Abstract
Latino day laborers (LDLs) are at elevated risks for disease and injury because of the environments in which they work. Despite this recognition, a comprehensive examination of factors related to LDLs’ health service use remains unexamined. Using the Andersen model, the current exploratory study examined predisposing (age, education level, location of educational training, legal status, and marital status), enabling (income, trust in medical personnel, whether the respondent has someone they consider their personal doctor, and whether their doctor speaks the same language, perceived barriers to care), and need (self-rated health, number of chronic conditions) variables to predict use of health services among a purposive sample of LDLs (N = 150). Cross-sectional data were collected in 2012 from 4 day laborer sites in Dallas and Arlington, Texas. Regression results suggest that the strongest predictor of health care use was trust in medical providers (β = .41). LDLs who were U.S legal residents (β = .21), reported multiple chronic conditions (β = .16), and had a doctor who spoke their language (β = .15) reported significantly higher levels of health care usage. In terms of barriers, not being able to pay for services (β = −.23), lacking health care insurance coverage (β = −.22), and being embarrassed or having a family member not approve of utilizing services (β = −.18) were significantly associated with lower health care usage among LDLs. These findings suggest that LDLs are faced with a number of predisposing, enabling, and need factors that comprise health care use.
Background
An understanding of factors associated with the use of health care services among underserved populations is critical in decreasing health disparities experienced by racial and ethnic minority groups in the United States. This is especially significant to Latinos who represent a growing proportion of the U.S. population (17.5%), partially due to the increase in immigration. Latinos immigrants, especially those who have limited or undocumented immigrations status, comprise 5.1% of the U.S. labor (Passel, Cohn, Krogstad, & Gonzalez-Barrera, 2014) and many of them work as day laborers. Latino day laborers (LDLs), generally comprised of undocumented immigrant men, work in the informal economy in some of the most dangerous work conditions where health and safety codes are not often enforced (Valenzuela, 2003). LDLs are also exposed to significant work and life stressors including workers’ rights abuses, poverty, and fear of deportation, which may negatively affect their health (Galvin, Wohl, Carlos, & Chen, 2015; Negi, 2011). LDLs’ hazardous work conditions compounded by marginalization and social isolation have led to disproportionately high rates of on-the-job-related injuries and fatalities among LDLs when compared with other workers in the United States (Lowry et al., 2010; Williams, Ochsner, Marshall, Kimmel, & Martino, 2010). Furthermore, LDLs have been reported to be at risk for sexually transmitted infections (Hong, Murga, Plankey-Videla, & Chavez, 2015; Organista & Kubo, 2005; Wong et al., 2003), are likely to experience chronic stress (Galvin et al., 2015; Salgado, Castañeda, Talavera, & Lindsay, 2012), and engage in unhealthy drinking(Ornelas, Allen, Vaughan, Williams, & Negi, 2015).
Despite the presence of salient risk-taking behaviors, LDLs’ health service utilization remains largely understudied. Only a handful of studies have qualitatively explored health service usage (Walter, Bourgois, Loinaz, & Schillinger, 2002) or the role of social networks in promoting health (Negi, Michalopoulos, Boyas, & Overdorff, 2013); however, a more comprehensive examination of enabling and need factors related to LDLs’ health service use remain unexamined. The only national study conducted with LDLs identified that despite high rates of work-related injury (1 in 5 days laborers suffered a work-related injury) more than half of injured day laborers did not receive medical treatment for their injuries (Valenzuela, Theodore, Melendez, & Gonzalez, 2006). The underutilization of medical services can be attributed to lack of employement-based or government-sponsored health care coverage, which means LDLs have to pay out-of-pocket for health services. Paying for services creates a financial hardship because the high costs of medical care make services unattainable for LDLs, who in general, experience deep levels of poverty with annual incomes of less than $10,000 (Galvin et al., 2015). This is further exacerbated by the fact that some employers may refuse to pay for their workers’ medical treatment and services, which may contribute to poorer health outcomes (de Castro, Voss, Ruppin, Dominguez, & Seixas, 2010; Leclere & López, 2012; Menzel & Gutierrez, 2010). Walter et al.’s (2002) ethnographic study of San Francisco’s LDLs, one of the few studies to qualitatively explore the health service use of LDLs, suggests that deportation fear (i.e., that seeking medical care may make them vulnerable to incarceration or deportation) was a major barrier to health service use.
