Abstract
Aseptic loosening is one of the main causes of failure for both primary and revision total knee arthroplasty (rTKA). Bone loss and bone quality can vary significantly across anatomical regions, potentially challenging long-term fixation. In recent years, zonal fixation in rTKA has become increasingly popular; this approach divides areas of fixation based on anatomy into 3 zones: epiphysis, metaphysis, and diaphysis. This system emphasizes the importance of preoperative planning and encourages surgeons to carefully select the fixation method for each respective zone. To plan proper fixation, adequate imaging is required to document bone defects and areas of sclerosis. While anteroposterior and lateral radiographs remain the gold standard for defect classification, computed tomography imaging has facilitated 3-D defect evaluation and bone density assessment. For many years cemented and hybrid fixation have been the main modes of fixation in rTKA, but recently these modes of fixation have been augmented by the use of uncemented cones and sleeves. Through bone ingrowth this type of fixation provides lasting fixation in the metaphysis and seems to reduce the need for longer stem fixation in the diaphysis. This narrative review provides an overview of advanced imaging techniques, defect grading, and principles of implant fixation using the concept of zonal fixation.
Introduction
As the number of primary total knee arthroplasty (pTKA) procedures increases, the incidence of revision TKA (rTKA) is projected to grow between 78% and 182% from 2014 to 2030. 1 The most common reasons for rTKA include infection, aseptic loosening, periprosthetic fracture, instability, and osteolysis.2,3 Achieving implant fixation is a common challenge in rTKA. 4 Regarding implant longevity, rTKA prostheses fall short of the results reported for pTKA, with implant survival continuously decreasing with each consecutive revision. 5 Aseptic loosening has been reported as one of the leading indications for re-revision. 6
The evaluation and management of tibial and femoral bone loss is one of the most demanding aspects of rTKA. Reasons for bone loss include stress shielding, osteolysis, infection, and implant loosening or removal.7,8
Traditionally, rTKA fixation has focused on epiphyseal anchorage at the joint level as well as diaphyseal anchorage, using uncemented and cemented stems. 9 With every additional revision surgery greater bone loss is encountered, resulting in defects deep in the metaphysis. Such cases require a challenging restoration of the epiphysis, relying on fixation in the metaphysis and diaphysis. 10 In revisions of stemmed components, the cortical bone in the diaphysis is often sclerotic and thinned, and the absence of cancellous and porous bone surface might interfere with durable cement fixation. 11
In recent years, metaphyseal fixation using cones and sleeves has become more advanced and clinically relevant. 9 With greater bone loss occurring in rTKA, proper bone-implant anchorage should be achieved on as much bone surface possible. To date, no standard fixation planning methodology has been established.
Regarding the solid fixation of revision implants, the concept of zonal fixation has been popularized by Morgan-Jones et al. 12 In this method, the 3 anatomical bone zones—epiphysis, metaphysis, and diaphysis—can be used for anchorage and solid fixation in at least 2 of the 3 zones is necessary for lasting fixation in rTKA. This concept focuses on individual anchorage and stabilization in each respective zone. The surgeon preoperatively analyzes which zones are available for fixation, noting if 1 or more is deficient, and then use this information to select the implant and fixation method for the case. 12 Optimal preoperative surgical planning helps to support maximal implant fixation.
Assessment of bone loss is essential for preoperative planning in rTKA, as the location and severity of defects determine which fixation strategies are appropriate in each anatomical zone. 13 Multiple bone loss grading systems have been established for pTKA and rTKA, to quantify the location and size of bone defects in preoperative radiographs and to standardize implant fixation as well as the evaluation of postoperative outcomes. The Anderson Orthopaedic Research Institute classification system and Nelson et al’s University of Pennsylvania system are some of the earliest and most commonly used defect classifications still popular today.13 -15 These grading systems are limited to the description of the defects in the epiphysis and metaphysis; they do not describe the integrity of the diaphysis. 16 More modern classification systems, such as Belt et al’s bone defect grading system for rTKA patients, can describing bone loss in all anatomical zones. 17 Scuderi et al’s bone loss classification system for failed stemmed TKA focuses on the integrity of the bone in the metaphysis and diaphysis and is based on radiographic assessments. This system is especially useful in grading the quality of the bone bed in the diaphysis, if fixation in this area is necessary in patients with larger epiphyseal and metaphyseal defects.4,10 These grading systems, however, fail to address the 3-D nature of bone defects. A modern bone defect classification system should provide a clear description of the location of defects in each of the 3 zones as well as their type (contained, uncontained). Considering the limitations of grading systems that rely on 2-D radiographic images and given the increasing utilization of 3-D imaging tools including computed tomography (CT) and magnetic resonance imaging (MRI), more 3-D classification systems are warranted.
