Abstract
The objective of the current study was to examine the associations between the transition to fatherhood and depressive symptoms scores among Hispanic men. Using the sample of Hispanic men included in the National Longitudinal Study of Adolescent to Adult Health, depressive symptom scores were examined from 1994 to 2008. A “fatherhood-year” data set was created that included the men’s Center for Epidemiologic Studies Depression Scale (CES-D) scores as well as residency status with the child. By regressing age-adjusted standardized depressive symptom scores, associations between mental health scores of Hispanic men and their transition to fatherhood were identified. Among the 1,715 Hispanic men, resident (n = 502) and nonresident (n = 99) Hispanic fathers reported an increase in depressive symptom scores (CES-D) during the first 5 years after entrance into fatherhood (β = 0.150, 95% CI [0.062, 0.239] and β = 0.153, 95% CI [0.034, 0.271], respectively) compared to non-fathers (n = 1,114), representing an increase of 10% for resident fathers and a 15% for nonresident fathers. Hispanic non-fathers reported a decrease in depressive symptom scores (CES-D) during parallel ages. Hispanic fathers, regardless of residency status, reported increased depressive symptoms in the first 5 years after the transition into fatherhood, a period critical in child development.
Given its effects on child development, fatherhood can be considered a social determinant of health for fathers and their children. Early father involvement in childhood is associated with better cognitive, social, and emotional outcomes in children, with both quantity and quality of father involvement being important (McWayne, Downer, Campos, & Harris, 2013; Pougnet, Serbin, Stack, & Schwartzman, 2011). Paternal depression has been reported to occur at a rate as high as 10% and the transition into fatherhood is associated with a rise in depressive symptoms among young fathers over the first 5 years of a child’s life (Garfield et al., 2014; Paulson & Bazemore, 2010). Depression in fathers has been linked to poorer parenting and consequently increased behavioral and conduct problems in children (Davis, Davis, Freed, & Clark, 2011; Edward, Castle, Mills, Davis, & Casey, 2015; Ramchandani, Stein, Evans, O’Connor, & team, 2005; Ramchandani et al., 2008).
While the importance of fatherhood has been realized over the past few decades, Hispanic fathers remain underrepresented in behavioral research despite the fact that Hispanic Americans are the fastest growing population in the United States and encompass nearly 25% of school-aged children (U.S. Census Bureau, 2016). As of 2015, 56.6 million Hispanics lived in the United States, having migrated themselves or their ancestors to the United States from the Caribbean, Central and South America, and Spain and identifying themselves as Hispanic by ethnicity and culture (Alarcon et al., 2016; U. S. Census Bureau, 2016). Hispanic men make up a unique population that faces higher socioeconomic burdens spanning from birth to adulthood. Compared to non-Hispanic white males, for instance, Hispanic males are less likely to be enrolled in early care and education programs, more likely to drop out of high school, less likely to complete a college degree or work a management or professional job, more likely to earn a lower income, and overall have poorer access to health care and insurance (Cabrera, Guzman, Turner, Malin, & Cooper, 2016; U. S. Bureau of Labor Statistics, 2017).
Despite these socioeconomic challenges, Hispanic immigrant men demonstrate lower rates of depression during their first years in the United States (without regard to fatherhood status) compared to non-Hispanics (Alarcon et al., 2016; Perreira et al., 2015). This may be in part due to Hispanics retaining certain cultural elements, such as familism and caballerismo, that offer protection against mental health disorders and poor parenting behaviors. Familism characterizes the strong attachment and connectedness of Hispanics to their family and is protective as low social support has been a proven risk factor for paternal depression (Wee, Skouteris, Pier, Richardson, & Milgrom, 2011). Caballerismo describes the social responsibility and loyalty that the Hispanic culture emphasizes for men (Perez & Cruess, 2014; Arciniega, Anderson, Tovar-Blank, & Tracey, 2008). Additional protective factors against mental disorders include lower rates of tobacco and alcohol use among Hispanic adolescents and young men compared to their white counterparts (Cabrera et al., 2016). A better understanding of how to both strengthen these protective factors as well as mitigate the aforementioned risk factors for depression among Hispanic men may lead to lower rates of depression in new Hispanic fathers and ultimately improved parenting.
