Abstract
Diet and lifestyle factors of young adults and their relationship to health risk factors are understudied. Data from the Bogalusa Heart Study population (n = 1214; 19-39 years; 74.1% white; 60.8% female) were used to study associations of lifestyle, health risk factors, and reported health problems with the National Institutes of Health body mass index (BMI) categories of normal, overweight, and obese. Data from self-reported questionnaires and laboratory measures were evaluated using covariate-adjusted multinomial logistic regression and analysis of covariance, linear trend test, and the Cochran–Armitage trend test. Obese individuals had lower odds of consuming high-fat dairy products (odds ratio [OR] = 0.77; 95% confidence interval [CI] = 0.62-0.96) and fruit/fruit juice/vegetables (OR = 0.83; CI = 0.75-0.93) and had higher odds of consuming hamburgers/sandwiches (OR = 2.81; CI = 1.52-5.20); processed meats (OR = 6.95; CI = 2.20-21.96); and sweetened (OR = 1.20; CI = 1.01-1.43) or diet beverages (OR = 1.27; CI = 1.02-1.58) than those of normal weight. Obese participants also had higher odds of being physically inactive versus being very active (OR = 2.65; CI = 1.64-4.29). Mean serum total and low-density lipoprotein cholesterol, triglycerides, apolipoprotein-B, and insulin resistance were higher (P < .05 for all) in the overweight/obese when compared with normal weight individuals. Values were higher in those with higher weight status (linear trend P < .0001 for all). Self-reported health problems also increased with BMI. Interventions to improve diet and physical activity patterns among overweight/obese adults in this age group are needed.
‘As individuals move from adolescence into young adulthood, their lifestyles change dramatically. Life stressors, including the transition to independent living, economic turmoil, and a role as a parent may contribute to unhealthy dietary and lifestyle habits.’
Overweight and obesity have been linked to many chronic diseases, including cardiovascular disease (CVD), hypertension, type 2 diabetes mellitus (T2DM), metabolic syndrome (MetS), some cancers, sleep apnea, and osteoarthritis.1,2 Using data from the 2007-2008 National Health and Nutrition Examination Survey, it was shown that 27.5% of men and 34.0% of women 20 to 39 years old were obese. 3 Compared with whites, the prevalence of obesity was higher among ethnic minority groups, with black females at the highest risk. 4 Although it appears that the levels of overweight/obesity is leveling off in most groups, it has been estimated that by 2030, obesity will cost the United States 860.7 to 956.9 billion dollars. 5 The cause(s) of overweight/obesity is multifactorial and includes physiologic, lifestyle, and sociodemographic factors. 6 Examining factors related to weight status is important to help plan effective prevention or treatment programs. 7
As individuals move from adolescence into young adulthood, their lifestyles change dramatically. Life stressors, including the transition to independent living, economic turmoil, and a role as a parent may contribute to unhealthy dietary and lifestyle habits.7-9 Young adults tend to skip breakfast, 10 consume foods away from home, 11 or consume energy-dense foods/beverages12-14 with large portion sizes. 14 These eating habits may result in poor nutrient adequacy or diet quality10,13 and may contribute to the development of overweight/obesity.12,14,15 Few studies have concentrated on the food habits of the young adult population as they relate to weight status.12,14,16
Other lifestyle changes may be associated with weight in this age group. Physical activity and exercise levels tend to decline with increasing age 17 and the percentage of those being “insufficiently active” (ie, 10-149 min/wk) increases from young adulthood to late adulthood. 18 Alcohol consumption and smoking behaviors may also relate to weight or adiposity measures in young adults; however, results from studies examining alcohol consumption19,20 or smoking21,22 and body weight or adiposity measures have been inconsistent.
Bogalusa, Louisiana, is a semirural community located in one of the poorest states in the United States. Populations from the rural or semirural southern United States are often susceptible to poor dietary habits23,24 and face nutrition-related health problems 25 at a younger age because of their low socioeconomic status. 24 Therefore, studies examining the role of correlates of overweight/obesity for this population are important. However, most studies examining the role of risk markers of CVD and T2DM by weight status have been conducted on adults older than 40 years. Studies, including the Coronary Artery Risk Development in Young Adults (CARDIA) Study and the Bogalusa Heart Study (BHS) have examined some risk factors in younger adults; however, additional studies are needed. The objectives of this study were to (a) examine the association of diet and other lifestyle habit correlates with overweight/obesity, (b) evaluate differences in risk markers of CVD and T2DM by weight status, and (c) determine the presence of obesity-related health problems by weight status in young adults from Bogalusa, Louisiana.
Subjects and Methods
Setting and Participants
The BHS began in 1973 as a cross-sectional investigation of CVD risk factors and their environmental determinants in a biracial (black/white) pediatric population from Bogalusa, Louisiana. The study was expanded to a mixed cross-sectional/longitudinal study design and included observations of young adults. Participants in the study presented here were from a cross-sectional survey on young adults (19-39 years; n = 1333) conducted in 1995-1996. Underweight participants (n = 50), pregnant or lactating women (n = 26), and those with extreme energy intakes (ie, <600 kcal in both genders (n = 2), men with energy intake >4200 kcal (n = 17), and women with energy intake >4000 kcal (n = 24) 26 were excluded for a final sample size of 1214. Details of the BHS study design, participation rates, and protocols have been published previously. 27 The BHS was approved by the Tulane University School of Medicine Institutional Review Board, and participants provided written informed consent prior to participating in the study.
Determination of Weight Status
Trained examiners collected data following the protocols of the BHS. 27 Briefly, the mean of 2 measurements for height (to the nearest 0.1 cm on a standard board) and weight (to the nearest 0.1 kg on a balance-beam metric scale) were taken. 27 Body mass index (BMI) was calculated as body weight (kg)/height (m2). The population was classed as normal weight (BMI ≥18.5 and ≤24.9 kg/m2), overweight (BMI ≥25.0 and ≤29.9 kg/m2), or obese (BMI ≥30.0). 28
Estimation of Food Group Consumption
The study population completed the youth/adolescent questionnaire (YAQ), a 131-food-item, self-administered, semiquantitative food frequency questionnaire (see the appendix).29,30 The YAQ is reliable 29 and valid 30 for use in epidemiologic studies in the adolescent populations, but it has also been used previously in the BHS on young adults. 31 The YAQ was chosen for use in this study since it contains more snack foods than most adult food frequency questionnaires and a review of 24-hour dietary recalls of the BHS showed that young adults consumed many snack foods. 32
A food/nutrient analysis program called the “hardvardsffq.042995” from the Harvard Food Frequency Questionnaire database 29 was used to process the food items in the YAQ. For the present study, food items from related foods/beverages (including alcoholic beverages) were grouped into similar food group categories, and 21 food/beverage groups from the YAQ were identified for the final analyses (Table 1).
