Abstract
Background:
Health care systems should be designed to provide the care that people need and want; person-centered metrics are therefore critical data inputs to this process.
Materials and Methods:
We used multiple national datasets to develop a more person-centered metric for estimating need for contraception, comparing results made using a conventional approach with this new approach. The conventional metric estimates the number of individuals who have a likely need for contraceptive services based on their sexual experience and presumed risk for pregnancy. The new metric estimates the number of individuals who have a self-defined need for contraceptive services based on their current or recent contraceptive method or service use or their expressed desires to use contraception.
Results:
We found that the overall number of individuals considered to have a need for contraceptive services is roughly similar when comparing the conventional approach (37.8 million) with the new approach (38.3 million or 39.2 million, depending on the survey). However, these numbers represent somewhat different people according to each metric, with the traditional metric misclassifying some individuals who themselves desire to use or not use contraception.
Implications:
A new, more person-centered metric will better align measurement of contraceptive service need with what people want and will improve estimates of potential demand for care and how many individuals are likely to seek care. This paper provides policymakers and program planners with the thorough methodology and justification for the new metric that will be needed if the new metric is to be accepted and adopted for wide use.
Introduction
Documenting the number of people who need specific health care services has long been a critical aspect of health care administration and planning, both to estimate needed resources and to understand the impacts of meeting people’s needs. In the field of sexual and reproductive health (SRH) care in the United States, one key metric that has been relied on for decades to determine allocation of resources—especially federal and state funding for the delivery of SRH care—is the “number of women 1 in need of contraceptive services and supplies” and those who may need public financial support for those services because they come from low-income families or are adolescents who need confidential care.1,2 Specifically, contraceptive need is defined as the need (or desire or demand) for contraceptive services and supplies over a one-year period, including medical services or counseling related to contraception; for example, information and services to start, stop, switch, or continue method use, as well as to obtain contraceptive supplies.
Historically, this metric of contraceptive need, heretofore called the “conventional need metric,” was designed to estimate the population of reproductive-aged women at risk of unintended pregnancy, 2 a group presumed to need contraceptive services and supplies. The conventional need metric has been widely used by a variety of stakeholders to demonstrate where and how to allocate public funds for SRH care delivery, especially funds via the Title X federally funded family planning program. 3
There has been growing recognition that this conventional metric may not accurately reflect the perspectives of those whom it purports to describe and is therefore not addressing a key aspect of health care quality according to the Institute of Medicine: 4 person-centeredness. 5 Taking a person-centered approach requires prioritizing a person’s lived experiences, desires, values, and reproductive autonomy. 6 Applying a person-centered lens to measurement, specifically, involves both allowing individuals to self-identify their needs, values, and/or preferences and ensuring individuals themselves determine the extent to which these needs, values, and/or preferences have been fulfilled. 7
In contrast to a person-centered approach, the conventional metric has assumed that individuals have a potential need for contraceptive services based on demographic and behavioral characteristics rather than their own reports of their desires. Further, the growing body of research demonstrating problematic conceptualization and measurement of unintended pregnancy likely undermines the conventional need metric, given its reliance on the assumption that being “at risk” of unintended pregnancy can be equated with a need for contraception and, therefore, contraceptive services. In addition, the conventional metric excludes individuals who use contraception for a variety of reasons beyond pregnancy prevention but are not considered “at risk” of unintended pregnancy (e.g., those who are not sexually experienced). Finally, the conventional need metric has historically focused on women (self-identified or identified by health centers) as the only individuals with a potential demand for contraceptive services, in contrast to the field’s current understanding that people of all genders may use and desire contraceptive services.
Several scholars have documented individual-level reports of desires regarding contraception among survey respondents at the national- and state-levels and among clinical patient populations in the United States.5,8,9 Drawing on their findings, a new population-level metric may be able to leverage individual reports in surveys to better understand aggregated desires and needs and apply that information to make need estimates at various geographic levels. Such a metric may also be especially useful for identifying barriers to care and gaps in where services are delivered and for understanding the extent of resources needed to provide this care. Hence, we set out to develop an updated, population-level metric that moves us closer to understanding person-centered need for contraceptive care. This process involved several stages, including convening meetings to gain the perspectives of stakeholders on the conventional and potential new approaches to measuring population-level contraceptive service need and drawing on individual-level nationally representative survey data to identify people’s reports of their own needs and desires regarding contraception and contraceptive services.
