Abstract
Rates of type 2 diabetes mellitus continue to rise around the world, largely due to lifestyle factors such as poor diet, overeating, and lack of physical activity. Diet and eating is often the most challenging aspect of management and, when disordered, has been associated with increased risk for diabetes-related complications. Thus, there is a clear need for accessible and evidence-based interventions that address the complex lifestyle behaviors that influence diabetes management. The current study sought to assess the efficacy and acceptability of a pilot lifestyle intervention for women with type 2 diabetes and disordered eating. The intervention followed a cognitive behavioral therapy guided-self-help (CBTgsh) model and included several pillars of lifestyle medicine, including: diet, exercise, stress, and relationships. Ten women completed the 12-week intervention that provided social support, encouraged physical activity, and addressed eating behaviors and cognitions. Results indicate the lifestyle intervention was a feasible treatment for disordered eating behaviors among women with type 2 diabetes and was also associated with improved diabetes-related quality of life. The intervention was also acceptable to participants who reported satisfaction with the program. The current CBTgsh lifestyle intervention is a promising treatment option to reduce disordered eating and improve diabetes management.
‘Importantly, a subset of individuals with type 2 diabetes also engage in eating behaviors that are disordered, which may interfere with diabetes management and cause significant distress.’
The steadily increasingly rates of Americans diagnosed with type 2 diabetes mellitus is related to numerous risk factors that are influenced by lifestyle, including poor dietary habits, overeating, and sedentary behavior. 1 For some individuals, typically those who are closer to a healthy blood glucose and at low risk for diabetes-related complications, type 2 diabetes can be managed entirely through engagement in disease-appropriate lifestyle behaviors such as dietary changes, physical activity, and blood-glucose monitoring. 2 For others, lifestyle behaviors are an important adjunct to other medical therapies. Lifestyle recommendations are some of the most common for diabetes management, indicating the potential value of these interventions. 3 Despite the importance of diabetes self-management, behavior change and maintenance is challenging for many, as it requires high levels of knowledge and motivation. 4
Eating behavior is a pivotal aspect of diabetes management, and thus one of the most important areas for intervention. Importantly, a subset of individuals with type 2 diabetes also engages in eating behaviors that are disordered, and may interfere with diabetes management and cause significant distress. Given the role of diet in blood glucose management, and ultimately diabetes outcomes, such disordered eating behaviors can be detrimental to outcomes and quality of life. Yet few interventions specifically address eating behaviors and related cognitions for individuals who struggle with disordered eating behaviors.
What Is Disordered Eating and Why Is It a Problem?
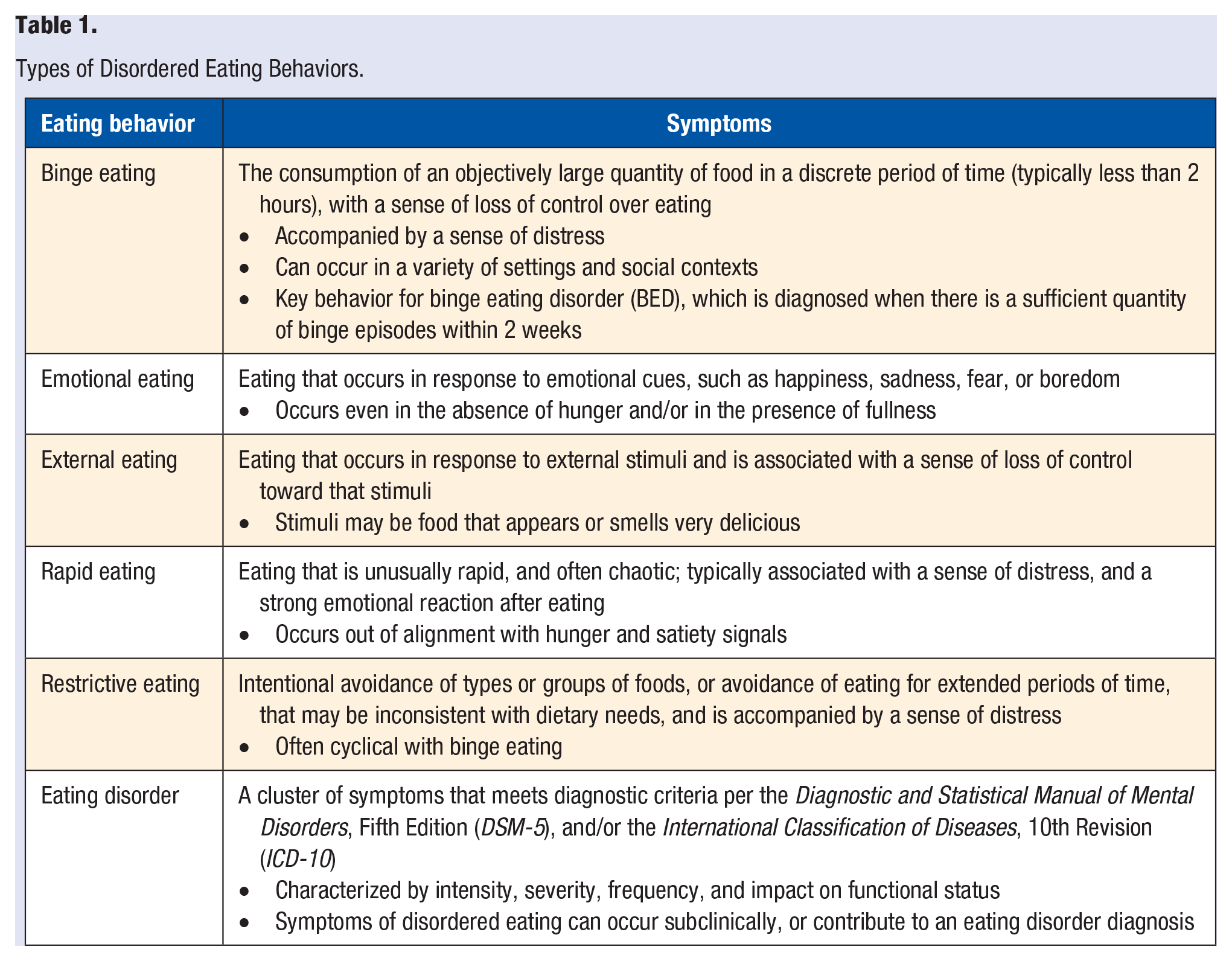
Disordered eating behaviors include binge eating (consuming a large amount of food in a discrete period of time with a sense of loss of control), emotional eating (eating in response to emotional cues), external eating (eating in response to external stimuli), eating that is rapid and chaotic, and restriction (avoidance of food groups, types of foods, or for long intervals).4,5 Of note, disordered eating refers to (clusters) of behaviors associated with distress, that may be related to, but do not meet criteria for a clinically significant eating disorder, such as binge eating disorder 6 (Table 1).
