Abstract
Health-related quality of life (HRQOL) measures among the African American populations have previously been inadequately studied. This study sought to further analyze the quality of life of African American men at the Cleveland Clinic Minority Men’s Health Center and Cleveland Clinic Minority Men’s Health Fair. Subjects were randomly selected at the Minority Health Fair and Minority Men’s Health Center clinics over the duration of 2 weeks to participate in the anonymous survey with the help of independent surveyors. Convenience sampling was done at the Minority Men’s Health Fair and at the Minority Men’s Health Clinics. Participants were administered in-person Short Form-36 (SF-36v2). A total of 83 participants were surveyed, and the response rate from the surveyed population was 100%. The only exclusion criterion for the study was the refusal to participate (n = 0). As compared with healthy U.S. norms, African American men reported lower HRQOL across six health domains: physical functioning (60.69 ± 2.82 vs. 84.2), general health (57.56 ± 2.41 vs. 72), social functioning (72.65 ± 3.17 vs. 83.3), role-emotional (55.89 ± 3.02 vs. 81.3), mental health (61.23 ± 2.34 vs. 74.7), and role-physical (62.5 ± 2.88 vs. 81). The largest difference between the health domains was reported in role limitations due to emotional problems (55.89 ± 3.02 vs. 81.3, 25.4). Marital analysis revealed clinically significant lower HRQOL in married African Americans as compared with nonmarried, statistically significant in physical functioning and physical health component (p < .05). African Americans disproportionally face pervasive disparities in health, as supported by extensive quality of life impairment. No other study, to our knowledge, has used quality of life assessment in African Americans to quantitate how such disparities are affecting important domains in their lives.
Keywords
Introduction
Racial health disparities are defined as the measurable occurrences of significantly increased differences in the incidence of certain diseases, as well as their observed increased morbidity and mortality in racial and ethnic minorities. In the United States, a disproportionate burden of disease and morbidity is borne by African Americans when compared with their Caucasian counterparts (Modlin, 2003). In fact, a 2002 report from the Institute of Medicine “Unequal Treatment: Confronting Racial and Ethnic Disparities in Health Care,” revealed that minorities tend to receive lower quality of health care than Whites, even if variables such as patient’s insurance status and income are adjusted (Institute of Medicine, 2002). African Americans have documented life expectancies 7 years shorter than non-Hispanic Whites (Modlin, 2003), the causality deeply rooted in social, cultural differences shaped by political, historical, environmental, hereditary, and economic factors (Institute of Medicine, 2002). Surprisingly, little research has been done to evaluate how health disparities among the African American population predicts decrements in quality of life (QOL). Relationships between health-related quality of life (HRQOL) and adverse outcomes have been well studied in patients with significant comorbidities (Ayanian, Landon, Newhouse, & Zaslavsky, 2014; Graham, 2014; Laiteerapong, Fairchild, Chou, Chin, & Huang, 2015; Porter et al., 2014), yet no research has been done to evaluate baseline African American QOL.
The Medical Outcomes Study 36-Item Short Form Version (SF-36v2) is one of the most extensively used HRQOL tools (Brazier et al., 1992; Garratt, Schmidt, Mackintosh, & Fitzpatrick, 2002; Ware, n.d.). The SF-36v2 was derived from 40 concepts captured in the Medical Outcomes Study (Stewart et al., 1989; Stewart, Hays, & Ware, 1988). The survey comprises eight domains: physical functioning (PF), role limitations due to physical health (RP), bodily pain (BP), general health perceptions (GH), vitality (VT), social functioning (SF), role limitations due to emotional problems (RE), and mental health (MH; Maglinte, Hays, & Kaplan, 2012). Additionally, the domains may be summarized and combined into physical and mental health components (PHC, MHC) scores.
The first version of SF-36 was available in 1990 (Maglinte et al., 2012), and further refined item wording and response categories were used to create the SF-36v2. The SF-36v2 uses norm-based scoring, derived from a 1998 National Survey of Functional Health Status sample of respondents, to be a representative of the noninstitutionalized adult U.S. population (Ware et al., 2007). Little to no evaluation of minorities has been done, and with an increasing proportion of minorities in the U.S. population, this study provides the first insight into African American men’s QOL as compared with U.S. norms.
