Abstract
The effect of marital status (MS) on survival varies according to cancer type and gender. There has been no report on the impact of MS on survival in male breast cancer (MBC). This study aims to determine the influence of MS on tumor stage at diagnosis and survival in MBC. Men with MBC ≥18 years of age in the SEER database from 1990 to 2011 were included in the study. MS was classified as married and unmarried (including single, divorced, separated, widowed). Kaplan–Meier method was used to estimate the 5-year cancer-specific survival. Multivariate regression analyses were done to determine the effect of MS on presence of Stage IV disease at diagnosis and on cancer-specific mortality. The study included 3,761 men; 2,647 (70.4%) were married. Unmarried men were more often diagnosed with Stage IV MBC compared with married (10.7% vs. 5.5%, p < .001). Unmarried men (compared with married) were significantly less likely to undergo surgery (92.4% vs. 96.7%, p < .001). Overall unmarried males with Stages II, III, and IV MBC have significantly worse 5-year cancer-specific survival compared with married. On multivariate analysis, being unmarried was associated with increased hazard of death (HR = 1.43, p < .001) and increased likelihood of Stage IV disease at diagnosis (OR = 1.96, p < .001). Unmarried males with breast cancer are at greater risk for Stage IV disease at diagnosis and poorer outcomes compared with married males.
Introduction
Male breast cancer (MBC) is rare, accounting for about 1% of all breast cancer diagnoses in the United States (American Cancer Society, 2014). The incidence of MBC is on the increase; from 0.85 to 1.42 per 100,000 populations during 1975 to 2011 (Howlader et al., 2015). Our understanding of the biologic predictors of survival in most cancers has increased but the impact of psychosocial factors such as marital status on survival in cancer patients is generally not fully understood. The relationship between marital status, stage at presentation, and survival has been studied for some cancers including prostate, colon, lung, ovarian, pancreatic, esophageal, and breast, with varying conclusions; while some studies reported a protective effect, others identified mixed or no significant effect (Aizer et al., 2013; Brusselaers et al., 2014; Cassileth, Lusk, Miller, Brown, & Miller, 1985). In addition, gender-specific impact of marital status on survival was reported in some studies (Nelles, Joseph, & Konety, 2009; Rendall, Weden, Favreault, & Waldron, 2011). Two previous studies on breast cancer, limited to female patients, reported that unmarried women (single, widowed, separated, divorced) were more likely to present with advanced disease and were at greater risk of death from breast cancer (Osborne, Ostir, Du, Peek, & Goodwin, 2005; Waxler-Morrison, Hislop, Mears, & Kan, 1991).
Generally males with breast cancer have more advanced stages at presentation and thus worse overall survival compared with females (Hill, Khamis, Tyczynski, & Berkel, 2005; Scott-Conner, Jochimsen, Menck, & Winchester, 1999). While studies have identified gender-related biological differences in breast cancer, there is limited evidence regarding the contribution of psychosocial factors to the observed more advanced presentations and poorer outcomes in male compared with female (Rayson et al., 1998; Shaaban et al., 2012). Specifically, there has been no report in the literature on the impact of marital status on survival or tumor stage at presentation in MBC. The objective of this study is to determine the influence of marital status on tumor stage at diagnosis and on survival in MBC using Surveillance, Epidemiologic, and End Results (SEER) database.
Material and Method
Patients and Study Design
This study was approved by the institution review board and included male patients 18 years or older in the SEER database who had histologically confirmed invasive breast cancer diagnosis from 1990 to 2011. The SEER program of the National Cancer Institute is a population-based cancer registry which covers approximately 30% of the U.S. population (http://seer.cancer.gov/). The period from 1990 to 2011 was selected because hormone receptor status, an important prognostic factor in breast cancer, was introduced to SEER in 1990 and at the time of this study the available data were limited to 2011 (Joslyn, Gesme, & Lynch, 1996). Patients with unknown marital status or stage of breast cancer, unknown or borderline hormone receptor status, incomplete survival data, those with a prior cancer diagnosis other than breast cancer, or those with breast cancer diagnosis at autopsy were excluded from the study. Marital status at diagnosis was classified as married or unmarried; the latter group included patients who were single, divorced, separated, and widowed. County-level median household income was determined using 2000 census tract as recorded in SEER database. Residence types were classified as metropolitan and nonmetropolitan as defined in the SEER database and used elsewhere (Klein, Ji, Rea, & Stoodt, 2011). Race was classified as White, Black, and others. Tumor, lymph node, and metastasis staging was determined as per American Joint Committee on Cancer–Sixth edition. Combined estrogen and progesterone receptor (ER/PR) status was used for analysis as this more closely represents the biologic state. SEER database includes treatment details such as surgery and radiotherapy but not chemotherapy. The primary outcomes of interest were Stage IV disease at diagnosis and cancer-specific mortality (CSM).
