Abstract
Physical activity during growth increases bone mass and strength; however, it remains unclear whether these benefits persist. The purpose of this study was to determine: (a) if bone loading during adolescence (13-18 years) or young adulthood (19-29 years) in men is associated with greater bone mineral density (BMD) in adulthood; (b) if current participation in high-impact activity (ground reaction force > 4 × body weight) and/or resistance training is associated with greater BMD; and, (c) if continuous participation in a high-impact activity from adolescence to adulthood is associated with greater BMD. Apparently healthy, physically active men aged 30 to 65 years (n = 203) participated in this cross-sectional study. Exercise-associated bone loading was estimated based on ground reaction forces of historical physical activity. Current BMD was measured using dual-energy X-ray absorptiometry. Participants were grouped based on current participation in a high-impact activity (n = 18), resistance training (n = 57), both (n = 14), or neither (n = 114); groups were compared by two-way analysis of covariance. Bone loading during adolescence and young adulthood were significant, positive predictors of BMD of the whole body, total hip, and lumbar spine, adjusting for lean body mass and/or age in the regression models. Individuals who currently participate in a high-impact activity had greater lumbar spine BMD than nonparticipants. Men who continuously participated in a high-impact activity had greater hip and lumbar spine BMD than those who did not. In conclusion, physical activity–associated bone loading both during and after skeletal growth is positively associated with adult bone mass.
Introduction
Osteoporosis, a condition characterized by low bone mass and increased fracture risk, affects approximately 52 million Americans. Although commonly believed to only affect postmenopausal women, approximately 2 million men in the United States have osteoporosis (National Osteoporosis Foundation, n.d.). Osteoporotic fractures occur in 25% of men older than 50, and the mortality rate for older men after a fall is ~40% higher than women (Centers for Disease Control and Prevention, 2013).
Because bone mass declines with age, maximization of peak bone mass is recommended as the most effective way to prevent osteoporosis (Heaney et al., 2000). Acquisition of at least 90% of peak bone mass occurs by the age of 18 years, with additional gains of 5% to 10% during young adulthood (Bachrach, 2001); therefore, these times of skeletal growth constitute a critical period during which time insults, such as nutrient or hormonal deficiencies, have lasting deleterious effects on skeletal health (Heaney et al., 2000). Conversely, because mechanical loading induces a greater adaptive response in young, compared with old, bone, adolescence and young adulthood constitute a unique window of opportunity to increase bone mass via physical activity (Bailey, Faulkner, & McKay, 1996). Although physical activity during adolescence and young adulthood is a key determinant of peak bone mass and, therefore, of future bone health, exercise after skeletal maturation can also reduce the risk of osteoporosis and related fractures (Daly & Bass, 2006; Michaelsson et al., 2007).
During physical activity, bone is subjected to mechanical forces exerted by muscle contraction and gravitational loading (e.g., impact). At the cellular level, bone cells (osteocytes) perceive these mechanical forces as cell deformation, changes in extracellular fluid shear stress, pressure gradients, and electric fields (Robling, Castillo, & Turner, 2006). The osteocytes communicate with osteoblasts and osteoclasts to modulate bone formation and resorption, thereby changing bone geometry and material properties (Turner & Robling, 2005). Physical activity recommendations for bone health consider the mechanical loading characteristics that have the greatest osteogenic effect and thus include activities that result in either high-impact (e.g., jumping) or high-muscle-contraction forces (e.g., resistance training).
The American College of Sports Medicine recommends weight-bearing endurance activities, including those that involve jumping (such as tennis) and jogging, three to five times per week and resistance exercise two to three times per week to preserve bone health during adulthood (Kohrt et al., 2004). Resistance training is recommended by the National Strength and Conditioning Association to increase bone mineral density (BMD) or to prevent age-associated reductions in BMD (National Strength and Conditioning Association, 2004). The Surgeon General’s Report on Bone Health also recommends progressive resistance training, as well as daily jump-training and participation in weight-bearing recreational activities, for individuals who can tolerate high-impact activity (U.S. Department of Health and Human Services, 2004).
