Abstract
As the rate of HIV infection continues to rise among men who have sex with men (MSM) in the United States, a focus of current prevention efforts is to encourage frequent HIV testing. Although levels of lifetime testing are high, low levels of routine testing among MSM are concerning. Using data from an online sample of 768 MSM, this article explores how perceptions of HIV prevalence are associated with HIV testing behavior. Ordinal logistic regression models were fitted to examine correlates of perceived prevalence, and binary logistic regression models were fitted to assess associations between perceived prevalence and HIV testing. The results indicate that perceptions of higher prevalence among more proximal reference groups such as friends and sex partners are associated with greater odds of HIV testing. Perceptions of HIV prevalence were nonuniform across the sample; these variations point to groups to target with strategic messaging and interventions to increase HIV testing among MSM.
In 2011, 62% of newly diagnosed HIV infections among adolescents and adults in the United States were attributable to male-to-male sexual contact (Centers for Disease Control and Prevention, 2013). Four decades into the HIV epidemic, men who have sex with men (MSM) continue to be the main risk group, and data indicate some concerning trends of increasing engagement in risk behaviors (Beyrer et al., 2012; Jaffe, Valdiserri, & De Cock, 2007; Sullivan et al., 2009). Based on evidence that early detection of HIV infection and adoption of antiretroviral therapy reduces transmission potential (Marks, Crepaz, & Janssen, 2006; Marks, Crepaz, Senterfitt, & Janssen, 2005), current prevention efforts are focused on strengthening the continuum of care to maximize viral suppression and reduce the risk of new infections (Cohen et al., 2011; The White House Office of National AIDS Policy, 2010, 2013). Foundational to this strategy is HIV testing, to engage in care and proceed along the continuum toward viral suppression, individuals must first be tested to know they are HIV-positive. In recognition of high rates of HIV transmission among MSM, the Centers for Disease Control and Prevention recommends that sexually active MSM test at least once per year (Branson et al., 2006). Although levels of lifetime testing appear high, less than two thirds of MSM report having tested in the past 12 months (Oster et al., 2011), and, accordingly, approximately 44% of HIV-positive MSM are unaware of their sero-status (Smith et al., 2010).
One factor that may influence MSM testing behaviors is recognition of personal risk of HIV infection. Many health behavior theories, including the health belief model (Janz & Becker, 1984; Rosenstock, Strecher, & Becker, 1988), protection motivation theory (Floyd, Prentice-Dunn, & Rogers, 2000; Rogers, 1975), and precaution adoption process (Weinstein, 1988), posit that perceived vulnerability to a health threat is essential to adoption of preventative behaviors. Although sexual behavior is shaped by a complex set of contextual and psychological factors, including relationship status, perceived behavioral control, emotions, and substance use (Albarracín, Johnson, Fishbein, & Muellerleile, 2001; Gerrard, Gibbons, & Bushman, 1996; Janz & Becker, 1984; Kowalewski, Henson, & Longshore, 1997), data indicate that perceptions of vulnerability to HIV are associated with lower sexual risk behavior (e.g., fewer sex partners and lower levels of participation in UAI [unprotected anal intercourse]; Aspinwall, Kemeny, Taylor, Schneider, & Dudley, 1991; Kalichman, Simbayi, Cain, & Jooste, 2008; Klepinger, Billy, Tanfer, & Grady, 1993).