Brenneis et al used 3-D CTs of tibial bone defects to create a new classification system. 16 According to the concept of zonal fixation, the 3-D defects were classified into 3 zones, further implementing a schematic classification visualizing the 3-D nature of the bone defect. While the technique includes evaluation of all anatomical zones, the study focused on metaphyseal and epiphyseal zones, since there were no cases of diaphyseal bone loss. 16
Preoperative Imaging
Radiographs are the most cost-effective imaging for preoperative TKA screening and allow an overall assessment of implant alignment and fixation, as well as the presence of secondary bone defects.11,18 In addition, radiographs allow for investigation of periprosthetic lucency and osteolysis, polyethylene insert wear, heterotopic bone formation, reactive bone formation, and periprosthetic fractures. 11
While radiographs are a valuable assessment tool, they have several disadvantages. They are technician-dependent, and implants often hide bony lesions.11,19 In general, 2-D radiographs cannot fully capture 3-D defects, which leads to underestimation of the size of bone defects. 20 In patients with suspected bone loss, CT scans can offer more accurate data. 16 While CT images can be limited by metal artifacts that obscure nearby soft tissue and bone, improvements in multidetector CTs and imaging protocols have decreased this impact. These improvements allow for 3-D analysis of bone defects, and their volumetric measurements. 21 Disadvantages include higher costs and exposure to radiation. 11
The use of MRI in TKA has been considered for the evaluation of the periarticular soft tissues, especially the extensor mechanism. Regarding the assessment of bone defect, it has been utilized for detecting osteolysis, particle disease, implant loosening, or intracapsular synovial deposits, which could indicate plastic wear and bone loss. 22 The use of MRI is mainly limited because of metal artifacts, which require special protocols. It is important to note that interpreting MRIs requires training and that adequate MRI is not widely available. 11
While significantly higher sensitivity for the evaluation of osteolytic lesions in MRI and CT compared to fluoroscopically guided radiographs has been reported, no difference in accuracy of defect volume measurements between CT and MRI was shown. 23 So far, there is a paucity of literature assessing the influence of imaging on surgical treatment. Greater use of cones/sleeves as well as epiphyseal augments in the tibia has been reported when assessing metaphyseal bone loss volume preoperatively using a CT scan; 3-D measured bone loss in the metaphysis has therefore been identified as a key factor for implant selection. 19
We believe that 3-D imaging assessment could have a similar impact on diaphyseal implant selection, specifically in cases with severe bone loss. Although preoperative imaging is constantly improving and therefore provides better visual assessment of bone loss, we can observe a lack of a quantifiable anatomical zone definition, leaving space for individual interpretation regarding zonal borders and transitions.
Anatomically Defined Zones
