Abstract
Objective. Physician physical activity (PA) counseling remains low due partly to lack of knowledge, emphasizing the importance of providing learning opportunities to develop competency, given the strong associations between PA and health. This study aimed to describe the behavior change techniques (BCTs) used in an “Exercise Expo” workshop and examine the workshop’s effectiveness for improving social cognitions to discuss exercise with patients. Methods. Second-year medical students (N = 54; Mage ± SD = 25.4 ± 2.95 years) completed questionnaires assessing attitudes, perceived behavior control (PBC), subjective norms, and intentions to provide PA counseling pre- and postworkshop. Repeated-measures analyses of variance evaluated changes in these theory of planned behavior constructs. Results. The most used BCTs included presenting information from credible sources, with opportunities for practicing the behavior and receiving feedback. Significant increases in attitudes, PBC and intentions to discuss PA were observed from pre-post Exercise Expo (P ≤ .01). No statistically significant differences in subjective norms were observed (P = .06). Conclusions. The Exercise Expo significantly improved social cognitions for PA counseling among medical students. Future interventions should target improvements in subjective norms to increase the likelihood the workshop improves PA counseling behavior. The evidence supports the usefulness of a workshop-based educational strategy to enhance medical students’ social cognitions for PA counseling.
‘PA [physical activity] promotion by physicians should be considered integral to routine medical counseling.’
Physical activity (PA) interventions are effective for chronic disease prevention; however, 31% of adults worldwide and 43% in the Americas, specifically, are not currently meeting guideline-recommended PA levels. 1 Primary care physicians play an important role in promoting PA, as patients perceive them as credible and respected sources of health information. 2 Since patients receiving PA counseling from their physicians are more likely to be active, 3 PA promotion by physicians should be considered integral to routine medical counseling. Unfortunately, only 28% of adults report receiving advice from their physicians to increase PA levels. 4 Lack of knowledge and skill are common barriers to PA counseling, 5 with one-third of physicians feeling adequately trained to counsel about PA. 6 Thus, physicians must be provided with opportunities to develop the skills and behaviors necessary to implement PA counseling into routine medical practice. 5
The undergraduate medical school curriculum provides an exciting opportunity to address the alarming knowledge gap that exists and yet, PA counseling in formal curriculum remains scarce, with few institutions formally offering coursework/practical learning in PA. 7 Several studies have evaluated a PA component in the medical school curriculum with varying levels of success for changing the attitudes, intentions, and behaviors of medical students regarding PA counseling.8-12 However, few of these investigations include pre- and posttesting measures in addition to a practical guide based on a strong theoretical framework to guide future implementation in alternate settings.10-12 Improvement in medical students’ training regarding PA counseling and prescription is necessary. Formal training by credible PA professionals early in training will equip medical students with knowledge and resources to counsel patients about active living from the onset of their professional practices. 13
Exercise Is Medicine Canada (EIMC) is a national initiative part of a global movement to increase exercise prescription among physicians. EIMC works closely with university and college campuses to achieve these aims in academic settings. EIMC at Queen’s University (EIMC-QU) was first established in 2013 as a graduate student-run group collaborating with many campus departments and community health care professionals to design and deliver 4 intervention types: (1) PA awareness and promotion; (2) educational workshops for students and/or community members; (3) consultation and collaboration with campus health services, local family health teams, and/or primary care networks; and (4) new medical program curriculum developments.
EIMC-QU, in partnership with an endocrinologist (RH) from Queen’s University School of Medicine and Kingston General Hospital, designed and implemented an innovative “Exercise Expo” (Expo) to address the gap in PA counseling within the current medical school curriculum. In 2014, the Expo was established as an annual half-day workshop for second-year medical students addressing PA counseling and prescription to reinforce the important role physicians have for incorporating PA assessment and intervention into patient interactions. To characterize the 2015 Expo’s impact on students’ social cognitions (thoughts and feelings) toward PA counseling, an evaluation founded in the theory of planned behavior (TPB) was used. The TPB has been demonstrated to predict health care providers’ intentions for discussing PA with patients 14 and theorizes that individuals’ attitudes, subjective norms, and perceived behavioral control (PBC) for discussing and prescribing exercise influences the individuals’ intention to perform that behavior. 15 Therefore, if intentions and PBC are improved, the likelihood of discussing and prescribing PA increases. The behavior change techniques (BCTs)—or mechanisms by which behavior change is produced 16 —used in the Expo aligned with TPB constructs. Thus, the Expo theoretically had the potential to change attendees’ thoughts and feelings toward PA counseling.
