Abstract
This article focuses on how health practitioners can better understand and intervene with gay men. Gay men’s health is situated within 3 prominent theoretical models (ie, minority stress, gender socialization, and identity development) and associated with 3 constructs (ie, internalized homonegativity, internalized homophobia, and internalized heterosexism) to contextualize gay men’s health concerns. Throughout the article, the authors draw particular attention to research that emphasizes the strengths of gay men, as this is a notable gap in the extant literature. Furthermore, HIV/AIDS is a central concern of gay men, and this article focuses on how cultural identities and factors may intersect with HIV/AIDS status among gay men and have implications for health decision making. Affirmative clinical interventions based on theory and research are presented throughout the article, which can be applied by health professionals in various settings. Given the confusion around terminology, lack of knowledge of available resources, and prevailing negative societal myths about gay men, the article provides a glossary of definitions for unclear terms, actively disputes myths that are not empirically supported, and provides a list of available resources.
Health practitioners are encouraged to help their gay clients discern and select what strategy may be most useful to them in the context of their environment, identity development, and available supports.
The extant literature on gay men’s health is large, covering many topics (eg, depression, HIV/AIDs) by several health disciplines (eg, nursing, medicine, counseling psychology). As we reviewed the known findings, a body of scholarship emerged that detailed the limitations of research involving gay men. The noted limitations have the potential to bias how practitioners interpret and apply research with their gay clients. As a result, we felt compelled to incorporate a critique of the extant literature as part of our review. We understand that the targeted audience of this journal is not researchers per se, but practitioners. Therefore, we do not intend to make statistical or research methodological critiques the basis of our review. Health practitioners are likely to benefit from this brief critique by becoming more aware of the research limitations and basing their practice with gay men on a fuller understanding of the literature.
Research Critique
Much of the current health research is based on a deficit model or a focus on diseases of gay men. 1 Indeed, we found that a collated body of research indicated that gay men are at an increased risk for self-harm, suicide ideation, eating disorders, legal and illegal substance abuse, tobacco use, panic attacks, depressive symptoms, and underutilization of health care services.2-11 A lack of research on the strengths of gay men and positive health outcomes compounds the focus on deficits.
Another potential bias is that research has often benchmarked gay men’s health outcomes comparatively to heterosexual men, which interprets the experience of a sexual minority population within the sexual majority’s worldview. 12 Such an approach emphasizes the idea that being heterosexual is normal and being gay is abnormal. Stigma associated with being gay may prevent disclosure on a research questionnaire. Therefore, benchmarks of gay men’s population do not exist, which limits generalizability based on a representative sample. 13
Phillips 14 adds that multiple identities are often overlooked, resulting in a simple presentation of sexual orientation and minimizing the complex cultural variations of gay men. Sexual orientation is almost impossible to operationalize because self-labeling techniques do not capture the complexity of identity intersection, there is a lack of a widespread/accepted measure of sexual orientation, and some LGB (lesbian, gay, bisexual) individuals have difficulty defining themselves within preexisting categories.13,15
As a result, defining the study’s sexual minority population of focus is critical as is clarity of terms used. For this study, we used literature based on the searchable terms “gay men” and “men who have sex with men” (MWSM). Although some studies consolidate different LGBT (lesbian, gay, bisexual, transgender) groups into their sample because of overlapping issues, we excluded studies that focused on bisexual men and transgendered individuals because we considered those populations distinct from gay men and MWSM since same-sex behavior does not necessarily equate with homosexual sexual orientation identification. 13 Gay men refer to individuals with the physical and biological makeup of a male who are attracted to other men and identify as a sexual minority (Table 1). MWSM is a behaviorally based definition of men who engage in sexual acts with other men but do not necessarily identify as a sexual minority (Table 1). As noted, Table 1 is a glossary of commonly confused terms in the gay men’s literature. Knowing and understanding cultural terminology and language is important for practitioners to be culturally sensitive with gay clients.
