Abstract
This review provides a summary of physical activity interventions delivered in faith-based organizations. Electronic databases were searched to identify relevant studies. After screening, a total of n = 27 articles matched our inclusion criteria; 19 were identified as faith-based interventions (some spiritual or Biblical element included in the intervention) and 8 as faith-placed interventions (no spiritual component). Among all interventions, the most common research design was a randomized controlled trial. African American women were the most commonly targeted population and predominately Black churches were the most common setting. The majority of studies used self-report measures of physical activity. Most of the interventions did not use a theoretical framework to shape the intervention and weekly group sessions were the most frequently reported intervention approach. Overall, 12 of the faith-based and 4 of the faith-placed interventions resulted in increases in physical activity. Recommendations for future faith-based physical activity interventions include more rigorous study design, improved measures of physical activity, larger sample sizes, longer study and follow-up periods, and the use of theory in design and evaluation. Although limited, literature on faith-based physical activity interventions shows significant promise for improving physical activity participation and associated health outcomes.
Introduction
Regular participation in physical activity (PA) has been shown to have a number of significant physical and mental health benefits, including improvements in fitness and strength, prevention of chronic diseases (ie, cardiovascular disease, diabetes, breast and colon cancer, osteoporosis), and a reduction in depression and anxiety.1,2 In Healthy People 2020, the US Department of Health and Human Services has set a number of objectives related to PA, with the overarching goal of improving the nation’s health and quality of life and reducing the incidence of health disparities. 3 Additionally, the current goals also include creating positive physical and social environments for supporting health and healthy behaviors, with a focus on multisectorial approaches that involve multiple institutions within the community, including schools, worksites, health care settings, or faith-based organizations (FBOs).
Spirituality and religion are often an integral part of a person’s well-being and may facilitate health behaviors and attainment of a healthy lifestyle.
Nearly 80% of the US population reports an association with a Christian denomination, 5% profess another faith, and nearly half report that their religious or spiritual conviction plays a major role in their daily lives. 4 Approximately 40% of Americans attend services at a religious institution once a week or more, and an additional 20% attend 1 to 2 times/month, indicating the significance of faith environments to many people. 5 Spirituality and religion are often an integral part of a person’s well-being and may facilitate health behaviors and attainment of a healthy lifestyle. Religious involvement is a strong predictor of longevity and lower mortality rates and has been associated with a lower risk of cancer development and better outcomes with cancer treatments. 6 A number of other chronic diseases and the multiple mental and physical complications associated with chronic diseases are minimized by regular religious involvement. 7 Evidence exists indicating that religion and spirituality are viable options for promoting the health and well-being in diverse populations of Americans. 8
Faith-based organizations may be particularly important for health promotion and behavior change initiatives designed to reach neglected and underserved populations. 9 Often, uninsured and underserved populations do not have the financial, transportation, and personal resources necessary to seek health promotion programs away from their communities or in private facilities. FBOs provide for trusting relationships, cultural sensitivity, access to services in their community, and at lower costs than other health promotion programs. 10 Community collaborative partnerships have been successfully established with FBOs to initiate health promotion programs and conduct research following formative contributions from church leaders, advisors, and individuals.10-13
Despite the breadth of knowledge on the importance of PA in promoting health and the importance of faith-based settings for reaching the general population, other reviews14-17 have not addressed faith-based PA interventions specifically. The purpose of this review was to systematically examine the existing literature describing faith-based PA interventions, outline relevant strengths and weaknesses of the literature, and suggest recommendations for future studies.
Methods
Data Source
In February 2011, PubMed, Medline, PsychInfo, Web of Science, CINAHL, Sport Discus, and ERIC were searched to identify relevant articles on faith-based PA interventions, defined as an intervention in a religious organization or institution that included and assessed PA as an outcome variable. The search terms included faith-based and church-based with PA, fitness, exercise, weight loss, weight management, cardiovascular disease prevention, cancer prevention, and diabetes prevention. Additionally, bibliographies of relevant review articles related to faith-based interventions were searched. The search was rerun in May 2011 using the criteria described above to capture any new articles that had been published.
Study Inclusion and Exclusion Criteria
A total of 734 references were identified from searching the electronic databases. The article titles and abstracts were reviewed by the authors to exclude duplicates and other publications categorized as not appropriate (eg, not in English, not a peer-reviewed publication). After this first review, the authors reviewed the articles in more detail, eliminating those that were deemed to be inappropriate. The remainder of the articles were reviewed in greater detail by 2 or more of the authors to ensure that the articles met the following criteria: (1) based in a religious or faith organization, (2) included PA as a behavioral target, (3) reported on outcomes, and (4) published in English in a peer-reviewed journal prior to May 2011. After the articles were reevaluated, they were classified as either faith based or faith placed. Using criteria similar to other faith-based reviews, 16 an intervention was determined to be faith based if it offered some degree of spiritual/religious involvement, reference to the Bible or other faith traditions, was institutionalized into the FBO, or delivered by trained FBO volunteers. An intervention was categorized as faith placed if it did not have a spiritual/religious component to the intervention and was the FBO as a recruitment location or physical space for intervention activities. Faith-placed interventions did not specifically exclude culturally tailored interventions. For the included studies, the reviewers noted the main behavioral and physiological outcomes and method of assessment for each, study design, population targeted (age, gender, race/ethnicity), setting details (denomination, size of FBO, location), intervention details (types of activities, degree of tailoring, control/comparison activities), and outcomes.