Accordingly, the purposes of this investigation were to (1) describe the BCTs used in the Expo to serve as a model for other training programs and (2) assess the Expo’s impact on enhancing second-year medical students’ social cognitions for discussing and prescribing PA to their future patients. It was hypothesized that medical students would report significant increases in attitudes, subjective norms, PBC, and intentions to discuss PA with their patients immediately following their attendance at the Expo.
Methods
Description of the Exercise Expo
Attendance at the Expo was mandatory for second-year medical students and the material was testable. The workshop provided practical information tailored to promote the effective incorporation of PA strategies in patient care plans. Students cycled through seven 25-minute stations: (1) Five Major Steps to Intervention (exercise counseling); (2) Exercise Prescription and Goal Setting; (3) Simple Strategies for Aerobic Activity; (4) Considerations for Rural and Remote Settings; (5) Strategies for PA Promotion; (6) Introduction to the Canadian PA Guidelines; and (7) Strategies for Resistance Exercise Training. The evidence-based station content was designed and developed by EIMC-QU graduate students, whose research and practical expertise included exercise physiology, health promotion, health psychology, biomechanics, and PA epidemiology.
Following the workshop, independent coding and examples of BCTs used in each station were completed by three of the station developers (AB, KD, AF) for students’ (1) own PA and (2) PA counseling behaviors (see the appendix). A researcher with expertise in exercise behavior change (JT) was consulted where disagreements or uncertainty existed. BCTs and corresponding examples were reviewed and confirmed by station facilitators.
Assessment of the Exercise Expo’s Impact
Protocol
The study received institutional ethics approval. To compare changes in second-year students’ TPB social cognitions for PA counseling, hardcopy questionnaires were administered 1 week prior to and immediately following the workshop.
Participants
Eligible participants (N = 100) were second-year medical students at Queen’s University who attended their scheduled endocrinology lecture 1 week prior to the workshop. Students received study information and interested students read and signed the Letter of Information/Consent before completing the hardcopy prequestionnaire (n = 77).
Questionnaire Measures
Demographics
Participants were asked about general demographic information, current PA levels, and academic background (Table 1). The majority of participants with complete data (pre- and postquestionnaire; n = 54 (54% participation rate) were women (53.7%), Caucasian (57.4%), and holding Bachelor-level degrees (53.7%). Few participants (3.70%) had previous academic experience in kinesiology/exercise science/physical education. Participants had a mean age of 25.44 ± 2.95 years and were active for 3.97 ± 1.71 days per week. There were no significant differences in demographic characteristics between those who completed only the prequestionnaire versus those who completed both pre- and postquestionnaires (P > .05).