To date, few attempts have been made to anatomically define the epiphyseal, metaphyseal, and diaphyseal zones. One of them is Heim’s “system of squares” definition for long bone segmentation, published by the Arbeitsgemeinschaft für Osteosynthesefragen in 1990. 24
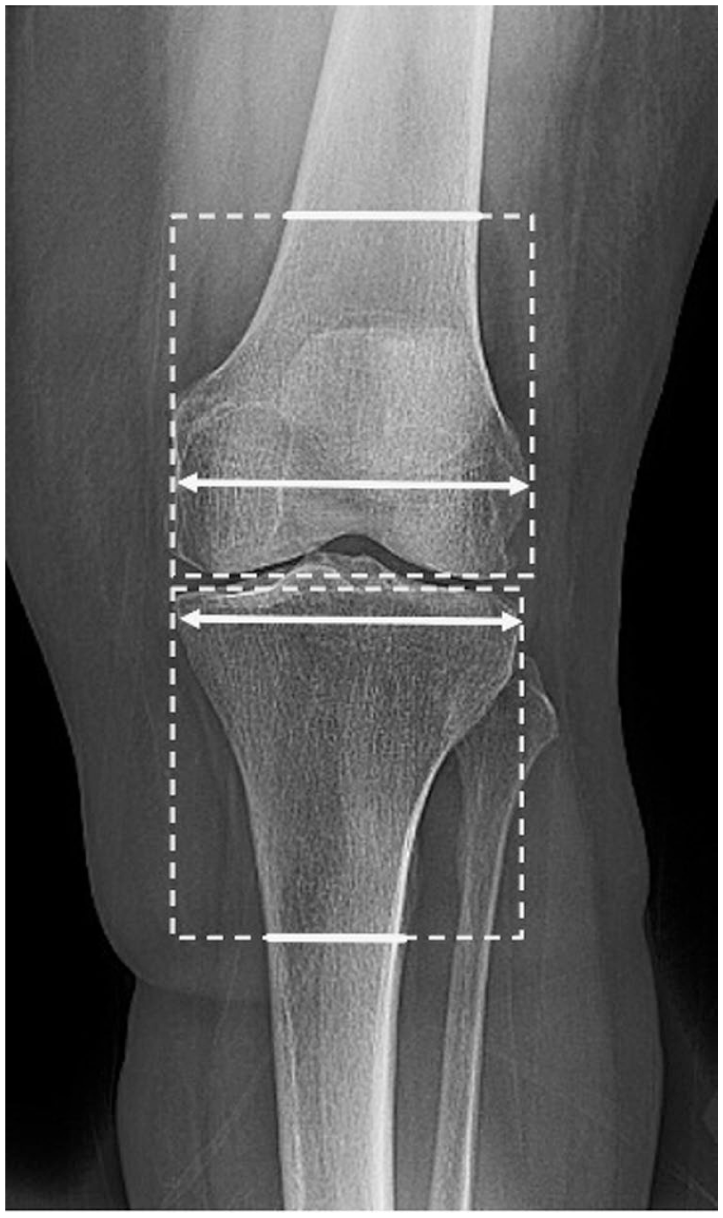
Heim’s “system of squares” established that a square is created starting from the most proximal (or distal) part of the bone as a reference line, with each line matching the distance of the widest part of the epiphysis in question. While the segment inside the square contains the epiphysis and metaphysis, without any clear anatomical separation, the diaphysis is defined as the bone outside the distal (or proximal) border of the square 24 (Figure 1).
The “system of squares,” proposed by Urs Heim and published by the AO. AO, Arbeitsgemeinschaft für Osteosynthesefragen.
Recent studies have modified this concept for the evaluation of implant fixation in rTKA.25,26 At the femur, the square length is defined by the widest condylar width. This delineating horizontal line further separates epiphysis from metaphysis. At the tibia, the square length is defined by the widest tibial width. Epiphyseal and metaphyseal separation is defined by the horizontal line delineating the widest fibular width. The implant aspect closest to the joint line marks the start of the respective square 25 (Figure 2).
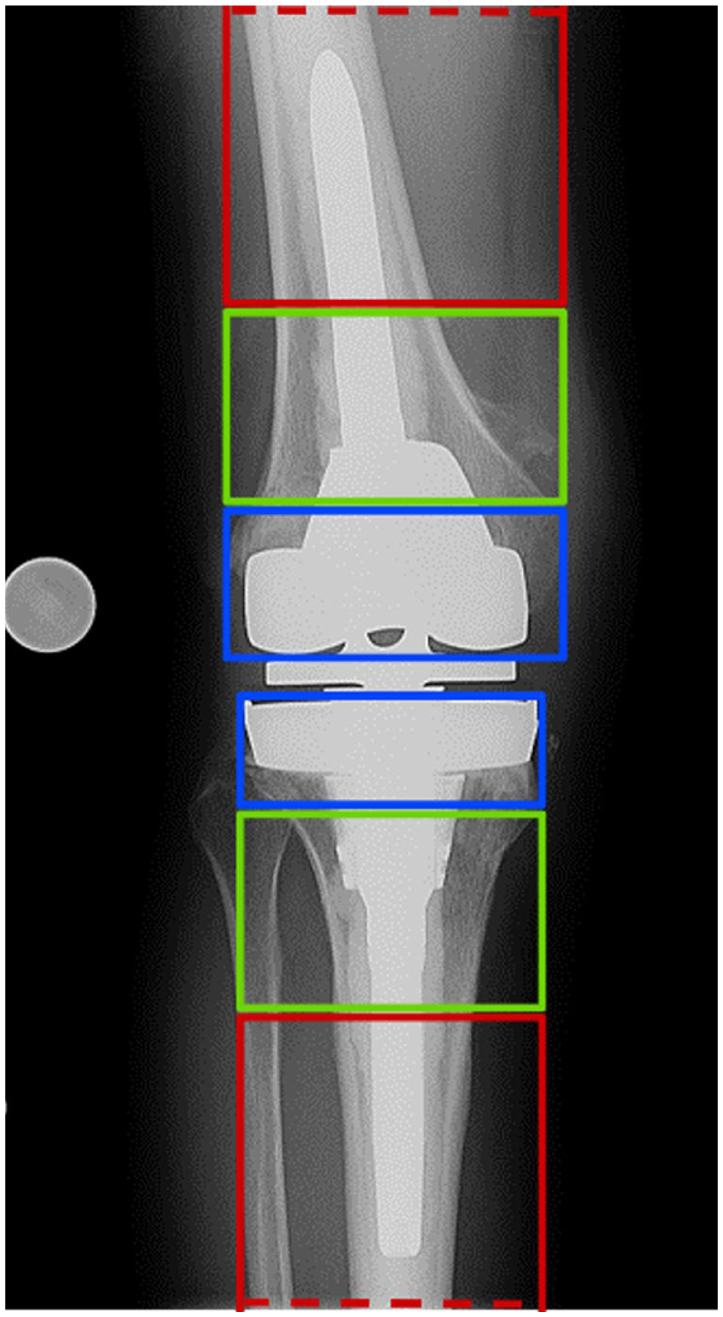
The modified “system of squares” with anatomic differentiation of epiphysis and metaphysis.
There are numerous approaches for femoral and tibial reconstruction, each addressing different bone defects and targeting different zones for fixation.8,11,27
A Closer Look at the 3 Zones
Zone 1: Epiphysis
One of the main rationales in the reconstruction of the epiphysis is restoration of implant alignment perpendicular to the mechanical axis of the femur and tibia, respectively. Bone defects within the epiphysis can be addressed using cement, bone graft, or augments. The latter are currently preferred for reconstruction of uncontained epiphyseal defects. 28
Oh and Scuderi advise the use of impaction bone grafting and/or cement filling for contained bone defects up to 5 mm in depth. 29 For small defects, good outcomes with pure cement technique have been reported. 30
Impaction bone grafting using morselized cancellous bone is usually applied for contained defects but can also be used for uncontained defects using a wired mesh to contain the defect. 31 Once a larger fraction of the epiphysis is affected by bone loss, metal augments should be used. 29 Augment use is recommended if more than 40% of the implant surface is unsupported by host bone or if the defect involves more than 25% of the peripheral cortical rim. 32
Femoral augments usually are block-shaped and can be applied on both condyles distally, posteriorly, or both. 33 Tibial augments can be block- or wedge-shaped and cover either the medial or lateral plateau or the entire tibial surface. Wedge augments are considered to be more resection friendly because intact cancellous bone can be preserved if partially present; however, they are also more likely to result in mechanical failure due to greater shear force. 34 Block augments present better load transfer to the underlying bone structure but require more bone resection. 27 Overall, augments can further provide a useful tool when restoring the adequate level of joint line in unilateral and bilateral bone lesions in both femur and tibia.35,36 Additionally, the asymmetric use can help to achieve rotational stability in unicondylar defects. 36