Glossary of Terms
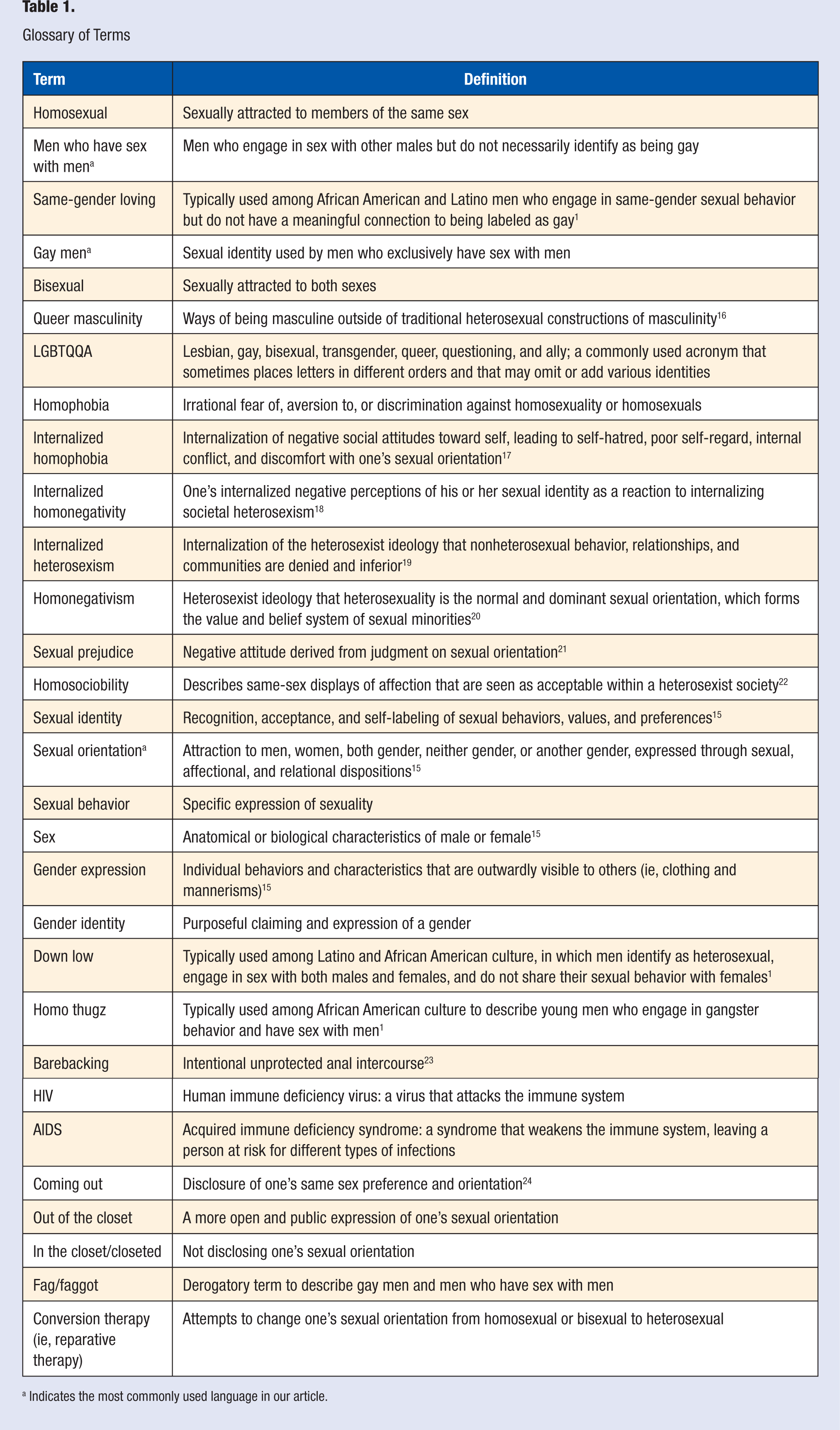
Indicates the most commonly used language in our article.
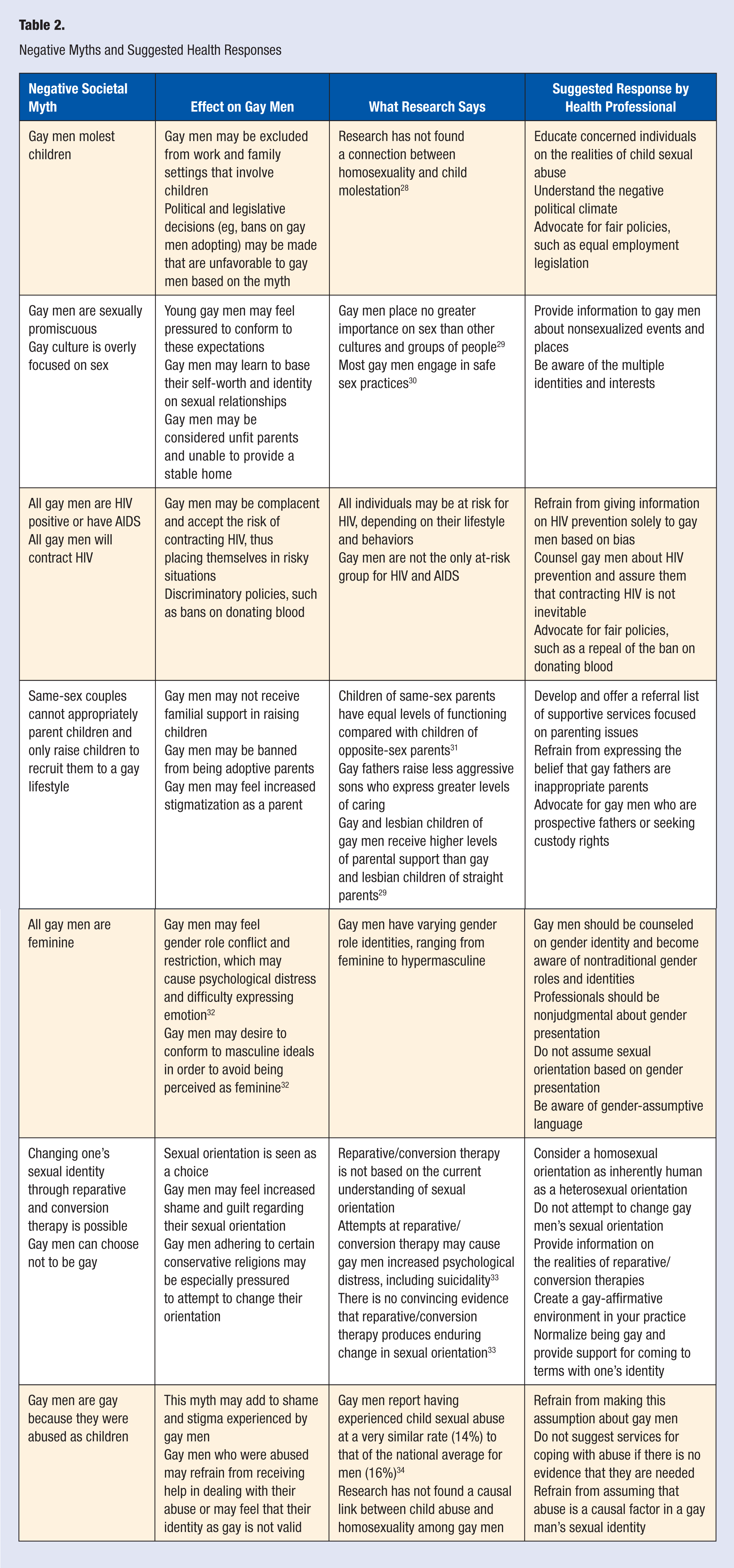
In response to these limitations, a primary aim of this literature review is to contextualize gay men’s health concerns and issues within prevailing theories and constructs familiar to sexual minority groups and culture. Understanding the sociocultural factors involved in gay men’s health and debunking negative stereotypes (Table 2) may help clinicians be more affirmative toward gay men, make more accurate diagnoses, and treat gay men with more clinical compassion.25,26 Another aim of this literature review is to detail the health benefits and strengths of gay men to facilitate the construction of a fuller picture of gay men’s health. We also seek to better understand the interaction between multiple identities (eg, ethnicity, age, spirituality) and HIV status for gay men. Since the health of gay men is situated within a hostile, systemic context, we demystify various societal myths about gay men (Table 2) and discuss ways for health practitioners to engage in systemic interventions. 27
Negative Myths and Suggested Health Responses
Contextualizing Gay Men’s Health
We discuss minority stress, gender socialization, and identity development theories as well as the overlapping constructs of internalized homonegativity, internalized homophobia, and internalized heterosexism to contextualize gay men’s health.
Minority Stress Model
Unfortunately, stigmatization, discrimination, and oppression of gay men is still prevalent in the United States; examples include negative societal myths (Table 2) about gay men as child molesters, verbal abuse, threats, hate crimes, and public policies that closet the mere identification as a sexual minority. The minority stress model posits that gay men are members of a minority group in the United States and experience chronic stress as a result of the discrimination, which leads to adverse health outcomes.11,35-37 The minority stress model has been correlated with suicidality, depression, workplace problems, alcohol and substance abuse, body image dissatisfaction, eating disorders, and risky sexual behavior in samples of gay men.37-42
Although considerably less studied than stress, the impact of one’s resilience and use of coping strategies to buffer against stress and maintain health is an emergent counter-process within the minority stress model.11,36 David and Knight 43 argue that coping is a potential mediator between stress and negative health outcomes. Stigma competence, defined as the ability to cope with stigma, is a coping skill for gay men that helps approach and overcome the unique challenges associated with being a sexual minority. 