Abstract
Chronic opioid therapy for pain management is known to induce several endocrine changes. The authors examined the effect of testosterone supplemental therapy (TST) in patients with chronic, noncancer pain undergoing opioid therapy. It was hypothesized that treatment of opioid-induced hypogonadism (OIH) can reduce opioid requirements in patients suffering from chronic pain and approve their quality of life. Over 18 months period, patients with OIH were identified in a tertiary referral pain center, Numerical Rating Scale (NRS) pain scores and daily morphine equivalent dose (MED) were the primary outcomes measured. Data were collected and comparative analysis performed between men undergoing TST versus nontreatment group. Twenty-seven OIH patients (total testosterone <300 ng/dL) were identified during the study period. TST group consists of 11 patients, while non-TST group consists of 16 patients as control cohort. Mean patient age (55 and 54.4, p = .4) and basic metabolic index (28.5 and 31.9, p = .07) in TST and non-TST groups, respectively. Mean follow-up total testosterone (ng/dL) was significantly higher after TST compared with the non-TST group (497.5 vs. 242.4 ng/dL, p = .03). Median follow-up NRS was 0 and 2 in the TST and non-TST groups (p = .02). Mean MED (mg) decreased by 21 mg in TST group and increased by 2.5 mg in non-TST group (p < .05). This study reports that treatment of OIH with TST can reduce opioid requirements in men with chronic pain as quantified by MED. It also confirms previous reports on the potential effects of OIH and that TST is effective in correcting opioid-induced endocrine abnormalities.
Introduction
Long-term use of opioids for chronic pain has increased dramatically over past two decades (Levy, Paulozzi, Mack, & Jones, 2015). An estimated 20% of patients presenting to physician offices with noncancer pain symptoms or pain-related diagnoses (including acute and chronic pain) receive an opioid prescription and about 10% have disabling chronic pain that limits work and family activities (Dowell, Haegerich, & Chou, 2016; Levy et al., 2015). In addition to the risks of tolerance, addiction, and overdose, chronic opioid use can cause endocrine abnormalities including hypogonadism. This syndrome, termed opioid-induced hypogonadism (OIH), is often associated with distressing symptoms such as reduced libido, erectile dysfunction, fatigue, hot flashes, depression, mood alterations, and reduced quality of life (QoL). Physical findings may include reduced facial and body hair, anemia, decreased muscle mass, weight gain, and osteopenia or osteoporosis. Additionally, both men and women with OIH may suffer from infertility (Daniell, 2002; Vuong, Van Uum, O’Dell, Lutfy, & Friedman, 2010).
Recent clinical data have demonstrated an increased prevalence of OIH in large population-based studies (Basaria et al., 2015). Chronic opiate therapy is known to induce several endocrine changes and alter nociception. In particular, the suppression of the hypothalamic–pituitary–gonadal (HPG) axis has been responsible for OIH through the inhibition of pulsatile gonadotropin releasing hormone which decreased the amount of luteinizing hormone, which directly stimulate Leydig cells, thus decreasing the amount of testicular testosterone produced (Aloisi et al., 2005; Elliott, Horton, & Fibuch, 2011; Smith & Elliott, 2012).
Recent clinical data suggested that testosterone supplemental therapy (TST) in patients with OIH can improve pain sensitivity, sexual desire, body composition, and aspects of QoL (Basaria et al., 2015). Despite the previously demonstrated subjective benefits, the effect of TST on the objective measurement of opioid requirements was unknown. The authors sought (a) to examine the effect of TST on chronic pain as measured subjectively with Numerical Rating Scale (NRS) and objectively with daily morphine equivalent dose (MED) and (b) to evaluate the effect of correcting OIH with TST on symptomatic hypogonadism as measured with Androgen Deficiency in Aging Males (ADAM) and sexual function with International Index of Erectile Function (IIEF-5). It was hypothesized that TST would not only improve hypogonadal symptoms but also improve pain control by decreasing opioid requirements, quantified by MED.
Method
Study Participants and Design
The study was performed with the approval and oversight of the institutional review boards of the University of California San Diego (#151169). A collaborative, retrospective review of men with OIH was conducted over a period of 18 months. None of these patients had known hypogonadism prior to initiating chronic opioid therapy. Patients with OIH were screened from a tertiary referral pain center for pain (>3 months) with NRS and MED as primary outcomes. Secondary outcomes were assessment of symptomatic hypogonadism ADAM and sexual function with IIEF-5. Appropriate evaluation and counseling was given for each patient with OIH participated in this study. Detailed discussion regarding risks, benefits, and potential complications of TST was undertaken prior to receiving TST. Patients who were symptomatic with OIH and wished to receive TST were consented and subsequently assigned to TST group, whereas symptomatic patients who did not wish to receive TST assigned to non-TST group as control cohort. Exclusion criteria included history of elevated prostate-specific antigen, erythropoiesis, breast cancer, and prostate cancer. Data collected at baseline and follow-up at 6 monthly intervals over a period of 18 months.
