Abstract
The aim of this study was to evaluate the efficacy and safety of extracorporeal shockwave therapy (ESWT) and acupuncture therapy for patients with chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS).
We searched electronic databases including PubMed, Cochrane Library, Embase and web of science from its inception to June 1, 2021. The randomized controlled trials (RCTs) that compared ESWT and acupuncture in the management of CP/CPPS were identified. A network meta-analysis was conducted with the software of STATA 14.0.
Nine RCTs with 525 patients were enrolled in our analysis. The results revealed that both ESWT and acupuncture were significantly better than the sham procedure in the outcomes of total score of NIH-CPSI, pain subscore, urinary symptoms subscore, QoL subscore, IPSS score, the IIEF score and response rates (p < .05). Both ESWT and acupuncture were well-tolerated and had no obviously increased adverse events. Compared with acupuncture, ESWT was associated with better short term (<4w) and mid-term (8-12 w) efficacy of total score, pain subscore, urinary symptoms subscore, and QoL subscore of NIH-CPSI, IPSS score, IIEF score, and response rate. However, ESWT did not present better long-term (<24 w) outcomes than acupuncture in total score, pain subscore, urinary symptoms subscore, and QoL subscore of NIH-CPSI.
Both ESWT and acupuncture were effective and well-tolerated in the management of CP/CPPS. ESWT seemed to have better short (<4 w) and mid-term (8-12 w) efficacy but similar long-term (>24 w) efficacy than acupuncture.
Keywords
Background
Chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS), the most common urological diagnosis in men under the age of 50, is defined as pelvic pain at least three months in the first six months with no other determinable causes (Engeler et al., 2013; 2018). It seriously harms the quality of life (QoL) of patients worldwide. The clinical features of CP/CPPS include pelvic pain, lower urinary tract symptoms and other symptoms like obstructive, irritating dysuria, painful ejaculation, and excessive sperm. The severity of CP/CPPS symptoms are commonly evaluated with the tool of the National Institutes of Health Index (NIH-CPSI) (Wagenlehner et al., 2013). The NIH-CPSI has shown its excellent reliability, validity, and responsiveness to change, which has been commonly used worldwide as the primary outcome of CP/CPPS treatment studies.
Many pharmacological therapies including antimicrobial drugs, alpha-blockers, anti-inflammatory drugs, and combined therapy have been applied in the management of CP/CPPS. Due to the frequent failure of available treatments and lack of long-term benefits, CP/CPPS remains a major challenge all around the world (Kessler, 2016; Magistro et al., 2016). In the past few decades, some non-pharmacological therapies, such as acupuncture and extracorporeal shockwave therapy (ESWT), have gained increasing attention in the management of CP/CPPS. Both acupuncture and ESWT have been applied to clinical practice for a long time and have been proven to be effective and safe (Franco et al., 2019; Qin et al., 2016). By hyperstimulating nociceptors, ESWT can reduce muscle tone to alleviate pain. Patients received varying amounts of pulses, most between 1000 and 3000 (Liao et al., 2019). Acupuncture treatment involves the insertion of fine, single-use, sterile needles in acupuncture points. The exact therapeutic mechanism of acupuncture on CP/CPPS is unclear, and its neuromodulation, immune-modulation, and anti-inflammatory efficacy may lead to beneficial therapeutic effects. There are no direct comparisons between acupuncture and ESWT in previous studies. All available evidence comes from comparisons with placebo controls. The number, duration and frequency of sham acupuncture at non-acupoints were the same as in the acupuncture group, while in the sham acupuncture group treated with WST, the same protocol was used, but the probe was closed. With the method of network meta-analysis, we can evaluate the efficacy and safety of acupuncture and ESWT indirectly through the sham procedure. The main goal of our study was to evaluate the efficacy and safety of ESWT and acupuncture therapy in the management of CP/CPPS.
