Abstract
The aim of the current study was to investigate the influence of different grades of abdominal obesity (AO) on the prevalence of testosterone deficiency syndrome (TDS), erectile dysfunction (ED), and metabolic syndrome (MetS). In a cross-sectional descriptive study, a total of 216 males underwent a complete urological, internal, and hormonal evaluation. Males were divided according to waist circumference into five groups: less than 94 cm (Grade [G] 0), 94 to 101 cm (G1), 102 to 109 cm (G2), 110 to 119 cm (G3), and more than 120 cm (G4). Incidence of ED, TDS, and MetS was compared in these groups and in participants without AO. Some degree of ED was identified in 74.7% of males with AO. In G1, there were 61% of males with ED, in G2 68%, in G3 83%, and in G4 87%. A strong correlation between testosterone (TST) level and AO was identified. Ninety-eight out of 198 (49.5%) males with AO and 1/18 (5.5%) males without AO had TDS. There were significant differences between individual groups. In the group of males with AO G4 (more than 120 cm), 87.1% had TDS. MetS was diagnosed in 105/198 (53.0%) males with AO, but in G4, 83.9% of males with AO had MetS. Males older than 40 years of age with AO have a higher incidence of ED, TDS, and MetS. Dividing males into five groups according to waist circumference seems to be reasonable. With growing AO, there were significantly more males with ED, TDS, and MetS.
Introduction
Testosterone deficiency syndrome (TDS) is a clinical and biochemical syndrome that results in a significant decrease in the quality of life and adversely affects the function of multiple organ systems. TDS is characterized by a decrease in testosterone (TST) and other hormones and is associated with changes in body mass index, obesity, osteoporosis, and sleep and mood disorders (Nieschlag et al., 2005), as reported in Table 1 (Jockenhovel & Schubert, 2007). Obesity appears to be a driving factor since adipose cells secrete leptin, which results in a decrease in TST level. TST has a wide range of reproductive (sexual) and nonreproductive actions: It preserves bone and muscle mass, it acts on nonsexual mental functioning, and it stimulates red blood cell formation.
Typical Clinical Symptoms in Older Men.

Erectile dysfunction (ED) is one of the most widespread chronic diseases in men (Nicolosi, Moreira, Shirai, Bin Mohd Tambi, & Glasser, 2003). It is widely agreed that atherosclerotic vessels of the penis are the cause of organic ED in the majority of cases (Melman & Gingell, 1999). Evidence of this can be seen from the fact that the risk factors of atherosclerosis, such as hypertension, diabetes mellitus (DM), dyslipidemia, sedentary lifestyle, obesity, and smoking are common in men with organic ED (Feldman, Goldstein, Hatzichristou, Krane, & McKinley, 1994; Nicolosi et al., 2003). The severity of ED is known to correlate with the number and severity of the aforementioned disorders, while the combination of these factors raises the risk of developing ED (Parazzini, 2000). Metabolic syndrome (MetS) is defined by the presence of at least three of the following: abdominal obesity (AO), arterial hypertension, decreased levels of high-density lipoprotein (HDL), elevated triglycerides (TG), DM, or other disorders of blood sugar tolerance. AO is defined by the World Health Organization (1999) and the International Diabetes Federation (2005) for European men as a waist circumference (WC) more than 94 cm and by the National Cholesterol Education Program (2001) as a WC more than 102 cm (Goncharov, Katsya, Chagina, & Gooren, 2008). Recent evidence suggests that TDS is likely to be a fundamental component of MetS (Corona et al., 2006; Kupelian et al., 2006; Makhsida, Shah, Yan, Fisch, & Shabsigh, 2005). There is an inverse relationship between plasma TST and severity of these symptoms (Kaufman & Vermeulen, 2005). Individuals with MetS carry a twofold increase in relative risk of cardiovascular disease and fivefold increase in relative risk of type 2 DM compared with those without the syndrome (Khan et al., 2005). Another cause of ED is a low level of TST. Research has presented convincing evidence that TST has profound effects on the tissues of the penis involved in the mechanism of erection and that TST deficiency impairs the anatomical and physiological substrates of erectile capacity (Gooren & Saad, 2006; Kaufman & Vermeulen, 2005). TST production decreases approximately 1.2% per year as men become older (Feldman et al., 2002). Male sex hormones play an important role in ED and a variety of TDS and may have an influence on the development of MetS. The number of men with AO, which constitutes a serious health risk, is continuously growing.
Materials and Methods
The authors examined 216 men at a preventive check. The mean age was 61.1 years (range = 43-78 years). There were 13 men younger than 50 years of age, 111 men were between 50 and 59 years of age, 78 were between 60 and 69 years of age, and 14 were older than 70 years of age.