43 Chenard 44 describes 3 stigma management strategies: (a) selective disclosure, which refers to a gay man’s incremental disclosure of sexual identity over time to a select group of trusted allies; (b) preemptive or open disclosure, which refers to a gay man’s proactive disclosure of sexual identity; and (c) reactive disclosure, which entails a gay man hiding or concealing his sexual identity to protect himself against stigma. In addition to stigma competence, crisis compe-tence is a strength that is derived from responding to difficulties, which gay men can use in various stressful situations. Research has yet to conclude which strategy is most effective or correlated with positive health outcomes. Health practitioners are encouraged to help their gay clients discern and select what strategy may be most useful to them in the context of their environment, identity development, and available supports.
In addition to stress from societal discrimination, gay men with HIV/AIDS may experience additional stress from the illness. Increased stress has been found to decrease the effectiveness of HIV medication, decrease T-cell counts, increase the speed at which the virus replicates, and trigger the onset of HIV symptoms.45,46 Therefore, interventions that reduce stress can actually slow the progression and decrease the severity of HIV symptoms. 45 For example, Weiss et al 47 found that simply providing educational materials to HIV-positive gay men is an efficient way to improve gay men’s psychosocial well-being and coping.
An unfortunate stressor for some HIV-positive gay men is the experience of loss and bereavement as individuals in their social networks die from an AIDS-related death.45,48,49 HIV-positive gay men encounter unique stressors to their grieving, such as coping with the real possibility that they will also die from the same illness and feelings of anger or guilt if the deceased individual infected the bereaved individual or was infected by the bereaved individual.49,50 Gay men have reported that many health services do not address grief and loss issues. 49 Therefore, health providers should make sure to discuss the possibility of AIDS-related bereavement with their gay, HIV-positive clients and incorporate relevant services into their treatment plan. For example, gay men may benefit from a group intervention that focuses on emotional expression, group cohesion, and accessing social support to deal with bereavement. 51 Health practitioners can work with HIV-positive gay men to access and use their strengths of independence and positive coping strategies that may have been used to deal with similar experiences of loss when faced with HIV-related bereavement.
