Abstract
Sexual activity is an important aspect of life in patients with spinal cord injury (SCI), rated as one of the top priorities for recovery of function. This study was conducted to establish an understanding of the severity of erectile dysfunction (ED), a major component of male sexual activity, and its correlates in patients with SCI in our community. In a cross-sectional study, 37 male veterans with SCI admitted for regular follow-up at our center were recruited. Demographic and SCI-related descriptive information was gathered through a self-administered questionnaire. Sexual Health Inventory for Men was used to assess the presence and severity of ED. Euro Quality of Life questionnaire and General Health Questionnaire (GHQ-12) were also administered. The mean age of the participants was 45.7 ± 6.5 years with injury duration of 24.7 ± 6.2 years. Mean GHQ-12 score of 3.65 ± 3.38 and mean Sexual Health Inventory for Men score of 11.57 ± 5.28 were measured. All participants had ED, and 27% were suffering from severe ED. Sleep deprivation, worse GHQ-12 score, and hypertension were significantly associated with higher risk of much severe ED (p < .05). In conclusion, ED is a common problem in veterans with SCI and is inversely associated with their general health status.
Keywords
Introduction
Sexual activity is an important aspect of life in patients with spinal cord injury (SCI) in both recreational and reproductive viewpoints. Sexual activity is rated as the first priority for recovery of function in paraplegics and the second among those with tetraplegia, after regaining arm and hand function (Anderson, 2004). Previous studies have reported that patients with SCI remain interested in sexual relationships, but the level of desire and the frequency of sexuality are decreased after injury (Benevento & Sipski, 2002; Reitz, Tobe, Knapp, & Schurch, 2004). Erectile dysfunction (ED), a major component of male sexual activity, is defined as “the inability to attain and/or maintain penile erection sufficient for satisfactory sexual intercourse”(p. 28), (NIH Consensus Conference, 1993) and is of mixed etiology that may be either predominantly psychogenic or organic (Rahimi-Movaghar & Vaccaro, 2012). “Erectile response is a vascular event initiated by neuronal actions and maintained by a complex interplay between vascular and neurological events”(p. 9), (NIH Consensus Conference, 1993). There are two nervous pathways for erectile function: (1) Reflexive, originating from the sacral segments (S2-S4) involving the parasympathetic center; (2) Psychogenic, originating from the thoracolumbar segments (T11-L2) involving the sympathetic center. After SCI, the level and the completeness of the injury will be the major predictive factors for the type of ED. Patients with complete upper motor neuron injuries above the T11 level will not have psychogenic erections, but the reflex erections may be preserved in these patients and patients with complete lower motor neuron injuries may not experience reflex erections but may still have psychogenic erections depending on the degree of preserved neurological function in the T11-L2 spinal level (Benevento & Sipski, 2002). Although high in prevalence (Taghipoor et al., 2009), ED has been allocated a low priority with regard to research topics and funding in SCI researches (Anderson, Borisoff, Johnson, Stiens, & Elliott, 2007b). The association of sexual function after SCI with quality of life is well clarified (Fisher et al., 2002; Kennedy, Lude, & Taylor, 2006; Reitz et al., 2004), and the past attitudes that people with SCI should be happy to be alive and should learn to live without sexual pleasure is outdated (Anderson, Borisoff, Johnson, Stiens, & Elliott, 2007a); hence, in order to provide the SCI patients with incremental functional recovery, we need to establish an understanding of the severity of ED and its correlates such as demographics, SCI related, lifestyle, general health, and quality of life factors in the SCI patients in our community. In the present article, ED and its correlates are evaluated in a population of veterans with SCI using a self-administered questionnaire.
Materials and Method
In a cross-sectional study performed between May and August 2011, the male veterans with SCI admitted to Khatam-Ol-Anbia Hospital for regular follow-up were recruited in the study. The patients were provided with a self-reported questionnaire accompanied by an introductory statement explaining the purpose of the survey, directions for participating, the right to privacy, and what the results were to be used for. This information served as the informed consent statement, as required by the institutional ethics committee.
