Abstract
The study examined men’s reproductive health problems and sexual behavior and their implications for men’s welfare in Nigeria. It used the Nigeria Demographic and Health Survey data set of 2013. The analysis used only male recode files, representing 17,359 males. The dependent variable is the computed wealth index, which was selected as proxy for welfare condition. Analysis involved univariate and multivariate levels. The findings indicated that 49.3% of the respondents currently have more than one sexual partner. The total lifetime sexual partner index identifies 70.2% of the men interviewed have had at least two sexual partners in their lifetime. It revealed that men who experience reproductive health challenges, such as sexually transmitted infections and genital ulcer, are 44% and 93%, respectively, less likely to enjoy good welfare condition. It also indicated that men in urban area are 7.256 times more likely to enjoy good welfare condition compared with their rural counterparts. There is a negative association between total lifetime sexual partnerships and exposure to good welfare. The study concludes that social workers, marriage counselors, other health personnel, and policy makers need to focus on the practice of multiple sexual partnership and reproductive health diseases as major determinants of men’s welfare. The authors suggest that the index of welfare should include reproductive health issues and indicators of sexual behavior. Also, there is need for the establishment of specialized reproductive health care services and centers that are accessible to all men for effective servicing of reproductive health needs of men in the country.
Introduction
Several macro-economic statistics or measurements have been traditionally adopted for monitoring human and national progress. These include human development index, consumer price index, producer price index and gross domestic product (GDP), gross national product, and a host of others. However, in recent years, the inherent challenges in using macro-economic statistics to capture economic progress are progressively unfolding. Their constant misuse or inappropriate use are inimical to the sustainable development and can engender disastrous consequences arising from wrong interpretations and policy recommendations (Costanza, Hart, Posner, & Talberth, 2009; Stiglitz, Sen, & Fitoussi, 2009). It is an irony that a lot of countries that are recording increase in their economic indicators such as GDP are also burdened with high level of disease, poverty, unemployment, insecurity, and lower life expectancy (International Monetary Fund, 2014; National Bureau of Statistics, 2012).
In addition, economic statistics always exclude in their calculations the import of reproductive health in increasing savings and investment, workers productivity, children education with concomitant effect on human welfare. In regions where the GDP is producing robust improvement, the epidemiology of sexually transmitted diseases (STIs)/HIV/AIDS is poor with disastrous consequences. The epidemic is visibly erasing health and other socioeconomic progress in the region. Decreasing life expectancy, poverty, debility, lower productivity, and pressure on limited economic and health services has become the order of the day in the region. While Africa constitutes relatively 10% of the world population, the region shares over 75% of the burden of STIs/HIV/AIDS (Nasidi & Harry, 2006). The cumulative AIDS deaths up to year 2000 was 800,000; this was estimated to have grown to almost 4.7 million in 2010 and it is expected to reach 9.4 million this year, 2015, and the current male gender burden is 42% (Nasidi & Harry, 2006; National Agency for Control of AIDS [NACA], 2014). Thus, the omission of indicators of reproductive health in the measurement of GDP might not make the statistics a good index of human progress especially as it relates to social welfare. Although the understanding and purpose of statistical systems are myriads, the fact that a metric that is adapted to one economic activity might not be suitable for another or omits certain noneconomic activity makes confusion inevitable. It is apparent that additional measures are inevitable to track at least social indicator of welfare. Thus, the search for mechanisms of action toward measuring human welfare is still an emerging field of social research that demands greater scientific investigation.