Although satisfactory results and survivorship have been reported for augment utilization with respect to bone loss, increasing augment thickness might negatively impact stability of the revision construct. 37 Therefore, further fixation in zone 2 (metaphysis) and zone 3 (diaphysis) is required, if a distal femoral or tibial augment is larger than 5 mm. 11
Zone 2: Metaphysis
The metaphysis is considered the key to stable implant fixation, 9 which can be achieved by cemented or uncemented fixation using cones or sleeves. 29 Designed with highly porous metals, usually titanium or tantalum, cones, and sleeves provide biological fixation through osseointegration over time. Furthermore, the availability of individual shapes and sizes enable the reconstruction of larger bone loss cavities and provide structural support. 27 While cones can be universally applied, there is discordant literature on the use of sleeves for uncontained defects.29,38
Mechanically, the expanded contact area serves to distribute the load and stress more effectively across the implant’s surface and stem extensions. Additionally, the highly porous coating creates significant friction with the surrounding bone, reducing implant movement and establishing a stable platform in the metaphyseal region with long-term fixation assured by bone ingrowth. 39
In addition to the long-term mechanical benefits, these techniques present several advantages including fast support for axial and rotational stability and reduced reconstruction complexity. However, their use also has disadvantages including high cost, potential need for host bone removal to facilitate placement, and difficulties in extraction if removal becomes necessary. 40 Furthermore, applying a broach for bone preparation can lead to intraoperative fractures. 29
Depending on the size of the defect, combined treatment including impaction grafting or structural allografts with cones can be performed. 31 First-generation designs showed limited viability due to less anatomic geometrical design and limited sizes, requiring additional host bone removal. 11 Newer generation cones are more compatible with different sizes and geometries, accommodating a lager range of bone defects. 41 However, excellent survivorship and ingrowth have been reported for both generations.42,43
Zone 3: Diaphysis
Fixation in zone 3 can be provided with diaphyseal stems, which can be inserted as an uncemented porous ingrowth stem, an uncemented press-fit stem in a hybrid construct, or as fully cemented stems. Stem fixation provides load sharing by distributing stress away from articular fixation and can further help bypass compromised metaphyseal bone. 44 In rTKA, significantly less implant failure can be witnessed when using stemmed prosthesis compared to nonstemmed implants. 45 Overall, both cemented and uncemented stem fixation techniques show comparable outcomes.