Types of Disordered Eating Behaviors.
For individuals who do engage in disordered eating behaviors, the potential implications for diabetes-related outcomes are numerous, and include increase in body mass index (BMI), poor glycemic control, diabetes distress, and lower quality of life.5,7 For individuals with type 2 diabetes, disordered eating alone can exacerbate risk for diabetes-related complications such as cardiovascular disease, and even subthreshold disordered eating symptoms are associated with severe and problematic health outcomes. 8 Research also has demonstrated that those who suffer from both disordered eating and type 2 diabetes are at greater risk for a number of serious health complications. 9
Notably, disordered eating is thought to occur more often in patients with type 2 diabetes than in the general population because diabetes-related stress can lead to overeating, major weight changes, and attempts to maintain diabetic-specific diets that are low in carbohydrates and sugars.8,10 These factors, related to key type 2 diabetes management behavior, may in turn exacerbate risk for disordered eating. Despite the understanding that disordered eating can exacerbate risk for diabetes-related complications, the current state of the literature suggests disordered eating is seldom addressed as part of diabetes self-management. The combination of high rates of type 2 diabetes mellitus and difficulties making lifestyle changes indicate the need for further development of accessible, cost-effective, treatment modalities to address disordered eating in populations with type 2 diabetes.
Lifestyle Interventions for Diabetes
The 2014 Community Prevention Services Task Force reported that programs focused on interventions that employed a combination of dietary change and physical activity were effective in the prevention of complications for individuals with recently diagnosed type 2 diabetes. 2 Furthermore, lifestyle interventions to prevent and treat diabetes, including the diabetes prevention program, have continued to emerge in recent years.11,12 The benefits of multifactorial lifestyle interventions include the attention to multiple, related lifestyle behaviors (ie, diet, stress management), as well as evidence-based interventions to facilitate sustainable changes that are incorporated into daily life. 13 The American College of Lifestyle Medicine emphasizes 6 key lifestyle pillars: diet, exercise, sleep, stress, interpersonal relationships, and tobacco cessation. These pillars align with the foundational aspects of lifestyle behaviors discussed in the empirical literature to date.14,15
Given the nature of diabetes management, and potential interference of disordered eating behaviors, the pillars of diet, exercise, stress, and relationships, are particularly relevant and offer opportunity to address disordered eating, as it affects diabetes management. Of note, for decades, the fields of health psychology and behavioral medicine have been employing interventions that combine traditional evidence-based psychotherapeutic approaches, such as cognitive behavioral therapy (CBT), with foundational aspects of lifestyle interventions, such as diet and physical activity, to address comorbid mental and physical health conditions. However, a lifestyle intervention to address disordered eating and improve lifestyle behaviors among women with type 2 diabetes, is a novel approach.