Although the welfare of people cannot be inferred from a single measurement, it is more misleading to appraise the welfare using national income without the components of reproductive health and even gender disparity. GDP, as it were, captures all manner of activities including air pollution, some advertisements and medical costs, and production and certain services. It is indifferent to sexual challenges, marital conflicts/harmonies, and the safety on our streets. It focuses primarily on the monetized economic activities and it is subject to the production boundaries used. While the gross national product measures all production by domestic companies regardless of where in the world that production takes place, the GDP captures goods and services produced in the country notwithstanding whether they are produced by domestic or foreign companies and by design exclude goods and services produced in other countries. The GDP provides insight into the rate of growth of the economy, the spending patterns on goods either by government or the population. It also sheds light on the inflationary rate, the investment or savings patterns, as well as consumption behavior within monetized environment (Costanza et al., 2009; McCulla & Smith, 2007). For the past eight decades since its introduction, GDP has become an indispensable barometer of business cycles and a leading benchmark of government performance and widely employed to justify fiscal, monetary, and regulatory policies (Beachy & Zorn, 2012; Marone, 2012).
According to Robert Kennedy (1968), GDP measures everything except what makes life worthwhile (Costanza et al., 2009; Kennedy, 1968; Stiglitz et al., 2009). Specifically, social health is intrinsically difficult to measure using economic indices. GDP does not capture infant mortality, suicide rates, family breakdown, and other environmental health decay. GDP may not necessarily reflect things that have no market price but are good for our society. It excludes those illegal, menial activities for which most of their transactions escape official financial media such as banks (Daly & Posner, 2011; Landefeld & Villones, 2009) and sexual activity on which continuity of life depends. Thus, there is an urgent need for more effective social indicators to guide policy and decision making especially among different gender categories.
General observations indicated that most economic metrics are statistically insufficient to capture human welfare. Although, well-being is often used as synonym to welfare, welfare as conceptualized in this study encompasses the health, happiness, and fortunes of a person or group and not just the monetized activities of a people. It also involves comfort and safety and fortune. While the current concept of well-being highlights the importance of considering income, consumption, and wealth together as part of a conceptual framework (Organisation for Economic Co-operation and Development, 2013), welfare considers good health which includes sexual health conditions. Welfare could also be described as a collection of programs by governments, its agencies, or other stakeholders usually intended to assist the poor. However, its broader usage encompasses the well-being of the population. Welfare is agglomeration of overall conditions, emphasizing contentment, standard of living, individual health conditions, and in most cases, condition of an entire economy including individual happiness. It can be considered as positive population outcome measure beyond production, morbidity, mortality, and economic status that indicates how people perceive their life is going from their own perspective (Centers for Disease Control and Prevention [CDC], 2013a; Diener, Lucas, Schimmack, & Helliwell, 2009; Diener & Seligman, 2004; Frey & Stutzer, 2002). Simply put, it encompasses perception of their own physical, mental, and socioeconomic progress including good living conditions, employment, and safety (CDC, 2013b).
Few of the existing social health indexes have not helped the situation. Fordham Index of Social Health measures socioeconomic indicators such as infant mortality, child abuse, drug abuse, school enrolment, housing and income inequalities, but totally excluded sexual and reproductive health conditions. Genuine Progress Indicator emerged in the 1990s attempting to measure quality of life using various indicators but omit human capital, workplace environment, and sexual diseases, among others. The United Nations Human Development Index is based on the assumption that economic growth/development does not necessarily equate human development or increased welfare. Despite these vagaries of indices to measure economic development, the most appreciable evaluation of human well-being is the degree to which their goals and aspirations are satisfied especially in terms of basic human needs such as food, shelter, participation in economic activity, fulfillment of their reproductive health care and rights.
Well-being is like a common metric in public health surveillance systems, helping the policy makers in tracking, shaping, and promoting human socioeconomic progress. Well-being also generally includes personal or global judgments of life satisfaction especially feelings over jobs, sexual relationship, earnings, family, and career (Berhan & Berhan, 2015; Lyubomirsky, King, & Diener, 2005). Men’s welfare is thus associated with their reproductive health conditions, occupation, family, as well as other economic benefits (Daly & Posner, 2011; Landefeld & Villones, 2009; Lyubomirsky et al., 2005). Wherever higher level of well-being is recorded, there is likely to be appreciable decline in population vulnerability to risks of disease, illness, and injury. Also, individuals with adequate well-being could, all things being equal, be better immune, productive at work, and live responsibly (Daly & Posner, 2011; Landefeld & Villones, 2009). Considering the negative effects of omission of reproductive health variables in the measurement of economic progress, it is apposite to examine the level of wellness (well-being) of people in relations to their positions among reproductive health indicators and perhaps other notable economic variables.
