Abstract
The Centers for Disease Control and Prevention and Healthy People 2020 call for improvements in meeting men’s reproductive health needs but little is known about the proportion of men in need. This study describes men aged 35 to 39 in need of family planning and preconception care, demographic correlates of these needs, and contraception use among men in need of family planning. Using data from Wave 4 (2008-2010) of the National Survey of Adolescent Males, men were classified in need of family planning and preconception care if they reported sex with a female in the last year and believed that they and their partner were fecund; the former included men who were neither intentionally pregnant nor intending future children and the latter included men intending future children. Men were classified as being in need of both if they reported multiple sex partners in the past year. About 40% of men aged 35 to 39 were in need of family planning and about 33% in need of preconception care with 12% in need of both. Current partner’s age, current union type, and sexually transmitted infection health risk differentiated men in need of family planning and preconception care (all
Introduction
The Centers for Disease Control and Prevention (CDC) guidelines recommend “women and
Studies have reported that the majority of men believe they share equal responsibility with their female partners for decisions about contraception and about 80% of men aged 35-44 report no future desire for children (Grady, Tanfer, Billy, & Lincoln-Hanson, 1996; Heinemann, Saad, Wiesemes, White, & Heinemann, 2005; Mitchell, Levis, & Prue, 2012). However, estimates of men in need of family planning are lacking. Policy makers in the United States assess “women in need of family planning” as (1) being sexually active, (2) believing that they and their partner are fecund, and (3) neither intentionally pregnant nor trying to become pregnant (Sonfield, 2006). This measure only accounts for male partners who are sterilized thus rendering a female not in need of family planning. For women, the most recent U.S. estimate finds that about 56% (37.4 million) are in need of family planning services and about 43% (16.0 million) of those in need are aged 30 to 44 (Frost, Zolna, & Frohwirth, 2013). Similar estimates for men can provide a greater understanding of men in need of family planning and specifically those men and their partners who are in need of contraception.
The goal of preconception care is to optimize a woman’s health prior to conception of a first or subsequent pregnancy in an effort to reduce adverse maternal and infant outcomes such as preterm birth, low birth weight, and infant mortality (Dunlop, Jack, & Frey, 2007; K. Johnson et al., 2006). More recent efforts recommend inclusion of males as part of preconception care to be attuned to “anticipatory fatherhood” and minimize gender disparities (Waggoner, 2013). Specific benefits of preconception care for men include improving men’s genetic and biologic contributions to a pregnancy, involving men in planning and spacing of pregnancies, and improving men’s overall health (Frey, Navarro, Kotelchuck, & Lu, 2008). Policy makers in the United States assess preconception care needs among women with recent live births in select states via the Pregnancy Risk Assessment Monitoring System (D’Angelo et al., 2007), but this represents a retrospective review of service receipt after a birth. The most current estimate identified that among all women with recent live births about 30% reported prepregnancy health counseling receipt, and among women aged 35 and older 42% reported such care (D’Angelo et al., 2007). Although a recent national survey identified 11% of men aged 18 to 64 reported having seen, heard, or read anything about recommendations for women’s preconception health from their health care provider, this study did not examine the proportion of men in need of preconception care (Mitchell et al., 2012). Estimates for men in need of preconception care can provide a greater understanding of men needing preconception health services.
Healthy People 2020’s and the CDC’s objectives call for increasing men’s access to reproductive health services (U.S. Department of Health and Human Services, 2010) and preconception care (K. Johnson et al., 2006), respectively. Receipt of such services by men in need can improve men’s overall health and benefit the health of men as well as their partners. Understanding how men in need of family planning and preconception care in their mid-30s vary by their background characteristics can assist in identifying strategies to target services and education to this population. Thus, the goals of this study are to examine (1) the proportion of men in need of family planning and preconception care in their mid-30s, (2) how needs vary by men’s background characteristics, and (3) among men in need of family planning, levels of current partner hormonal method and condom use in the past year and characteristics of men reporting less than 100% of either using the fourth wave of the National Survey of Adolescent Males.
