Abstract
Men with hypogonadism (HG) who choose testosterone replacement therapy (TRT) may have distinct characteristics that provide insight as to why they may/may not initiate therapy. The aim of the current study was to identify trends in patient characteristics and attitudes in men diagnosed with HG who initiated TRT (TRT+) compared with men who were diagnosed with HG but did not initiate TRT (TRT−). The market research-based online survey conducted between 2012 and 2013 included patients from a Federated Sample, a commercially available panel of patients with diverse medical conditions. The current analysis was composed of two groups: TRT+ (n = 155) and TRT− (n = 157). Patient demographics, clinical characteristics, and attitudes toward HG and TRT were examined as potential predictors of primary adherence in men with HG; cohorts were compared by using Fisher’s exact test. Significant associations among sexual orientation, relationship status, educational level, presence of comorbid erectile dysfunction, area of residence, and TRT initiation were present (p ≤ .05). College-educated, heterosexual, married men with comorbid erectile dysfunction living in suburban and urban areas were more likely to initiate treatment. The most bothersome symptoms reported were lack of energy (90% vs. 81%, p = .075), decreased strength and endurance (86% vs. 76%, p = .077), and deterioration in work performance (52% vs. 31%, p = .004); lack of energy prompted men to seek help. Patients (48%) in the TRT+ group were more knowledgeable regarding HG as compared with TRT− respondents (14%, p < .001), and most men obtained their information from a health care professional (89% vs. 82%, p = .074). The current analysis identified distinct demographic and clinical characteristics and attitudes among TRT users compared with men who were diagnosed with HG yet remained untreated.
Introduction
Hypogonadism (HG) affects up to 39% of men 45 years of age or older and is associated with testicular failure and/or deficient hypothalamic–pituitary function resulting in low circulating testosterone levels and impairment of spermatogenesis (Araujo et al., 2007; Mulligan, Frick, Zuraw, Stemhagen, & McWhirter, 2006; Spitzer, Huang, Basaria, Travison, & Bhasin, 2013). To restore testosterone levels, treatment guidelines suggest initiating testosterone replacement therapy (TRT). Of the available preparations, transcutaneous testosterone gels are the most frequently prescribed testosterone formulation in the United States (U.S. Food and Drug Administration, 2014). While on TRT, guidelines suggest monitoring testosterone levels 3 to 6 months after treatment and then annually to assess HG symptoms (Bhasin et al., 2010). After 6 months of TRT, the extent to which HG symptoms are reduced is evaluated and a decision is made regarding whether to continue treatment (Swerdloff & Anawalt, 2014).
Clinical data report that TRT or TRT combination therapy restores testosterone to normal physiological range and improves HG symptoms when taken as prescribed (Bhasin et al., 2010; Isidori et al., 2014). As with any treatment, benefits, risks, and comorbid conditions should be considered prior to initiating treatment; however, in men with consistently low testosterone levels, TRT may restore testosterone levels, increase muscle mass and energy, raise bone density, stimulate libido and sexual function, and ultimately improve health and quality of life (Donatucci, Zhanglin, Fang, & Muram, 2014; Miner, Barkin, & Rosenberg, 2014).
Testosterone prescriptions have increased 3-fold over the past decade, including $1.6 billion testosterone prescriptions written in the United States in 2011 (Baillargeon, Urgan, Ottenbacher, Pierson, & Goodwin, 2013; Spitzer et al., 2013). Yet recent studies reported that as many as 28% of e-prescriptions for new TRT were not filled (Fischer et al., 2010), and up to 20% of hypogonadal men who initiate treatment with TRT fill only one prescription (Vigen et al., 2013). New, filled prescriptions were about three times more likely to be abandoned (e.g., not collected) at pharmacies, compared with previously filled prescriptions; among daily use therapies, higher rates of “return to stock” were seen with insulin (2.2%) and proton pump inhibitors (2.6%) compared with hormone replacement therapy (1.3%; Shrank et al., 2010). In general, causes of this primary nonadherence have been postulated, implicating cost, patient–physician communication, and prescription education. Ultimately, the implications of TRT nonadherence are of clinical concern, as patients will not receive the benefits of symptom relief (Fischer et al., 2010; Shrank et al., 2010).