For a communicable disease like HIV, an individual’s risk of infection depends on the prevalence and infectiousness of the disease agent in the population to which he is exposed. Operationalized through metrics such as community viral load (Castel et al., 2012; Das et al., 2010; Montaner et al., 2010) and the proportion of the population with a viral load above a specified cutoff (Kelley et al., 2012), the burden of disease at the population-level has gained increasing recognition as an informative indicator of HIV transmission potential. Given the epidemiologic importance of this population-level variable and its role in shaping patterns of individual risk, it is relevant to consider how it is perceived by susceptible individuals and whether these perceptions shape behavior. Based on data from men and women recruited from an STI (sexually transmitted infection) clinic in Milwaukee, Kalichman and Cain (2005) proposed that people modify their behavior according to an intuitive sense of the prevalence of the health risk in the population—a phenomenon they termed
A handful of other studies lend support to the theoretical link between the perceived prevalence of a health threat, perception of personal vulnerability, and motivation to engage in a risky or protective behavior. In a study of women who have sex with women, participants who perceived a higher prevalence of human papillomavirus in their city were more likely to consider themselves to be personally vulnerable to infection (Eaton et al., 2008). Among injection drug users in San Francisco, Downing et al. (2001) report that participants described feeling more at risk for HIV if they lived in communities where the disease was more prevalent. Higher perceived local prevalence of HIV has also been linked to perceived risk and condom use in South Africa (Chao, Gow, Akintola, & Pauly, 2007; Kalichman et al., 2008) and in the United States (Klepinger et al., 1993). Focusing on associations with HIV testing, Shi, Kanouse, Baldwin, and Kim (2012) report that adults in Los Angeles who perceived HIV to be a serious health issue in their community were more likely to have tested for HIV in the past 2 years.
Notably, however, few studies have examined the influence of perceived prevalence on HIV risk-reduction behaviors among MSM. In light of the disproportionate burden of HIV among MSM in the United States, this presents a critical gap in the literature. Using data from a national online sample of 768 MSM, this article explores the role of perceived prevalence in shaping patterns of HIV testing for this important risk group. The first stage of analysis assesses social and demographic variations in men’s perceptions of the HIV prevalence in four reference groups of increasing familiarity: gay and bisexual men in the United States, gay and bisexual men in the participant’s city, his gay and bisexual friends, and his male sex partners. The second stage examines how these perceptions of prevalence are associated with men’s HIV test history and test frequency, controlling for the variations observed in stage one. Understanding the associations between perceived prevalence and HIV testing behavior among MSM has the potential to help refine messages and prevention efforts to promote the importance of routine HIV testing.
Method
Participants for this study were recruited through banner advertisements on Facebook targeting men in the United States whose profiles indicated that they are interested in men. Over 10 days in October and November 2012, 4,638 individuals clicked on the ads, of whom 1,793 (39%) started the survey and 1,739 (37%) consented to participation. Of those consenting, 37 were younger than 18 years (2%), 15 reported a gender other than male (0.8%), 335 reported that they had not had sex with a man in the past 6 months (19%), 15 lived outside the United States (0.8%), and 86 did not respond to one or more of these 6 eligibility criteria (5%). This resulted in a sample of 1,285 eligible men (74% of those who consented). For this analysis, self-reported HIV-positive men (81, 6%) were excluded from the sample to focus on those at risk of infection. Ethical approval for the study was obtained from the [Emory University ]Institutional Review Board.
To measure perceived prevalence, participants were asked to indicate the percentage of gay and bisexual men they perceive to be HIV-positive in the United States, in their city, in their friend group, and among their male sex partners. Participants could select from a dropdown menu of response options ranging from “fewer than 10%” to “90% to 100%.” Because of the small number of participants that selected a prevalence of 30% or greater among friends and sex partners (
Three variables were used to measure men’s patterns of HIV test behavior. The first indicator distinguished those who had ever tested from those who reported never having tested for HIV. In line with recent recommendations that MSM test as often as every 3 to 6 months (Oster et al., 2011), a second indicator was constructed to indicate whether men had tested in the 6 months preceding the survey based on the reported date of their last test. To further assess patterns of testing, participants were asked to select 1 or more items to describe how they typically decide to get tested: routinely, after UAI with someone whose HIV status is unknown, after UAI with someone known to be HIV-positive, before/when starting to have sex with a new partner, on noticing symptoms of an STI, whenever the opportunity arises, or when notified by a sex partner that he/she has an STI. Participants who reported routine testing were asked to indicate their frequency of testing. From these responses, an indicator of routine testing was constructed to identify men who reported testing on a regular basis, at least once every 12 months.