In recent years, reports of conventional need metric results have defined contraceptive need as the potential demand for contraceptive services and supplies and used the terms need and demand interchangeably. We considered moving away from the term “need” for the new metric, but input from concurrent activities aimed to elicit perspectives from people who may have a need for contraception indicated that the term was not problematic and, in fact, resonated with them. Hence, we decided to continue to use the term “contraceptive need” for the new metric, while offering definitions to clarify what this means and focusing on the needs that individuals report. Contraceptive need as used here is unrelated to the metric “unmet need,” commonly used to measure the number of individuals in developing countries who do not have access to or have not used a modern contraceptive method.
The key aim of this paper is to provide a solid methodological description of a new contraceptive need metric, along with substantive justification for adopting this new metric. To achieve that aim, the specific objectives of the current analysis are: (a) to compare who is represented within the numerator and denominator according to the conventional need metric and a new proposed need metric that moves closer to being person-centered and represents survey respondents’ self-defined need for contraceptive services; (b) to leverage insights from this comparison to integrate several person-centered items into the calculation of a new population-level metric of contraceptive need using currently available data sources; and (c) to compare results from two data sources and determine the acceptability for making regular on-going estimates of self-defined contraceptive need at the national, state, and potentially county levels, as has been done with the conventional need metric, and with a big enough sample size to make need estimations for population subgroups.
Materials and Methods
To inform our thinking about how best to update the analytic approach to calculating contraceptive need at a population level, we drew on discussions with technical experts (November 2023 and June 2024) and lay experts with lived experience of being potential or actual contraceptive users (June 2024). Colleagues at the Coalition to Expand Contraceptive Access (CECA) hosted and facilitated these virtual discussions, which included specific questions about interpretation of the conventional need metric, how it was used, and how it resonated with participants, among broader discussions about receiving SRH care.
We used two national-level datasets to construct three population-level metrics of contraceptive need over a one-year period and compared the results. The conventional need metric was estimated using data from the 2017–2019 National Survey of Family Growth (NSFG). We then estimated two versions of a new self-defined need for contraceptive care metric. These metrics move toward a more person-centered approach by centering the contraceptive care preferences of individuals (i.e., whether respondents express a desire to use contraception or obtain contraceptive services), thus moving away from the conventional approach of assuming individuals need contraceptive services due to their demographic and behavioral characteristics.
