Abstract
Background:
Decreasing wound healing complications is important for total joint arthroplasty. 2-Octyl cyanoacrylate with polymer mesh tape (2OPMT) is a skin closure system that works by combining a liquid adhesive with a polymer mesh to form a waterproof microbial barrier over surgical wounds. However, allergic contact dermatitis (ACD) has been a reported complication of 2OPMT use, with an incidence ranging from 0.5% to 2.5%.
Purpose:
We sought to report our results of 2OPMT with primary total hip arthroplasty (THA) and total knee arthroplasty (TKA) and determine the incidence of ACD.
Methods:
We conducted a single-institution, single-surgeon retrospective cohort study of 185 TKA and 154 THA patients who underwent procedures at a tertiary referral institution from October 2021 to November 2023.
Results:
Overall incidence of ACD associated with 2OPMT was 3.8% (13/339). Incidence of ACD in TKA was 3.8% (7/185) and in THA it was 3.9% (6/154). All skin reactions were recognized at the first postoperative visit and treated with a combination of topical and/or oral steroids and oral antihistamines. All ACD reactions resolved by the second postoperative visit, and none of these patients developed a surgical site infection or a periprosthetic joint infection.
Conclusions:
We found an ACD incidence of 3.8% with 2OPMT use in TKA and THA. This is similar to other studies reporting on ACD in TKA and THA. While it can be treated with routine use of steroids, antihistamines, and antibiotics, ACD is uncomfortable for patients and presents them with a concerning clinical appearance that requires additional treatment.
Level of Evidence:
Level III: retrospective cohort study.
Plain Language Summary
Keywords
Introduction
Periprosthetic joint infection (PJI) is a devastating complication after total joint arthroplasty (TJA), causing increased mortality and decreased quality of life.20,22 Despite advances in antiseptic techniques and antibiotic use, PJI is now the most common diagnosis associated with all-cause revision of total knee arthroplasty (TKA) and total hip arthroplasty (THA) in the United States. 15 It has been previously established that wound healing issues, in particular persistent drainage and hematoma formation postoperatively, can increase the risk of developing PJI.12,16 Therefore, there has been substantial interest in investigating the best methods of skin closure in TJA to minimize these complications. Historically, the literature has not been clear as to the best methods, as there is significant heterogeneity in the type of superficial closure chosen by surgeons, and studies comparing closure types have lacked the highest quality of evidence.4,7,17
In 2016, it was established that a subcuticular layer closure maintained the best perfusion in TKA, compared to either skin suture or staples. 21 Subsequently, there has been increased interest in the use of skin adhesive dressings to seal the skin over a subcuticular closure. It has been shown that compared to other techniques, skin adhesives have similar strength and efficacy in closure for TJA 9 and patients indicate they prefer the cosmesis of adhesives. 19