As covariates, the analysis included participant age (18-24, 25-34, 35-44, and ≥45 years), race/ethnicity (non-Hispanic White, non-Hispanic other, and Hispanic), educational attainment (high school or less, some college or a 2-year degree, and college or higher), employment status (employed part-time, employed full-time, and unemployed or retired), region of the county (West, Midwest, Northeast, and South), relationship status, and experience of intimate partner violence (IPV). Only 3% (
A total of 300 participants (24.9%) had missing data on HIV testing behavior, an additional 28 participants (2.3%) did not respond to one or more indicators of prevalence, and 142 (11.8%) had missing data on IPV or demographic indicators. The analysis was restricted to complete cases; accounting for these missing responses yielded a final analysis sample of 768 MSM. Excluded participants were more likely to be older (≤45 years;
The first stage of the analysis aimed to identify factors associated with each of the 4 measures of perceived prevalence. For each reference group—the United States, city, friends, and partners—an ordinal logistic regression model was fitted. These models each satisfied the proportional odds (parallel regression) assumption for ordinal regression. The second stage of analysis assessed the associations between the indicators of perceived prevalence and the three HIV testing outcomes, with separate logistic regression models fitted for each outcome. Models in both stages included as covariates: respondent age, race, educational attainment, employment status, region, relationship status, and experience of IPV in the past 12 months. Analyses were conducted using Stata version 12.0 (StataCorp LP, College Station, TX).
Results
The mean age of participants was 30 years and the modal age-group was 18 to 24 years (Table 1). Nearly 80% (604) of the sample was non-Hispanic White, 39% (302) had a college degree or higher education, 53% (410) were employed full-time, and 24% (176) were employed part-time. By region, 30% (223) of the sample reported residence in the West, 30% (233) in the South, 22% (167) in the Midwest, and 19% (145) in the Northeast. Slightly more than half of participants reported a main partner (431), and 31% (234) reported an experience of IPV in the past 12 months. The most commonly reported type of IPV was psychological (25%), followed by physical (12%) and sexual (8%).
Descriptive Statistics of an Online-Recruited Sample of Men Who Have Sex With Men in the United States (

Of the four reference groups, participants perceived the prevalence of HIV to be highest among gay and bisexual men in the United States and lowest among their male sex partners (Table 1). Nearly two thirds of the sample (61%; 467) indicated that the prevalence among gay and bisexual men in the United States is 20% or higher; in comparison, 45% (344) of participants perceived 20% or higher prevalence among gay and bisexual men in their city, 11% (82) perceived that level of prevalence among their gay and bisexual friends, and 7% (52) perceived high prevalence among their male sex partners. The proportions of the sample reporting a perceived prevalence of 10% or lower at the country, city, friend, and sex partner levels were 9% (70), 29% (222), 75% (572), and 89% (685), respectively. The vast majority of men (81% [623]) reported having ever been tested for HIV, yet only 36% (278) reported having tested in the past 6 months and 43% reported that they routinely test at least once per year.