Methods
Search Strategy
A systematic review was conducted according to the guidelines for the Preferred Reporting Items for Systematic Reviews and Meta Analyses (PRISMA). The databases of PubMed, Embase, Cochrane Library, and Web of Science from its inception to June 1, 2021 were retrieved. The MeSH terms and related synonyms including “chronic pelvic pain syndrome,” “chronic prostatitis,” “extracorporeal shock wave therapy,” “ESWT,” and “acupuncture” were combined and searched. There were no limitations placed on language. The retrieval results were evaluated by reading the title, abstract, and full text by two independent investigators.
Selection Criteria
The trials were included when they met the following criteria: (1) randomized controlled trials (RCTs). (2) CP/CPPS was diagnosed according the NIH classification. (3) The interventions were ESWT, acupuncture therapy or sham procedure (SP).
The following criteria were used for study exclusion: (1) Patients were accompanied with other diseases such as acute prostatitis, urinary tract infection, bladder and urethral stones, and so on. (2) Other treatments were performed besides ESWT and acupuncture. (3) Important information for data analysis was incomplete or missing. (4) The data were unable to combine and analysis.
Extraction and Quality Assessment
All available data were extracted by two researchers independently. The total score, pain subscores, urine subscores, QoL subscore, International Prostate Symptom Score (IPSS) score, International Index of Erectile Function (IIEF) score and response rate regarded as the main efficacy outcomes. The total adverse events were regarded as the safety outcomes.
The quality of the included studies was evaluated by two independent reviewers in accordance with the tools proposed in the Cochrane Handbook, version 5.1.3. Each trial was evaluated and graded with the following standards: random sequence generation, participant blind and outcome evaluator blind, incomplete result data reporting, allocation hiding, selective data result reporting, and other deviations. The disagreements between two reviewers were resolved through discussion or inquiries with a third reviewer.
Data Synthesis and Analysis
Odds ratio (OR) and 95% confidence interval (95% CI) were used as statistical analysis of dichotomous variables, and weighted mean difference (WMD) and 95% CI were analyzed for the continuous variables. Random effect model was used due to the inconsistency between the trials. The forest graph was used to analyze the differences between the interventions. The ranking chart was used to analyze the ranking of the pros and cons of different interventions in the same outcome. All analyses were performed the software of STATA version 14.0. P < 0.05 was regarded as statistical difference.
Results
Baseline Characteristics of Included Studies
A total of 1216 records were retrieved in the databases. All of them were screened by reading titles and abstracts. The full-text assessment was performed in 45 publications. Nine RCTs (Lee & Lee, 2009; Lee et al., 2008; Moayednia et al., 2014; Qin et al., 2018; Sahin et al., 2015; Salama & Abouelnaga, 2018; Vahdatpour et al., 2013; Zeng et al., 2012; Zimmermann et al., 2009) with 525 patients were finally included in the analysis. The whole process of literature searching and screening is presented in Figure 1. Baseline characteristics of the included studies are presented in Table 1.
Basic Characteristics of Included Studies in the Meta-analysis.

Note. RCT, randomized controlled trial; CP/CPPS, chronic prostatitis/chronic pelvic pain syndrome.

Preferred reporting items for systematic reviews and meta-analyses flow diagram of the study selection process for network met analysis.
For the qualities of the included trials, the Cochrane Collaboration tool was adopted to assess the risk of bias. All included studies were randomized grouped, and six of them described adequate randomization. Five trials were conducted with blind design, Attrition bias and reporting bias were well-performed in most of the included studies. The risk-of-bias assessment of the included RCTs is summarized in Figure 2.

Risk of bias graph and summary of the included studies: (A) reviewers, judgements about each risk of bias item for eligible studies and (B) the judgements about each risk of bias item presented as percentages across all eligible studies.
Network Meta-analysis of the Total Score of NIH-CPSI
Four included studies described the short-term (<4 weeks) total score of NIH-CPSI, recruiting 164 patients. The pooled results showed that both ESWT and acupuncture therapy significantly reduced the total score than SP [EWST: MD = −5.86, 95% CI (10.30, −1.41); acupuncture: MD = −0.84, 95% CI (−8.45, 6.77)]. The differences between EWST and acupuncture were not statistical [MD: −5.02, 95% CI (−13.83, 3.80)] (Table 2). The ranking results showed that ESWT was the best intervention for total score, followed by acupuncture and sham procedure. These results are presented in Figure 3A1.
