Abstract
Obesity-related pathophysiological mechanisms adversely affect human fertility and infertility treatment. Conventional anthropometric indices for assessing obesity poorly differentiate visceral adipose tissue (VAT) and subcutaneous adipose tissue (SAT). This explains inconsistencies between the studies evaluating the influence of obesity on semen parameters and assisted reproductive technology (ART) outcomes. A Body Shape Index (ABSI) and body roundness index (BRI) are novel indices that offer better differentiation of VAT and SAT. Our study assessed the correlation between traditional and novel indices with semen parameters and ART outcomes.
A cross-sectional study, conducted at a tertiary fertility center from January 2023 to March 2025, encompassed 319 men undergoing ART. They were divided into four groups based on body mass index (BMI), waist-to-hip ratio (WHR), waist-to-height ratio (WHtR), BRI, and ABSI quartiles. Anthropometric indices were measured and correlated with semen parameters (semen volume, sperm concentration, motility, and morphology) and ART outcomes (number of obtained embryos, transferred embryos, frozen embryos, and usable blastocyst development and embryo utilization rates).
Our analysis revealed that anthropometric indices correlated differently with semen parameters and ART outcomes. BMI, BRI, and WHtR correlated negatively with semen parameters, whereas WHR and ABSI did not. ABSI negatively correlated with all analyzed ART outcomes, while WHR significantly correlated only with total number of embryos.
Traditional anthropometric indices that inform us on general obesity are linked to semen analysis parameters. Novel indices that differentiate VAT and SAT are linked with ART outcomes, suggesting possible epigenetic consequences of increased VAT.
Keywords
Introduction
Subcutaneous adipose tissue (SAT) is deposited under the skin, and therefore, it can be visualized, palpated, and measured by skinfold caliper or ultrasound. In contrast, visceral adipose tissue (VAT) stowed around internal organs (Ibrahim, 2010). The primary function of VAT is to protect internal organs by providing the insulation from heat, cold, sound waves, and electricity (Kolb, 2022; Rahman & Jun, 2022; Rosen & Spiegelman, 2014), and by cushioning body parts exposed to high levels of mechanical stress (Rosen & Spiegelman, 2014). Excessive deposition of SAT and VAT carries different health risks, with VAT more strongly associated with general and reproductive health issues. Cardiovascular disease is associated more to the local distribution of adipose tissue and VAT than to total body fat (Cesaro et al., 2023; Suárez-Cuenca et al., 2021). Moreover, increased amount of VAT is linked with reproductive health risks, including infertility (Z. Zhou et al., 2024). Observation that obesity and infertility “pandemics” have parallel fast-paced prevalence trends led to hypotheses linking men’s obesity and reproductive health. Decreased levels of sex hormone-binding globulin, inhibin B, and androgens with increased serum estradiol are linked to the degree of obesity (Hammoud et al., 2008; Hofny et al., 2010). Furthermore, obesity-derived oxidative stress leads to sperm DNA damage and compromised sperm function (Heydari et al., 2021). Following the hypotheses, extensive research has been performed evaluating the influence of nutritional status on male fertility. While some authors claim that increased body weight adversely affects sperm quality (Jensen et al., 2004; La Vignera et al., 2012), others refute such association (MacDonald et al., 2013; Nikolic et al., 2024). Even systematic reviews and meta-analyses do not provide conclusive answers or deliver conflicting results regarding this issue (Y. Li et al., 2024; Santi et al., 2024; Sermondade et al., 2013). In the past, traditional anthropometric indices served as indicators of nutritional and obesity status, and index of metabolic, cardiovascular, and diabetogenic risks, due to their simplicity and usefulness (Kahn et al., 2019; Xing et al., 2020; Zhao et al., 2018). Since 1972, body mass index (BMI) has served as a diagnostic index for general obesity and indicator of health risks (Batsis et al., 2016; Blackburn & Jacobs, 2014). Still, BMI only reflects the general dispersal of adipose tissue in body (Hsieh et al., 2010). In the interim, other conventional anthropometric indices, such as waist circumference (WC), waist-to-hip ratio (WHR), and waist-to-height ratio (WHtR) have been established as indicators of risk for metabolic syndrome (Hsieh et al., 2010; Jenkins et al., 2018). Nevertheless, the traditional anthropometric indices do not discern between muscle and adipose tissue (Myint et al., 2014; Xu et al., 2021). Novel indices have been introduced to overcome these limits. A Body Shape Index (ABSI) mirrors the silhouette of body using WC, weight, and height, while body roundness index (BRI) deploys height and WC to envisage the proportion of total and regional fat (Christakoudi et al., 2020; G. Li et al., 2020; Mouchti et al., 2023; Zhao et al., 2018). Earlier studies found that ABSI and BRI are more linked with VAT and cardiometabolic risks, diabetes and premature mortality hazards compared to traditional anthropometric indices such as BMI and WC (Nkwana et al., 2021; Xu et al., 2021).