Factors associated with patient treatment initiation, or primary adherence, have been identified in multiple therapeutic areas (Jin, Sklar, Oh, & Li, 2008; Shah et al., 2008; Shah et al., 2009; Strathdee et al., 2005). Although TRT product-related characteristics, such as convenience, persistence of low testosterone levels in men with HG while on other treatment, and physician recommendation have been reported to influence treatment initiation (Smith et al., 2013), limited data exist regarding distinct patient clinical or demographic characteristics and attitudes that help explain why men diagnosed with HG may or may not initiate TRT.
Aims
To better understand patient characteristics associated with TRT initiation, the authors sought to identify trends in characteristics and perceptions in men who were diagnosed with HG and who initiated TRT (TRT+), compared with men who were diagnosed with HG, obtained a prescription, but did not actually receive/initiate TRT (TRT−).
Method
Survey Development/Study Design
An expert panel with backgrounds in marketing, marketing research, and statistical analysis developed a series of questions focusing on issues potentially related to initiating TRT. Questions from this online survey captured patient demographic information, as well as perceptions and knowledge of HG and TRT. The survey was (a) vetted by the experts, (b) reviewed and approved for appropriate patient privacy parameters by the Eli Lilly and Company internal protocol review committee and a separate patient privacy committee, and (c) pretested with a small group of respondents prior to full data collection to confirm clarity of all questions and scales. Responses were anonymized and aggregated prior to reporting. Informed consent was obtained from all participants.
The market research-based online survey was conducted during 2012 to 2013. Participants were compensated.
Inclusion Criteria
Patients from the Federated Sample, a commercially available panel of patients with diverse medical conditions, received an invitation to complete an online survey. Respondents were screened according to their responses to the first few questions. Potential participants were asked about their gender and age, and only males age 35 and older were allowed to proceed with questions eliciting details of their medical history as well as demographic information. The goal was to have 700 men qualify and complete the questionnaire, and half (N = 350) of these men were diagnosed with HG. The sampling strategy allowed for the first 300 respondents to be included, regardless of which group they were ultimately assigned to. After that, minimum quotas were set for each of the groups, and patients were accepted only if there were unfilled quotas in the group for additional patients.
The data set included five distinct populations of men with self-reported HG who may or may not have had concomitant benign prostatic hyperplasia. The current analysis was composed of two groups: men who were diagnosed and elected to receive TRT (TRT+; n = 155) and men who were diagnosed and prescribed TRT, but did not actually receive TRT (TRT−; n = 157). The latter were men diagnosed with HG and, based on their responses, indicated that they elected not to receive therapy. This group included patients who refused a prescription, those who received a prescription but did not fill it, and those who filled a prescription but elected not to pick it up or use it, or a combination of these circumstances. Patients in the remaining three groups received a prescription but were excluded from the analyses, because either their diagnosis was not confirmed or they discontinued treatment.
Main Outcome Measures
Patient demographics, clinical characteristics, and attitudes toward HG and TRT were examined as potential predictors of primary adherence in men with HG.
Statistical Analyses
All the variables measured on this survey were categorical by nature (e.g., education level, income-level class, marital status, knowledge and attitudes regarding TRT). Percentages of patients per level for each of these categorical variables were summarized by group (TRT+ vs. TRT−) and group comparisons were accomplished by using the Fisher’s exact test. Because of the exploratory nature of the survey, no formal power calculations were performed a priori. The authors determined that utilizing 150 patients per group in a comparison via Fisher’s exact test would have approximately 90% power to detect an odds ratio of 3 or more for the largest percentage group compared with the smallest percentage group assuming the lowest percentage was at least 10%. Statistical significance level of .05 was chosen; however, comparisons yielding p values <.10 (but larger than .05) are considered marginally significant.