Men’s well-being is perceived to be just a component of welfare but intrinsically related to their health and this includes reproductive health conditions and problems (Laumann et al., 2005). As a matter of fact, male reproductive disorders may affect three fundamental aspects of a man’s life namely: the health status, sexual relationship, and overall quality of life. It affects directly the men’s economic productivity and welfare. This is more real in patriarchal resource-based African economies like Nigeria. Men’s reproductive health is crucial to the health of the spouses/sexual partners, children, families, workplace performance, communities and creates hope and future for the entire nation. On one hand, men’s health is important to men themselves. On the other hand, it is more exigent because it is only healthier men who can raise or contribute to healthier families and communities across the world. However, as crucial as it is, there exists a dearth of statistics on the contribution of reproductive health problems to men’s welfare in Nigeria. The cultural sanctity around sexual matters in sub-Saharan Africa also undermines proper investigation to their impacts in the society. Thus, the study examined men’s welfare conditions in the context of their exposure to reproductive health diseases. It also explored the current challenges they face in accessing reproductive health care services.
Materials and Method
The study used Nigeria Demographic and Health Survey (NDHS) data set released in 2013 by Measure DHS, ICF International. The survey collated data on fertility, family planning, men, maternal, and child health. Other issues covered include knowledge on HIV/AIDS, sexual behavior, domestic/partner violence, orphanhood, nutritional practices, and harmful traditional practices against women. The survey target groups were women and men aged 15 to 49 years in randomly selected households across Nigeria (National Population Commission [NPC] & ICF International, 2014). This analysis used the only male recode files, covering 17,359 males. The dependent variable used in this study is the computed wealth index which was selected as proxy for welfare condition. Measure DHS computed this index from a set of social and economic factors (NPC & ICF International, 2014). The index was constructed using household asset data via a principal components analysis (NPC & ICF International, 2014). It has five categories (poorest, poorer, middle, richer, and richest). These were reclassified into two. The first three categories were recoded as poor (renamed as “exposure to poor welfare,” coded 0), while the last two were grouped as “exposure to good welfare” and coded as 1 in order to satisfy the condition for binary logistic regression model. They were recoded into two categories in order to measure welfare through respondent’s change from poor welfare (0) to good welfare (1).
The indicators of reproductive health diseases constitute the independent variables. These include the following: ever experienced any reproductive health disease, age at first intercourse, presence and number of sexual partners, use of condoms, and patronizing sex workers. The intervening or confounding variables adjusted for in regression analysis include age, education, marital status, working condition, and place of residence. Analysis involved univariate and multivariate levels. The univariate segment features descriptive statistics such as frequencies and means where necessary. The section was used to assess the sociodemographic characteristics of the respondents and the distribution of all other important variables that are done according to whether the individual has reproductive health challenges. Multivariate analysis used the binary logistic regression technique to estimate whether men’s reproductive health status (presence/absence of reproductive health defect) significantly influence their welfare conditions (low or high).
The model is therefore represented as:
Where, α is the Y intercept, that is, the estimated value of Y when all Xs are set at zero. β is a multiple regression coefficient representing the expected change in Y per unit change in X1 assuming that all other Xs are held constant. Y is thus defined as that measures the log-odds of welfare improvement with men reproductive health disease. p defines the probability that an individual enjoys good welfare status with reproductive health disease, while 1 − p stands for the probability of not enjoying good welfare status with reproductive health disease.
