Abstract
Cerebral toxoplasmosis is common in AIDS patients; however, pneumocystosis of the brain is rarely documented. We report a patient with AIDS hospitalized for brain abscesses. Stereotactic brain biopsy with immunofluorescence staining was positive for Pneumocystis jiroveci. The patient received high doses of cotrimoxazole and had a favorable clinical course.
Presentation of Case
A 48-year-old man was admitted to the hospital in early August 2007, because of progressive changes in behavior and ataxia. The patient had been well until 1 week earlier, when a bilateral headache developed, with low-grade fever, confusion, disorientation, and a stumbling gait. The white cell count was 6800/mm3, with 54% neutrophils and 38% lymphocytes. A magnetic resonance imaging (MRI) of the brain (Figure 1) disclosed a large enhancing lesion of the left occipital cuneus measuring 3.3 cm surrounded by an edema, and multiple bilateral lesions varying between a few millimeters and 1.5 cm. Other small enhancing cerebellar lesions were also present. The patient was referred to our hospital.

Brain MRI showing multiple enhancing lesions
The patient is known to have HIV for 2 years with a CD4 count of 1045 cells/mm3 at that time. He resided in Africa (Abidjan) and had paludism. The patient has a history of diabetes and high blood pressure. He is unmarried and heterosexual. He had unprotected sex during his sojourn in Abidjan. He had no other sexually transmitted diseases (STD) and did not use any intravenous drugs. He did not smoke, or consume alcohol, but he eats raw meat. There was no history of other exposure to animals, contact with ill persons, photophobia, neck stiffness, visual problems, seizures, focal neurologic deficits, dyspnea, cough, vomiting, diarrhea, arthralgia, or rash. His medications included valsartan 80 mg ½ tab/d, bisoprolol fumarate 5 mg ½ tab/d, glimepiride 2 mg 2 tab/d, and omeprazole 20 mg 1 tab/d, and he has no known allergies.
His body temperature was 36.5°C, heart rate 72 pulsations/min, and blood pressure 160/110 mm Hg. A general physical examination showed no abnormalities except multiple small bilateral cervical lymphadenopathy. On neurologic examination, the patient was sleepy but was easily aroused and able to follow 1-step and 2-step commands. He was confused but not agitated. His speech was good. The cranial nerve functions were intact. He had difficulty cooperating with the motor examination but there were no obvious abnormalities. Sensitivity to a pinprick was intact in all the extremities. The finger-to-nose test was performed well. The gait was not tested. The biceps and knee jerks were ++ on the right and the left; the ankle jerks were + on both sides. The left and right plantar responses were flexor.
Fundus examination was normal. Laboratory tests were performed (C-Reactive Protein = 5.62 mg/L, CD4 = 137/mm3, CD8 = 1757/mm3 Treponema Pallidum Haemagglutination test negative, and Venereal Disease Research Laboratory test negative). HIV viral load was 100 000 copies/mL. All culture specimens were sterile (blood, urine). An electrocardiogram showed no abnormalities. Chest radiographs showed that the lungs were clear and that the cardiomediastinal silhouette was normal. A cardiac ultrasonographic examination showed no vegetations or other abnormalities.
Evolution
A stereotactic biopsy of the brain was performed: no germs were identified on direct examination, culture of the pus was sterile, microscopic examination of the biopsy specimen showed a histological aspect in favor of an inflammatory process; and absence of tumor, specific microorganisms, or viral cytopathic effects. Lumbar puncture, serologic tests, and polymerase chain reaction (PCR) for Toxoplasma gondii were not done. The patient was treated for CNS toxoplasmosis with clindamycin 1200 mg/d because sulfadiazine was not available, pyrimethamine 100 mg/d, folinic acid, valproic acid, prophylactic cotrimoxazole; and 2 weeks later antiretroviral therapy (lamivudine [3TC], zidovudine [ZDV], and indinavir [IDV]) was introduced.