To our knowledge, no study has previously been published that assessed the general HRQOL of African American men. The objective of this study was to characterize the relationship between racial demographic, health disparities, and HRQOL of African American men.
Method
Participants and Characteristics
Participants were randomly recruited from the Minority Men’s Health Fair (MMHF) at the Cleveland Clinic in April 2014. MMHF is a comprehensive program with a multidisciplinary team of volunteers from primary care, psychology, and urology, among other fields. MMHF is a free and open event to all minority groups, and specifically targeted toward men. Since its inception in 2003, MMHF has attracted thousands of minority men (and nonminority men) to participate in free health services and preventive health screenings, health education, outreach, and treatment programs.
Participants were randomly invited to participate in the anonymous survey with the help of independent surveyors at the MMHF and Minority Men’s Health Center clinics over the duration of 2 weeks. Convenience sampling at the MMHF and at the Minority Men’s Health Clinics was performed. Participants were administered in-person SF-36v2. A total of 83 participants were surveyed and within the time frame of the health fair. The response rate from surveyed population was 100%. The population surveyed had no acute medical needs, and no information on health status and comorbidities was collected. The cross-sectional analysis was done to evaluate baseline QOL of the minority men population. The only exclusion criterion for the study was the unwillingness to participate (n = 0).
The survey contained demographic information including age, marital status, and number of children. Out of 83 participants, 15 (18%) did not provide demographic information, but did complete the survey. Gender composition of the responders included 100% African American men (Table 1).
Characteristics of Survey Responders.

Statistical Analysis
Scores for the eight domains of the SF-36v2 were transformed to a 100-point scale, and higher scores indicated better HRQOL. The study compared QOL scores within a sample population using two-sample t tests under the assumption of equal variances. All analysis was performed using StatPlus software LE Version 2009. To determine the difference between this sample population and those of published U.S. norms (derived from cross-sectional study of 2,474 persons age 18 years and older), a difference of 5 or more points from the norms was considered clinically relevant for all HRQOL domains except for role-physical and role-emotional, for which a 10-point difference was required for a sample this size (Ware et al., 2007). Clinically important difference used for comparison has previously been established by Ware et al. in 2000 (Ware, Kosinski, & Gandek, 1993, 2000) and listed in Table 2. Specific age group analysis as well as marital status subgroup analysis was performed. Linear regression approach with respect to age was used to compare domain scales.
Health-Related Quality of Life Scores of African American (AA) Men Within Study Sample as Compared to U.S. Norms.

Note. SEM = standard error of mean; CI = confidence interval.
Clinically significant differences from U.S. norms, that is, those exceeding the criteria required by Ware et al. (1993, 2000). bNo Clinical Significance set point available.
Additionally, construct validity was evaluated through hypothesis testing. It was hypothesized that physical functioning should decline with age, which this survey analysis proved valid (Pearson correlation R = .69, p < .05). Additionally, the reliability of study findings was measured for Cronbach’s alpha (α), with a cutoff α = .6 as reliable. Mental health (α = .681), Physical Functioning (α = .954), Role Function (α = .894), Social Function (α = .892) all displayed high levels of reliability, and thus proven valid.
Comparison to U.S. Norms
Compared with healthy U.S. norms as established by Ware et al. (2007), African American men reported clinically significant lower HRQOL for physical functioning (60.69 ± 2.82 vs. 84.2), general health (57.56 ± 2.41 vs. 72), social functioning (72.65 ± 3.17 vs. 83.3), role-emotional (55.89 ± 3.02 vs. 81.3), mental health (61.23 ± 2.34 vs. 74.7), and role-physical (62.5 ± 2.88 vs. 81; see Table 2 and Figure 1). The table is a representative of African American men in this sample compared with those of U.S. norm as established by Ware et al. (2007).

Comparison of health-related quality of life in African American men. Clinically significant differences noted as ‡, those that met criteria defined by Ware et al. No Clinical Significance set point available.
Correlation Between Age and Health-Related Quality of Life Domain Scores
Correlations between age and the impact of HRQOL each of the eight domains were evaluated by Pearson’s correlations analysis. Statistically significant correlation was seen in the evaluation of age versus role limitations due to physical health (RP; Pearson correlation coefficient R = .69, p < .05), as well as strong correlation in age versus role limitations due to emotional problems (RE; R = .81, p < .015). While physical functioning (PR; R = .56, p < .15), physical health component (PHC; R = .52, p < .18), and mental health component (MHC; R = .55, p < .15) displayed strong correlation, they did not reach statistical significance (Figure 2).