Results
The socioeconomic characteristics of the study sample are presented in Table 1. The age distributions show that the estimated mean age is 29 years. Highest proportion of the sample population was obtained for the lowest age group (15-19 years) and lowest value (10.0%) was obtained for the highest age group (45-49 years). The result reports a gradual decrease in the number of the sample as the age increases. The urban coverage was 41.2% while the rural was 58.8%. The three prominent religions affiliations in Nigeria covered were Christianity (51.7%), Islam (46.8%), and traditional practice (1.4%) as indicated in Table 1. The proportion of male without education was 19.3%, those with primary and secondary education constituted 65.5% of the total respondents, while only 15.2% have attained higher educational level.
Selected Socioeconomic Characteristics of Respondents.

Source. NDHS (2013).
About 23.9% of the sampled males were not working at the time of the survey, while 76.1% were working. However, occupation distribution revealed that majority of the respondents were in agriculture and manual jobs (49.5%). Those who are professionals or in higher managerial levels represented only 9.4% of the total sample; the clerical, sales, or service group represented 19.9%, while the domestic and household workers stand at 0.4% (Table 1). In the marital status analysis, almost half of the men interviewed claimed they were never married and 47.8% indicated they were married. The result, however, revealed that 1.5% were only living with partners, while about 1.6% were widowed, separated, or divorced (Table 1).
House ownership identifies that a higher proportion of the respondents (61.5%) do not own house and by implication, it means they were either living in rented accommodation or in slums. The category of home owners was estimated to be 38.5%. Out of this proportion, 25.6% own the house, while 12.9% are jointly owned (Table 1). The welfare status revealed that relatively more than half of the men in the study are in poor category, while 46.9% are in the rich category.