At the present time, few studies have evaluated association of traditional anthropometric parameters with semen parameters, and none have evaluated this association with novel anthropometric parameters. We aimed to test correlation between anthropometric indices (both traditional and contemporary) and semen analysis parameters. We also aimed to test correlation between traditional and novel indices and in vitro fertilization (IVF) outcomes.
Method
Study Design
The cross-sectional study was conducted among couples undergoing fresh autologous ART cycles in the the Clinic for Obstetrics and Gynecology Narodni front, referral tertiary health care center in Belgrade, Serbia. The study period was between June 2023 and March 2025. The study was approved by Ethical Committee of Clinic for Gynecology and Obstetrics “Narodni Front” (Approval number 22008/2023/009343 on June 18, 2023).
Aim of the Study
Primary End Point
We aimed to examine the correlation between WHR, WHtR, BMI, BRI, and ABSI with semen parameters (semen volume, sperm concentration, motility, and morphology of spermatozoa).
Secondary End Point
The impact of above-mentioned anthropometric parameters on IVF outcomes: total number of obtained embryos, number of obtained good-quality (GQ) embryos, number of transferred embryos, number of obtained blastocysts, number of frozen blastocysts, usable blastocyst development rate (UBDR) and embryo utilization rate (EUR) were performed. The key predictors of IVF success considered among female participants are age, ethnicity, antral follicle count, and the duration and cause of infertility; therefore, these characteristics were evaluated in the female partners of the male participants.
Study Population
Inclusion criteria were men no younger than 18 years of age. Exclusion criteria were a history of chronic diseases and the use of medications known to impair semen quality, as reported in previous studies (Ding et al., 2017). Specific chronic conditions were azoospermia with previously frozen spermatozoa, chronic endocrine (diabetes mellitus, hypergonadotropic hypogonadism, androgen and estrogen excess, hyperprolactinemia), and other diseases (malignancies treated with chemotherapy and/or radiation, autoimmune diseases, such as lupus, rheumatoid arthritis, and multiple sclerosis, chronic kidney disease, etc.) that affect semen analysis. Furthermore, all men with genetic conditions (cystic fibrosis, hypogonadotropic hypogonadism in Kallmann syndrome, and Klinefelter syndrome) and other conditions (trauma and surgery of the genitals, undescended testicles or mumps in the childhood) that could influence semen analysis were excluded.
With regard to medications, 12 patients were taking antihypertensive agents, 3 were on anti-arrhythmic therapy, 9 were receiving antidepressants, 1 was on antiepileptic therapy, 8 were using anti-inflammatory agents for rheumatic diseases, 7 were on testosterone therapy, and 8 patients were receiving antibacterial agents. These patients were therefore excluded from further participation in the study. All participants without all the necessary data and documentation were also excluded. A flow diagram from Figure 1 illustrates these data.