Statistical Analysis
The study included 3,761 patients. Baseline clinicopathological characteristics were compared using the t test and the χ2 test as appropriate. Five-year cancer-specific survival (CSS) and 5-year overall survival were estimated with the Kaplan–Meier method and the resulting curves compared with the log rank test. Multivariate logistic regression analysis was performed to determine the association between marital status and the presence of Stage IV disease at diagnosis. Cox proportional hazards regression analysis was performed to determine the effect of marital status on CSM.
In building the multivariate models, univariate analyses were performed and all variables with p values <.1 were initially included. For the Cox proportional hazards regression, age was included although the p value in the respective univariate analysis was >.1 because it is an important confounder of CSM. The final logistic and Cox proportional hazards regression models were then chosen by backward selection to achieve parsimony using the likelihood ratio test and included only variables that were necessary to achieve the best model fit. Results were expressed in odds ratio (OR) and hazard ratio (HR) with 95% confidence intervals, respectively. All reported p values were two sided and values <.05 were considered significant. Statistical analysis was done using R 3.1.1 (R Foundation for Statistical Computing, Vienna, Austria; www.r-project.org).
Results
Patient Characteristics
Baseline clinicopathologic characteristics of the patients are reported in Table 1. Of the 3,761 patients included in the study, 2,647 (70.4%) were married and 1,114 (29.6%) were unmarried. There was no significant difference in the mean age (64.8 vs. 65.0, p = .74) and residence type (metropolitan: 88.9% vs. 88.6%, nonmetropolitan: 10.7% vs. 10.5 %, p = .34) between the married and unmarried men. Unmarried males (compared with married) had significantly less median household income ($47,445 vs. $48,538, p = .006) and were more likely to present with Stage IV disease (10.7% vs. 5.5%, p < .001). There was no significant difference in grade (p = .305), histologic type (p = .165) and combined ER/PR status (p = .642) between the two groups (Table 1). Unmarried males were less likely to undergo surgery compared with the married (92.4% vs. 96.7%, p < .001).
Baseline Clinicopathological Characteristics of Patients.

Note. ER = estrogen receptor; PR = progesterone receptor.
Survival Analyses
Kaplan–Meier curves are shown in Figures 1 to 4. Unmarried men had worse CSS compared with the married (Figure 1); 5-year CSS was 77.1% and 87.8%, respectively (p < .001). Subgroup analyses by stage identified that unmarried males compared with the married counterparts had significantly worse CSS in Stages II, III, and IV but not in Stage I (Figures 2A -2D). However, unmarried men had worse overall survival in all stages of MBC (Figures 3A -3D). Survival analysis by decade of cancer diagnosis (Figure 4) identified that the observed CSS difference between the two groups was only significant in the decade after the millennium (year 2000-2009).
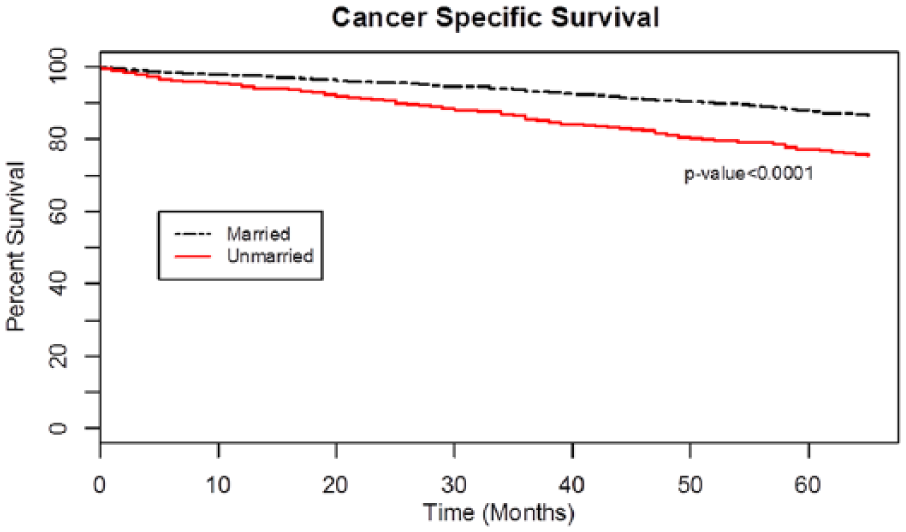
Kaplan–Meier curves of the effect of marital status on cancer-specific survival for all stages.

