Abstract
This study tested a modification of the Andersen behavioral model of health services use to assess the effects of predisposing factors, enabling resources, need, and personal health practices on the use of complementary and alternative medicine providers, products, and practices in the past 12 months. Data were from the 2007 National Health Interview Survey (n = 23 149 adults). Prevalence estimates and logistic regression results were weighted and adjusted for complex sample design. Overall, 16.6% used providers, 18.8% products, and 22.2% practices. There were significant associations in the expected directions between variables in each domain of the model and each type of complementary and alternative medicine use. There were also notable differences in patterns across types: for example, income was more strongly associated with use of providers. The findings support the potential usefulness of a modified health services approach to better understand differences in types of complementary and alternative medicine use.
Close to 40% of United States adults report using some form of complementary and alternative medicine in the past 12 months 1 at an out-of-pocket cost of $33.9 billion. 2 Identifying what constitutes complementary and alternative medicine continues to evolve, as do the ways in which to classify specific modalities. 3 Early research often used an aggregate measure of “any type of complementary and alternative medicine use” as the outcome of interest. Later, the National Center of Complementary and Alternative Medicine (NCCAM) organized modalities loosely according to mechanism of action and/or belief system (eg, “Alternative Medicine Systems,” “Biologically Based Therapies”), 3 and a decade of research often relied on this classification. 1,4 –7 More recently, yet another set of categories have been proposed, focusing on issues of access, time, and cost, 8 consumer decision processes, 9 or motivations for use. 10
Researchers and policy makers have articulated the need to move beyond paradigms of efficacy trials and simple, descriptive studies of characteristics of complementary and alternative medicine users. 2 The most commonly recommended model for such explanatory complementary and alternative medicine studies draw heavily from the widely accepted Andersen behavioral model of conventional health services. 11 –14 The Andersen behavioral model was developed in the early 1960s and has been applied extensively and successfully to better understand the health service behaviors in a diversity of populations. 11 –15 The original Andersen behavioral model proposed that individuals’ use of health services is a function of their predisposition to use services, factors that impede or enable use, and their need for care. Later extensions of the model included personal health practices. 14 A smaller number of investigations frame complementary and alternative medicine as health self-management and as part of “wellness lifestyle.” 4 –6,16 However, to our knowledge, few studies have empirically and comprehensively applied the Andersen behavioral model to examine use of complementary and alternative medicine providers, products, and practices in the general adult population, as we do here. Moreover, we incorporate and acknowledge complementary and alternative medicine use for wellness into our conceptual framework.
Sociobehavioral Model of Use of Complementary and Alternative Medicine Providers, Products, and Practices
Drawing on recent theoretical developments, including our own, 8,9,17,18 we have developed a sociobehavioral model of complementary and alternative medicine use. Informed by earlier work, 8 we categorize complementary and alternative medicine modalities as (a) providers, (b) products, and (c) practices. This reformulation of complementary and alternative medicine outcomes according to access, cost, and time required fits more appropriately within our health services perspective of complementary and alternative medicine use. Complementary and alternative medicine modalities are more variable than those in conventional medicine with regard to how potential users gain access to them and the time required for their use. Therefore, it is imperative that we extend and modify the Anderson behavioral model such that these ways of accessing can be examined separately. Providers include services that are delivered by an alternative health care practitioner, many of whom are licensed and regulated and more closely resemble conventional medicine than other modalities. There are potentially greater barriers to use because of minimal health insurance coverage and geographic availability. Also, the course of treatment often requires multiple visits, increasing time and cost commitments. Complementary and alternative medicine products are purchasable items or resources (eg, supplements, herbal products) that generally have lower financial or geographic barriers to use than providers. Time investments are modest. Complementary and alternative medicine practices include both individual and communal activities (eg, yoga, meditation) and may not have financial barriers but are often time-intensive and require lifestyle choices and/or changes.