One of the adhesives in use combines a 2-octyl cyanoacrylate liquid adhesive with polymer mesh (2OPMT) to maintain a waterproof microbial barrier over the surgical incision (Dermabond Prineo Skin Closure System; Ethicon, Inc). Despite good clinical efficacy in reducing wound complications, 2OPMT use has been associated with reports of allergic contact dermatitis (ACD).8,18 Diagnosis of ACD is primarily clinical. Patients will typically develop a pruritic, erythematous, dry, scaly rash in the outline of the offending allergen (Figure 1). Early reporting on ACD with 2OPMT use showed an incidence of 0.5% in a large series. 5 With increasing awareness of ACD, other centers have recently reported rates >0.5%. 6
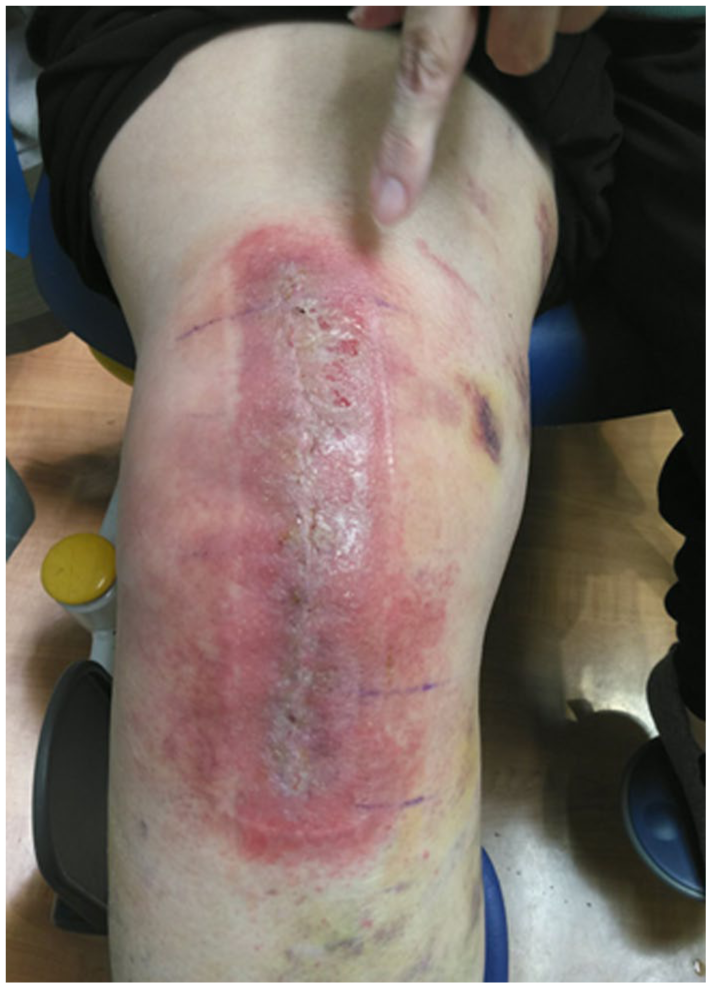
Example of allergic contact dermatitis reaction to 2-octyl cyanoacrylate mesh tape.
The purpose of this study was to report our results using 2OPMT with primary THA and TKA and determine (1) if the incidence of ACD was higher at our center than what had previously been reported, (2) what the results of treatment are for ACD patients, and (3) the final wound healing outcomes.
Methods
We conducted a single-institution retrospective consecutive cohort study of patients who underwent primary TKA or THA at a single tertiary referral institution from October 2021 to November 2023. All patients were treated by 1 primary surgeon. We identified 195 primary TKA and 173 primary THA patients who met these inclusion criteria. Of these patients, 10 primary TKA cases and 19 primary THA were removed because the 2OPMT wound closure system was not used in their procedures. Ultimately, 185 primary TKA cases and 154 primary THA cases were included for analysis. The overall group had 53.5% women and was 64.9 ± 10.8 years on average, with a BMI of 30.6 ± 6.5 (Table 1). All primary TKAs were performed with the medial parapatellar approach, and all primary THAs were performed with the posterior approach. In all cases, 0 vicryl and 2-0 Monocryl were used for the subcuticular closure and then 3-0 Monocryl for the skin and lastly the 2OPMT was covered with a Mepilex AG surgical dressing once dry. This dressing was kept on until the first follow-up visit at ~2 weeks post-op. ACD reactions, in addition to other postoperative complications and patient variables (Table 1), were extracted from the electronic medical record (EMR). In addition, postoperative treatments for presumed ACD reactions to 2OPMT were gathered from the EMR after diagnosis by the treating physician and followed until resolution. Cellulitis and ACD were differentiated by whether a red, itchy, dry/scaly rash appeared along the border of the surgical dressing as opposed to the diffuse, red, hot, swollen, and painful pattern indicative of cellulitis. Patients who had more severe ACD reactions were prescribed oral antibiotics to help prevent secondary infection.
Patient Characteristics.