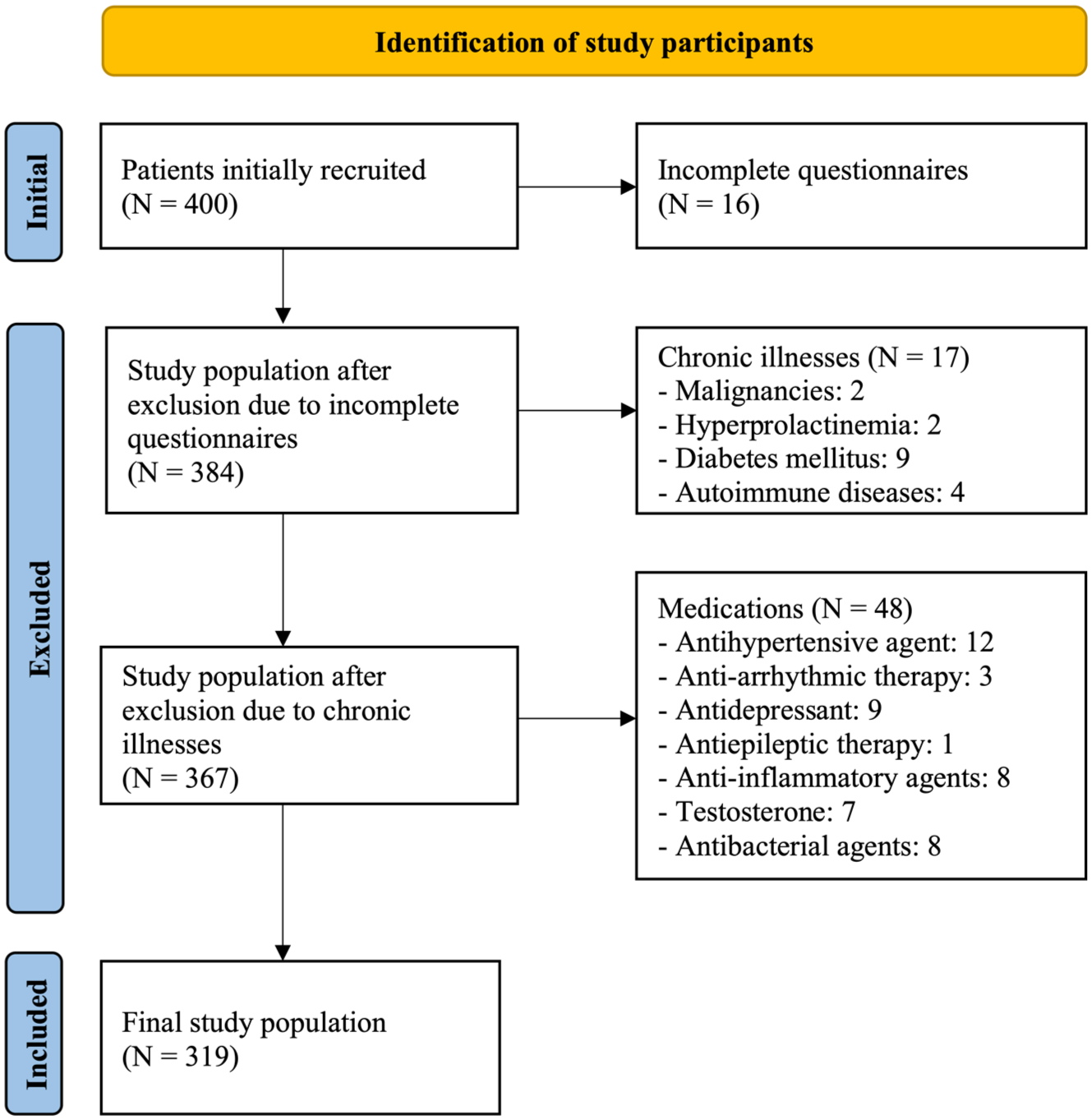
Identification of Study Participants
After consenting in signing form, the required data were gathered: age, smoking habit, education level, profession, sedentary/active lifestyle, exposure to harmful, and/or toxic substances. Anthropometric parameters: WC and hip circumference (HC), weight, and height were measured by qualified and trained physicians, and ABSI, BMI, and BRI are calculated. Waist and hip measurements are performed to the nearest 0.1 cm using a flexible, non-elastic tape wearing minimal clothing, standing upright without sucking in their stomachs. Waist measurement is recorded at the midpoint between the lower ribs and the iliac crest, while hip measurement is taken at the widest point around the buttocks (Eaton–Evans, 2005). The height was measured as participants standing barefoot and upright, feet together, using a stadiometer, and recorded in centimeters. Weight was recorded in kilograms (kg), using a calibrated electronic scale, with a maximum weight of 200 kg. Participants were weighed while standing in the center of the scale, facing forward, and wearing minimal clothing (Sekgala et al., 2022). BMI was calculated by dividing weight (kg) by the square of height (meters), whereas BRI was calculated as 364.2 − 365.5 × √ (1 − [WC in cm / 2π]2 / [0.5 × height in cm]2). The ABSI is calculated by dividing WC with BMI2/3 × height1/2 (Zhao et al., 2018).
