Abstract
The construction of Caribbean male identities based on ideas of masculinity has raised widespread concerns across the island states, and in a region with such high rates of teenage pregnancy (18%), stigmatizing safe sex, contraception, and HIV/AIDS prevalence can only exacerbate the problem. The purpose of this study was to examine the extent to which males use condoms and to explore the association of condom use with their concern with acquiring and transmission of sexually transmitted infections.
Keywords
Introduction
A Caribbean male is often characterized as “powerful, exceedingly promiscuous, derelict in his parental duties, often absent from the household, and, if present, unwilling to undertake his share of domestic responsibilities” (Lewis, 2003, p. 107). Multiple partnering and informal polygamy are often used as ways for males to exert their masculinity in the region (Kempadoo, 2009). In this way, fertility and masculinity are inextricably intertwined. Young men are celebrated for their virility and taught to take risks, whereas young girls are taught complacency and are educated about sex and sexuality only in religious and moral terms of disapproval (Kempadoo, 1999). This male desire to express masculine attributes has been linked to decreased condom use during sexual intercourse (Chevannes, 2001). However, the notion that masculinity is contingent on risky behavior patterns perpetuates the sexual health risks to the Caribbean youth.
According to the United Nations Population Fund (United Nations Family Planning Authority, 2011), the Caribbean is second only to sub-Saharan Africa as the region most affected by the HIV/AIDS epidemic. Considering the high rates of early sexual initiation and teen pregnancy recorded, (United Nations Office on Drugs and Crime, 2005), the sexual health of the region is vulnerable. When considering the dangers involved with initiating sexual activity, the International Council of AIDS Service Organizations (2009) recommends sex education and condom use promotion as part of a comprehensive solution to the problem. However, cultural, economic, political, and structural barriers can restrict accessibility to condoms (International Council of AIDS Service Organizations, 2009).
In an effort to evaluate Grenada Planned Parenthood Association (GPPA), this study examined male perspectives of condom use in Grenada. Specifically, the purpose of this article was to examine the extent to which males use condoms and explore the association of condom use with their concern with acquiring and transmitting of sexually transmitted infections (STIs).
Method
To examine condom usage, a sample of men aged 18 to 27 years was recruited to participate in a self-administered, anonymous survey regarding condom accessibility and use and STIs. The survey was constructed as part of a larger evaluation of GPPA. Using GPPA staff, an anthropologist, a sociologist, and a statistician, the survey consisting of 15 items was developed, asking participants about their current condom usage, perceptions of STI transmission risk, reasons why or why they do not use a condom, and where they learned about condom usage. For the purpose of this article, the questions regarding condom usage and concerns of contracting a STI were used. The study obtained institutional review board approval on October 21, 2011.
A convenience sample of 98 males representing the parishes of St. George’s, St. Andrew’s, and St. Patrick’s, Grenada, completed the survey. These locations represent both the rural and urban parishes of Grenada. Six surveys were discarded because they were out of the age range. Another 11 surveys were not used in the analysis because the participants reported that they were not sexually active. The survey questions were orally administered and completed by administrators of the survey when persons were uncomfortable with reading or unable to read but wanted to participate in the study. Approximately 26.5% of the participants had the survey read to them. No incentives were given. To ensure cultural sensitivity and appropriateness, all questions were pilot tested on local Grenadian colleagues prior to conducting the survey.
Condom use at last sexual encounter was used for analysis because it is used as an indicator to monitor HIV behavioral interventions and will generally reflect trends in condom use (Allen & Bombereau, 2008). However, we also considered how often participants used condoms to get an idea of consistency and the reasons for behavioral change if the last–sex encounter condom use was inconsistent with typical usage. Participants were grouped as either consistent condom users, if they reported always using a condom and using a condom during their last sexual intercourse, or inconsistent condom users, which included all other participants. A total of 12 of the 13 males were classified as consistent condom users. Associations between consistency of condom usage and individual factors, such as age, education level, reasons for condom compliance or noncompliance, and concern about STIs were examined. The data were analyzed through SPSS Version 19 and qualitatively evaluated for these among the responses.
Results
A total of 81 males 18 years of age and older who are sexually active participated in this study. Table 1 presents the demographic characteristics of the participants. Participants ranged in age from 18 to 27 years, with an average age of 22 years (SD = 2.4). The majority of participants completed secondary school (61.7%), were concerned with contracting a sexually transmitted infection (STI; 59.3%), and were taught to use and used a condom (74.1% and 91.4%, respectively).