The first version of a new contraceptive need metric was estimated using data from the Person-Centered Contraceptive Access Metrics Study5,10 (PCCAM). The aim of this study was to develop holistic and person-centered approaches to measuring contraceptive access and provide national estimates for four contraceptive preference metrics using a national survey. The second version of a new contraceptive need metric was estimated using data from the 2017–19 NSFG. The purpose of estimating this second version was to determine if it would be possible to do so using a data source that is part of an ongoing data collection effort and could be replicated sustainably going forward.
Across all three metrics, survey respondents were broadly classified into two groups: those in need of contraceptive services and those not in need of contraceptive services. Figure 1 details the data available from each survey (data inputs), including population groups included in each survey and how the survey’s data on these groups is used for calculating the three metrics. To operationalize self-defined need for contraceptive services, we used variables from each survey that measured:
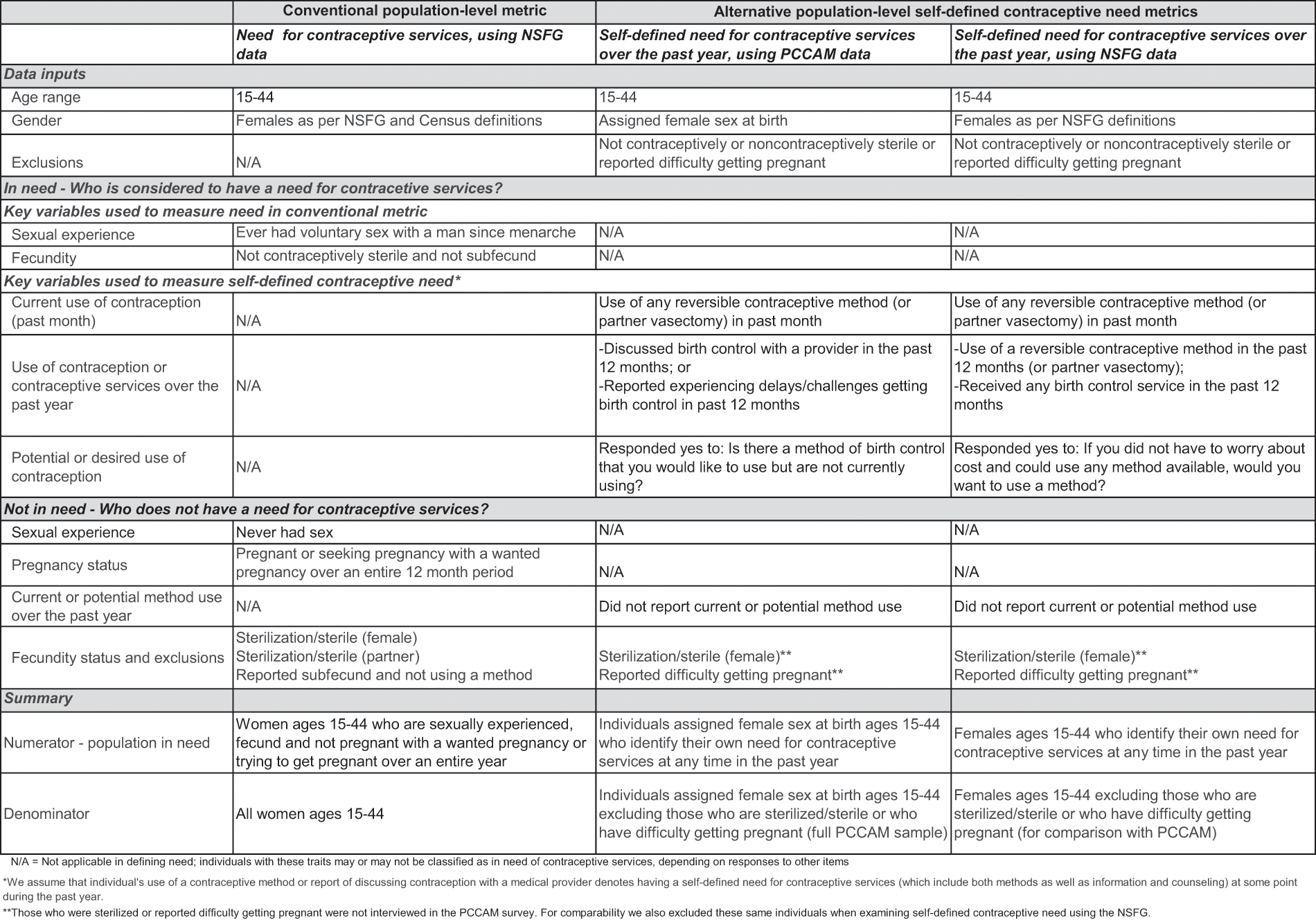
Data inputs and variables used for metrics to examine the potential need for contraceptive services using the conventional approach and an alternative approach designed to be more person-centered and focused on individuals’ self-defined need for contraceptive services. Text table providing data inputs and key variables used to define the need for contraceptive care using the conventional approach and a new, more person-centered approach and two different data sources.
current month or past year use of contraceptive methods or a reported visit for contraceptive or related services, including partner’s use of condoms or vasectomy or
affirmative desire to use contraception or obtain contraceptive services.
We assume that these variables and responses are a proxy for self-defined contraceptive need and that they signal a person’s own report of having a need for some type of contraceptive service or care over a one-year period. All users of reversible contraception or partner methods may need services during the year if they have questions or side effects or need to stop or switch their method, including contraceptive information or counseling, services (including removals), supplies, prescriptions, etc. We assume those who are currently dependent on partner vasectomy as their only method are similar to those who are currently using long-acting reversible methods, and both are likely to need ongoing services over an entire year. While not fully person-centered given that this metric does not address whether individuals’ needs have been fulfilled, operationalizing contraceptive need in this manner moves us in that direction, and thus we consider it to represent self-defined need.
Key variables used for the conventional contraceptive need metric (NSFG)
For the conventional metric, individuals’ need for contraceptive care is assessed only among those who reported prior sexual experience and those assumed able to become pregnant. Respondents who reported having had voluntary sexual intercourse with a male since menarche were classified as sexually experienced, and those who reported that they had not undergone a sterilization procedure and believed they could become pregnant were classified as fecund and in need of contraceptive care. Respondents who reported difficulty getting pregnant were classified as in need of care if they also reported using a contraceptive method.