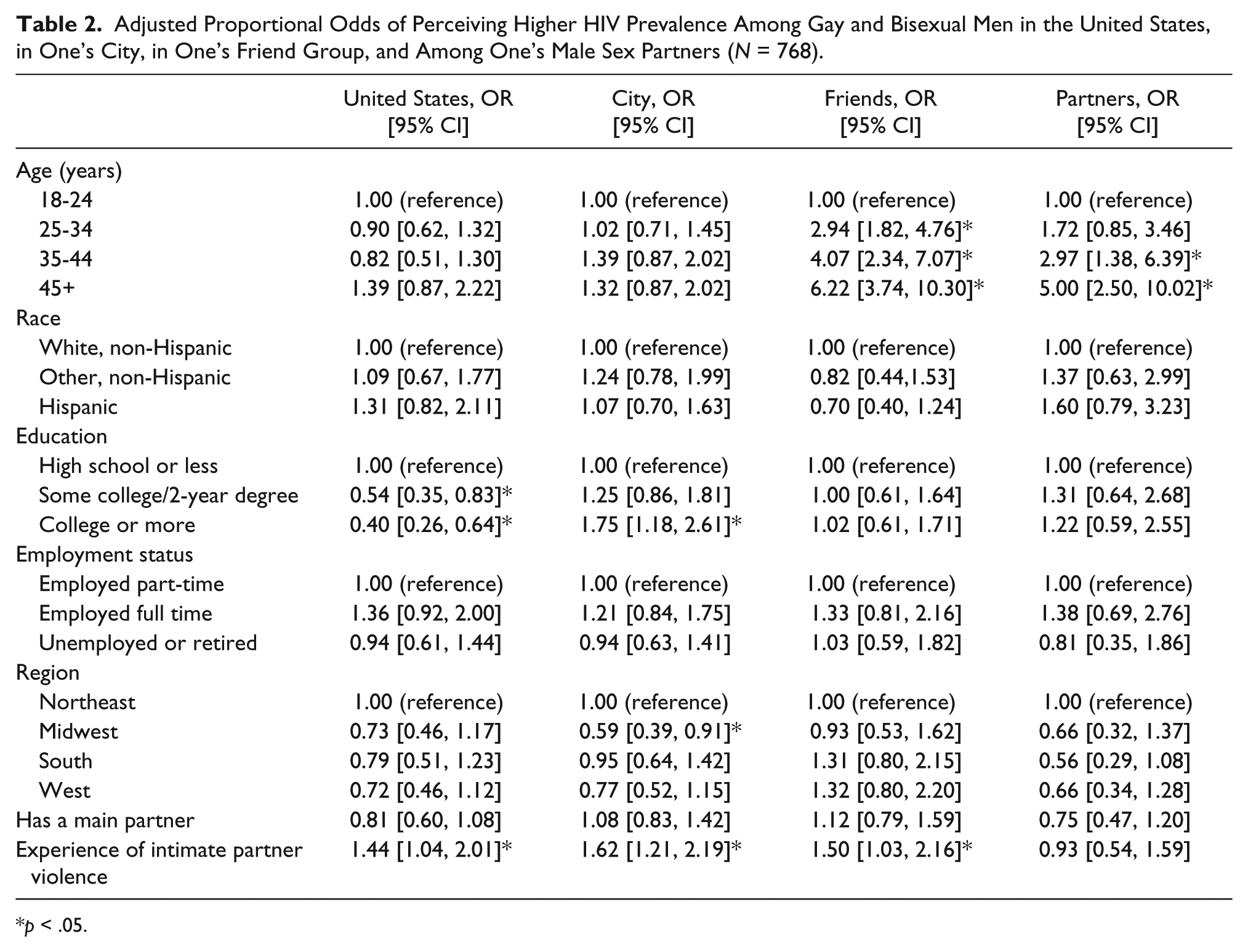
From the ordinal logistic regression models in Stage 1 of the analysis, inconsistent associations were observed across the four indicators of perceived HIV prevalence (Table 2). Relative to men with a high school education or less, the adjusted proportional odds (pOR) of perceiving higher prevalence among gay and bisexual men in the United States were 50% lower among participants with some college or a 2-year degree (pOR = 0.5, 95% confidence interval [CI] = [0.4, 0.8],
Adjusted Proportional Odds of Perceiving Higher HIV Prevalence Among Gay and Bisexual Men in the United States, in One’s City, in One’s Friend Group, and Among One’s Male Sex Partners (
The results from Stage 2 of the analysis indicate several associations between perceptions of HIV prevalence and testing behavior (Table 3). Independent of variation by age and education, participants who perceive 10% to 19% HIV prevalence among their friends had 2.8 times the odds of having ever tested for HIV relative to participants who perceive the HIV prevalence to be less than 10% (OR = 2.8, 95% CI = [1.3, 6.2],
Adjusted Odds of Having Ever Tested for HIV, Having Tested in the Past 6 Months, and Testing Routinely (

Discussion
The results of this analysis suggest that perceptions of HIV prevalence are associated with HIV testing behaviors among MSM in the United States. The use of four reference groups to assess perceived prevalence provided nuance to the measure, allowing for comparison of associations as the reference group became more proximal to the participant. Adjusting for the sociodemographic variations in men’s perceptions observed in Stage 1 of analysis, perceiving higher prevalence among friends and sex partners was associated with higher odds of lifetime and routine testing. These findings suggest that targeted messaging aimed at increasing recognition of HIV prevalence in men’s personal social and sexual networks has the potential to contribute to efforts to promote HIV testing.