The objective of the present study was threefold: (a) to examine the relationships between current BMD of the whole body, hip, and lumbar spine and physical activity–associated bone loading during adolescence (13-18 years), young adulthood (19-29 years), and current physical activity–associated bone loading; (b) to investigate the effects of current participation in a high-impact physical activity and/or resistance training on BMD of the whole body, total hip, and lumbar spine in apparently healthy, physically active men; and, (c) to evaluate the effects of continuous participation in high-impact activity throughout the life span on BMD of the whole body, total hip, and lumbar spine.
It was hypothesized that physical activity–associated bone loading during adolescence, young adulthood, and current bone loading would be positively associated with BMD of the whole body, hip, and lumbar spine in apparently healthy, physically active men. It was also postulated that men whose current physical activity includes a high-impact activity and/or resistance training would have greater BMD than men who do not participate in high-impact exercise or resistance training, and that men who participate in both high-impact exercise and resistance training would have the highest BMD. Finally, it was expected that men who continuously participated in a high-impact activity throughout skeletal growth (i.e., adolescence and young adulthood) or those who participated in a high-impact activity from adolescence to adulthood (i.e., time of study participation) would have greater BMD than those who did not.
Subjects and Method
Experimental Design
A cross-sectional study design was used to examine relationships between bone loading during adolescence, young adulthood, and current activity-associated bone loading and BMD of the whole body, total hip, and lumbar spine in physically active, apparently healthy middle-aged men.
Subjects
Physically active males (n = 203) aged 30 to 65 years were recruited from the University of Missouri and Columbia community via flyers posted on campus, at local sporting goods stores and fitness centers, and on websites of local cycling and running clubs for participation in an exercise intervention study of men with low bone mass for age. The participants in the present study include all men who were screened for eligibility in the intervention study. Thus, the sample size for the present study was determined by the number of participants screened to meet the enrollment target for the intervention study. Inclusion criteria were as follows: male, 30 to 65 years of age, and at least 4 hours of purposeful physical activity per week for the past 2 years. Exclusion criteria included current or previous medical condition or use of medication affecting bone health, implanted metal that would interfere with determination of BMD, cigarette smoking, and excessive alcohol consumption (more than three drinks per day on average). Prior to initial screening, all participants were informed of any risks associated with this study (e.g., radiation associated with the dual-energy X-ray absorptiometry [DXA] scans), they read a consent form, and they gave written consent. This study was approved by the University of Missouri Health Sciences Institutional Review Board.
Procedures
Anthropometric Data
Participant weight was determined to the nearest 0.05 kg, height was determined to the nearest 0.5 cm, and the results were used to calculate body mass index (kg/m2).
Bone Mineral Content and Density
Dual-energy X-ray absorptiometry (Hologic QDR 4500, Waltham, MA) was used to measure bone mineral content (BMC) and areal BMD of the whole body, lumbar spine, total hip, and femoral neck. Areal BMD (g/cm2) was calculated from bone area (cm2) and BMC (g). Each participant underwent a whole body, total hip, and lumbar spine (L1-L4) DXA scan. CVs for BMC and BMD were <1%. The International Society of Clinical Densitometry’s guidelines were used to categorize participants as having normal BMD (Z score > −2.0 SD) or low bone density for age (z score ≤ −2.0 SD) based on z scores of the spine and hip (Lewiecki et al., 2008).