The present study contributes to the LDL and men’s health literature by being one of the first to quantitatively use a comprehensive model of social determinants of health services use among LDLs. While it can be assumed that LDLs are not likely to use health services due to lacking health insurance coverage and their undocumented immigrant status, there has been relatively minimal exploration regarding which factors LDLs themselves indicate to be barriers to their health care utilization. Using the behavioral model of health service use (Andersen, 1995), which seeks to explicate factors associated to health service use, the present study examines the impact of predisposing variables (i.e., age, education level, location of educational training, legal status, and marital status), enabling variables (i.e., income, trust in medical personnel, whether the respondent has someone they consider their personal doctor, and whether their doctor speaks the same language, perceived barriers to care), and need variables (i.e., self-rated health, number of chronic conditions) on the use of health services by LDLs. Findings from the present study have the potential to inform community-based health interventions with this hard-to-reach population.
Behavioral Model of Health Service Use
The behavioral model of health service use postulates that using health care services are largely due to individual and social predispositions, the presence of community and personal enabling factors, and an individual’s perception of their general health (Andersen, 1995). Specifically, predisposing factors include biological features such as gender and age as well as social characteristics such as education, occupation, citizenship, and ethnicity. These characteristics are important in determining social status and a person’s ability to cope with their health problems. Enabling factors relate to community and personal resources that facilitate or deter use, such as income, health insurance coverage, having a regular source of medical care, as well as travel and waiting time. Finally, perceived need factors for care, encompass an individual’s perceptions of their own general health and whether they perceive their health issues to be critical enough to seek care (Andersen, 1995).
The behavioral model of health service use has particular application to understanding health care use among LDLs, since significant gaps exist in health and health service knowledge, which has potential negative physical health consequences among LDLs (Walter et al., 2002). Walter et al. (2002) reported that LDLs’ perceived health care needs could be influenced by their fear of driving to work and related fear that a hospital stay could lead to a loss of earnings, or even deportation. Moreover, LDLs are often placed in the stigmatized social category of “illegal aliens” (Quesada, 1999), which could predispose them against accessing health services in the United States. Exploring the significance of predisposing, enabling, and perceived need factors in LDLs’ lives is critical to understand health care–seeking behaviors among this vulnerable population. After all, in the United States, access to health care services is driven by differential access to social resources, which is often limited for vulnerable populations, such as LDLs (Andersen, Lewis, Giachello, Aday, & Chiu, 1981).
The current exploratory study examined whether predisposing variables, enabling variables, and need variables are significantly associated with health care use among LDLs. It was hypothesized that LDLs who are older, have achieved higher levels of education, received their educational training in the United States, are legal residents or citizens, and married were more likely to use health services. It was also hypothesized that LDLs who earned a higher income, professed higher levels of trust in medical personnel, had someone they considered their personal doctor, and had a doctor who spoke their same language would use more health services. It was also assumed that perceived barriers would discourage health care use. Last, it was posited that LDLs who were in poorer health and suffered from chronic conditions would use more health care resources.
Method
Procedures
This study used a cross-sectional research design. A purposive sample of LDLs (N = 150) was street recruited to participate in this study. The study eligibility criteria were as follows: (a) self-identify as either Hispanic or Latino, (b) be at least 18 years of age, and (c) actively be seeking informal or short-term contingent employment.