Methods
Conceptualization of Men in Need Measures
Measures of men in need of family planning and preconception care were conceptualized by modifying the women’s measures and considering multiple sexual partners since
Men in need of family planning are those who have had sex with a female in the past year, fecund, have at least one fecund partner who is not currently pregnant, and do not intend to have future children.
Men in need of preconception care are those who have had sex with a female in the past year, fecund, have at least one fecund partner, and intend to have children.
Data Source and Procedures
Data analysis used data from Wave 4 (collected 2008-2010) of the NSAM. NSAM began in 1988 with a nationally representative multistage area probability sample of noninstitutionalized never-married males aged 15 to 19 with a response rate of 74% (
Variables Contributing to Men in Need Measures
NSAM survey questions about men’s sexual and reproductive health were used to define men in need measures. Sexual behavior questions asked respondents about ever having had sexual intercourse, ever having had sex with a female, having had vaginal sex in the past 12 months, and ever having done any of the following with a male (ever received and/or gave masturbation, oral sex, or anal sex; current, other recent, or past partner was ever male; or in past 12 months used the Internet to find a male sex partner(s)). Based on responses to these questions, respondents were coded as never having had sex, having had sex only with males, or sexual behavior in the past year with a female. Respondents were considered fecund if they reported no vasectomy or physical condition that makes it difficult or impossible to have a child. Men who reported their partner did not have a physical condition that makes it difficult or impossible to have a child or was not sterilized were considered to have a fecund partner. Respondents indicating that they had a currently pregnant partner were coded as such. Respondents who replied yes to the question “Do you intend to have a child/another child sometime?” were coded as intending to have future child(ren). Men were coded as having multiple sexual partners if they recorded two or more partners in the past 12 months. Data were collected about every partner’s sterilization status but data regarding partner’s physical ability to have children was only available for the current partner. Respondents with multiple partners who were fertile and met prior criteria were designated as being in need of family planning and/or preconception care; all respondents reported at least one nonsterile partner.
Background Characteristics
Sociodemographic factors included participants’
Family Planning Method Use
Respondents reported on the percentage of time they used a condom and the percentage of time their current partner used a hormonal method of contraception in the past year, respectively. Responses ranged from 0 to 100 and responses were coded as none of the time (0%), some of the time (1% to 99%), or all of the time (100%) for condom and hormonal use, respectively.
Data Analysis
Frequencies of the indicators contributing to the classifications of men in need or not in need categories were generated (Table 1), and men were classified as being in need of family planning, preconception care, both, or neither. Frequencies and cross-tabulations were then conducted to examine participants’ characteristics in general and by need measures using bivariate Poisson analyses to assess associations (Table 2). Poisson analyses were applied to calculate a relative risk (RR) because odds ratios overestimate RR when the outcome event is common (incidence of ≥10%; Barros & Hirakata, 2003). Next, among men in need of family planning, frequencies of condom and hormonal birth control use with current partner were generated (Table 3), and bivariate Poisson analyses were conducted to examine associations between each participant characteristic with 100% versus <100% condom and current partner hormonal method use, respectively. All analyses were weighted to be nationally representative, adjusting for NSAM’s clustered sample and overrepresentation of Black and Hispanic respondents, and also taking into account screening nonresponse rate, interview nonresponse rate, and attrition (Ku, Williams, Lindberg, Pernas, & Martinez, 1999). Given the relatively large sample size and multiple tests, stringent criteria (
Men in Need of Family Planning and Preconception Care.