Three weeks later, the patient developed a generalized seizure, loss of consciousness for 20 minutes followed by left hemiplegia. An urgent computed tomography (CT) of the brain revealed a large edema of the left frontal and parietal white substance with mass effect (Figure 2).
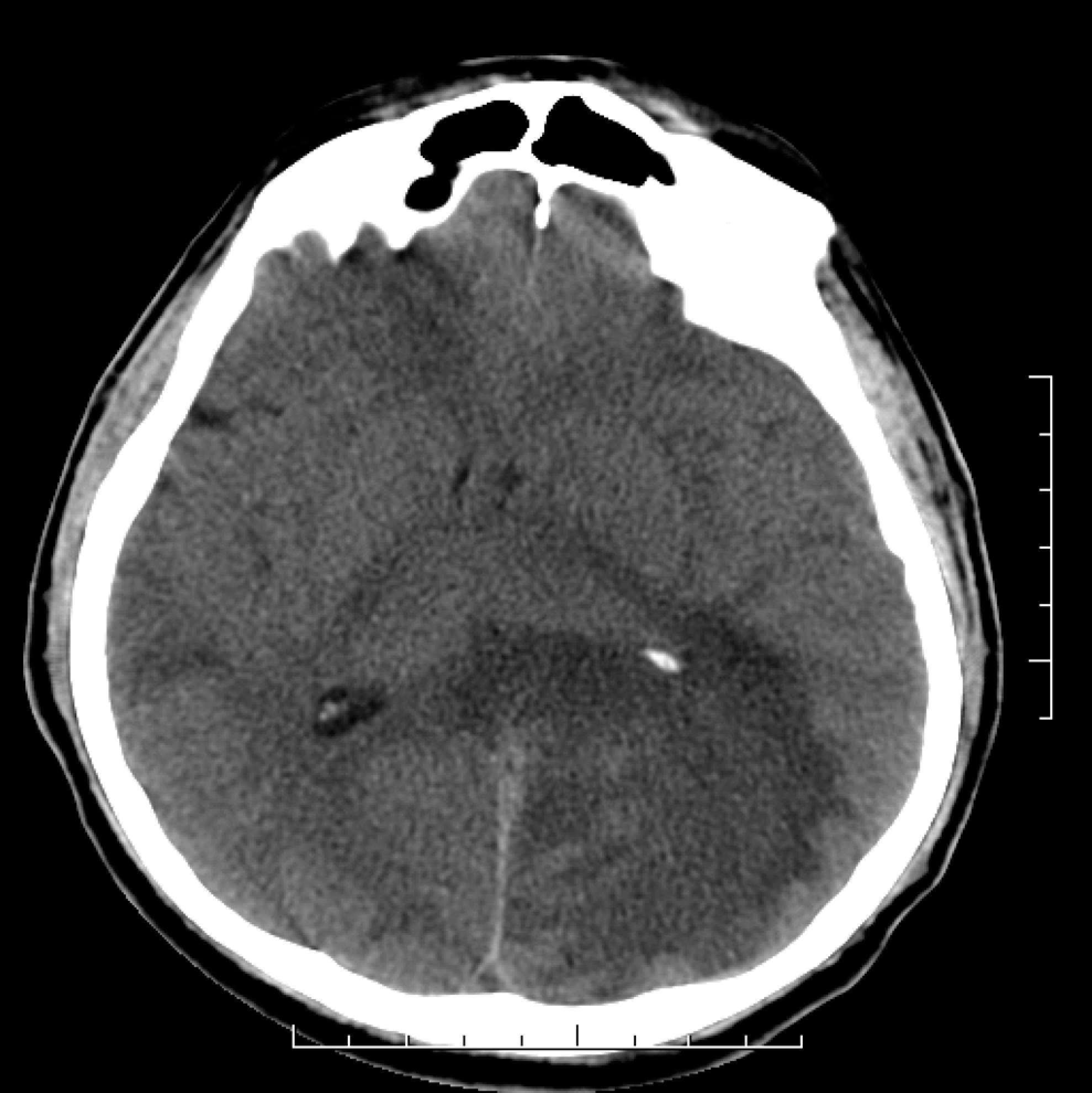
Computed tomography of the brain disclosing a large edema with mass effect
Because of the neurological deterioration despite current treatment, we thought to add corticosteroids to treat an eventual immune reconstitution syndrome. Phenytoin, piperacillin-tazobactam 4.5 g 3 times/d, and ciprofloxacin 600 mg/d were also added for 6 weeks. Subsequently, the patient had a partial recuperation of his left side motility. Antitoxoplasma therapy was kept on, given the persistence of the same CNS-enhancing lesions.