Demographic Characteristics of Young Adults (19-39 Years) Participating in the Bogalusa Heart Study by Weight Status a
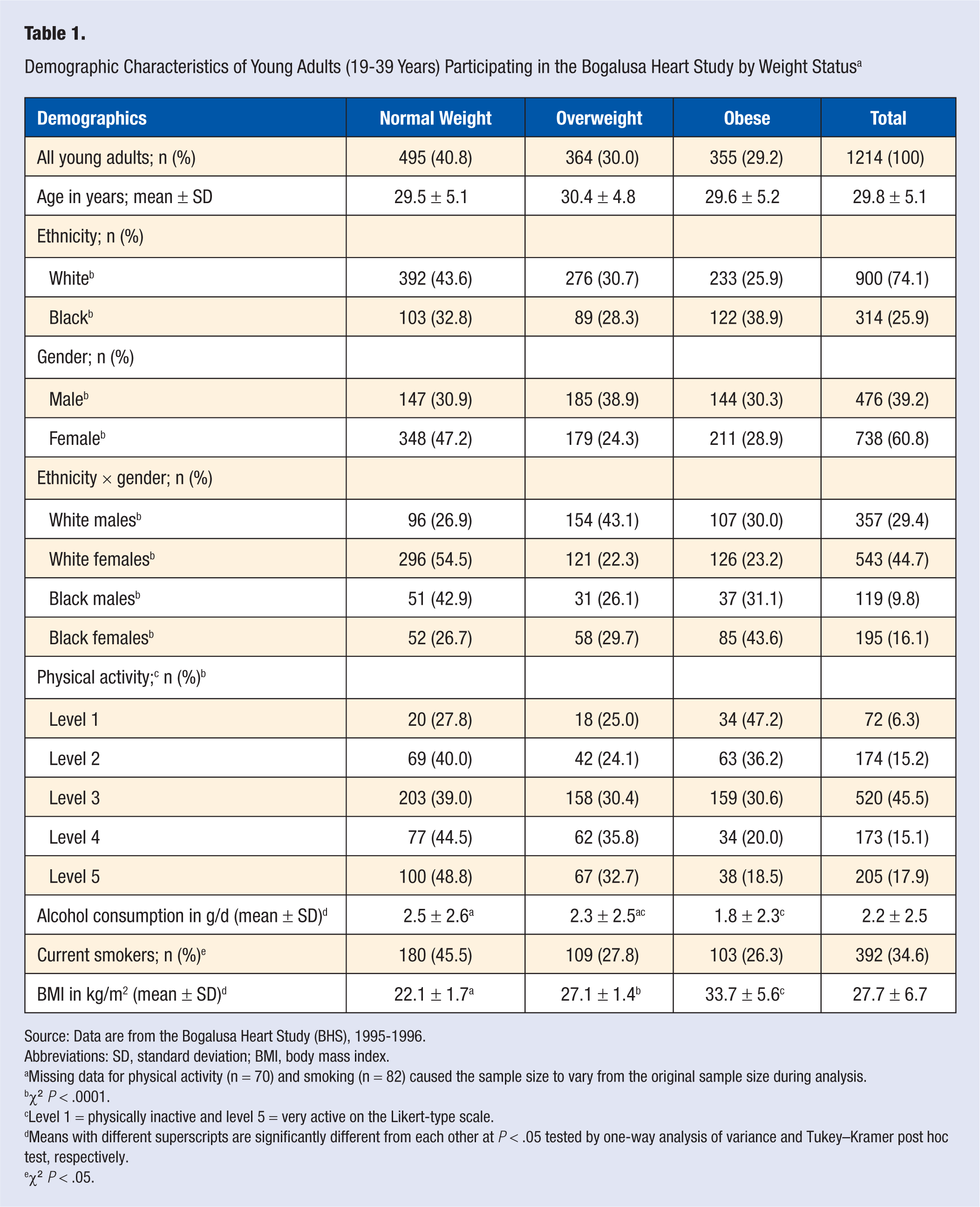
Source: Data are from the Bogalusa Heart Study (BHS), 1995-1996.
Abbreviations: SD, standard deviation; BMI, body mass index.
Missing data for physical activity (n = 70) and smoking (n = 82) caused the sample size to vary from the original sample size during analysis.
χ2 P < .0001.
Level 1 = physically inactive and level 5 = very active on the Likert-type scale.
Means with different superscripts are significantly different from each other at P < .05 tested by one-way analysis of variance and Tukey–Kramer post hoc test, respectively.
χ2 P < .05.
Other Lifestyle Habit Correlates
Self-administered health habits questionnaire to determine demographic and lifestyle habits were used. Data on leisure physical activity were obtained as a subjective rating given by the participants on a Likert-type scale, from 1 (physically inactive) to 5 (very active), adapted from the Lipid Research Clinics Questionnaire. 33 This questionnaire has high test–retest reliability (r = .85) and has been significantly associated with a 4-week physical activity history. 33 Alcohol consumption (grams) was calculated from the YAQ. Smoking status was defined as current smokers or nonsmokers.
Information on Medical/Health History
Self-administered questions elicited information on medical/health history. Questions were answered on a yes/no basis, indicating either the presence or absence of health problems (eg, high blood pressure).