Kaplan–Meier curves of the effect of marital status on cancer-specific survival by stage.
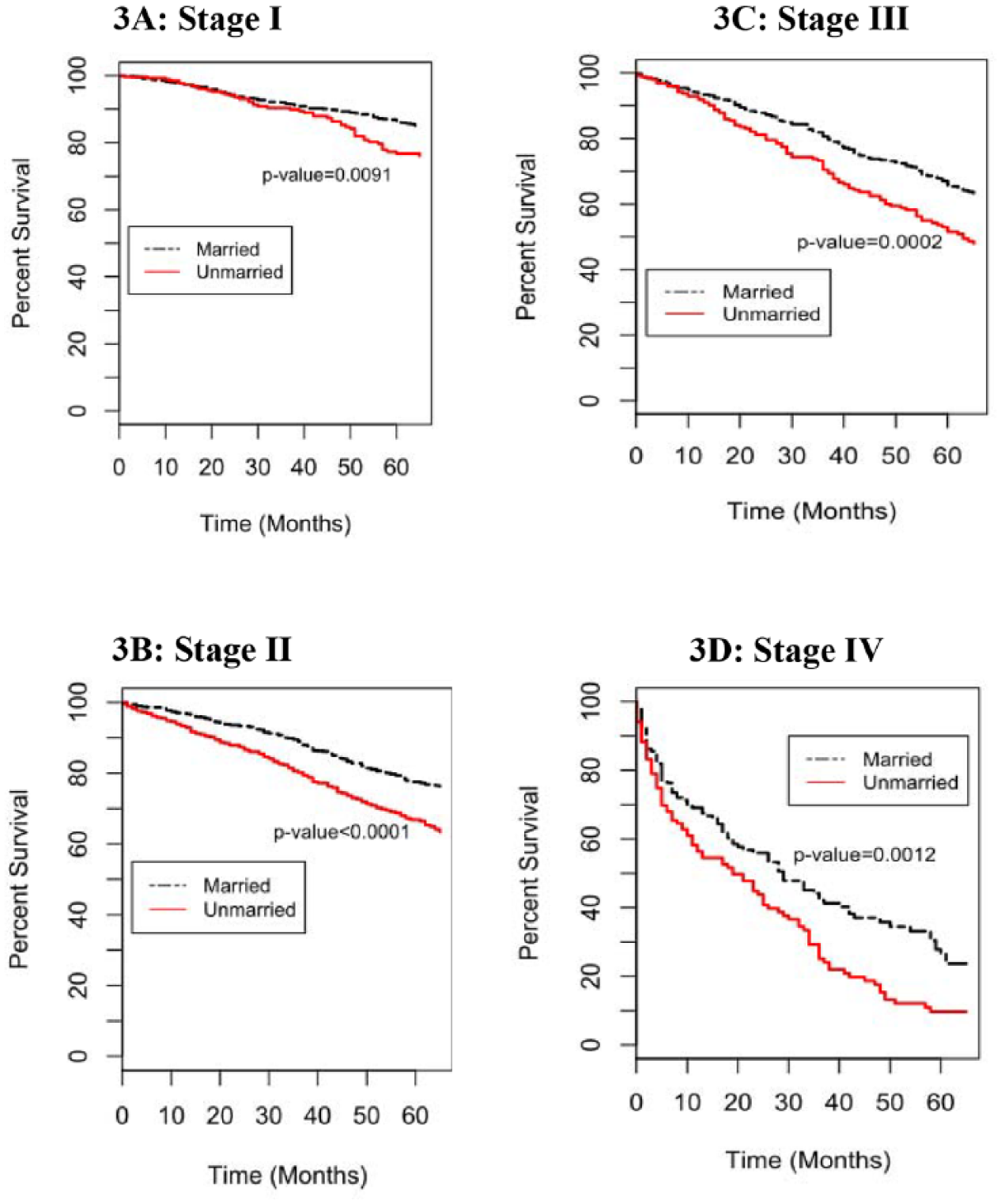
Kaplan-Meier curves of the effect of marital status on overall survival by stage.
