individuals that is likely to continue driving despite lower quality of vision. Future studies should incorporate objective measures of driving capability and distracted driving and also aim to increase the sample size of the study. The sample characteristics are representative of older adult drivers, and this study is generalizable to older adult drivers in the United States. There are also several strengths to this study. The visual measurements in this study were completed objectively at baseline and prior to the completion of the driving survey. The survey was based on a previously validated survey and there was a high response rate among those that the survey was distributed to.
Despite potentially reduced visual acuity and visual fields, participants with glaucoma had the same self-perceived driving ability, distracted driving ability, and distracted driving behaviors compared to participants without glaucoma. Additional research would be required to understand if individuals with glaucoma who have worse visual measures practice more unsafe driving behaviors and/or experience harmful outcomes related to driving. Ongoing education and training of the public is required by multiple sectors including physicians, public health officials, and law enforcement in order to transition older adults into safer driving practices.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