Data were collected face-to-face from April 2012 through July 2012 from e four popular day laborer sites in Dallas and Arlington, Texas. The first author and three bilingual/bicultural research assistants carried out the data collection. All research assistants were trained for 2 hours on culturally responsive data collection procedures. The survey questionnaire was translated to Spanish using procedures outlined by Marin and VanOss Marin (1991). Specifically, the research team members first carried out all translations independently. Next, the group consensually modified the survey items to best meet linguistic and cultural equivalence. Pilot testing with 25 LDLs in Arlington, Texas, was conducted to further maximize the face validity of the questionnaire. Their responses were not included in the current analysis.
Surveys were self-administered with an option of reading verbatim of the survey offered to all participants to ensure that respondents with literacy concerns were not discouraged from participating. Roughly 40% of the participants opted for the oral reading. No significant differences in health care utilization were identified between respondents who had the survey orally read to them compared with those who completed the survey on their own. Written informed consent was obtained from all participants. Participants were given a $20.00 research honorarium. The institutional review board at the University of Texas at Arlington approved the protocols in order to ensure minimal risk to study participants.
Instruments
Dependent Variable
The health care utilization index dependent variable was a sum of three single items previously used in the National Health Interview Survey (Centers for Disease Control and Prevention, n.d.). Each item asked participants to report how many times he has visited a health clinic, doctor, and emergency in the past 12 months. The health care utilization index had a high internal consistency (Cronbach’s α = .87).
Predisposing Variables
Several individual sociodemographic characteristics were collected: racial and ethnic origin, age, education level, location of educational training, legal status, and marital status. Ethnic origin was a single item that asked participants to state with which ethnic group they identify. Age was a continuous measure. Education was dichotomized: beyond high school diploma = 1; high school diploma or less = 0. Location of educational training was a dichotomy for respondents who were foreign-born: educated in native country = 1; educated in the United States = 0. Legal status was also dichotomized: not U.S. citizen = 0; U.S. citizen = 1. Marital status: married or partnered = 1, not partnered or married = 0. In the survey, several categories of marital status were included; however, the number of other categories that were checked off were small in number. Thus, they were dichotomized for the analysis.
Enabling Variables
The present study examined whether the following determinants provided the means for using health services: income, whether the respondent has someone they consider their personal doctor, and whether their doctor speaks the same language, and trust in medical personnel. Income was also dichotomized: 2011 income greater than $20,000 = 1; 2011 household income lower than $20,000 = 0. Whether the respondent has someone they consider their personal doctor, and whether their doctor speaks the same language were single items with dichotomous responses (1 = yes, 0 = no).
Trust in medical personnel was measured using a scale developed by Boyas and Valera (2011). The four self-report single items asked respondents to report how much trust they had for doctors who work in hospitals and clinics, nurses, social workers, and medical personnel who are not of similar race/ethnicity. These questions were answered on a 4-point Likert-type scale coded as follows: trust them not at all = 1; trust them only a little = 2; trust them some = 3; trust them a lot = 4. These three items were dichotomized: no trust and trust them only a little = 1; trust them some and a lot = 0. Cronbach’s alpha for the trust in medical personnel scale was .95.
Situational variables were presented to participants to measure perceived barriers to health care (Manos et al., 2001). These 13 single items asked participants to identify if the following were reasons for why they did not seek care: lack of transportation, lack of health insurance, could not afford to pay for services, was afraid to seek services because of immigration status or the immigration status of my family/friends, waiting time at the clinics is too long, reputation of the service providers is not good, could not take time off work, language and/or cultural barriers, did not know where to go, belief that the treatment would be ineffective, was embarrassed or my family would not approve, the service hours were inconvenient, and did not seek services due to racial or ethnic discrimination at clinic/facility.
Perceived Need Variables
Several variables were included to determine need for services: self-rated health and number of chronic conditions. Self-rated health was measured as a single-item, dichotomized variable: excellent, very good, and good = 1; poor/fair = 0. The variable on chronic conditions asked participants to check off how many conditions they had been diagnosed with diabetes, heart disease, obesity, asthma, hypertension, cancer, stroke, and liver disease. These single-item questions were derived from the National Health Interview Survey (Centers for Disease Control and Prevention, n.d.).