Results
Demographics
Of the 312 men included in this study, the majority were Caucasian, heterosexual, married men from age 35 to 65 years with private insurance plans (Table 1). Significant trends were observed among men with HG in TRT+ versus TRT− groups: educational level (taking some college courses or completing a 2-year degree: 32% vs. 43%, p = .036; completed undergraduate degree: 50% vs. 36%, p = .012), household income >100,000 (30% vs. 17%, p = .006), enrollment in an insurance plan (private insurance: 70% vs. 55%, p = .005; Medicare: 29% vs. 16%, p = .007; Medicaid: 12% vs. 4%, p = .022; no insurance; 4% vs. 22%, p < .001), geographical area (urban: 32% vs. 20%, p = .028 and suburban: 45% vs. 57%, p = .041), sexual orientation (heterosexual; 88% vs. 96%, p = .022), and relationship status (married: 72% vs. 59%, p = .018).
Patient Demographics and Clinical Characteristics.
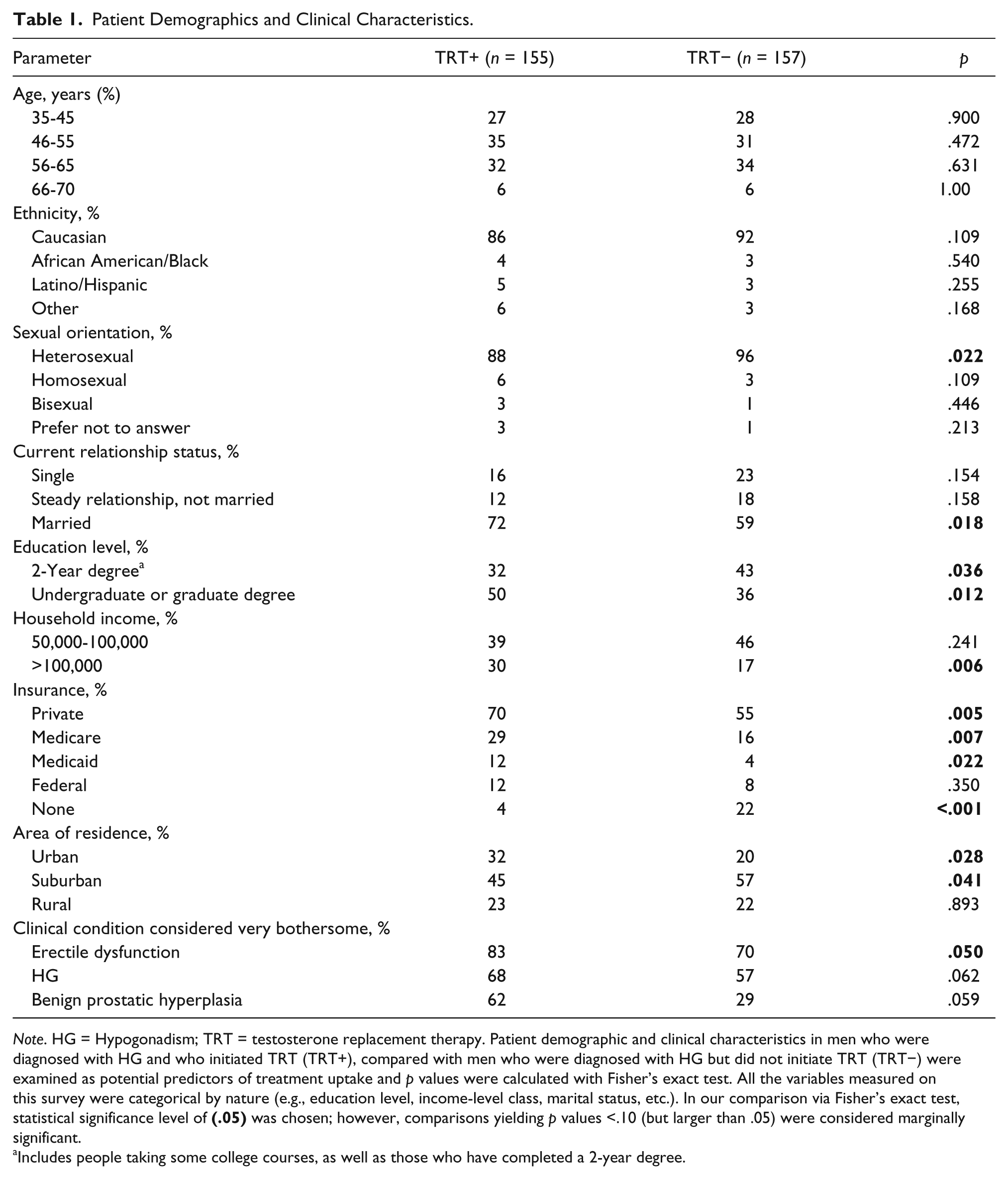
Note. HG = Hypogonadism; TRT = testosterone replacement therapy. Patient demographic and clinical characteristics in men who were diagnosed with HG and who initiated TRT (TRT+), compared with men who were diagnosed with HG but did not initiate TRT (TRT−) were examined as potential predictors of treatment uptake and p values were calculated with Fisher’s exact test. All the variables measured on this survey were categorical by nature (e.g., education level, income-level class, marital status, etc.). In our comparison via Fisher’s exact test, statistical significance level of
Includes people taking some college courses, as well as those who have completed a 2-year degree.
Clinical Characteristics
With respect to clinical characteristics (Table 1), a higher percentage of TRT+ reported erectile dysfunction (83% vs. 70%, p = .050), HG (68% vs. 57%, p = .062), and benign prostatic hyperplasia (62% vs. 29%, p = .059) as very/extremely bothersome male disorders when compared with TRT− men. Of men in both TRT+ and TRT− groups, the most bothersome symptoms reported were the lack of energy (90% vs. 81%, p = .075), decreased strength and endurance (86% vs. 76%, p = .077), and deterioration in work performance (52% vs. 31%, p = .004); of these symptoms, men indicated that the lack of energy prompted them to seek help (Figure 1).