Six weeks later, the patient developed severe dyspnea, a high-resolution thoracic CT scan showed a diffuse bilateral centrolobar infiltration that predominates at the apex. CD4 count was 185 cells/mm3, and HIV viral load was 1500 copies/mL. A bronchoalveolar lavage (BAL) was performed, and immunofluorescence staining for Pneumocystis jiroveci (PJ) was doubtful. The patient received high-dose cotrimoxazole for 21 days and had a rapid clinical and radiologic improvement.
Repeated MRI of the brain 2 and 3 months after the start of antitoxoplasma therapy showed no change in the size of the lesions; a second stereotactic biopsy of the brain was performed: immunofluorescence staining with monoclonal antibodies for PJ was positive.
Clindamycin and pyrimethamine were stopped and high doses of cotrimoxazole (20 mg/kg trimethoprim [TMP] and 100 mg/kg sulfamethoxazole [SMX]) were reintroduced with atovaquone 750 mg twice daily for 2 months. New brain MRIs performed 2, 4, and 10 months after the beginning of anti-pneumocystis treatment revealed a clear reduction in the size of the cerebral lesions as in their enhancement. The size of the left occipital cuneus lesion has been decreased to 16 x 18 mm (Figure 3).

Repeated brain MRI revealing a clear reduction in the lesions size
Discussion
Pneumocystis jiroveci infections may extend beyond the lungs, and extrapulmonary pneumocystosis has been described in 0.5% to 2.5% of HIV-positive patients. 1,2 A search of the English-language literature from 1981 to 1995 was performed to identify reports or reviews of cases of histologically confirmed extrapulmonary pneumocystosis. A total of 109 HIV-positive patients with confirmed extrapulmonary pneumocystosis were identified, and 7 of these patients had central nervous system (CNS) pneumocystosis. 3 All 7 cases were diagnosed after death, during necropsy. 2 –8 Of these 7, 2 underwent CT of the head; 1 patient had cerebral atrophy 4 and the other 1 showed abnormalities. 3 Six of these had some concomitant infectious CNS involvement: cryptococcal meningitis in 2 patients, 5,6 HIV-1 encephalopathy in 2 patients, 3,4 and CNS toxoplasmosis in 2 patients. 7,2 Three had a history of PJ pneumonia. 2,3,8 No one underwent lumbar puncture.
Vidal and colleagues reported the first premortum diagnosis of CNS pneumocystosis. 9 Their patient was a 38-year-old homosexual man who presented with confusion and mild neck rigidity. A cranial CT scan indicated mild cerebral atrophy. Pathological examination of lumbar puncture revealed cryptococci and PJ; the latter was identified by immunohistochemistry with monoclonal antibodies. The patient was treated successfully with high doses of cotrimoxazole. 9
To our knowledge, the present case is the first diagnosis of CNS abscesses due to PJ in HIV-positive patients. The abscesses might be caused by other germs, but it is certain that pneumocystis participates in their pathogenesis. The immunofluorescence staining was positive; the abscesses had clearly decreased in size after the treatment with high doses of cotrimoxazole, and the patient showed continuous clinical improvement. The present report may allow us a new diagnostic and therapeutic approach for refractory and persistent CNS abscesses in HIV-positive patients in whom sulfadiazine was not used.
Footnotes
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
The author(s) received no financial support for the research, authorship, and/or publication of this article.