Questionnaires
Subjects completed a medical history questionnaire and the Historical Leisure Activity Questionnaire (HLAQ; Kriska et al., 1988). The HLAQ was developed to measure historical leisure time physical activity across the life span and to relate prior activity to bone density in postmenopausal women. The original interviewer-administrated version of the HLAQ has been modified for self-administration with good reliability, that is, intraclass correlation coefficients of ~0.86 for lifetime vigorous-intensity activities (Chasan-Taber et al., 2002). The HLAQ has been used to examine the relationship between lifetime weight-bearing activity and current bone density in adult men (Daly & Bass, 2006; Hinton & Eaton, 2013; Rogers & Hinton, 2010). In the present study, the HLAQ was used to assess participation in physical activity during adolescence (13-18 years) and young adulthood (19-29 years), as well as current physical activity. To enhance recall of past physical activity, participants were provided standardized verbal prompting by study personnel. Study personnel reviewed responses on the medical history and HLAQ with each participant to verify completeness of the written history. The Compendium of Physical Activities was used to estimate daily energy expended during purposeful exercise for current physical activity (Ainsworth et al., 2000).
Physical Activity–Associated Bone Loading
Bone loading scores were calculated for adolescence, young adulthood, and current physical activity using the responses provided in the HLAQ and the biomechanical ground-reaction force (GRF) for each activity (Groothausen, Siemer, Kemper, Twisk, & Welten, 1997). In brief, each reported physical activity was classified into one of four categories (0-3) based on the GRF it induces: 0 (GRF < 1 × body weight; e.g., cycling, swimming), 1 (GRF between 1 and 2 × body weight; e.g., rowing, weight-lifting), 2 (GRF between 2 and 4 × body weight; e.g., jogging), and 3 (GRF > 4 × body weight; e.g., basketball, volleyball).
For each developmental period, a loading score was calculated as the sum of the classification scores listed for each activity (GRF SCORE), which is analogous to exercise intensity. The GRF SCORE was, therefore, an indicator of exercise-induced bone-loading intensity. Studies in experimental animals that used extrinsic bone loading have reported that bone becomes refractory to mechanical loading after as few as 40 loading cycles and requires a “rest” period of ~8 hours to gain responsiveness (Robling et al., 2006). Therefore, it is possible that physical activity intensity, that is, its ground reaction force, is more important than the frequency and duration of participation, as strain magnitude must exceed a threshold (i.e., 1,500 microstrains) to induce adaptive modeling/remodeling (Robling et al., 2006).
Statistical Analyses
Data were examined for normality of distribution. Outcome variables, that is, whole body, hip, and lumbar spine BMD, were normally distributed.
The effects of bone loading during adolescence and young adulthood and current physical activity on current BMD were examined using multiple linear regression. Lean body mass was significantly correlated with BMD at all sites (r values ranged from .4 to .5, p < .001), while age was significantly correlated with hip BMD (r = −0.15, p <.05). Thus, lean body mass was included as a covariate in all models, while age was also included as a covariate in models for which hip BMD was the dependent variable. Because body weight and lean body mass were highly correlated in our study sample (r = .88, p < .001), inclusion of body weight or lean body mass as a covariate in the regression models gave similar results. Therefore, for clarity and brevity, only the models that included lean body mass and age as covariates are reported. The assumptions of regression, that is, linear relationship between dependent and independent variables and constant error, were verified by plots of residuals versus predicted values.
The second aim of the study was to examine the effects of current participation in a high-impact physical activity and/or resistance training on whole body, hip, and lumbar spine BMD. Thus, based on the GRF categories of the activities listed in the HLAQ, subjects were categorized as currently participating in a high-impact activity if they had at least one activity with a GRF category score of 3 (i.e., greater than four times body weight, such as basketball, volleyball, or jumping events in track and field). Current resistance training was defined as participation in any activity facilitating a resistance that stimulated the contraction of muscles (i.e., calisthenics, weights, stability balls, etc.; Czaprowski et al., 2014; Galvao et al., 2006). The numbers of participants in the resulting four categories were as follows: not currently participating in a high-impact activity or resistance training (n = 114), current participation in a high-impact physical activity (n = 18), current participation in resistance training (n = 57), and current participation in both a high-impact activity and resistance training (n = 14). Two-way analysis of covariance was used to test for significant main and interaction effects of high-impact activity and resistance training, including lean body mass and/or age as covariates in the generalized linear model. Lean body mass and age were included in the models as covariates because they were significantly correlated with the outcome variables, as mentioned above. In the case of a significant main or interaction effect, post hoc LSD pairwise comparisons were performed.
