Abstract
Lower back pain is a leading cause of work absence and activity limitations globally, with a 60% to 85% lifetime chance of occurrence. This article highlights the role that lifestyle medicine plays in managing lower back pain as a cost-effective intervention strategy. It is suggested that lifestyle medicine strategies, such as incorporating whole foods and a plant-based diet, sustainable physical activity and mind-body exercises, restorative sleep, stress resiliency, awareness and mitigation of substance abuse and addiction, and establishing meaningful social networks and self-care strategies, be a part of managing chronic lower back pain.
Factors that may influence pain include physical and emotional health, nature of the injury or illness, social environment or cultural upbringing, acuity or chronicity of the symptoms, memory, and personality.
Introduction
An individual has a 60% to 85% lifetime chance of experiencing lower back pain.
1
Based on sample interviews of the US civilian population in 2018, 31.6% of women and 28.0% of men aged ≥18 years reported having lower back pain in the past 3 months.
2
In 2014, a report
3
in the
According to the Mayo Clinic health information resource on back pain,
5
there is an increased risk of developing back pain as a result of factors such as advancing age, diseases (such as arthritis or cancer), excess body weight, improper lifting, lack of exercise, psychological conditions such as depression and anxiety, and smoking. Incorporating lifestyle medicine strategies into a clinical care program may help individuals suffering from chronic lower back pain. In the
Basic Pain Science
The
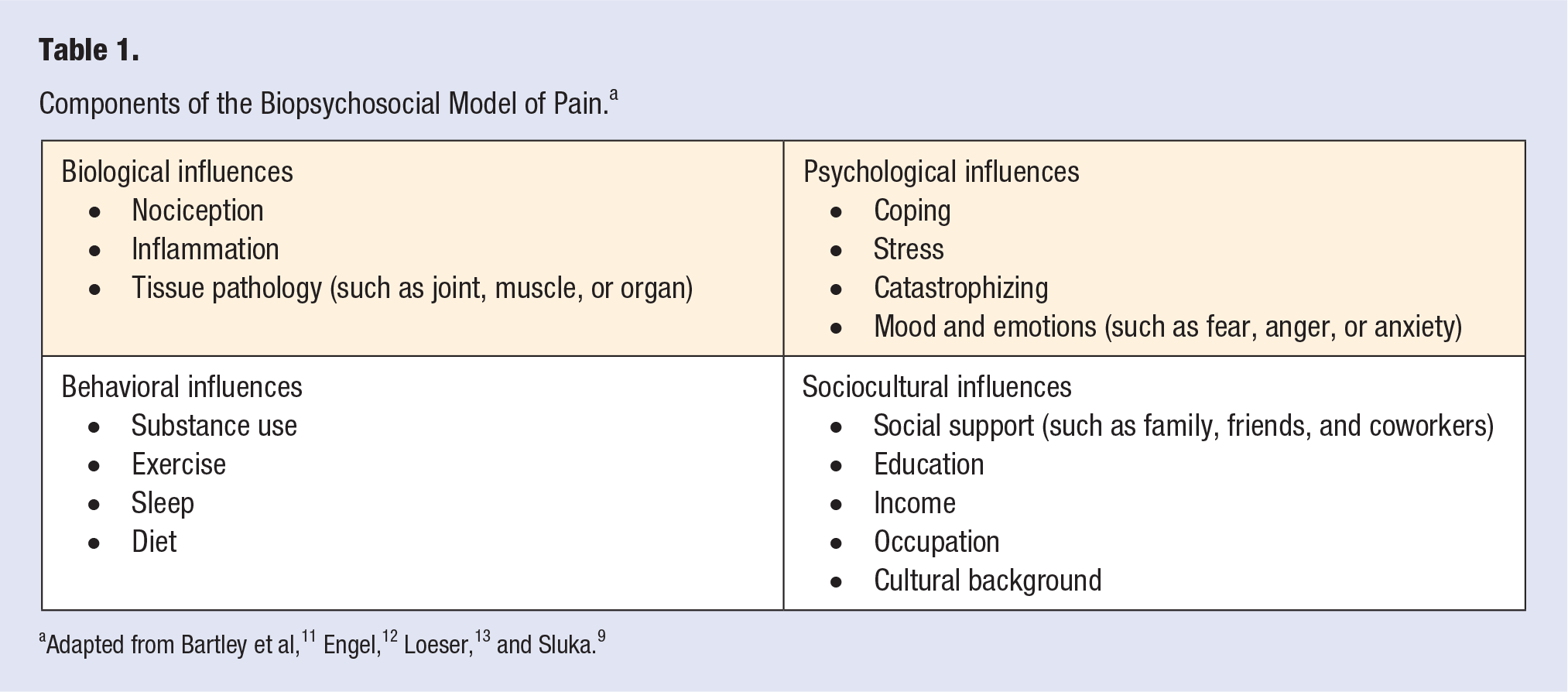
The biological model of pain assumes that all pain has a distinct physiological cause. The current medical approach uses the Biopsychosocial Model of Pain because it incorporates the interaction between the biological, psychological, and sociocultural variables. 9 Many of the Biopsychosocial Model of Pain variables are also components of lifestyle medicine (Table 1).6,10
Clinical Concepts
The focus on clinical care should target not only the latest therapeutic interventions, but also the manner in which the therapy is effectively delivered to the patient. Clinicians need to improve other aspects of clinical care, such as building a therapeutic alliance, including shared decision-making, motivational interviewing, and establishing interprofessional collaborations.