Drawing from the Anderson behavioral model, our framework also proposes that complementary and alternative medicine use is influenced by 4 separate domains, each of which is discussed below. Predisposing factors include demographic variables characterizing individuals’ social placement and status, which shape how they cope with health conditions and their ability to access resources to address these conditions. They also include health-related knowledge, attitudes, and beliefs, including those specific to complementary and alternative medicine. In general, women are more likely than men to use complementary and alternative medicine. 1,19 –22 Racial and ethnic patterns are complex and depend on the complementary and alternative medicine modality considered; however, rates tend to be higher among whites and Asians. 1,5,6,20,22,23 Foreign-born individuals are less likely to use complementary and alternative medicine than US born individuals. 24 Age patterns tend to be curvilinear and use more common among middle-aged individuals. 1,19,21,25 Complementary and alternative medicine use is also greater among those with higher education. 19 –21,25 Marital status has been less commonly investigated, but married individuals tend to have lower rates of use than those who are not. 1,7,26
Enabling resources are factors that facilitate or impede use of health services. They include personal resources such as income and health insurance and structural conditions such as proximity to services. In general, higher levels of income are associated with increased complementary and alternative medicine use. 1,21,25 Most studies find either a positive or no relationship between insurance status and use. 1,19,27 However, individuals who did not receive or delayed needed conventional care because of cost are more likely to use complementary and alternative medicine. 1,25,27 –29 There is also regional variation in use with those living in the West having the highest use. 1,30
Need includes both perceived and evaluated medical need. Perceived need is how individuals view their own general functional health and how they experience symptoms. Evaluated need represents health professionals’ assessment and diagnosis regarding health status. Those who report poorer health are more likely to use complementary and alternative medicine. 1,25 Also, those who report a greater number of diagnosed health conditions are more likely to use complementary and alternative medicine. 1,19,21,25,31 –33
Personal health practices include individuals’ health behaviors and overall lifestyle. Concordant with our thesis that complementary and alternative medicine may also be used for health and wellness promotion, those who engage in “healthier” behaviors have higher rates of use. 1,21,25
Distinguishing users of complementary and alternative medicine providers, products, and practices. Because this is the first study that characterized complementary and alternative medicine use according to providers, products, and practices, proposing hypotheses directly from earlier work is not straightforward. In general, we anticipate many of the above-described patterns to also be associated with use of providers, products, and practices. However, because we have categorized complementary and alternative medicine according to access, cost, and time, we necessarily anticipate some differences across the groups. For example, since there are greater cost barriers to use providers, we expect income to be more strongly associated with their use. In contrast, income may be less important for use of practices. We are also interested in assessing the extent to which barriers to conventional care may be positively associated with each type of use. Moreover, because there are varied motivations for use, there may be differences in patterns of use across the three complementary and alternative medicine types according to health status and personal health practices.
Methods
Survey Description, National Health Interview Survey 2007
The National Health Interview Survey is an annual, cross-sectional household interview survey of the United States civilian, noninstitutionalized population. 34 The survey uses a multistage clustered sample design with oversamples of black, Hispanic, and Asian persons. Basic health information is collected on all household members and more detailed information is collected on one randomly selected adult aged 18 years or older (Sample Adult Core) in each household. The final 2007 Sample Adult response rate was 67.8%. 34 The 2007 National Health Interview Survey included a Complementary and Alternative Medicine supplement administered to the Sample Adult. 1,35 The supplement includes questions on 36 types of specific complementary and alternative medicine modalities 1 asked of 23 393 adults. Individuals who provided at least one valid response for complementary and alternative medicine therapies in each of the 3 categories we consider (see below) were included. Individuals who reported race or ethnicity as “other” (n = 244) were excluded because of small sample size and substantial heterogeneity. The final analytic sample was n = 23 149. The study was approved by the institutional review board for research subjects.