Measurement of Laboratory Values
Total serum cholesterol and triglyceride levels were measured on fasting blood samples using enzymatic procedures on the Abbott VP instrument (Abbott Laboratories, North Chicago, Illinois); serum lipoproteins were analyzed using a combination of heparin-calcium precipitation and gel electrophoretic procedures. 34 Serum apolipoprotein A (Apo-A) and apolipoprotein B (Apo-B) were assayed by electro-immunoassay.35,36 Trained nurses measured right arm systolic and diastolic blood pressure in triplicate using the first and fifth Korotkoff phase readings. 27 Plasma glucose concentrations were determined using the glucose oxidase method using a Beckman glucose analyzer (Beckman Instruments, Fullerton, California); a radioimmunoassay kit was used to measure plasma immunoreactive insulin concentration (Padebas Pharmacia, Piscataway, New Jersey). Indices of insulin resistance and sensitivity were calculated according to the homeostasis model assessment (HOMA) formula 37 : [fasting glucose (mg/dL) × fasting insulin (µU/mL)]/405 and the Quantitative Insulin Sensitivity Check Index (QUICKI) formula: 1/[log fasting glucose (mg/dL) + log fasting insulin (µU/mL)], 38 respectively. Blind duplicates were used for quality control for all analyses. 27 Means of all replicate measures were used for statistical analyses.
Statistical Analyses
All analyses were performed with the Statistical Analysis System (SAS) software (version 9.2, Cary, North Carolina). Descriptive statistics, including means, standard deviations, and percentages summarized the demographic data. χ2 tests determined differences in the distributions of categorical variables and one-way analysis of variance determined differences in the means for continuous variables. Covariate-adjusted multinomial logistic regression was used to determine the association of being normal weight, overweight, or obese with the consumption of specific food group servings and presence or absence of other lifestyle habits. Outcomes consisted of comparisons between overweight versus normal weight and obese versus normal weight. The percentage variance explained by each of the dietary and other lifestyle habit correlates and demographics in overweight/obesity was determined using a single multinomial logistic regression model with weight status categories as the dependent variables. Pseudo R2 was calculated from the −2 log likelihood for the full model and the intercept. Partial correlation coefficients were used to determine the correlations between the food groups. Analysis of covariance, adjusted for covariates with Tukey–Kramer post hoc test was used to test the differences in the mean blood/serum levels of risk markers for CVD and T2DM among the 3 weight status groups. Linear trend testing was used to determine whether the presence of CVD and T2DM risk markers increased with increased weight status. The Cochran–Armitage trend test was used to determine the increasing trends in the presence of health problems by weight status. A significant association was defined if the unity was not in the 95% confidence interval (CI) of an odds ratio (OR) and a P value of <.05.
Results
Sample Characteristics
The final sample consisted of 74.1% whites and 39.2% men; with 29.4% white men, 44.7% white women, 9.8% black men, and 16.1% black women (Table 1). The mean age of the young adults was 29.8 ± 5.1 years. Among all young adults, 40.8% were normal weight (mean BMI 22.1 ± 1.7 kg/m2), 30.0% were overweight (mean BMI 27.1 ± 1.4 kg/m2), and 29.2% were obese (mean BMI = 33.7 ± 5.6 kg/m2). A higher percentage of white women was normal weight versus overweight or obese; a higher percentage of white men was overweight versus being normal weight or obese; and a higher percentage of black women was obese versus being normal weight or overweight (P < .0001; Table 1).
Dietary and Other Lifestyle Habit Correlates of Overweight/Obesity
The percentage variance explained by dietary and other lifestyle habit correlates, along with demographics, for overweight was 15% and for obesity was 23% (Figure 1). Diet explained only 4% and 9% of the variance in overweight/obesity, respectively (Figure 1); thus, a major percentage of variance in overweight (85%) and obesity (77%) remained unexplained (Figure 1).
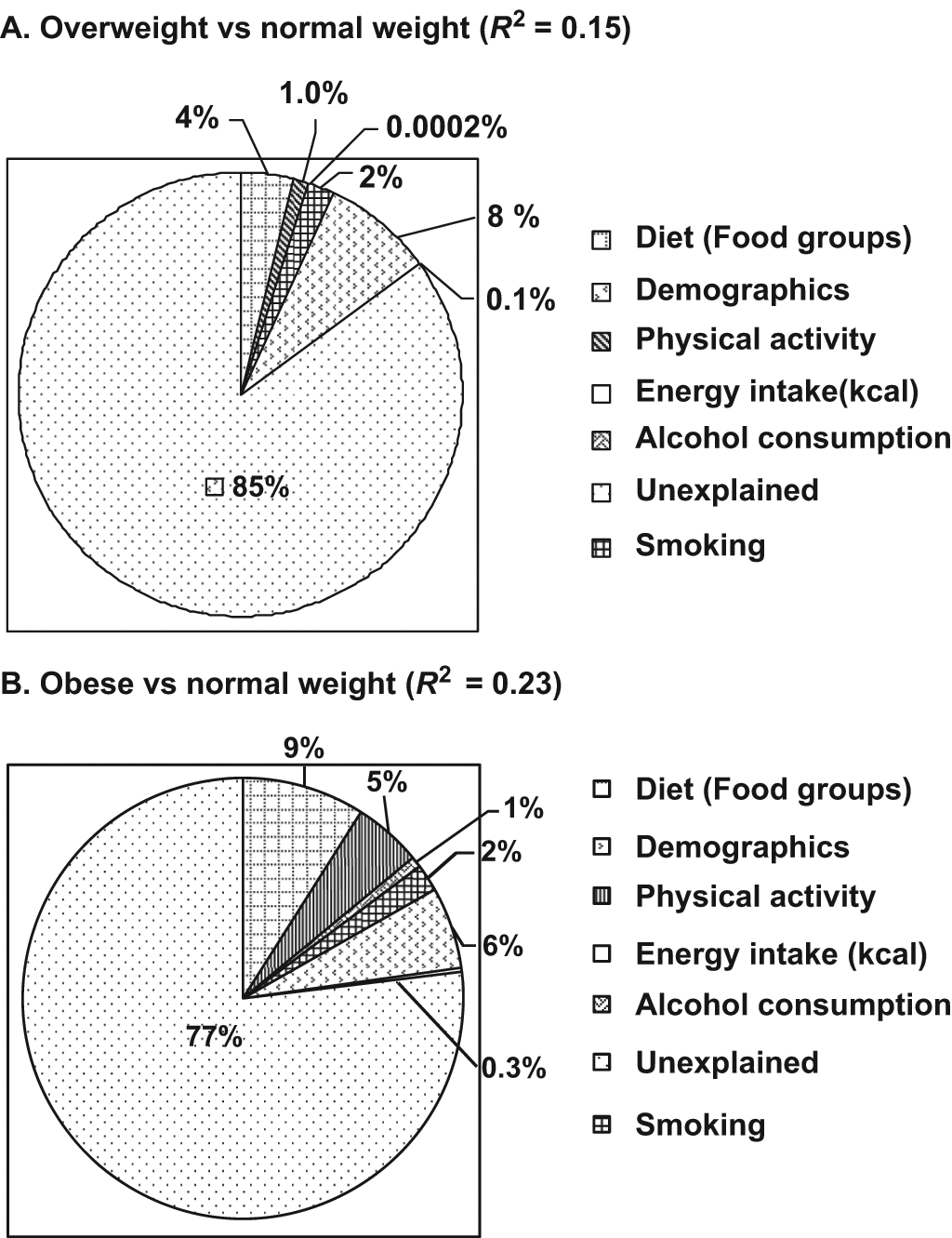
Variance Explained by Dietary and Other Lifestyle Habit Correlates of Overweight/Obesity in Young Adults (19-39 Years).