Data Analysis
Descriptive, bivariate, and multivariate analyses were computed using the Statistical Package for the Social Sciences 22 software program. A multiple regression model was computed to determine the influence of the predictor variables on health care utilization. Statistical significance was measured at the 95% confidence interval level.
Results
Descriptives
Univariate statistics revealed that the majority of respondents were of Mexican ancestry (n = 112; 75%). The median age of the participants was 42 years. The youngest respondent was 18 years old, while the oldest was 63 years of age. The majority of LDLs were foreign-born (n = 140, 93%) and undocumented (n = 108, 72%; see Table 1). Respondents who were foreign-born reported being in the United States, a median of 10 years. Several respondents reported being in the United States less than 6 months, while one respondent reported being in the United States for at least 42 years. Most of respondents reported having less than an elementary school education (n = 86, 57%) and of those that were foreign-born, 125 (87%) reported receiving their education in their native country. The majority of respondents earned less than $20,000 in 2011 (n = 123, 82%).
Sociodemographic Characteristics of the Study Sample (N = 150).

A majority of LDLs reported either poor or fair health assessments (66%), 34% rated their health as poor, while another 32% rated their health as fair. A majority of LDLs did not report having multiple chronic conditions (n = 102, 68%); with the most commonly reported condition being diabetes (n = 19, 13%). A total of 110 LDLs reported not visiting an emergency in the past 12 months. Overall, 85 LDLs reporting not visiting a doctor, while 74 LDLs reported not visiting a health clinic. Visiting a health clinic was the most frequently reported service use (µ = 1.23). When all three items were combined, 46% (n = 69) of the LDLs reported not using any health services in the past 12 months. The most common number of reported times visiting either a health clinic, doctor, or emergency room, combined, was three (range: 1-21). Surprisingly though, of those LDLs who reported visiting a health clinic, doctor, or emergency room, their average was 2.83 times in the past 12 months. Indeed, 25% of LDLs reported having a person they think of as their personal doctor or health care provider. Of those, only 13.5% stated that their doctor spoke the same language.
LDLs reported several barriers to health care usage (see Table 2). The most frequently reported barriers were lacking health insurance (n = 141, 94%), not being able to afford paying for services (n = 116, 77%), and waiting time at clinics (n = 103, 69%). The least perceived barriers reported were reputation of the service providers (n = 55, 37%), not seeking services due to racial or ethnic discrimination at clinic/facility (n = 57, 38%), and the belief that the treatment would be ineffective (n = 58, 39%).
Perceived Barriers to Use of Health Care Among LDLs.

Multiple Regression
The research question examined the extent to which predisposing, enabling, and perceived need factors predicted use of health service. The overall regression model was significant (F = 4.843, p = .001) and the independent variables explained 41% of the variance. With all else held constant, legal status, the sum of multiple chronic conditions, lack of health insurance coverage, could not pay for services, being embarrassed or family not approving, having a personal doctor who spoke the same language, and trust in medical providers significantly predicted health care usage (see Table 3). The strongest predictor of health care usage was trust in medical providers (β = .41). On average, LDLs who were legal in the United States also reported higher levels of health care usage (β = .21), having multiple chronic conditions (β = .16), and having a doctor who spoke the same language (β = .15) was significantly associated with higher health care usage. In terms of barriers, not being able to pay for services (β = −.23), lacking health insurance coverage (β = −.22), and being embarrassed or family not approving (β = −.18) were significantly associated with lower health care usage among LDLs.
Regression Coefficients Predicting Health Care Use Among LDLs.