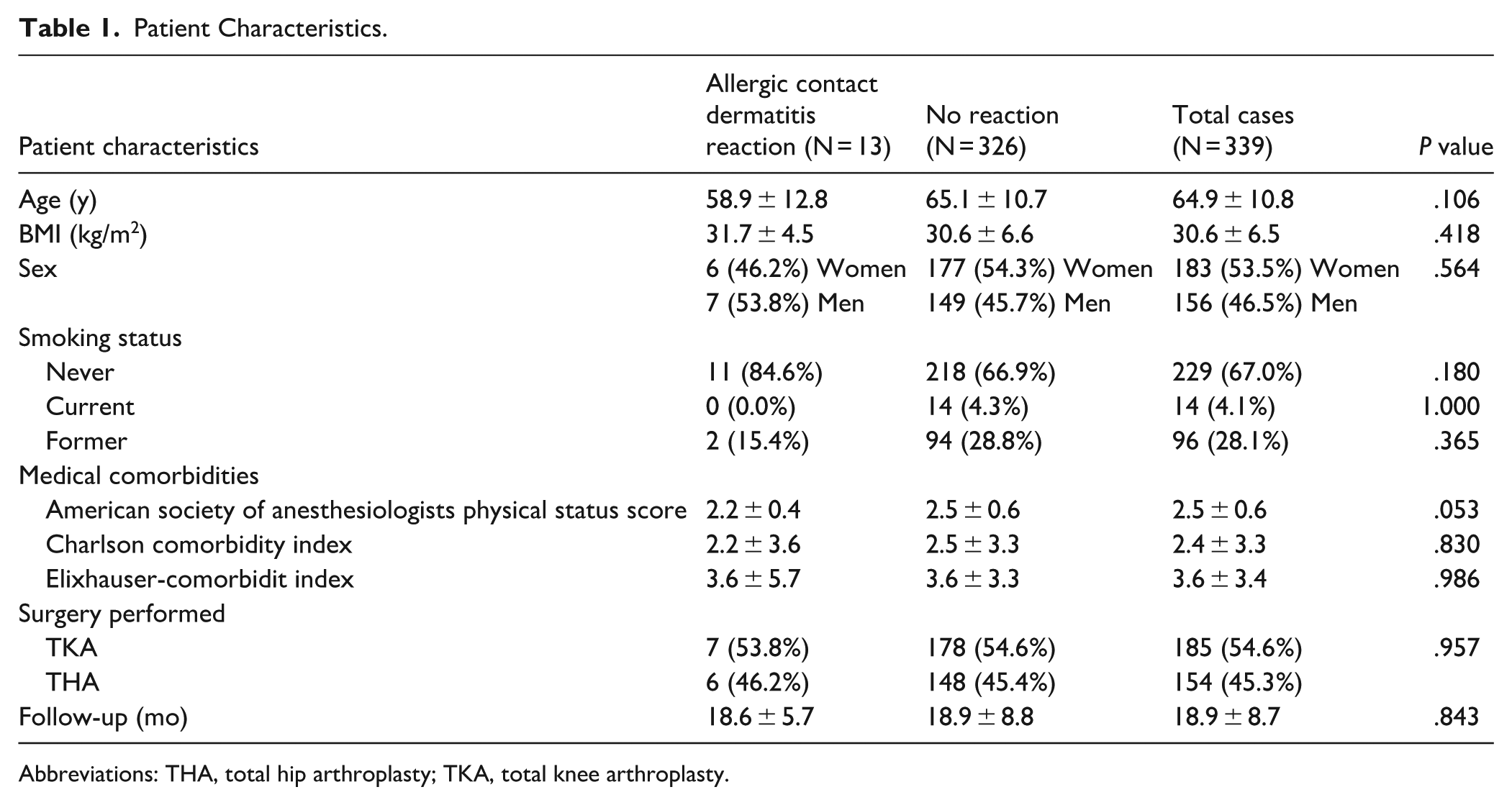
Abbreviations: THA, total hip arthroplasty; TKA, total knee arthroplasty.
Statistical Analysis
Two-tailed independent samples t-tests and χ2 analyses were used to calculate differences in demographic variables between cases with suspected 2OPMT ACD reactions and those with no reactions. Type I error was set at α = .05 for all analyses. The RECORD checklist was utilized in reporting this cohort analysis.
