Abstract
Excess weight continues to exact high costs at the individual, national, and global levels. Traditional methods used to reduce excess weight and promote healthy weight regulation have not been overly successful. Therefore, rigorous quantitative and qualitative research is needed to assess emerging and alternative approaches to determine effective strategies to confront this public health challenge. One such approach is applying mindfulness, or a nonjudgmental acceptance of living in the moment, to eating. Mindful eating is a nonjudgmental acceptance of physical and emotional feelings while eating or in an eating environment. Mindful eating constructs include recognizing one’s own cues of physical hunger and satiety in order to make decisions about what food and how much to eat, choosing foods that are nutritious and pleasurable, not participating in other activities while eating, and knowing the consequences of unmindful eating. The nascent mindful eating literature shows success in increasing mindfulness and promising but less robust outcomes with anthropometric biomarkers of healthy weight regulation. Mindful eating is an emerging healthy weight regulation approach that has the potential to address the challenges clients and patients experience with healthy weight regulation, but additional research is needed to confirm which health outcomes will be consistently affected.
‘Younger generations may for the first time have a shorter life expectancy than their parents due to negative health outcomes from unhealthy, excess weight.’
Healthy weight regulation continues to challenge the domestic and global public health systems with high economic and personal costs. 1 Cawley and Meyerhoefer 2 estimated that each obese American spends $2741 annually and that the United States spends over $209 billion on obesity-related illness such as diabetes, coronary heart disease, and cancer. Younger generations may for the first time have a shorter life expectancy than their parents due to negative health outcomes from unhealthy, excess weight.3,4 Most traditional approaches to healthy weight regulation focus on which foods and amounts to eat but suffer from low success rates.5,6 The practice of mindfulness has been proposed as an emerging and alternative approach to address healthy weight regulation7-9 because it takes into account maladaptive responses to internal and external signals 5 and people feel more in control of their food- and beverage-related decisions. 10
Introduction to Mindfulness
Mindfulness is maintaining a nonjudgmental, nondeliberative awareness of physical feelings, thoughts, and perceptions in the present moment.8,11,12 Though its origins come from meditation rituals of Eastern religions, 13 one can learn and practice mindfulness skills5,8,14 without participating in the religious component.12,15 A primary goal of mindfulness is reducing the “automatic pilot” state, or times when humans are normally unaware of life’s individual moments. 11 Mindfulness, or decreasing time on “automatic pilot,” enhances awareness of internal, physical cues that can optimize health 8 via higher levels of perceived control for lifestyle behavior choices that result in better health outcomes. 11 Mindfulness programs, like Jon Kabat-Zinn’s mindfulness-based stress reduction program, have been used to improve health outcomes 8 of those suffering from stress, 13 chronic pain, 16 anxiety disorders, 17 and cancer.6,11 Since practicing mindfulness promotes self-regulation, 12 applying mindful eating skills could help with healthy weight regulation through healthier food choices and recognizing the internal, physical cues of when one has eaten enough. 8
Introduction to Mindful Eating
Mindful eating is an emerging and alternative approach to address unhealthy eating behaviors, healthy weight regulation,14,18,19 and weight loss. 20 The practice takes into account responses to internal and external cues to reduce automatic pilot. 5 Mindless eating, or making food- and beverage-related decisions while on automatic pilot, may contribute to overeating and increased caloric intake,10,21 since it results in a significant underestimation and/or no monitoring of how much one has eaten.9,22 In a cross-sectional study by Wansink and Sobal, 22 participants (n = 139, 75% female, and mean age of 42.9 years) estimated they made 14.4 food- and beverage-related decisions per day. However, the actual mean number of just food-related decisions made by participants was 59 per day while the mean number of food- and beverage-related decisions was 226.7 per day. 22 In another study by Wansink, Painter, and North, 23 participants served soup from “bottomless” bowls ate 73% more than participants who ate soup from traditional bowls but estimated that they only ate ~5 calories more.
Mindful eating is a nonjudgmental awareness of physical (hunger and satiety cues) and emotional (ie, stress, boredom) feelings when eating or in situations that have environmental eating triggers.14,19 The increased awareness and response to internal, physical cues rather than emotions or environmental triggers partially explains how mindfulness promotes healthy weight regulation 14 and better diet quality. 19 A summary of the main constructs of mindful eating are presented in Table 1.
