Abstract
The goal of this study was to determine if parents’ beliefs about social norms of human papillomavirus (HPV) vaccination for sons were associated with knowledge of HPV, intention to vaccinate sons, or beliefs about side effects. A cross-sectional, survey-based study of parents with sons was performed in 2010. Fisher’s exact tests were used to examine associations between demographics and responses about social norms. Multivariate logistic regression models examined beliefs about social norms of male HPV vaccination and primary outcomes. Few parents agreed that others were vaccinating sons (n = 31/267, 12%), including 1% responding strongly agree and 11% responding agree. Most parents, 52%, disagreed that others were vaccinating (40% disagree, 11% strongly disagree), and 37% chose prefer not to answer regarding others’ vaccination practices. Hispanic parents and those with a high school education or less were significantly more likely to choose prefer not to answer than their respective counterparts regarding vaccination norms. In multivariate models, parents agreeing others were vaccinating sons had greater odds of having high knowledge of HPV (adjusted odds ratio [aOR] high vs low knowledge 3.15, 95% confidence interval [CI] 1.13, 8.77) and increased intention to vaccinate sons (n = 243, aOR = 4.41, 95% CI = 1.51, 12.89). Beliefs about side effects were not significantly associated with beliefs about social norms. Parents’ beliefs about others’ vaccination practices are important with regard to knowledge of HPV and intention to vaccinate sons. Studying how various public messages about HPV vaccine may influence normative beliefs could be relevant to improving vaccination coverage.
A quadrivalent vaccine against human papillomavirus (HPV; i.e., HPV4) was approved for use in males in 2009 for the prevention of genital warts (Centers for Disease Control & Prevention, 2010). Subsequently, in 2010, the Food and Drug Administration approved HPV4 vaccine for the prevention of anal cancer in both males and females (Food and Drug Administration, 2011). Although the Advisory Committee on Immunization Practices issued a recommendation that HPV4 vaccine should be routinely given to males aged 11–12 years in 2011 (Centers for Disease Control & Prevention, 2011), vaccination rates in young males have been slow to improve (Stokley et al., 2014). As of 2013, only about 35% of males ages 13–17 years had received at least one dose, and only 14% had completed the three-dose vaccine series (Stokley et al.).
Although many factors may play a role in parents’ vaccination decisions, one understudied factor with regard to HPV vaccination for boys is parental beliefs about vaccination norms. HPV vaccine acceptability has been tied to beliefs about social norms of vaccination for females (Allen et al., 2009; Allen et al., 2010; Conroy et al., 2009; Hertweck et al., 2013; Marlow, Waller, & Wardle, 2007), and in some (Gerend & Barley, 2009; Reiter, McRee, Kadis, & Brewer, 2011), but not all (Wheldon, Daley, Buhi, Nyitray, & Giuliano, 2011), studies among adult men and boys.
Available data are limited and conflicting with regard to the importance of social norms to parents considering HPV vaccine for sons. Two available studies suggest that social norms are important in terms of vaccine acceptability (Dempsey, Zimet, Davis, & Koutsky, 2006) and intention to vaccinate sons (Dempsey, Butchart, Singer, Clark, & Davis, 2011). A third study reported that beliefs about norms were not consistently associated with vaccine acceptance for males (de Visser & McDonnell, 2008). Notably, these studies were done prior to FDA licensure of HPV vaccine for males (de Visser & McDonnell, 2008; Dempsey et al., 2011; Dempsey et al., 2006).
Given low vaccination rates in boys, it is essential to further investigate factors that may influence vaccination decisions, including parents’ beliefs about social norms of HPV vaccination for boys. Normative beliefs are especially important to consider as they could plausibly be influenced by public messages, including promotional messages about HPV vaccine for boys, or even persistent messages about low vaccination rates. Beliefs about social norms may be relevant to parents’ intention to vaccinate (Dempsey et al., 2011) and could plausibly be associated with degree of concern about vaccine side effects, still a concern among some parents (Berenson & Rahman, 2012; Reiter, Oldach, Randle, & Katz, 2013). Normative beliefs may also be relevant to knowledge of HPV, as identified in one prior study (de Visser & McDonnell, 2008).
The objectives of this study included first, to describe parents’ beliefs about social norms of HPV vaccination for boys post vaccine licensure for boys. Second, this study sought to determine if beliefs about social norms are associated with knowledge of HPV, intention to vaccinate sons, or beliefs about side effects of HPV4 vaccine.