Indicators of sexual behavior among men in the study location and the risk of exposure to HIV/AIDS are featured in Table 2. The selected parameters for sexual behavior include number of sexual partners, partner’s age, total lifetime sexual partners (TLSP), ever paid for sex in the past 12 months, and cohabitation. Majority of the wives are young in age and at least one in every five wives is less than age 25. About 46.9% are in the age group of 25 to 34 years. The proportion in age 35 and above is 24.5%. The distribution of sexual partner cuts across all age groups. Among other information presented in Table 2 is that more than half of the partners (55.3%) are less than 30 years of age. Relatively half of the respondents (49.3%) have more than one sexual partner; TLSP is very high. About 70.2% of the respondents have had at least two sexual partners. Further detail from the result indicates that those who have had up to five partners constituted 51.5%, while the men who have had more than six partners and above are 18.8%.
Sexual Behavior and Exposure to Risk of HIV/AIDS Among the Male Respondents.
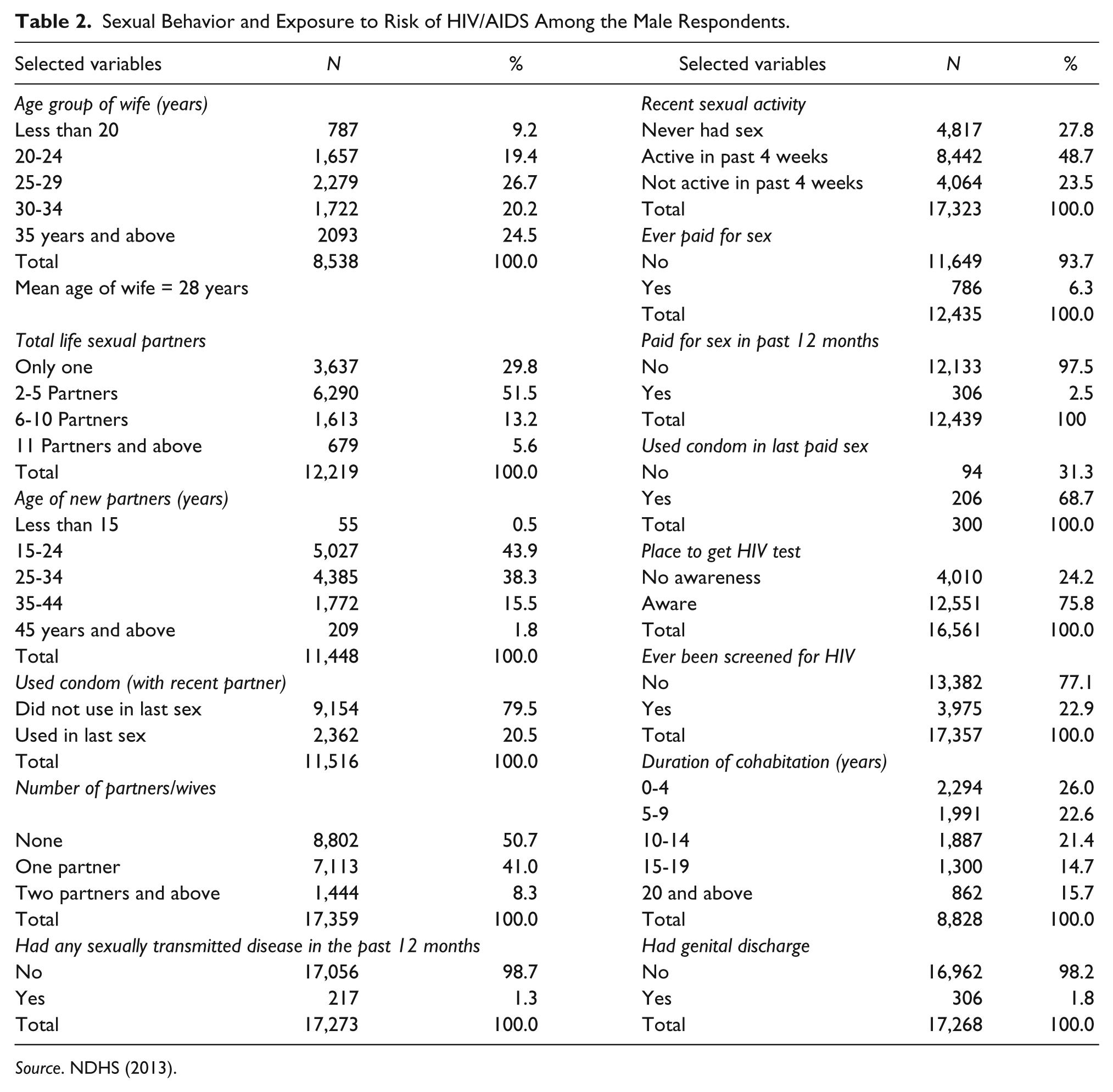
Source. NDHS (2013).
Cohabiting is prevalent among the men sampled and almost half of the respondents (48.6%) indicated they were cohabiting. The lengths of years the respondents have been involved in this practice, however, varied. While it is as low as 4 years in some cases, extreme cases were observed in certain cases. Specifically, while about 26.0% have been cohabiting for less than 5 years, 22.6%, 21.4%, and 30.4% have been in the practice for 5 to 9 years, 10 to 14 years, and 15 years and above, respectively. The result further revealed that, at least one out of three new sexual partners fall below age 25. While the proportion of new sexual partners decreases as age increases, cursory observation identifies that 43.9% and 38.3% of the new partners are in age group of 15 to 24 years and 25 to 34 years, respectively.
Recent sexual activity among the respondents is that 48.7% were very active in the past 4 weeks prior to the survey period, while 23.5% claimed they were not active during the same period. Despite the practice of multiple sexual partnerships and the number of cumulative lifetime partners (TLSP) observed, the knowledge and awareness about HIV including its mode of transmission or where to go for check is amazingly high. The results report that more than three quarters of the men knows at least one HIV test/screening center; however, an overwhelming number (77.1%) had never been screened for HIV or know their HIV statuses. In addition, 79.5% did not use condom in their last sex with their recent partner. Also, out of the proportion that paid for sex in the past 12 months, 31.3% did not use condom in their last sexual intercourse.