A key contemporary element of understanding the bidirectional impact of fathers and children’s involvement and ultimate well-being is father’s residency status, that is, if he lives or is resident with the child. Nonresidential fathers are more likely to be younger, less educated, and more depressed than residential fathers (Fagan & Palkovitz, 2007; Huang & Warner, 2005). Fathers’ involvement with their children has widespread positive effects, ranging from academic success to emotional well-being; unfortunately, nonresidential fathers are less likely than residential fathers to eat meals together, play together, or read to their children (Jones & Mosher, 2013). Similar to nonresidential status, contact between unmarried fathers and their children declines over time, which can lead to children losing the aforementioned benefits of paternal involvement (McLanahan & Beck, 2010). Compared to non-Hispanic unmarried couples, however, unmarried Hispanic couples are more likely to live together and less likely to break up, and among the fathers, more likely to exhibit pro-social behaviors such as eating meals with their children (Jones & Mosher, 2013; McLanahan & Beck, 2010).
There is a growing body of research on the prevalence of paternal depression as well as the risk factors for the development of postnatal depression among men (Edward et al., 2015; Wee, Skouteris, Pier, Richardson, & Milgrom, 2011). While there are several cross-sectional and longitudinal studies examining depression among men in the months prior and after their child is born, this study is unique because it explores the mental health of men years prior to fatherhood. This study is also unique by focusing on Hispanics, who have many risk factors as well as protective factors against depression. An improved understanding of the trends and associations for depression in this population can lead to more focused interventions during a crucial time in child and family development.
The goal of this study therefore was to examine the transition to fatherhood for Hispanic men and its association with depression symptoms, and to also examine this within the context of fatherhood residency. The longitudinal scope and national representation of the National Longitudinal Study of Adolescent to Adult Health (Add Health) allows one to examine mental health before and after becoming a father among Hispanic men. The two-sided hypothesis that change exists between depressive symptoms and becoming a father was examined.
Methods
Study Design and Sample
The Add Health project is an ongoing, nationally representative study of the social, behavioral, and biomedical health of adolescents as they transition into adulthood. Initiated in 1994, Add Health follows the development and health trajectories of 20,745 students in grades 7–12. Three additional waves of data have been collected with the most recent data in 2008 when respondents were 24–33 years old. Of the 10,623 males included in Add Health, 1,715 (16%) identified as Hispanic. All four waves were combined to support a 19-year longitudinal analysis of the 1,715 Hispanic men that spans the ages of 14–33. The Northwestern University institutional review board approved this study.
Measures
Hispanic origins
Race/ethnicity was categorized as white, black, Asian, Hispanic, and other. Respondents selected the race/ethnicity, immigration status, and Hispanic origin with which they most identified in wave I. Hispanic participants were allowed to choose multiple Hispanic identities, but the majority chose only 1 (93%). The respondents’ parents disclosed their Hispanic identities during the parent survey taken during wave I.
Depressive symptom scores
Using the 10-item Center for Epidemiologic Studies Depression Scale (CES-D), all participants reported on their depressive symptoms at each wave of the survey. The CES-D is a screening tool for depression that has been well-validated, including in Spanish among several different Hispanic populations (Ruiz-Grosso, 2012; Sutin et al., 2013). The mean, standard deviation (SD), and quartiles for all 10 questions of the CES-D were examined across each wave; total scores were produced by summing the items and centering them to a standard normal distribution using the total sample of men in Add Health. The depressive symptoms scores had adequate internal reliability at each wave (α1 = 0.762, α2 = 0.767, α3 = 0.759, α4 = 0.811) and have been used in similar analyses (Garfield et al., 2014; Rushton, Forcier, & Schectman, 2002). An age-adjusted standardized depressive symptoms score was created from this unadjusted score to control for differences of depressive symptoms across ages along fatherhood-years. Therefore, changes in the age-adjusted depressive symptoms scores represent a relative change in a normally distributed depressive symptoms outcome over time and are comparable across all three groups throughout fatherhood-years (Garfield et al., 2014). Age adjustment helped control for the natural changes of depressive symptoms associated with getting older, and standardization allowed for inferences to be made relative to the mean level of depressive symptoms of the population.