A general questionnaire covering demographic and SCI-related descriptive information, as well as information related to general health status, quality of life, and sexual function was developed to assess the possible associations between sexual function and other factors. The participants’ quality of life was assessed using EuroQoL (EuroQoL Group, 1990), which consists of EuroQoL 5-Dimensions 3-Levels questionnaire and EuroQoL Visual Analog Scale (EQ-VAS) to describe five dimensions of mobility, self-care, usual activities, pain/discomfort, and anxiety/depression in three levels of no problems, some problems, and extreme problems and also to obtain a subjective quantitative health status (a health ruler with minimum level of 0 and maximum level of 100 was provided to the patients). General Health Questionnaire (GHQ-12; Goldberg & Hillier, 1979) was also applied to assess general well-being; the GHQ-12 is a measure of current mental health that focuses on two major areas of inability to carry out normal functions and appearance of new and distressing experiences. The patients were also asked if they felt recovered after night sleep and if they experienced problems going to sleep. Sexual Health Inventory for Men (SHIM; Rosen, Cappelleri, Smith, Lipsky, & Pena, 1999), which is an abridged and slightly modified 5-item version of the 15-item International Index of Erectile Function (Rosen et al., 1997), was used; the questionnaire is designed as an easily administered, patient-reported assessment tool to assess the presence and severity of ED in clinical settings and is intended to assess sexual function over the past 6 months. SHIM asks about five dimensions of sexual function in the form of confidence to keep an erection, keeping a penetrative erection, maintaining an erection, completion of intercourse, and having a satisfactory intercourse. All questionnaires had been previously translated and validated in Persian (Alipour, Ghaffari, Jensen, Shariati, & Vingard, 2007; Montazeri et al., 2003; Nikoobakht et al., 2012). Height was measured using a wall mounted stadiometer for patients able to stand erect and using supine stadiometer for those unable to stand. Patients’ weight was measured by subtracting the wheelchair weight from patient and wheelchair total weight on a wheelchair balance scale. For able-bodied patients, weight was measured standing on the same scale. Body mass index of the patients was calculated using the “weight/(height)2” formula. The level of injury and presence of pressure ulcer were confirmed by a neurosurgeon; however, no further attempt was made to validate the respondents’ answers with medical records. For demographic and SCI-related questions, a list of answers was provided for each question to assist in standardization of the responses. Using the conventional scoring for GHQ, the mean GHQ score for the whole population of respondents was used as the cutoff threshold for presence of an indication of mental health problems (Goldberg, Oldehinkel, & Ormel, 1998). The scores of SHIM questionnaire were interpreted (Rosen et al., 1999) as follows: 22 to 25 for no ED, 17 to 21 for mild ED, 12 to 16 for mild-to-moderate ED, 8 to 11 for moderate ED, and 5 to 7 for severe ED.
Statistical analysis was conducted using SPSS software version 16.00 (SPSS Inc., Chicago, IL). Quantitative values are expressed as the M ± SD and compared using Student’s t test. The chi-square test or Fisher’s exact test was applied to compare the proportions. Level of statistical significance was set as p < .05.
Results
A total of 134 SCI patients were admitted to Khatam-Ol-Anbia Hospital, in Tehran, Iran, during May 2011 to August 2011; however, 62 patients were either not able or not willing to participate in the study, resulting in survey return rate of 53.73%. A total of 35 subjects refused to answer the SHIM questionnaire or partially completed the questionnaire, leaving 37 cases (27.61%) for final analysis. According to the low response rate and to identify that our sample was not biased, a random sample of 25 patients who did not fill the questionnaire was prepared and the two samples were compared in terms of demographic and medical characteristics. As the differences were not significant, the data are not reported here. Demographic and SCI-related descriptive information of the 37 survey respondents are presented in Table 1. As most injuries had occurred during Iran–Iraq War from 1980 to 1988, mean age of 45.72 ± 6.46 years and mean time since SCI of 24.68 ± 6.22 years were recorded. All the patients were living with their spouses.