The third aim of the study was to determine the effects of continuous participation in a high-impact activity throughout the life span (i.e., during adolescence, young adulthood, and currently) on adult BMD. Using the method described above to classify activities as high impact or non–high impact, subjects were categorized into four groups based on their history of participation in high-impact activity: high impact throughout the life span (i.e., adolescence, young adulthood, and currently, n = 17); high impact only throughout skeletal growth (i.e., adolescence and young adulthood, n = 43); high impact only during one phase of skeletal growth (i.e., adolescence or young adulthood, n = 50); and no high-impact activity (n = 93). One-way analysis of covariance was used to test for significant effects of group, including lean body mass as a covariate in the generalized linear model. In the case of a significant group effect, post hoc LSD pairwise comparisons were performed to determine which groups differed from each other.
All statistical analyses were performed using SPSS (Version 11). Descriptive data are means or least-square means ± standard error of the mean. P < .05 was considered statistically significant.
Results
The anthropometric, physical activity, and bone density characteristics of the men (mean age = 45.2 ± 0.6 years) who participated in the study are reported in Table 1. Regarding BMD, although the mean Z scores for the total hip and lumbar spine BMD indicated average bone density for age, there were individuals whose total hip or lumbar spine BMD was considerably more than or less than the age-adjusted mean (hip Z scores = −2.30 to 2.60; lumbar spine Z scores = −3.30 to 3.90). Of the 203 participants, 13 (6.4%) were classified as having low bone density for age of the hip or lumbar spine.
Subject Characteristics.

Note. BMI = body mass index; GRF = ground reaction force; PA = physical activity. Data presented as mean ± standard error of the mean (n = 203).
Physical activity–associated bone loading during adolescence was a positive predictor of current BMD of the whole body, total hip, and lumbar spine (Table 2, Adolescence Model 1) and remained a significant positive predictor of total hip and lumbar spine BMD after adjusting for covariates (Table 2, Adolescence Model 2). Bone loading during young adulthood was also a significant positive predictor of BMD at all measured sites (Table 2, Young Adulthood Model 1) and remained significant for total hip and lumbar spine after adjusting for covariates (Table 2, Young Adulthood Model 2). Current bone loading was a positive predictor of total hip BMD only after adjusting for lean body mass and age (Table 2, Current Activity Model 2). Current bone loading also was a significant positive predictor of lumbar spine BMD and remained significant after adjusting for lean body mass (Table 2, Current Activity Models 1 and 2).
Areal Bone Density and Life-Span Period.

Note. BMD = bone mineral density; GRF = ground reaction force (sum of the GRF classifications for all activities); LBM = lean body mass; LS = lumbar spine; WB = whole body. Standardized regression coefficients (β) and p values for independent variables (n = 203). Results significant for the whole body, hip, and lumbar spine if p ≤ .05 (ANOVA).
The effects of current participation in a high-impact activity and/or resistance training on whole body, total hip, and lumbar spine BMD were examined (Figure 1). For lumbar spine BMD, there was a statistically significant main effect for participation in a high-impact activity. Men who currently participate in a high-impact physical activity had significantly greater age– and lean body mass–adjusted BMD (1.134 ± 0.024 g/cm2) than those who do not (1.053 ± 0.011 g/cm2). There were no statistically significant main or interactive effects for whole body or total hip BMD, although men who currently participate in resistance training tended to have greater lean body mass–adjusted whole body BMD than men who do not currently resistance train (1.232 ± 0.015 g/cm2 vs. 1.196 ± 0.012 g/cm2, main effect p value = .06).