Fatherhood status and time in fatherhood
The household roster (comprising data about the members of each participant’s household) and the live child data set (comprising data about each child for every participant) were used to determine fatherhood status. Men who had listed a biological child in the household roster or live child data set were categorized as a father. Men further indicated either residing with their child or not. Resident or nonresident father classification was held constant through all future waves. For analysis, one’s fatherhood status was coded into three categories: resident fathers, nonresident fathers, and non-fathers (men who did not list having biological children). Non-fathers were the referent group for all the analyses. A person-year file was created in which all relevant interview years of any given sample male’s longitudinal record were broken into separate data records containing the male’s unique identification number and demographic and mental health (CES-D 10). For these “fatherhood-year” records, fatherhood status was calculated on the basis of wave-specific information regarding the age of the firstborn child. For example, a participant who first mentioned a 3-year-old in wave IV was coded as having +3 fatherhood-years in wave IV and −3 fatherhood years in wave III (conducted 6 years before wave IV), −9 in wave II, and −10 in Wave 1. Data from males who were never observed to be fathers were centered at the mean age of entrance into fatherhood for all fathers in the sample, which was 23. “Fatherhood-years” for a non-father observed when the non-father was 26 are coded as +3. This allows for comparisons of fatherhood-years over a 19-year span between non-fathers and fathers and resembles other approaches to defining person-years surrounding events of interest (Huang & Warner, 2005). The term “fatherhood-years” is used for fathers and non-fathers.
Control variables
Covariates in Table 1 were coded for each person-year observation included respondents’ own parents’ income and mother’s education (wave I) and own education, physical health, employment, income, marital status, number of children, and Spanish version of the survey (each wave). Marital status was measured at entrance into fatherhood. Although there was a significant difference between resident and nonresident fathers and marital status, marital status was not collinear with fatherhood status and had minimal effect on other regression coefficients when removed (change in βi = ±0.005) and was retained.
Sociodemographics of Hispanic Fathers and Non-Fathers.

Note. aMean (SD). bN (%). cAs of 0 Fatherhood-Years.
p values derived from t-test for continuous and X2 for categorical variables.
Statistical Analysis
Mean levels of depressive symptoms scores were first analyzed by using tests of differences (i.e., 2-group t-tests, analysis of variance) over fatherhood status. Next, a generalized estimating equation (GEE) model was constructed to estimate the relationship of fatherhood status and other covariates with change in depressive symptoms over time. The GEE allowed for outcomes to correlate over time by featuring an exchangeable correlation structure. The GEE impose neither stringent assumptions on the mean, variance, and distribution of the outcome nor on the intervals of time for the longitudinal data. Missing data were handled as missing completely at random as no missingness patterns could be ascertained. Splines were created from the GEE model using 3 knots to estimate the change in depressive symptoms scores over 4 mutually exclusive time category intervals. The intervals examined for nonlinear change before and after fatherhood were predicated on a life course perspective: adolescence (defined as −9 to −4 fatherhood-years), late adolescence (–4 to 0 fatherhood-years), early fatherhood (0 to +5 fatherhood-years), and later fatherhood (+5 to +10 fatherhood-years). Using splines has the benefit of estimating linear segments of time-based functions that might be nonlinear across the entire period. Splines can be thought of as piecewise linear regression functions. Weights provided by Add Health were used to estimate the GEE, which allowed consistent parameter estimates in light of the missing data. Analyses were performed by using Stata/SE 12.1.
Results
Demographics
Of the 1,715 Hispanic males, 601 (35%) identified as fathers with 502 (83%) resident fathers and 99 (17%) nonresident fathers. Among non-fathers (N = 1,114), 49% (n = 552) identified as the child of an immigrant and 20% (n = 220) as an immigrant himself (Table 1). For resident fathers and nonresident fathers, 43% (n = 43) identified as the child of an immigrant and 18% (n = 18) as an immigrant himself. Nearly half of all subjects identified their background as Mexican (47%, n = 815).
The average age at fatherhood entrance for both resident fathers and nonresident fathers was 23 years. Ninety four percent of fathers were married (n = 293), including 57% (n = 285) of resident fathers and 7% (n = 7) of nonresident fathers, compared to only 10% (n = 107) of non-fathers. Resident fathers were more likely to have multiple children than nonresident fathers. Resident fathers were more likely to have at least some college or graduate/professional education (46%, n = 233) compared to either nonresident (33%, n = 33) or non-fathers (32%, n = 349).