Measures
Complementary and alternative medicine use measures
Respondents were asked if they had “ever” used a given modality and if the response was “yes,” they were asked if they used that modality in the past 12 months. The use of complementary and alternative medicine in the past 12 months was defined as “recent use” and is what was analyzed here. Three separate dichotomous outcome variables were created for providers, products, and practices. Providers: Respondents were specifically asked if an alternative health practitioner provided the following services: acupuncture, Ayurveda, biofeedback, chelation therapy, chiropractic/osteopathic, energy healing, hypnosis, massage, naturopathy, traditional healers, and movement techniques. Any mention of use of any one of the above was coded as affirmative (n = 3 534). Products: These included all nonvitamin, nonmineral, natural products (eg, herbs, natural supplements) and homeopathic medicine not given by a provider. Any mention of use of any one of the above was coded as affirmative (n = 4 046). Practices: These included yoga, tai chi/qi gong, meditation, guided imagery, progressive relaxation, deep breathing, diet-based therapies (eg, vegetarian), support group, stress management techniques. Any mention of use of any one of the above was coded as affirmative (n = 4 811).
Predisposing factors
Demographics included gender, race/ethnicity (white, black, Hispanic, Asian), nativity status (US born or not), age (coded in 10-year age categories except for the youngest and oldest categories), education (less than high school, high school, more than high school), and marital status (never married, married, cohabiting, divorced/widowed).
Enabling resources
These included household income (<$34 999, $35 000-49 999, $50 000-74 999, $75 000-99 999, ≥$100 000), current health insurance status (public, private, uninsured), whether conventional care was delayed or not received because of cost (yes, no), whether there was a usual place for health care (yes, no), and United States Census Bureau geographic region (Northwest, Midwest, South, West).
Need
Health variables included self-reported health status (excellent, very good, good, fair, poor), and the number of diagnosed chronic health conditions (0, 1-2, 3-5, 6+).
Personal health practices
These included 4 standard public health indicators. Leisure time physical activity (regular activity—light or moderate activity performed at least 30 minutes 5 or more times per week and/or vigorous activity performed at least 20 minutes 3 or more times per week, some activity—less than regular, but more than none, and no activity). Smoking status (current—smokes every day or some days, former—smoked at least 100 cigarettes in life, never—smoked less than 100 cigarettes in lifetime). Drinking status (lifetime abstainer—≤12 drinks in lifetime, former—0 drinks in past year, but ≥12 in lifetime, current infrequent/light—3 or fewer drinks per week, current moderate/heavy—more than 3 drinks per week). Body mass index (underweight— less than <18.5, healthy—18.5 to 24.9, overweight—25 to 29.9, obese— more than 30).
Analysis
All analyses and estimates used the individual-level sampling weights that adjust for nonresponse and poststratification. Variance estimates were adjusted to account for complex sample design. 34 Descriptive statistics and bivariate prevalence estimates of recent use of complementary and alternative medicine providers, products, and practices were estimated using the design-based F test. Weighted logistic regression was used to estimate the effects of predisposing factors, enabling resources, need, and personal health practices on each of the three outcomes. For ease of presentation and interpretation, adjusted odds ratios are presented. All analyses were performed using Stata 12.0. 36
Results
Predisposing Factors
Overall, 16.6% reported using complementary and alternative medicine providers in the past 12 months, 18.8% use products, and 22.2% use practices (Table 1). At the bivariate level, all predisposing factors were significantly associated with use each type of complementary and alternative medicine. Women had higher prevalence of complementary and alternative medicine use than men, whites and Asians had higher prevalence rates than blacks or Hispanics, and US born individuals had higher prevalence of use than foreign born. For each complementary and alternative medicine type, middle-aged individuals reported higher rates of use than younger or older individuals. Higher levels of education were associated with higher rates of use. Last, marital status was associated with use, although the highest rate depended on type of complementary and alternative medicine.