Results
After running all searches, several references were found to be duplicates (n = 310), not peer-reviewed publications (n = 35), just a published abstract (n = 7), and not published in English (n = 3). On further review by the authors, other articles (n = 379) were excluded for the following reasons: not faith based (n = 70), not related to PA (n = 145), and not an intervention outcome article (eg, cross-sectional, commentary, descriptive, or review paper; n = 110), leaving 54 publications to be reviewed in greater detail. These papers were reviewed in greater detail by 2 authors and several (n = 27) were not included in the review because it was not faith based18-22 (n = 5), not enough information about PA available23-30 (n = 8), descriptive11,31-41 (n = 12), or a review paper15,42 (n = 2), leaving 27 to be included in the final review. Of these 27, 19 were determined to be faith-based interventions and the remaining 8 were classified as faith-placed interventions (Figure 1).
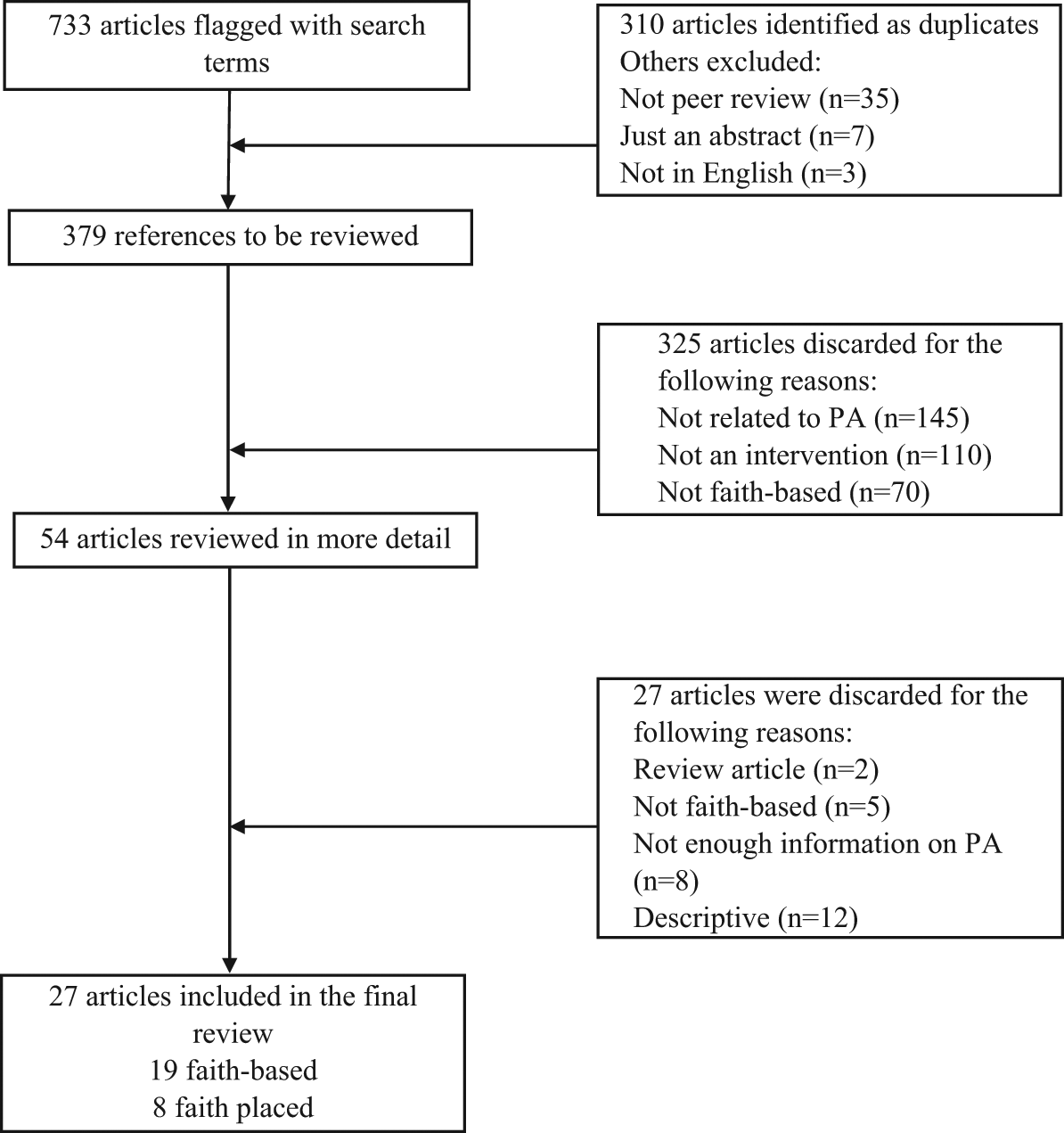
Review Process of Faith-Based Physical Activity Interventions.