Mean ± standard error of the mean of whole body, hip, and lumbar spine BMD for subjects currently participating in high-impact activities (GRF > 4 × body weight) and resistance training (n = 14), high-impact activities only (n = 18), resistance training only (n = 57), or neither type of exercise (n = 114).
The effects of continuous participation in a high-impact activity from adolescence through adulthood on BMD of the whole body, total hip, and lumbar spine was evaluated. Of the 110 men who participated in high-impact activity during adolescence, 43 (39%) also participated in a high-impact activity during young adulthood, and an additional 17 (15%) continued to participate in a high-impact activity until the time of the present study. Men who continuously participated in a high-impact activity during skeletal growth (i.e., adolescence and young adulthood) or who participated continuously from adolescence until the time of the study had greater BMD of the total hip and lumbar spine than men who did not (Figure 2).
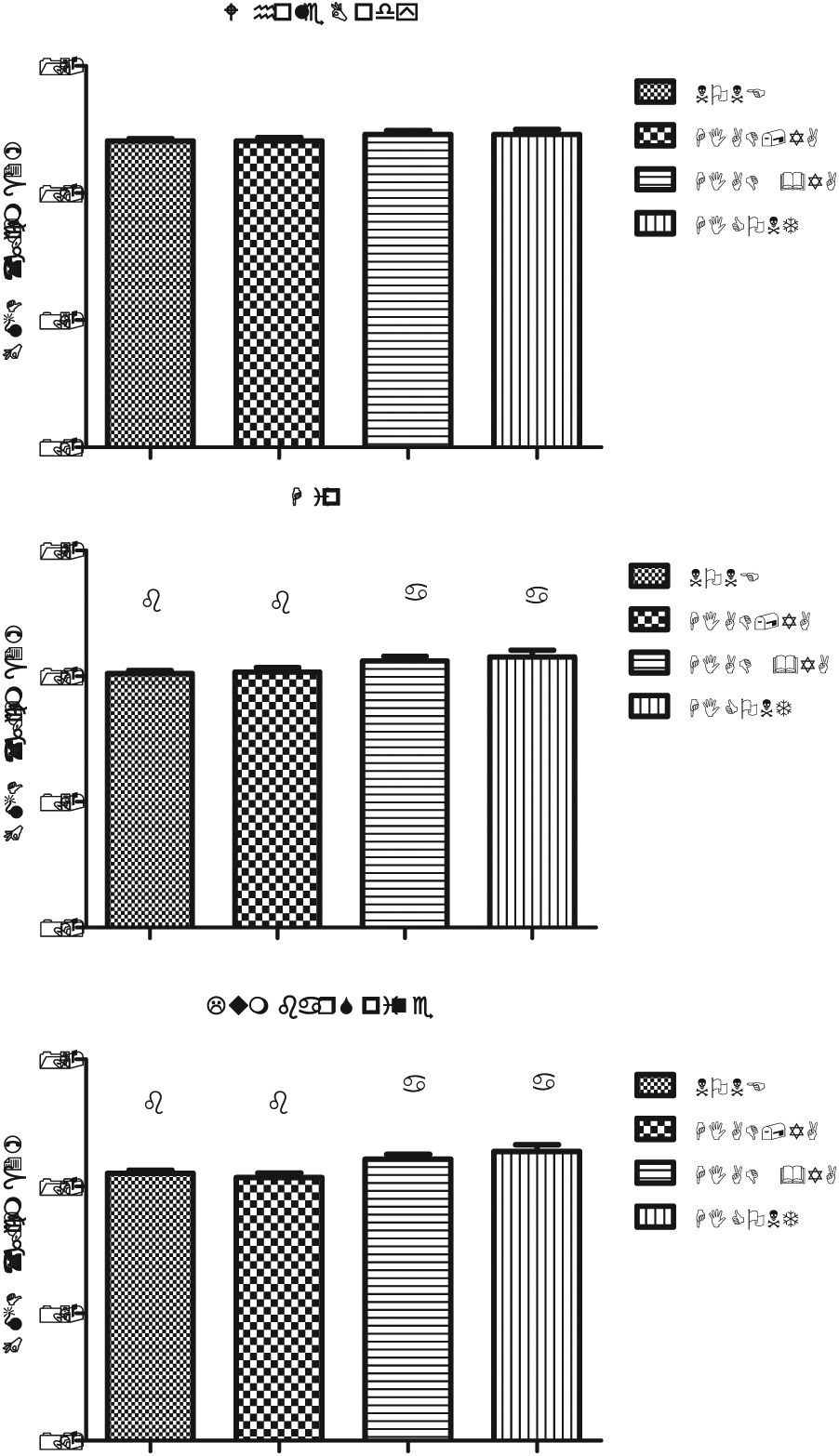
Mean ± standard error of the mean of whole body, hip, and lumbar spine BMD for subjects participating in high-impact activities (GRF > 4 × body weight) throughout the life span (CONT; n = 17), adolescence and young adulthood only (HI AD & YA; n = 43), adolescence or young adulthood (HI AD, YA; n = 50), or neither (NONE; n = 93).
Discussion
The results of our study suggest that physical activity–associated bone loading during adolescence and young adulthood is positively associated with BMD of the whole body, hip, and lumbar spine during adulthood. Our results also indicate that current physical activity–associated bone loading is a positive predictor of hip and lumbar spine BMD, and participation in a high-impact (i.e., GRF > 4 times body weight) physical activity is associated with greater BMD of the lumbar spine. Our results are consistent with previous studies, which suggest that increasing physical activity at any point throughout the life span positively affects bone health (Allison, Folland, Rennie, Summers, & Brooke-Wavell, 2013; Baxter-Jones, Kontulainen, Faulkner, & Bailey, 2008; Michaelsson et al., 2007; Nilsson, Ohlsson, Mellstrom, & Lorentzon, 2009; Rogers & Hinton, 2010; Van Langendonck et al., 2003). A unique finding of the present study is that high-impact activity during adulthood was associated with greater hip