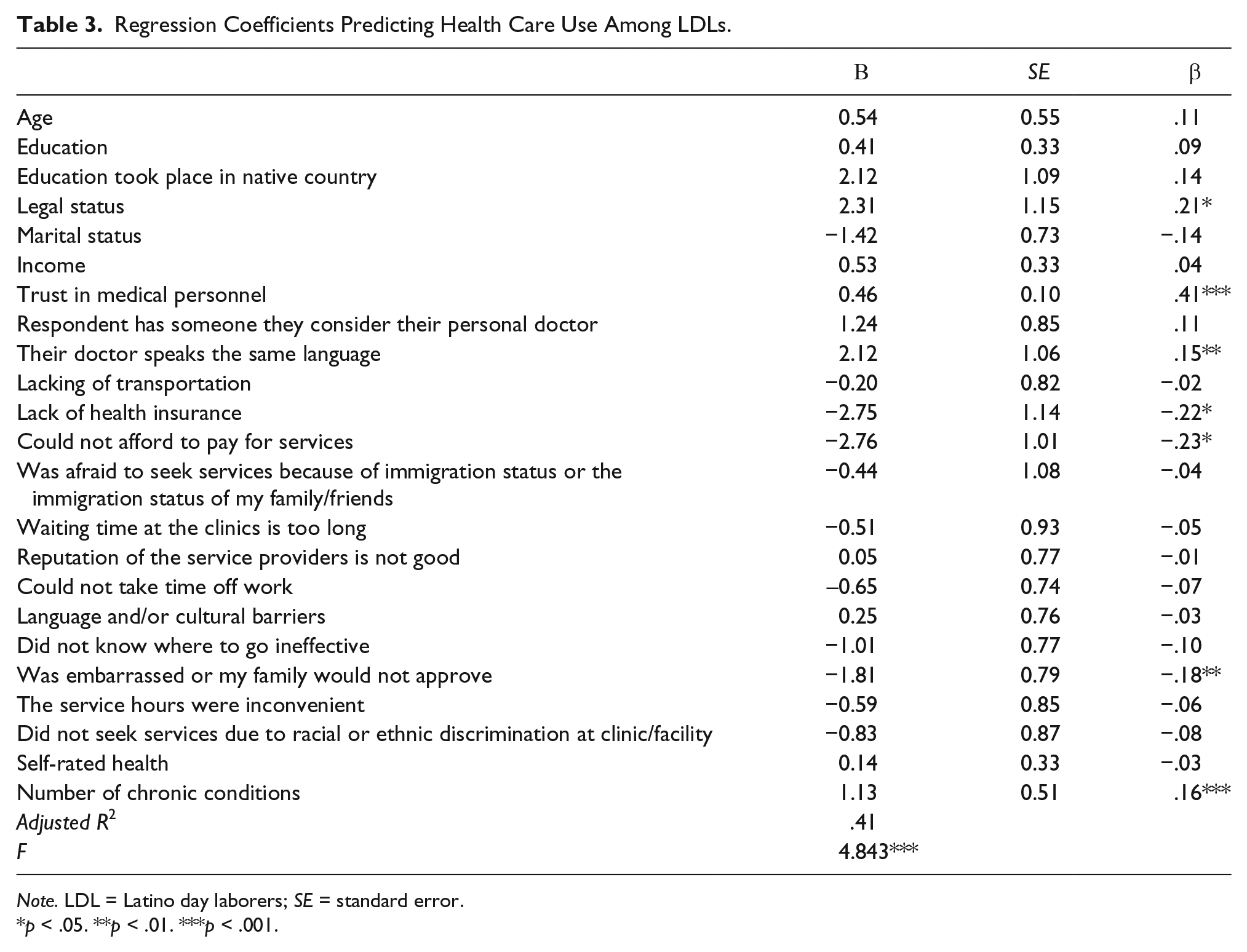
Note. LDL = Latino day laborers; SE = standard error.
p < .05. **p < .01. ***p < .001.