The Meta-analysis Results for All Outcomes.

Note. SP, Sham procedure; ESWT, extracorporeal shock wave therapy; MD, mean difference; OR, odds ratio; 95% CI, 95% confidence interval; QOL, quality of life; IPSS, International ostate Symptom Score; IIEF, International Index of Erectile Function.

The ranking plots based on probabilities of interventions: (A1) Total score <4 week; (A2) Total score 8–12 week; (A3) Total score >24 week; (B1) Pain subscore <4 week; (B2) Pain subscore 8–12 week (B3) Pain subscore >24 week; (C1) Urine subscore <4 week; (C2) Urine subscore 8–12 week; (C3) Urine subscore >24 week;
Seven studies with 426 patients described the outcome of mid-term (8–12 weeks) total score of NIH-CPSI. The overall results showed that EWST and acupuncture had significantly lower total score than SP [EWST MD = −2.08, 95% CI (−4.92, −0.75); acupuncture MD = - 4.51, 95% CI (−7.01, 2.00)]. The score of EWST was obviously lower than acupuncture [MD: −2.42, 95% CI (−6.20, −1.35)]. These results are presented in Table 2. The ranking results were similar to the short-term total score.
As for the long-term (>24 weeks) outcomes, 4 studies with 263 patients were taken into analysis. Compared with SP, acupuncture and EWST had significantly lower scores of NIH-CPSI. No obvious differences were detected between acupuncture and EWST. The ranking results showed that acupuncture was the best, EWST was the second, and SP was the last (Figure 3A3).
Network Meta-analysis of Pain Subscore
Four studies with 172 patients reported the short-term pain subscore of NIH-CPSI. The pooled results showed that the pain subscore of EWST was significantly lower than that of acupuncture [MD = −1.40, 95% CI (−2.74, −0.06)]. The acupuncture was associated with significantly lower than the SP treatment [MD = −1.16, 95% CI (−2.06, −0.26)]. These results are presented in Table 2. The ranking results revealed that EWST had the lowest pain subscore, followed by acupuncture, and the pain subsocre of SP was the highest. The ranking results are presented in Figure 3B1.
As for the mid-term pain subscore of NIH-CPSI, seven studies with 366 patients were analyzed. Compared with SP, acupuncture and EWST had an obvious lower pain subscore [acupuncture vs. SP: MD = −0.99, 95% CI (−3.47, −1.49); EWST vs. SP: MD = - 2.28, 95% CI (−4.78, −0.23)]. The difference between acupuncture and EWST were also statistical [MD = −1.29, 95% CI (−4.81, −2.24)]. The ranking results showed that EWST ranked 1st, acupuncture ranked 2nd, SP ranked last (Figure 3B2).
Four studies provided the long-term outcomes. The results showed that acupuncture had a significantly lower pain subscore than that of SP [MD = −3.89, 95% CI (−6.71, −1.08)]. No obvious differences were detected between EWST and acupuncture (Table 2).The ranking results showed that acupuncture was the best, followed by EWST and SP (Figure 3B3).
Network Meta-analysis of Urine Subscore
Four studies with 172 patients reported the short-term (<4 weeks) urine subscore EWST and acupuncture had lower subscore than SP [ESWT MD = −2.43, 95% CI (−5.34, 0.47)]; acupuncture MD = −1.46, 95% CI (−4.35, 1.42)]. There were no significant differences between EWST and acupuncture (Table 2). The results of ranking plots were as follows: ESWT was the best, followed by acupuncture and SP. These results are presented in Figure 3C1. Eight studies of included studies reported mid-term (8-12w) outcomes. Compared with SP, EWST had an obvious lower urine subscore [EWST vs. SP: MD = −2.53, 95% CI (4.74, −0.33)]. The difference between acupuncture and SP were not statistical. In addition, no significant difference was found between EWST and acupuncture (Table 2). The results of rank probabilities were as follows: ESWT, acupuncture and SP (Figure 3C2).