Trends in patient characteristics and attitudes in men who were diagnosed with HG and who initiated TRT (TRT+), compared with men who were diagnosed with HG but did not initiate TRT (TRT−).
Knowledge and Perceptions of Hypogonadism (Figure 1)
Patients (48%) in the TRT+ group were more knowledgeable regarding HG as compared with TRT− respondents (14%, p < .001); regardless, most men obtained their information from a health care professional (HCP; 89% vs. 82%, p = .074). In comparison with TRT− men, TRT+ men (93%) were more likely to view HG as a medical condition requiring treatment (p < .001) and more likely to feel comfortable bringing up personal topics with their HCP (p = .002), whom they felt was more knowledgeable (p < .001). Low percentages (29%) of untreated men viewed hypogonadal treatments as similar to steroids with safety issues compared with 18% of treated men (p = .034).
Discussion
Distinct baseline demographic and clinical characteristics were observed among men with HG in TRT+ versus TRT− groups. Sexual orientation, relationship status, educational level, household income, insurance plan, and geographical area were significantly associated with initiating TRT, as was the presence of comorbid erectile dysfunction (p ≤ .05). Patients with erectile dysfunction who were heterosexual, married, taking some college courses or completing a 2-year or undergraduate degree, living in a suburban or urban area were more likely to elect TRT and may be potential candidates for interventions to improve primary adherence for initiating therapy. Among patients without health insurance, there was a significant difference in the number who chose to adopt TRT (p < .001). Cost has been identified as potentially prohibitive for the use of TRT (Jannini, Isidori, Aversa, Lenzi, & Althof, 2013), which may explain the significantly higher percentage of men with no health insurance who did not choose TRT. In a subgroup analysis, Donatucci et al. (2014) identified statistically significant differences in patient characteristics, specifically the comorbid condition, erectile dysfunction (p = .025), in patients stratified by a pattern of TRT use (e.g., short-term, long-term, cyclic, complete discontinuation); this corroborates the current assertion that patient characteristics have an impact on treatment initiation/use, in general.