Predisposing Factors: Percentage Prevalence of Use of Complementary and Alternative Providers, Products, and Practices, National Health Interview Survey 2007.a
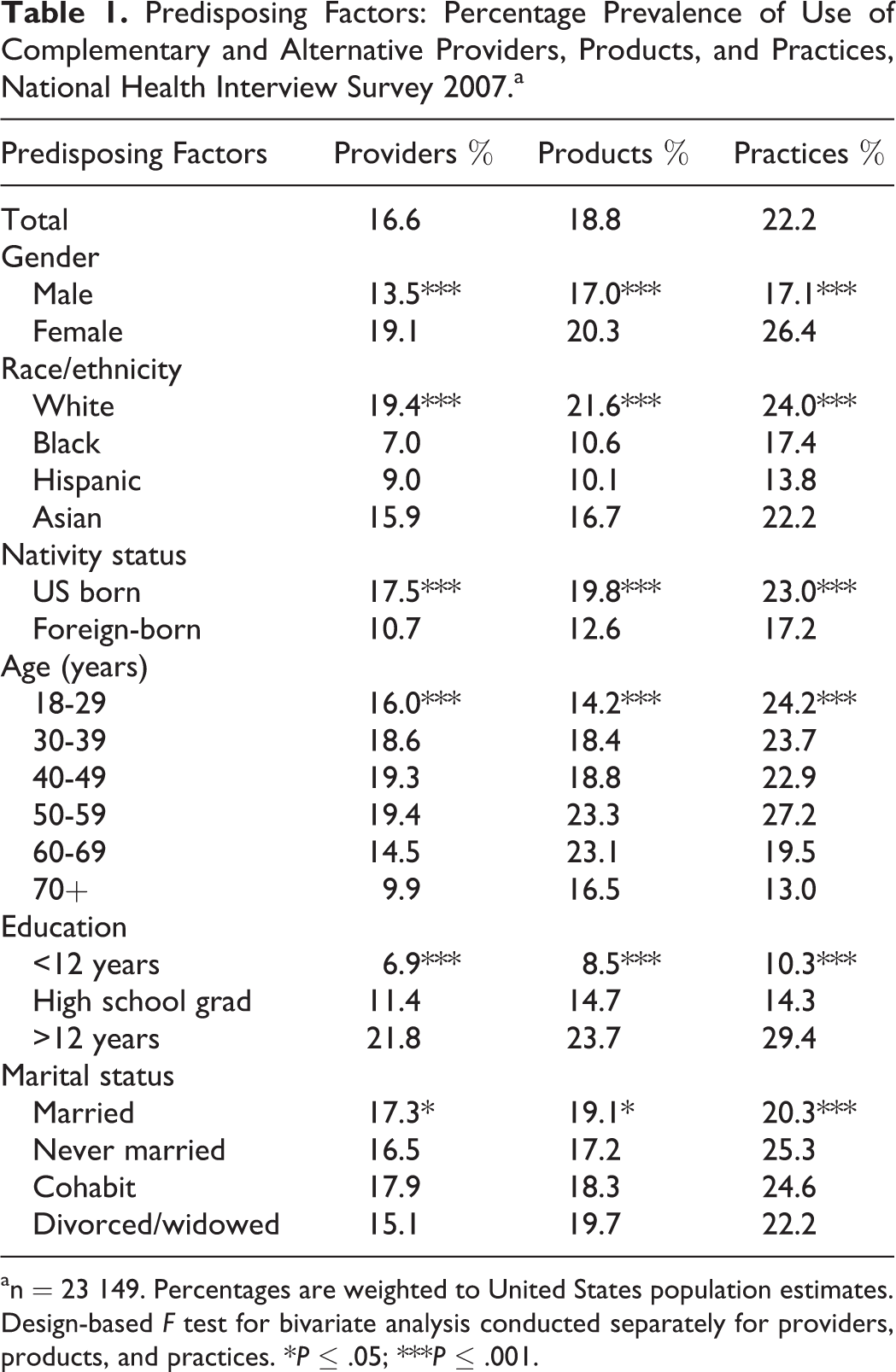
an = 23 149. Percentages are weighted to United States population estimates. Design-based F test for bivariate analysis conducted separately for providers, products, and practices. *P ≤ .05; ***P ≤ .001.