Semen Analysis
Semen analysis of the study participants was performed by adhering to the WHO Laboratory Manual for the Examination and Processing of Human Semen (World Health Organization, 2021). All men were instructed to maintain a minimum of 2 days of sexual abstinence prior to sample collection. Although male partners provided semen analysis reports from both our laboratory and external facilities prior to initiation of the ART process, for the purpose of this study, only the semen samples utilized in the current ART cycle were analyzed. The analyzed semen parameters were semen volume (ml), sperm concentration (millions [M]/ml), motility, and morphology of spermatozoa.
IVF Outcomes
The correlation was tested between all previously mentioned anthropometric parameters and following IVF outcomes: total number of obtained embryos, number of obtained GQ embryos, number of transferred embryos, number of obtained blastocysts, and number of frozen blastocysts. Furthermore, correlation analyses between anthropometric parameters and UBDR and between anthropometric parameters and EUR were performed. UBDR was defined as the proportion of two pronuclear zygotes, which subsequently became blastocysts of sufficient quality for clinical use (Chaillot et al., 2024; Tiegs & Scott, 2020). European Society of Human Reproduction and Embryology defined EUR as the number of utilized embryos, either transferred or/and frozen embryos, per number of 2 pro-nuclei (2PN) zygotes (“The Vienna Consensus,” 2017).
Statistical Analysis
Descriptive statistical methods were used: absolute and relative numbers (N, %), measures of central tendency (arithmetic mean, median), and measures of dispersion (standard deviation, percentiles). Analytical statistical methods were used for testing the differences. Analysis of variance (ANOVA) was used as parametric test, and chi-square test and Kruskal–Wallis test as nonparametric tests. The Pearson or Spearman correlation was performed according to the type of data and its distribution. For normal distribution data, parametric methods were used, whereas nonparametric methods were performed in a situation where the distribution was not normal. The normality of the distribution was examined based on descriptive parameters, normality of distribution tests (Kolmogorov–Smirnov and Shapiro–Wilk test) and graphic methods (histogram, boxplot, QQ plot). All statistical differences and correlations were considered significant if they met the criteria of p-value less than .05. All data were analyzed using SPSS 29.0 (IBM Corp. Released 2023. IBM SPSS Statistics for Windows, Version 20.0. Armonk, NY, USA).
Results
Three hundred and nineteen men were included in the study who underwent ART with their partners in our clinic. Baseline characteristics of the study participants along with characteristics of female partners are presented in Table 1.
Characteristics of the Study Participants (N = 319).

Note. SD—standard deviation; Perc—percentile; WC—Waist circumference, HC—Hip circumference, ABSI—A Body Shape Index, BMI—body mass index, BRI—body roundness index, WHR—waist-to-hip ratio, WHtR—waist-to-height ratio, AFC—antral follicle count.
In addition to the baseline characteristics of the female partners, we also recorded the underlying causes of infertility. The three most prevalent causes among the female participants were PCOS, observed in 93 women (29.15%), followed closely by unexplained infertility in 92 women (28.84%), and poor ovarian response in 73 women (22.88%). Other identified causes included fallopian tube pathology in 30 women (9.4%) and endometriosis in 7 women (2.19%). In addition, 24 women (7.52%) were diagnosed with more than one contributing factor to infertility.