Many patients (both TRT+ and TRT−) indicated that the three most bothersome symptoms were lack of energy, decreased strength and endurance, and deterioration of work performance; lack of energy led them to seek help from their HCP. These results are consistent with Shortridge et al. (2014) who reported that 59% of patients experiencing fatigue indicated that this most bothersome symptom was the reason for seeking treatment; about 20% of men reported challenges with concentration and focus as their reasons for seeking medical care. Shortridge et al. (2014) concluded that the percentages of patients experiencing most bothersome symptoms did not vary according to whether TRT was initiated.
Patient age may be related to the perception of most bothersome symptoms. Most of the patients in the current data set were <65 years of age and reported negative effects on strength/endurance, energy, and work performance as most bothersome. Schoenfeld, Shortridge, Cui, and Muram (2013) hypothesized that younger men (<65 years of age) may be bothered more by symptoms of HG, sexual dysfunction, and lack of energy; older men (≥65 years of age) may attribute their lack of energy and reduction of sexual activity to the normal aging process. Regardless, the overall severity of HG symptoms appears to affect a patient’s quality of life and may affect the decision initiate TRT (Shortridge et al., 2014).
Of the modifiable determinants for initiating TRT, about half of patients (48%) in the TRT+ group were knowledgeable regarding HG as compared with TRT− (14%). If the current finding are extrapolated to those reported by Schoenfeld et al. (2013), factors influencing patient adherence and intentional nonadherence, we could hypothesize that patients who did not choose TRT were not as knowledgeable about HG and, therefore, had doubts about their own need for medication. Direct-to-consumer marketing of newer testosterone formulations to men in the United States (Layton et al., 2014) has likely fueled interest and awareness of normal and abnormal testosterone levels and the link to HG symptoms, especially for men in the current TRT+ group. Consumer health information regarding andropause is prolific in the public domain on the Internet, and there remains an unmet need for appropriate information to manage the condition (Harrison, 2011).
The increased awareness among men may have influenced their perceptions of andropause, in general, and may also have been one of the factors prompting them to get their testosterone levels measured. According to Harrison (2011), varying degrees of acceptance and understanding of andropause by both patients and HCPs exist that create an education gap. Anderson et al. (2002) reported that both HCPs and consumers harbor misconceptions pertaining to the nonsexual aspects of andropause (e.g., testosterone’s effects on lean body mass, osteoporosis, and loss of urinary control). Many factors may be driving the increase in testing, including changing physician attitudes, drug detailing, and reimbursement. Layton corroborates this by reporting the substantial increase in testosterone testing since 2000 in the United States (Layton et al., 2014).
In addition to consideration of patients’ perceptions of HG and TRT, physicians’ perceptions of TRT are equally important. The current analyses revealed that, although a high percentage of both TRT+ (93%) and TRT− (71%) men viewed HG as a medical condition requiring treatment, similar to other conditions, some men did not view HG as a medical condition requiring treatment and viewed hypogonadal treatments as similar to steroids with safety issues. This could potentially be linked to physicians’ perceptions of TRT for HG per Gooren, Behre, Saad, Frank, and Schwerdt (2007) who reported that approximately 68% of physicians worldwide associate TRT with greater risks than benefits, resulting in up to 35% of HG men not receiving treatment.
The high level of interest in the debate among prescribers regarding whether or not to recommend initiating TRT continues (Swerdloff & Anawalt, 2014). In their interactive case study, Swerdloff and Anawalt (2014) present two sides of the issue to educate clinicians. Donatucci et al. (2014) report that among the primary prescribers of TRT are urologists and primary care physicians. Based on the current analysis, a significantly larger percentage of TRT+ men believed their HCP was knowledgeable and were comfortable discussing personal information with and obtaining information from them. To adequately address concerns of TRT− men, it is important that HCPs be perceived as informed, aware of the symptoms of HG, and knowledgeable of available treatment options to be able to educate the patient, as well as address and potentially alleviate patient anxiety by discussing the benefits and risks of TRT. According to a survey conducted by Anderson et al. (2002), about half (47%) of people receive health-related information from their primary care doctor. Ultimately, HCPs and patients might decide not to use TRT; but for HCPs who choose to prescribe treatment, increased patient education regarding HG, as well as the potential risks and benefits of TRT options, could potentially facilitate physician and subsequent patient decision making with confidence.