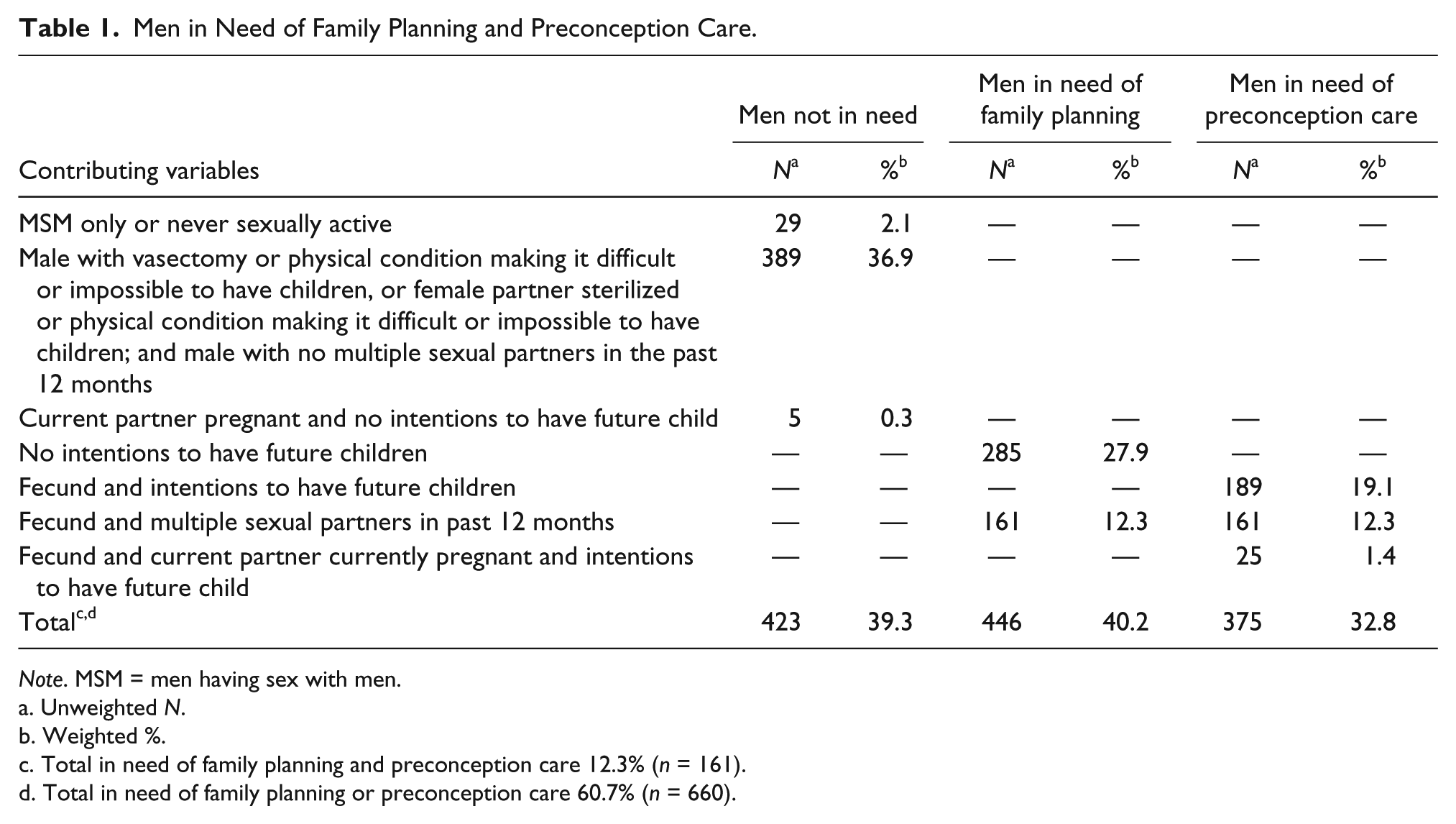
Unweighted
Weighted %.
Total in need of family planning and preconception care 12.3% (
Total in need of family planning or preconception care 60.7% (
Participants’ Background Characteristics, Percentage of Men in Need Among Background Characteristics, and Association Between Background Characteristics With Being in Need.

Unweighted
Weighted %.
Data represent unadjusted RR and 95% CIs from separate bivariate Poisson regression models examining the association between participants’ background characteristics with being in need of family planning and preconception care. Significant findings are bolded.
Modeled as a continuous variable.
Based on 2008 national averages.
Level of Current Partner Hormonal and Condom Use Among Men in Need of Family Planning Who Were Sexually Active in the Past 12 Months (

Unweighted
Weighted %.