Scatter plot of the simple linear regression analysis between the age and (A) Role limitations and physical health (RP), Pearson correlation coefficient R = .69, p < .05; (B) Age and Physical functioning (PF), R = .56, p < .15; (C) Age and Vitality (VT), R = .46, p < .24; (D) Age and role limitations due to emotional problems (RE), R = .81, p < .015; (E) Age and mental health, R = .49, p < .22; (F) Age and Social Functioning (SF), R = .178, p < .67; (G) Age and Bodily Pain (BP), R = .091, p < .83; (H) Age and General Health (GH), R = .021, p < .96; (I) Age and Physical Health Component (PHC), R = .52, p < .18; and (J) Age and Mental Health Component (MHC), R = .55, p < .15.
Marital Status
A within-sample, statistical analysis was performed to explore differences in QOL based on marital status. Statistically significant differences, as determined p < .05, were apparent in this sample analysis. Differences were most pronounced in physical functioning (p < .049) and physical health component (p < .047). Clinically significant lower domain scores were also reported in married men in vitality (55.22 vs. 62.72, p < .29), social functioning (66.07 vs. 75.96, p < .81), bodily pain (65.86 vs. 72.12, p < .36), and general health (53.5 vs. 60.7, p < .16), although none of the aforementioned domains reached statistical significance (Figure 3, Table 3).

Comparison of health-related quality of life in African American married versus nonmarried men, *Clinically significant differences noted, as those that met criteria defined by Ware et al. §p-values for continuous variables are from 2-sample t tests under the assumption of equal variances, and represent the difference between married and nonmarried men from same sample. Statistically significant difference is seen in PF and PHC.
HRQOL Scores of African American Married Versus Nonmarried Men Within Study Sample as Compared With U.S. Norms.

Note. HRQOL = health-related quality of life; PF = physical functioning; RP = role-physical; RE = role-emotional; VT = vitality; MH = mental health; SF = social functioning; BP = bodily pain; GH = general health; PHC = physical health component; MHC = mental health component.
Clinically significant differences from U.S. norms, that is, those exceeding the criteria required by Ware et al. bNo Clinical Significance set point available. cp Values for continuous variables are from 2-sample t tests under the assumption of equal variances, and represent the difference between married and nonmarried men from same sample. *Statistically significant difference is seen in PF and Physical Health Components.
Age
Within-sample stratification of responders to age groups revealed differences within the sample (Table 4). QOL impairments were most prominent among African American men 65 years and older. Men in that particular age group scored significantly lower than counterparts in other age groups across all QOL domains, as well as significantly lower than U.S. norms across all 10 domains. Statistically significant difference in HRQOL among men 65 years and older was seen in 3 of the 10 domains, physical functioning (p < .007), physical health component (p < .0056), and mental health component (p < .014) as graphically represented in Figure 4. Although, not statistically significant, differences were also apparent in role limitations due to physical health (40.21 vs. 62.5, p < .129) and role limitations due to emotional problems (33.33 vs. 55.89, p < .125), as represented in Table 4.
HRQOL Scores of African American Men Within Age Distribution, as Compared to U.S. Norms.

Note. HRQOL = health-related quality of life; PF = physical functioning; RP = role-physical; RE = role-emotional; VT = vitality; MH = mental health; SF = social functioning; BP = bodily pain; GH = general health; PHC = physical health component; MHC = mental health component.
Single data collection. bp Values for continuous variables are from 2-sample t tests under the assumption of equal variances, and represent the difference between African American men versus men >65 years or older from same sample. Statistically significant difference is seen in PF, PHC, and MHC.