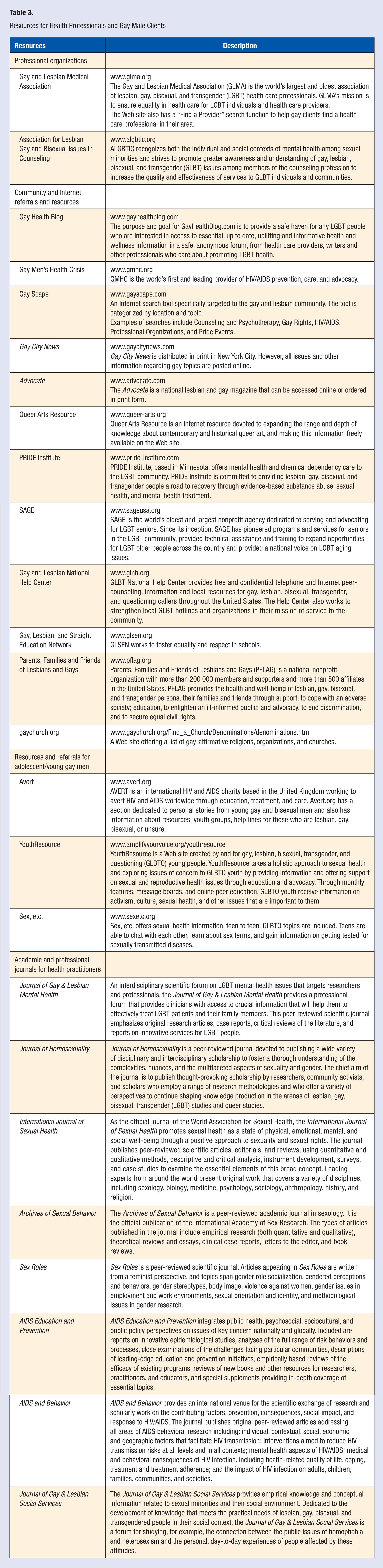
In a related line of research, gay men are at an increased risk to have lost social and family support through the coming-out process and therefore are likely to develop necessary networking strategies and skills to enhance social supports. 22 In addition to personal coping skills, social support may also represent a mediator between stress and negative health outcomes for gay men. 45 For gay men who report a lack of support from family or peers, health practitioners can offer referrals to community organizations and groups such as gay-friendly therapy groups, support groups, and religious organizations (Table 3). HIV-positive gay men, often strained from family support and stigmatized by society, have noted that social support from other HIV-positive gay men was integral to their self-care and helped to buffer them from stress and to feel safer.44,48,50 Ideally, practitioners would be involved in local, regional, or national gay communities and therefore, know of resources for gay men. If a practitioner lacks such experience, Table 3 provides a list of available supports for gay clients. Health practitioners can help gay men identify both the positive and negative supports in their lives, suggest the appropriate source of support to access, and provide necessary referrals.
Resources for Health Professionals and Gay Male Clients
Internalized Homonegativity, Homophobia, and Heterosexism
Internalized homonegativity, internalized homophobia, and internalized heterosexism are 3 overlapping, yet distinct, constructs in the literature (see Table 1 for clarification). The basic premise of each construct is that an individual of sexual minority status applies negative messages from society about sexual orientation to the self. 15 To convey the literature appropriately, we will use the terminology used in each particular study within our review.
Internalized homonegativity is described as the internalizing negative “reaction to stigma associated with being homosexual” by individuals who identify as a sexual minority. 52 Frost and Meyer 27 described stress as processing along a continuum of proximity to the self, with distal stressors based in the environment (eg, antigay stereotypes) and the most proximal stress of internalizing heterosexist social attitudes (ie, internalized homonegativity). Internalized homonegativity with samples of gay men has been found to be associated with depression, relationship difficulties, and unprotected anal intercourse.18,27,37 Internalized homonegativity has also been found to lead to an increase in mood disorders and substance abuse, which ultimately may increase the risk of HIV infection and lead to poorer response to HIV treatment. 53
Internalized homophobia is the internalizing of an irrational fear of homosexuality. 18 Internalized homophobia has been found to induce emotions of shame, guilt, and fear of one’s sexual orientation as well as risky behaviors (eg, suicide and self-harm). 54 Sexual minorities have been found to cope with internalized homophobia using 3 strategies: (a) Routinization and minimizing of homophobia, in which acts of discrimination are expected and viewed as normal. This strategy reduces the intense victimization that can accompany homophobia, and minimizes the severity of the impact of the dominant heterosexist view. (b) Maintaining individual “adult” responsibility, which is described as developing the skills necessary to emotionally and physically cope with homophobia, and developing the capacity to manage stigma. (c) Constructing “proud” identities, which can be explored in many different realms such as mature conversations, sexual exploration, and taking responsibility for actions and decisions. Positive and open conversations with adults about sexuality can reinforce a positive identity and self-acceptance for gay men, thus negating the influences of homophobia. 54
Internalized heterosexism is the internalization of the overt and covert societal stance that sexual minorities are inferior to heterosexuals. 19 Internalized heterosexism has been linked to risky sexual practices and low compliance with HIV medications. 53 Although results are mixed, a moderate positive correlation is prevalent between internalized heterosexism and alcohol and substance abuse with gay men.55-57 Mediating variables, such as disclosure of sexual identity, anxiety, depression, and self-acceptance can influence internalized heterosexism’s effect on substance use. 55
The associations between internalized homonegativity, homophobia, and heterosexism and adverse health outcomes and risks present a difficult challenge to health practitioners to understand internal processes that may not be explicitly manifested. We suggest that health practitioners respect the individual differences among gay men and be open to hearing personal experiences and learning their unique stories as well as investigating emergent literature about current gay culture. Furthermore, understanding the client’s experience of heterosexist beliefs and its impact on social relationships can help identify areas that need support. 55 Encouraging the gay client to inform his social network of the impact of heterosexism may help reduce these harmful perceptions and ultimately enhance support networks. When encouragement is insufficient, assertiveness training may help gay clients develop the necessary skills to initiate difficult conversations with people in their social network.