Four studies with 263 patients described the outcome of long-term urine subscore. Acupuncture was associated with lower urine subscore than SP [MD = −4.32, 95% CI (−7.84, −0.79)]. There were no significate differences between EWST and acupuncture. The ranking results showed that acupuncture was better than EWST (Figure 3C3).
Network Meta-analysis of QoL Subscore
Four studies including 172 patients described the short-term QoL subscore. The subscore of SP was significantly higher than that of EWST [ESWT vs. SP: MD = −0.98, 95% CI (−1.41, −0.54)] and acupuncture [MD = −2.41, 95% CI (−3.00, −1.82)]. ESWT was significantly better than acupuncture [MD = −1.44, 95% CI (−2.17, −0.70)] (Table 2). The ranking results showed that EWST was the best and SP was the last (Figure 4A1).
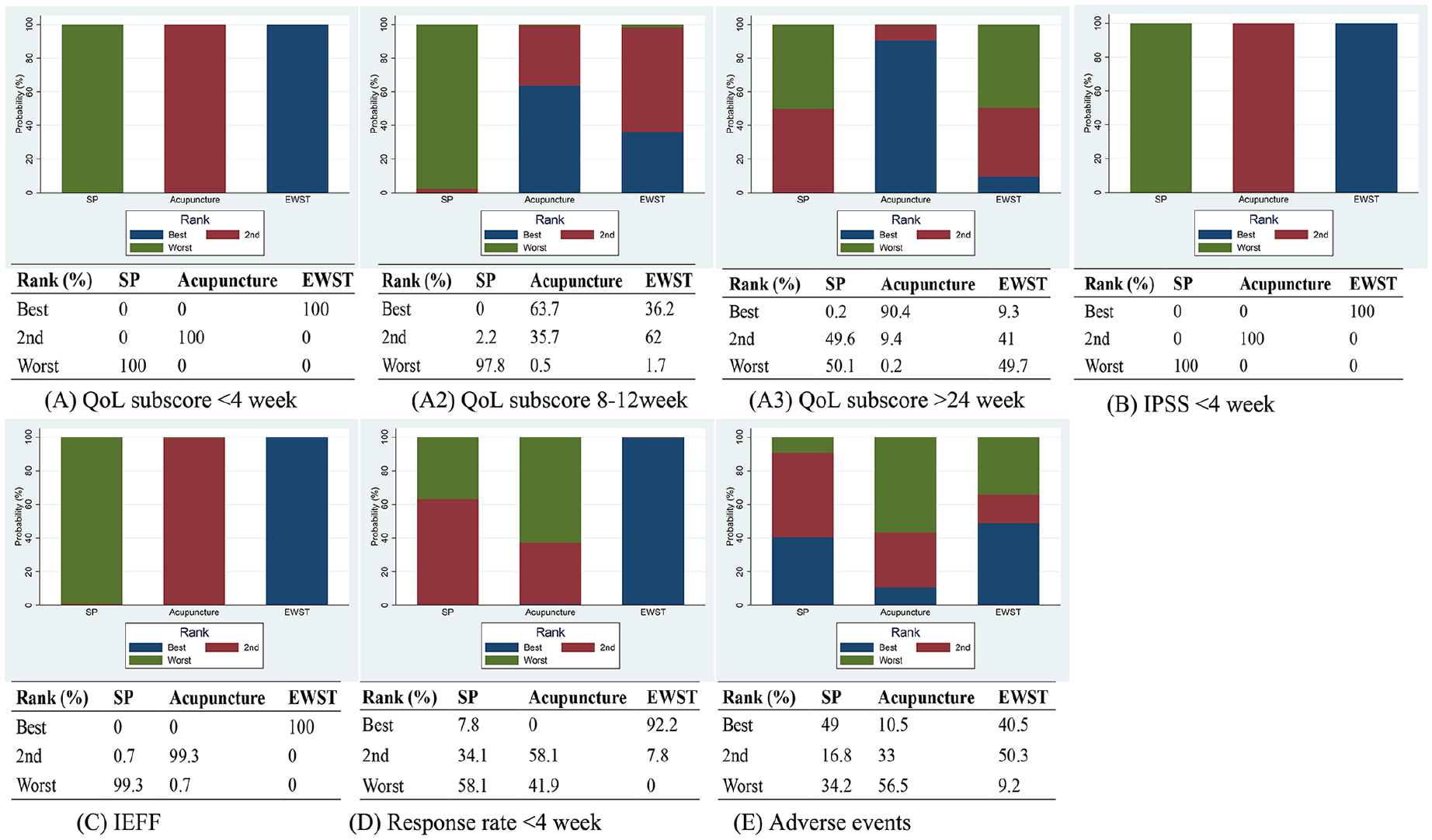
The ranking plots based on probabilities of interventions: (A1) QoL subscore <4 week; (A2) QoL subscore 8–12 week; (A3) QoL subscore >24 week; (B) IPSS <4 week; (C) IIEF; (D) Response rate; (E) Adverse events.