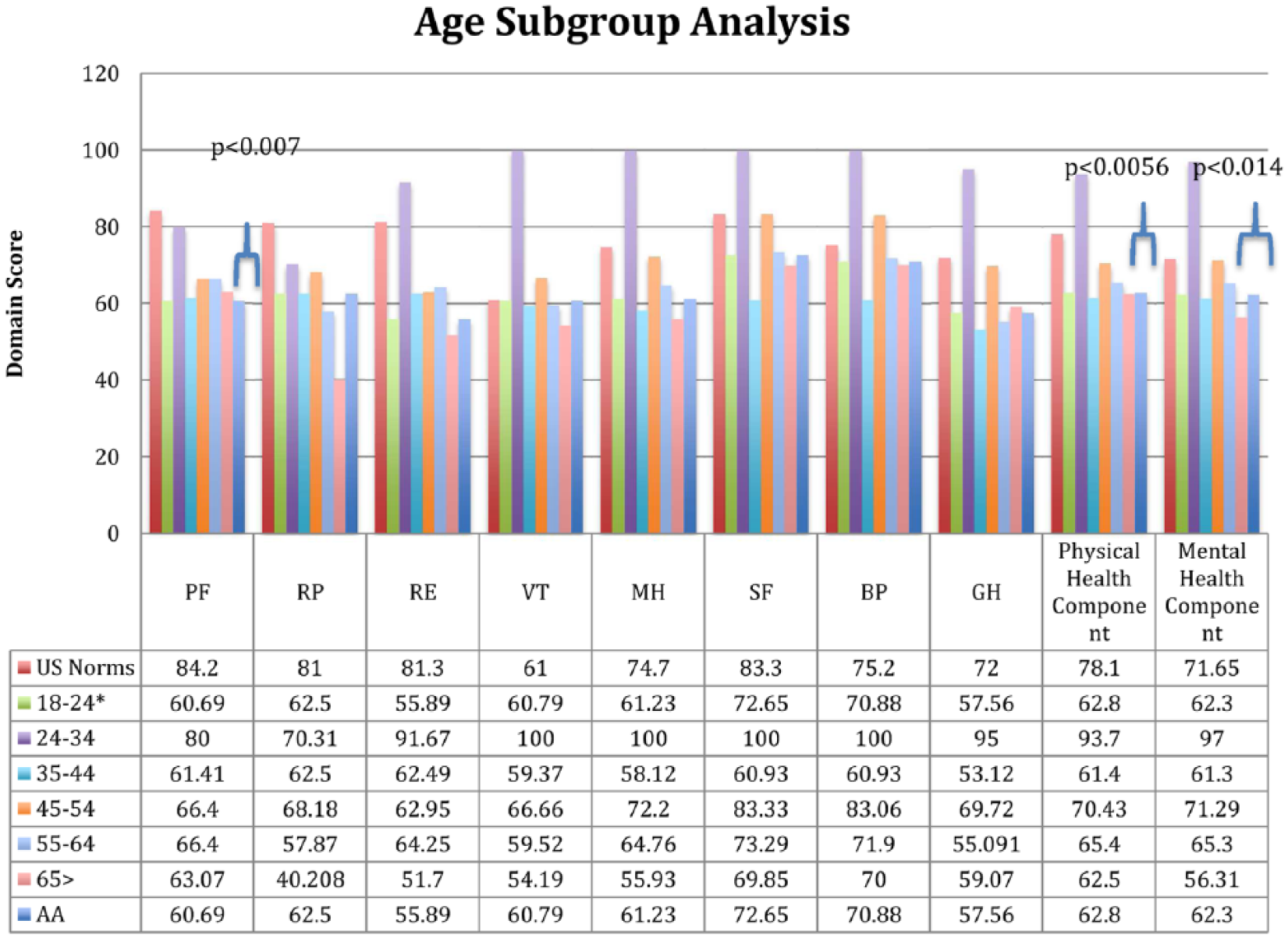
Health-related quality of life scores of African American men within age distribution, as compared to U.S. norms.
Discussion
HRQOL, defined as an individual’s or group’s self-perception of physical and mental health, is increasingly used to assess the effect of chronic diseases and their treatments in patients rather than solely using objective measurements such as morbidity and mortality (Zhang, Ferguson, Simonsen, Chen, & Tseng, 2014). Accordingly, future health care policy for numerous conditions may depend more heavily on HRQOL indicators than in the past (Zhang et al., 2014). Healthy People 2020 has identified QOL improvement as a central public health goal (U.S. Department of Health and Human Services, 2013), while the Centers for Medicare & Medicaid Services (2013) have selected HRQOL as the primary outcomes measure for evaluating managed care delivery programs.