A therapeutic alliance is where clinicians and patients establish a collaborative and purposeful relationship. This professional bond can lead to positive therapeutic changes and may improve pain outcomes. 14 In other words, the context of clinical interventions can enhance the therapeutic effect. A study in 2020 by Kinney et al 15 showed that establishing a therapeutic alliance with patients may positively affect chronic musculoskeletal pain. For example, to build a therapeutic alliance, the clinician could allow the patient to be a part of the decision-making process, make the patient feel welcome with their words and actions, and minimize distractions during treatment. 16 Other strategies to interact effectively with patients may include allowing sufficient time for empathetic dialogue, being attentive and sensitive to personal and cultural needs, and showing a genuine interest in their life circumstance. 17
Shared decision-making, where the clinician and patient decide using the best evidence available and include the patient’s values and preferences into the decision-making process, may also help improve long-term therapeutic outcomes.18-20 For example, besides providing treatment options for the patient, the clinician could explain the pros and cons of selected interventions and identify the patient’s treatment preferences. Furthermore, to improve decision making, the clinician could use phrases such as, “What if we try . . . ?”, “Would you consider trying . . . ?”, or “Would you be open to . . . ?” 21
Another clinical strategy to treat patients with lower back pain is to use motivational interviewing to empower and motivate patients to change their behavior. 22 This collaborative approach uses a goal-oriented communication style and pays attention to the language of change.23,24 The 5 necessary communication skills used in motivational interviewing include24,25 asking open-ended questions, affirming (or praising) a person’s good intentions or efforts, using reflective listening, summarizing the person’s situation, and finally, informing and advising the person. For example, an open-ended question may be phrased as, “How can I help you with your back pain?” To affirm or praise the person’s good intentions, the clinician could say, “You did a great job quitting smoking six weeks ago.” The health care professional could address reflective listening by stating to the patient, “I understand you feel overwhelmed with your current situation.” Additionally, the person’s situation can be summarized by the clinician as, “Let me see if I understand you so far. Your back pain started . . .” Some practitioners may end the motivational interviewing session with, “Did I miss anything?” before moving into the physical examination or intervention phase.
Engaging with different professionals in a collaborative approach can help patients, families, and caregivers receive quality care while enhancing a clinician’s knowledge and presence in the community and potentially reducing health care costs.
26
An article
27
in
Finally, clinicians also need to be aware of a person’s readiness for change. To help a patient change a lifestyle behavior, such as to quit smoking or increase physical activity, it would be helpful to know if the person is ready and open to making changes. There is some evidence for using the Pain Stages of Change Questionnaire in assessing if a person is likely to join a self-management intervention program.