and spine BMD, while resistance training was not. Moreover, this study adds to the existing literature with the observation that continuous participation in high-impact activity throughout skeletal growth was associated with greater BMD of the hip and lumbar spine than noncontinuous participation (Baxter-Jones et al., 2008; Neville et al., 2002; Nichols, Palmer, & Levy, 2003; Nilsson et al., 2008; Rogers & Hinton, 2010; Tervo, Nordstrom, Neovius, & Nordstrom, 2008). From a practical perspective, our results suggest that the physical activity “prescription” for bone health should be continuous high-impact activity throughout the life span during both skeletal growth and adulthood.
Exercise during skeletal growth increases bone mass and strength (Bradney et al., 1998; Duckham et al., 2014; Neville et al., 2002; Van Langendonck et al., 2003). In particular, high-impact physical activity during growth is associated with greater BMD, as well as favorable changes in bone geometry and structure (Callreus, McGuigan, Ringsberg, & Akesson, 2012; Deere, Sayers, Rittweger, & Tobias, 2012; Nilsson, Ohlsson, Mellstrom, & Lorentzon, 2013). In the present study, physical activity–associated bone loading during adolescence and young adulthood was positively associated with age– and lean body mass–adjusted BMD of the hip and lumbar spine in adulthood. This result is consistent with previous reports that the favorable skeletal effects of exercise during growth persist into adulthood (Nilsson et al., 2008; Nilsson et al., 2009). A recent study (Nilsson et al., 2014) suggests that the enduring benefits of high levels of exercise during growth on bone strength may be because of changes in bone geometry and structure. In older men (mean age 80 years), high levels of exercise during skeletal growth (ages 10-30 years) were associated with differences in bone geometry and structure that favorably affected estimates of bone strength at age 80 years. Specifically, older men who were competitive athletes during adolescence/young adulthood had greater cross-sectional area, cortical thickness, periosteal circumference at the tibial diaphysis, and greater estimated failure load, stiffness, trabecular thickness, and trabecular bone volume fraction of the tibial metaphysis than 80-year-old men with the lowest level of activity. Thus, exercise at a young age may have both short- and long-term positive implications.