Participant Demographic Characteristics. a
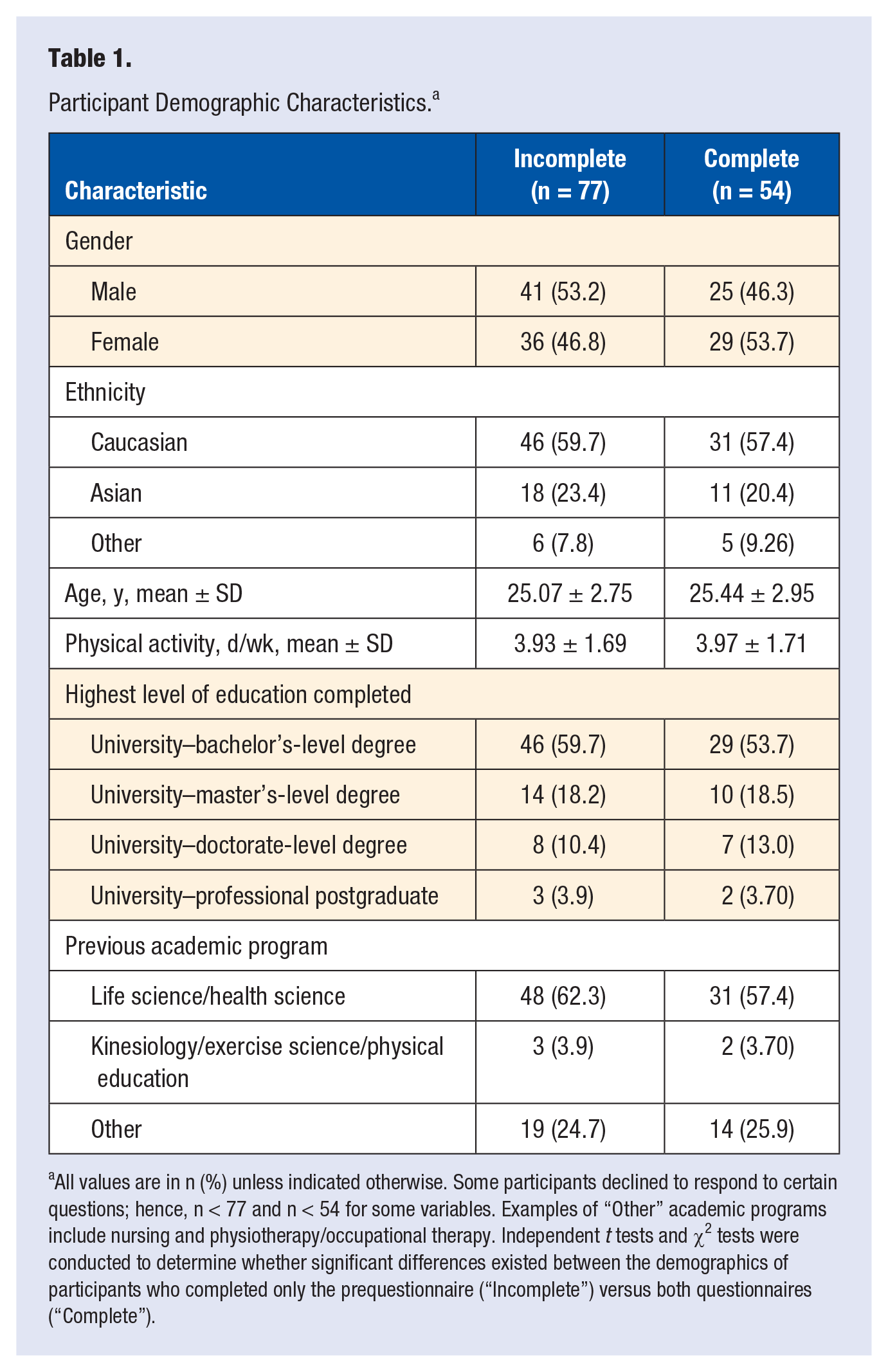
All values are in n (%) unless indicated otherwise. Some participants declined to respond to certain questions; hence, n < 77 and n < 54 for some variables. Examples of “Other” academic programs include nursing and physiotherapy/occupational therapy. Independent t tests and χ2 tests were conducted to determine whether significant differences existed between the demographics of participants who completed only the prequestionnaire (“Incomplete”) versus both questionnaires (“Complete”).
Social cognitions
Participants were asked about their attitudes, subjective norms, PBC, and intentions for exercise counseling and prescription. These items were adapted from a questionnaire shown to be reliable in a study that examined health care professionals’ social cognitions for discussing and prescribing PA, 14 in order to reflect the specific population (medical students) and context (Exercise Expo) of the current intervention. Table 2 contains full item descriptions.
Questionnaire Items Assessing Medical Students’ Social Cognitions for Discussing Physical Activity With Future Patients and Changes in Medical Students’ Social Cognitions Over Time.