Evidence-Based Interventions for Disordered Eating
While lifestyle interventions alone may be effective for some women with diabetes, disordered eating is understood to be a barrier to lifestyle change, particularly in the context of diet and eating. Distress related to eating has been associated with negative implications for other lifestyle factors such as interpersonal relationships and exercise. 16 Based on the existing literature, intervening to reduce disordered eating behaviors may reduce the burden of dietary adherence and, thus, could lead to improved diabetes management. 17 CBT is the gold-standard psychotherapeutic intervention for many conditions and has been demonstrated to be a highly effective treatment for disordered eating behaviors. The goal of CBT is to eliminate rigid patterns of thinking in order to facilitate change in maladaptive eating behaviors and to establish a healthy pattern of eating. 18 A 2002 study assessed a group-based CBT intervention for binge eating among women with type 2 diabetes, and found CBT to be an effective intervention for binge eating, mood, and glycemic control. 8 Addressing disordered eating may also lead to improvements in important diabetes-related outcomes including maintaining an appropriate BMI, glycemic control, distress, and quality of life.10,17
However, traditional CBT is a form of psychological treatment that can only be provided by a trained clinician, such as psychologist and, thus, can be expensive and inaccessible to some populations. As an evidence-based intervention, CBT is distinct from the application of CBT principles, which may be utilized by a greater range of providers. To address the cost and accessibility issues of CBT, a guided self-help version of the CBT protocol for binge eating (CBTgsh) was developed. The intention of CBTgsh was to address barriers to treatment by providing participants with an opportunity to follow a self-help manual while also receiving guidance from a “supporter” who aids the participant in employing the manual, still allowing for some of the benefits of traditional CBT. 19 Research has indicated that CBTgsh programs are effective in reducing binge eating symptoms for women of various racial and ethnic groups.20,21 To date, CBTgsh has not been employed with women with comorbid disordered eating behaviors and a chronic medical problem, such as type 2 diabetes. Of note, much of the research to date on disordered eating among populations with and without type 2 diabetes mellitus has been conducted with female samples.22,23
Purpose of the Current Study
The current feasibility study sought to assess the efficacy and acceptability of a low-cost, highly accessible, lifestyle intervention, coupled with CBT principles and interventions, for women with type 2 diabetes who self-reported difficulties with eating behaviors and associated distress. The combination of lifestyle intervention with CBT principles sought to address disordered eating behaviors from both psychological and behavioral perspectives, while supporting participants to achieve sustainable lifestyle changes that would benefit not only disordered eating behaviors but also diabetes management and quality of life. A feasibility study, which can be used to assess the need for further study of an interventions, was warranted given minimal study of interventions for disordered eating among individuals with type 2 diabetes. The current study addressed 2 areas of the 8 areas of focus within feasibility studies: efficacy-testing, which is the assessment of an intervention with a small or convenience sample, and acceptability, which assesses how intended recipients view the intervention. 24
The primary outcomes expected as a result of the current intervention included (1) the reduction of the frequency and severity of disordered eating behaviors and (2) satisfactory participant ratings of the intervention. We also expected the intervention would indirectly contribute to secondary diabetes-related outcomes, including reduction of diabetes-related distress and improved diabetes-related self-efficacy and quality of life. All outcomes were assessed via self-report. In sum, the current study examined the feasibility and acceptability of a multicomponent CBTgsh lifestyle intervention to improve disordered eating behaviors among women with type 2 diabetes.
Methods
The current human subjects research was dually approved by the Carolinas Medical Center (now Atrium Health) and the University of North Carolina at Charlotte’s Institutional Review Boards, and conforms to all recognized standards. Participants were recruited via flyers and emails at a large public university and from community health care organizations in an urban southeastern setting. Inclusion criteria included self-reported type 2 diabetes mellitus diagnosis, female gender, at least 18 years of age, and self-report of current disordered eating behavior. Disordered eating was assessed in a phone-based prescreen and was confirmed by trained research assistants who asked select questions from the Eating Disorder Questionnaire 25 to determine both behaviors and associated distress. At prescreen, potential participants were also asked to provide one or more examples of disordered eating behaviors, to confirm eligibility. Fifteen women were screened and eligible for the current study. Of the eligible individuals, 4 refused/declined participation. Ten women completed all sessions of the 12-week intervention and follow-up assessment, and 1 women completed 4 sessions before dropping out. The participant who dropped out was distinct from the sample in regard to both greater BMI and severity of disordered eating, and therefore was excluded from all analyses.