Discussion
The findings of this study advance the literature on health care use and men’s health among LDLs, a subpopulation of Latinos in the United States. To the best knowledge of the authors, this is one of the first studies to quantitatively document factors associated with the health care use among LDLs, which previous studies have largely attributed to their undocumented immigrant status. However, current findings reveal a rather complex picture of health care usage that does not easily fit current knowledge that LDLs do not access health care services. Contrary to previous studies (Galvin et al., 2015; Negi, 2011), approximately half of this sample of LDLs reported accessing health services in the past 12 months. Furthermore, of those that accessed health services, LDLs reported visiting a health clinic, doctor, or emergency room, an average of nearly 3 times (2.83 times) in the past 12 months. Of potential interest to public health, while 25% of the sample reported having a personal doctor or health care provider, only 13.5% of the study participants indicated that their provider spoke their language of preference. This is highly significant as health care services that do not meet the linguistic needs of racial and ethnic minorities may negatively contribute toward poorer quality of care outcomes, and subsequently, lead to health disparities and poorer health (Casado, Negi, & Hong, 2012; Ponce, Ku, Cunningham, & Brown, 2006).
The findings suggest that the sample of LDLs in the present study had higher predisposing factors associated with health care usage than one might find in the general population of LDLs. Aligned to conceptualizations postulated by previous studies (Galvin et al., 2015; Negi, 2011), undocumented status was a predisposing factor that was reported to be significant and negatively associated to health care usage. One possible explanation could be that 28% of the sample had legal immigration status, which could have increased their opportunity to access health care services. Another explanation could be the age of LDLs in the sample were significantly older (~42 years old) when compared with the average age of LDLs reported in previous studies (Valenzuela, 2003). Their comparative older age could have had an impact on perceived need factors because 33% of the sample reported one, or more, chronic conditions. In the present study, higher sums of chronic conditions was identified to be a significan predictor associated with health care usageThis finding is supported by Andersen and Newman (2005), who maintained that an illness level is judged to be the major element in whether to utilize health care services.
Among enabling factors, lack of health care insurance, inability to pay for medical services, and embarrassment or family not approving the use of health care services, were all significantly associated with health care usage. As expected, having health insurance was significantly associated to health care service usage but intriguingly, and as indicated above, approximately half of the sample accessed health services despite only 6% of them being insured. This finding could be reflective of the setting where these data were collected. Consistent with Andersen’s theory, the community itself can be a major enabling factor. Texas is a traditional immigrant settlement state with an established population of Latinos that could provide comfort to recent immigrants (Negi, Cepeda, & Valdez, 2013) and thereby ease or enable the process of using safety net programs such as health services. This is helped by the volume of available health care resources, such as community clinics and hospitals, in the Dallas–Fort Worth metroplex. Community clinics in, or near, ethnic enclaves often mitigate the health care barriers experienced by Latinos who may be unemployed, lack health insurance coverage, and/or is limited English-language proficient (Moore, Sorensen, & Bowden-Bryan, 2014). Future research should examine whether these finding can be replicated within new immigrant settlement cities where immigrants tend to be more socially isolated, few linguistically and culturally responsive health services exist, and where deportation fear might be heightened (Flippen & Parrado, 2012).
This study contributes to the existing literature of Latino men’s health by examining a subpopulation of Latinos who are predominately middle-aged and who are employed as day laborers. It is well established in previous population-based studies that young Latinos, those with less formal education, without health care insurance, those who are foreign-born with Spanish as their primary language, and who lacks legal immigration status such as citizenship or permanent resident are less likely to use health care services (Livingston, Minushkin, & Cohn, 2008). Some of the findings in this study corraborate what other studies have found; however, the findings also suggest that age and chronic health conditions may impact health service use. In addition, the issue of language has been seen as a barrier to accessing health care services and further underscored in other studies focusing on Latino health (Morales, Cunningham, Brown, Liu, & Hays, 1999; Mutchler & Brallier, 1999).