A complete urological evaluation (including hormonal evaluation) and internal evaluation was carried out on every participant. To assess subjective symptoms related to TDS, the Aging Males’ Symptoms Scale (AMS) was used. To assess subjective symptoms of sexual health, the International Index of Erectile Function (IIEF 5) was used (0-10 points severe ED, 11-15 medium ED, 16-20 mild ED). The authors used an algorithm for the diagnosis of TDS according to the 2001 Consensus Conference of the American Endocrine Society (Jockenhovel & Schubert, 2007). The presence of prostate cancer was ruled out in all men. TST was examined two times between 8:00 a.m. and 10:00 a.m. due to the highest level of TST in men in the morning. The authors excluded those with diseases such as adenohypophysis, hyperprolactinemia, and congenital nontreated hypogonadism (Kallman syndrome). Normal ranges of TST are from 7 to 28 nmol/L. Free TST was examined when the results were in range of 7 to 14 nmol/L and also bone mineral density in men with low TST. The authors wanted to know if more obese men had more disorders. Therefore, the participants were divided into five groups: men with WC less than 94 cm (Grade [G] 0), men with WC from 94 to 101 cm (G1), men with WC from 102to 109 cm (G2), men with WC from 110 to 119 cm (G3), and men with WC more than 120 cm (G4). For diagnosis of MetS, the authors used the classification from Berlin 2005: Berlin Modification of Criteria NCEP-ATP III (Corona et al., 2007; Eckel, Grundy, & Zimmet, 2005; Goncharov et al., 2008; Tkac, 2005) and the ATP III Modification of MetS for men:
Abdominal obesity (waist circumference)
Two out of the next risk factors: Elevated blood pressure >130/85 mm Hg TG >1.7 mmol/L HDL-cholesterol level <1.0 mmol/L (men) Glucose fasting >6.1 mmol/L
Statistical analysis was carried out using SPSS software. Contingency tables and p value of Fisher’s exact test were calculated.
Results
Erectile Dysfunction
Among men without AO, 50% had ED (33% had a mild form, 17% medium, and none had a severe form of ED). Altogether 74.7% of men with AO had some grade of ED. In group G1, 61% of men had ED; in G2, 68% of men had ED; in G3, 83% of men had ED; and in G4, 87% of men had ED. With growing WC there occurred a more severe form of ED (Figure 1). Differences were significant (p = .047).

Abdominal obesity and EDa.
Testosterone Deficiency Syndrome
The authors report a strong correlation between TST level and AO. There were more participants with growing AO and a low level of TST. These objective data, TST level, were more significant than a subjective evaluation of men with IIEF 5 and AMS questionnaire. The influence of AO on testosterone level can be seen in Figure 2. The differences were significant (p = .000). The authors report that nearly 89% of men without AO had a TST level more than 14 nmol/L, and none of these men had a TST level less than 7.0 nmol/L. With growing AO there were more men with a low level of TST and only 13% of men in G4 had a TST level more than 14.0 nmol/L. When the authors compared ED (points from IIEF 5 questionnaire) with TST level, they identified more men with ED and a low level of TST. The authors report that most men with normal erectile function (IIEF 5 more than 21) had a TST level more than 14 nmol/L and most men with the worst ED (0-10 points) had a TST level less than 7 nmol/L, but this was not significant (p = .828). With the AMS questionnaire, more and severe problems were identified in men with increasing AO. Men without AO (39%) had an AMS questionnaire in the normal range and the remaining had small and medium problems. With growing AO there were a smaller number of men without problems, and in G4, it was only 13% of men (Figure 3). These differences were significant (p = .017). This is also a subjective evaluation.

Influence of AO on TST level.
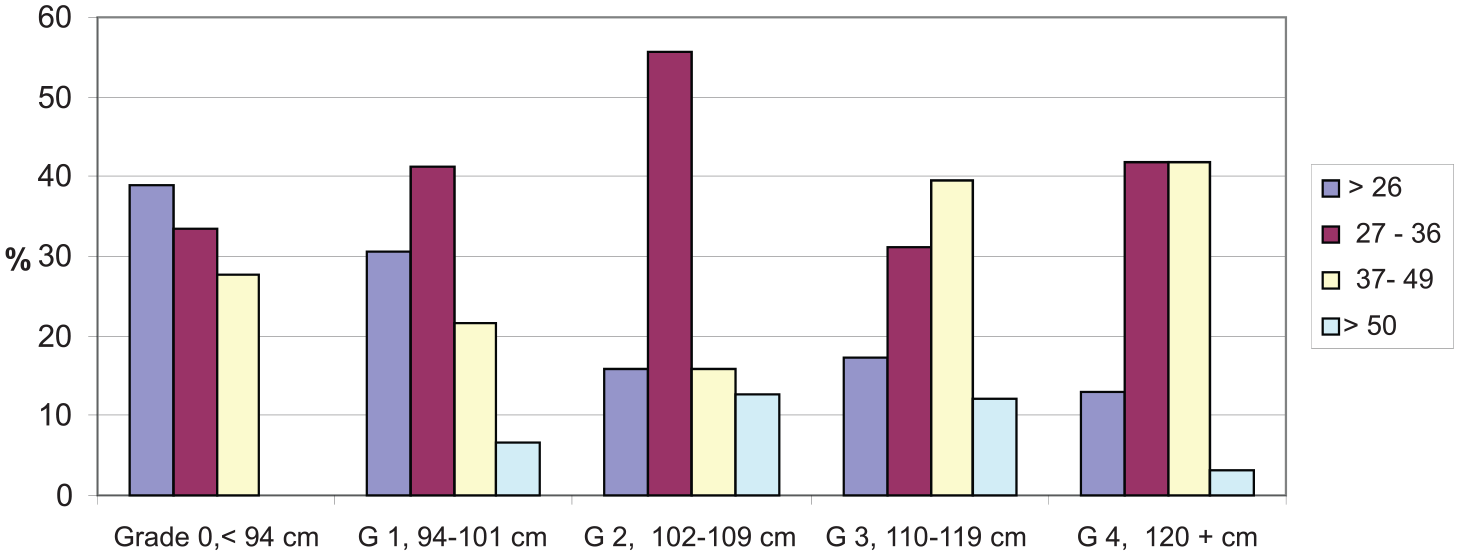
Points from AMS questionnaire and AO grade.