Faith-Based Interventions
Study design and details
The summary of faith-based interventions is found in Table 1. The majority of the faith-based interventions used a randomized controlled trial approach (n = 11),12,43-52 whereas the remaining studies were either single group design53-56 or quasi-experimental.57-60 The majority of the studies specifically targeted African American women in their interventions to test spiritually and culturally appropriate approaches to increase PA.* Of those studies that targeted African American adult men and women,12,50,56,57,59 the samples were predominantly women (mean 78% females). The racial/ethnic composition of a study conducted in Birmingham, Alabama, was not reported, but the sample was 67% female. 54 Only 2 studies targeted Latino populations. A sample of Latino adult men (81%) and women (62%) were recruited from 3 churches that participated in Faithful Footsteps PA intervention. 43 In another study, middle-aged minority women (48% Hispanic; 46% African American; 6% other race) were assigned to either one of 2 churches or 1 clinic setting to receive a culturally appropriate music and aerobics intervention. 58 Other populations of faith-based interventions targeted children, 49 predominantly rural Caucasian women, 48 or Australian women. 46 The most common setting for faith-based interventions were predominately Black churches (n = 12) of multiple denominations (including Baptist and African Methodist Episcopal). Six studies indicated that the intervention took place in urban settings, † 1 in suburban FBO 56 and 2 in rural FBOs.47,48
Faith-Based Physical Activity Interventions
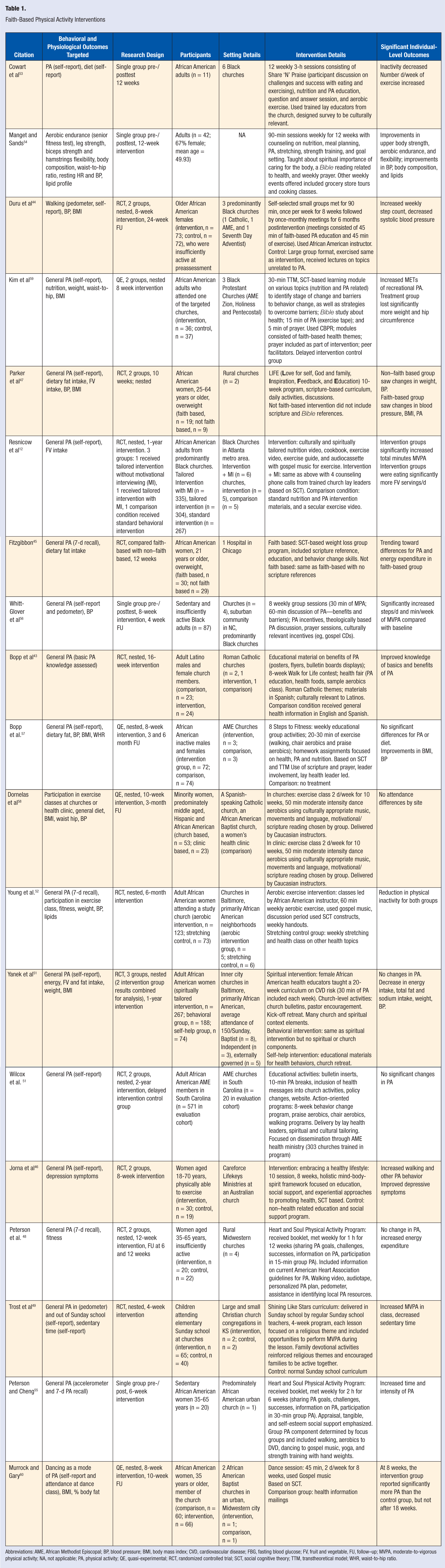
Abbreviations: AME, African Methodist Episcopal; BP, blood pressure; BMI, body mass index; CVD, cardiovascular disease; FBG, fasting blood glucose; FV, fruit and vegetable, FU, follow–up; MVPA, moderate-to-vigorous physical activity; NA, not applicable; PA, physical activity; QE, quasi-experimental; RCT, randomized controlled trial; SCT, social cognitive theory; TTM, transtheoretical model; WHR, waist-to-hip ratio.
Outcomes and measurement
Regarding PA measurement among the faith-based interventions, only 444,49,55,56 used a form of objective monitoring for PA behavior (ie, accelerometers, pedometers); 4 of the studies used the 7-day PA recall,45,48,52,55 a valid and reliable self-report instrument; 2 used attendance at classes or events as their measure of PA58,60; and the remaining 12 used a variety of validated self-report PA surveys. Eight studies targeted diet or nutritional variables in addition to PA participation.* Several studies also targeted additional physiological outcomes (body composition, n = 9 † ; blood pressure, n = 544,47,54,57,58; cardiorespiratory fitness, n = 348,52,54; blood lipids, n = 152). Twelve of the interventions saw improvements in PA variables, ‡ 6 reported positive physiological outcomes, § and 2 reported dietary changes.12,51
Intervention details: Theory
Of the 19 studies reviewed, 10 studies delineated the theoretical basis for the intervention.* Several theories were used to guide the faith-based interventions reviewed, most commonly the transtheoretical model,50,57,59 the social cognitive theory, † and social support theory or models.48,55,59 One study was based on the social ecological model 50 and one study indicated the theoretical background was to test a culturally tailored self-help intervention based on cultural sensitivity including deep and surface structure components. 12 Two studies did not specifically state a guiding theoretical basis for the intervention but measured social support and self-efficacy outcomes.52,58 Although approximately half of the faith-based studies indicated that the intervention was theoretically driven, little difference in study outcomes were noted based on whether theory was used or not. The most commonly used theory was the social cognitive theory, which has been widely used in other PA intervention research.
Intervention details: Intensity and duration
The duration of the interventions varied, however, the majority of the faith-based interventions were conducted over an 8- to 12-week period,43-48,54,56-60 and only 2 studies were 6 weeks or less in duration.49,55 Studies with longer durations were variable in length; 16 weeks, 53 6 months, 52 1 year, 51 and 2 years. 50 The time frame from baseline to follow-up outcome data collection also markedly differed in the studies. The shortest time frame from baseline to follow-up was 4 weeks and coincided with the shortest duration of an intervention. 49 Outcome data in most of the studies were collected in 8 to 12 weeks from baseline and the beginning of the intervention.* Several studies collected outcome data from 16 weeks to 24 months,52,53,57 although Bopp et al 57 and Cowart et al 53 had collected prior outcome data at 12 weeks. The studies that collected long-term PA outcome data ranged from 1 year 51 to 56 weeks, 12 and 2 years. 50 The interventions with the longest durations generally had a longer time frame from baseline to outcome data collection.