The mean consumption of food/beverage groups per day and their association(s) with overweight/obesity are shown in Table 2. Relative to normal weight, obese young adults had 23% lower odds of consuming dairy products (high fat; P = .02) and 17% lower odds of consuming fruits/100% fruit juices/vegetables (P = .001). Relative to normal weight, obese young adults had 2.8 times the odds of consuming hamburgers/sandwiches (P = .001), respectively. Relative to normal weight, obese young adults had almost 7 times higher odds of consuming processed meats (P = .001); 20% higher odds of consuming sweetened beverages (P = .04); and 27% higher odds of consuming diet beverages (P = .03; Table 2).
Dietary and Other Lifestyle Habit Correlates of Overweight/Obesity in Young Adults (19-39 Years) a
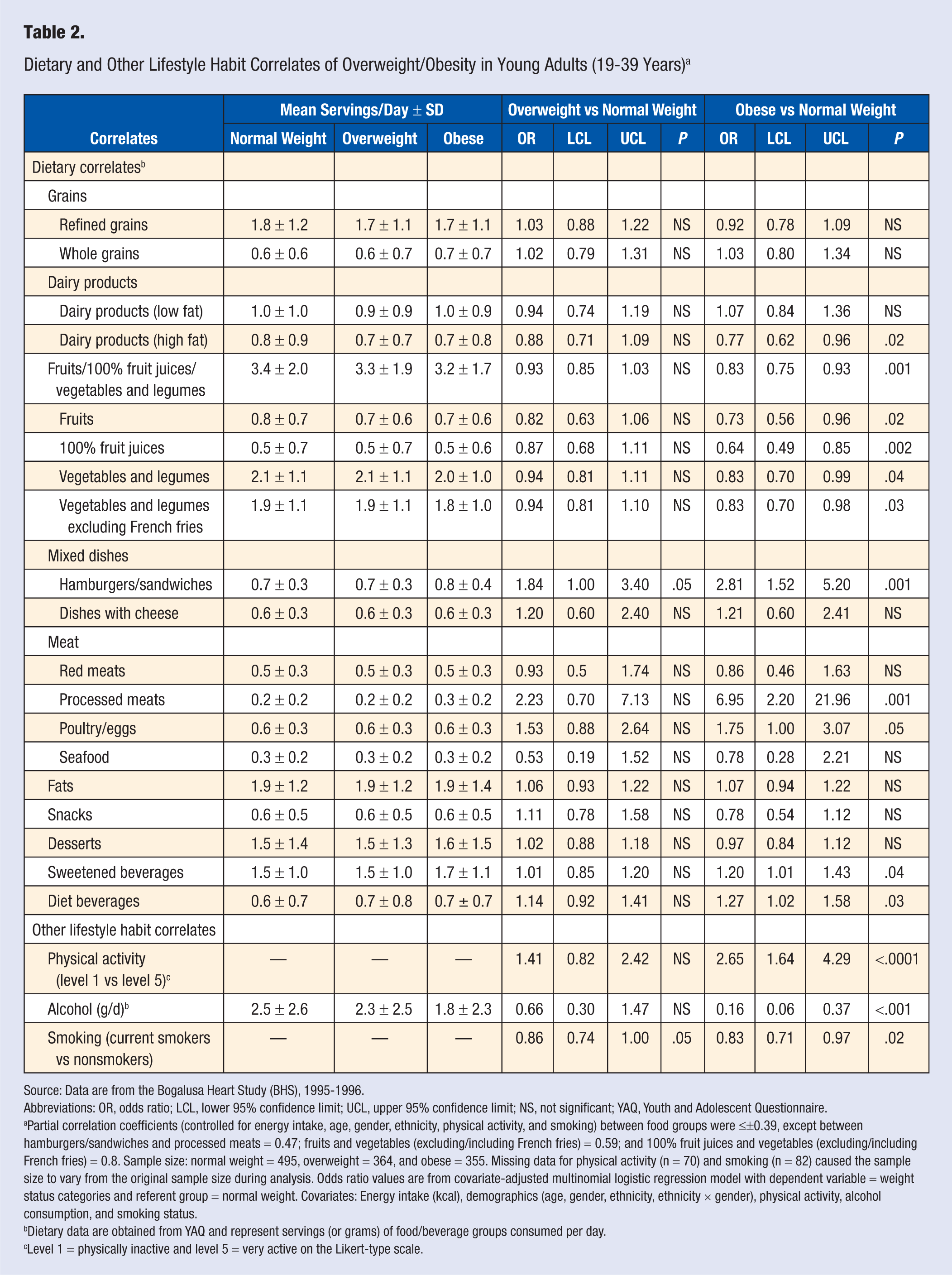
Source: Data are from the Bogalusa Heart Study (BHS), 1995-1996.
Abbreviations: OR, odds ratio; LCL, lower 95% confidence limit; UCL, upper 95% confidence limit; NS, not significant; YAQ, Youth and Adolescent Questionnaire.
Partial correlation coefficients (controlled for energy intake, age, gender, ethnicity, physical activity, and smoking) between food groups were ≤±0.39, except between hamburgers/sandwiches and processed meats = 0.47; fruits and vegetables (excluding/including French fries) = 0.59; and 100% fruit juices and vegetables (excluding/including French fries) = 0.8. Sample size: normal weight = 495, overweight = 364, and obese = 355. Missing data for physical activity (n = 70) and smoking (n = 82) caused the sample size to vary from the original sample size during analysis. Odds ratio values are from covariate-adjusted multinomial logistic regression model with dependent variable = weight status categories and referent group = normal weight. Covariates: Energy intake (kcal), demographics (age, gender, ethnicity, ethnicity × gender), physical activity, alcohol consumption, and smoking status.