The results suggest that being embarrassed or their family would not approve the use of health care services was significantly associated with lower levels of health care service use. This is not unusual given that men, in general, are uncomfortable seeking health care. This finding may be related to notions of masculinity (Moynihan, 1998). In Western societies, including Latin America, men are socialized to put up a courageous façade and tackle illness “like a man” (Moynihan, 1998). This partially may explain why some men may become embarrassed when they experience illness as this may challenge conventional notions of masculinity and subsequently result in reluctance to seek care (O’Brien, Hunt, & Hart, 2005). Thus, it is understandable when men themselves are viewed as a major obstacle to improving men’s health (Banks, 2001). More research is recommended to further explore, if and how masculinity, or machismo, is related to LDLs’ use of health care services.
The most robust predictor of health care usage was trust in medical providers. Higher levels of trust in medical providers were associated with higher levels of health care usage. This finding may relate to core Latino cultural values including personalismo (cooperation and personal relationships), respeto (esteem for others), familismo (family orientation that often extends beyond nuclear families), and confianza (trust and social intimacy developed over time; Bordas, 2001), all of which facilitate relationship building and reciprocity (Alvarez, 1994). There is growing recognition that culture provides a context through which worldviews are shaped and may dictate how individuals manage their health problems (Andrulis & Brach, 2007; Boyas, 2013). Thus, the notion of culture should be taken into consideration when LDLs interface with the health care system. Overlooking culture may come across as an impersonal patient approach, which may function as a deterrent to utilizing services (Scheppers, van Dongen, Dekker, Geertzen, & Dekker, 2006).
While perceived discrimination by medical provider has been reported to contribute to health disparities among racial/ethnic minority populations (Lee, Ayers, & Kronenfeld, 2009), this variable was not significant in the current model. It is possible that the one item measure (“did not seek services due to racial/ethnic discrimination”) did not validly measure the construct of perceived provider discrimination. It is also possible that for LDLs that may not have a history of medical care or treatment in the United States, perceived provider discrimination may not have played a significant role in their decision to seek medical care when compared with other groups that have a history of interactions with the American health care system. It is recommended that future studies use more comprehensive and culturally tailored measures of perceived discrimination within health care settings to further advance the understanding of discrimination’s relationship to health disparities (Williams & Mohammed, 2009).
Implications for Practice
This study has several implications for practice. Specifically, the enabling factors identified to be significantly associated to the health care use of LDLs may serve as potential opportunities for culturally responsive interventions. Since trust was a significant factor in LDLs’ health care use, medical providers ought to emphasize culturally responsive best practices in building more effective “bedside” manners as this may have importance for implications for providing quality health care services and by extension, increasing treatment adherence (Williams & Mohammed, 2009). Related, the significant association between a medical provider who speaks the same language and health care usage underscores how critical it is to recruit, train, and retain doctors, nurses, social workers, and other health professionals from diverse backgrounds and who are able to speak multiple languages (Smedley, Stith, & Nelson, 2003).
The importance of language concordance between a patient and the medical provider when it comes to health care usage is aligned with this present study and previous literature (Morales et al., 1999). One study reported that when Latino patients were cared for by a Spanish-speaking primary care provider, the patient reported feeling more connected and respected, which partially explained why their experience was rated more satisfactory than those who were cared for a by non-Spanish-speaking medical provider (Kanter et al., 2009).
Moreover, the notion of masculinity is a critical concept worth exploring when working with LDLs (Moynihan, 1998). Outreach efforts should incorporate an understanding of men’s potential resistance to medical care and consider that LDLs are highly mobile (they typically move from one place to another to find work). Such mobility may make it harder for them to identify a primary care provider and/or one who speaks their language (Hoerster, Beddawi, Peddecord, & Ayala, 2010). A mobile medical care unit may be a better approach of providing health care services as this type of health care usage interventions has been previously reported to be effective in reaching underserved groups (Krol, Redlener, Shapiro, & Wajnberg, 2007).