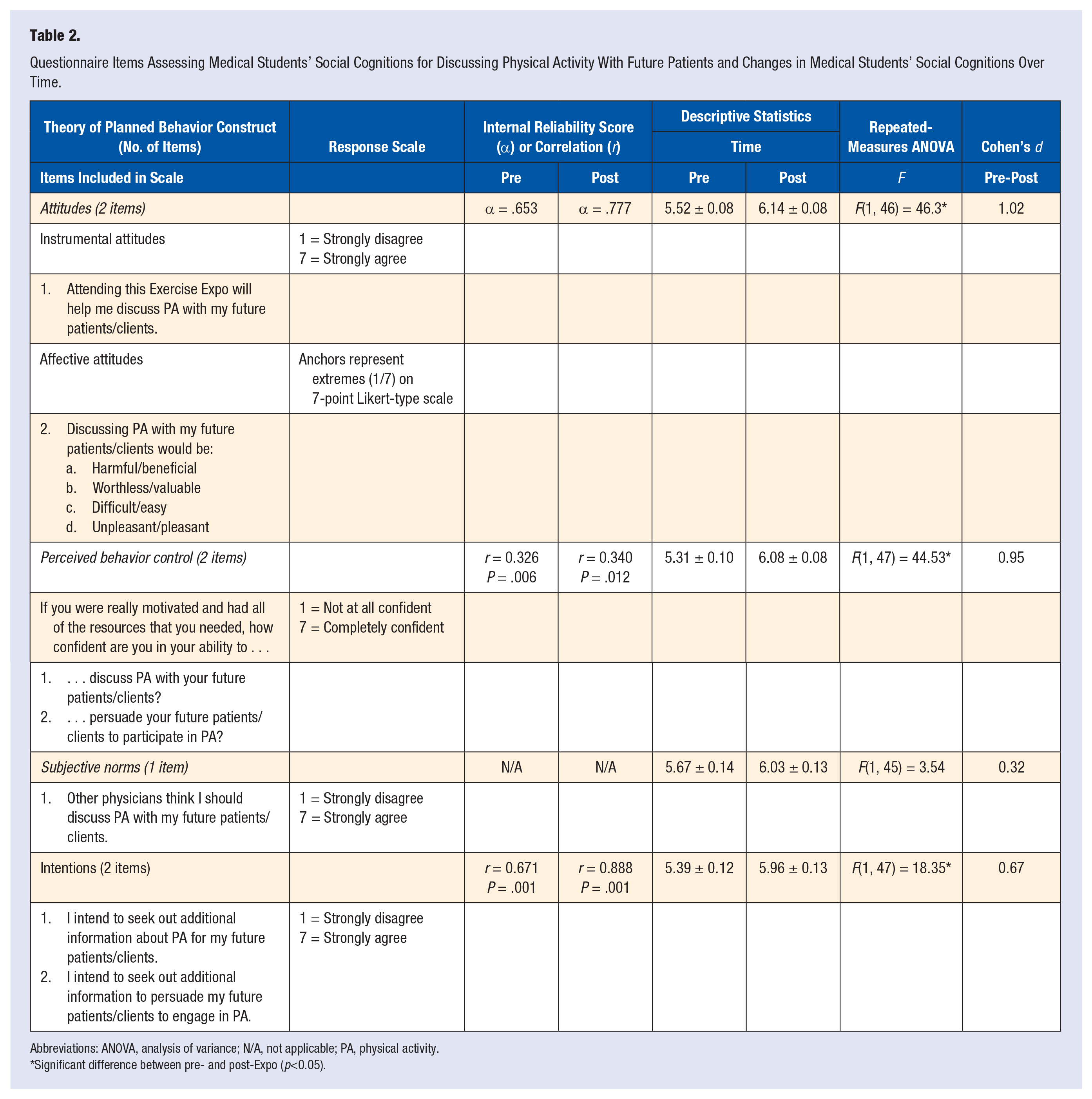
Abbreviations: ANOVA, analysis of variance; N/A, not applicable; PA, physical activity.
Significant difference between pre- and post-Expo (p<0.05).
Knowledge of EIMC and PA guideline recall
Participants were asked 3 questions regarding their awareness and knowledge of (1) EIMC, (2) EIMC-QU, and (3) any Canadian PA Guidelines. They were also asked to identify which of the provided multiple-choice answers represented the adult Canadian PA Guidelines. 17
Quality assessment
Participants were asked 9 questions regarding their evaluation of the Exercise Expo (Table 3).
Medical Students’ Quality Assessment Evaluation of the Exercise Expo.