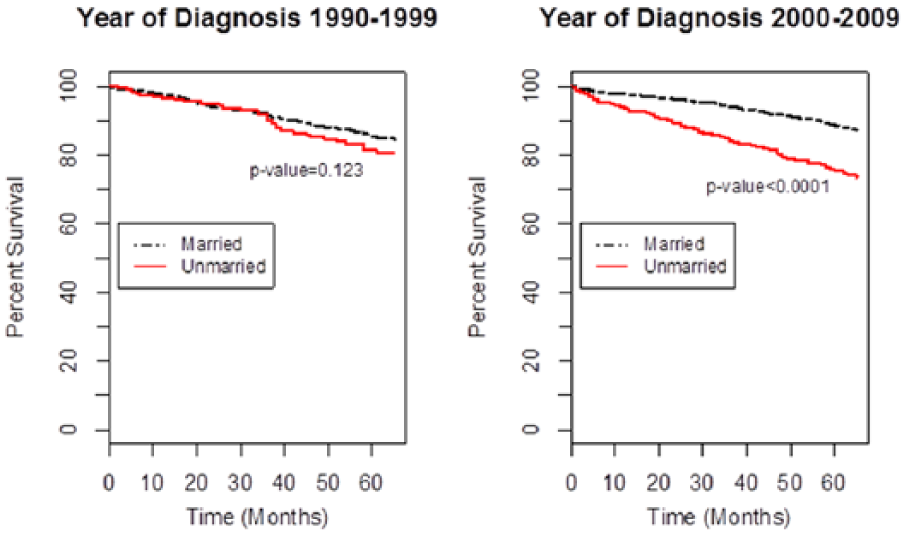
Kaplan–Meier curves of the effect of marital status on cancer-specific survival by decade.
Univariate Analyses
On univariate analysis, factors that significantly predict the presence of Stage IV disease at diagnosis include age <65 years (OR = 1.30, p = .039), African American race (OR = 1.89, p < .001), unmarried status (OR = 2.05, p < .001), moderately differentiated (OR = 2.40, p = .009) or poorly differentiated (OR = 4.47, p < .001) grade, and ER+PR− (OR = 2.20, p < .001) or ER−PR+ (OR = 2.85, p = .019) or ER−PR− (OR = 3.59, p < .001) receptor status. Factors that significantly predict worse CSM include African America race (HR = 1.96, p < .001), unmarried status (HR = 1.78, p < .001), nonmetropolitan residence type (HR = 1.29, p = .043), higher stages (Stage II: HR = 3.03, p < .001; Stage III: HR = 7.21, p < .001; Stage IV: HR = 43.44, p < .001), higher grades (moderately differentiated: HR = 2.46, p < .001; poorly differentiated: HR = 4.12, p < .001; undifferentiated: HR = 4.59, p < .001), progesterone negative receptor status (ER+PR−: HR = 2.33, p < .001; ER−PR−: HR = 1.83, p < .001) and nonuse of recommended surgical treatment (HR = 10.66, p < .001). Higher median household income (HR = 0.47, p < .001), papillary (HR = 0.16, p = 0.002) or mucinous (HR = 0.27, p = .024) histologic types and nonuse of radiation therapy (HR = 0.66, p < .001) are associated with better CSM (Supplemental files 1 and 2 available online at http://jmh.sagepub.com/content/by/supplemental-data).
Multivariate Models for Primary Outcomes
The results of the logistic and Cox proportional hazards regression models are reported in Tables 2 and 3. Being unmarried was associated with increased likelihood of Stage IV disease at diagnosis (OR = 1.96, p < .001) after controlling for age, race, grade, combined ER/PR status, and histological type. Other significant predictors of Stage IV disease at diagnosis include moderately and poorly differentiated grade and a hormone receptor status other than ER+PR+ (ER+PR−, ER−PR+, ER−PR−; Table 2).