Mindful Eating Is 24
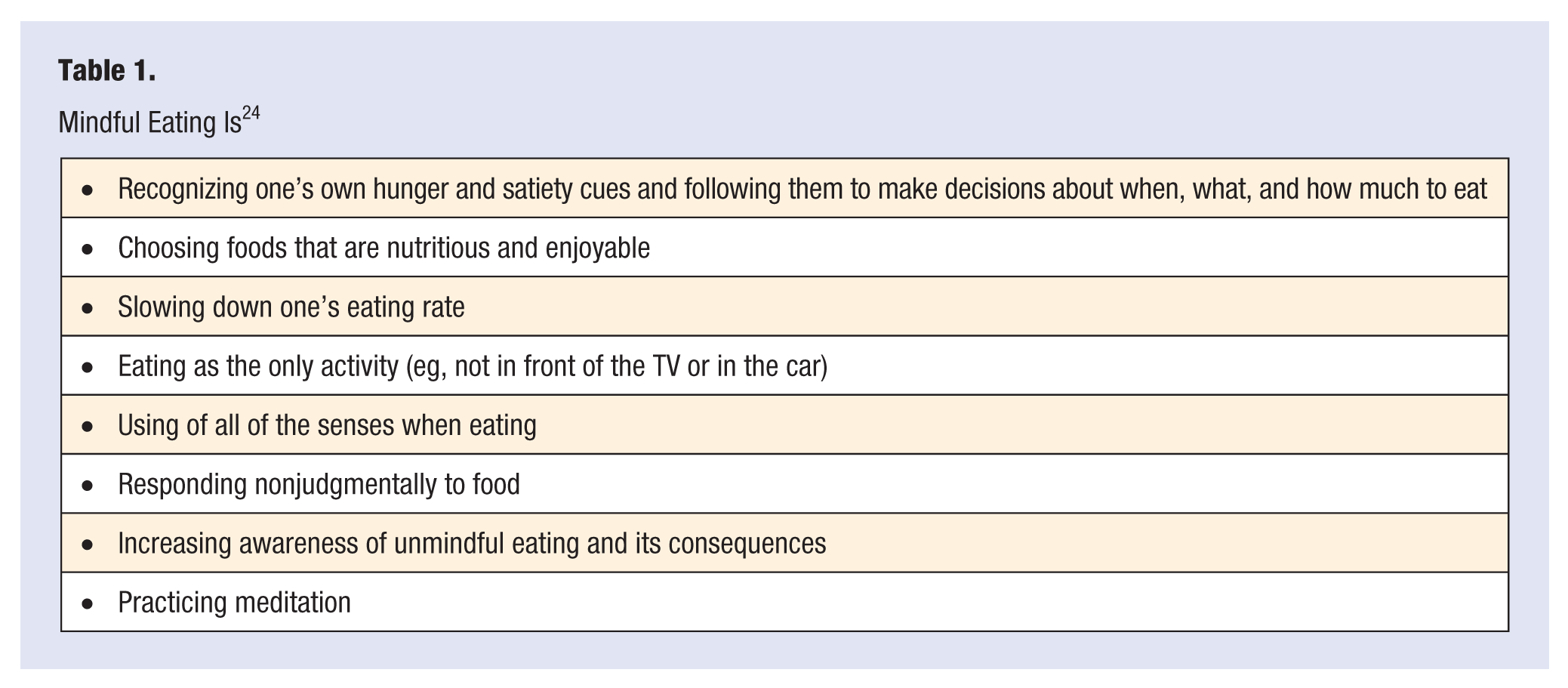
These constructs of mindful eating target consistently identified factors that contribute to overeating and therefore weight gain. These factors include increased consumption norms, such as bigger portion sizes at home and when eating out,23,25,26 less monitoring of consumption,26,27 and being on automatic pilot or responding to emotional and environmental cues when eating. 14
While the terms mindful eating and intuitive eating are sometimes used interchangeably,
28
there are significant differences. Though similar and complementary,24,28 compared with mindful eating, intuitive eating (
Previous Research on Mindful Eating: Highlighting Weight Regulation
Traditional weight loss and healthy weight regulation methods have not been overly successful; therefore, emerging and alternative approaches are needed.29,32 While mindful eating has been proposed as one of these emerging approaches, it is still in its infancy of robust scientific testing. However, the nascent research does provide evidence that mindful eating may be successful in healthy weight regulation via changes in mindfulness and resulting associations with negative eating behaviors and anthropometric biomarkers.