Biochemical Studies
All patients underwent screening for hypogonadism with total testosterone (TT), luteinizing hormone, follicle-stimulating hormone, estradiol, and human binding globulin (Table 1). Patients with symptomatic hypogonadism defined as TT less than 300 ng/dL as per the American Endocrine Society Clinical Practice Guidelines for male hypogonadism (Bhasin et al., 2010).
Baseline Demographics and Clinical Characteristics of Both Testosterone Supplemental Therapy and Nontestosterone Supplemental Therapy.

Note. IQR = interquartile range; SR = sustained release; ns = nonsignificant.
Questionnaires Evaluation
The NRS, ADAM, and IIEF-5 questionnaires are well-validated surveys that are often used to assess pain, hypogonadism, and sexual function, respectively (McCormack, Horne, & Sheather, 1988; Mohamed et al., 2010; Rosen, Cappelleri, Smith, Lipsky, & Peña, 1999). The NRS scores ranged from 0 to 10, which quantifies the pain level using verbal and visual descriptors. The ADAM questionnaire consists of 10 “yes or no” questions concerning symptoms of hypogonadism. The IIEF-5 score is the sum of the ordinal responses to the five items: no erectile dysfunction (22-25), mild erectile dysfunction (17-21), mild to moderate erectile dysfunction (12-16), moderate erectile dysfunction (8-11), and severe erectile dysfunction (5-7). An opioid dose calculator was utilized to calculate the MED in each patient of both groups. This opioid dose calculator was developed by the Washington State Agency Medical Directors’ Group to be used in conjunction with the Interagency Guideline on Opioid Dosing for chronic noncancer pain (Morse et al., 2011; http://www.agencymeddirectors.wa.gov/opioiddosing.asp.
Statistical Analysis
Statistics were generated and compared using an independent t test and chi-square tests. p Values <.05 were considered statistically significant. Delta MED and TT are defined as the difference of the MED or TT values at baseline and follow-ups for both groups.
Results
Twenty-seven OIH patients were enrolled with mean follow-up of 18 months. TST group consists of 11 patients, while non-TST group (control) consists of 16 patients. Median patient age (55 and 54.4, p = .4) and basic metabolic index (28.5 and 31.9, p = .07) in TST and non-TST groups, respectively. The majority of patients were Caucasian (91% and 88% in TST and non-TST groups, respectively; Table 1). Baseline demographics and clinical characteristics of both TST and non-TST groups were summarized in Table 1. The types of the TST offered to patients in the TST group are listed in Table 1. In patients who received TST, there were no reported adverse effects and TST was well tolerated.
In the TST group, both cervical and lumbar pain were the most common pain locations (36% for each), whereas the lumbar region was the most common location of pain in the non-TST group (81%). Median duration of pain therapy was comparable between groups (4.5 vs. 5.5 months). Methadone was the most common pain medication administrated in the TST group (45%), whereas oxycodone sustained release and morphine sulfate sustained release were the most common pain medications administrated in the non-TST group (25% for each; Table 1).
Baseline NRS was comparable between two groups (0-2), whereas median follow-up NRS was 0 and 2 in the TST and non-TST groups, respectively (p = .02). Median MED (mg) decreased by 21 mg in TST group and increased by 2.5 mg in non-TST group (p < .05; Table 2).
Baseline and Follow-up Chronic Pain Measurements With Numerical Rating Scale and Morphine Equivalent Daily (mg) in Both Testosterone Supplemental Therapy and Nontestosterone Supplemental Therapy.

Note. IQR = interquartile range; ns = nonsignificant.
Baseline ADAM and IIEF-5 were comparable between groups (8 and 10 vs. 7 and 11 in TST and non-TST groups, respectively). At follow-up, the median improvement of hypogonadal symptom for ADAM was 3 in TST group compared with 7 in the non-TST (p < .05). Likewise, the median follow-up IIEF-5 was also improved in the TST group (20) compared with non-TST group (12; p < .06). Median follow-up TT (ng/dL) was significantly higher after TST compared with the non-TST group (497.5 vs. 242.4 ng/dL, p = .03; Table 3). Patients who received TST tolerated treatment well and there was no reported adverse effects from the administration of testosterone treatment in the TST group.