Multivariate Logistic Regression Analysis for Predictors of Stage IV Disease at Diagnosis. a

Note. OR = odds ratio; CI = confidence interval; ER = estrogen receptor; PR = progesterone receptor.
Final model chosen by backward selection using the likelihood ratio test. bNo patients with Stage IV in these categories.
Multivariate Cox Regression Analysis for Cancer-Specific Mortality. a

Note. HR = hazard ratio; CI = confidence interval; ER = estrogen receptor; PR = progesterone receptor.
Final model chosen by backward selection using the likelihood ratio test.
Unmarried males were also more likely to die from breast cancer (HR = 1.43, p < .001) after controlling for age, race, median household income, stage, grade, combined ER/PR status, histological type, and surgical treatment. Other characteristics associated with significantly worse CSM include moderately differentiated, poorly differentiated or undifferentiated grade, progesterone negative receptor status (ER+PR−,ER−PR−), higher stages (II, III, and IV) and nonuse of surgical treatment (Table 3). Every $5,000 increment in the median household income (HR = 0.55, p = .002), age less than 65 years (HR = 0.81, p = .012), or papillary histology (HR = 0.24, p = .015) was associated with better CSM.
Discussion
The current study identified that unmarried males with breast cancer are more likely to present with Stage IV disease and have a higher risk of breast cancer-related death than their married counterparts after controlling for important socioeconomic and previously identified biological prognostic factors.
Previous studies in female breast cancer reported mixed findings (Cassileth et al., 1985; Neale, 1994; Osborne et al., 2005). Osborne et al. (2005) in a study of older women (age ≥65 years) with breast cancer reported that unmarried women are more likely to have Stages II to IV disease at diagnosis, less likely to receive definitive treatment and more likely to die from breast cancer, similar to the current findings in males. Earlier studies by Cassileth et al. (1985) and Neale (1994) did not identify any significant association between marital status and the extent of disease, therapy, and overall survival. These two studies, however, did not control for ER/PR status, an important biologic prognostic factor in breast cancer (Joslyn et al., 1996). Only a few published studies evaluated the effect of gender on the impact of marital status on survival in cancers (Aizer et al., 2013; Lai et al., 1999). Aizer et al. (2013) and Lai et al. (1999) reported a more pronounced benefit of marriage on cancer survival in males compared with females in cancers at various primary sites. Dilling et al. (2011) in a study on head and neck cancers paired marital status with gender and noted that unmarried males had the worst overall survival compared with unmarried females, married males, and married females.
The presentation of unmarried males with more advanced disease probably results from poorer access to health care (Abraham & Royalty, 2005), but this cannot be the only explanation as studies from countries with universal free health coverage also reported this trend (Ayanian, Kohler, Abe, & Epstein, 1993; Farley & Flannery, 1989; Neal & Allgar, 2005). Unmarried males may lack the important spousal encouragement (enjoyed by their married counterparts) to seek medical attention early for worrisome symptoms (Neal & Allgar, 2005). In a recent study on men with prostate cancer, Forbat, Place, Hubbard, Leung, and Kelly (2014) observed that spouses were not only involved in encouraging men to see their primary care providers, but were also active in symptom interpretation.
The underlying mechanism for the protective effect of marriage on cancer-specific and all-cause mortality is not fully elucidated, but multiple pathways are likely involved (Aizer et al., 2013; Baine et al., 2011). The dominant mechanism appears to be the psychosocial support enjoyed by the married (Baine et al., 2011). Breast cancer diagnosis is associated with significant psychological and socioeconomic stress and being unmarried is one of the strongest correlates of serious psychological distress following cancer diagnosis (Kaiser, Hartoonian, & Owen, 2010). In a study on men with colon and rectal cancers, Goldzweig et al. (2010) reported that single males (compared with married males) have significantly higher psychological distress and they observed a negative correlation between the distress and social support in married but not in single men. The reported higher level of potential support from family and friends available for single males did not translate to a reduction in psychological distress. The authors concluded that any beneficial social support received by male cancer patients from friends and family may be mediated by spousal support. The psychosocial support from the spouse may ultimately translate to less risk for depression and improved adherence to cancer treatment (Burgess et al., 2005; Goodwin, Zhang, & Ostir, 2004). Previous studies have identified unmarried status as a significant predictor of outright refusal of curative treatment, early discontinuation, and nonadherence to adjuvant therapy (Aizer et al., 2014; Hershman et al., 2010).