Although physical activity during growth appears to have beneficial effects on bone that persist into adulthood, activity-associated bone loading after skeletal growth is complete is also important for bone health during middle-age and older adulthood (Bakker, Twisk, Van Mechelen, Roos, & Kemper, 2003). In the present study, current physical activity–associated bone loading was positively associated with BMD of the hip and lumbar spine. In addition to increasing BMD, bone loading during adulthood increases bone size, cortical area, and strength (Daly & Bass, 2006) and reduces fracture risk (Michaelsson et al., 2007; Qu et al., 2014). Even in much older men (~80 years) current physical activity positively affects bone, in part by reducing endosteal expansion, that is, bone loss (Nilsson et al., 2014).
In the present study, men who currently participate in a high-impact physical activity had greater BMD of the lumbar spine than men who do not participate in a high-impact activity. In addition, men who continuously participated in a high-impact activity during skeletal growth or from adolescence until adulthood had greater hip and lumbar spine BMD than those who did not. Other studies suggest that regular participation in high-impact activity is associated with greater bone mass, while low-impact activity is not. For example, individuals who participate in sports/activities that result in gravitational loading have greater BMD than those who participate in a weight-supported or low-impact activity (Deere et al., 2012; Nilsson et al., 2013; Rector, Rogers, Ruebel, Widzer, & Hinton, 2009). Most human data that compare activities that differ in impact magnitude are cross-sectional studies of participants in various sports or leisure time activities. Randomized longitudinal studies that evaluate the effects of exercise or compare the effect of different types of exercise on bone mass in men are limited. In a randomized high-impact, unilateral exercise intervention, high-impact exercise (jumping) increased femoral neck BMD in 70-year-old men (Allison et al., 2013). Similarly, 18 months of resistance training combined with jumping exercises led to significantly improved femoral neck BMD and lumbar spine trabecular BMD in men aged 50 to 79 years (Kukuljan et al., 2011). Therefore, high-impact activity is an important determinant for bone health during growth and adulthood.
A strength of the present study is that it included participants with varied sports participation histories, including variations in both sport and level of competition, which increases the generalizability of the results. The relatively large sample size is another strength of the present study. However, because the participants in this study were physically active and apparently healthy, the results cannot be generalized to men who are diseased or inactive. There are other limitations to this study, several of which are common to all cross-sectional studies that rely on retrospective measures of physical activity. Although a previously validated questionnaire was used to assess physical activity history, any retrospective measure will have greater error than prospective measures or direct observation. Regarding the measured outcome variables, DXA permits only measurement of areal BMD and cannot be used to assess activity-associated changes in bone geometry and structure that affect bone strength and fracture risk independent of BMD. Finally, other factors that might have affected the ability of bone to adapt to activity-associated loading, for example, dietary intake, hormonal status, and use of medications, during adolescence and young adulthood was not assessed.
In conclusion, the results of the present study suggest that the benefits of physical activity–associated bone loading during adolescence and young adulthood persist into adulthood. In addition, bone loading during adulthood also has skeletal benefits; in particular, high-impact physical activity during adulthood was associated with greater BMD of the hip and lumbar spine. Therefore, health professionals should recommend participation in high-impact activity beginning during skeletal growth and continuing through adulthood. In addition, health professionals should clearly communicate that it is never too late to exercise for bone health and that even middle-aged adults who were inactive as teenagers or young adults might benefit from beginning a bone-strengthening exercise program.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: Department of Nutrition and Exercise Physiology Summer Research Internship (MS).