Jacobs et al 33 completed a cross-sectional study examining the impact of a 1-hour mindful eating education session on mindfulness and food consumption. After the training, participants reported more mindfulness (as measured by 3 different surveys including the Toronto Mindfulness Scale 34 ) and just over 85% of the participants had healthy food intake during the lunch provided by the investigators. 33 Though only one point in time, the results suggest that mindfulness training can affect dietary intake and therefore may support healthy weight regulation. 33 Another cross-sectional study was completed by Beshara et al 9 in which they reported that mindfulness enhanced one’s feeling of control and decision-making process with regard to portion size. Participants who self-reported as more mindful eaters as measured by the Mindful Eating Questionnaire, moderated their portion sizes better, ate less energy dense foods, and reported less emotional and stress eating. 9
Grinnell et al 35 reported on a mindful eating intervention with first-year college students. The 3 sessions delivered over 8 weeks during a regularly schedule course introducing the students to the university resulted in increased mindfulness, as measured by the Mindful Attention Awareness Scale. 12 The increased mindfulness was positively associated with self-regulation and negatively associated with external and emotional eating. 35 Additionally, at postintervention, those who received the mindful intervention had significantly smaller waist circumferences than participants who received a traditional dietary intervention. 35 Unfortunately, the study’s short intervention period did not permit examination of more robust changes in additional anthropometric measures. Tapper et al 36 examined the impact of a randomized, controlled trial of a mindfulness-based weight loss intervention versus a nontreatment control group in women trying to lose weight. The participants met with study staff for 3 weekly sessions and then a follow-up 3 months later. While the intent-to-treat analysis did not show a significant difference in weight parameters, the efficacy analysis showed that those who attended the mindfulness sessions lost ~3 pounds. 36 As speculated, changes in emotional eating were significantly associated with changes in body mass index. 36 Kidd et al 10 completed an 8-week intervention as well, but the participants met with study staff weekly. They examined the impact of a mindful eating program on eating behaviors, biomarkers of weight, and weight loss self-efficacy in urban, obese women. Though there was a significant improvement in reported self-efficacy for weight loss among participants trained in mindful eating, contradictory to other mindfulness and mindful eating research, there were no improvements in mindful eating or any anthropometric biomarkers. 10
The study by Miller et al 19 had a more intensive and lengthy intervention (10 sessions delivered over 3 months) than did Tapper et al 36 (intensity) or Grinnell et al 35 and Kidd et al 10 (intensity and length). Miller et al 19 enhanced diabetes self-management education sessions with mindful eating constructs and reported significant increases in mindfulness and weight loss and less overeating compared with traditional diabetes self-management. Additionally, these changes at postintervention were also observed at follow-up 3 months later. 19 Collectively, the outcomes from these cross-sectional, quasi-experimental, and randomized clinical trials are promising in light of the challenges seen with traditional methods for healthy weight regulation. Further research on the applicability of mindful eating constructs, as well as the use of valid assessment tools, is warranted and will help inform clinicians aiming to support patients’ weight management goals.
Measuring Mindful Eating
Identifying effective and reliable measures of mindful eating are critical for researchers and clinicians. 37 Currently available mindful eating assessments are based on surveys that measure general mindfulness 14 as a trait 34 : such as the 15-item Mindful Attention Awareness Scale, 12 The Freiburg Mindfulness Inventory (30 items and 14 items), 38 and the 39-item Kentucky Inventory of Mindfulness Skills 15 ; or a state, such as the Toronto Mindfulness Scale. 34 For reviews of various mindfulness assessment tools, including strengths and limitations, see Baer et al 37 and Park et al. 39
One of the most commonly used mindful eating assessments is the Mindful Eating Questionnaire with 28 items that measures the major constructs of mindful eating (disinhibition, awareness, external cues, distraction, and emotional response) and can be used in clinical and research settings. 14 However, the sample sizes used in the development and validation of the Mindful Eating Questionnaire have been small. 14 Therefore, researchers have used additional measures in conjunction with the Mindful Eating Questionnaire.9,10 Some of these other measures include the Weight Efficacy Lifestyle Questionnaire, which produces a more focused measure of mindfulness 10 ; the Dutch Eating Behavior Questionnaire, which assesses emotional eating 18 ; the Weight Efficacy Lifestyle Questionnaire, which assesses one’s ability to control eating in various situations 40 ; and the Three-Factor Eating Questionnaire, 41 which measures hunger, susceptibility to nonphysical hunger and dietary restraint, and disinhibition. 19 Measuring mindful eating suffers from the same limitations as measuring general mindfulness: additional, rigorous research, quantitative and qualitative, is needed to improve psychometric properties and construct validity. 39 As research and assessment methodologies in mindfulness advances, clinicians will have additional instruments that are valid and reliable to use while implementing the mindful constructs with their clients and patients.
Conclusion
When deciding on an approach to help a client or patient maintain a healthy weight, mindful eating is one such option to consider. While mindful eating is an emerging technique that needs further study,14,24,33 clinicians may find that this noninvasive approach works well with clients and patients who are open to the constructs of mindful eating. The literature does suggest, as with most behaviorally based dietary interventions, that it is important to incorporate mindfulness in incremental steps, 10 since some participants reported having difficulty with incorporating all the constructs at once. 36 In order for research to provide a robust assessment of mindful eating, an accepted, operational definition of mindful eating is needed,8,15,34 as well as validated and clinically applicable assessment tools. This will help researchers with reproducibility and clinicians to interpret the results. Additionally, more randomized, clinical trials with larger participant populations and more diversity are needed to increase the generalizability of results/outcomes and reproducibility of the research.7,8,14 Health care professionals, including registered dietitians, 24 nurses, 10 and primary care providers, 8 may find mindful eating practices a strategy to promote healthy weight regulation with clients and patients. 10