Summary of Demographic Characteristics (n = 81).
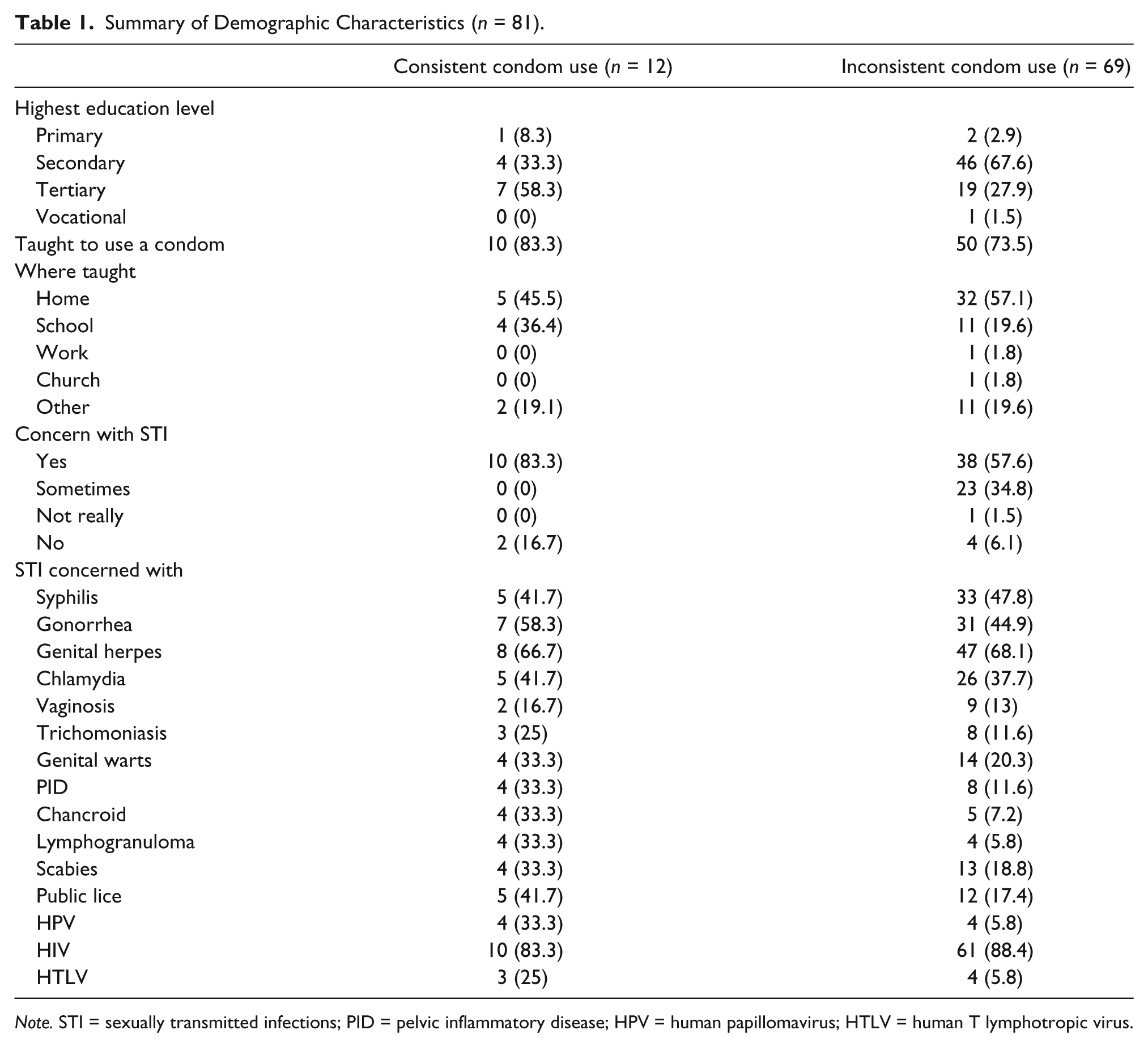
Note. STI = sexually transmitted infections; PID = pelvic inflammatory disease; HPV = human papillomavirus; HTLV = human T lymphotropic virus.
There is certainly a degree of awareness and attempt to use condoms especially among people with higher education as only 9% of the respondents reported never using a condom. Although most participants use condoms at some point, there were no statistically significant differences in the proportion between consistency of condom use and education level (χ2 = 13.322, p = .15), if they were taught to use a condom (χ2 = 2.67, p = .45), or concerned with contracting a STI (χ2 = 9.73, p = .37).