Methods
This was a cross-sectional, survey-based study of parents with sons eligible to receive HPV vaccine. The survey for parents was developed using concepts from the Health Belief Model (Janz & Becker, 1984), one of the most commonly used theoretical frameworks for immunization studies. Parents recruited from a pediatrics clinic that provides primary and subspecialty care were surveyed in 2010. Parents of sons between the ages of 9 and 21 years were recruited to participate. Although HPV vaccine may be given to males ages 9–26 years, this study focused on the 9–21-year age range because patients older than 21 are not cared for in the pediatrics clinic used for recruitment. English- and Spanish-speaking parents were invited to participate in the survey. Spanish-speaking parents received a survey written in Spanish that was translated from English with the purpose of using the survey for research purposes. Study staff presented some questions verbally to parents, including questions about the sex and number of children, and intention to vaccinate sons. Verbally presented questions were delivered to Spanish-speaking parents by Spanish-speaking study staff. Otherwise, parents completed most portions of the survey independently in the clinic. Parents were asked to respond to survey questions based on the oldest son aged 9–17 years. If there was not a son in the 9–17-year age range, parents were asked to answer based on their oldest son aged 18–21 years. The institutional review board at the University of North Carolina approved the study.
Measures
Parents’ beliefs about social norms in the context of HPV vaccine for boys were assessed by proposing the following statement: “Other parents in my community are getting their sons the HPV vaccine.” Response options included strongly agree, agree, disagree, strongly disagree, and prefer not to answer. Responses were categorized for analyses into agree (including strongly agree and agree), disagree (disagree and strongly disagree), and prefer not to answer.
Parent knowledge of HPV was determined through developing one composite variable for knowledge, and incorporating responses from five individual questions about HPV. For example, the statement “HPV causes genital warts” was proposed to parents. Response options included true, false, don’t know, and prefer not to answer. True was considered to be the correct response, and the remaining responses were considered incorrect. The same method was used to assess parents’ knowledge of HPV in cervical, penile, anal, and oropharyngeal cancers. Parents were considered to have high knowledge of HPV if they answered four to five items correctly of five. Low knowledge was defined as zero to three correct answers of five.
Parents’ intention to vaccinate sons was assessed using one item. Study staff asked parents, “How likely is your son to get the [HPV] vaccine next year?” Possible responses included definitely won’t, probably won’t, probably will, and definitely will. Responses were dichotomized for analyses into probably will (including probably and definitely will) and probably won’t (including definitely won’t and probably won’t). Prefer not to answer was not offered as a response option for this item.
Parents’ beliefs about side effects were determined using one item. The following statement was proposed to parents: “The HPV vaccine may cause unknown long-term side effects.” Response options included strongly agree, agree, disagree, strongly disagree, and prefer not to answer. Responses were again dichotomized into agree (strongly agree, agree) and disagree (strongly disagree and disagree) and excluded prefer not to answer responses.
Analyses
Descriptive statistics were performed on each variable. The social norms item was treated as a three-category variable with prefer not to answer responses considered as a separate category; categorizing prefer not to answer responses separately was deemed necessary given the fairly high proportion of parents who chose this response, and the possibility that respondents in this category may be a meaningfully different group. Fisher’s exact tests were used to determine if demographic characteristics were associated with prefer not to answer responses for the social norms item. Multivariate logistic regression models were used to determine if parents’ beliefs about social norms, with respect to HPV vaccine for sons, were associated with parents’ knowledge of HPV, intention to vaccinate sons, or beliefs about side effects of HPV vaccine. Models adjusted for parent age, sex, race, ethnicity, marital status, education, and age of the index son. An alpha of .05 was used for all analyses. Analyses were conducted in Stata 11.1 (Stata Corp., College Station, TX).
Results
Two hundred ninety parents participated in the survey, and 92% (n = 267) were included in analyses, after excluding three participants who did not respond to the social norms item, and 20 participants who reported that sons had received any doses of HPV vaccine. Most parents were female (79%, n = 210), white (51%, n = 136) or black (40%, n = 108), and non-Hispanic (94%, n = 251). Most parents (74%, n = 197) reported some college experience (Table 1).
Participant Demographics (n = 267).

Includes multiracial (n = 9), other race/Hispanic (n = 8), other race/unspecified (n = 2), Native American/Alaska Native (n = 3), missing (n = 1).
Unmarried includes single, separated, divorced, or widowed.
High school education or less category also includes GED. Any college education includes any college experience, bachelor’s degree, or associate’s degree.