Missing data = 53 cases (13.4%).
Missing data = 33 cases (9.1%).
Results
Forty percent of men (
About 39% (61%;
Background Characteristics of Men in Need
The percentage of men in need of family planning varied by current partner’s age, union status, and STI health risk (all
The percentage of men in need of preconception care varied by current partner’s age and respondents’ race/ethnicity, current union status, and STI health risk (all
Levels of Current Partner Hormonal Method and Condom Use Among Men in Need of Family Planning
The majority of men in need of family planning reported in the past 12 months their current partner used a hormonal method none of the time (55%;
Discussion
This study highlights among men aged 35 to 39, 40% were in need of family planning and 33% in need of preconception care. Furthermore, among men in need of family planning, only about one quarter reported using condoms all the time and one fifth reported their current partner used hormonal methods all of the time.
This is one of the first studies to use a similar approach that has been used to define women in need of family planning to describe the proportion of men in need of family planning. This study also examined men with future child intentions and described the proportion of men in need of preconception care. Both measures incorporated an additional factor from the original definition—that of multiple sex partners in the past year—without which men in need for family planning would have been underestimated by about 12%. Furthermore, these same men reported intentions to have future children with at least one of their partners and thus were identified to be in need of both family planning and preconception care. Gaining a better understanding of men in need of reproductive care is important to understand the proportion of men in need of such services, how to better target services to this population, as well as track those who receive or do not receive related services. Future work should consider applying the measurement strategy used here to describe men in need of family planning and preconception care among a wider age-range of men as well as examine their access to appropriate care.
This study identified that among men aged 35 to 39 in need of family planning who were sexually active in the past year, less than one quarter reported all of the time partner hormonal method use or condom use. These findings are relatively consistent with 2002 data from the National Survey of Family Growth (NSFG; Martinez, Chandra, Abma, Jones, & Mosher, 2006). However, the NSFG tabulations on condom and partner hormonal method use in the past year consider all men within an age group, rather than just among men who are in need as defined in this study; thus, NSFG estimates represent the entire population and may underestimate the reporting of men’s and their partners’ contraceptive method use. The NSFG tabulations on contraception method use also do not account for men with multiple partners or respondents’ partners’ fecundity status. Findings from this study highlight the need to identify strategies to improve contraceptive behaviors among men in their mid-30s as well as that of their partners since interventions with this age group has historically received little attention. Preliminary findings from a large-scale national evaluation suggest that recruitment of males through clinic outreach and in-reach, restructuring clinic environments, and training clinic staff on the delivery of male services results in an increase in male patients and ultimately may translate in increased receipt of family planning services (D. M. Johnson Warner, Carlon, & Fine, 2014).
This study identified similar participant background characteristics differentiated men in greater need of family planning and preconception care (i.e., participants with current partners 29 years old or younger, not in a union and not cohabiting, and high STI health risk) that can serve as targets for potential interventions. These findings should not be too surprising and are consistent with other studies that have reported increased risk of unintended pregnancy and STIs among college-aged men with younger aged partners (Manlove, Terry-Humen, & Ikramullah, 2006). These findings also highlight the need to better integrate STI, family planning, and preconception care services for men as has been highlighted for women (Farr, Kraft, Warner, Anderson, & Jamieson, 2009).
Race/ethnicity also differentiated men in greater need of preconception care (with Black and Hispanic males in greater need than White males). These findings are consistent with U.S. natality data (2011) that reports higher birth rates for Black men aged 35 to 39 (66.7 births per 1,000) than similarly aged White males (62.5 births per 1,000; U.S. father’s birth rate data are not reported by ethnicity; Hamilton, Martin, & Ventura, 2013). Although guidelines for preconception care are not specific with respect to race/ethnicity, one study reported that among male and female clients aged 13 to 44 seeking reproductive health care desired timing of childbearing varied by race/ethnicity (Foster, Biggs, Ralph, Arons, & Brindis, 2008). In this study, more White clients were identified to be seeking to delay pregnancy than Latino or African American clients, and more Latino and African American clients were identified to be currently pregnant or seeking pregnancy or want no more children.