Gender Socialization Theory
Gender socialization theory contends that masculinity is a construct that is constantly negotiated within physical, psychological, and social interactions that include modeling, reinforcement, and punishment.58,59 In the United States, men typically experience pressure to conform to norms of being independent, fearless, tough, invulnerable, self-reliant, stoic, and nonfeminine.60,61 Research has indicated that men may be more likely to engage in negative health behaviors because of the gender socialization process, which discourages self-care and help-seeking while encouraging risky behavior. 62
Indeed, masculinity construction is difficult to negotiate for some gay men. A prevailing antigay stereotype is that all gay men are overly feminine (Table 2). However, expression of masculinity is quite variable among gay men and is often in direct reaction to the feminine stereotype. 32 Research with gay men has found that those who placed more value on traditional norms of masculinity expressed negative feelings about being gay. 63 Nonconformity to traditional masculine norms has led to paternal, maternal, and peer rejection during the childhood of gay men. 64 For gay men, masculinity construction and conflict has been linked to substance use, steroid use, risky sexual behavior, dissatisfaction if their body does not meet the physically powerful masculine ideal, anger, anxiety, and depression.65-68
Health practitioners can intervene by asking their gay clients what effect masculine ideals and gender role socialization have on their presenting concerns and stress during the initial assessment process. 32 For example, traditional gender socialization has been linked to gay men having difficulty being in relationships with other men; a cost–benefit analysis of traditional masculinity’s effect on relationships has been identified as an appropriate intervention in these instances. 69 Health practitioners could begin the conversation by asking, “Do masculine ideals contribute to stress for you or in your relationships?” Many of the basic concerns (eg, emotional restriction, family conflict, relationship difficulties) related to gender role conflict and masculine socialization are found in both gay and nongay men; health practitioners are urged to acknowledge those similarities with gay men. 68
Identity Development Theories
Several stage models exist in the literature that detail the identity development process of gay individuals.70-73 As summarized by Hill, 74 important themes are seen in each model: (a) awareness of difference prior to exploring sexuality, (b) initial exploration of sexuality and tentative self-identification, (c) feelings of separation from heterosexual others, (d) feelings of connection with homosexual others, (e) deepening connection with homosexual others, (f) awareness of and response to oppression, and (g) sense of sexuality as one part of a complex identity and increased skill interacting with both heterosexual and homosexual others. 74
The stage, timing, and pattern of identity development have implications for gay men’s health. Friedman et al 75 created 3 categories based on the pattern and timing of identity development for gay men: early developing (experiencing same sex attraction by 3rd grade, coming out by 12th grade), middle developing (experiencing same-sex attraction by sixth grade and coming out by 21 years old), and late developing (experiencing same-sex attraction by eighth grade and coming out by 28 years old). HIV status, gay-related victimization, and depression were associated with the early developing category. Victimization during the coming-out process may be of importance beyond the individual trauma for those who come out at a young age, as gay-related harassment experienced prior to age 17 years predicted 189% greater odds of experiencing gay-related victimization in adulthood. 75
“Coming out,” which refers to individuals disclosing their sexual orientation to others and establishing a public identity as a gay individual, is a significant process in the identity development of gay men (Table 1). 76 Coming out may best be understood as a continuous social process rather than as a single disclosure. 77 Many scholars consider coming out to be a long, complex, difficult, stressful, anxiety-provoking, and complicated process for gay men. Challenges and risks associated with the coming-out process among gay men might include more sexual risk behaviors, internalized homophobia, stigmatization, and disturbances to social relationships.56,78 Other scholars contend that a current climate of openness and available supports may make coming out less daunting. 78 For example, gay adolescents are coming out an average of 10 years earlier than their counterparts from 30 years ago. 24
Riley 24 defined coming out as a 5-dimensional process, which entails involvement in gay activities, development of attitudes toward a gay identity, becoming comfortable with being gay, disclosing that one is gay to others, and identifying a specific sexual identity. Within the Riley 24 model, the dimension involving being comfortable with being gay correlated positively with self-esteem and negatively with anxiety and depression. The dimension involving participation in gay activities was positively correlated with the number of sexual encounters but negatively correlated with unsafe sex, indicating that participation in gay activities might lead to meeting more sexual partners but that individuals would be less likely to take sexual risks, perhaps because of social support from people at these events.
An exemplary study conducted by Riggle et al 79 explored the positive aspects of identity development in relation to disclosure of sexual identity and took a strength-based approach to understanding the characteristics of sexual minorities that develop due to their minority status. Coming out was seen as a critical step in the development of a positive identity, as it provided the opportunity to foster close relationships with other sexual minorities and generate a greater sense of self-awareness. Because of the very nature of disclosure, self-exploration forces gay men to be honest with who they are (and who they are not), which is integral to the emergence of an authentic self. With the continual presence of societal discrimination, participants described an ability to look within for self-acceptance rather than externally for reinforcement. This process of reflection and disclosure further promotes an authentic understanding of self, a strengthened identity, and an opportunity for gay men to become an affirmative role model for younger sexual minorities in the coming-out process.
