Abstract
This study aimed to investigate the effects of testosterone replacement therapy (TRT) on lower urinary tract symptoms (LUTS) in men with late-onset hypogonadism (LOH) and to identify parameters predicting the efficacy of TRT in improving LUTS. This study included 60 consecutive Japanese men who were diagnosed with LOH and subsequently received TRT between January 2009 and December 2014. In this series, 250 mg of testosterone was injected intramuscularly every 3 or 4 weeks in all patients. The following parameters were retrospectively reviewed: body mass index (BMI), Aging Male Symptom (AMS) score, International Prostate Symptom Score (IPSS), International Index of Erectile Function–5 (IIEF-5) score, residual urine volume, prostate volume, serum levels of the prostate-specific antigen (PSA), and total- and free-testosterone levels before and 6 months after TRT. No significant differences were observed in BMI, residual urine volume, or prostate volume between surveys before and after TRT. The AMS score, IPSS, and IIEF-5 score were significantly improved and significant increases were noted in the serum levels of PSA and total- and free-testosterone levels after TRT. An analysis of IPSS subscores documented the significant improvement in storage symptom scores, but not in voiding symptom scores after TRT. Multivariate analyses of parameters assessed in this study identified the pretreatment AMS score, posttreatment IIEF-5 score, and prostate volume as independent predictors of improvements in IPSS following TRT. This study revealed that TRT appeared to have considerable therapeutic effects on LUTS, particularly on storage symptoms, in men with LOH.
Introduction
The worldwide population is aging and increases in the incidences of age-related health care issues have been documented. Testosterone deficiency is currently attracting wide attention because of the high prevalence of hypogonadal symptoms in aging males such as fatigue, lack of physical strength, loss of libido, erectile dysfunction, depressed mood, and visceral obesity (Laughlin, Barrett-Connor, & Bergstrom, 2008; Lunenfeld, Saad, & Hoesl, 2010; Tivesten et al., 2009). Various clinical symptoms and important pathological states observed in men have been associated with low testosterone levels, including hypertension, hypercholesterolemia, diabetes mellitus, osteoporosis, and ischemic heart disease (Bassil, Alkaade, & Morley, 2009). An international consensus document recently published provides guidance on the diagnosis, treatment, and monitoring of late-onset hypogonadism (LOH) in men (Nieschlag et al., 2005).
Several studies have reported that testosterone replacement therapy (TRT) has the ability to normalize testosterone levels and improve a number of hypogonadal symptoms in men with LOH (Kava, 2014; Wang et al., 2009). TRT has been widely performed for men with LOH and is regarded as the standard therapeutic strategy for these patients. A previous study also identified the efficacy of TRT for aging Japanese men diagnosed with LOH, exhibiting comprehensive improvements in their symptoms following the introduction of TRT without any severe adverse events (Okada, Yamaguchi, Chiba, Miyake, & Fujisawa, 2014). TRT is assumed to aggravate symptoms associated with benign prostatic hypertrophy (BPH) because prostate growth is dependent on the presence of androgens, which play crucial roles in the development of BPH. Information to suggest that TRT has a negative impact on lower urinary tract symptoms (LUTS) in men with LOH is limited (Nieschlag et al., 2005; Ko, Moon, & Moon, 2013). Based on these findings, the clinical outcomes of 60 consecutive Japanese men with LOH who received TRT were retrospectively assessed with a focus on its impact on changes in LUTS in this cohort of patients.
Method
Sixty consecutive Japanese men who were diagnosed with LOH and subsequently received TRT for at least 6 months between January 2009 and June 2014 were enrolled. Informed consent was obtained from all patients prior to their participation in this study. In this series, the diagnosis of LOH and indication for TRT were determined according to the Clinical Practice Manual for Late-onset Hypogonadism Syndrome in Japan (Namiki et al., 2008). Exclusion criteria for TRT included prostate cancer, a serum prostate-specific antigen (PSA) level ≥4 ng/mL, polycythemia, severe liver dysfunction, and/or a previous history of treatments for LOH. After the diagnosis of LOH, testosterone enanthate (250 mg every 3 or 4 weeks) was used as TRT. Administration was by intramuscular injection in all patients.