29
The readiness for change model is based on the Transtheoretical Model of Behavior Change or the Stages of Change Model.30,31 One version of the model starts with the
Lifestyle Interventions
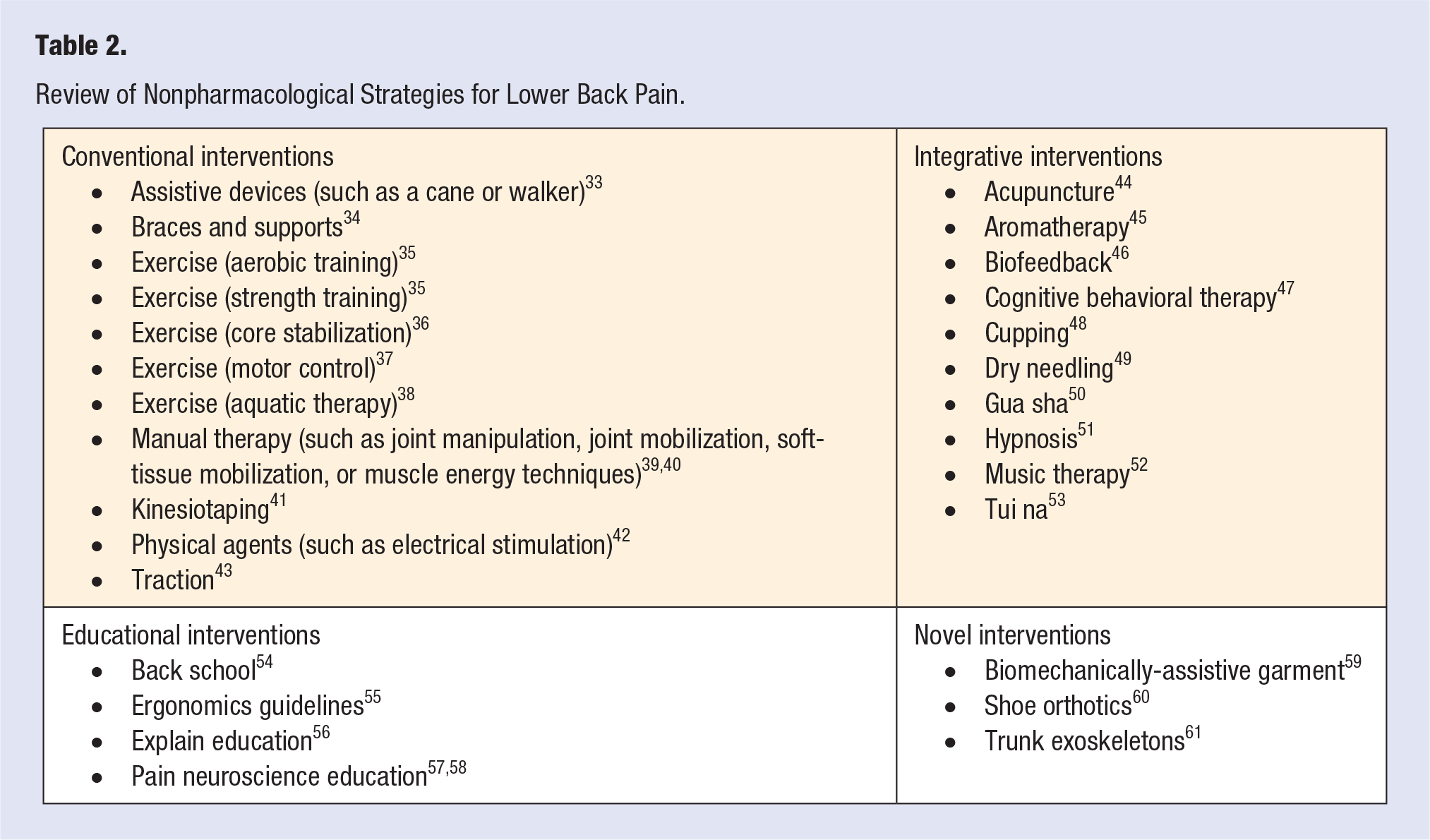
Evidence-based practice involves scientific research, clinical expertise, and patient values. 32 This section will highlight selected scientific research using lifestyle interventions for managing chronic lower back pain. Table 2 provides a review of various nonpharmacological and conventional, integrative, educational, and novel intervention strategies for addressing back pain.
Review of Nonpharmacological Strategies for Lower Back Pain.

A review
44
in the
Why should clinicians use lifestyle medicine interventions for managing chronic lower back pain? A randomized controlled trial
62
in the
Nutrition and Back Pain
Healthy eating patterns play a crucial role in not only reducing lower back pain but also reducing excess body weight, which is one of the risk factors for developing back pain. A randomized controlled trial
63
in
As a part of an interprofessional collaboration program, the patient could consult with a culinary medicine 65 specialist or a registered dietitian in order to gain knowledge about the foundations of cooking to reduce pain and inflammation using foods. 66 The patient may also be counseled to try the Mediterranean diet for weight loss 67 or use a targeted diet that includes low glycemic foods to help modulate pain. 68
Conventional Exercise, Physical Activity, and Back Pain
Clinicians understand the value of physical activity in helping prevent and treat a variety of medical conditions. Conventional exercises that include aerobic, strength, flexibility, and balance training may help patients improve endurance, increase core strength, loosen tight muscles, and improve coordination and stability. A systematic review
69
in the
Mind-Body Exercises and Movements
Mind-body or integrative movements may be another form of exercise or physical activity. This type of exercise combines specialized movements, controlled breathing, and mental focus to improve overall health, balance, flexibility, and strength. 71 Mind-body movements may include yoga, tai chi, qigong, and Pilates.