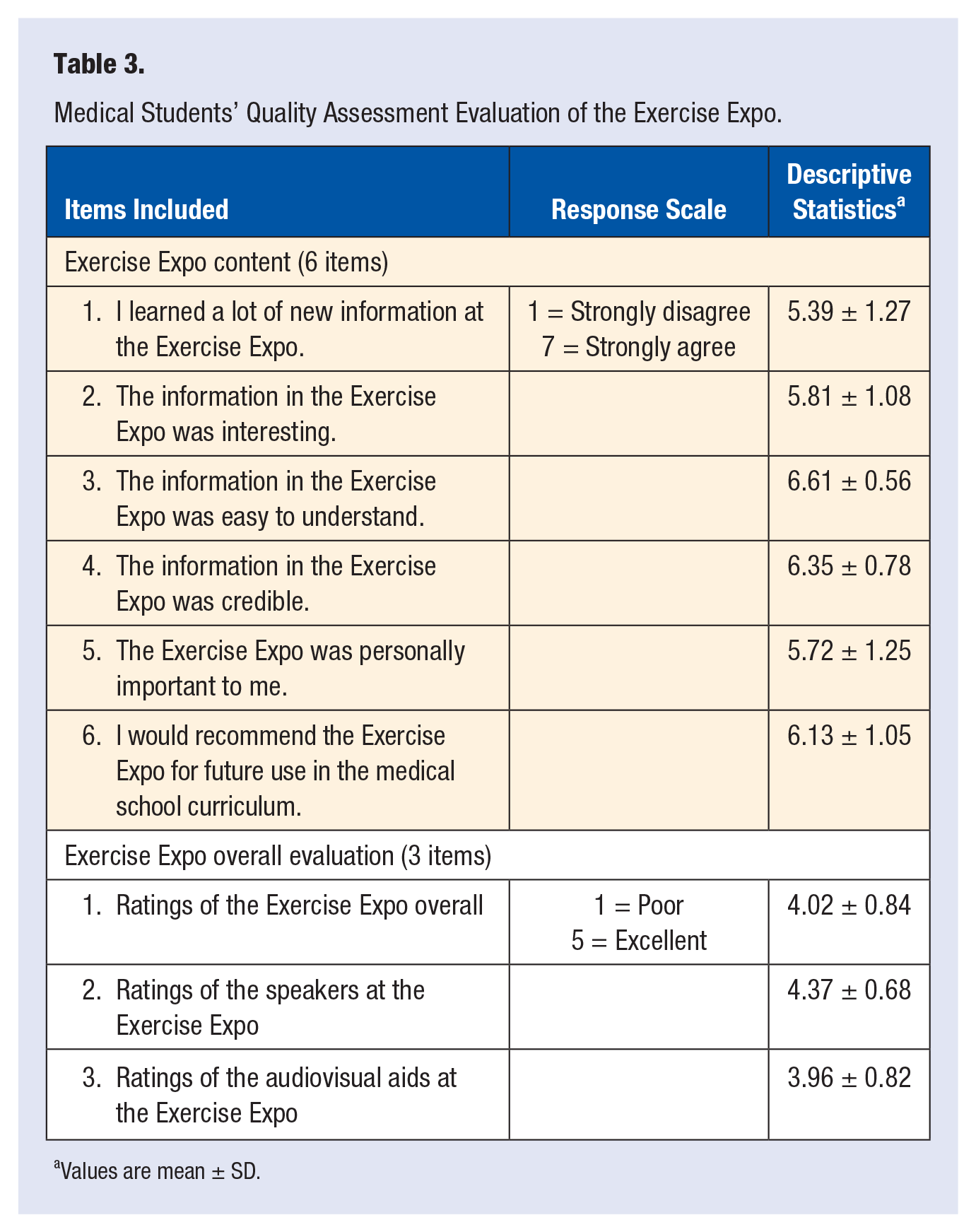
Values are mean ± SD.
Statistical Analyses
Repeated-measures analyses of variance were conducted for the 4 TPB cognitions across the 2 time points. Using the Bonferroni method, alpha was adjusted for the 4 comparisons (α = .05/4 comparisons = .0125). Cohen’s d was calculated to determine effect sizes.