Results
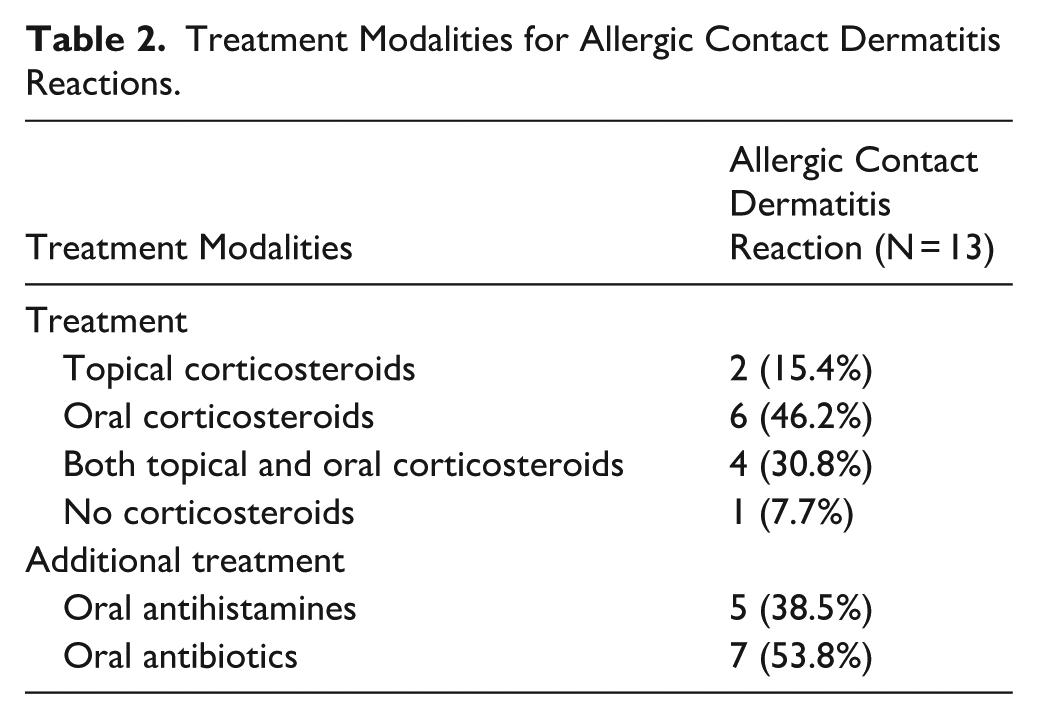
Overall, the incidence of ACD associated with 2OPMT was 3.8% (13/339). The incidence of ACD was 3.8% (7/185) in TKA and 3.9% (6/154) in THA. Of the 13 ACD cases, 6 (46.2%) had prior documented exposure to 2OPMT from a past surgery. All skin reactions were recognized at the first postoperative visit. Patients were treated with a combination of medications, including topical and/or oral steroids, oral antihistamines, and oral antibiotics, although no single regimen was used for all patients (Table 2). All skin reactions resolved at the time of the second postoperative visit at 12 weeks after surgery. There were no residual healing effects or complications in the ACD group. None of the patients with ACD developed PJI or required surgical intervention for wound complications at a mean follow-up time of 45.8 ± 14.1 months.
Treatment Modalities for Allergic Contact Dermatitis Reactions.
Discussion
Our retrospective cohort study reported a 3.8% incidence of ACD in a cohort of 339 primary TKA and THA cases. All cases were treated with a combination of topical and/or oral steroids, oral antihistamines, and oral antibiotics; each reaction resolved with no residual wound complications or PJI.
This study has several limitations. Primarily, this is a retrospective chart review, which is prone to selection bias and data accuracy, as it is contingent upon charting accuracy. ACD diagnosis was a purely clinical diagnosis in our study. It is possible that other factors could have caused a similar clinical appearance. This was a single-institution, single-surgeon study, and therefore, the results may not be generalizable to different populations.