Yoga is a system of physical postures and coordinated diaphragmatic breathing that originated in India.
7
A randomized noninferiority trial
72
in the
Tai chi is a traditional Chinese martial art that uses a series of slow, controlled movements to improve balance, strength, flexibility, relaxation, and mental concentration.
7
A randomized controlled trial
74
in
Qigong is an ancient Chinese practice that uses movement, breathing exercises, relaxation, and meditation.
7
In 2019, Li et al
76
concluded that a type of qigong called Baduanjin was effective for lower back pain. Another systematic review
77
in the
Pilates is a bodywork system created by Joseph Pilates that uses specialized equipment or mat exercises to improve strength, flexibility, balance, and mental concentration. Randomized controlled trials in 2017 and 2018 by Cruz-Diaz et al78,79 reported that a Pilates intervention effectively managed chronic lower back pain.
Sleep and Back Pain
Clinicians need to be better informed about sleep hygiene guidelines because sleep quality may affect individuals with lower back pain. A review article
80
in
Furthermore, appropriate light exposure through outdoor light and sunshine is especially essential in the morning on awakening and during the day because it is necessary to improve sleep quality, mood, alertness, cognition, and reaction time and prevent depression. 81 A randomized controlled trial in 2014 by Leichtfried et al 82 reported that “light therapy even in low dose could improve depressive symptoms and reduce pain intensity in chronic nonspecific back pain patients.” Strategies that may increase natural light exposure include having breakfast near a window or on a balcony, porch, or patio, sitting near a window at work, going for an outdoor walk at lunch, working in a garden, including more outdoor activities, and remodeling the home to add more windows or skylights.
Stress and Back Pain
A study by Herman et al 83 found that mindfulness-based stress reduction may be a cost-effective strategy for helping individuals with chronic lower back pain. There are many different mindfulness-based stress reduction techniques, such as diaphragmatic breathing, 84 square breathing (also known as box breathing), 85 mindfulness-based body scan, 86 and walking meditation. 87 The essential component of many of these strategies is to help the individual get their breath under control. Therefore, teaching patients breathing control may be a good start. For example, during a square breathing technique, the person could breathe in slowly for 3 s, pause the breath for 3 s at the end of the inhale, exhale slowly for 3 s, and finally, pause the breath for 3 s. This sequence could be repeated 2 to 10 times or longer to promote relaxation.
Substance Use, Addiction, and Back Pain
Yang et al
88
in
Social Connections and Back Pain
Individuals with lower back pain may find that workplace, financial, and social pressures can affect their ability to manage their condition.
95
For this reason, clinicians can help patients find counselors, social workers, or connections in their community to help them heal and recover. In 2020, a perspective article
96
in the
Self-care and Back Pain
Self-care and self-management strategies, such as ergonomic instructions, proper body mechanics, joint protection and energy conservation guidelines, self-massage, self-acupressure, flare-up management, and pain neuroscience education, may be useful techniques to help patients manage their back pain. For example, the patient may be advised to use variable sitting postures to migrate tissue loads in the hip and back region. 97 Also, instructions in proper body mechanics and joint protection guidelines 98 may help patients properly lift, push, pull, carry, and bend during activities of daily living. Furthermore, one energy conservation strategy 99 may advise a patient to alternate between difficult and easy tasks at home or work to avoid overloading muscles and joints.
Other simple self-care techniques may include teaching the patient self-massage and self-acupressure techniques100,101 to reduce spasm and pain. Additionally, many patients with back pain could benefit from flare-up management education. 102 This educational strategy would empower individuals to create their own “toolbox” of useful techniques and strategies to manage symptoms when flare-ups occur. Finally, some individuals may need pain management education or counseling.57,103
Conclusions
Research supports the use of lifestyle medicine strategies outlined by the American College of Lifestyle Medicine (https://www.lifestylemedicine.org/) to manage lower back pain with low-cost nonpharmacological interventions. Clinicians should incorporate a plant-based diet, sustainable physical activity and mind-body exercises, restorative sleep, stress resiliency, awareness of substance abuse and addiction, establishing meaningful social networks, and self-care strategies. Also, using motivational interviewing, shared decision-making techniques, and interprofessional collaborations may help clinicians establish a therapeutic alliance with their patients to improve desired medical outcomes.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Not applicable, because this article does not contain any studies with human or animal subjects.
Informed Consent
Not applicable, because this article does not contain any studies with human or animal subjects.
Trial Registration
Not applicable, because this article does not contain any clinical trials.