The result of the multivariate analysis (model testing) is presented by Table 3. The model illustrated the odds ratios of association between reproductive health challenges and welfare condition among men in Nigeria. The study recoded the exposure to good welfare condition from the original wealth index computed in the NDHS. As indicated earlier, the rich is coded as 1 and the poor is designated as 0. The rich are therefore designated as having “exposure to good welfare condition,” while the poor were defined as not having exposure to good welfare. The result of the analysis revealed that lower age group is negatively related to good welfare compared with the reference category (i.e., age 35 and above) as reported in Table 3. It shows most men who live in urban area are 7.256 times more likely to be exposed to good welfare condition compared with their rural counterparts. The usual place of residence demonstrated a statistical significant relationship with exposure to good welfare at p value = .000 with positive beta coefficient of 1.982 as indicted in Table 3.
Logistic Regression Illustrating Odds Ratios of Association Between Male Reproductive Health Problems and Men Welfare.

Note. STI = sexually transmitted infection; RC = reference category.
Source. NDHS (2013).
The results also identify that men in lower educational statuses might not likely be exposed to good welfare condition compared with individual men with tertiary education. The beta coefficients identify negative correlations with exposure to good welfare condition. However, the relationship between educational attainment and exposure to good welfare condition is statistically significant at p values = .000. This, by implication means that men with lower education might be facing wealth challenges coupled with their vulnerability to sexual reproductive health infections as demonstrated by the practice of multiple sexual partnership that is predominant in the area. Lack of health insurance cover/policy is also negatively related to good welfare condition but statistically significant at p values = .000. The result indicated that men without insurance cover will be 57% less likely to be exposed to good welfare condition.
In terms of cohabitation and exposure to good welfare condition, men who are not living with partners are only 19% and are less likely to be exposed to good welfare condition compared with men who are cohabiting with sexual partners. The farmers and unemployed are 80.0% and 27.0% less likely to be exposed to good welfare condition compared with men who are engaged in domestic or household chores. The professional/managers and clerical assistants and the salesmen are 3.119 times and 1.060 times more likely to be exposed to good welfare condition compared with individual men who do domestic and household jobs. There is negative association between total lifetime sexual partnership and exposure to good welfare. The finding from the analysis identifies that men without multiple sexual partners are more likely to be exposed to good welfare condition compared with the men with multiple sexual partners.
In addition to sexual activity indicators explained above, other predictors of welfare condition tested are the reproductive health problems as contained in the data set. Prominent among these variables are STIs, genital ulcer, and discharge from genitals. These are considered relevant considering the fact that they are symptoms or real manifestation of reproductive health problems and can directly impair harmonious relationship between couple as well as the community as a whole. The result further revealed that the presence of reproductive health problems make the men to be vulnerable to poor welfare condition. Specifically, men who experience STIs are 46% less likely to be exposed to good welfare condition. Similar result is obtained from genital ulcer and discharge from the genitals. Men who experience these diseases are 93% (Exp[Β] = 0.074) and 96% (Exp[Β] = 0.0415) less likely to be exposed to good welfare condition. The results obtained demonstrated significant negative correlations between reproductive health problems and men’s welfare condition. Those who have never tested for HIV are 33% less likely to be exposed to good welfare condition compared with those who have gone for the screening. Men that are not engaging in sexual intercourse at all and those who have not being active in the past 4 weeks are 1.281 and 1.263 times more likely to be exposed to good welfare condition compared with men who were sexually active in the past 4 weeks. The former variable is statistically significant at p value = .014.
Overall percentage of the model suitability indicated that the model employed is 86% adequate in the measurement of welfare condition of men and the associate predicted variables. The Cox and Snell R2 indicated that 52% of the variations in predicted variable (i.e., welfare condition) is explained by the predictors. Similar evidence was provided by Nagelkerke R2 of 0.698 showing that almost 70% of the variation in Y (i.e., welfare condition) is explained by the selected independent variables (i.e., Xs).