ACD is a rash caused by a skin irritant that provokes an immune reaction. 1 This is thought to be a type-IV hypersensitivity reaction that requires an initial sensitization upon first contact with an allergen, followed by the development of dermatitis with repeat exposure. 8 Sensitization may occur with exposure to not only the specific 2OPMT product but also other acrylates or methacrylates, due to cross-reactivity.3,18 For example, Chalmers et al showed that in their cohort of 29 patients with ACD after 2OPMT use, up to a third of the patients had a prior exposure to an adhesive. 5 In our cohort, 6/13 (46%) of patients who developed ACD had a documented prior use of 2OPMT.
In this study of 2OPMT use with primary TKA and THA, our incidence of ACD was 3.8%. This is slightly higher than some other reported series in the hip and knee arthroplasty literature; for example, Chalmers et al showed an incidence of 0.5% in a large series of over 6000 cases, and Coles et al reported 2.3% in their group of over 1700 cases.5,6 Multiple other studies within the broader orthopedic literature outside of hip and knee arthroplasty report rates of ACD in the 2% to 4% range.10,18 Collectively, with the inclusion of our study, the reported incidence rate appears to be increasing over time. This may be due to increased awareness and improved clinical diagnosis of ACD, but it may also be a result of increased use of adhesives or methacrylates within the population, therefore increasing the base of patients who have previously been sensitized and are primed for a dermatitis reaction.
Diagnosis of ACD is primarily clinical. Patients will typically develop a pruritic, erythematous, dry, scaly rash in the outline of the offending allergen. In our study, patients first noticed a rash at an average of 11 days postoperatively. This is consistent with a recent meta-analysis of 47 studies and 193 cases of ACD after cyanoacrylate adhesive use, where symptoms were reported at an average of 10 days post-application. 11 The severity of the rash can vary, ranging from small papules to significant bullae. 5 In some instances, ACD can be confused with an infectious etiology such as cellulitis. If the rash appears within the initial perioperative period, inflammatory markers are likely to be elevated and thus unhelpful in diagnosis. 18 The primary distinguishing feature between the 2 entities is pruritus in ACD and pain in cellulitis. Other common signs of cellulitis or surgical site infection distinct from ACD include fever, purulent discharge, and malodor. 18
After recognition and diagnosis of ACD, the offending agent should be promptly removed and treatment initiated immediately. In our study, patients were treated with a combination of topical and/or oral corticosteroids, oral antihistamines, and sometimes antibiotics, depending on the clinical appearance of the rash. In our cohort, we had follow-up data on 8 of 13 patients with ACD who showed a resolution of symptoms at an average of 12 days after initiation of treatment. At the time of the second follow-up visit at 3 months, all clinical signs of the rash had dissipated. This time course and treatment outcome is similar to others, such as Ricciardo et al, who found a resolution of symptoms at 14 days. 14
To date, none of the patients in this study with ACD have developed a PJI, which is consistent with the broader literature in which no clear relationship has been established between ACD and infection. However, there is a theoretical risk as dry, scaly, potentially cracked skin is vulnerable to bacterial penetration, and therefore, expedient diagnosis and treatment are important. 18
There continues to be debate about the optimal methods of skin closure in TJA. Recently, a cohort of 20 expert orthopedic surgeons from the United States, Canada, and Europe were convened to provide guidance about preferred wound closure and management. 2 Using available evidence, they determined that there was no difference in wound complication rates between suture, staples, and skin glue for closure of the skin layer. However, as newer data becomes available, ACD associated with 2OPMT use is increasingly becoming recognized as a troubling clinical entity. Premkumar et al did a retrospective review of over 13 000 patients undergoing primary THA or TKA and found that 2OPMT use resulted in nearly triple the rate of ACD compared to Dermabond (glue without mesh adhesive), suture, or staples without any skin adhesives. 13 They also found no difference in wound drainage in patients using either 2OPMT or Dermabond, though there was a finding of higher overall drainage with staples alone. These data, in conjunction with clinical experience, have influenced the senior author to move away from using 2OPMT completely. The protocol now used for skin closure by the senior author is 3-0 running Monocryl, followed by Dermabond and a silver-impregnated dressing. Dermabond still provides preferable cosmesis and wound sealing, though with an apparent decreased risk of developing ACD. Anecdotally, since changing to Dermabond only, there have been no further reports of ACD postoperatively.