From the first phase of analysis, variations in perceived prevalence by age and educational attainment point to possible differences in men’s understanding of the epidemic. Unfortunately, due to uncertainty in the size of the MSM population, actual prevalence data are lacking at the subnational level, such that the analysis is unable to consider the accuracy of men’s perceptions in reference to their cities. In the United States overall, estimates of the prevalence of HIV among MSM fall between 9% (Xu, Sternberg, & Markowitz, 2010) and 19% (Centers for Disease Control and Prevention, 2010), suggesting that the majority of participants in this study overestimated national HIV prevalence. Evidence from prior research indicates that people are inaccurate at estimating the probability of rare events (Kowalewski et al., 1997), often relying on heuristics. The increased odds of perceiving higher HIV prevalence among participants in older age-groups, for instance, may reflect the influence of the availability heuristic (Tversky & Kahneman, 1973); men in older age-groups are more likely to have encountered more people with HIV/AIDS, which has been reported to increase perceptions of prevalence and personal risk (Downing et al., 2001; Klepinger et al., 1993). Additionally, the nature and content of media and programmatic messages on HIV/AIDS that men have been exposed to may vary by age cohort, resulting in different outlooks on the severity and impact of the disease. Men who were sexually active during the start of the epidemic, for example, may perceive of HIV as a more serious threat than younger MSM who have grown up in the age of ART (antiretroviral therapy). Since 2004, HIV incidence has been increasing among young MSM more than any other risk group (Prejean et al., 2011), and HIV-infected young MSM are more likely to be unaware of their infection than older HIV-infected MSM (Smith et al., 2010). These patterns point to a need to target specifically younger MSM with messages aimed at increasing awareness of the prevalence of HIV and their own risk of infection.
The association between higher educational attainment and higher perceived HIV prevalence at the city level may indicate that men with more education have received more information about the magnitude of the epidemic. Perhaps men with lower levels of educational attainment are more likely to distance themselves from the epidemic by assuming lower risk in their community than in the United States overall. Another possible explanation is that the observed associations are driven by socioeconomic status and patterns in place of residence. Men with higher education may be more likely to live in urban centers, where the HIV epidemic is more concentrated (Centers for Disease Control and Prevention, 2008; Hall, Espinoza, Benbow, & Hu, 2010). Men may also have the ability to move to areas with a higher density of gay and bisexual men. In this case, perceptions of relatively high local prevalence may reflect actual trends. Better data on actual HIV prevalence among MSM at the city level are needed to understand and assess the implications of these patterns.