Responses to EIMC and PA guideline questions were dichotomized (yes = 1, no = 0 and correct = 1, incorrect = 0, respectively). Frequency counts and exact McNemer’s χ2 tests were conducted to determine differences between the proportion of students who were aware of EIMC and the Canadian PA Guidelines between pre- and post-Expo. Descriptive statistics were used for each quality assessment item.
Results
Description of the Exercise Expo
The appendix lists and operationalizes all BCTs used in each of the 7 stations. 25 BCT items were identified in total with 34 uses targeting students’ personal PA behavior, while 41 uses targeted students’ clinical PA counseling behavior. The most commonly used BCTs for both personal and clinical included 4.1–Instruction on how to perform a behavior, 9.1–Credible source, 8.1–Behavioral practice/rehearsal, and 2.2–Feedback on behavior. 16
Assessment of the Exercise Expo’s Impact
Descriptive statistics for the TPB variables at both time points are presented in Table 2. Despite initially high values for each social cognition (all means ≥5.31 out of 7), significant increases in attitudes, PBC, and intentions to discuss PA were observed from pre- to post-Expo (P ≤ .01). No significant differences in subjective norms were observed from pre- to post- Expo (P = .06).
Increases in the proportion of students reporting awareness of EIMC and EIMC-QU from pre- and post-Expo were observed (33.3% vs 54.2%; χ2(2) = 13.0, P = .0003 and 33.3% vs 54.2%; χ2(1) = 7.14, P = .008, respectively). While there was no change in students’ awareness of the PA guidelines between pre- and post-Expo (83.3% vs 87.5%; χ2(1) = 0.40, P = .527), there was an increase in the proportion of students correctly reporting the PA guidelines (23% vs 93.8%; χ2(1) = 34.0, P = .001).
Participants positively rated the Expo (Table 3; all means ≥5.39 out of 7). The students’ highest ranking indicated information was easily understandable and credible (M = 6.35 ± 0.56 and 6.35 ± 0.78, respectively). Notably, participants indicated they would recommend the Expo for future use in the medical school curriculum (6.13 ± 1.05). When asked to provide an overall evaluation of the Expo, speakers and audiovisual aids, the feedback was positive (Table 3; all means ≥3.96 out of 5).
Discussion and Conclusion
The purposes of this study were to (1) characterize the BCTs used in an innovative workshop-based Expo to assist with developing future educational training programs and (2) examine the impact of this intervention on enhancing second-year medical students’ thoughts and feelings toward PA counseling with their future patients.
Discussion
The primary findings of this study were that, in agreement with our hypothesis, immediately following the Exercise Expo, participants reported significant increases in attitudes, PBC, and intentions to discuss PA with their future patients. This demonstrates that the “Exercise Expo” is a viable educational component that can be incorporated in a variety of medical education contexts.
Our findings are supported by prior investigations that examine medical school interventions targeting PA counseling. 2 Three separate studies investigating the utility of various PA education components demonstrated a significant improvement in awareness of the importance and ability to discuss PA with their future patients10-12; however, these studies were limited by their postquestionnaire design. These limitations have been addressed by subsequent investigations. Bass Iii et al 9 examined the influence of a 2-hour interactive lecture including performance practice for PA and nutrition counseling skills among 57 medical students and found significant improvements in knowledge and self-confidence for PA counseling from pre- to postintervention. Furthermore, Frank et al 8 observed a significant association between exercise counseling habits and participation in a 4-year project involving numerous lectures and activities directly related to PA counseling. All the preceding interventions, including our own, incorporate experiential learning and are supported by theoretical frameworks, which are both important aspects of effective PA education programs. 2 The current investigation extends existing literature by providing a detailed description of the active ingredients of the Exercise Expo for future replication and evaluation.