Gay men have been theorized to have the capacity to successfully navigate and understand multiple cultures and identities, which contributes to an adaptable worldview. Such adaptability has roots in the coming out process, which fosters self-acceptance as well as acceptance of others, empathy, openness, tolerance, diversity, and compassion for others, specifically other minority populations.79,80
With the potential for families to react negatively to their child coming out, gay men often find a creative way to develop their own family. Additionally, some gay men have felt liberated from pressure to conform to restrictive gender roles and norms while considering the opportunity to form their own gendered identity to be a powerful experience. Gay men have expressed their sexual minority status as positive because it cultivated freedom both in terms of gender roles and expression, and the choice of one’s own family. 80
It is important for clinicians to know that developmental sequences vary greatly among individual gay men and that identity development is not a simple linear progression through stages. 81 Clinicians are cautioned to meet the client where he is in terms of identity development and disclosure to ensure that the client is not being pushed beyond his comfort. 55 Health care providers are at the front line to encourage the development of positive social supports in addition to providing a compassionate and safe health care environment. 82 Through medical education and multicultural training in gay issues, practitioners can become well-equipped to provide appropriate and supportive services to gay males from adolescence into adulthood. 83
Impact of Age
Age is an important factor in considering how coming out and identity development impact a gay male. Young adult and adolescent gay men tend to have different experiences, but research samples often combine the 2 populations, which makes it difficult to detail differences between the 2 groups. This section includes the use of the terms adolescents and young gay men, depending on the language used by each study.
As much of the literature indicates, gay adolescents are at a critical developmental stage, which can either promote well-being and self-acceptance or induce feelings of shame and guilt. 11 Higher levels of internalized heterosexism are found to be present in young gay men, which may help to further contextualize their increased risk in health concerns. 55 One of the challenges that adolescent gay males are likely to encounter when coming out is being raised by heterocentric families that do not know how to prepare them for or support them through the identity development process.24,84,85 Additionally, gay adolescent males who came out before age 18 years reported fewer peer contacts than heterosexual adolescent males their age. 86 Social support is a critical component to buffer gay adolescent males from anxiety and stress, so this lack of support from family and peers is detrimental to the well-being of gay adolescents.87,88 Young MWSM are more likely to have depressive symptoms, less likely to use mental health services, more likely to use illegal substances such as Ecstasy, and more likely to have unprotected anal sex than older MWSM, and closeted young gay men have a higher risk of contracting HIV and other STDs than young gay men who come out.86,89,90 Abusing substances was correlated with an increase in risk factors for having a positive HIV status in young MWSM, including greater odds of having multiple sexual partners and of having unprotected sex. 91
These factors may indicate a need to design and implement more comprehensive interventions for adolescent and young MWSM by focusing on mental health, stigma reduction, substance abuse, and safe sex practices, with the school being a natural setting for service delivery.90,91 Gay adolescents may benefit from parental involvement in HIV prevention programs in order to address communication skills and family dynamics. 92
Intersecting Identities With HIV/AIDS Status
For many gay men, sexual orientation composes only one part of their identity of many intersecting identities. HIV/AIDS status, age, ethnicity, and spiritual beliefs represent some examples of a complex web of interrelated identities that affect gay men’s health and well-being. Describing the intersections between all factors is beyond the scope of this article. We focused this section on the intersections listed above.
HIV/AIDS may be the most central and complex health issue facing some gay men, although the prevalence is not as high as stereotypes might suggest (Table 2). The centrality of HIV/AIDS to gay men’s health is highlighted in one study that found that HIV status mediated health differences between gay and heterosexual men and increased the likelihood of physical health complaints and mental health disorders. 4 In the United States, MWSM account for 48.1% of the estimated 1.1 million individuals who are HIV-positive and gay men are considered the only population in which the rate of new HIV infections is increasing.86,93
HIV/AIDS is not curable at this time but is managed with medications such as highly active antiretroviral therapy (HAART), which slow virus replication within the body. 94 Rerks-Ngarm et al 95 discovered the first vaccine demonstrating some effectiveness in preventing HIV infection, but the supporting data are not definitive. Patients are often reluctant to take antiretroviral treatment and/or are inconsistent with adhering to the regimen despite the survival benefits. 96 Many strategies have been employed and researched to address those treatment issues; we briefly highlight the intriguing role of spirituality. Research focused on spirituality and gay men with HIV/AIDS is scarce and inconsistent, but initial findings indicate that contracting HIV/AIDS is a life-changing event, moving individuals to feel more religious and spiritual.97,98 Health practitioners can tap into specific religious and spiritual beliefs that motivate HIV-positive gay men to take antiretroviral medications and adhere to the treatment. 99 Yet health practitioners are urged to carefully approach conversations about religion and spirituality with gay men as sexual minorities often have had hostile, conflictual, and discriminatory experiences with their religious community. 100
Although medications and vaccines may offer some benefit and may improve in efficacy in the future, we contend that current HIV management must focus on preventative efforts that consider the intersecting identities while targeting risky behavior and improving sexual health decision making among gay men.