Demographic Characteristics of the Study Population (M ± SD or N, %) a .
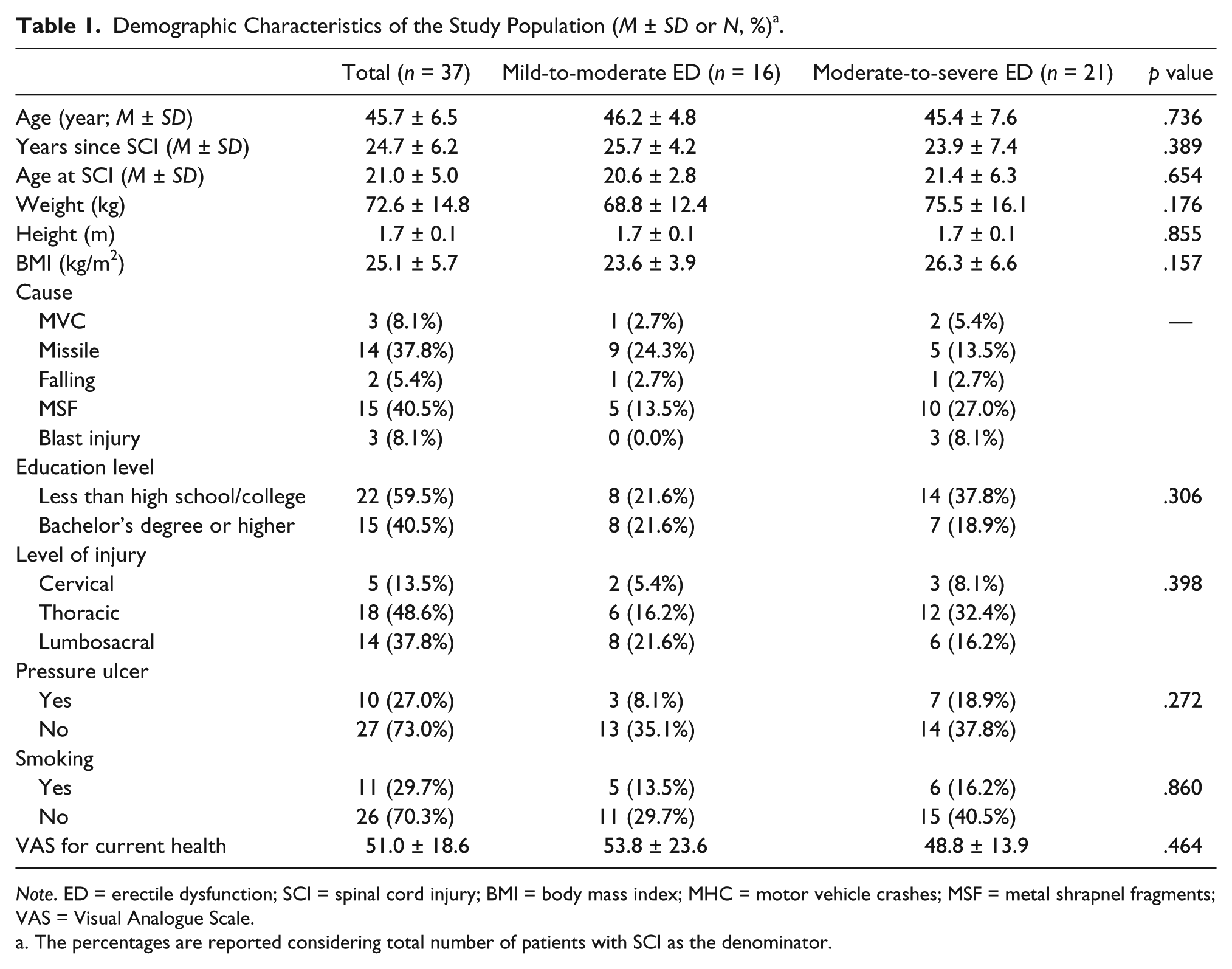
Note. ED = erectile dysfunction; SCI = spinal cord injury; BMI = body mass index; MHC = motor vehicle crashes; MSF = metal shrapnel fragments; VAS = Visual Analogue Scale.