Enabling Resources
Prevalence rates of use for each type of complementary and alternative medicine significantly increased with income (Table 2). Individuals with private insurance had the highest rates of use compared to those with public insurance or who were uninsured. However, individuals who reported they delayed or did not receive conventional care because of cost also had higher rates of use. Having a usual place of care was not associated with use of products or practices, but was associated with use of providers. Those living in the West had the highest rates of use of each type of complementary and alternative medicine compared with other regions.
Enabling Resources: Percentage Prevalence of Use of Complementary and Alternative Medicine Providers, Products, and Practices, National Health Interview Survey 2007.a

an = 23 149. Percentages are weighted to United States population estimates. Design-based F test for bivariate analysis conducted separately for providers, products, and practices. ***P ≤ .001.
Need
Self-reported health status was significantly associated with use of each type of complementary and alternative medicine; in general, those reporting better health had higher rates of use than those reporting poorer health (Table 3). In contrast, individuals who reported higher numbers of diagnosed health conditions also had significantly higher rates of use of each type of complementary and alternative medicine.
Need: Percentage Prevalence of Use of Complementary and Alternative Medicine Providers, Products, and Practices, National Health Interview Survey 2007.a

an = 23 149. Percentages are weighted to United States population estimates. Design-based F test for bivariate analysis conducted separately for providers, products, and practices. **P ≤ .01; ***P ≤ .001.
Personal Health Practices
Each health practice was significantly associated with use of each type of complementary and alternative medicine (Table 4). Rates of use increased with levels of physical activity. Former smokers reported the highest rate of use of providers and products, although current smokers had a slightly higher rate of use of practices. Current drinkers had a higher rate of use, especially those reporting moderate alcohol consumption, than abstainers or former drinkers. Last, individuals with body mass index in the healthy range had the highest rates of complementary and alternative medicine use compared with those with less healthy body mass index scores.
Personal Health Practices: Percentage Prevalence of Use of Complementary and Alternative Medicine Providers, Products, and Practices, National Health Interview Survey 2007.a

an = 23 149. Percentages are weighted to United States population estimates. Design-based F test for bivariate analysis conducted separately for providers, products, and practices. ***P ≤ .001.
Multivariate Results
Predisposing factors
Women were significantly more likely than men to use each type of complementary and alternative medicine and the difference was greatest for practices (Table 5). Compared with whites, blacks and Hispanics were less likely to use each type of complementary and alternative medicine. Asians were more likely to use practices than whites. Nativity status was no longer significant. Compared with the youngest age group, the 2 oldest age-groups were less likely to use providers and practices (as were 40- to 49-year-olds). However, all age-groups except for the oldest were more likely than the youngest to use products. Individuals with higher levels of education compared to those with less were more likely to use each type of complementary and alternative medicine (although high school graduate was only marginally significant for providers). Marital status was not associated with use of providers. Compared with married individuals, those who were never married or divorced/widowed were more likely to use products and practices.
Adjusted Odds Ratios for Predisposing Factors, Enabling Resources, Need, and Personal Health Practices on Use of Complementary and Alternative Medicine Providers, Products, and Practices, National Health Interview Survey 2007.a

an = 23 149. Weighted logistic regression. † P ≤ .1; *P ≤ .05; **P ≤ .01; ***P ≤ .001.
Enabling resources
Use of providers and products was significantly higher for each income level relative to the lowest income. Income effects for use of practices were significant only for the highest income level. Compared with those with private insurance, those with public were more likely to use providers and those who were uninsured less likely to use products. Individuals who delayed conventional care because of cost were more likely to use each type of complementary and alternative medicine than those who did not delay. Those who said they received no conventional care because of cost were more likely to use providers than those who did receive care. Individuals with a usual source of conventional care were more likely to use products and practices than those who did not. Compared with living in the Northeast, individuals living in the West were more likely to use each type of complementary and alternative medicine. For products, those living in any other region than the Northeast were more likely to be users. Those living in the South were less likely to engage in practices than individuals in the Northeast.