Responses to the social norms item demonstrated that 12% (n = 31) of parents agreed that other parents in their community were vaccinating sons against HPV (1%, n = 2 of parents strongly agreed, and 11%, n = 29, of parents agreed). Approximately 52% (n = 138) of parents disagreed that other parents were vaccinating sons (40%, n = 108 disagreed, 11%, n = 30 strongly disagreed). Thirty-seven percent of participants chose prefer not to answer for this item (Table 2).
Parent Responses on Whether Other Parents Are Vaccinating Sons Against HPV (n = 267).

In bivariate analyses, ethnicity and education were significantly associated with selecting the prefer not to answer response for the social norms item. Specifically, parents that self-identified as Hispanic, and those with a high school education or less, more often chose prefer not to answer compared to their respective counterparts (Hispanic 75%, non-Hispanic 34%, p < .01, high school or less 56%, any college 30%, p < .001; Table 3).
Demographics by Prefer Not to Answer Responses (vs Any Other Response) for Social Norms Item Regarding HPV Vaccination for Boys (n = 267).

Includes multiracial (n = 9), other race/Hispanic (n = 8), other race/unspecified (n = 2), Native American/Alaska Native (n = 3), missing (n = 1).
Unmarried includes single, separated, divorced, or widowed.
High school education or less category also includes GED. Any college education includes any college experience, bachelor’s degree, or associate’s degree.
Knowledge
Overall, approximately 12% (n = 31) of parents had high knowledge of HPV (answering 4–5 questions correct of 5) in the context of HPV’s role in genital warts, cervical, penile, anal, and oropharyngeal cancers. Parents were most knowledgeable about the role of HPV in cervical cancer, with 57% (n = 152) answering this item correctly, followed by genital warts, with 35% (n = 94) answering this item correctly. Parents were generally less knowledgeable about the role of HPV in anal, penile, and oropharyngeal cancers (15%–18% correct responses for each respective item). Parents who agreed others were vaccinating sons against HPV had significantly greater odds of having high knowledge of HPV than their counterparts in multivariate analyses (aOR = 3.15, 95% CI = 1.13, 8.77; Table 4).
Unadjusted and Adjusted Odds Ratios (aOR) a for Knowledge of HPV, Intention to Vaccinate, and Beliefs about Vaccine Side Effects According to Responses About Social Norms of HPV Vaccination for Boys.
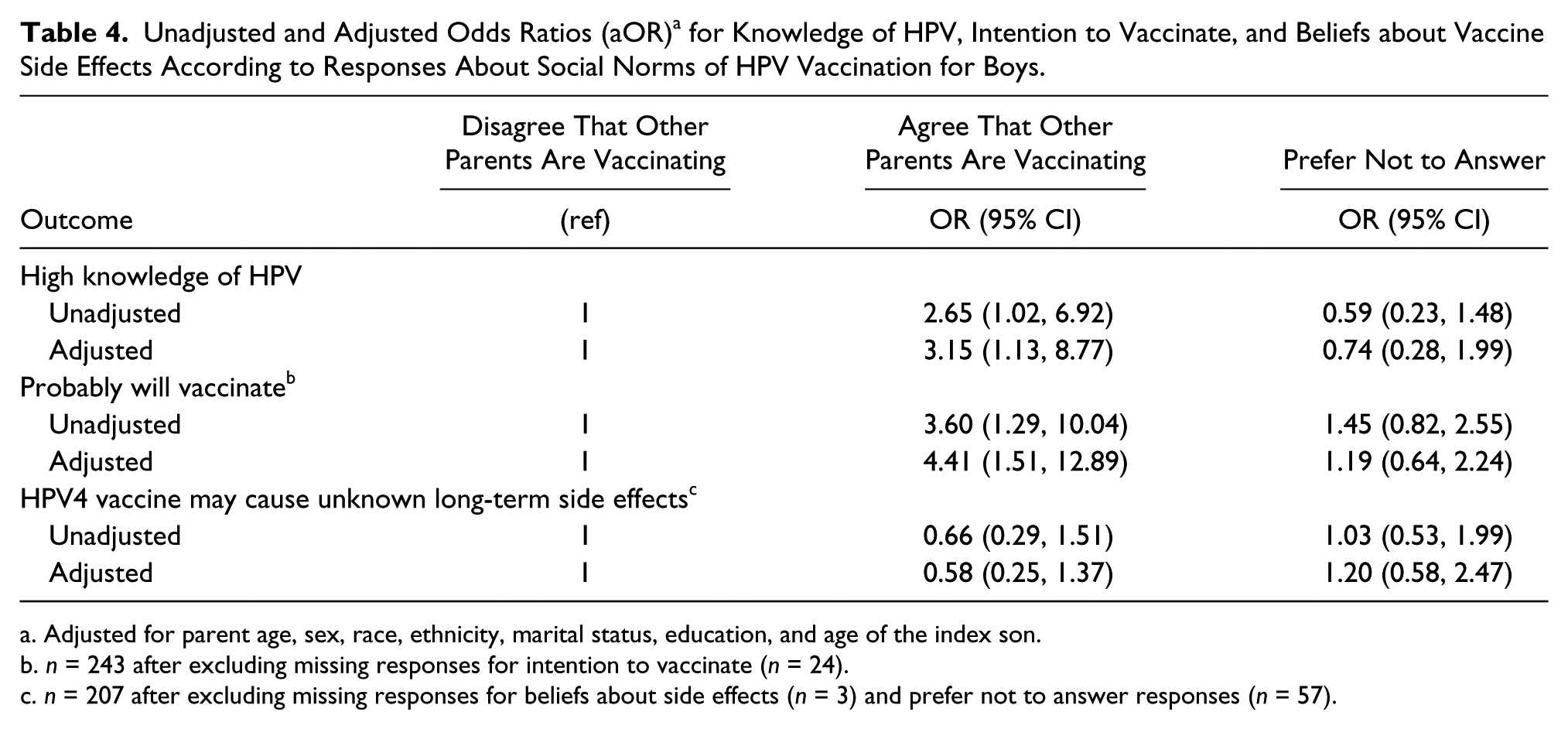
Adjusted for parent age, sex, race, ethnicity, marital status, education, and age of the index son.
n = 243 after excluding missing responses for intention to vaccinate (n = 24).
n = 207 after excluding missing responses for beliefs about side effects (n = 3) and prefer not to answer responses (n = 57).
Intention to Vaccinate