Metabolic Syndrome
No men without AO had MetS (p = .000). Of men with AO, 105/198 (53.0%) had diagnosed MetS. There were significant differences among groups (p = .000). MetS was diagnosed in 35% of men in G1, 51% of men in G2, 84.5% of men in G3, and 84% of men in G4 (Figure 4). There was no significant difference in the number of men with MetS between groups G3 and G4, but when the number of disorders was compared, differences were identified. In G3, 17% of men had five comorbidities, but in G4, there were nearly twice as many—32%.

Metabolic syndrome and abdominal obesity.
Discussion
The number of obese people in developed countries is continuously growing. AO seems to be of the same or even higher importance than the calculated body mass index (Makhsida et al., 2005). Adipose tissue has a suppressive effect on the synthesis of TST. The adipocyte functions as an endocrine cell that produces and secretes adipocytokines/adipokines of which leptin is a prominent member. Leptin receptors are located in Leydig cells and inhibit the TST generated by the administration of human chorionic gonadotropin (Isidori et al., 1999). The examination of those with ED on TDS becomes important for more reasons. The occurrence of TDS is 38.7% in men older than age 45 (Mulligan, Frick, Zuraw, Stemhagen, & McWhirter, 2006). In the current group of participants with AO, 98/198 (49.5%) were identified with TDS, but in the group of men with AO more than 120 cm, it was 87.1%. The American Urological Association guidelines recognize the importance of screening and treatment of individuals with ED. The authors report a strong correlation between AO, ED, TDS, and MetS.
Mortality
Shores, Matsumoto, Sloan, and Kivlahan (2006) reported in a study of male veterans older than 40 years without prostate cancer, followed-up for a mean of 4.3 years, that men with low and fluctuating values (low and normal) of serum TST levels had an increased all-cause mortality and shorter survival times compared with men with normal TST levels. In an unadjusted model, low TST levels were associated with an increased mortality risk of 88% greater than that for men with normal TST levels. Khaw et al. (2007) reported that TST level is in an inverse relationship with cardiovascular death. Men with a TST level more than 19.6 nmol/L have a 41% lower relative risk of death for all reasons than those who have a TST level less than 12.5 nmol/L. Multivariate analysis with TST identified that an elevation of TST level of 6 nmol/L decreased all reasons of mortality of 14%, p < .001 (Nieschlag et al., 2005).
Diabetes Mellitus and Insulin Resistance
Cross-sectional epidemiological studies have reported a direct correlation between plasma TST and insulin sensitivity. Low TST is associated with an increased risk of type 2 DM in men (Laaksonen et al., 2004). Fillo et al. (2012) identified an increased number of men with DM (p = .025) in a group of men with a TST level less than 10 nmol/L. Tsai, Boyko, Leonetti, and Fujimoto (2000) identified that three factors—obesity, insulin resistance, or hypogonadism—can start MetS.
Sufficient Level of TST
There is no constant level of TST that is sufficient for proper metabolism. In the authors’ previous work (Fillo et al., 2012), it was reported that men with TST more than 14 nmol/L had the smallest number of DM, hypertension, and the best results of HDL and triglycerides. There was a significant difference between participants with TST less than 10nmo/L and more than 14 nmol/L in DM, hypertension, HDL, and TG levels. There were differences between groups of men with a TST level between 10 and 14 and more than 14 nmol/L in the level of HDL and TGs. These findings suggest, similar to Khaw et al. (2007), that a sufficient level of TST should be a minimum of 10 nmol/L but better more than 14 nmol/L.
Conclusion
A significant difference between males with and without AO was observed. Males with AO had a higher occurrence of ED (74.7%), TDS (49.0%), and MetS (53%). The authors report that classification of central obesity into four grades appears to be useful as with growing WC the number and severity of comorbidities significantly increases. Out of all the men with AO, 74% had ED. Eighty-three percent of men in G3 had ED and 87% of men in G4 had ED. A total of 49.5% of men had TDS, but in G4, 87% of men had TDS. In G1, 35% of men had MetS, but in G4, 84% of men had MetS. An elevated level of TG and low level of HDL and obesity are three risk factors that lead to MetS and increase the risk of cardiovascular disease. Dividing men according to AO simplifies finding men with these problems. Early diagnosis and treatment of ED, TDS, and MetS may significantly improve the quality of life of the affected men.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