Measures
Age, race/ethnicity, height, and weight, level of education, and annual income were collected via self-report. Diabetes history was collected via self-report to assess diagnostic history, current diabetes treatment, and most recent HbA1c. BMI, the gold-standard indirect indicator of body fatness, was calculated using self-reported height and weight by dividing weight in pounds by height in inches squared and multiplying by 703. 26 Disordered eating was assessed using the Eating Disorder Examination Questionnaire (EDE-Q) and the Dutch Eating Behaviors Questionnaire (DEBQ).16,27 The EDE-Q, a 41-item self-report questionnaire, is an adaptation of the Eating Disorder Examination, used to assess problematic eating behaviors, such as binge eating. A higher overall score on the EDE-Q suggests greater eating pathology. Scores for the EDE-Q range from 1 to 6, with higher scores indicating more severe eating, shape, and weight concerns.16,28 For the external eating subscale DEBQ, participants responded using a scale ranging from 1 to 5, where higher scores are indicative of greater external eating. The external eating subscale has demonstrated high internal consistency, as well as appropriate validity. 27
Diabetes distress, emotional distress specific to diagnosis and management of diabetes, was assessed with the 17-item Diabetes Distress Scale (DDS); higher scores are indicative of greater distress. The DDS has been empirically validated and is a reliable measure of diabetes distress for individuals with type 2 diabetes mellitus. 29 The 8-question Diabetes Self-Efficacy Scale (DSES) assessed self-efficacy specific to type 2 diabetes mellitus management. Higher scores on the DSES relate to greater self-efficacy, or self-confidence to effectively manage diabetes. The DSES has demonstrated appropriate content and construct validity, internal consistency, and stability. 30 Diabetes quality of life was assessed by the diabetes-related quality of life. Higher overall score as well as score on the satisfaction subscale are indicative of better diabetes quality of life. The measure has demonstrated reliability and validity for individuals with diabetes who use other forms of management strategies as well as medication. 31 Blood glucose was assessed at baseline by most recent self-reported hemoglobin A1c (HbA1c).
Participant satisfaction with the intervention was assessed at follow-up by the 8-item Client Satisfaction Questionnaire, 8th Edition (CSQ-8). Participants responded using a scale ranging from 1 to 4. Higher scores indicate greater satisfaction with the intervention. The CSQ-8 has demonstrated appropriate reliability, construct validity, criterion validity, and internal consistency. 32 Participants also completed 5 open-ended questions to assess acceptability of the program. Open-ended questions addressed likes, dislikes, suggested changes, recommendations, and opportunity for additional feedback.
Intervention
Eligible participants completed an in-person orientation session during which they were administered electronic baseline questionnaires. Participants received a copy of the lifestyle intervention manual, an electronic spreadsheet for daily food and physical activity monitoring, and a scale for measuring their weight. The intervention consisted of eight 20-minute phone-based support sessions to guide participants through the 12-week lifestyle intervention. Sessions took place weekly for 4 weeks and biweekly for 8 weeks. The supporter’s role was to guide the participant through the program while also providing encouragement and positive feedback. Supporters were female graduate and undergraduate students who completed a semistructured training protocol on delivery of the intervention. Supporters also engaged in regular supervision from program faculty during weekly lab meetings.
Participants followed the 8 steps outlined in the self-help manual adapted for this study (“A Lifestyle Guide: Managing Eating and Physical Activity,” unpublished), which incorporates steps from Fairburn’s CBT grounded book Overcoming Binge Eating, in conjunction with established daily physical activity and fruit and vegetable consumption recommendations.16,33 Consistent with CBT, the intervention focuses on food monitoring, establishing a regular pattern of eating, development and use of strategies to prevent disordered eating behaviors, and relapse prevention. To complement the eating behavior components, discussion of strategies to increase physical activity, and fruit and vegetable consumption, occurred throughout the intervention. Stress associated with disordered eating, and the role of interpersonal relationships in addressing disordered eating and lifestyle change, was also incorporated throughout. At the end of the 12-week intervention, participants completed follow-up versions of the questionnaires online. Participants received up to $75 in the form of gift cards as compensation.
Analysis
The primary outcomes expected as a result of the intervention included the reduction of the frequency and severity of disordered eating behaviors, and that participants would rate the intervention as acceptable and satisfactory. We also expected the intervention would indirectly contribute to secondary diabetes-related outcomes, including reduction of diabetes-related distress and diabetes-related self-efficacy, and improvement of diabetes quality of life. Paired t tests were conducted to examine changes in disordered eating behaviors and secondary outcomes from pre- and postintervention.