Discussion
The analysis carried out in this study used a nationally representative multigeopolitical zones data set. It highlights the sociodemographic characteristics and the indicators of sexual behavior of men in Nigeria as captured by Measures DHS’s latest demographic health survey. It also presented the extent to which men are vulnerable to the risks of STIs/HIV/AIDS and tested the hypothesis whether men’s reproductive health status significantly influences their welfare statuses. The geopolitical distribution of respondents selected is almost proportional to the population and the prevalence of divorce rates in the country (Adegoke, 2010; NPC, 2010). The proportion reported for education relatively followed the same pattern with the NPC report where more than half of the male population have had primary and secondary education and only few individuals were reported to have attained above secondary school education (NPC, 2010). The low level in higher educational attainment and lack of insurance coverage are significant factors when treating the subject of reproductive health issues as well as welfare. The high numbers of men in upper welfare status index could be said to be tallied effectively with the background characteristic of the men involved in this study.
Although, accurate assessment of men’s sexual behavior could be difficult considering the degree of silence surrounding sexuality in sub-Saharan Africa and the cultural permissiveness of plural marriage where a man is allowed to have more than one wife, the selected parameters used are those who are related to sexual activities as confirmed by other studies (Amoo & Adeyemi, 2010; Bingenheimer, 2010; Laumann et al., 2005; Sonfield, 2002; Zacharie, Jacques, & Osman, 2014). The confirmation by this study of the existence of sexual risk behavior signals a great concern and might continue to be a challenge in the future. Sexual risk behavior in men is a public health policy priority especially due to its linkage with STIs.
In addition, most of the wives/cohabiting partners are young and this could be extremely dangerous for healthy continuity of life and sustainable development of a nation (Casey, Kimberly, & William, 2013; Rector, Johnson, Noyes, & Martin, 2003). Age in sexual exposure is crucial and indispensable in the contribution to economic productivity. Young population are potential fathers and leaders of tomorrow; thus, indulgence in multiple sexual partnership make them more vulnerable to sexual transmitted infections including HIV and AIDS (NACA, 2014).
The high number of TLSP reported in this study sends fear regarding the spread of HIV/AIDS. The TLSP measures the cumulative number of sexual partners a man has had since exposure to sexual union till date (Chandra, Mosher, Copen, & Sionean, 2011). The result is in tandem with other past reports. A 1994 study in United States reported that 55% of men in heterosexual relationship had between 2 and 20 sexual partners and that 25% had more than 20 sexual partners (Seidman & Rieder, 1994). NDHS (2013) reported that men are more likely to engage in high-risk sexual activity and on the average, Nigerian men have many more sexual partners over their lifetime than women (4.1 compared with 1.5). Another report indicated that by the age 44, an average man must have had up to five sexual partners and that almost one in every five men of ages 15 to 44 years have had more than 10 sexual partners in their lifetime (Chandra et al., 2011).
While it could be conjectured that men’s socioeconomic status is the driving force for multiple sexual partnership as raised by another study (Berhan & Berhan, 2015), we can also raise a question on the import of multiple sexual partners on welfare of men. Multiple sexual partnerships are not benign practices: The cost of maintaining numerous sexual partners, the ill-health consequences of unprotected sex, and energy expended in “sexercise” cannot be understated. In addition, Sabia and Rees (2009) noted that multiple sexual partnerships is negatively related to educational attainment, the observation that is in agreement with the argument that romantic involvements are time consuming and can impose substantial emotional costs on the men involved especially if they are young in age (Ang’iro, Mwalili & Kinyanjui, 2015, 2015; Rector et al., 2003; Rector & Johnson, 2005; Sabia & Rees, 2009). There is therefore no doubt that these conditions can infringe on the welfare or access to adequate means of livelihood.
It is also insightful to know that despite the practice of multiple sexual partnerships and the observed level of TLSPs, the awareness about HIV and knowledge of where to go for check is very high. When the above observation is considered with the fact that over two third of the men did not use condom in their last sex and that majority are still involved in paid sex, it is obvious to assume that awareness and knowledge of STIs/HIV has no effects on the index of sexual behavior in the study population.