Fixation of uncemented stems is considered more technically difficult and is dependent on an ideal press-fit design with adequate stem size. In normal bone anatomy uncemented stems are more likely to generate desired anterior-posterior alignment and less deviation from the mechanical axis compared to cemented stems. 46 A major advantage for the use of uncemented stems is a potential better fixation in sclerotic bone, which can be frequently witnessed in re-rTKA. It is the belief of the authors that porous ingrowth stems should only be used in combination with distal femur replacement or proximal tibia replacement implants. Use of porous stems in combination with standard revision implants should be avoided if uncemented fixation can be achieved using metaphyseal sleeves or cones. Cemented stems are relatively easy to implant, especially in cases with asymmetric bone anatomy. 47 Cement itself can be loaded with antibiotics, which can be beneficial in the avoidance of infection following rTKA. 48 While adequate stem length has been extensively discussed in the literature, the “ideal” stem length has yet to be identified.
Short cemented stems have been shown to provide the same fixation strength as long uncemented press-fit stems. 27 However, whenever the epiphysis cannot be relied on for implant alignment, longer uncemented stems might be needed to ensure adequate implant alignment. In cases of prior diaphyseal instrumentation with failed stemmed TKA, the presence of a sclerotic canal can impair cement interdigitation for cemented stem fixation. Impaction grafting within the diaphysis can be used to reconstruct bone loss and, more importantly, improve bone-cement interdigitation for cemented stems. 49
Many prior studies compare cemented and uncemented stemmed prostheses in rTKA, reporting different results and advocating for different fixation methods, making a definitive statement on superiority impossible.
In the setting of extensive bone loss in rTKA that makes fixation in the metaphysis unreliable, segmental reconstructions, such as distal femoral replacements or proximal tibial replacements, are considered the last resort. Depending on the affected zones, resection levels can be adjusted accordingly and individual construct as well as stem length can be used to ensure appropriate fixation. 11 The outcome significantly depends on the extend of bone resection. 50 Proximal tibial replacements are less common due to the involvement of the patella tendon insertion and are mainly reported for oncologic indications. 51
In summary, the concept of zonal fixation offers a systematic approach for preoperative planning and intraoperative execution of rTKA, applicable to both tibial and femoral reconstructions. While proper anchorage in all 3 zones is most desirable, implant fixation in at least 2 zones is crucial for secure long-term fixation. 12 The metaphyseal zone has been identified as the key location for successful fixation that has resulted in a widespread use of uncemented cones and sleeve to augment fixation. 29
A Quantitative Implant Fixation Classification
To date there has been only 1 grading system that incorporates the concept of zonal fixation. d’Amato et al reported on a radiographic grading system that evaluates epiphyseal, metaphyseal, and diaphyseal fixation and considers bone loss (including previous instrumentation), bone quality, and fixation method and quality. 26 Due to the low occurrence of aseptic loosening, the study could not provide reliable correlation of overall score to survivorship for aseptic loosening. 26
While this classification provides a useful tool for preoperative evaluation and decision making on zonal fixation, the lack of clinical validation for the threshold of 1.5 points indicating good implant fixation should be taken into consideration. Although reporting excellent inter- and intra-observer reliability, d’Amato et al acknowledge the subjectivity of bone grading as sclerotic or cancellous, which is essential to metaphyseal and diaphyseal assessment in this classification system. 26
Conclusion