While there have been studies previously published on African American QOL in chronic conditions, no evaluation of African American population QOL at large has been explored. African Americans disproportionally face pervasive disparities in health, and quantification of how such disparities are affecting important domains of everyday life is an essential aspect to be further explored. Racial status has a profound effect on a patient’s QOL, both through social and health care disparities, and through considerable morbidity and mortality associated with race. QOL deficits in African Americans may be correlated with decreased survival in a number of contexts, a subject that will further need evaluation.
Among an exclusively African American male sample, this study identified that decrements in summary scores across all health domains were considerably lower as compared with U.S. norms. Those differences were especially evident in men over 65 years old. African American men also experienced significant role limitations secondary to physical health and emotional problems.
Results were surprising in that the social support effect of marital status did not positively improve the QOL and reduce death rates across all chronic and acute medical conditions in this African American male population, unlike the multitude of studies in the literature in which marital status has been reported to strongly affect death and QOL across all chronic and acute medical conditions (Heo, Lennie, Moser, & Kennedy, 2014; Miller et al., 2010; Morrow et al., 2014). The level of social support in this study did not positively affect QOL. Married men had statistically lower scores in both physical functioning as well as physical health component. A plausible explanation could be attributable to an absence of an active disease, which mitigates a level of social support that might be needed in an otherwise acute medical diagnosis or a chronic illness. The nature of this study does not permit us to draw conclusions of why such a difference exists, but possible causes of why such a differences exists might also be explained by previous observation, in which married patients reported higher pain frequencies and physical limitations, as compared with single patients (Miller et al., 2010). Additionally, as divorced men were grouped as single at the time of the survey, there is potential for misclassification bias.
African Americans with a diagnosis of a mental health problem are significantly less likely to report having past or current treatment for depression, anxiety, or schizophrenia (Dixon et al., 2001), suggesting that the U.S. mental health system unequally serves the minority population (Modlin, 2003). The current investigation did report a clinically significant lower mental health component score across all age groups of African Americans men, and statistically significant lower mental health component score in African Americans men over 65 years old. African American men also reported significant role limitations due to emotional problems. An exceedingly negative correlation was observed between age and role limitations due to emotional problems. The findings of the interrelation of race, age, mental, and emotional problems likely illustrated the anticipated stigma among older African American men in seeking care and referral for mental health. These findings are similar to other studies of mental health disparities among African American men and are associated with major implications in unequal mental health treatment of African American communities (Sirey, Franklin, McKenzie, Ghosh, & Raue, 2014). Psychosocial factors may effect QOL as greatly as any chronic or acute disease status, and failure to recognize such disparities significantly contributes to the persistence of health disparities.
There are potential limitations to the current study. The study was only able to assess the QOL of African American men attending the Men’s Health Fair and Minority Men’s Health Center, which could be limiting in assessing baseline HRQOL in all African American men. Convenience sampling of the study protocol also predisposes to a selection bias. Future studies could address this limitation by assessing the African American population at baseline, through phone surveys. As with other QOL studies, one cannot definitely conclude that the study measured QOL and not the various effectors of it, including comorbidities that were not recorded. Psychosocial and socioeconomic factors are known to affect QOL, something the current study did not measure, and could be a potential research implication for the future. Despite the obvious limitations of this study, this is the first study to focus on QOL in African American men, compared with U.S. norms. The sample size of the study, although large enough to detect a clinical difference, is not large enough for subgroup analysis, especially if considering some subgroups of the study population over 65 years old only had 10 participants. Future studies could address this limitation by increasing the sample size for subgroup analysis.
Considering the crisis of racial health disparities in the United States and the limited research in how such disparities effect QOL of the minority population, this study is the first quantitative analysis of how much health disparities negatively affect and negatively impact QOL in African American males.
Conclusion
Impaired HRQOL was identified in African American men across the majority of health domains, with certain age groups felt to be more vulnerable to this effect. Despite advances in medicine, minority Americans face pervasive disparities in health, measurable difference in disease outcomes, and mortality. By examining and appreciating how these health disparities influence the QOL of minority populations, physicians and health care professions will be better positioned to understand and be able to deliver and provide culturally sensitive/competent solutions to eliminate health care disparities in minorities.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