The number of TRT prescriptions have doubled since 2007 (Baillargeon et al., 2013), and it is important to understand what motivates increasing numbers of men to initiate testosterone therapy. The current study identifies that most men, regardless of whether they initiated testosterone therapy, believed that HG is a medical condition requiring treatment. Yet some of these men elected not to initiate therapy. This suggests the interplay of multiple factors contributing to prescription-filling behavior and a need for a deeper understanding of patient motivators when attempting to predict primary patient adherence. Of men who decide to initiate TRT for HG, over 76% of patients were satisfied with their treatment choice (e.g., gel, injection, pellet; Kovac et al., 2014; Shortridge et al., 2014). Treatment satisfaction has been a result of alleviating the most bothersome symptoms of fatigue and improving energy levels (95%), libido (92.9%), and concentration (77.4%) in patients with restored testosterone levels as a result of TRT (Dandona & Rosenberg, 2010; Kovac et al., 2014).
Given the anonymous nature of the current market research survey, information regarding demographics and clinical characteristics (e.g., baseline testosterone levels) was limited. Also, the online survey excluded men who were not comfortable or experienced with Internet use. The HG was self-reported, and the authors were unaware whether the diagnosis was based on measurement of testosterone levels or presentation of symptoms. The authors were unable to determine how much time passed between the HG diagnosis and decision to treat/not treat or how they obtained their prescriptions. For men who were categorized as discontinuing therapy, specific reasons and timing for their discontinuation were not obtained. Unfortunately, the authors were not privy to details regarding health insurance information (e.g., providers, copays, specific plan details), household income, and areas of residence that could potentially add an additional layer of complexity to the descriptive interpretation. With regard to attitudes toward sex, sexual activity is strongly influenced by cultural values and may dictate help seeking (Bhavsar & Bhugra, 2013). Furthermore, cultural factors can be leveraged when initiating treatment; however, the current survey did not explore the possibility of whether cultural influences on treatment initiation existed (Bhavsar & Bhugra, 2013; Moreira et al., 2005). Patient preferences for testosterone formulations have been reported previously (Smith et al., 2013), although the current study did not discriminate among TRT products and, therefore, the authors were unable to link the initiation of specific TRT formulations with characteristics, attitudes, compliance, or perceptions. In addition, the characterization of patients who elected TRT does not necessarily mean that they received ≥1 prescription; rather, the authors relied strictly on patients’ ability to recall details. Also, it is important to keep in mind that treatment does not necessarily equate with compliance; the current study did not explore length of therapy in men who initiated TRT. Last, the current study did not rank order complaints in HG men who had multiple complaints, because the survey did not capture an order of severity.
Conclusions
In an era of patient-centered therapy, identifying patient characteristics, demographics, and attitudes toward HG and TRT can guide clinical decisions and meet patient expectations. Understanding why men initiate therapy has the potential to not only improve treatment strategies but also improve adherence to TRT. The current analysis identified distinct differences between men being actively treated for HG compared with those who declined treatment in terms of demographics, clinical and lifestyle characteristics, and attitudes toward HG and TRT. These insights may be extrapolated to provide hypotheses for why some men seek TRT and others do not. Ultimately, andropause education is essential for both physicians and patients to better understand the benefits and risks of TRT to facilitate decision making. Further study is warranted to gain deeper insight into the clinical rationale for advising patients against this treatment.
Footnotes
Acknowledgements
The authors would like to thank Gina Moore, MS (inVentiv Health Clinical) who provided technical expertise in preparing this manuscript.
Declaration of Conflicting Interests
The author(s) declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Raymond C. Rosen and Allen D. Seftel have no conflicts of interest to report. Dustin D. Ruff and David Muram are employees and minor shareholders of Eli Lilly and Company.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The study was funded by Eli Lilly and Company.