Need
Self-reported health status was only modestly associated with use of complementary and alternative medicine products and practices. Compared with individuals with excellent health those reporting poor health were less likely to use products and those reporting good health less likely to use practices. However, increasing numbers of diagnosed health conditions was significantly associated with increases in use of each type of complementary and alternative medicine. This was especially true for practices; compared with individuals with no health conditions, those reporting 6 or more were 3.90 times as likely to be users (P ≤ .001).
Personal health practices
There were significant increases in use of each type of complementary and alternative medicine with increasing physical activity. Compared with never-smokers, former smokers were more likely to be users of each type of complementary and alternative medicine. Current smokers were also slightly more likely to be users of practices. Compared with lifetime abstainers, former drinkers and current drinkers (regardless of level) were more likely to use each type of complementary and alternative medicine. Compared to those with healthy body mass index, individuals in any other category were less likely to use providers. Those who were overweight were less likely to use products. There was no association of body mass index with use of practices.
Discussion
This is the first national study to empirically test a sociobehavioral model of complementary and alternative medicine use that reformulates complementary and alternative medicine outcomes according to access, cost, and time. Prevalence rates of recent use of complementary and alternative medicine providers, products, and practices show that each type of complementary and alternative medicine is fairly common. The multivariate analysis shows significant associations of multiple predisposing factors, enabling resources, need, and personal health practices for each of the 3 complementary and alternative medicine outcomes, suggesting that the model shows promise. Moreover, although the general patterns associated with use of each type of complementary and alternative medicine are similar, there are also important differences highlighting the utility in distinguishing complementary and alternative medicine types in this way.
Predisposing Factors
As expected, women were more likely to use all forms of complementary and alternative medicine, especially practices. These findings are in line with earlier studies examining gender differences in outcomes, most often characterized as “any type of complementary and alternative medicine” use. 1,19 –22 Women also use conventional health care more than men and tend to be more “health conscious,” factors that may also contribute to their increased complementary and alternative medicine use. 37,38 Blacks and Hispanics are less likely than whites to use each type of complementary and alternative medicine, but Asians are more likely to engage in complementary and alternative medicine practices. These race and ethnic patterns reflect not only differences in social placement but also underlying cultural beliefs about health and health care, including complementary and alternative medicine. 21,24,29 Practices such as tai chi, qi gong, and meditation are often part of many Asian cultures and are components of traditional East Asian medicine. However, a limitation of the National Health Interview Survey is that it does not include information on health and illness beliefs and values, predisposing factors known to be associated with complementary and alternative medicine use. 39,40 Thus, further studies are needed to more fully understand the observed racial and ethnic differences in use.
Age patterns depend on the complementary and alternative medicine type under consideration. Although the bivariate results confirmed the bimodal relationship often found in earlier studies, 1,19,21,25,30 the multivariate findings offer a more complex picture. When other factors are taken into account, age effects are somewhat modest for use of providers and practices with the oldest age categories less likely to use them compared with the youngest. This may be due, in part, to differences in health status and physical abilities among older adults. In contrast, all older age-groups are more likely to use products than youngest ages. People become more health conscious as they age 41 and this may explain their use of products. The effects of education and marital status are in the expected directions, 1,7,19 –21,25,26 although marital status differences are strongest for practices.