Study participants were divided into four groups based on quartiles for BMI, WHR, WHtR, BRI, and ABSI. No statistically significant differences were found between the quartile groups with respect to smoking habits, education level, physical activity level (sedentary vs. active), or exposure to harmful and/or toxic substances (p > .05). Across all groups and subgroups, non-smokers were more prevalent than smokers, except in the WHR quartiles, where the proportions of smokers and non-smokers were equal (50% each). In terms of educational background, none of the participants had only primary education. The majority had completed secondary education (57.7%), while the remaining 42.3% held higher education degrees. With regard to occupational exposure, 62.7% of participants reported working in potentially hazardous occupations, whereas 36.1% reported no such exposure. However, no significant differences in exposure were observed between the different quartile groups. The most common occupational risk factor was a sedentary lifestyle, which was consistently identified as the primary potentially harmful exposure across the entire sample and within each subgroup.
Results of correlation analysis between anthropometric indices of study participants and semen analysis parameters and IVF outcomes are presented in Table 2.
Correlation Between Anthropometric Indices and Semen Analysis Parameters and IVF Outcomes.
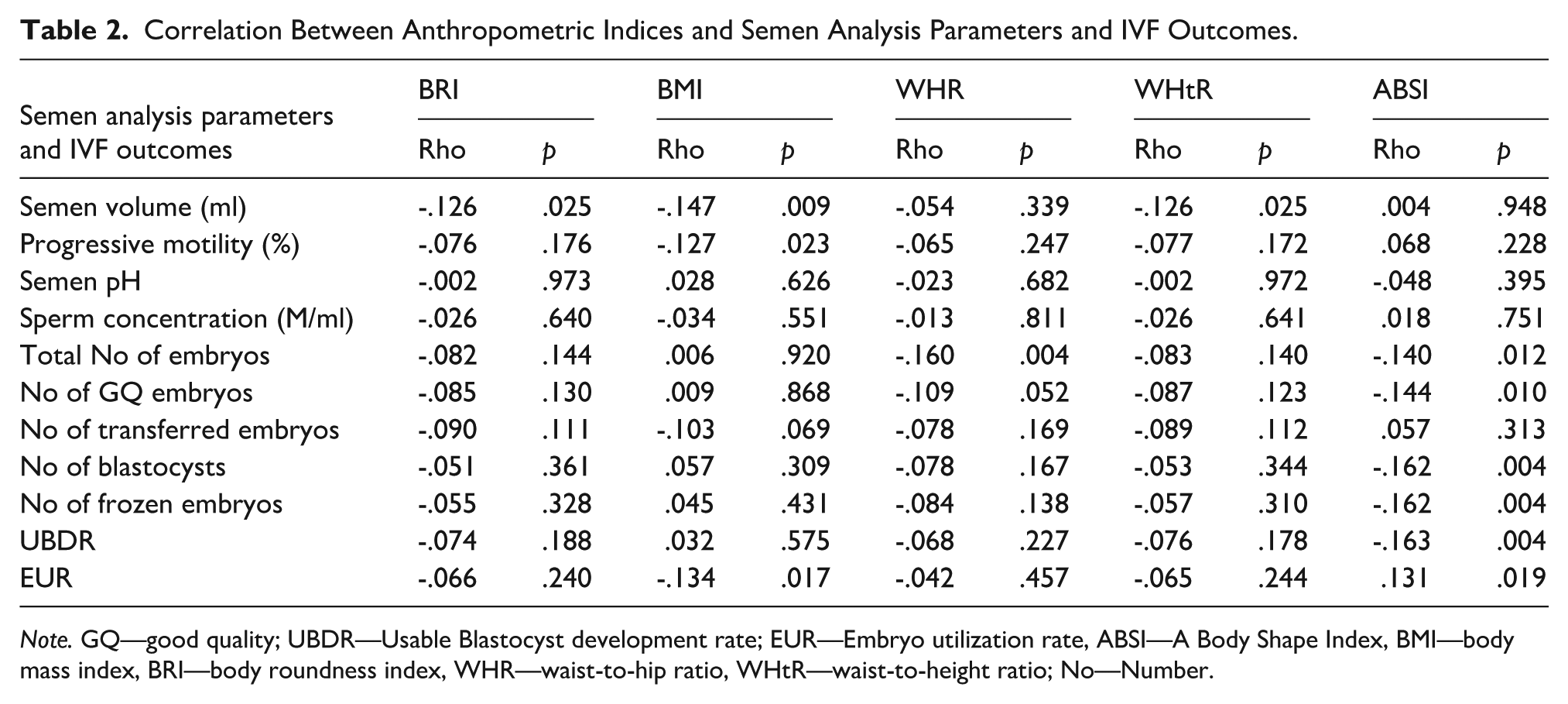
Note. GQ—good quality; UBDR—Usable Blastocyst development rate; EUR—Embryo utilization rate, ABSI—A Body Shape Index, BMI—body mass index, BRI—body roundness index, WHR—waist-to-hip ratio, WHtR—waist-to-height ratio; No—Number.