Baseline and Follow-Up Hypogonadism and Sexual Function Measurement With Androgen Deficiency in Aging Males, International Index of Erectile Function, and Total Testosterone (ng/dL) in Both Testosterone supplemental Therapy and Nontestosterone Supplemental Therapy.
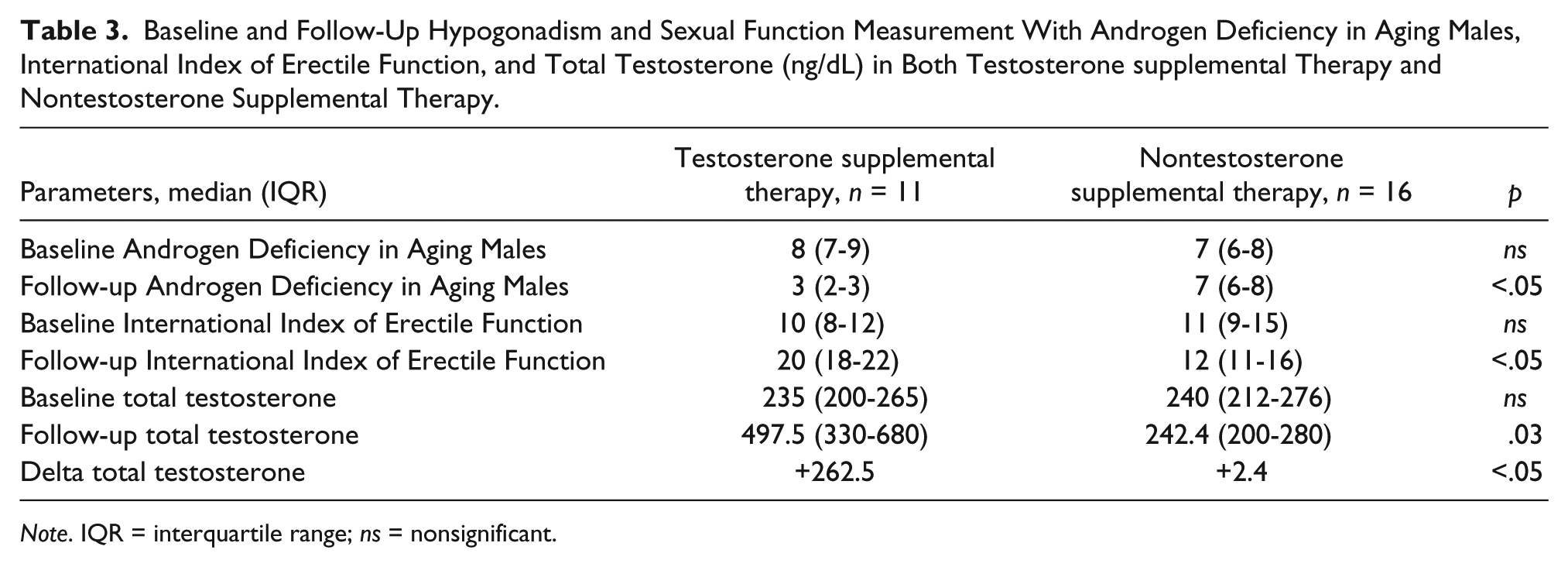
Note. IQR = interquartile range; ns = nonsignificant.
Discussion
With the substantial rise in the use of chronic opioid prescriptions to treat chronic pain, opioid dependence has become an epidemic in our society (Dowell et al., 2016; Levy et al., 2015). In 2012, health care providers wrote 259 million prescriptions for opioid pain medication, enough for every adult in the United States to have a bottle of pills (Dowell et al., 2016). This alarming pattern of increased opioid prescriptions and its serious health-related risks, including hypogonadism, has prompted the U.S. Centers for Disease Control and Prevention to publish a comprehensive evidence-based guideline for physicians who are prescribing opioids for chronic pain (Dowell et al., 2016). This guideline is intended to improve communication between clinicians and patients about the risks and benefits of opioid therapy for chronic pain, improve the safety and effectiveness of pain treatment, and reduce the risks associated with long-term opioid therapy, including opioid use disorder, overdose, and death (Dowell et al., 2016).
It is now known that chronic opioid therapy can induce several endocrine-related changes and alter nociception through the suppression of the HPG and its secreted pulsatile gonadotropin releasing hormone. This suppression causes a decrease in serum testosterone and systemic symptom resulting in OIH (Aloisi et al., 2005; Elliott et al., 2011; Smith & Elliott, 2012). There is increasing evidence suggesting that TST in those patients with OIH can reduce hyperalgesia, improve sexual desire, body composition, and aspects of QoL (Basaria et al., 2015).