The percentages are reported considering total number of patients with SCI as the denominator.
The records for EuroQoL 5-Dimensions 3-Levels questionnaire are reported in Figure 1. Using conventional scoring of GHQ-12, a mean score of 3.65 ± 3.38 was measured. As recommended by Goldberg et al. (1998), the mean GHQ score for the whole population of respondents provides a rough guide to the best cutoff threshold; hence, 17 patients (45.9%) had an indication of mental health problems. The mean visual analogue scale self-score for current health status was 51.0 ± 18.6 (minimum = 20 and maximum = 100).
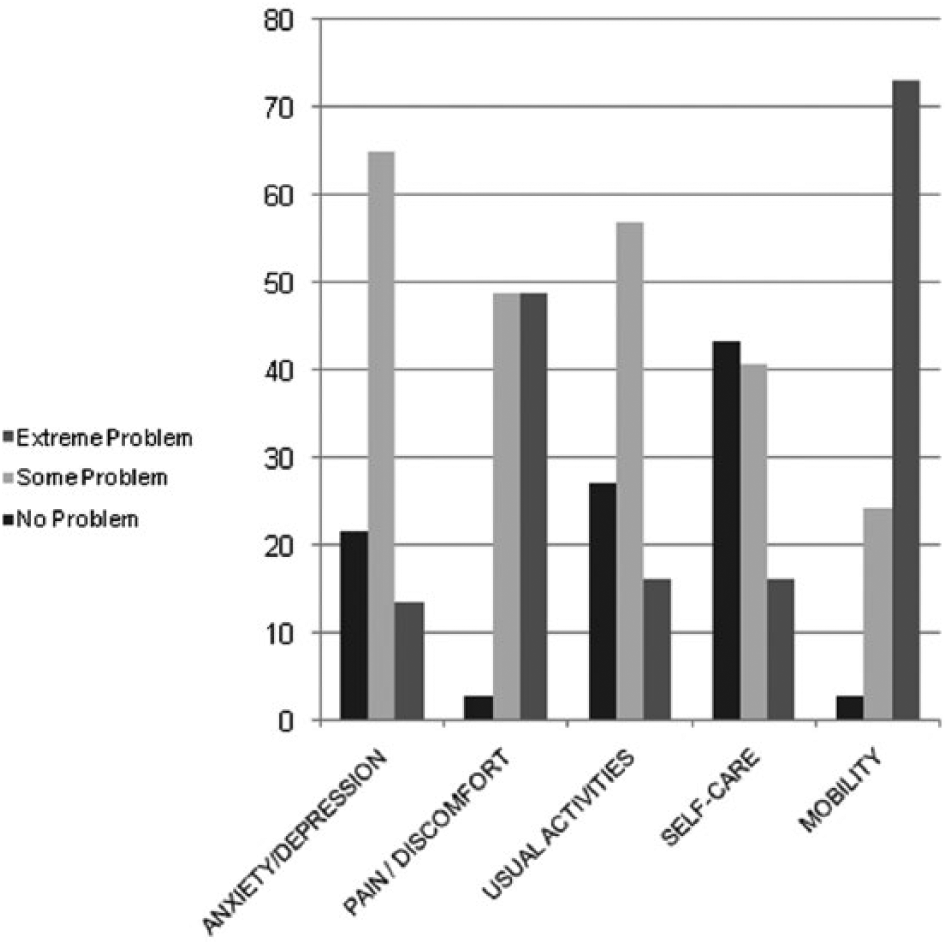
Proportion of reported problems by EuroQoL dimensions in male veterans with traumatic spinal cord injury.