Dietary data are obtained from YAQ and represent servings (or grams) of food/beverage groups consumed per day.
Level 1 = physically inactive and level 5 = very active on the Likert-type scale.
Other lifestyle habit correlates, that is, physical activity, alcohol consumption, and smoking together explained approximately 3% and 8% of the variance in the occurrence of overweight and obesity, respectively (Figure 1). Relative to normal weight, obese young adults had 2.7 times higher odds of being physically inactive (level 1) versus being very active (level 5; P < .0001). Relative to normal weight, obese young adults had 84% lower odds of consuming alcohol (P < .001). Relative to normal weight obese young adults had 17% lower odds (P = .02) of being smokers versus being nonsmokers (Table 2).
Occurrence of Risk Markers for CVD/T2DM by Weight Status
After adjusting for covariates, the mean values for serum total cholesterol, low-density lipoprotein cholesterol (LDL-C), triglycerides, Apo-B, Apo B: Apo A ratio, plasma glucose and insulin, and insulin resistance were all higher in overweight and obese than in normal weight young adults (P < .05), and the values increased with increased weight status (linear trend P < .0001, for all; Table 3). Mean values for serum high-density lipoprotein cholesterol (HDL-C) levels and insulin sensitivity were lower in overweight and obese than in normal weight young adults (P < .05), and the values decreased with increased weight status (linear trend P < .0001, for both). The mean value of serum Apo-A was lower (P < .05) in overweight and obese than in normal weight young adults. Mean values for systolic and diastolic blood pressure were higher (P < .05) in obese than in normal weight and overweight young adults (Table 3).
Cardiovascular Disease and Type 2 Diabetes Mellitus Risk Markers by Weight Status in Young Adults (19-39 Years) a
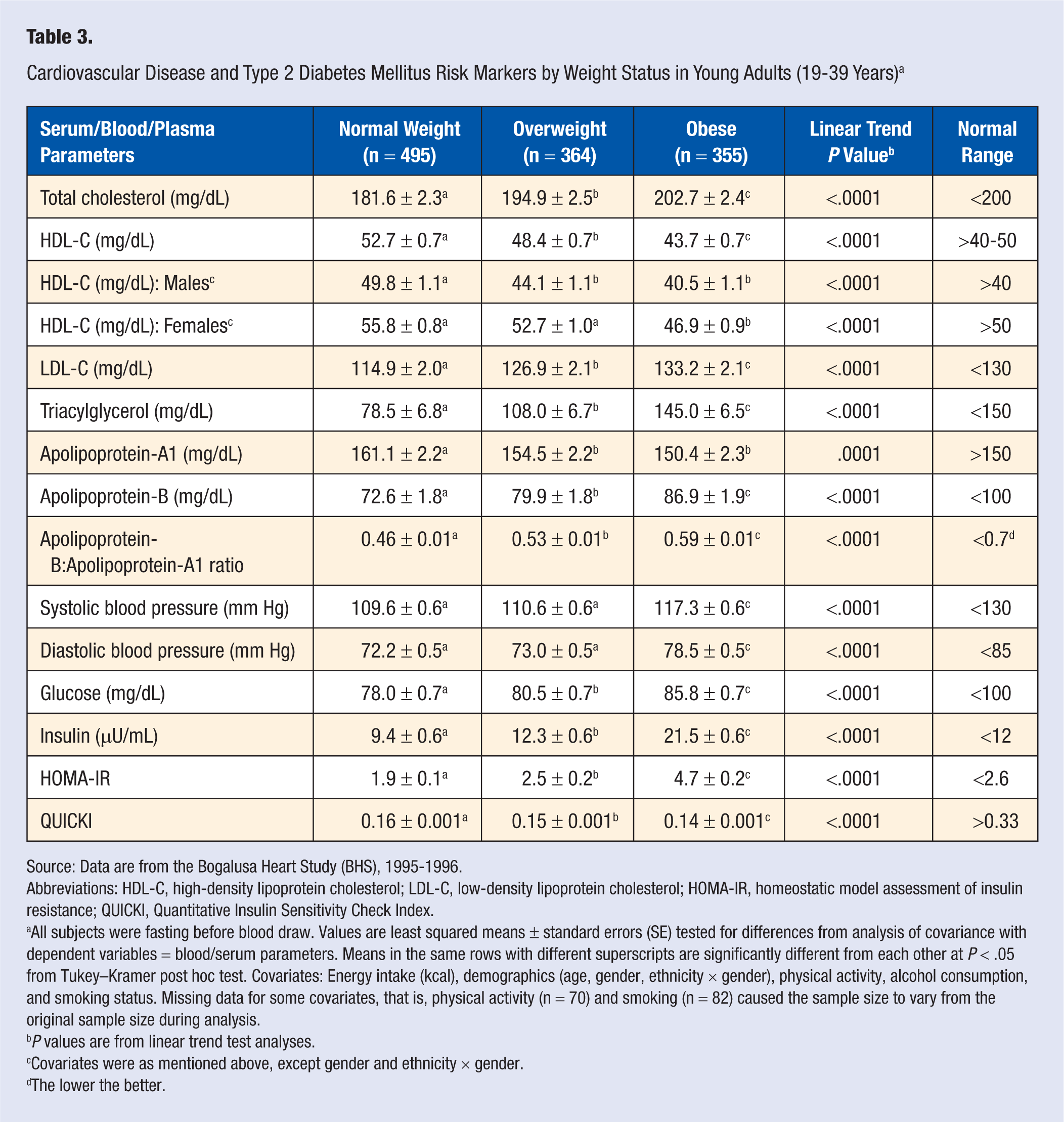
Source: Data are from the Bogalusa Heart Study (BHS), 1995-1996.
Abbreviations: HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; HOMA-IR, homeostatic model assessment of insulin resistance; QUICKI, Quantitative Insulin Sensitivity Check Index.