Although not consistently reported, the intensity of the interventions varied. Most of the faith-based PA interventions were approximately 75 to 90 minutes per session or per week (approximately 900-1000 minutes for the total intervention).* The most intense intervention was the Share ‘N’ Praise intervention, which consisted of 1.5-hour exercise and 1.5-hour nutrition and health information sessions for 12 consecutive weeks for a total intervention time of 2160 minutes. 53 Several studies had less intensive intervention lasting 60 minutes or less per week and were less than 12 weeks in duration (≤ 600 minutes in the entire intervention).43,49,57,59 Faith-based PA interventions varied considerably from 90 minutes per week for 12 weeks 53 (most intense) to unstructured interventions in which participants were provided information, yet were asked to implement PA behaviors on their own.12,50
In contrast to what one might expect, the interventions with higher intensity and longer duration did not necessarily improve program outcomes. In the most rigorous intervention reviewed, fewer participants reported “no exercise” following the intervention (decreased from 45% to 27%), yet more participants reported “no exercise in the last month” than at baseline. 53 Although, one minimally intensive unstructured RCT did not find significant changes in PA following the intervention, the 2-year follow-up was relatively long term. 50 Resnicow et al 12 identified significant increases in PA behavior immediately following a brief, unstructured intervention (56 weeks) in the 2 interventional groups as compared with the control group. Most faith-based PA interventions were conducted in 75 to 90 min/week and positive changes in PA behaviors were generally noted. An increase in various short-term (≥6 months or less) PA behaviors was noted in most studies; however, studies rarely evaluated long-term PA behaviors or outcomes.
Intervention details: Approaches
Of the 19 studies reviewed, the most common intervention approach was the use of weekly class sessions (n = 15) that were held in churches (n = 13) or in clinic/hospital settings (n = 2).45,58 In a study of urban minority women, 2 intervention groups were conducted in churches and attendance outcomes were compared with a group that was conducted in a women’s clinic. 58 Faith on the Move spiritual intervention was compared with a similar nonspiritual intervention, yet both study groups were conducted in a hospital setting. 45 Faith on the Move researchers chose not to use a church setting in order to minimize the likelihood that the comparison group would inherently include elements of religion/spirituality in their sessions if held in a church. 45
Most of the faith-based PA interventions reviewed included an informational/educational session and a guided PA or exercise component. Exercise sessions typically last 30 to 45 minutes in length, ranging from 10 minutes of exercise 50 to 90 minutes 53 at each session. Several of the PA components included culturally appropriate spiritual or gospel music during exercise52,58 or spiritual dancing/ aerobics.50,55,60 A number of the studies used lay leaders of the same race/ethnicity as the study population to lead the exercise sessions 53 whereas others used certified fitness instructors.52,58,60 Although, the leader of the exercise sessions was not consistently identified, in some interventions, sessions were conducted by research study staff in collaboration with church lay health educators.* Little evidence has been found delineating specific characteristics of exercise leaders or the ideal length of exercise sessions.
Although, most of the faith-based interventions included both informational and active participation in exercise during the sessions, the 2 larger interventional studies12,50 were less structured. Educational materials to promote PA were provided, and the participants were encouraged to use the materials to exercise on their own.12,50 In the Healthy Body Healthy Spirit intervention, 12 4 motivational interviewing telephone counseling calls were added to supplement fruit and vegetable consumption (but not PA) in 1 of the 3 study groups that receive the initial educational materials. In the Health-e-AME Physical-e-Fit intervention, 50 trained lay health leaders were provided instruction on how to deliver both action-oriented (behavior and skill-based class, walking programs, praise aerobics, and chair aerobics) as well as educational activities. Leaders were expected to implement the activities that were appropriate for their church, with some leaders implementing minimal activities and some implementing several from the available choices.
Of the faith-based studies reviewed, all but one 60 provided educational materials or didactic educational sessions to promote attainment of PA recommendations among study participants. The one study that did not provide an educational component promoted culturally appropriate dance routines with guidance on dance steps and a dance video to do on their own. 60 Several of the educational sessions were taught by trained lay health educators in the churches,* and in other studies, professional health educators or exercise trainers were hired to deliver the information.46,52,53,56,58 Yet, in a number of studies, research staff with various professional health backgrounds (eg, psychologist, nurse, health educator) conducted the study interventions. † In one study, 47 a county extension agent taught both the spiritual and nonspiritual LIFE project weight loss intervention. Modest, short-term PA behaviors have improved following brief, moderate, and longer informational sessions provided by qualified fitness trainers or health professionals.