The distribution according to the severity of erectile dysfunction as defined by the classification of Rosen et al. (1999) is reported in Table 2. As there was a group with 0 patients and other groups included a small number of patients, to improve the accuracy of the statistical analysis, we categorized the patients into two groups of mild-to-moderate ED including 16 patients (43.24%) and moderate-to-severe ED including 21 patients (56.76%).
Severity of Erectile Dysfunction According to Rosen’s Classification in 37 Male Veterans With Traumatic Spinal Cord Injury.

The mean SHIM score was 11.57 ± 5.28 and there was no veteran without ED. Table 3 reports the results for each question of the SHIM. The difference between the two groups was significant in all domains (p < .001).
The Mean Score for Each Question of SHIMa in 37 Male Veterans With Traumatic Spinal Cord Injury (M ± SD).

Note. SHIM = sexual health inventory for men; ED = erectile dysfunction. p value < .001 for the difference between two groups regarding the mean score in all five questions and the total score.
The association between education, sleep, and recovery difficulties, GHQ, physical activity, smoking, and comorbidities with different domains of the SHIM is presented in Table 4.
Association Between Education, Sleep and Recovery Difficulties, GHQ, Physical Activity, Smoking, and Comorbidities With Erectile Function Assessed by SHIM in 37 Men With Traumatic Spinal Cord Injury a .

Note. GHQ = General Health Questionnaire; SHIM = Sexual Health Inventory for Men; EuroQoL = Euro Quality of Life; HTN = hypertension; DM = diabetes mellitus; CAD = coronary artery disease.
Only data for significant differences are shown—p value < .05.
Discussion
The SHIM questionnaire was used to assess sexual dysfunction in a population of spinal cord–injured male veterans in Iran. In our study population, the prevalence of ED according to Rosen’s classification was 100%; however, severe ED was present in 27%. A previous study has reported ED in 86% of patients with SCI (Cobo-Cuenca et al., 2012). The high rate of ED in our population may be attributed to the method of sampling. Several studies have reported that SHIM is a suitable instrument to be used in men with disabilities (Cappelleri & Rosen, 2005; Nikoobakht et al., 2012). After categorizing the patients into two groups with mild-to-moderate ED and with moderate-to-severe ED, the first group recorded a significantly higher score in all five dimensions. However, Game et al. (2006) identified “difficulty in maintaining an erection” as the principal origin of erectile dysfunction in young men with SCI and suggested treatment with five phosphodiesterase inhibitors to improve the situation. A case–control study identified patients with SCI had a higher frequency of ejaculatory disorders. Besides, decreased sexual disorder, ED, and premature ejaculation were more responsible for sexual dysfunction in patients without SCI (Virseda-Chamorro, Salinas-Casado, Lopez-Garcia-Moreno, Cobo-Cuenca, & Esteban-Fuertes, 2013). However, regardless of the origin, several studies have agreed on the role of medical and surgical management in improvement of ED (Belkoff et al., 2013; Lombardi, Nelli, Celso, Mencarini, & Del Popolo, 2012; Maheronnaghsh, Yousefian, & Rahimi-Movaghar, 2012).
Although it is suggested that erectile dysfunction is more likely if the sacral reflexes are impaired (Game et al., 2006), the level of injury did not identify any significant association with developing ED in our study. A previous study has reported that psychological distress is more likely in men with cervical lesions than in men with thoracolumbar lesions, and it is inversely correlated with SHIM score (Barbonetti, Cavallo, Felzani, Francavilla, & Francavilla, 2012). Also, another study suggested that sexual function in patients with SCI mainly depends on the completeness of injury and the level of neurological damage (Dimitriadis et al., 2010). Though studies with larger sample size may contribute in better understanding. A previous study reported that patients with younger age at injury had better sexual adjustments after injury (Siosteen, Lundqvist, Blomstrand, Sullivan, & Sullivan, 1990). Anderson et al. (2007a) suggested involvement in sexual relationships is greater in patients with more years after injury and these patients are more willing to address their sexual function. It is also reported that most men resume their sexual activity within 1 year of injury (Alexander, Sipski, & Findley, 1993). However, factors such as age, duration of disability and age at the time of injury were neither significant factors affecting sexual function.