Over the past decade, significant investigative efforts have been directed at exploring strategies to maintain testosterone levels in the eugonadal range while reducing pain sensitivity or hyperalgesia with the goal of decreasing MED in patients on chronic opioid therapy. There have been outcomes drawn from large randomized trials showing overall improvement of pain perception and QoL aspects including mental health, energy, and sexuality. However, there has not been clear evidence quantifying a reduction of MED in patients on chronic opioids who were treated with TST for their symptomatic hypogonadism (Basaria et al., 2015; Daniell, Lentz, & Mazer, 2006).
The current study examined the effect of TST in patients with chronic noncancer pain undergoing opioid therapy, with particular emphasis on treatment of OIH with TST to reduce opioid requirements. Both TST and non-TST groups are well matched with comparable age, ethnicity, basic metabolic index, baseline NRS, MED, ADAM, and IIEF scores (Table 1). The current result demonstrated an appropriate biochemical response to TST with significant rise in median TT by 262.5 ng/dL (p < .05), coupled with significant improvement of hypogonadal symptoms (ADAM and IIEF-5 scores) on follow-ups (p < .05). Likewise, NRS was also significantly improved in the TST group, compared with non-TST group (p = .02) and most important, an observed reduction in the delta MED by 21 mg in TST group (p < .05). These findings are consistent with published animal studies that highlighted male gonadal hormones can play a key role in inhibiting the behavioral responses to repeated nociceptive stimulation and suggested that the lower incidence of chronic pain syndromes in male rats could be caused by the presence of these hormones (Aloisi, Ceccarelli, & Fiorenzani, 2003).
In a study by Dina, Green, and Levine (2008), a panel of inflammatory cytokines has been evaluated and have shown that the presence of interleukin-6 (IL-6) and tumor necrosis factor-alpha (TNF-alpha) as inflammatory mediators produced during acute muscle inflammation, can mediate the production of chronic pain state in which subsequent exposure to inflammatory mediators produces a markedly prolonged chronic pain. The results of Dina et al.’s (2008) study identify a role for IL-6 in acute inflammatory muscle pain and as a potential target against which therapies might be directed to treat chronic pain. Basaria et al. (2015) examined the role of TST in the setting of OIH and its effect on the reduction of proinflammatory cytokines (IL-6 and TNF-alpha) but did not identify a statistically significant reduction in cytokine levels after TST.
In addition, Rubinstein, Carpenter, and Minkoff (2013) compared the effect of long-acting with short-acting opioids on testosterone suppression in patients treated for chronic pain in a retrospective cohort study of Kaiser Permanente health care system patients. This study hypothesized that there was a greater suppression of the HPG axis with long-acting opioids due to the more stable serum levels of opioids. Adding to this, the suppression of the HPA axis is short-lived in patients who are not on chronic therapy, as it has been reported that Morphine can cause a reduction of the levels of testosterone as early as 4 hours, but this testosterone suppression reversed after 24 hours (Daniell, 2002; Rubinstein et al., 2013). Despite this reversibility of OIH after cessation of treatment, most chronic pain patients require long-term opiate therapy with dose escalation over time. In the present study, the patient population received both short- and long-acting opioids.
This pilot study demonstrates that TST is associated with improvement in the QoL and reduction of opioid requirement in chronic pain patients. Clinicians should consider screening male chronic pain patients undergoing long-term opioid therapy for OIH. TST should be offered in appropriate men with the goal of not only improving hypogonadal symptoms but also decreasing opioid requirements.
The limitations of the study include a small sample size, single center design, relatively short follow-up interval, and heterogenic cohort. Future directions should be focused on delineating the underlying pathophysiology and mechanism of OIH and TST’s ability to alter nociception while affecting pain and opioid requirements (MED). Additionally, the reduction in MED after TST in chronic pain patients with OIH need to be replicated in larger randomized studies.
Conclusion
This study identifies that treatment of OIH with TST can reduce opioid requirements in men with chronic pain as quantified by MED. It also confirms previous reports on the potential effects of OIH and that TST is effective in correcting opioid-induced endocrine abnormalities. Clinicians need to be aware of the endocrinologic effects of opioid therapy and offer TST treatment when clinically indicated coupled with appropriate monitoring and follow-ups. Future study is needed to better understand the role of testosterone on nociceptive processing and transmission.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