When asked about their concern with contracting an STI, 59% reported they were concerned and 28% indicated that they were concerned sometimes. The distribution of STIs is presented in Table 1. Of the STIs listed, the majority of the participants were concerned with HIV (87.7%). To a lesser extent, participants were concerned with genital herpes (67.9%), syphilis, and gonorrhea (46.9% each). Few (<25%) were concerned with vagniosis, thrichomonasis, genital warts, pelvic inflammatory disease, canchroid, lymphogranouma, scabies, pubic lice, human papillomavirus (HPV), and human T lymphotropic virus. Even though participants were concerned with HIV, 14% of the men expressing concern reported always using a condom.
To further examine the reasons for condom use, participants were asked why they used or did not use a condom during their last sexual intercourse; the results are presented in Tables 2 and 3. Some participants reported that the reason for their consistent use of condoms was protection. Other reasons stated included the lack of trust in their partner. The respondents rarely cited “protecting my partner” (6%), “my partner asked me to” (6%), or respect for my partner (0%) when asked openly why they used a condom. And when asked why they did not use a condom, 15% said that they simply did not want to or that it took away from the pleasure, and 30% were unprepared. The lack of consideration for the females as an equal within the act of sexual intercourse is evident in many of the respondents’ answers. This result may suggest that the social construction of the fertile, dominant male and the complacent female in the Caribbean society can negatively affect the sexual health of the population. Gender inequality and lack of dialogue among partners regarding condom use could lead to higher rates of unprotected sexual intercourse (Sarkar, 2008).
Reasons for Using a Condom by Frequency of Condom Use.

Reasons for Not Using Condom by Frequency of Condom Use.

At the societal level, structural rigidity in the education system and prevailing moral norms in Grenada contribute to a culture of condom noncompliance. With 45.7% of participants learning how to use condoms at home and only 18.5% in schools, there appears to be a discrepancy between what families are willing to teach their children and what the schools in Grenada will provide. Males who were taught to use condoms, regardless of the means by which they were taught, were more likely to have used them during their last sexual encounter. The lack of concern among participants about STI transmission is likely a symptom of a poor sexual education program. Less than 10% of the respondents expressed concern about HPV. HPV is the cause of all cervical cancers, which is the leading cause of death among women in developing countries (World Health Organization, 2007). The high incidence rates of HPV in the Caribbean women correspond to the high rates in men as well (World Health Organization, 2007). The fact that HPV is a concern to only 10% of those surveyed is evidence of a failure in public health education.
Discussion
The males in this study appear to exude a confidence or possible ignorance when it comes to sexual health. This implies that the perceived susceptibility and perceived severity that are essential for health behavioral modification is deficient with regard to condom compliance in Grenada. To address this issue, public health professionals need to raise awareness to susceptibility and severity of STIs and unintended pregnancy and to educate the public about the benefits of consistent, proper condom use.
Even though the participants are aware of HIV/AIDS, the results suggest that men are not optimally using protection to safeguard themselves and their partners from acquiring and transmitting HIV/AIDs. In addition, the other top STIs the men are concerned with indicate that they are not as emphasized as HIV/AIDS in public awareness and social campaigns.
The results of this study suggest that the majority of men continue to engage in high-risk sexual behaviors. Therefore, it was expected that 57.6% of the men who are inconsistent with their condom use report being concerned with STI. However, the concerns of respondents were primarily with HIV/AIDS, gonorrhea, syphilis, gonorrhea, and herpes, all of which have been highly publicized through media campaigns and public health messages worldwide. The range in awareness about STIs suggests that the emphasis of HIV in social awareness campaigns is effective.
Unfortunately, however, there are concerns that fewer than 25% of the men with inconsistent condom use behavior and 40% of the consistent condom users reported being concerned with the other STIs listed, in particular HPV, human T lymphotropic virus, and pelvic inflammatory disease. Furthermore, the remaining STIs with fewer than 25% of the men responding about their concern indicate that males may not be aware that they can contract the infection, since some of the infections are marketed toward women (e.g., HPV).
Limitations
Limitations to the study include bias arising from the nature of the topic and the convenience sampling method. Although the survey was anonymous, respondents may have been more likely to give socially acceptable responses to the questions, especially if the survey was orally administered to them.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by Global Health Collaborating Center, Las Vegas, Nevada, United States.