Among the comorbidities of diabetes, hypertension, and coronary artery disease, which are the known risk factors of ED, only the patients suffering from hypertension recorded a significantly lower SHIM score. The small sample size and the sedentary life style of the SCI patients that increases the rate of cardiovascular risk factors in the patients may justify this lack of difference.
Sleep deprivation is suggested to inhibit nocturnal erections (Montorsi & Oettel, 2005). Previous studies have also reported direct association between sleep disturbances with ED (Andersen, Santos-Silva, Bittencourt, & Tufik, 2010). It is identified that sleep loss reduces testosterone levels in males, which is associated with sexual dysfunction (Andersen, Alvarenga, Mazaro-Costa, Hachul, & Tufik, 2011). Smoking and obesity are also frequently reported to be associated with ED in the general population (Akkus et al., 2002; Kratzik, Schatzl, Lunglmayr, Rucklinger, & Huber, 2005; Lucca, Paduch, Pralong, & Vaucher, 2012); an increase in body mass index by 1 kg/m2 is reported to reduce the SHIM score by 0.141, independent of age (Kratzik et al., 2005). We evaluated the possible association between the above factors and ED; however, in our study there was no significant difference observed between the two groups of ED regarding smoking, body mass index, and having difficulties going to sleep. Nevertheless, the patients reporting night sleep as never refreshing had a significantly lower sexual function score; this was also prominent in the domains of confidence to keep an erection and the ability to maintain an erection. Insomnia in general practice is related to anxiety and depression, which are known risk factors for ED (Shapiro & Dement, 1993). As a result, it can be suggested that nonrefreshing night sleep can affect ED indirectly, through its effect on patients’ mental well-being.
A previous study has reported that sexual satisfaction is an important aspect of life in patients with SCI and considering different methods for management of sexual dysfunction will result in higher quality of life in these patients (Maheronnaghsh et al., 2012). Also, another study reported that, in patients with SCI, ED would result in lower quality of life, independent of etiology, degree, and the time of the evolution of the SCI (Cobo-Cuenca et al., 2012). In our study, the GHQ-12 questionnaire analysis adds to the knowledge that the SCI patients with better GHQ scores than the mean of whole study population are at lower risk of experiencing severe ED; this was significantly observed in four domains of SHIM and the total SHIM score and was marginally meaningful for having satisfactory intercourse. Although medical management of ED is desirable in SCI patients, improving their confidence may also improve their sexual function.
Although the investigation was restricted to men to obtain a homogeneous sample, our study identified that a survey of sexual dysfunction using a self-administered questionnaire is feasible. The study sample was small and the response rate was quite low, and there were limitations in gathering complete data in some fields such as completeness of injury. Also, patients’ answers were not validated with medical records, as the information was not available for all patients. These factors may impose limits to our results. Appropriate information about current and past drug history of the patients was not gathered; however, a long list of medications and recreational drugs that are commonly associated with ED are described, which makes such analysis difficult. Anderson et al. (2007b) made such analysis using number of medication types a patient was taking at the time of study. Further studies with larger sample size may provide the literature with such information.
The results of our study identify that ED is a common problem in veterans with SCI and this is associated with lower rate of self-reported general health status. More severe ED is accompanied by more difficulties in confidence to keep an erection, keeping a penetrative erection, maintaining an erection, and completion of intercourse. Sleep deprivation and hypertension are also contributors of ED in SCI patients.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