Enabling Resources
In general, higher levels of income are associated with increased use, 1,19,21,25 independent of education. However, as expected, income effects are stronger for use of providers and products than use of practices. There are greater financial barriers to providers, especially since many types of providers are not covered by health insurance. Although generally less expensive than visiting a provider, complementary and alternative medicine products also require substantial out-of-pocket payment. In fact, nonvitamin, nonmineral products accounted for $15.4 billion in out-of-pocket health expenses in 2007. 42 The effects of health insurance are modest 1,21,27 and depend on complementary and alternative medicine type. There is some support that individuals who have less access to conventional care may be substituting complementary and alternative medicine. 1,25,27,29 At the same time, those with a usual source of care are also more likely to use products and practices, suggesting some individuals may be higher users of multiple types of care, both conventional and complementary and alternative medicine. Additional research is needed to tease apart differing motivations and patterns of use of multiple types of health services.
Need
When evaluated need (operationalized as number of diagnosed chronic health conditions) is taken into consideration, self-reported health status is not associated with complementary and alternative medicine use. Although prior research has reported that each are associated with use, 1,19,25,31 –33 few considered both simultaneously, as we do here. Increasing number of health conditions is associated with significant increases in use of all types of complementary and alternative medicine. This is especially true for the use of practices among those reporting 6+ conditions. These individuals may be using complementary and alternative medicine practices to help manage their health conditions and improve quality of life.
Personal Health Practices
In general, those with healthier personal health practices were more likely to use complementary and alternative medicine, 1,21,25 although the strength of the effects depended on the particular health practice and complementary and alternative medicine type. For example, those who engaged in regular physical activity are almost three times as likely to also engage in complementary and alternative medicine practices. Both former smokers and former drinkers are more likely to use all types of complementary and alternative medicine, which may suggest these individuals incorporate complementary and alternative medicine as part of new, healthier lifestyles. Our finding that even moderate to heavy drinkers are also more likely to use all types of complementary and alternative medicine is a bit more perplexing, although has been found by others looking at use of “any type of complementary and alternative medicine.” 1,25 Other studies have found moderate alcohol consumption to be associated with positive health behaviors. 43 Additional studies are needed to more comprehensively explain the intersections of alcohol use, positive health behaviors, and complementary and alternative medicine use. Last, those with less healthy body mass index are less likely to use complementary and alternative medicine providers. Since the most common forms of therapies delivered by providers involve body manipulation (eg, massage, chiropractic), individuals with less healthy body mass index may be disinclined to use these methods.
Taken together, it appears that individuals who are less healthy (as measured by number of health conditions) and those who engage in healthier lifestyle behaviors are both more likely to use complementary and alternative medicine. These somewhat contradictory findings point to possible differences in motivation for complementary and alternative medicine use. In fact, some may use complementary and alternative medicine as part of a healthy lifestyle, 16 whereas others may use complementary and alternative medicine in conjunction with conventional medicine for treatment or to improve quality of life. 31 –33,44
Although this research is one of the first to comprehensively examine use of complementary and alternative medicine providers, products, and practices among American adults, there are limitations beyond those already discussed. The National Health Interview Survey data are generalizable to the United States adult population and has good external validity, but the cross-sectional design does not allow disentangling the timing of health conditions, personal health practices, and complementary and alternative medicine use. Also, important psychosocial measures are not present in the data, which could help to especially explain differences in predisposing factors.
Conclusions
The findings demonstrate the potential usefulness of the sociobehavioral model to assess predisposing factors, enabling resources, need, and personal health practices associated with use of complementary and alternative medicine providers, products, and practices. The results show that many of the characteristics associated with use of conventional care are also associated with complementary and alternative medicine use, underscoring the utility of a unified theoretical approach to understanding a variety of health services behaviors. However, the results also demonstrate the need to incorporate motivations for use to include health promotion and wellness.
Footnotes
Author Contributions
Dawn M. Upchurch conceptualized the article, directed the analysis, and wrote the manuscript drafts. Bethany K. Wexler Rainisch executed the analysis, managed and cleaned the data, and contributed to the writing of the manuscript drafts.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was funded by a grant to Dr Upchurch from the NIH National Center of Complementary and Alternative Medicine (K01AT002156).
Ethical Approval
This research was approved by the university’s institutional review board.