Qualitative analysis was employed to analyze open-ended responses regarding participant’s assessment of the intervention, including likes, dislikes, suggested changes, and recommendations. Constant-comparative analysis was used to develop themes while focusing on participant’s lived experiences and patterns among those experiences. 34 Qualitative analyses were conducted by a 2-person coding team, with agreed-upon themes. Disagreements regarding themes were resolved through discussion until consensus was reached. Validity of the results is supported by triangulation, or convergence among sources of information, in this case, participants’ reports of subjective experience. 35
Results
Participant characteristics of the final study sample (N = 10) are presented in Table 2. On average, participants were 49.5 years old (SD = 7.28), all were overweight or obese (BMI = 34.15; SD = 4.55), and had been diagnosed with type 2 diabetes mellitus for an average of more than 7 years. Regarding the primary outcome, there was a statistically significant reduction from pre- to posttreatment in disordered eating behaviors, including binge eating, as measured by the EDE-Q total score and each of its subscales (Table 3). Women also reported decreased problematic eating behavior assessed with the DEBQ, especially external eating, and a significant change in perception of one’s weight and shape. In consideration of the secondary outcomes, participants reported a statistically significant increase in diabetes quality of life from pre- to postintervention (Table 3). No further statistically significant changes emerged with respect to diabetes self-management.
Participant Characteristics (N = 10).
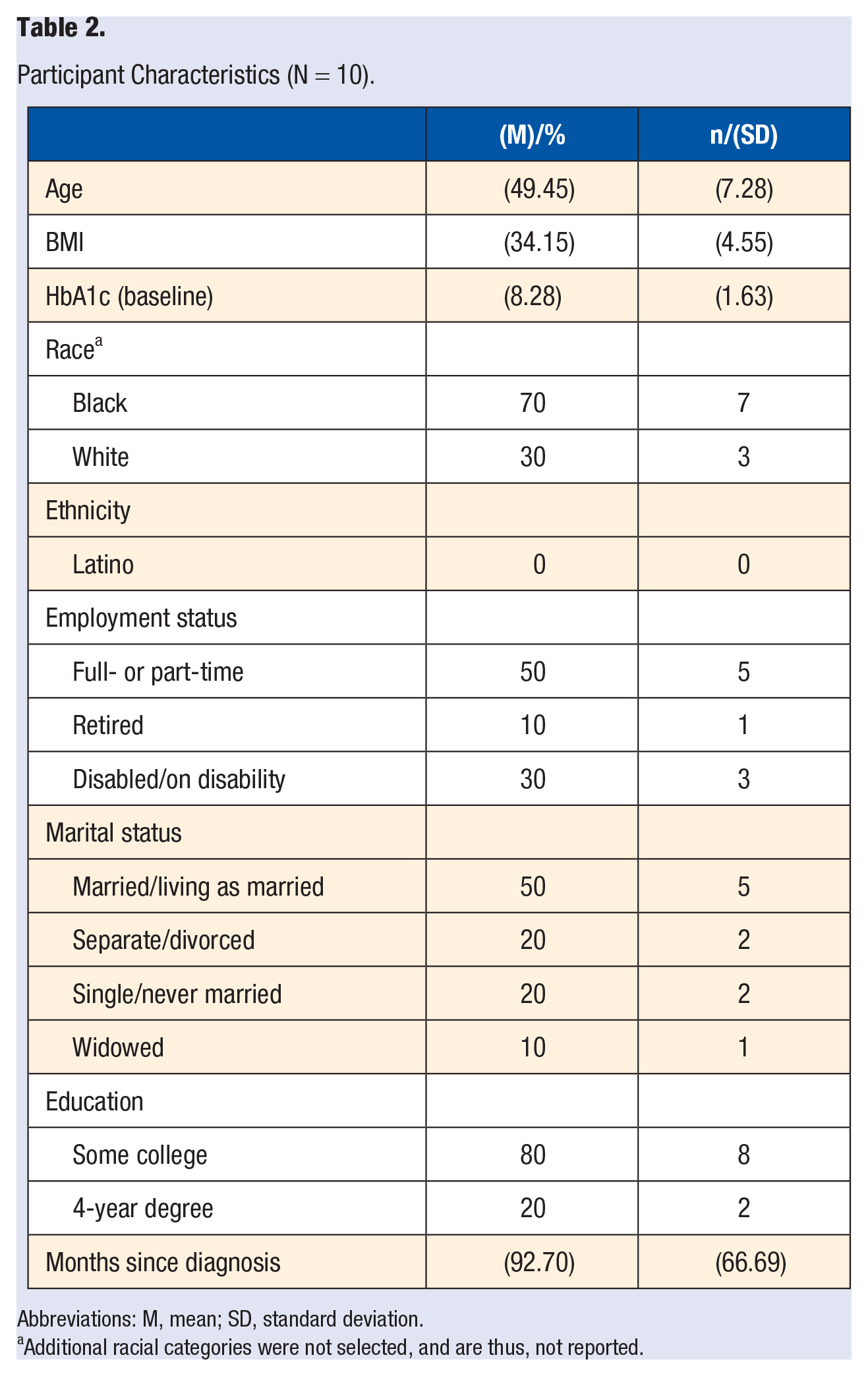
Abbreviations: M, mean; SD, standard deviation.