Study Strengths and Limitations
Although there is growing literature on the health and mental health needs of LDLs (Galvin et al., 2015; Lowry et al., 2010; Negi, 2011; Williams et al., 2010), this study is the first to explore whether trust is a critical factor when using health care services among LDLs. Related, the present study has established how many LDLs have a regular health care provider or if their providers speak their same language. In addition, this study is the first to provide a comprehensive list that documents perceived barriers to accessing health care resources among LDLs. The present study also established how LDLs assess their health status and established how many of them suffer from chronic health conditions. Last, the present study documented the frequency of how often LDLs utilize health care services. All of these factors are important given that health is one of the most pressing issues that LDLs face.
Despite these strengths, a number of limitations should be acknowledged. First, the nonrandom sampling techniques used in this study limits the generalizability of the findings. Second, the overall research design does not allow for any causal inferences. Third, the current study did not include health beliefs as part of the analysis. Andersen (1995) maintains that health beliefs and knowledge shape an individual’s perception of how the social structure affects the enabling resources, perceived need, and subsequent use. Future studies should establish the health knowledge, values, and the literacy levels of this population given that those are salient factors associated with accessing health services. Fourth, a “healthy worker effect” could have affected who participated in the current study. Healthy looking workers (young and fit) were typically the ones that were hired first and often opted not to participate in the study. This might partially explain why the current sample was older, suffered from multiple chronic conditions, and utilized health care resources more often than other samples of LDLs. To establish the rates of health care usage among all LDLs, future studies should seek to survey respondents who are routinely hired for work. Fifth, LDLs were not asked specifically why they sought medical attention. Therefore, it could not be established if LDLs sought care for a work-related injury, an illness associated with the working conditions, or a common cold. Future research should distinguish the reasons for which LDLs seek care. It can then be determined the extent to which on-site workplace safety programs are needed.
Last, it should be recognized that the number of independent variables examined in the regression analysis was higher than what is typically acceptable. However, Crosby, Salazar, DiClemente, and Lang (2009) have maintained that research should be a balance between methodological rigor and the value of the issues being examined with a hard-to-reach population.
Although smaller samples may be limited in their statistical power to effectively test hypotheses and the precision of effect estimates may be less stable, a key consideration is the value of the findings in addressing gaps in the empirical literature as these gaps may be valuable for information public health policy and practice. (Crosby et al., 2009, p. 3)
This is applicable in this case where LDLs are a hidden population and many may not be willing to participate in any form of research because of fear of being identified and possibly face deportation. While the ratio of independent variables-to-sample size in a regression may be higher than normal, the findings are unique and are additive to the literature.
Conclusion
LDLs are often employed in jobs that involve a number of workplace threats, such as working with unsafe tools and equipment, exposure to dangerous chemicals, work at risky heights, lack of personal protective equipment, and little or no safety oversight (de Castro et al., 2010; Lowry et al., 2010) as well as experience psychosocial risk factors to their mental and physical health (Quesada, Hart, & Bourgois, 2011). These factors partially explain why individual health is one of the most salient challenges facing LDLs. Thus, research related to health and health care usage among LDLs is significant. Since LDLs are at elevated risks for disease and injury, the current study’s findings suggest that this is an important health disparity population. Applying Andersen’s behavioral model of health service use was a useful analytic framework in predicting and understanding health care–seeking behavior among LDLs. The findings suggest that LDLs, particularly older LDLs, are faced with a number of enabling and need factors that compromise their health care usage. The findings highlight the importance of establishing trust between LDLs and health care providers. To decrease mistrust and increase health care usage among LDLs, health structures should consider utilizing resources to ensure to recruit and retain medical personnel who can directly communicate in Spanish and can employ practices consistent with the cultural values of this population. The results also point to the importance of understanding the environment as a salient predictor of health service use. The data collected suggests that LDLs are finding opportunities to access care, despite reporting undocumented legal status. Thus, the findings underscore the urgent need for expanding the understanding on men’s health among LDLs, immigration status, and their use of health care services at the local level. These enabling and need factors can be used as prevention and intervention targets that could guide outreach and health service efforts with this population. Doing so may provide a pathway to lessen mistrust and disparities in health care usage among LDLs.
Footnotes
Authors’ Note
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