The majority of the faith-based interventions used a spiritual component, including scripture, Bible verses, prayer, or gained various levels of pastor support and commitment. The intensity of the spiritual intervention varied across the faith-based studies. The 2 least intensive spiritual interventions involved the use of gospel music for dance 60 or in exercise sessions 52 and a health program using a holistic “mind–body–spirit” framework. 46 Most of the faith-based interventions used scripture readings and Bible verses to supplement the health interventions.* More intensive faith interventions included not only Bible references and scripture readings but also included prayer supplications.44,48,53,55,56 Although not always delineated, pastor support varied from involvement in planning the program (community participatory approach) and consenting to church participation to supporting the health intervention in sermons and other church activities. Of the 15 studies that used an experimental design with a control or comparison intervention, the most common approach was to deliver a similar but nonspiritual condition (n = 8), † followed by a delayed intervention (n = 2),50,59 and no treatment (n = 1).46,57 Other studies randomized to 2 different faith-based interventions: church or clinic setting 58 and aerobic exercise versus stretching intervention. 52 In the faith-based PA interventions reviewed, no obvious distinctions could be made indicating that a higher degree of spiritual or religious engagement had a greater impact on outcome behaviors. However, spiritual and religious outcomes are rarely measured pre-/postintervention, and only one study reviewed in this study assessed spiritual and religious characteristics in the intervention and comparison groups at baseline. 45
Faith-Placed Interventions
Study design and details
The summary of faith-placed interventions is found in Table 2. Five faith-placed interventions used a randomized controlled trial approach,61-66 whereas the remaining 2 interventions67,68 used a single-group design. African Americans were the most common race/ethnicity targeted (n = 5), followed by Pacific Islanders (n = 1), 65 with 266,67 targeting both Caucasians and African Americans. Five of the interventions61-65 targeted individuals with diabetes or those at risk for diabetes. Predominately Black churches were the most commonly targeted setting (n = 6).62-64,66-68
Faith-Placed Physical Activity Interventions
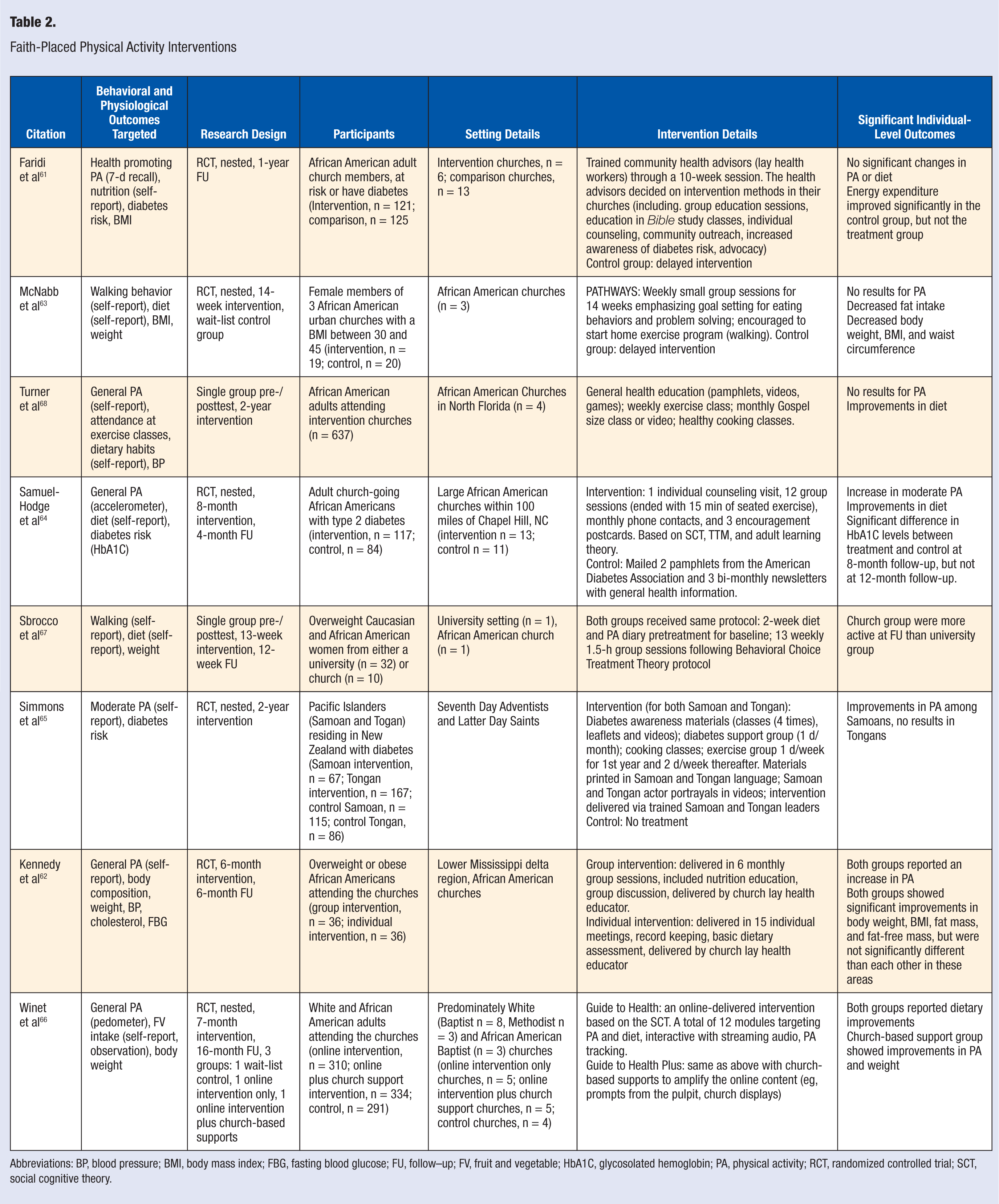
Abbreviations: BP, blood pressure; BMI, body mass index; FBG, fasting blood glucose; FU, follow–up; FV, fruit and vegetable; HbA1C, glycosolated hemoglobin; PA, physical activity; RCT, randomized controlled trial; SCT, social cognitive theory.