In conclusion, we found an ACD incidence of 3.8% with 2OPMT use in TKA and THA. This rate is similar to, though slightly higher than, other studies reporting on ACD in TJA. Collectively, there is increasing awareness and recognition of ACD with the use of 2OPMT. ACD is very effectively treated with a combination of corticosteroids and antihistamines, and as of yet, no long-term deleterious changes in clinical course have been associated with ACD development, to include infection. Nonetheless, ACD is uncomfortable for patients and presents them with a concerning clinical appearance that requires additional treatment. Physicians should consider evaluating other skin closure systems with similar clinical efficacy and cosmesis to 2OPMT that may not have as high a rate of ACD.
Supplemental Material
sj-docx-1-hss-10.1177_15563316251388424 – Supplemental material for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis
Supplemental material, sj-docx-1-hss-10.1177_15563316251388424 for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis by Richard S. Fuld, Jennifer W. Liu, Thomas C. Sullivan, Robert S. Neff, Terry A. Clyburn, Kwan J. Park and Timothy S. Brown in HSS Journal®
Supplemental Material
sj-docx-2-hss-10.1177_15563316251388424 – Supplemental material for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis
Supplemental material, sj-docx-2-hss-10.1177_15563316251388424 for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis by Richard S. Fuld, Jennifer W. Liu, Thomas C. Sullivan, Robert S. Neff, Terry A. Clyburn, Kwan J. Park and Timothy S. Brown in HSS Journal®
Supplemental Material
sj-docx-3-hss-10.1177_15563316251388424 – Supplemental material for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis
Supplemental material, sj-docx-3-hss-10.1177_15563316251388424 for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis by Richard S. Fuld, Jennifer W. Liu, Thomas C. Sullivan, Robert S. Neff, Terry A. Clyburn, Kwan J. Park and Timothy S. Brown in HSS Journal®
Supplemental Material
sj-docx-4-hss-10.1177_15563316251388424 – Supplemental material for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis
Supplemental material, sj-docx-4-hss-10.1177_15563316251388424 for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis by Richard S. Fuld, Jennifer W. Liu, Thomas C. Sullivan, Robert S. Neff, Terry A. Clyburn, Kwan J. Park and Timothy S. Brown in HSS Journal®
Supplemental Material
sj-docx-5-hss-10.1177_15563316251388424 – Supplemental material for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis
Supplemental material, sj-docx-5-hss-10.1177_15563316251388424 for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis by Richard S. Fuld, Jennifer W. Liu, Thomas C. Sullivan, Robert S. Neff, Terry A. Clyburn, Kwan J. Park and Timothy S. Brown in HSS Journal®
Supplemental Material
sj-docx-6-hss-10.1177_15563316251388424 – Supplemental material for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis
Supplemental material, sj-docx-6-hss-10.1177_15563316251388424 for The Incidence of Allergic Contact Dermatitis to 2-Octyl Cyanoacrylate With Polymer Mesh Tape in Total Joint Arthroplasty: A Retrospective Cohort Analysis by Richard S. Fuld, Jennifer W. Liu, Thomas C. Sullivan, Robert S. Neff, Terry A. Clyburn, Kwan J. Park and Timothy S. Brown in HSS Journal®
Footnotes
Ethical Considerations
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration.
Consent to Participate
Informed consent was waived from all participants included in this study by the IRB at Houston Methodist Hospital.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared the following potential conflicts of interest with respect to the research, authorship, and/or publication of this article: Kwan J. Park, MD, declares a relationship with Zimmer Biomet. Timothy S. Brown, MD declares relationships with Stryker Orthopaedics and AO Foundation. The other authors declare no potential conflicts of interest.
Required Author Forms
Disclosure forms provided by the authors are available with the online version of this article as supplemental material.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