After excluding 24 parents who did not respond to the intention to vaccinate item, we found 63% of remaining parents (n = 154) reported they would probably vaccinate sons in the next year (15%, n = 36 definitely will; 49%, n = 118 probably will). Remaining parents responded they probably would not vaccinate (29%, n = 70) or definitely would not (8%, n = 19). Parents that agreed that others in their community were vaccinating sons had more than four times the odds of intending to vaccinate sons in the next year, compared to parents who did not agree others were vaccinating sons, in multivariate analyses (aOR = 4.41, 95% CI = 1.51, 12.89; Table 4).
Beliefs About Vaccine Side Effects
A substantial proportion of parents (21%, n = 57) in the analytic sample chose the prefer not to answer response regarding unknown, long-term side effects from HPV vaccine. Excluding these parents, and three missing responses, yielded an analytic sample of 207. Approximately 59% (n = 122) of these parents agreed that HPV4 vaccine may cause unknown, long-term side effects (14%, n = 28 strongly agree, 45%, n = 94 agree). Remaining parents disagreed (38%, n = 79) or strongly disagreed (3%, n = 6) with this statement. Parents that agreed other parents were vaccinating had lower odds of agreeing HPV4 vaccine may cause unknown, long-term vaccine side effects than their counterparts, but this estimate did not reach statistical significance (aOR = 0.58, 95% CI = 0.25, 1.37; Table 4).
Discussion
The findings of the present study highlight the relevance of beliefs about social norms of HPV vaccination in the context of vaccinating sons. The positive association between belief that others are vaccinating and high knowledge of HPV is consistent with one prior study (de Visser & McDonnell, 2008). Also consistent with some previous findings, parents in this sample agreeing others were vaccinating sons had greater intention to vaccinate (Dempsey et al., 2011; Dempsey et al., 2006). This is the first study dedicated to examining parents’ beliefs about social norms of HPV vaccination for boys in the context of beliefs about side effects of HPV vaccine. It this study sample, belief that other parents were vaccinating sons did not appear to carry with it significantly lower concern for unknown, long-term side effects of HPV vaccine.
Connections between parents’ beliefs about social norms of male HPV vaccination and high knowledge of HPV are interesting, but the reasons behind this association are not completely clear. It is plausible that parents who believed their peers were vaccinating sons developed greater interest in obtaining information about HPV, and therefore become better educated on the topic. Conversely, it is possible that parents who were quite knowledgeable about HPV disease better understood the rationale for vaccinating, and more often expected that others would vaccinate sons. The connection between knowledge of HPV and beliefs about social norms may be important to explore further, as improving parent knowledge has been reported, in some cases, to improve vaccine acceptance (Walhart, 2012).