Culture and Ethnicity: Latino, African, Asian, and Native American Gay Men
Understanding the culture of African Americans, Native Americans, Asian Americans, and Hispanics and Latinos has been highlighted as central to offering competent interventions to historically stigmatized groups in American society. 101 Variations and differences exist within and across these subgroups of gay men; however, research indicates that those 4 groups may uniquely experience double and triple minority status as a gay man, an ethnic minority, and an individual positive for HIV/AIDS.102,103 The result of the multiplied minority status could be additive stress, which reinforces the call for tailored interventions for ethnic minority gay men. 104
Many Native/Indian American cultures maintain a unique and more accepting set of beliefs related to homosexuality, which is manifested in individuals of “two-spirit,” that is, a male and a female spirit. 105 When working with two-spirited Native American men, health practitioners are encouraged to explore the role of alcohol as a coping mechanism, emphasize the spiritual nature of the man’s identity over the sexual nature, avoid stereotyping all characterizations of gay men as two-spirited, and carefully explore the family’s role relative to the client’s coming out. 106 Latino, African American, and many Asian cultures often maintain negative perceptions of homosexuality, perhaps as a result of outdated beliefs that homosexuality is a disease and traditional gender roles that do not accept homosexuality.102,107-109 Additionally, spirituality and religious issues may be salient for African American gay men, either as a source of positive support and coping or alienation, oppression, and conflict.110,111
A clear distinction in the Latino, Asian, and African American cultures exists between sexual behavior and sexual identity; for example, “down low” (Table 1) refers to Latino and African American men who do not identify as gay but have sex with men and do not tell their female partner. Furthermore, “homo thugz” (Table 1) refers to Latino and African American men who are considered tough and involved in gangster behavior but have sex with men; the hypermasculine external appearance has been interpreted as a coping mechanism against antigay prejudice. 1 Among Chinese men who have unprotected sex with men, a large proportion are married or maintain a romantic partnership with a woman. 112
For gay men in ethnic minority groups, there are several factors that may increase the risk of HIV infection, and these factors are sometimes unique to different groups of men. African American and Latino gay men who maintain more allegiance to their cultural background had a more traditional ethnic identity, experienced lower levels of acceptance from their families and communities, have been found to participate in riskier sexual behaviors, and to be at an increased risk for contracting HIV.113,114 Regarding African American men in particular, Myers et al 115 identified psychological distress, older age, and lower socioeconomic status as factors that increase risky sexual behavior. In Mexico and some other Latin American countries, cultural heterosexism and judgmental attitudes toward MWSM are considered to be contributing factors to the risk of HIV infection. 116 Increased risk of unprotected anal intercourse was found in younger, more “out” Asian American/Pacific Islander MWSM. 117 Finally, experiences of victimization have led to increased HIV risk behaviors among two-spirited American Indian men. 118
Cultural norms among ethnic minority groups may create stigma for men to openly disclose their gay sexual orientation making it difficult to develop and implement preventative interventions. 116 Gay men of color have been considered “forgotten” in HIV/AIDS prevention research, and scholars have noted that there is a lack of empirically supported prevention interventions for gay men of color.104,119 For example, research with men of color on the “down low” and condom use produced mixed findings.120,121 Some recommendations may be considered based on the limited research in this area. When addressing HIV prevention with African American, Asian, and Latino MWSM, it may be necessary to target behavior rather than identity as a way to maintain their outward heterosexual identity but decrease risky sexual practices.121,122 When approached by men for advice on safe sexual practices, health professionals should ask what genders the man is sexually active with rather than what the man’s sexual orientation is to provide appropriate information. Health practitioners are recommended to provide all men, regardless of sexual orientation, information on abstinence-only approaches to sexual practices, proper condom use, and the increased risk of HIV contraction when sexual behavior is mixed with illicit drug use.
Interventions focusing on improving the self-view of gay men as well as their positive roles and places in their communities may also be useful. Training Latino and African American gay men to be positive role models for safe sex behaviors may be an effective preventative strategy to decrease unsafe sexual practices among at-risk men in those communities.123,124 Consistent with the minority stress model, supportive family and friend networks helped Asian/Pacific Islander gay men cope with discrimination, which decreased depressive symptoms and HIV risk. 104 Increasing the self-efficacy of Asian gay men to avoid risky sexual practices represents an additional preventative intervention that has been found to decrease HIV risk. 125
Applying Contextualization to Gay-Affirmative Practices
Throughout the literature review, we connected research findings to interventions for health practitioners to implement with gay men. This section elaborates on those connections and provides additional practical recommendations for health practitioners working with gay men in various settings.
In line with scholarship on multicultural competencies in the health disciplines, we also contend that health practitioners need to be active in examining their own feelings, biases, attitudes, and stereotypes related to sexual orientation, homophobia, heterocentrism, and homonegativity. 126 Reflective health practitioners understand their worldview and how it may be manifested in their practice with gay men, which can help avoid potential harm through implicit or explicit pathologizing or discrimination of gay clients. 74 In addition to self-awareness, health practitioners are urged to learn as much as possible about gay men, subgroups of gay men, and associated cultural norms and resources in order to understand their worldview more fully and to more effectively and ethically treat gay male clients.22,126,127 Indeed, research has indicated that increased self-awareness and knowledge of culturally different clients enhances clinical care and contributes to positive treatment outcomes. 128
To avoid a pathological view of gay men, health practitioners should recognize that homosexuality per se is not indicative of health pathology and integrate these theoretical models (minority stress, gender socialization, and identity development) and constructs (internalized homonegativity, homophobia, and heterosexism) into their practice with gay men.127,129,130 For example, health practitioners can ask gay men, “Sometimes sexual minorities internalize societal messages. How do you think societal messages have affected you?” or “Where do you think stress comes from in your life as a sexual minority?” In line with a nonpathological view of gay men, health practitioners are urged to adopt a strength-based approach that is accepting of sexual orientation diversity, focuses on health instead of deficits, and actively works to enhance the strengths of gay men. 74 Asking a gay client to “tell me about the strengths that you have developed as a sexual minority man” may go a long way toward building a supportive therapeutic relationship.