Respondents were classified as not in need of contraceptive care if they reported never having voluntary sex since menarche or if they reported being pregnant with a desired pregnancy or seeking pregnancy over the entire prior 12-month period. Respondents who were surgically or nonsurgically sterile (including those who had undergone tubal sterilization) and those with male partners who were surgically or nonsurgically sterile (including those who had undergone vasectomy) were classified as not in need, along with respondents who reported thinking they would have difficulty getting pregnant or carrying a pregnancy to term, so long as they were not using a contraceptive method. These classification protocols relate to the conventional metric’s focus on measuring the need for contraceptive services to prevent pregnancy. Although people who are sterile or who report difficulty getting pregnant may need or use contraceptive services for other reasons, if they do not need ongoing services for pregnancy prevention, they were not classified as ‘in need.’
Key variables used for the self-defined contraceptive need metric (PCCAM version 5 )
Using the PCCAM, we considered individuals to have a self-defined need for contraceptive services based on responses to items regarding current and prospective contraceptive use, experiences of barriers to obtaining contraception, and discussion of birth control with a health care provider. All PCCAM respondents were asked to indicate which contraceptive methods they had ever used. For any methods they indicated having ever used, respondents were asked about use of that method in the last month. Current contraceptive users included all respondents reporting use of a contraceptive method in the last month, including respondents who reported partner use of condoms and vasectomy. In addition, respondents were asked if there was a method of contraception that they were not currently using that they wanted to use. Those nonusers of contraception who indicated a preference to use a method were considered prospective users of contraception. Respondents who reported ever using or attempting to obtain contraception were asked if they had experienced a challenge or delay obtaining desired contraception in the last 12 months. Those responding affirmatively were considered to have a potential need for contraception. All respondents were asked if they had ever discussed contraception with a health care provider and, if they had, when they had most recently discussed contraception. Those who reported discussing contraception in the prior 12 months were also considered to have a potential need for contraceptive services.
Respondents who did not report either current or prospective contraceptive use as defined above were classified as not having a self-defined need for contraceptive services. Finally, individuals who were sterile or who reported difficulty getting pregnant were not eligible for inclusion in the PCCAM Survey, although they may have a self-defined need for services.
Key variables used for the self-defined contraceptive need metric (NSFG version)
Using the NSFG, we constructed a metric of self-defined need for contraceptive care that aligned as closely as possible with the data inputs from the PCCAM. We considered individuals to have a self-defined need for contraception if they reported current or past use of a contraceptive method in the prior 12 months, including partner use of condoms or vasectomy, receipt of contraceptive or contraceptive-related care from a medical provider in the prior 12 months, or a desire to use a contraceptive method if cost were not an issue.
Respondents who did not report either current or prospective contraceptive use as defined above were classified as not having a self-defined need for contraceptive services. Finally, individuals who reported being sterile or having difficulty getting pregnant were excluded from the analysis and not considered regarding their contraceptive need status for the self-defined need metric defined using the NSFG. This exclusion was made for comparability with the PCCAM survey.
Across all three metrics, we drew on the following socio-demographic characteristics that were available in both the NSFG and PCCAM datasets: age (5-year groups), race/ethnicity, poverty status or income level based on federal poverty level (FPL), marital status, insurance status, and education.
Analysis
We first conducted overall descriptive analyses to examine distributions of all individuals assigned female at birth that were classified as either having or not having a contraceptive need, comparing the conventional need metric and the PCCAM version of the self-defined need metric. Next, we compared the two self-defined contraceptive need metrics (PCCAM and NSFG versions) on distributions of need according to current or potential past-year contraceptive use, method use, and sexual experience status. All analyses were conducted using Stata 17 or 18.0.
Results
Who is classified as having a need for contraceptive care?
Overall, 76% of fecund females, ages 15–44 (about 37.8 million females), are classified as having a need for contraceptive care under the conventional metric. All of them are classified as such because they are sexually experienced and did not report being intentionally pregnant or seeking pregnancy during the 12 months prior to the survey (Table 1 and Fig. 2).