Outcomes and measurement
Five interventions targeted diet or nutritional outcomes in addition to PA,63,64,66-68 5 targeted body composition,61-63,66,67 2 targeted blood pressure,62,68 2 targeted diabetes risk,61,64 and 1 targeted blood lipid profiles. 62 Five of the interventions reported significant improvements in PA variables,62,64-67 4 reported improvements in physiological variables,62-64,66 and 4 indicated that there were improvements in dietary outcomes.63,64,66,68 Among the faith-placed interventions, only 2 used objective measurement for PA (accelerometer 64 and pedometer 66 ), with the remaining studies using self-report measures (n = 5),39,62,63,67,68 7-day PA recall (n = 1), 61 or attendance at exercise classes (n = 1). 68
Intervention detail: Theory
Only one of the faith-placed studies specifically reported a theoretical basis for their interventions. Winett et al 66 compared the Guide to Health (GTH) and the GTH-Plus interventions with a control group to promote healthy eating and PA. The GTH-Plus was based on the social cognitive theory and church-based supports, including reminders in church bulletins, from the pulpit and on posters that were used to promote self-regulation. Several of the interventions were based on a guiding model in the development of evaluation of the intervention; Turner et al 68 and Sbrocco et al 67 used the Planned Approach to Community Health Program Model as part of an empowerment learning process in an African American community and the PRECEDE model 69 in the development of the evaluation processes. The Behavioral Choice Treatment approach to weight management is based on tenets of cognitive behavioral theory and has been tested in previous research. 67
Intervention detail: Intensity and duration
The faith-placed interventions reviewed were not specifically targeted to increasing PA but for diabetes prevention/control,61,63-65 weight management/loss,62,66,67 or prevention of cardiovascular disease, 68 which included a wide-range of emphasis on PA behavior. The faith-placed studies (n = 7) generally had a longer intervention period when compared with the faith-based interventions. Three studies lasted 12 to 14 weeks,63,66,67 2 studies had a duration of six 62 to eight months, 64 and 2 studies extended a year,61,68 and 1 lasted 2 years. 65 In several of the interventions that lasted a year or longer, significant changes in PA were not found,61,68 and in the 2-year study conducted in New Zealand, significant changes in the Samoan group were noted but not in the Tongan group. 65 Both studies that had intervention durations of 6 to 8 months found significant increases in PA and in the 1-year follow-up.62,64 Sborocco et al 67 found that the group of African American church women and the university Caucasian women maintained or slightly increased time spent in PA over the year compared with the university African American women who decreased exercise minutes. The GTH and GTH-Plus interventions were 12 weeks in duration with follow-up at 7 and 16 months from baseline. 66 The number of steps/day was significantly greater at 7 months and to a lesser extent at long-term follow-up (16 months). 66
In several of the studies reviewed it was difficult to determine the amount of time and intensity devoted to promotion of PA behaviors as this was but one component of a multibehavior intervention.61,64,67 In other studies, regularly scheduled exercise sessions were held, including weekly, 68 biweekly, 64 or triweekly 65 for the duration of the intervention. The instructional sessions that appeared to be the most intense were 90 to 120 minutes weekly 63 and biweekly 64 for 12 to 14 weeks, as few studies specifically described the intensity or duration of specific components of their interventions. The GTH was a Web-based program delivered in 12 weekly modules that took 5 to 10 minutes to complete but the amount of time devoted to PA was not indicated. 66 Samuel-Hodge et al 64 reported that the exercise component was brief; 15 minutes of chair exercises at each biweekly sessions.
Intervention detail: Approaches
All of the faith-placed interventions targeted adults only (n = 8) and 2 targeted African American women only.63,67 Several studies included both educational and exercise sessions,64,65,68 and others had educational sessions61-63 or cognitive behavioral sessions 67 only. The GTH-plus had both educational and self-regulation behavioral strategies. 66 When reported, trained lay health educators, who were selected at the recommendation of pastors or church health advisory councils, often conducted the interventions.61-65,68 Of the 5 interventions that had more than 1 condition, 361,63,66 used delayed intervention groups, 164 used an information-only approach, 165 used a no-treatment control group, and 162 compared group and individual approaches.
Discussion of Literature
This comprehensive literature review of faith-based PA interventions has yielded a number of important insights on the current status of the science. A number of consistent trends were identified across the studies included in this review; most notably issues related to the specifics of the study as well as elements of intervention themselves. The lessons learned from many of these studies provide some strong recommendations for future studies.
Study Design and Details
Research design
From a study design standpoint, there were several studies included in this review that did not use rigorous methods for evaluating the effectiveness of the intervention on PA behavior or other outcomes of interest, including single group or nonrandomized designs. However, it was promising to note that the majority of studies used randomized controlled trial approaches, the gold standard for determining the effectiveness of interventions, and of those, 6 were faith-placed61-66 and 11 were faith based12,43-52 with the remaining studies using less rigorous designs. Almost all of the faith-placed studies used a strong research design compared with the faith-based studies although, not specifically stated many of the faith-placed interventions targeted a combination of physiological health variables and behavioral outcomes.
Among the faith-based studies, study design remains a concern for examining the efficacy of the interventions. The lack of research control that is missing in single group designs and other nonrandomized approaches threatens internal validity and limits the ability to draw conclusions from the existing literature. Several studies50,51,57 have noted challenges in partnering with community faith settings and in using a traditional research design, especially a no-treatment control group, as FBOs may be hesitant to participate in a study where participants could be randomized into a “less-desirable” situation. Some acceptable strategies to counterbalance these design issues although maintaining experimental standards could include wait-list or delayed control groups, self-help conditions, or attention-only control groups in which participants receive a worthwhile intervention with a completely different focus. One control group strategy that may not be effective is to use a similar intervention to target the same behavior and outcomes, only without the spiritual components. As one study noted, 51 participants in any intervention delivered in a faith-based setting are likely to implement spiritual or faith qualities (eg, fellowship, prayer before meetings, including FBO leadership) that are inherent to faith settings leading to a situation where the intervention and comparison groups receive essentially the same intervention, which could lead to a type III error.