Cohabitation and the length of years a man has been cohabiting are also crucial to analysis of reproductive health diseases as well as men’s welfare. Cohabitation in this context implies the practices where two people who are not married live together in an emotionally and heterosexually intimate relationship on a long-term or permanent basis. This pertains to unmarried couples who live together without formally registering their relation either legally or in manner acceptable by their community custom. Examples of such include unmarried-living with partner, married-living with partner other than husband and divorced/separated/widow-living with partner. Wherever cohabitation is permitted in the face of rampant multiple sexual partnerships, the well-being of such society is at risk. Considering the high level of awareness and knowledge of the mode of HIV transmission and the practice of multiple sexual partnerships, it is easy to assume that the awareness and such knowledge is not affecting risky sexual behavior positively.
This finding therefore reflects the extent to which efforts on how to translate information received about HIV/AIDS and STIs into practice are still needed. Having multiple sexual partners enhances risks in reproductive health as well as men welfare. It is glaring that the continuous societal permissiveness or tolerance of the risky sexual behavior exhibited by the men (in this study) could be inimical to exposure to good welfare. The more sexual partners a man has, the greater the risk for STIs including HIV/AIDS and other life-threatening conditions like prostate cancer, cervical cancer, and oral cancer. In addition, having large number of sexual partners has been linked to shorter longevity, lower levels of happiness and well-being, and considered as a risky route to violence and sexual abuse (Bingenheimer, 2010; Kirby, L’Engle, & Prickett, 2012); NACA, 2014; Travasso, Mahapatra, Saggurti, & Krishnan, 2014).
Conclusion and Recommendations
The article describes the impact of male reproductive health challenges on men’s welfare as distinct from previous studies that only considered men’s reproductive health as function of women’s general reproductive health and rights especially as it relates to women’s fertility and prevention of STIs (Makarow & Hojgaard, 2010 ). The test of the association between male reproductive health problems and men’s welfare is relatively new or has not been overflogged in social research. The outcomes of the analyses portray the urban men as having potential for high-welfare condition compared with their rural counterparts. The lower educational statuses represent a fundamental variable in accessing high-welfare condition notwithstanding the presence of reproductive health disease. This by implication means that men with lower education might be facing welfare challenges coupled with their vulnerability to sexual reproductive health infections as demonstrated by their involvement in multiple sexual partnerships. Lack of health insurance cover/policy is negatively related to good welfare condition but statistically significant.
Multiple sexual partnerships are inimical to healthy living and engender male reproductive health sicknesses or infections and are harmful to national productivity especially due to cost of treatment and healthy life-year lost. The practice (of multiple sexual partnerships) is a key driver to STI/HIV/AIDS epidemic. Notwithstanding, the experience of one or more of these infections/disease transcend the men who are involved especially in patriarchy system of Africa, where men are the breadwinners of the family and some have more than one sexual partners. The study highlights that increase in awareness about the major consequences of male reproductive health is inevitable in Nigeria. It provides advice on the indicators of sexual behavior and the need to extend the index of welfare to reproductive health issues. The authors concluded that social workers, marriage counselors, other health personnel, and policy makers need to focus on sexual activity of the men especially multiple partnerships practice as well as reproductive health problems as major determinants of men welfare and by extension of sustainable development. The main policy insight could be seen on the path of increase in awareness of male reproductive health issues, the need for better understanding on the interconnections among specific male reproductive health challenges, and welfare status. It is also important to state here that treatment of male reproductive health through the medical angle without the social and economic consideration could only yield bodily soundness but immeasurable drain on or no value added to the national welfare. The authors therefore recommend the establishment of specialized reproductive health care services and centers that are accessible to all men for effective servicing of the reproductive health needs of men whether working or not working and include the same in human welfare measurement.
Footnotes
Acknowledgements
This research uses data from Measure NDHS and we wish to thank the Demographic Health Survey project for making these data available freely for our use.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.