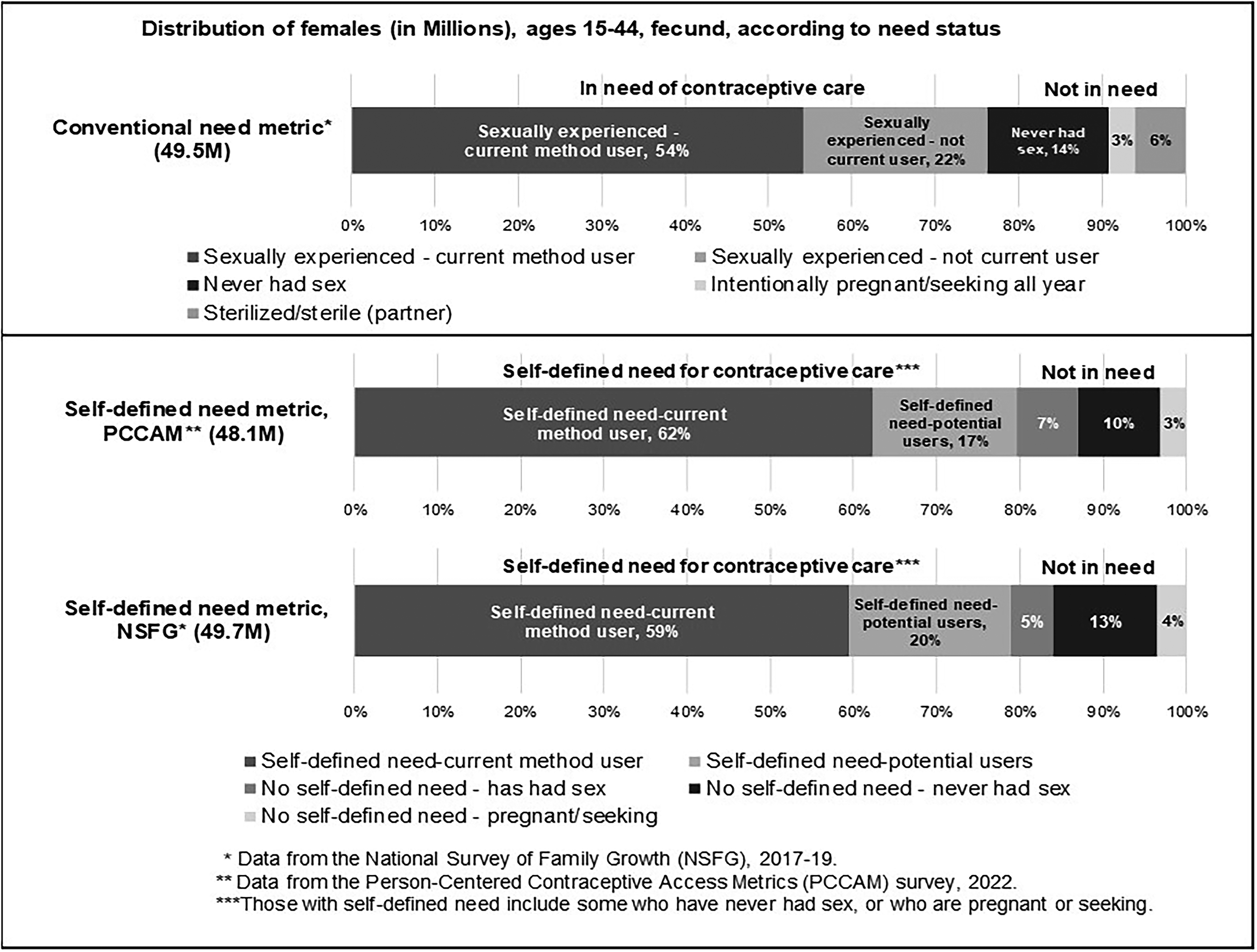
Comparison of conventional and self-defined contraceptive need metrics. Bar graph showing the distribution of females according to whether they have a need for contraceptive care or not according to current method use, sexual experience, and pregnancy status, and comparing the conventional need metric and two versions of a new self-defined need metric.