All subjects were fasting before blood draw. Values are least squared means ± standard errors (SE) tested for differences from analysis of covariance with dependent variables = blood/serum parameters. Means in the same rows with different superscripts are significantly different from each other at P < .05 from Tukey–Kramer post hoc test. Covariates: Energy intake (kcal), demographics (age, gender, ethnicity × gender), physical activity, alcohol consumption, and smoking status. Missing data for some covariates, that is, physical activity (n = 70) and smoking (n = 82) caused the sample size to vary from the original sample size during analysis.
P values are from linear trend test analyses.
Covariates were as mentioned above, except gender and ethnicity × gender.
The lower the better.
Trends between Self-reported Health Problems and Weight Status
The percentage of young adults self-reporting health problems increased with higher weight status specifically, high blood pressure (P < .0001), liver/gall bladder disease (P < .001), heart trouble in family (P < .01), pains in chest (P < .01), difficulty in breathing (P < .0001), shortness of breath (P < .0001), swollen ankles (P < .0001), and frequent leg cramps (P < .01; Figure 2).
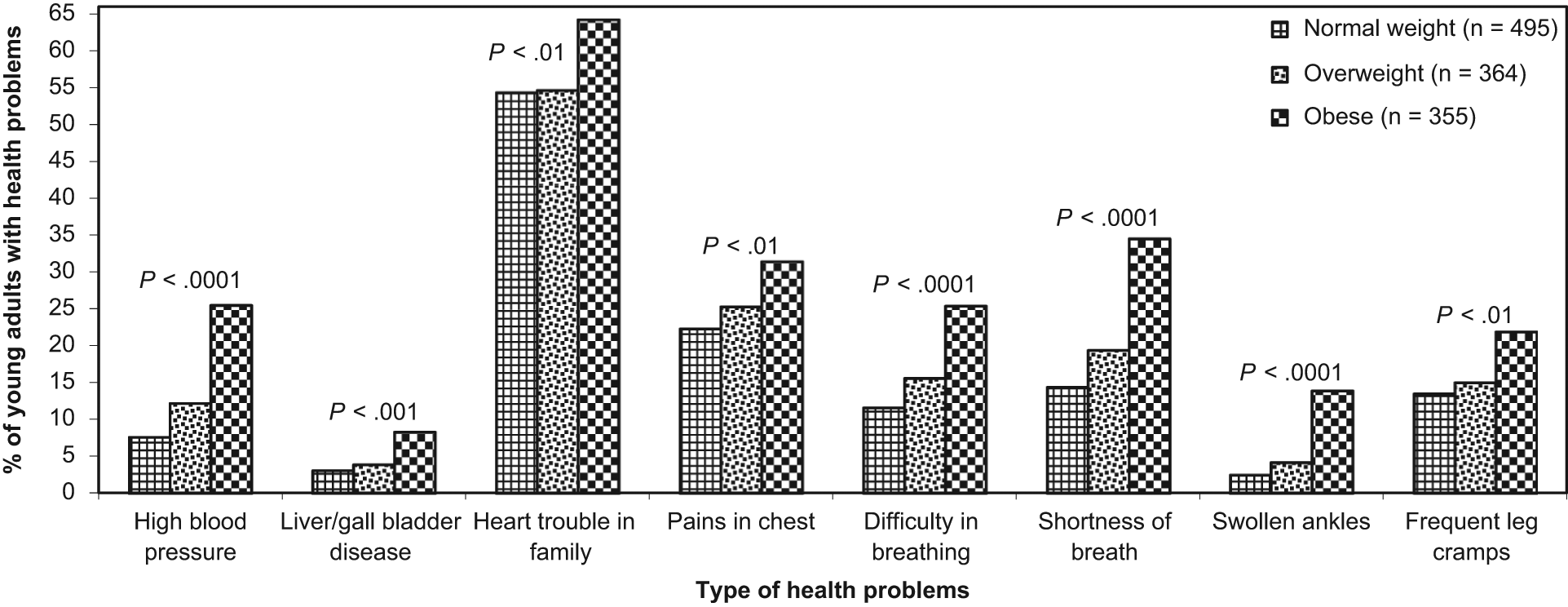
Trends Between Self-reported Health Problems and Weight Status in Young Adults From the Bogalusa Heart Study.
Discussion
The present analyses of BHS data provided insight on dietary and other lifestyle habit correlates of overweight/obesity in young adults. Significant positive associations were found between consumption of hamburgers/ sandwiches, processed meats, and sweetened and diet beverages with obesity; and significant negative associations were found between consumption of high-fat dairy products, fruit, 100% fruit juices, and vegetables with obesity. When comparing weight categories, positive linear trends were seen for all measures of CVD and T2DM, including serum lipid levels, systolic and diastolic blood pressure, glucose, and insulin levels.
Previous studies have shown that frequent consumption of fast foods 12 or high energy-dense diets,39,40 especially those with large portion sizes, 41 are associated with increases in energy intake,40,41 weight gain,12,39,40 insulin resistance, 12 or MetS. 40 Low consumption of dairy foods 16 and fruit/vegetables 39 has been linked with overweight/obesity. Higher intakes of fruit/vegetables may help with weight maintenance 42 ; however, the strength of this relationship in adults may not be strong. 43
Consumption of sweetened beverages has been associated previously with increased weight gain in females 44 and with obesity in the present study; however, a recent review failed to confirm that high-fructose corn syrup, the principal sweetener of many sweetened beverages, was associated with obesity to a degree higher than other energy sources. 45 More research is needed in this area. The present study also found a positive association of diet beverage consumption with obesity. Overweight/obese individuals may consume diet beverages as a weight loss strategy. 46
Consumption of whole grain, total fat, snacks, and sweets/desserts was not associated with overweight/obesity in this study. Previous studies have suggested that consumption of whole grains was negatively associated with BMI. 47 Consumption of energy-dense foods and snacks (with large portion sizes), 14 sweets, 48 and high-fat/low fruit/vegetable diets 39 may also contribute to high BMI or obesity; however, others have shown that the prevalence of overweight/ obesity decreases with increased snacking frequency and with increased percentage of energy from snacks, at least in adolescents. 49
In the present study, more food groups were associated with obesity than with overweight suggesting that diet was not a sensitive correlate of being overweight compared with being obese in this population. Dietary patterns of overweight individuals may be different from those of the obese and the association(s) with foods may be difficult to detect, especially with a food frequency questionnaire. Overall, consumption of specific food groups explained little variance.