The Exercise Expo is rooted in the TPB and the specific BCTs that align with this theory are outlined at length in the appendix. The BCT taxonomy of Michie et al 16 allows researchers to determine the “active ingredients” of interventions that function to change cognitive processes regulating behavior. By using standardized definitions and labels for the intervention components in the Expo, the intent of this article was to provide a well-specified educational model that can be replicated by others to address the knowledge gap in clinical PA counseling. On retrospective identification of the BCTs, it was evident that 2 complementary elements of clinical exercise prescription were targeted: personal PA behavior and clinical PA counseling, with a greater focus on the latter. Common elements across the stations included presenting medical students with “how to” information from credible sources, with opportunities for practicing the behavior and receiving feedback. Continued exposure to PA-related content throughout medical school will equip future physicians to become credible sources in this area, feeling confident to discuss this lifestyle change with their patients (C. H. Shirazipour et al, unpublished data, 2017).
In contrast to our hypothesis, there was no change in subjective norms. On review of the TPB constructs targeted in each of the 7 stations, the Expo primarily targeted students’ PBC, followed by attitudes and to a lesser extent, subjective norms; therefore, this finding is not surprising. Furthermore, we are limited in evaluating this construct as only 1 item on the questionnaire was specifically designed to evaluate subjective norms. A shortened TPB questionnaire modeled after a previously used questionnaire for similar purposes 13 was used to enable feasible data collection. Future research should examine the validity of shorter theory-based questionnaires for use in similar settings. Furthermore, while having kinesiology graduate students and exercise physiologists present the content strengthened the credibility of the information source, the incorporation of physicians’ self-described experience with PA counseling should be considered. Tomasone et al 13 suggest that this would strengthen students’ perceptions that others in their field view engaging in PA and PA counseling as important and relevant. Future iterations of the Exercise Expo should consider the use of both an exercise professional and a physician as the interventionists.
Participants demonstrated greater awareness of EIMC and recall of PA guidelines following the Expo, which is important for physicians as they develop evidence-based practices to ensure effectiveness of treatment and patient safety. An encouraging outcome of this study was the positive feedback received from medical students who found the Expo content and delivery to be engaging and worthwhile, indicating enthusiasm for the continued development and integration of PA counseling into medical school curriculum. While this is promising, it has recently been demonstrated that improvement in PA guideline knowledge is often not maintained 1-month postintervention (C. H. Shirazipour et al, unpublished data, 2017). Furthermore, awareness of guidelines does not necessarily indicate adoption of behavior. Continued exposure to the importance of PA for health throughout medical school will be important to consider for long-term retention. Further research is required in this population to address the most effective means of implementing PA into physicians’ lifestyles and PA counseling into demanding clinical schedules to improve physician confidence in and feasibility of discussing PA with their patients.
Conclusion
The global health problem of physical inactivity necessitates a collaborative effort from key stakeholders, including health care providers. This evaluation study provides evidence for the usefulness of a workshop-based educational strategy to increase medical students’ knowledge and social cognitions surrounding PA counseling and prescription. The evidence-based material presented using interactive approaches and interpersonal communication likely was influential in changing knowledge and attitudes toward clinical PA counseling. The identified BCT components of the Expo can be used as a foundation to replicate this intervention in other schools. Future studies evaluating the long-term maintenance of clinical behavior following initiatives similar to the Expo are required.
Practice Implications
Patients who receive PA counseling from their physicians are more likely to be active; thus, PA promotion by physicians should be considered an important component of medical counseling. However, many physicians report lack of knowledge and skills as an important barrier to physician PA counseling. 5 Therefore, it is important that physicians be provided with learning opportunities throughout their training to integrate PA counseling into clinical practice. The Exercise Expo, rooted in the TPB, made effective use of BCT’s 16 to improve social cognitions for PA counseling among medical students. This workshop can act as a model for other medical schools to implement into medical school curricula to address the serious gap in PA-related education.
Footnotes
Appendix
Acknowledgements
The authors wish to thank all the medical students who participated in the Exercise Expo. Additionally, the authors are grateful for the time and expertise that all station facilitators dedicated to the Expo. This includes: Alyssa Fenuta, Robert Thomas, Annie MacGregor, Celine Girard, Aleksandra Velickovic, Carla Teixera, Ashley Johnson, Hoda Gharob, Brittany Hammond, Taryn Davidson, Louise De Lannoy. The Expo was first developed in 2014 with leadership from former EIMC at Queen’s University co-President, Meghan Plotnick.
Authors’ Note:
First list of references is part of appendix.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