Depression and Fatherhood Status
The CES-D depressive symptom score questions and descriptive statistics for the sample are presented in Table 1. Using non-fathers as the referent group in regression analysis, resident fathers reported a decrease in depressive symptoms (β = −0.145, 95% CI [−0.275, −0.015]) prior to entrance into fatherhood and an increase of depressive symptoms for the first 5 years after entrance into fatherhood (β = 0.143, 95% CI [0.055, 0.232]), as reported in Table 2. Nonresident fathers reported a statistically significant decrease in depressive symptoms (β = −0.182, 95% CI [−0.344, −0.021]) prior to entrance into fatherhood and a significant increase in depressive symptoms for the first 5 years after entrance into fatherhood (β = 0.192, 95% CI [0.037, 0.311]). In contrast, non-fathers reported a decrease in depressive symptoms during the parallel ages where fathers were in early fatherhood (β = −0.116, 95% CI [−0.193, −0.039]). While results were statistically significant for both groups of fathers from the 5- to 10-year post-fatherhood entrance period, this time period had a smaller sample size of fathers requiring inferences made about fathers in this period to be made with caution.
Age-Adjusted Depressive Symptoms Score Over Fatherhood-Years for Hispanic Men.

Note. aReferent group is non-fathers. CI = confidence interval.
p ≤ .05. **p ≤ .01.
Figure 1 demonstrates the trajectories of depressive symptom scores for the three groups. Both resident and nonresident fathers have statistically significant increases in depressive symptoms in early fatherhood compared to a decrease in depressive symptoms among non-fathers. Symptom scores decrease again in later fatherhood though the sample is smaller.
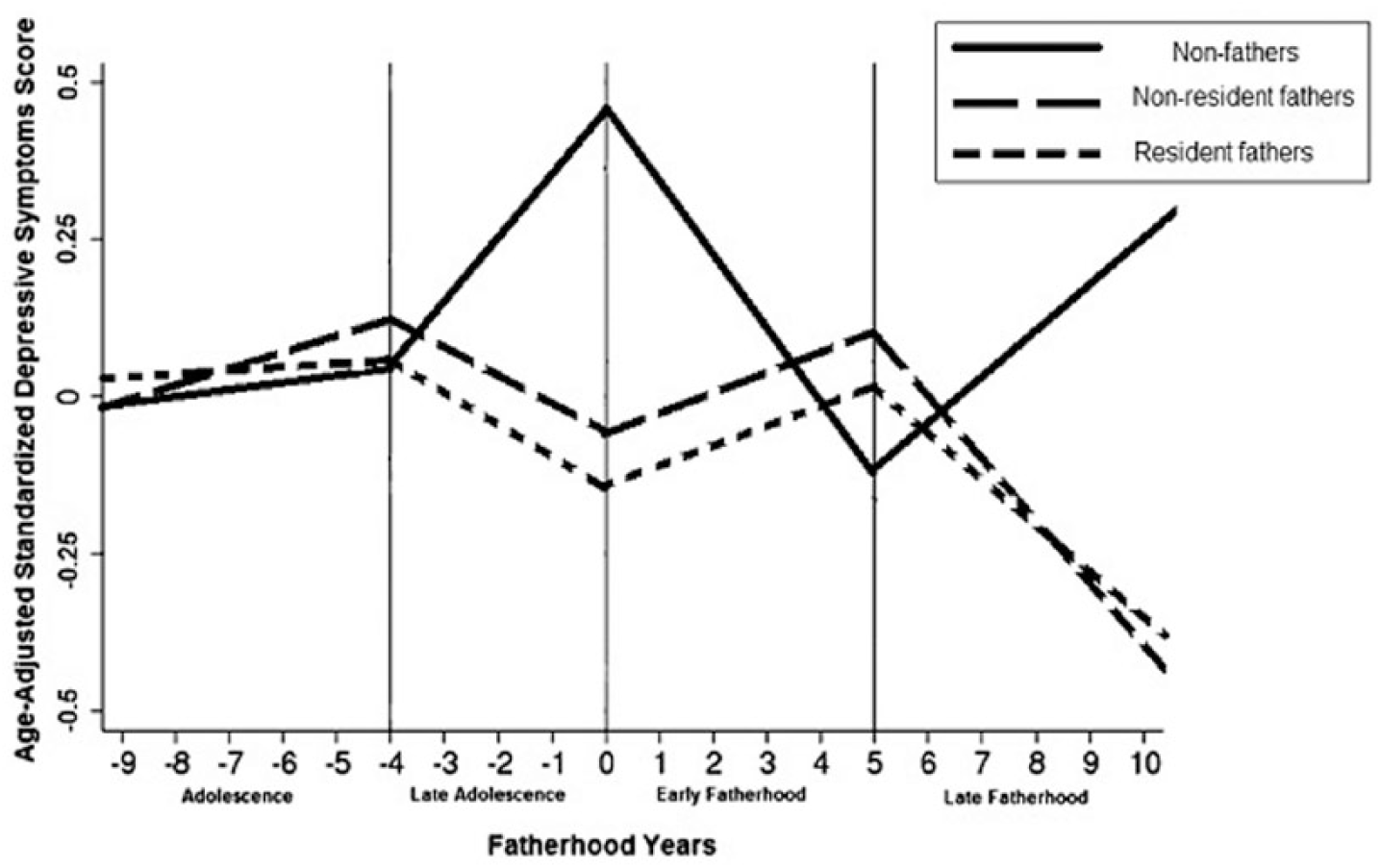
Change in depression scores across fatherhood-years among Hispanic fathers and non- fathers.