Need for Contraceptive Services over a One-Year Period-Measurement Options Comparing the Conventional Metric with Self-Defined Need Metric Options Using the Person-Centered Contraceptive Access Metrics Study, 2022, and the National Survey of Family Growth, 2017–19
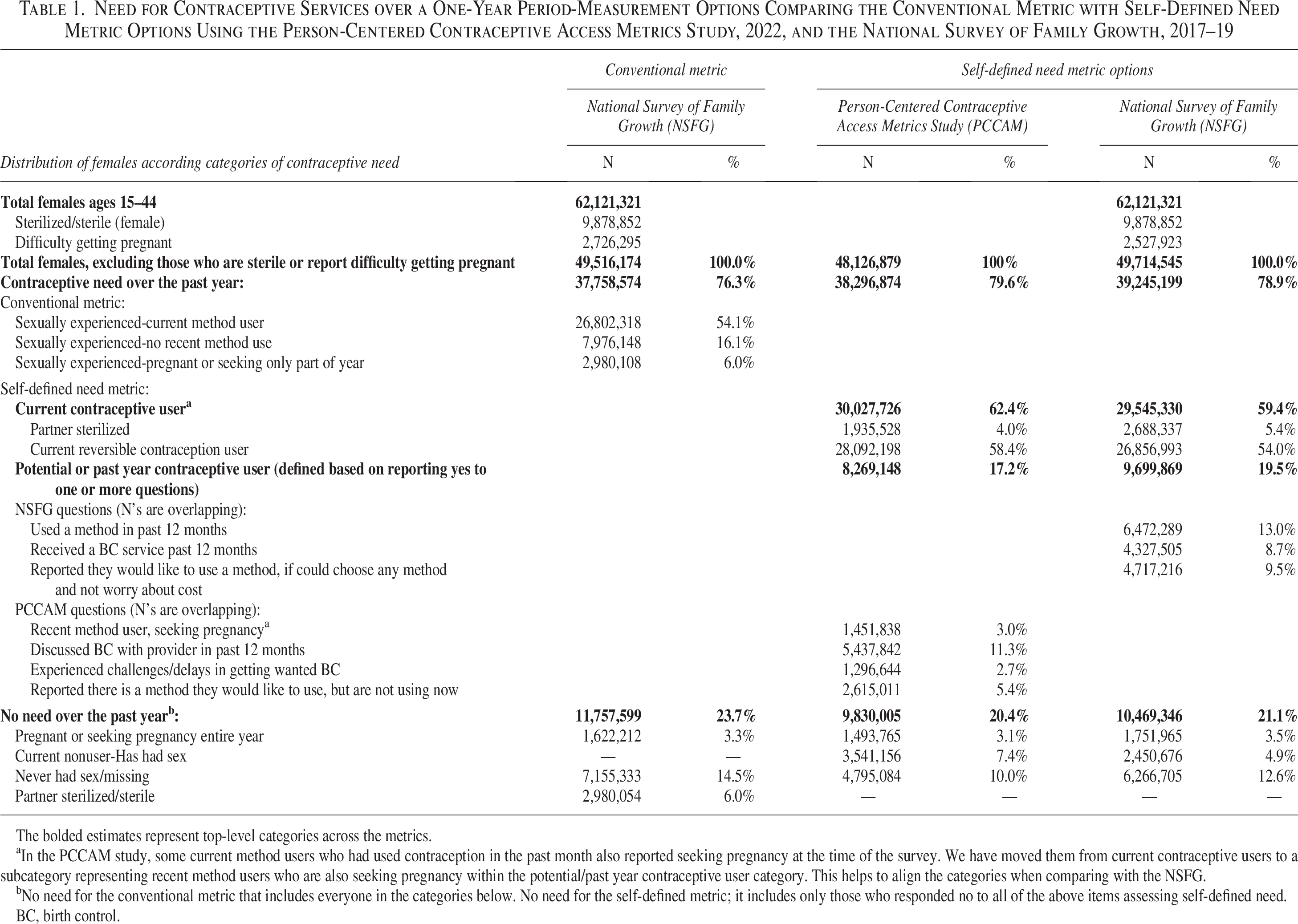
The bolded estimates represent top-level categories across the metrics.
In the PCCAM study, some current method users who had used contraception in the past month also reported seeking pregnancy at the time of the survey. We have moved them from current contraceptive users to a subcategory representing recent method users who are also seeking pregnancy within the potential/past year contraceptive user category. This helps to align the categories when comparing with the NSFG.
No need for the conventional metric that includes everyone in the categories below. No need for the self-defined metric; it includes only those who responded no to all of the above items assessing self-defined need.
BC, birth control.