In this series, blood tests were performed at baseline and 6 months after the initiation of TRT to measure PSA levels and total- and free-testosterone levels. Ultrasound sonography was conducted to measure residual urine and prostate volumes. Body mass index (BMI) was also recorded. In addition, Aging Male Symptom (AMS) scores were investigated to evaluate changes in the health-related quality of life (HRQOL) status of these men. The urinary symptom status and erectile function were analyzed using the International Prostate Symptom Score (IPSS) and International Index of Erectile Function–5 (IIEF-5) score, respectively, before and 6 months after the introduction of TRT (Barry et al., 1992; Rosen, Cappelleri, Smith, Lipsky, & Peña, 1999). One week after testosterone injection, blood tests were performed and patients filled out the questionnaires. Regarding the evaluation of IPSS, storage and voiding symptom scores were defined as the sum of items of frequency, urgency, and nocturia and that of those of intermittency, a weak stream, and straining, respectively. The following classification was used based on the sum of all 7 items: mild, total score ≤7; moderate, total score 8 to 19, and severe, total score 20 to 35.
All statistical analyses were performed using Statview 5.0 software (Abacus Concepts, Inc., Berkley, CA), and p < .05 was considered significant. Differences between several parameters were compared using Wilcoxon’s signed-rank test. A logistic regression analysis was used to determine the relationships between several parameters and changes in IPSS.
Results
The baseline characteristics of the 60 Japanese men included in this study and treatment results with TRT for 6 months are summarized in Table 1. No significant changes were observed in BMI, residual urine volume, or prostate volume between surveys before and 6 months after the initiation of TRT. However, TRT for 6 months resulted in statistically significant improvements in the AMS score, total IPSS score, and IIEF-5 score from baseline, while statistically significant increases in the serum levels of PSA and total- and free-testosterone levels were noted after TRT for 6 months.
Baseline Characteristics and Treatment Results.

Note. BMI = body mass index; AMS = Aging Male Symptom; IPSS = International Prostate Symptoms Score; IIEF-5 = International Index of Erectile Function–5; PSA = prostate-specific antigen.
The subscale scores of IPSS for all patients and those according to the status of LUTS are presented in Table 2. In the assessments for all patients, the storage symptom score was statistically significantly improved 6 months after the initiation of TRT. However, no significant difference was noted in the voiding symptom score between surveys before and after TRT. As reported in Table 2, when evaluated by dividing 60 patients into 34 with mild LUTS and 26 with moderate or severe LUTS, no significant difference was observed in total IPSS score, storage symptom score, or voiding symptom score in men with mild LUTS between surveys before and after TRT. In men with moderate to severe LUTS, TRT resulted in clinically significant improvements in total IPSS score and the storage symptom score, but voiding symptom score was not statistically improved after TRT.
Changes in IPSS According to the Degree of LUTS 6 Months After TRT.

Note. IPSS = International Prostate Symptom Score; LUTS = lower urinary tract symptoms; TRT = testosterone replacement therapy.
Univariate and multivariate logistic regression analyses were conducted to assess the contribution of several factors to improvements in the IPSS score by TRT in LOH patients (Table 3). The univariate analysis identified the pretreatment AMS score, posttreatment IIEF-5 score, and pre- and posttreatment prostate volumes as significant predictors of improvements in IPSS after TRT. Furthermore, the pretreatment AMS score, posttreatment IIEF-5 score, and posttreatment prostate volume appeared to be independently associated with improvements in IPSS in the multivariate analysis.
Univariate and Multivariate Analyses of Associations Between Various Parameters With the Improvement of IPSS 6 Months After TRT.