Additional racial categories were not selected, and are thus, not reported.
Disordered Eating, Diabetes, and Participant Satisfaction Outcomes.
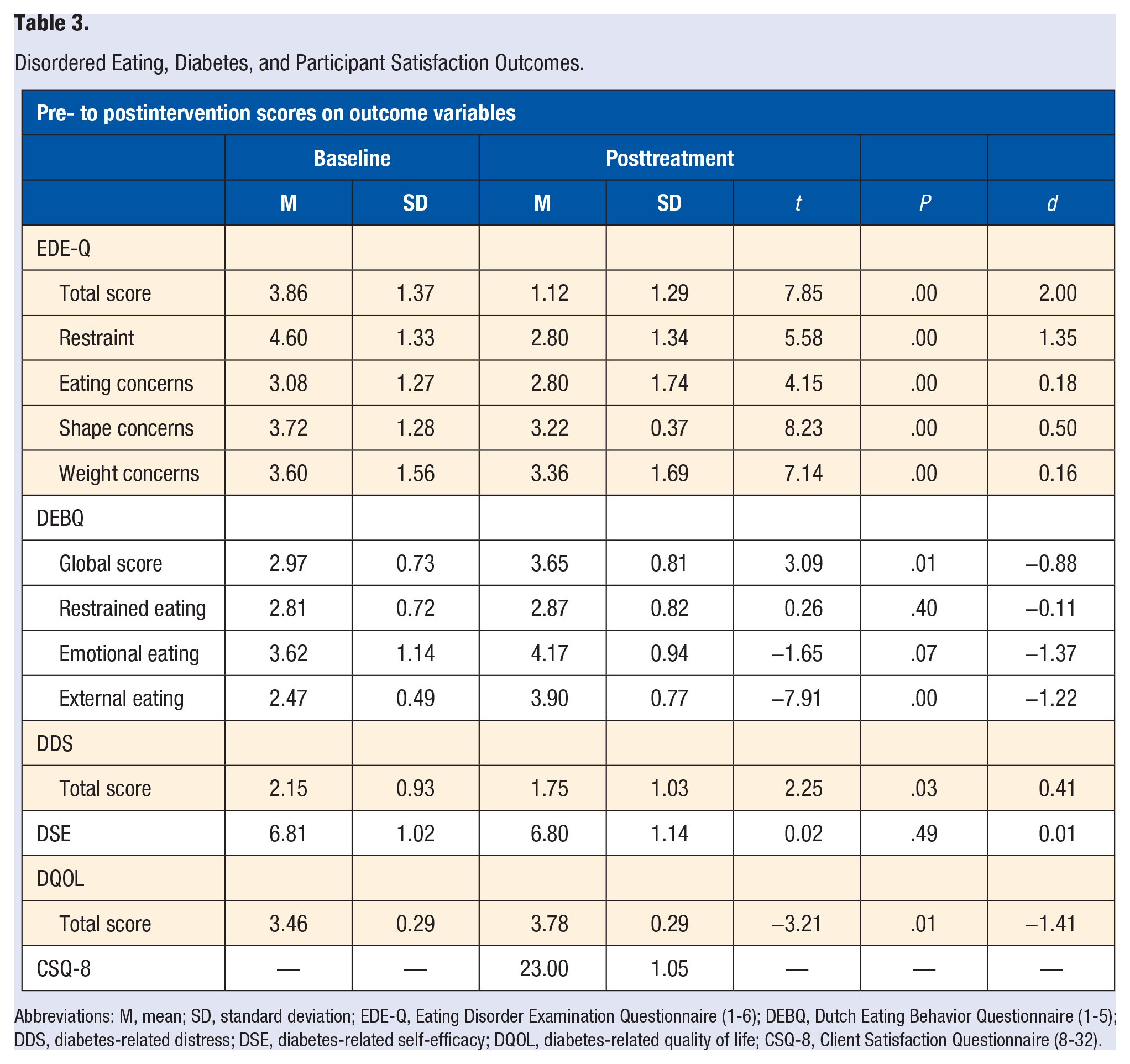
Abbreviations: M, mean; SD, standard deviation; EDE-Q, Eating Disorder Examination Questionnaire (1-6); DEBQ, Dutch Eating Behavior Questionnaire (1-5); DDS, diabetes-related distress; DSE, diabetes-related self-efficacy; DQOL, diabetes-related quality of life; CSQ-8, Client Satisfaction Questionnaire (8-32).