The positive association of physical inactivity with obesity was expected. Being highly physically active or doing high levels of exercise with a suitable dietary regimen may result in a significant weight loss and its maintenance. 50 Yet it is difficult for some to maintain high levels of physical activity for long periods of time. 50 Individuals with high BMIs, especially those with comorbidities may have a decreased capacity to exercise. 51 Efforts to increase long-term physical activity through planned exercises and daily lifestyle physical activity modifications may benefit obese young adults.
Alcohol consumption was negatively associated with obesity in this study. Inconsistent findings have been reported by others when examining this relationship.19,52,53 Alcohol contributes energy to the diet; however, consumption may lead to “inefficient” energy utilization 54 and potentially to weight loss. Heavy drinkers may also modify their dietary habits with a resulting weight loss. 55 It is difficult to pinpoint the cause of the results seen in this study, since the consumption of alcohol was not considered heavy. Conversely, in a prospective study on younger US females, heavy drinking, but not moderate, was associated with weight gain (and in black females, even light drinking was associated with weight gain). 20 Alcoholic beverages contribute to the intake of discretionary calories, and recommendations regarding alcohol consumption need to take into consideration age, gender, and physiologic conditions.
Cigarette smoking was negatively associated with overweight/obesity in this study. Similar results were reported earlier. 56 These findings may be because of the several metabolic effects of nicotine from cigarettes leading to inefficient energy storage among smokers. 57 Nicotine may also suppress appetite by enhancing post-meal satiety. 58 Cigarette smoking may be initiated because of weight concerns and the pressures to remain thin, especially among young females. 59
In this study, more than half (59.2%) of the young adults were overweight or obese, and there was an increased occurrence of risk markers for CVD/T2DM with increased weight. Besides the well-established CVD risk markers, for example, high serum total cholesterol or LDL-C, or low serum HDL-C; the mean serum levels of Apo-B and the Apo-B:Apo-A ratio were higher in overweight/obese young adults in this study. Apo-B is an important predictor for developing hypercholesterolemia within 5 years in healthy adults (35-65 years and >65 years). 60 Yet the mean levels for Apo B and Apo B:Apo A ratio in overweight and obese young adults were within the normal limits in this study. The mean values for serum total cholesterol, LDL-C, plasma insulin, and insulin resistance in obese young adults were above normal limits. The constellation of these risk markers among the BHS young adults may have important implications in the development of MetS, CVD, and T2DM. Previous BHS and CARDIA studies have shown similar results.61,62 These findings in young adults is concerning. Efforts to lower the prevalence of overweight/obesity among young adults are necessary.
The strengths of this well-studied population were its large biracial sample and that diet and other lifestyle correlates of overweight/obesity were examined. Rigorous standards of diverse measures of health habits and metabolic-related assays were adhered to. Furthermore, this study specifically examined food group intakes in relation to weight gain. Since individuals eat foods and not nutrients, understanding the role of food groups in relation to the occurrence of overweight/obesity is important.
The present study has some limitations. Because of its cross-sectional nature, causal links among dietary and other lifestyle habit correlates and the presence of overweight/obesity cannot be established. The age of BHS data is another limitation in interpreting the results. Furthermore, some results may have been confounded by the possibility of reverse causality. Dietary and other lifestyle habit correlates explained little variance in overweight/obesity; and many of the dietary associations were weak. The low variance explained by dietary factors in obesity could be because of some inherent inadequacies in the self-reported dietary assessment methods. For example, a food frequency questionnaire has a fixed list of foods and therefore may not capture all foods consumed by the subjects and the food intake responses depend on their memory. Individuals with higher than normal BMI tend to underreport food/energy intake, 63 thereby leading to biased results. In addition, food frequency questionnaires may underestimate intake of total energy,64,65 and energy adjustment is used to reduce the effects of measurement error, that is, regression dilution.66,67 Blacks and males were underrepresented in this research. Finally, the present findings may be specific to young adults of Bogalusa, Louisiana, and not representative of national populations.