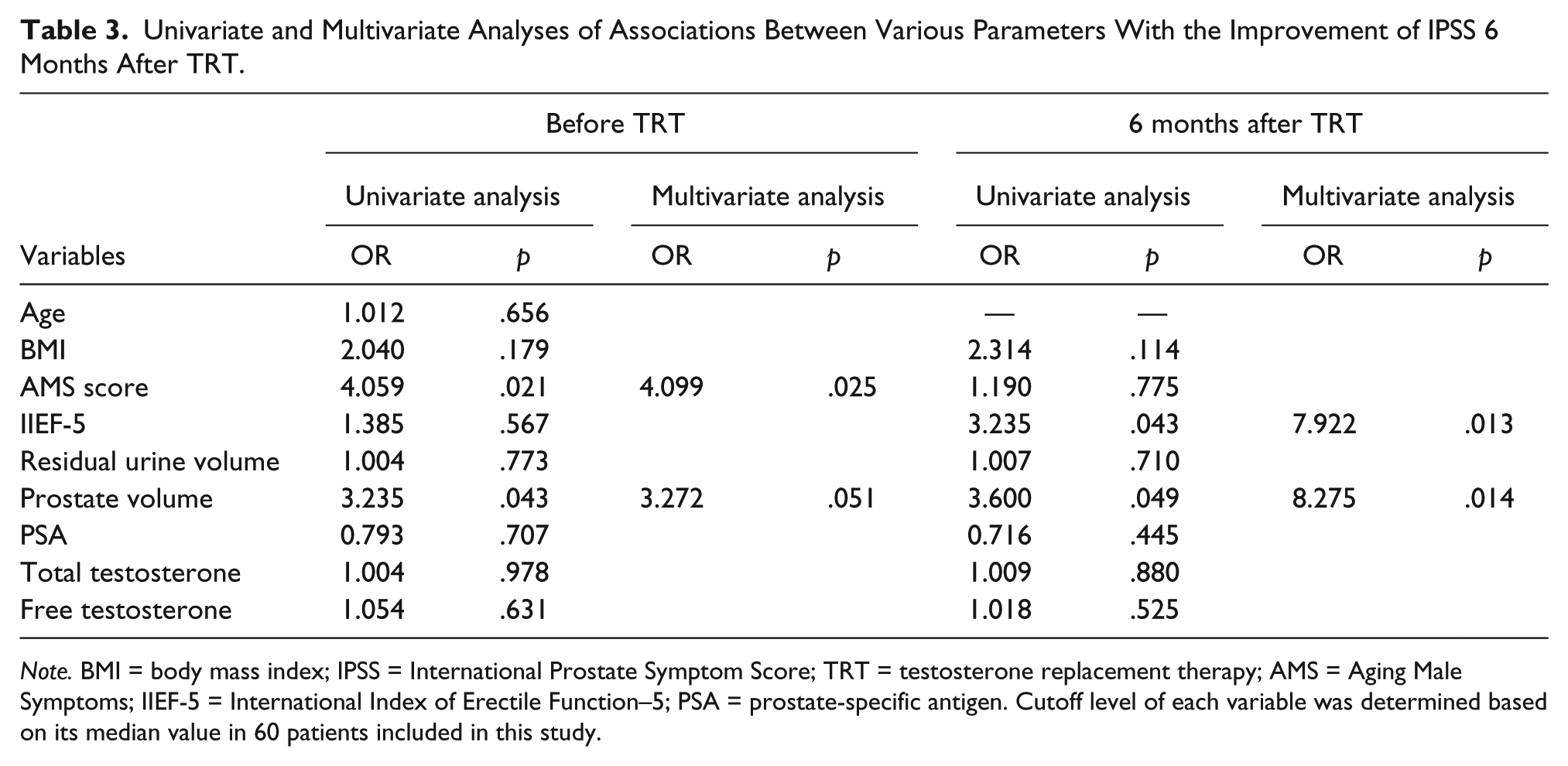
Note. BMI = body mass index; IPSS = International Prostate Symptom Score; TRT = testosterone replacement therapy; AMS = Aging Male Symptoms; IIEF-5 = International Index of Erectile Function–5; PSA = prostate-specific antigen. Cutoff level of each variable was determined based on its median value in 60 patients included in this study.
Discussion
A number of studies have demonstrated the beneficial effects of TRT on various unfavorable symptoms in men diagnosed with LOH without severe adverse events related to this therapy. Thus, TRT has become the mainstay of treatment for aging men with testosterone deficiency who exhibit clinical signs associated with hypogonadism (Mäkinen & Huhtaniemi, 2011; Shames, Gassman, & Handelsman, 2007). Some concerns remain regarding the negative effects of TRT on men with LOH, of which the possible deterioration of symptoms associated with BPH is regarded as one of the most considerable events for the following reasons: the onset of LUTS in men occurs at a time in life when testosterone levels begin to decline, and the growth of the prostate gland is closely regulated by testosterone levels (Huggins, & Stevens, 1940; Imperato-McGinley, Guerrero, Gautier, & Peterson, 1974; Oesterling, Epstein, & Walsh, 1986; Wu, & Gu, 1991). There are some randomized controlled trials and meta-analyses which investigated the relationship between testosterone and LUTS. According to one meta-analysis, TRT increases the risk of prostate growth (Cui, & Zhang, 2013), while another indicated that TRT does not worsen LUTS among me with LOH (Kohn, Mata, Ramasamy, & Lipshultz, 2016). Thus, the findings that have been reported are controversial. For example, Schatzl et al. (2003) identified hypogonadism in approximately 20% of elderly men with LUTS, albeit without an impact on the symptom status, while Litman, Bhasin, O’Leary, Link, and McKinlay (2007) reported a correlation between the symptoms of LUTS and plasma concentrations of testosterone. Herein this series of TRT in 60 consecutive Japanese men who were diagnosed with LOH and underwent TRT were retrospectively reviewed, with a focus on the impact of TRT on changes in the status of LUTS.