All study participants were subsequently divided into four groups regarding each anthropometric index to observe possible differences across these groups in characteristics of their female partners that could possibly influence analyzed IVF outcomes. Analyses revealed that among study groups regarding BRI and BMI, significant differences were present. Unlike BMI and BRI quartiles groups, ABSI quartile groups showed no differences in characteristics of the female partners. These data are presented in Table 3.
Female Partners’ Characteristics Across ABSI, BRI, BMI, WHR, and WHtR Quartile Groups of Men Participants.

Note. Results are presented as number (percentage), M ± SD or median (25-75th percentile); ABSI—A Body Shape Index, BMI—body mass index, BRI—body roundness index, WHR—waist-to-hip ratio, WHtR—waist-to-height ratio; AFC—antral follicle count; PCOS—polycystic ovary syndrome.
Fallopian tubes pathology.
Since the strongest correlations between anthropometric indices and different IVF outcomes were found in ABSI, and considering that the differences between characteristic of women that influence the most IVF outcomes were not found between ABSI groups of men, we believe that ABSI of men could also be the most reliable indicator of IVF success regarding male factor. Therefore, we also aimed to graphically present the correlation between ABSI and IVF outcomes (Figure 2).

Correlation Between ABSI and Different IVF Outcomes
Discussion
Our study evaluated the correlation of several anthropometric indices with semen analysis parameters and IVF outcomes. It was established that different indices correlate differently with semen analysis parameters and IVF outcomes. While BMI negatively correlated with both semen volume and progressive motility, BRI and WHtR correlated negatively only with semen volume, while ABSI and WHR did not correlate with any of sperm analysis parameters. Interestingly, the correlation between anthropometric indices and IVF outcomes was statistically significant only in two cases, WHR and ABSI. Whereas ABSI negatively correlated with all analyzed IVF outcomes, WHR significantly correlated only with total number of obtained embryos.
Possible explanations for the observed discrepancies regarding the influence of anthropometric indices on semen parameters and IVF outcomes include following facts. Semen volume is influenced not only by estrogen and testosterone equilibrium, function of testicles, prostate, and seminal vesicles but also by oxidative stress, inflammation, and scrotal temperature (Liu & Ding, 2017). Oxidative stress, inflammation, and scrotal temperature are increased by abdominal fat. On one hand, BMI measures overall body fat (although not fat distribution) and correlates with low testosterone and high estrogen levels, increased scrotal temperature, and oxidative stress, whereas BRI estimates the fat percentage of body fat more accurately than BMI. Furthermore, BRI more intensely reflects abdominal obesity and body shape, which is directly tied not only to hormonal disturbances and inflammation but also to seminal vesicle dysfunction (Y.-F. Zhou et al., 2023). In addition, WHtR as an indicator of central obesity is also a solid predictor of metabolic syndrome and hormonal imbalance, both of which influence semen parameters. Although ABSI and WHR are even better indicators of central obesity, they underestimate direct obesity-related dysfunction in reproductive organs (Hoermann et al., 2019), and this could explain the lack of correlation between semen analysis parameters, ABSI, and WHR. On the other hand, WHR and ABSI, as obesity indices superior than BMI, WHtR, and BRI, could detect more thoroughly subtle obesity-related changes that are disturbing spermatogenesis, increasing DNA sperm fragmentation and histone retention, therefore influencing epigenetic profile of embryo (Akhatova et al., 2025), which BMI, WHtR, and BRI are not able to spot. Moreover, BMI and WHtR do not precisely distinguish between fat and muscle tissue. While BRI estimates shape and fat percentage of body and provides body visual approximation, still it does not precisely distinguish between fat and muscle tissue. In contrast to BMI, BRI, and WHtR (which assess overall/central obesity), ABSI and WHR focus more on fat distribution (distinguishing VAT and SAT), which is a strong predictor of disease even in people with “normal” BMI.