In conclusion, dietary and other lifestyle habits were associated with weight status. In particular, obese young adults had poor dietary and physical activity habits. In addition, higher weight status was associated with adverse biochemical risk markers for CVD and T2DM and greater reported health problems, especially among obese young adults. These findings warrant clinical and public health interventions catered to improving dietary and physical activity habits among the obese young adults.
Footnotes
Appendix
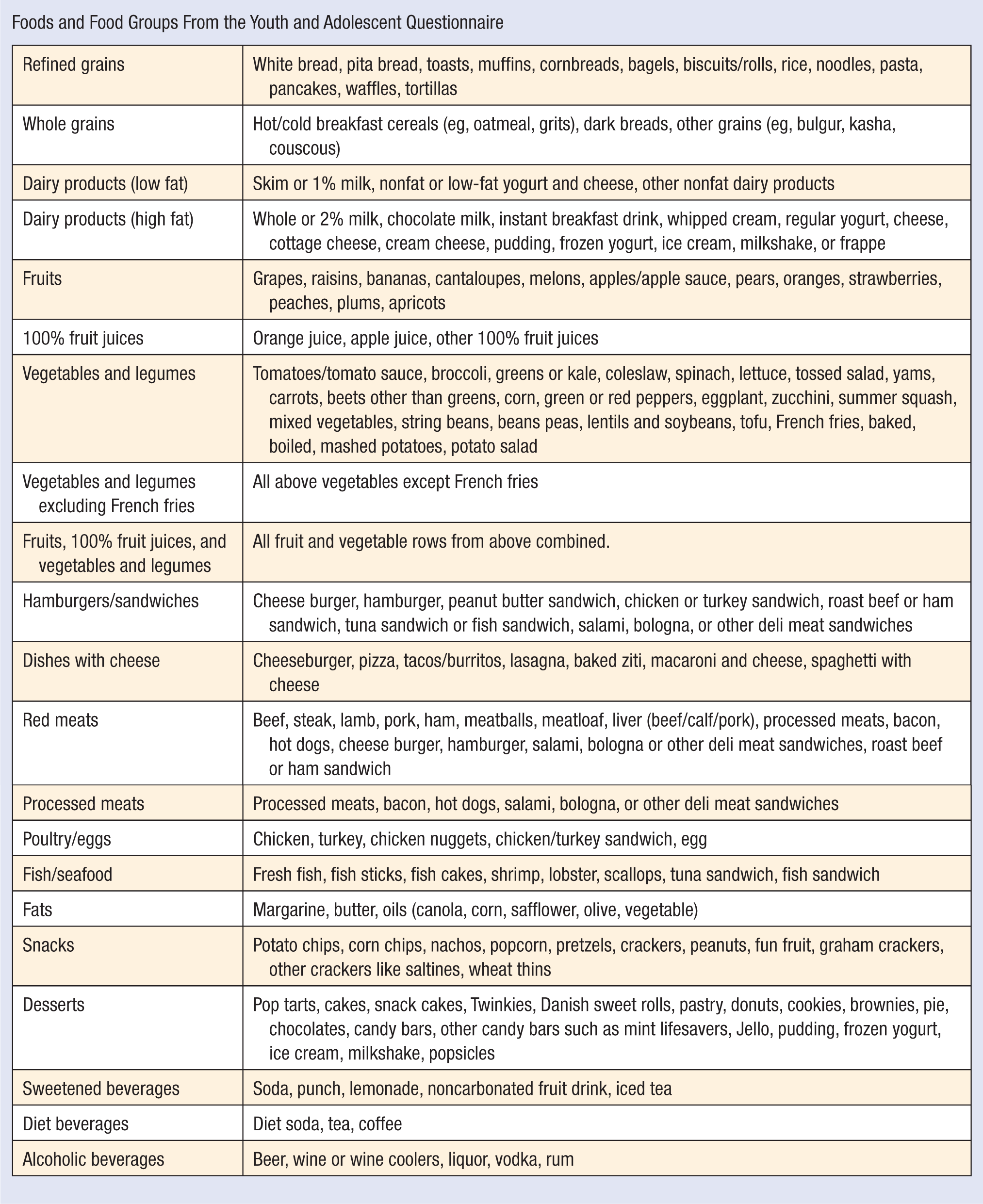
Foods and Food Groups From the Youth and Adolescent Questionnaire
| Refined grains | White bread, pita bread, toasts, muffins, cornbreads, bagels, biscuits/rolls, rice, noodles, pasta, pancakes, waffles, tortillas |
| Whole grains | Hot/cold breakfast cereals (eg, oatmeal, grits), dark breads, other grains (eg, bulgur, kasha, couscous) |
| Dairy products (low fat) | Skim or 1% milk, nonfat or low-fat yogurt and cheese, other nonfat dairy products |
| Dairy products (high fat) | Whole or 2% milk, chocolate milk, instant breakfast drink, whipped cream, regular yogurt, cheese, cottage cheese, cream cheese, pudding, frozen yogurt, ice cream, milkshake, or frappe |
| Fruits | Grapes, raisins, bananas, cantaloupes, melons, apples/apple sauce, pears, oranges, strawberries, peaches, plums, apricots |
| 100% fruit juices | Orange juice, apple juice, other 100% fruit juices |
| Vegetables and legumes | Tomatoes/tomato sauce, broccoli, greens or kale, coleslaw, spinach, lettuce, tossed salad, yams, carrots, beets other than greens, corn, green or red peppers, eggplant, zucchini, summer squash, mixed vegetables, string beans, beans peas, lentils and soybeans, tofu, French fries, baked, boiled, mashed potatoes, potato salad |
| Vegetables and legumes excluding French fries | All above vegetables except French fries |
| Fruits, 100% fruit juices, and vegetables and legumes | All fruit and vegetable rows from above combined. |
| Hamburgers/sandwiches | Cheese burger, hamburger, peanut butter sandwich, chicken or turkey sandwich, roast beef or ham sandwich, tuna sandwich or fish sandwich, salami, bologna, or other deli meat sandwiches |
| Dishes with cheese | Cheeseburger, pizza, tacos/burritos, lasagna, baked ziti, macaroni and cheese, spaghetti with cheese |
| Red meats | Beef, steak, lamb, pork, ham, meatballs, meatloaf, liver (beef/calf/pork), processed meats, bacon, hot dogs, cheese burger, hamburger, salami, bologna or other deli meat sandwiches, roast beef or ham sandwich |
| Processed meats | Processed meats, bacon, hot dogs, salami, bologna, or other deli meat sandwiches |
| Poultry/eggs | Chicken, turkey, chicken nuggets, chicken/turkey sandwich, egg |
| Fish/seafood | Fresh fish, fish sticks, fish cakes, shrimp, lobster, scallops, tuna sandwich, fish sandwich |
| Fats | Margarine, butter, oils (canola, corn, safflower, olive, vegetable) |
| Snacks | Potato chips, corn chips, nachos, popcorn, pretzels, crackers, peanuts, fun fruit, graham crackers, other crackers like saltines, wheat thins |
| Desserts | Pop tarts, cakes, snack cakes, Twinkies, Danish sweet rolls, pastry, donuts, cookies, brownies, pie, chocolates, candy bars, other candy bars such as mint lifesavers, Jello, pudding, frozen yogurt, ice cream, milkshake, popsicles |
| Sweetened beverages | Soda, punch, lemonade, noncarbonated fruit drink, iced tea |
| Diet beverages | Diet soda, tea, coffee |
| Alcoholic beverages | Beer, wine or wine coolers, liquor, vodka, rum |
Acknowledgements
This research was supported by grants from the National Heart, Lung, and Blood Institute of the US Public Health Service (USPHS), Early Natural History of Arteriosclerosis R01 HL 38844, National Institute of Aging AG16592, and the United States Department of Agriculture, Economic Research Service Cooperative Agreement No. 43-3AEM-0-80071. Partial funding was received from the USDA HATCH project LAB 93951.
This work is a publication of the United States Department of Agriculture (USDA/ARS) Children’s Nutrition Research Center, Department of Pediatrics, Baylor College of Medicine, and Houston, Texas. The contents of this publication do not necessarily reflect the views or policies of the USDA, nor does mention of trade names, commercial products, or organizations imply endorsement from the US government.
The Bogalusa Heart Study represents the collaborative efforts of many people whose cooperation is gratefully acknowledged. We thank the children and young adults of Bogalusa without whom this study would not have been possible. The authors also wish to thank Ms Nisha Mohindra for her help in the initial data management for the manuscript and Michael Zanovec for assistance in formatting and submitting the manuscript.