In this series, TRT for 6 months statistically significantly elevated PSA levels in the 60 men with LOH, but the changes in PSA levels may not be clinically significant. Rhoden and Morgentaler (2006) retrospectively assessed the effects of TRT on PSA responses and reported that TRT caused a mild increase in PSA levels in most hypogonadal men. Marks et al. (2006) conducted a randomized controlled trial study and identified that exogenous testosterone given to men with LOH did not accumulate in the prostate, did not produce abnormal levels of dihydrotestosterone, and did not induce any marked biological changes in the prostate gland. Despite the increase in PSA levels, no significant changes in the prostate or residual urine volume after TRT were noted in the series (Marks et al., 2006). Collectively, these findings suggest that TRT for men with LOH may cause mild elevations in PSA levels, accompanying no biologically meaningful impact on the prostate gland.
As reported in previous studies, this study confirmed the significant improvement in symptoms associated with hypogonadism including the AMS score, IPSS, and IIEF-5 score by TRT (Okada et al., 2014). According to the results for IPSS, the improvements observed in LUTS, particularly those in storage symptoms, were likely to be achieved by men with LOH classified into the moderate or severe LUTS group. Although previous studies reported the adverse effects of TRT on LUTS, more recent studies reported the benefit of TRT in improving LUTS in men with LOH. For example, Yassin et al. (2014) analyzed data from 261 hypogonadal men receiving TRT and reported a significant decrease in IPSS with time following the initiation of TRT. These findings are supported, at least in part, by experimental studies investigating the biological mechanisms mediating TRT-induced improvements in LUTS, particularly those focusing on the effects of testosterone on the autonomic nervous system through androgen receptors localized on the lower urinary tract (Pearl et al., 2013; Shigehara & Namiki, 2011). Of the 60 men included in this series, there were only 8 with severe LUTS. The total IPSS score was statistically and clinically improved from 26.6 ± 36 to 21.6 ± 6.9 in these 8 patients (p = .028). This finding was consistent with the studies assessing the data for men with severe LUTS (Pearl et al., 2013; Tan et al., 2013). TRT may not aggravate LUTS in most men with LOH; however, this needs to be confirmed by performing a prospective study with a larger sample size.
The clinical characteristics influencing changes in LUTS after TRT warrant further study because there have been no parameters that have a substantial impact on the post-TRT status of LUTS. In this series, the pretreatment AMS score, posttreatment IIEF-5 score, and posttreatment prostate volume were identified as independent predictors of improvements in IPSS. Based on the results of the present study, LUTS in men with a high baseline AMS score may be improved by TRT, whereas a favorable impact on LUTS cannot be expected in those with a low IIEF-5 score or small prostate volume 6 months after the initiation of TRT.
There were several limitations to the present study. The primary limitations were its retrospective design, lack of a control group, and its small sample size. Additionally, this was a short-term, nonrandomized study, which may limit the ability to draw definitive conclusions concerning the long-term effects of TRT on LUTS in men with LOH. These patients met the criteria of the TRT, but the average age were relatively young and BMI was low. Accordingly, it has to be considered whether these findings can be applied to the general cohort of the aging male. Furthermore, testosterone enanthate was used at 3- or 4-weekly intervals in this study according to the Japanese guidelines, which is a lower dose than that in the American and European guidelines. Therefore, it may be difficult to apply the results of this study to overall cohorts receiving TRT for men with LOH.
Conclusion
Changes in several parameters in 60 consecutive men who were diagnosed with LOH and received TRT were assessed. LUTS, particularly storage symptoms, in these men were significantly improved 6 months after the initiation of TRT, and the improved status of LUTS appeared to be independently affected by the pretreatment AMS score, posttreatment IIEF-5 score, and posttreatment prostate volume. Future studies with a larger sample size need to be performed as a prospective setting in order to further examine the results presented herein.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