Most of the studies randomized to study group by church and not by an individual participant, leading to “nesting” or the extraneous influences of the church environment on study outcomes rather than the intervention alone. Only a few studies* addressed the nesting issue in the statistical analyses. Overall, the studies were short in length, many with an intervention period of 12 weeks or less, and only 8 † followed up with the participants after the intervention period was over. This short study length is often too brief to see changes in physiological outcomes, which can take several months to adapt to regular participation in PA.1,70 Previous research indicates that most people who start an exercise program quit within 6 months. 71 Several studies also inexplicably found changes in physiological outcomes without finding changes in PA participation and suggested PA mediated those physiologic changes. This may indicate that there is some measurement issues associated with the behavioral outcomes or lack of control
Physical activity measurement issues
Compounding the issues associated with a weak study design are those associated with the measurement of the main behavioral outcome of interest, PA. Of the 27 studies included in this review, only a few44,49,56,64-66 used some method of objective PA assessment (eg, accelerometer or pedometer), and 3 assessed cardiorespiratory fitness.48,52,54 Several studies58,60,68 used attendance at exercise classes or intervention programs/activities as a main behavioral outcome, which does not consider PA done in addition to the intervention (eg, lifestyle, occupational, transportation related). The remainder of the studies used a subjective form of assessment, generally self-report, which presents challenges for validity and reliability for PA participation and may not be sensitive enough to detect changes in PA pre-/postintervention. It is interesting to note that all of the studies that measured fitness as an outcome or used an accelerometer or pedometer reported improvements in PA participation among participants.
There are important considerations for choosing an appropriate measure of PA for research in community setting that is reasonably priced, feasible to use, valid, and reliable. Accelerometers are an expensive method of evaluation, require advanced knowledge for processing outcomes, and may not be available to all researchers and practitioners. Pedometers are a less expensive option, but may be reactive and less accurate, and skew outcomes. Both these devices require a commitment from participants to be worn properly and record important daily information, which can increase participant burden. With self-report measures, there is clear benefit in being able to capture domain or type of PA and other context-related information about PA, although they are less able to accurately capture information on intensity, frequency, or duration of PA compared with objective assessments. 72 The selection of a valid, reliable, sensitive, and culturally appropriate self-report measurement tool for the population may be an acceptable alternative to objective measures. The addition of other objective forms of assessments would provide the most comprehensive approach for determining the effectiveness of interventions for improving PA behavior and is recommended for future faith-based PA interventions.
Participants and setting
The statistical power of the studies was potentially limited by the number of participants. The majority of the studies had small sample sizes and less than half* reported a combined sample size greater than 100, increasing the chance of type II error, though among these largest studies, only 8 studies † saw significant outcomes for PA. Overall the targeted populations were very similar; all but one study 49 targeted adults and many ‡ targeted women only, whereas none targeted men only. Most of the studies targeted African Americans, whereas only 2 studies43,58 targeted Latinos and 1 study 65 targeted Pacific Islanders. The limited samples and study populations create a significant gap in the knowledge for generalizing the effectiveness of faith-based PA interventions to multiple racial/ethnic groups, age, or gender. Corresponding to the populations targeted, the majority of the settings targeted were predominately African American churches. In the majority of the studies, there was a lack of detail on the faith settings, including size of the setting, denomination, or urban/rural location. This information is essential for other researchers and practitioners to extrapolate findings and apply in partnerships with FBOs in their own communities. Future studies should include a complete description of the setting and the population to allow for study replication.
Effectiveness
The majority of the studies saw some significant improvements in PA behavior from baseline to follow-up and where appropriate, relative to the comparison group. Half of the studies that targeted physiological health outcomes (eg, body composition, blood pressure) were successful (9 of 17 studies). Several of the studies included behavioral outcomes that included dietary changes as a main variable. The evidence on the effectiveness of interventions targeting multiple behavior change across different settings and delivery approaches is somewhat mixed,73-76 and the results of these studies (6 of 9 studies that targeted dietary outcomes identified significant improvements) indicate that additional research is warranted in targeting multiple health behaviors. Several issues associated with study design, sample size, and measurement issues are significant factors that may have limited the ability of these interventions to find positive outcomes for PA, diet, and physiological outcomes, similar to interventions in other settings and populations.71,77 Future faith-based interventions should consider using rigorous experimental design, valid, reliable, and sensitive measures of behaviors and outcomes, and adequate sample sizes to increase the likelihood of seeing significant results and truly examining the effectiveness of the designed intervention.
Intervention Strategies
Use of theory
Only about half of the faith-based studies* and one of the faith-placed studies 66 reviewed were guided by theoretical frameworks. The lack of a theoretical basis in this area of research makes it difficult to identify relationships and to determine the mechanisms of action that led to the desired outcomes of health behavior change. The most common theory used to guide research in the faith-based studies was the social cognitive theory, 78 which emphasizes health behavior change predominantly at the personal or indivi dual level. An important step in advancing faith-based PA research would be to design and critically evaluate the theoretical frameworks guiding the interventions.
Many health behaviors, including PA, depend on influences beyond an individual’s personal choice, and changes at multiple levels are needed to encourage healthier lifestyles at the individual, social, community, and policy levels. The social–ecological model of health promotion has been used to explain the multilevel components and the interrelationship of individual, social, organizational, community, governmental, and public policy factors that affect health. 79 To guide continued research in faith settings, the community-based participatory research approach should be used to foster health promotion at multiple levels. Environmental and structural capacities, social capital and social networks, and social support should be assessed and strengthened in collaboration with the faith setting to develop and test effective health promotion interventions. Only the Health-e-AME study 50 used the social–ecological model as a guiding framework to steer the wide reaching intervention that partnered with the African Methodist Episcopal church statewide. The faith, activity, and nutrition study, 80 also delivered in African Methodist Episcopal churches, outlined an interventional strategy within an ecological framework and serves as an example of multilevel strategy. Aside from these examples, this review indicates the need for broader theoretical approaches for greater institutionalization and potential public health impact.