Acceptability
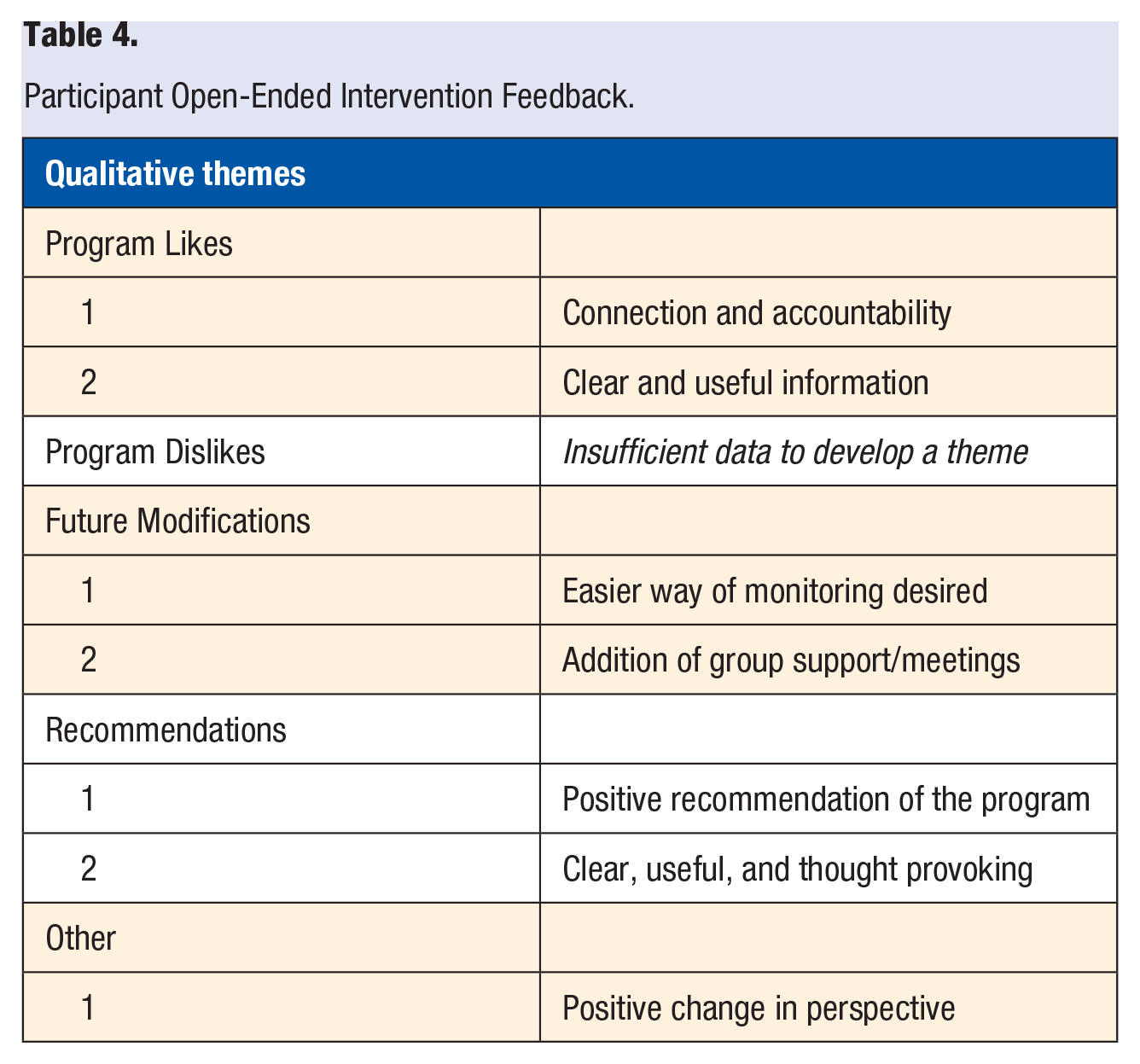
Results on the CSQ-8 indicated moderately high satisfaction with the intervention (M = 23.00, SD = 1.05). An examination of the open-ended questions revealed several themes (Table 4). Overall, participants reported predominantly positive feedback. For example, one participant reported that “I would recommend it to others to get real current information about others like us. There is less judgment in the material and it confirms for women that we are not alone in our pursuit of better health.” Participant feedback was full of pride, and suggested they were positively impacted by the intervention. “It helped me want to manage my diabetes instead of just letting it go,” is one example of the “other” theme. Further indicative of an acceptable intervention, participants described appreciation for the regular support calls that provided a sense of connection and accountability, in line with the stress and relationship pillars of lifestyle medicine.
Participant Open-Ended Intervention Feedback.
Discussion
Overall, the results indicated the intervention is a feasible treatment to support the reduction of disordered eating behaviors, such as binge eating and external eating, for women who report disordered eating behaviors and associated distress. The decrease in focus on one’s weight and shape demonstrated the multifaceted reduction in overall disordered eating behaviors and related cognitions addressed by the intervention. Such change is essential, as overvaluation of one’s weight and shape has been linked to binge eating, and probable binge eating disorder, as well as to greater difficulty with emotion regulation. 36 These findings highlight the potential utility of CBTgsh interventions to address disordered eating among women with type 2 diabetes mellitus.