Relationships between beliefs about social norms of vaccination and intention to vaccinate may be especially important, as this association may play a role in the evolution of HPV vaccine acceptance for boys over time. Capitalizing on, and publicizing, modest recent improvements in vaccination rates (Stokley et al., 2014) may be key to continuing improvements in vaccine uptake. Publicizing improvements in vaccine uptake in boys may inspire confidence in some parents about the merits of HPV vaccine, suggest that vaccinating boys is becoming more normative, and potentially drive further improvements in vaccination. Conversely, it is plausible that consistently emphasizing continued suboptimal vaccination rates may also resonate with parents, and doing so could potentially bolster confidence in decisions against HPV vaccine for sons. Consequently, studying the intended and unintended consequences of all messages, including marketing efforts and news stories about HPV vaccination rates in boys, may be relevant in anticipating future changes in vaccination rates.
Apart from intention to vaccinate, social norms are interesting to consider in relation to parents’ beliefs about side effects. Concerns still persist among parents about potential, and sometimes undocumented, side effects (Berenson & Rahman, 2012; Reiter et al., 2013; Schuler, Hanley, & Coyne-Beasley, 2014). It is plausible that parents’ concerns about side effects could be shaped, in part, by beliefs about social norms. If parents perceive that many others are vaccinating, this could potentially allay fears about side effects. However, if parents believe few others are choosing to vaccinate their sons, this could drive further skepticism about HPV vaccine and its possible side effects, and potentially contribute to a plateau in vaccination rates.
Although the estimate for the association between beliefs about social norms of male HPV vaccination and beliefs about side effects did not reach statistical significance, this association may be worthy of further exploration in future, larger studies. It is possible that the timing of our study influenced the association between parents’ beliefs about social norms and concern for side effects. Perhaps at the time of this study, before a routine recommendation for HPV vaccine for boys, concern for unknown, long-term side effects was more pronounced, and could not be mitigated by reassurance that others were vaccinating sons. Consequently, studying the relationship between beliefs about social norms and concern for side effects after the recommendation for routine male vaccination may be helpful.
It is notable in this study that a substantial proportion of parents selected the prefer not to answer response for the social norms item, approximately 37%. Interestingly, Hispanic ethnicity and lower educational level (high school education or less) were identified as factors significantly associated with choosing the prefer not to answer response. Given the very low number of participants of Hispanic ethnicity, no definitive conclusions can be drawn from this single finding, but beliefs about social norms among different ethnicities should be studied further. With regard to educational level, our findings may signify discrepancies in beliefs about social norms according to educational level that need to be further investigated. The proportion of parents who responded prefer not to answer may also indicate some degree of reluctance to comment on other parents’ practices, especially in light of the prior controversy around HPV vaccine (Colgrove, 2006).
This study has both limitations and strengths. Limitations of this study include that it was performed before the routine recommendation for HPV vaccine for males. This is a notable factor because of lack of a routine recommendation could potentially influence parents’ beliefs about social norms, general attitudes toward and concerns about HPV vaccine, and intention to vaccinate. This study was a cross-sectional study and was conducted in one geographical area, which limits the generalizability of results. It should also be noted that surveys provided to Spanish-speaking parents were not specifically designed to address cultural factors that may be specific to this population. Strengths of this study include that it was performed after licensure of HPV vaccine for males, and that it explored beliefs about vaccination norms in the context of factors currently relevant to vaccine decisions, including knowledge and concern for side effects (Stokley et al., 2014).
Conclusion
The findings of the present study highlight the importance of parents’ beliefs about social norms in the setting of HPV vaccine for boys. However, the true extent to which beliefs about social norms are important still remains to be fully determined in larger populations and over time. Beliefs about other parents’ practices with regard to HPV vaccine for sons are a potentially powerful factor. Although beyond the scope of this study, parents’ beliefs about their peers’ decisions and practices could potentially influence not only vaccination decisions, but a variety of other factors not explored in this study, including decisions to seek information about HPV, whether or not parents discuss HPV vaccine with their sons or their child’s health care provider, or even opinions about mandates for HPV vaccine. Further research should consider parents’ beliefs about norms of vaccination seriously in efforts to improve vaccination rates and investigate further whether beliefs about vaccination norms may be a contributing factor to vaccine refusal.
Footnotes
Author Note
Data used in this work are stored on servers at the University of North Carolina.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Christine L. Schuler received training grant support for Preventive Medicine from 2009 to 2010 from the American Cancer Society, which did not support this work. Tamera Coyne-Beasley received grant support from Merck And Co., Inc. (MISP 40108). This study was funded in part by Merck.