Role of faith leader
Although many other reviews13,81,82 have noted the importance of pastor or faith leader involvement, the majority of the studies did not note how or if the leader was incorporated into the intervention beyond initial contact or how support was garnered for recruiting participants. Recent evidence has suggested the importance of the faith leader’s health, health behaviors, and perceptions toward health are an important influence on the physical and social environment toward health in the church.83,84 Future studies should attempt to more carefully document the role and influence of the leader in designing, implementing, and facilitating the intervention process.
Dissemination
Many of the faith-based and faith-placed studies did not clearly delineate their interventions in the dissemination of the study findings. A few studies did report the amount of time devoted to structured education and exercise sessions, but many did not. Even though most studies reported some positive results, replication of the interventions would be difficult. In future faith-based and faith-placed research, the amount of time, intensity, and duration of interventions needs to be specified in order to repeat the interventions in future research or in implementing health programs in faith settings. Additionally, the faith-based lay health leaders of the exercise and educational sessions were not always described. Therefore, the qualifications, training, and ability to conduct a culturally appropriate intervention are not well delineated. The specific characteristics and training used in preparing the lay health leaders would be important information to use in other research with diverse groups of participants.
Conclusion
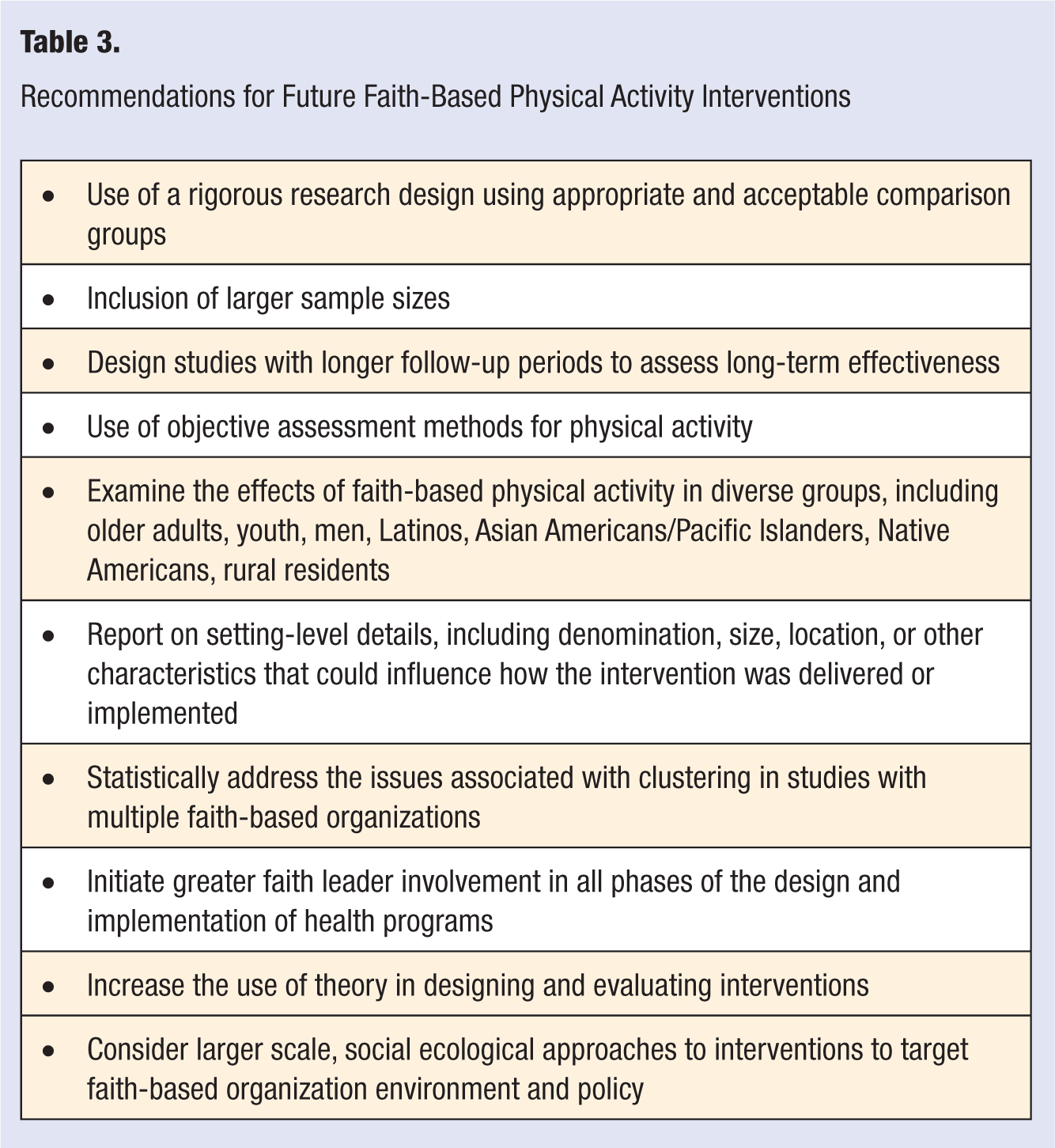
A summary of recommendations for future faith-based PA interventions can be found in Table 3. This in-depth review of the literature has provided significant insight into the current state of the science. Our recommendations are similar to other recommendation papers,13,81,82 indicating that there are a number of factors that can influence the success of faith-based interventions. Specific to the literature on faith-based PA interventions, the literature, though limited, shows significant promise for improving PA participating and associated health outcomes. Improvements in study design, measurement, and theoretical framework will improve the strength of the evidence for future interventions that are culturally appropriate to the specific community setting with widespread reach. Health promotion and PA interventions conducted in faith settings have shown promise in promoting healthy lifestyles in Americans and warrants further research efforts to create effective community partnerships by applying a model that faith settings can easily use to promote healthy lifestyles in their congregations and communities.
Recommendations for Future Faith-Based Physical Activity Interventions