Our results reveal correlations between anthropometric indices and semen analysis parameters and are in line with published literature data, pointing out to the lack of single anthropometric index that consistently predicts all semen parameters. This suggests that different indices capture distinct aspects of body composition and metabolic status. Among the evaluated indices, BMI remains the most extensively studied and widely used in the context of male fertility. However, BMI-based data in the literature are often contradictory, making it difficult to draw reliable conclusions or place full trust in the findings, as discussed earlier. MacDonald et al. found no significant correlation between BMI and most semen parameters, except for normal sperm morphology (MacDonald et al., 2013). We noted that significant proportion of BMI values in study of MacDonald et al. were self-reported by study participants, while in our study, all measurements and anthropometric indices were calculated and measured by qualified and trained physicians. In addition, in contrast to our study where all study participants were from public clinic, they recruited participants both from private and public fertility clinics. We could assume that significant differences in socio-economic and lifestyle characteristics between men in private and public clinics could lead to different semen analysis parameters since high socio-economic status could be linked favorable with all semen parameters (Horns et al., 2023). This could explain discrepancies between findings of MacDonald and colleagues and our results. Our results are partially in line with another study that observed differences in semen parameters. Keszthelyi and authors found that BMI has a significant impact not only on progressive motility but also on total sperm count (Keszthelyi et al., 2020). The authors tested association between BMI and semen analysis parameters by regression analysis, but we performed correlation analysis and that could explain slight discrepancies between the results. In that context, our results are supported by more recent meta-analysis by Sermondade et al. (2013), which also found no significant correlation between BMI and sperm concentration.
Our study identified a negative correlation between both BRI and WHtR with semen volume. To the best of our knowledge, these specific anthropometric indices have not been previously investigated in relation to semen quality. A limited number of studies have examined the association between body composition and ejaculate volume, consistently reporting negative correlations (Eisenberg et al., 2014; Fejes et al., 2005; Hammiche et al., 2012). These findings suggest that increased adiposity may be associated with reduced semen volume. In that context, Fejes et al. (2005) found that both WHR and WC were negatively correlated with semen volume, while the LIFE study (Eisenberg et al., 2014) reported inverse associations between semen volume and both BMI and WC. Nonetheless, it is important to note that semen volume is often not included in the primary analysis in many studies, as it is generally considered a secondary marker of male fertility, with less clinical relevance compared to parameters such as sperm concentration, progressive motility, and morphology (Bostofte et al., 1982; Keszthelyi et al., 2020).
To the best of our knowledge, our study is the first one to evaluate how novel anthropometric indices of men (ABSI and BRI) influence important IVF outcomes such as number of total obtained embryos, GQ embryos, number of transferred embryos, number of blastocysts, number of frozen embryos, UBDR, and EUR. We believe that our results are of great importance since they enlighten relationship between body shape composition, body fat distribution (VAT vs. SAT), and UBDR, because UBDR is a crucial indicator of embryo quality and a strong predictor of IVF outcome success (Chaillot et al., 2024). Prominent finding of our study is the lack of influence of majority of anthropometric indices (exceptions are ABSI and WHR) on IVF outcomes. The majority of indices (BMI, WHtR, BRI) that detect obesity but do not distinguish VAT and SAT are significantly correlated with semen analysis parameters but not with IVF outcomes. That confirms the seemingly paradoxical finding that male obesity may not significantly affect conventional semen analysis parameters (volume, concentration, motility, or morphology), still impairing embryo quality by profound molecular mechanisms, particularly involving oxidative damage and epigenetic alterations. We found that ABSI and WHR significantly correlate with IVF outcomes. This may suggest that specific patterns of fat distribution influence fertilization at a higher, systemic level (e.g., through effects on spermatogenesis, hormonal balance, or inflammation) (Mintziori et al., 2020) or at epigenetic level (Akhatova et al., 2025). Moreover, many studies before concluded that semen quality is not a strong predictor of successful pregnancy in couples undergoing ART (Buck Louis et al., 2014). Apart from that, contemporary lifestyle characteristics of the 21st century (diet, sedentary lifestyle, and environmental exposures) could influence the male epigenome and, consequently, fertility (Turner et al., 2020). Balanced diet, providing essential nutrients for proper function of body, maintaining of health, and for support of growth and development, called a nutritional diet, has impact on men’s fertility (Xia et al., 2015). It supplies body with key nutrients (macronutrients, micronutrients, water, and fiber) in the right proportions. Inadequate dietary intake contributes to disturbances in nutritional status, which can be identified using anthropometric indices such as ABSI and WHR. We noted that ABSI exhibited a consistent negative correlation with all examined IVF outcome variables, while WHR was significantly linked only to the total number of embryos obtained. This may suggest that this index may capture risk-related aspects of body composition that go beyond BMI and abdominal indices, potentially including chronic inflammation or oxidative stress.