The associations between experience of IPV and perceptions of higher HIV prevalence suggest that men who experience IPV recognize greater vulnerability to HIV. Men who reported recent IPV were more likely to perceive higher HIV prevalence among gay and bisexual men in the United States, their city, and among their friends. Prior research has established a link between the experience of IPV and poor mental health (Houston & McKirnan, 2007; Stall et al., 2003); the findings from the current study may reflect a tendency for men who have been abused to have a more negative or fatalistic outlook. However, the lack of association between experience of IPV and perceived prevalence among male sex partners is perplexing. One possible explanation is that the measure of perceived prevalence used in this study was too crude to detect differences in reference to male sex partners; only 11% of the sample (
Considering HIV test behavior, this analysis indicates that the strength and direction of the associations with perceived prevalence depend on the reference group for which prevalence is assessed. Perceiving higher prevalence among friends and sex partners was associated with greater odds of testing, while perceiving higher prevalence among men in one’s city had a null association with testing, and perceiving higher prevalence among men in the United States was marginally associated with
In interpreting these findings, it is important to note that perceptions of HIV prevalence are one of many factors that influence testing behavior. Prior research has pointed to the influence of constructs such as self-efficacy, perceived behavioral control, perceived benefit from testing, and perceived severity of HIV infection (Albarracín et al., 2001; Floyd et al., 2000; Janz & Becker, 1984; Lau et al., 2012), which were not assessed in this study. Many subjective factors also influence perceptions of the risk posed by specific partners, including physical attractiveness and the level of intimacy and trust (Agocha & Cooper, 1999; Kowalewski et al., 1997; Lorenc et al., 2011; Mitchell & Horvath, 2013; Schmälzle, Renner, & Schupp, 2012). Furthermore, the decision to test may not be rational. From a systematic review of barriers to testing among gay and bisexual men, Lorenc et al. (2011) report that some men avoid testing for fear of dealing with the consequences of receiving a positive result or fear of stigma. Among men with main partners, the presence and type of sexual agreement could influence men’s test behavior as well (Mitchell, 2014; Mitchell & Horvath, 2013). In particular, men with monogamous agreements may not perceive a need for routine testing if they believe their partner to be HIV-negative, despite evidence that stepping outside the terms of agreement is common and often undisclosed (Gass, Hoff, Stephenson, & Sullivan, 2012; Gomez et al., 2012; Mitchell, 2014). Future studies should consider including measures of these other constructs alongside to perceptions of prevalence to better understand the contributions of each factor to HIV testing and sexual behavior.
An additional limitation is that this study was cross-sectional, such that the associations cannot be interpreted as causal. As reported by Gerrard et al. (1996), many health behavior theories, including the Health Belief Model, Protection Motivation Theory, and Precautionary Adoption Process, assume that the link between perceptions of vulnerability and behavior is reciprocal. Past behavior is thought to influence perceptions of risk and vulnerability, which in turn influence future behavior. Extending this reasoning to the present study, it is possible that men who test for HIV are more likely to perceive higher prevalence in their networks, perhaps due to counseling and information received during testing. Further research using longitudinal data is needed to explore the causal nature of the associations. Future studies should also ask participants to indicate how many people they know to be HIV-positive, as this factor likely shapes perceptions. Finally, the results of this study may not be generalizable to all MSM. Although the demographic characteristics of the sample are consistent with other online-recruited samples of MSM (Chiasson et al., 2007; Mitchell & Horvath, 2013; Mustanski, 2007), given the disproportionate rate of HIV infection among Black MSM (Lieb et al., 2011; Prejean et al., 2011), future research should examine perceptions of prevalence among more diverse samples.
Despite these limitations, the results of this study contribute to understanding of HIV test behavior and have important programmatic implications. Demographic variations in perceptions of prevalence point to groups to target with programming and messages to enhance their understanding of the epidemic. To get men to seek testing for HIV, the results from this study indicate that it is important to focus on perceptions of HIV prevalence among proximal reference groups, such as friends and sex partners. Rather than presenting information on the prevalence of HIV among gay and bisexual men as a whole, data indicate that messages and interventions should aim to overcome optimism bias and encourage men to recognize that people in their own networks could be HIV-positive and that frequent HIV testing is critical to protecting their health and the health of their partners.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This original research was supported by funding from Emory Center for AIDS Research under Grant P30 AI050409.