Depression and Other Covariates
Education, employment, and physical health were associated with lower levels of age-adjusted depressive symptom scores (Table 2). Maternal education, marital status, number of children, and income were not associated with differences in depressive symptoms. The Spanish language survey version was not reported to be statistically significantly different from the English version.
Discussion
This study is distinct from others as it examines the mental health changes among young Hispanic men years prior to and after a key life event, the transition to fatherhood (Edward et al., 2015; Wee, Skouteris, Pier, Richardson, & Milgrom, 2011). Both residential and nonresidential fathers demonstrated an increase in depressive symptoms in the 5 years after entrance into fatherhood. Residential and nonresidential fathers had similar increases in depressive symptoms during their transition into fatherhood with nonresidential fathers having a higher absolute depressive score. Non-fathers, however, demonstrated a decrease in depressive symptoms in the years paralleling early fatherhood.
An earlier study reported an increase of depressive symptom scores associated with the transition to fatherhood among resident fathers without regard for race or ethnicity and the current study demonstrates this association in Hispanic residential fathers in particular (Garfield et al., 2014). While the findings for depression symptoms among all nonresidential fathers may be underpowered, the current study identified that Hispanic nonresident fathers have similar rates of increase in depressive scores as residential fathers but higher absolute depressive scores over the first 5 years of fatherhood. The increase in depressive symptoms during the transition to fatherhood among Hispanic fathers in this study supports prior research that depressive symptom scores increase once men become fathers (Garfield et al., 2014; Paulson & Bazemore, 2010). While the magnitude of these changes may be small, the implications of these associations on the mental health of Hispanic men and the development and well-being of their offspring can be significant.
Earlier research demonstrates that nonresidential fathers are more likely to develop depressive symptoms than married or cohabiting fathers and the current study confirms this trend among Hispanic men specifically (Fagan & Palkovitz, 2007; Huang & Warner, 2005). Interestingly, while Hispanic couples are more likely to be cohabiting than any other group of unmarried parents (Martinez, Daniels, & Chandra, 2012), a prior study of all Add Health fathers reported similar rates of cohabiting fathers between Hispanics (83%) and non-Hispanic whites (84%) (Garfield et al., 2014). This is significant since nonresidential fathers have a higher risk of depression, less involvement with their children, and potentially less impact on their child’s development than residential fathers. Recent research has demonstrated that high quality relationships between nonresidential fathers and their children tends to positively affect children’s outcomes, most notably benefiting their social skills and relationships (Adamsons & Johnson, 2013). On the contrary, paternal depression among nonresidential fathers increases their child’s risk of behavior and emotional problems and later psychiatric disorders (Fagan & Palkovitz, 2007; Ramchandani et al., 2005; Ramchandani et al., 2008).
Hispanics in general and young men in particular face unique challenges. Debate continues regarding how acculturation influences the development of depression among Hispanic immigrants and U.S.-born Hispanics. One study reported Hispanic immigrants were at a significantly lower risk for psychiatric disorders compared with non-Hispanic Americans (Hasin & Grant, 2015); others have identified that an increase in mental illness among Hispanic immigrants occurs within years of moving to the United States, possibly due to exposure of new stressors combined with a loss of protective social and cultural factors, (Steffen & Smith, 2013; Perreira et al., 2015). Additional stressors that may contribute to higher rates of depression among Hispanics include family disruption, social or financial reasons influencing the decision to migrate, and significant change in social and gender roles (Alarcon et al., 2016). For undocumented Hispanic immigrants, a fear of deportation when seeking medical care may explain their decreased use of medical services.