Bone loss after pTKA and rTKA can impact the epiphyseal, metaphyseal, and diaphyseal zones, requiring a tailored reconstruction strategy. The concept of zonal fixation provides an excellent systematic framework for a multizonal approach to ensure stable implant fixation, especially in rTKA. Preoperative planning with respect to zonal availability and defect assessment leading to optimal implant selection provide great clinical impact for the surgeon. The evolution of imaging modalities, particularly CT and MRI, have enhanced the preoperative assessment of the extent and morphology of 3-D bone defects. This information leads to a better understanding of which zones are compromised and enables more precise planning of fixation strategies and further validating the zonal fixation approach. Nevertheless, standard radiographs remain the most common screening tool, and many classification systems are based on this imaging technique. Future research should focus on developing standardized imaging protocols for bone loss assessment in rTKA, refining 3-D classification systems for bone defects that could help standardize the intraoperative defect reconstruction. Long-term studies need to be conducted to correlate preoperative bone loss patterns, implant alignment, patient demographics and function, and reconstruction techniques with postoperative outcomes. In addition, implant fixation classification systems should be further explored to evaluate their ability to predict implant longevity and guide intraoperative defect reconstruction and implant fixation.
Supplemental Material
sj-pdf-1-hss-10.1177_15563316261432646 – Supplemental material for Reconstruction According to Zonal Fixation and Adequate Imaging Techniques in Revision Total Knee Arthroplasty: A Narrative Review
Supplemental material, sj-pdf-1-hss-10.1177_15563316261432646 for Reconstruction According to Zonal Fixation and Adequate Imaging Techniques in Revision Total Knee Arthroplasty: A Narrative Review by Johannes M. Herold, Christian Manuel Sterneder, Peter K. Sculco and Friedrich Boettner in HSS Journal®
Supplemental Material
sj-pdf-2-hss-10.1177_15563316261432646 – Supplemental material for Reconstruction According to Zonal Fixation and Adequate Imaging Techniques in Revision Total Knee Arthroplasty: A Narrative Review
Supplemental material, sj-pdf-2-hss-10.1177_15563316261432646 for Reconstruction According to Zonal Fixation and Adequate Imaging Techniques in Revision Total Knee Arthroplasty: A Narrative Review by Johannes M. Herold, Christian Manuel Sterneder, Peter K. Sculco and Friedrich Boettner in HSS Journal®
Supplemental Material
sj-pdf-3-hss-10.1177_15563316261432646 – Supplemental material for Reconstruction According to Zonal Fixation and Adequate Imaging Techniques in Revision Total Knee Arthroplasty: A Narrative Review
Supplemental material, sj-pdf-3-hss-10.1177_15563316261432646 for Reconstruction According to Zonal Fixation and Adequate Imaging Techniques in Revision Total Knee Arthroplasty: A Narrative Review by Johannes M. Herold, Christian Manuel Sterneder, Peter K. Sculco and Friedrich Boettner in HSS Journal®
Supplemental Material
sj-pdf-4-hss-10.1177_15563316261432646 – Supplemental material for Reconstruction According to Zonal Fixation and Adequate Imaging Techniques in Revision Total Knee Arthroplasty: A Narrative Review
Supplemental material, sj-pdf-4-hss-10.1177_15563316261432646 for Reconstruction According to Zonal Fixation and Adequate Imaging Techniques in Revision Total Knee Arthroplasty: A Narrative Review by Johannes M. Herold, Christian Manuel Sterneder, Peter K. Sculco and Friedrich Boettner in HSS Journal®
Footnotes
Ethical Considerations
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This article was funded by the Stavros Niarchos Foundation Complex Joint Reconstruction Center at Hospital for Special Surgery.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Peter K. Sculco receives royalties from Enovis and is a consultant for Zimmer Biomet. Friedrich Boettner receives royalties from OrthoDevelopment and is a consultant for OrthoDevelopment, Inc, J&J Depuy, Medacta International S.A., and Symbios Orthopaedics S.A. Additionally, he has stock or stock options for AccuPredict, Inc. The other authors declare no potential conflict of interest regarding the publication of this paper.
CME Credit
Required Author Forms
Disclosure forms provided by the authors are available with the online version of this article as supplemental material.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