Four studies with 366 patients reported the mid-term QoL subscore. Acupuncture had a significant higher QoL subscore [MD = −2.08, 95% CI (−3.68, −0.48)] than SP. No significant differences were detected between ESWT and Acupuncture [MD = 0.38, 95% CI (−1.89, 2.66)] (Table 2). The ranking results showed that acupuncture was the best, followed by ESWT and SP (Figure 4A2).
There were 4 articles with 263 patients described the long term QoL subscore. The subscore of acupuncture was higher than that of SP [MD = −3.99, 95% CI (−6.94, −1.04)]. No significant differences were detected in the rest comparisons. The ranking results showed that acupuncture was the best, followed by ESWT and SP (Figure 4A3).
Network Meta-analysis of IPSS Score
Three studies with 152 patients described the IPSS score. The pooled results presented that both ESWT and acupuncture had significantly reduced the IPSS score than SP [EWST MD: −9.95, 95% CI (−12.18, −7.72); ESWT MD: −1.19, 95% CI (−2.15, −0.23)]. EWST was also significantly better than acupuncture [MD: −8.76, 95% CI (−11.19, −6.33)]. For the ranking results, EWST was the best, acupuncture was the second and SP was the last (Figure 4B).
Network Meta-analysis of Adverse Events
Four studies including 315 patients described the adverse events, which include pain at needling sites, hematoma and lower back pain near the needling site. All adverse events resolved quickly. There were no significant differences between the comparisons of acupuncture, EWST and SP for the total adverse events (Table 2). The ranking results were as follows: SP had the lowest rate of adverse events, EWST was the second lowest, and acupuncture was the last (Figure 4E).
Consistency and Convergence Analysis
Node-splitting analysis was adopted to evaluate inconsistency by comparing the differences between direct and indirect evidence. The publication bias was evaluated by funnel plots. No obvious inconsistency and publication bias were detected in all outcomes.
Discussion
Both ESWT and acupuncture have been performed in clinical practices and have been proven effective for CP/CPPS. Requiring little time or personnel cost, ESWT alters pain by interrupting the nerve impulse flow, revascularization processes, and reducing muscle tone and spasticity. Acupuncture is one of the oldest standardized neuromodulatory remedies which is commonly used in traditional Chinese medicine for chronic pain. Acupuncture at acupuncture points close to the skin may correct imbalances of energy flow then improve pain symptoms. However, the efficacy and safety differences between ESWT and acupuncture were still unclear. Our study was the first study comparing the efficacy and safety of ESWT and acupuncture in the management of CP/CPPS.
The results in our analysis showed that both ESWT and acupuncture could significantly reduce the total score of NIH-CPSI, pain subscore, urinary symptoms subscore, QoL subscore, IPSS score, improve the IIEF score for patients with CP/CPPS. Both ESWT and acupuncture didn’t increase the adverse events. In a randomized, sham-controlled trial, Sahin et al. (2015) reported that the treatment of acupuncture resulted in a significant decrease in total NIH-CPSI scores for men with CP/CPPS. Several previous studies (Franco et al., 2018; Wazir et al., 2019) also identified that the benefits of acupuncture in men with CP/CPPS. Some studies (Qin et al., 2018; 2019) revealed that acupuncture had clinically long-lasting benefits for CP/CPPS. Another study reported that a dose-response relationship between acupuncture sessions and CP/CPPS outcomes seemed to be existed (Qin et al., 2019). Prolonged acupuncture sessions were associated with less NIH-CPSI scores.