This study identified that men in need of family planning who also did not use condoms 100% of the time reported having current partners 29 years old or younger (representing more than half of 9% of the sample in need or about 5% of the total sample). Lack of consistent condom use may be one of the contributing factors, in part, to the high rates of unintended pregnancy among women aged 20 to 29 (Finer & Zolna, 2011). Future work should consider examining event specific contraceptive method use since it is possible that more than one method is being used by couples to prevent pregnancy that cannot be measured here. Future research is also needed to gain a better understanding of the factors associated with men in need of family planning who are also in need of using contraceptive methods including condoms and partner hormonal methods since this study was not able to differentiate these men by their background characteristics.
Overall, study findings highlight the need to identify strategies to promote well-men’s care among men in their mid-30s that effectively integrates sexual and reproductive health to ensure men receive appropriate family planning or preconception care since many of these services aim to improve men’s overall health. One such approach is the promotion of men to make a reproductive life plan to assist them in considering their family planning and/or preconception care needs. Health care providers may also need to take a more proactive approach with their male patients by assessing reproductive life plans so that patients’ contraception histories can be better understood in context. Although adult men do not need to see a doctor to get condoms, findings from this study suggest that health care providers who see men of this age group may also want to address these men’s partners’ hormonal method needs. Among men with preconception care needs, such care can provide an opportunity to address their overall health and, specifically, optimize their health prior to a planned pregnancy. Although the impact of preconception interventions on men’s reproductive capacity, the subsequent pregnancy, and infant outcomes have yet to be conducted, it is known that certain medical conditions, medications, substance abuse, STIs, and exposure to occupational and environmental toxins can negatively influence a man’s future reproductive capacity (Frey et al., 2008; Jack et al., 2008). Furthermore, it is possible that some men with preconception care needs may also have other concerns, such as concerns about their fertility that was not assessed in this study. For example, according to the NSFG, men aged 30 or older are twice as likely to report an infertility problem as compared with males aged 15 to 29 (Martinez et al., 2006). Estimates of men with concerns about infertility would be more precise when considering infertility concerns among men in need of preconception care.
This study has a number of limitations. Estimates described in this study were representative of men aged 35 to 39 who resided in the United States in 1988. Men who immigrated to the United States after the initial cohort was recruited in 1988 were not represented. Furthermore, estimates were dependent on information solicited by the survey. In 2008 to 2010, the instrument asked only about future child intentions but did not clarify whether the child was desired immediately or sometime in the future. This lack of clarity may have potentially deflated the percentage of men in need of family planning and inflated the percentage of men in need of preconception care. Since the study sample was composed of men in their mid-30s; however, the majority may be closer to the end of their childbearing and the estimate may be more accurate than one developed for younger aged men. Finally, for 12% of the sample with more than one partner in the past year, physical inability to have children was not assessed for all partners. While this may have led to an overestimate of men in need, this is probably minor as it is unlikely that all nonsterile partners have a physical inability to have children. Offsetting these limitations were the study’s reliance on data from a national sample of men.
Conclusions
This study highlights that about 40% of men aged 35 to 39 are in need of family planning, 33% in need of preconception care, and 12% are in need of both secondary to involvement with multiple sex partners. Furthermore, among men in need of family planning, all of the time use of condoms and current partner use of hormonal methods was reported by less than one quarter of these men, respectively. Future work should apply the measures used in this study to describe family planning and preconception needs among a wider age range of men and evaluate the extent to which these men receive related services.
Footnotes
Authors’ Note
The sponsor (National Institute for Child Health and Human Development) had no role in the study design, collection, analysis, data interpretation, report, or decision for submission.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Freya L. Sonenstein, Nan M. Astone, Joseph H. Pleck, Jacinda K. Dariotis, and Arik V. Marcell, MD, MPH, has funding support provided by the National Institute for Child Health and Human Development (RO1 HD036948).