Health practitioners can incorporate additional principles of gay-affirmative therapy (GAT) into their clinical care of gay men such as (a) creating a safe place to discuss complex and difficult sexual orientation issues; (b) communicating empathy, care, and affirmation to facilitate a positive health practitioner–gay client relationship; (c) willingness to equalize power in the health practitioner–gay client relationship vis-à-vis presenting as more personable and self-disclosing; and (d) viewing the gay client through a holistic perspective by recognizing that the gay clients’ sexuality is only one part of a whole person and sexual health concerns are intertwined with the entire person.131,132
The risk of a mental disorder is largely reduced among MWSM when discrimination and perceived threat are controlled. 133 Awareness of the social contexts that increase health risks for gay men may pose a unique challenge for some health practitioners to become involved in systemic interventions. 134 As some gay men consider general health materials and settings to be nonaffirmative, health practitioners may start by ensuring that the environment in which they work is comfortable and safe for gay men to feel at ease to openly disclose and discuss their health concerns. 135 For example, health practitioners can stock the office with relevant educational materials (eg, Gay and Lesbian National Help Center), develop inclusive patient intake and other forms, and pay attention to office décor and waiting room publications.135,136 Health offices can offer Gay City News and the Advocate as publications to stock in waiting rooms and use Queer Arts Resource to generate ideas about gay-friendly art to display in the health setting (Table 3). Health professionals can play pivotal roles in challenging negative policies against gay men such as restrictions and bans against adopting children, donating blood, and even simply the freedom to disclose their sexual orientation.
Some health practitioners may be inclined to intervene on behalf of gay men at other systemic levels by focusing on professional organization initiatives, public health, advocacy, and awareness education in the community.137-139 For example, health practitioners can become involved at a professional organization level such as sitting on the GLBT Advisory Committee of the American Medical Association or the American Psychological Association’s task force that developed treatment guidelines for lesbian, gay, and bisexual clients. If such groups and initiatives do not exist in a particular health discipline or organization, an obvious opportunity to make systemic changes on behalf of gay men’s health is to develop such committees, groups, and initiatives in your home professional organization. In addition, for adolescent gay males, health practitioners can collaborate with schools by providing information on gay male development and the impacts of heterosexism and homophobic victimization, which can improve the school environment for sexual minority youth. 83 Understanding the language surrounding sexual prejudice increases cultural competence and allows for clinicians to advocate for social change by knowing and debunking the negative societal stereotypes about gay men (Table 2). 140
Conclusions and Directions for Future Research and Practice
As noted, the extant literature lacks a full understanding of gay men’s strengths and positive developmental processes related to their health. An unfortunate consequence of this gap in the literature is that health practitioners may lack the appropriate knowledge and training to implement a strength-based treatment approach with gay men. We suggest that interdisciplinary efforts are made to address this gap in both research and practice. Along those lines, health professionals should always critically examine the research they draw on when working with gay clients to avoid being influenced by the noted research limitations and negative implications of the deficit models (see Table 4 for a summary of main points for health practitioners). The adoption of a gay-affirmative perspective can be more beneficial to the health of gay clients and to the professional development of health practitioners.
Summary of Main Points for Health Practitioners

Health practitioners are encouraged to further develop their multicultural competences in relation to gay men. The development of multicultural competences is an ongoing, intentional process that entails increased self-awareness, knowledge of gay men, and appropriate choice of interventions for your gay client. For example, it is important to remember that minority stress is the basis for contextualizing gay men’s health, in that it is stress and discrimination that underlie negative health outcomes, rather than being gay in and of itself. Such an understanding of gay men’s health may lead health practitioners to choose more systemic interventions in order to address negative societal discrimination that contributes to negative health outcomes for gay men. We advocate for practitioners and researchers to continue to collaborate on empirical support for systemic interventions.
A reoccurring theme in the literature is the vast and differing roles of social support in the lives of gay men. Overall, social support is viewed as a positive factor for gay men’s health and a buffer against negative stress. Health practitioners should not assume who or what group is a support for gay men. Rather, we suggest that health practitioners work with gay men to maximize and encourage the use of their identified support networks.
Furthermore, gay men have many components to their identity beyond their sexuality and should be treated as multifaceted individuals. With this in mind, it is crucial to remember that gay men who are members of other minority groups may be especially vulnerable to the negative impact of stress and discrimination, and therefore may experience even more negative health consequences from a double or even triple minority status.
When interpreting literature, including this review, it is important to keep in mind that individual gay men have unique differences and cannot be treated uniformly. Results from studies with a particular group of gay men may not generalize to all gay men. Even within gay culture, there are subcultures and variations that call for health practitioners to interact with each gay client on an individual basis, much as practitioners would do for any client.