Though the intervention did not directly target or discuss diabetes management, results illustrate that the intervention had a positive impact on diabetes quality of life (satisfaction with treatment, impact of diabetes on daily life, and worry). Thus, addressing disordered eating for women with type 2 diabetes mellitus may be an important means to improving quality of life. The intervention was not associated with significant improvement of other common indicators of diabetes management, including diabetes distress and self-efficacy. However, across the 12-week intervention, participants maintained moderate levels of diabetes self-efficacy. Given baseline levels of diabetes self-efficacy, and the intervention’s lack of focus on blood glucose monitoring and other diabetes-specific management behaviors, these findings are not surprising. Additional tailoring of the intervention to include diabetes-specific information and behavioral information, as well as further research, is necessary to improve glucose monitoring and other self-management behaviors in an effort to improve overall diabetes outcomes.
Overall, results of the CSQ-8 and analyses of the open-ended questions revealed that participants reported moderately high satisfaction with the intervention and that the intervention was acceptable to women with type 2 diabetes mellitus and comorbid disordered eating. Specifically, participants indicated that they would recommend the program to other women and described the information presented in the manual as clear, thought-provoking, and nonjudgmental. Furthermore, participants described appreciation for the regular support calls that provided a sense of connection and accountability. Other studies have similarly demonstrated the efficacy of phone-based interventions for individuals with type 2 diabetes mellitus or disordered eating with attention to increased access and reduced burden.21,37 Participants also provided suggestions for future adaptations, such as the addition of group meetings or support. To date, there have been no published studies of CBT protocols with group-based support for disordered eating. However, group-based interventions have been effective in improving type 2 diabetes outcomes in primary care settings and can help patients learn from, and gain support from, their peers. 38
Limitations
The current study was not without limitations. While the results and rich participant feedback provide meaningful support for the potential value of the current intervention, the nature of the pilot study was to assess general proof of concept of a CBTgsh lifestyle intervention for women with type 2 diabetes. Thus, although the intervention lead to meaningful improvement in disordered eating symptoms, with no control group we cannot conclusively determine that improvements occurred as an effect of the intervention. Furthermore, any changes in participant’s diabetes management regiment made by their individual medical providers during the course of the intervention are unknown.
The very low rate of attrition was a strength of the current study; however, the one participant who dropped out during the intervention, and who was also an outlier with regard to both weight and disordered eating severity, was encouraged to do so by her physician. This indicates that such interventions would benefit from the involvement of medical professionals who can help address diabetes-related health issues concurrently with the behavioral intervention. Additional strengths of the study include high engagement, and foundational feasibility for further study, such as a randomized controlled trial.
Future Directions
The current CBTgsh lifestyle intervention is a low-cost, accessible, and feasible treatment for women with type 2 diabetes mellitus who experience disordered eating and associated distress, and warrants further study. To expand upon the results and success of the current study, future iterations of the intervention should incorporate participant recommendations, including a more explicit focus on diabetes management, access to peer support, more efficient methods for self-monitoring, and a randomized control group. Future research would also benefit from inclusion of diabetes education and comparison of the CBTgsh intervention to an education-only group, in an effort to better differentiate the benefits of various aspects of the intervention. Finally, future partnership with a medical institution and/or providers would allow for inclusion of important biometric health data, such as HbA1c, and standardized weight and waist circumference, to better assess the effects of the intervention on important diabetes metrics.
The current study is an important proof of concept that lays foundation for the development of interventions to address disordered eating among individuals with type 2 diabetes mellitus, an area of great public health importance, yet little research. The lifestyle intervention, addressing 4 of the 6 pillars of lifestyle medicine, in combination with an accessible, evidence-based psychotherapeutic intervention (CBTgsh), is also a promising approach to addressing the complex nature of life with type 2 diabetes.
Footnotes
Acknowledgements
We thank the following for their contributions to this project: Jennifer Webb, PhD, Maren Coffman, PhD, Alyssa Minnick, MS, and undergraduate members of the Women’s Health Project at The University of North Carolina at Charlotte.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Funding was provided by The University of North Carolina at Charlotte Department of Psychology Student Research Award.
Ethical Approval
The current human subjects research was dually approved by the Carolinas Medical Center (now Atrium Health) and the University of North Carolina at Charlotte’s Institutional Review Boards, and conforms to all recognized standards.
Informed Consent
Informed consent was completed for all participants in accordance with insitututional IRB standards.
Trial Registration
Not applicable, because this article does not contain any clinical trials.