Limitations and Strengths of the Study
In a growing body of research in the field of reproductive health that tries to clarify the association between nutritional status and obesity with semen analysis parameters and IVF outcomes, our study is the first one that tested correlation between novel anthropometric indices and multiple important IVF outcomes including the total number of obtained embryos, GQ embryos, blastocysts, frozen embryos, UBDR, and EUR. This is considered as a strength of the study. The main limitation of our study is that we did not fully control for potential confounding factors. Since we used correlation analysis, the inclusion of women undergoing IVF with different causes of infertility, rather than restricting the analysis to those with unexplained infertility, may have introduced confounding. Future studies with larger cohorts and more comprehensive designs, including factor analysis, will be needed to address this issue. In addition, other potential confounders were not assessed, such as male hormonal status, presence of varicocele, or urogenital infections. Similarly, in female partners, data on detailed hormonal status and lifestyle habits were not included, which may also have influenced the outcomes. Besides, the study was performed in University Hospital, which is considered as the national referral clinic; hence, our data derive from the single center which is recognized as another study limitation. Moreover, further analysis and comparison of procedures regarding sperm preparation for ART were not performed, and this could be another limitation, since different sperm preparation techniques have diverse effects on DNA fragmentation in viable spermatozoa (Muratori et al., 2019).
Conclusion
In conclusion, traditional anthropometric indices, which are primarily used to assess overall obesity, are associated with semen quality parameters. Novel anthropometric indices that distinguish between VAT and SAT are linked with IVF outcomes, indicating a potential role of VAT in epigenetic mechanisms. Therefore, further studies are needed to explore the influence of VAT on epigenetics. In addition, studies with larger sample sizes and more robust statistical models are needed to confirm and extend these findings.
Footnotes
Acknowledgements
We would like to express our sincere gratitude to Dr. Biljana Popovic Todorovic for her valuable time and effort in reviewing and providing insightful corrections to the manuscript. Her constructive comments and careful editing significantly contributed to improving the clarity and quality of the final version.
Ethical Considerations
The study was approved by the Ethical Committee of the Clinic for Gynecology and Obstetrics “Narodni Front” (approval number 22008/2023/009343 on June 18, 2023). The requirement for written informed consent was waived due to the retrospective design and the use of de-identified data.
Author Contributions
Ana Nikolic: Conceptualization, Data curation, Investigation, Writing—original draft, and Visualization; Vladimir Gerginic: Data curation, Investigation, and Writing—original draft; Svetlana Dragojevic Dikic: Supervision, Project administration, and Conceptualization; Dragana Bojovic Jovic: Methodology, Conceptualization, and Supervision; Bojana Salovic: Data curation, Formal analysis, Methodology, Validation, and Writing—original draft; Milan Perovic: Conceptualization, Supervision, Project administration, and Writing—review and editing.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Human Rights Statements
All procedures followed were with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and its later amendments.
Animal Studies
This article does not contain any studies with animal subjects performed by any of the authors.
Data Availability Statement
The data set generated and analyzed during the current study is available from the corresponding author on reasonable request.