While unmarried males compared with married counterparts had poorer CSS in Stages II, III, and IV but not in Stage I, they have poorer overall survival in all stages of MBC. The treatment for Stages II to IV MBC involves a complex multimodal approach which requires intense psychosocial support compared with Stage I which is usually treated by surgery and adjuvant tamoxifen for hormone receptor positive tumors (Fentiman, Fourquet, & Hortobagyi, 2006; Kiluk et al., 2011). Although marriage may not have a protective effect on breast CSS in Stage I MBC, it may still be protective in other ways not related directly to breast cancer and its treatment. This finding is consistent with those from multiple population studies which reported generally longer life spans for married compared with unmarried subjects (Jaffe, Manor, Eisenbach, & Neumark, 2007; Rendall et al., 2011).
In the current study, the obtained survival benefit from marriage reached statistical significance only in the decade after the millennium (2000-2009) and not earlier; this was a decade of significant financial and psychosocial stress (Connelly, 2011). An increase in the mortality inequality over time based on marital status in developed countries has been reported in some studies (Jaffe et al., 2007; Kravdal & Syse, 2011). Although the reasons for the observed increase in the protective effect of marriage are not fully understood, the changes in social architecture of most industrialized societies over time with resultant reduction or loss of social cohesion has been cited (Beauvais & Jenson, 2002). Furthermore, studies on the past financial crises in the United States and the current one in Greece reported exacerbations of baseline health disparities during these periods (Alley et al., 2011; Kentikelenis et al., 2011).
Since unmarried males represent a high-risk group for poor outcome in breast cancer, specific psychosocial support intervention may help improve survival. It is of note that just as studies on the effect of marital status on survival in female breast cancer have mixed reports, so do studies on the implementation of psychosocial support programs. An earlier study reported a survival benefit from psychosocial support intervention in women with metastatic breast cancer but this finding was not consistently replicated in subsequent studies (Andersen et al., 2008; Spiegel, Bloom, Kraemer, & Gottheil, 1989; Spiegel et al., 2007). A recent Cochrane review identified benefit of psychological intervention on survival at 12 months, but not at 5 years, in women with metastatic breast cancer (Mustafa, Carson-Stevens, Gillespie, & Edwards, 2013). It is possible that such psychosocial intervention programs as used in these studies may not fully replicate all the support domains provided by marriage or that some subgroups of patients may still benefit (Cunningham et al., 1998).
The relative rarity of MBC limits the possibility of a prospective study with adequate sample size and power to detect any impact of marital status on stage and survival. The use of the SEER database in this study helped overcome the sample size limitation.
The current study has some limitations which need to be considered in the interpretation of the findings. The SEER database captures marital status at cancer diagnosis only; changes in marital status following diagnosis are not tracked. However, a previous study evaluated changes in marital status following cancer diagnosis and observed no significant change over time (Brusselaers et al., 2014). Second, it is possible that some men reported as unmarried in SEER database may be cohabiting with a partner and thus enjoying psychosocial supports similar to their married counterparts. However, the resultant effect is likely an underestimation of the benefits of marriage on the primary outcomes. Third, data on chemotherapy treatment are not available in the SEER database and a control for this treatment modality was not possible. Last, data on individual household income are not recorded in the SEER database and the county-level data applied in this study may not closely match individual incomes.
Despite these limitations, the current study identified that unmarried patients with MBC are more likely to present with Stage IV disease and are at a higher risk of death from breast cancer compared with the married. It is known that males with breast cancer have worse survival compared with females due to presentation with more advanced disease (Hill et al., 2005; Scott-Conner et al., 1999), but unmarried males are at an even greater risk for poorer outcomes. They may represent an important target group for supportive intervention. There is a need for a prospective, multicenter study in MBC to verify the findings of the current study and to test the implementation of a comprehensive psychosocial support program tailored to the needs of unmarried males with breast cancer.
Footnotes
Acknowledgements
The authors thank McLaren Foundation for their support for this project.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