However, existing research also highlights the beneficial cultural factors young Hispanic men offer to young children. Familism has been explored as a protective factor against depression among Hispanic adults by providing them with a strong sense of social support (Alarcon et al., 2016; Cardoso & Thompson, 2010). In a review of familism and its potential impact on Hispanic health, multiple studies reported associations between features of familism and healthier behaviors, including decreased substance use, less risky sexual behavior, and increased treatment adherence and use of health-care services (Perez & Cruess, 2014). Among Hispanic males in particular, caballerismo is a construct that comprises the positive aspects of the machismo, including social responsibility, loyalty, and an ability to explain one’s emotions. Hispanic men expressing more traits of caballerismo demonstrate better problem-solving and coping skills, resulting in a lower likelihood of developing depressive symptomatology (Arciniega et al., 2008). Consequently, children of these men report more positive father involvement.
Three major health implications arise from these findings as they relate to Hispanic young men. First, like their non-Hispanic counterparts, many young Hispanic men have limited or no access to health-care system (Hinton & Artiga, 2016). Even following the implementation of the ACA, only 64% of young adult Hispanic males had health insurance in 2014 compared to 85% of white men (Cabrera et al., 2016). Low-income Hispanic young men overall are less likely to have health insurance than their low-income white counterparts, illustrating that limitations to care extend beyond economic factors alone (Cabrera et al., 2016). The second implication involves identification of depressive symptoms among Hispanic young men. While the CES-D used in this study is a validated screening tool for depression in general, there are validated tools specific to postpartum depression. The Edinburg Postnatal Depression Scale (EPDS) is a 10-item scale widely used to screen for postpartum depression in women and it is validated in Spanish (Alvarado-Esquivel, Sifuentes-Alvarez, & Salas-Martinez, 2014). While the EPDS is considered a valid screen for paternal depression, (Edmondson, Psychogiou, Vlachos, Netsi, & Ramchandani, 2010; Edward et al., 2015) additional studies are needed to generalize the utility of the EPDS among all fathers, especially in those who are exclusively Spanish speaking. Finally, additional challenges exist in connecting Hispanic fathers identified with elevated depressive symptoms with mental health services. Hispanics overall are less likely to receive specialty mental health care or take antidepressant medication than their non-Hispanic white counterparts (Ault-Brutus, 2012; Wassertheil-Smoller et al., 2014). Since the lack of health insurance is one of the most important factors for untreated depression in Hispanics, policy decisions that broaden health insurance coverage and make mental health services more accessible may have the most significant impact on rates of untreated depression (Wassertheil-Smoller et al., 2014). Stigma of psychological disorders, reliance on spiritual or religious guidance, and emphasis on family rather than self all may play additional roles in the lower use of mental health services (Villatoro, Morales, & Mays, 2014).
This study has limitations. First, while the designation of Hispanic ethnicity is straightforward and accepted in the literature, there may be nuances unmeasured in these designations. Second, data collection in Add Health occurred over many years and respondents had varied ages while the point estimates were estimated to be linear. By using splines, the linear slopes provide reasonable estimates during each time interval. Third, given the average age of the sample (22.7) and follow-up only until the mid-30s, the findings cannot be generalized to older fathers, men who have been fathers for >10 years, and fathers younger than 18 years old. In fact, the number of older fathers in the sample is small. Fourth, fatherhood residency status was determined by a single entry and any changes from resident to nonresident or vice versa were not taken into consideration. Lastly, the CES-D is a validated screen among Hispanic populations that detects depressive symptoms and not clinical depression (Ruiz-Grosso, 2012).
In this longitudinal study of Hispanic males, the transition to fatherhood was associated with an increase in depressive symptoms among fathers. Compared to non-fathers, residential and nonresidential fathers demonstrated increases in CES-D scores in the 5 years following becoming a father. Paternal depression during such a crucial time of child development has been linked to long-standing effects on children’s cognitive, behavioral, and psychiatric outcomes. Improving strategies to identify and support Hispanic fathers are key as young Hispanic men are less likely to have health insurance and to seek mental health services. Prioritizing the mental health of new Hispanic fathers and promoting direct father involvement may significantly impact the health and well-being of their children.
Footnotes
Abbreviations
Add Health= The National Longitudinal Study of Adolescent Health
CES-D =- Center for Epidemiologic Studies Depression Scale
GEE =- generalized estimating equation
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by an NIH grant #K23HD060664 to CFG from the Eunice Kennedy Shriver National Institute for Child Health and Development.