As for ESWT in the management of CP/CPPS, many studies also evaluated its efficacy and safety. Zimmermann et al. (Zimmermann et al., 2009) reported that EWST had statistically significant effects in comparison of placebo for men with CPPS in a prospectively randomized, double-blind study. A Cochrane systematic review (Franco et al., 2018) also revealed that some non-pharmacological interventions like ESWT and acupuncture were associated with decreased prostatitis symptoms and without greater incidences of adverse events. A study (Yuan et al., 2019) reported that the efficacy of low- intensity ESWT on CP/CPPS was obvious during the follow-up of 4–12 weeks, but seemed to be not significant in 24 weeks after the treatments. Another study (Zhang et al., 2019) compared the efficacy of radial ESWT with medical treatments (a-blocker and anti-inflammatory agent) in a prospectively nonrandomized controlled trial. They identified that the efficacy of radial ESWT only significant at least 3 months after cessation of treatment. A study (Al Edwan et al., 2017) reported that the efficacy of ESWT maintained without any side-effect over one year after the treatment of refractory CP/CPPS. The combination of ESWT and pharmacotherapy seemed to have improved outcomes than pharmacotherapy alone (Pajovic et al., 2016; Rayegani et al., 2020).
For the comparison of ESWT and acupuncture, our study was the first study comparing these two treatments. According to the pooled results in our study, we found that ESWT seemed to be associated with significantly better short (<4 weeks) and mid-term efficacy (<12 weeks) in the outcomes of the total score, pain subscore, urine subscore, QoL subscore than acupuncture. ESWT was also associated with significantly reduced IPSS score, improved IIEF score, higher response rates, and similar adverse event rate than that of acupuncture. However, as for the long-term efficacy (>24 w), acupuncture seemed to be better than ESWT in most of the analyzed outcomes. Therefore, ESWT seemed to be associated with better efficacy in the short- and mid-term but poorer efficacy in the long-term than acupuncture. Both ESWT and acupuncture were well tolerated and didn’t increase the adverse events.
Our study does have certain limitations. Firstly, although all of the nine included studies were randomized controlled trials, some of them were not in high quality. The number and quality of included studies may affect the summary results. Secondly, the detailed intervention of ESWT or acupuncture was not always the same in the included studies. Their efficacy was closely related to the dose and duration of treatments. However, limited by the number of included studies, dividing ESWT and acupuncture into small groups according to the dose and duration of treatments might be inappropriate to perform. Because smaller groups meant more limited data, the accuracy and reliability of results will be seriously affected by these limited data. Thirdly, the follow-up time of included studies was quite different. Some of the included studies only followed up for a short period which might influence the pooled results. Therefore, more high-quality studies are needed to evaluate the results in our study in the future.
Conclusion
Both ESWT and acupuncture were effective and well tolerated in the management of CP/CPPS. ESWT was associated with better short (<4 w) and mid-term (8-12 w) outcomes but similar long-term outcomes in total score, pain subscores, urine subscores, and QoL subscores, IPSS score, IIEF score and response rate than acupuncture.
Footnotes
Author Contributions
(I) Conception and design: Kang Y, Song P and Dong Q
(II) Administrative support: Kang Y, Song P, Dong Q and Cao D
(III) Collection and assembly of data: Kang Y, Song P, Di X, and Liu P
(IV) Data analysis and interpretation: Song P, Yanyong Lu and Di X
(V) Manuscript writing and revising: Kang Y, Song P, and Yanyong Lu
(VI) Final approval of manuscript: All authors
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by an independent academic research project of Suining Central hospital, Grant ID: 2015y19.
Ethical Statement
No-ethical approval is needed in this study as all data is from the previous publications.
Data Sharing Statement
All data in this analysis was derived from previous publications which is publicly available. The raw data can be obtained by contacting the corresponding author