In comparison, 80% of fecund females, ages 15–44 (about 38.3 million females), are classified as having a self-defined need for contraceptive services under the new metric using PCCAM data. Of these, 62% are classified as being in need due to their current use of a reversible contraceptive method or their partner’s use of vasectomy. An additional 17% were classified as having a self-defined need because they indicated potential interest in using a method or recent method use or contraceptive counseling over the past year.
Similarly, 79% of fecund females ages 15–44 are classified as having a self-defined need for contraceptive services under the new metric using NFSG data. Compared with the PCCAM distribution, slightly fewer (59%) reported self-defined need due to current contraceptive use, and slightly more (20%) were classified as having self-defined need because of either recent method or contraceptive service use in the past year or potential use if they could use any method available.
Overall, the proportion of individuals in need who are current method users is lower for the conventional metric (54%) compared with the self-defined need metric (59–62%). Some of this difference is due to how those with partners who have undergone sterilization are classified, with the new metric purposefully classifying such individuals as in need and the conventional metric excluding them. (Four to five percentage points of current method users for the self-defined metrics are females with sterilized partners.) In addition, there is variation among the metrics in the number of individuals in need who are not currently using a method, with the highest percentage for the conventional metric (22% versus 17–20%). This is primarily due to the conventional metric classifying everyone who is sexually experienced (and not otherwise excluded) as needing contraception, compared with the self-defined need metrics, which classify respondents who are not current method users as being in need if they indicate recent or potential interest in contraceptive use, regardless of their sexual experience status. These can include individuals who have never had sex or who are currently pregnant or trying to get pregnant if they report any recent or potential interest in using contraception or contraceptive services.
Who is classified as not in need of contraceptive care?
Overall, 24% of fecund females are classified as not in need under the conventional metric and 20–21% under the self-defined contraceptive need metrics. Over half of this group have never had sex under the conventional metric (14%), with the rest reporting being intentionally pregnant or seeking pregnancy over the entire year (3%) or having partners who use vasectomy (6%). For the self-defined need metrics, about half have never had sex and do not report any recent contraceptive method or services use, and the remainder either have had sex or report being pregnant or seeking pregnancy but do not report any of the self-defined need criteria.
Variation in items used to measure self-defined need
Table 1 also illustrates the variation between the PCCAM and NSFG survey items by comparing the reported numbers and percentages of respondents who were not currently using a method but who responded positively to each of the potential use questions. The NSFG questions are somewhat more direct, identifying all who either used a method or received a birth control service in the past year. In contrast, the PCCAM survey was not specifically designed to measure prior-year use, so the questions utilized to capture this were less direct, such as whether respondents reported discussing contraception with a provider or having difficulty obtaining wanted contraception over the past year. Both surveys identify those who were not currently using a method but who reported that they would like to use contraception. However, the question wording, as well as the proportions of respondents responding affirmatively, were quite different (9% for the NSFG and 5% for the PCCAM).
In sum, the overall estimates of the numbers of individuals who are classified as in need versus those not in need are not dramatically different when comparing the conventional and the two self-defined contraceptive need metrics. However, the numbers do vary, and there are key differences in approach and in the items used to define how individuals are classified as having a potential need for contraception over the year. The self-defined need metrics include individuals who report that they have used or would like to use contraception or contraceptive services as having a self-defined contraceptive need, including some who have never had sex. They also include those with partners who use vasectomy as being in need (in contrast to the conventional metric, which does not). Finally, the self-defined need metrics do not classify all sexually experienced individuals as needing contraception (in contrast to the conventional metric) unless they also report current contraceptive method or service use or interest in using a method.
In addition to comparing the distributions of respondents to the NSFG and the PCCAM according to self-defined contraceptive need, we also looked at the socio-demographic distributions of individuals in need across the surveys (age [5-year groups], race/ethnicity, poverty status or income level, marital status, insurance status, and education) and found that they were very similar (Table 2). This suggests that the conventional and self-defined approaches to calculating population-level contraceptive needs result in identifying groups with largely the same sociodemographic characteristics.
Distribution of Females (Assigned Female at Birth a ) Who Are Fecund and Estimated to Have a Contraceptive Need over a One-Year Period According to Sociodemographic Characteristics, Comparing Those Identified Using the Conventional Need Metric, and Those Identified Using a Self-Defined Need Metric Based on Either the Person-Centered Contraceptive Access Survey, 2022 or the National Survey of Family Growth, 2017–19
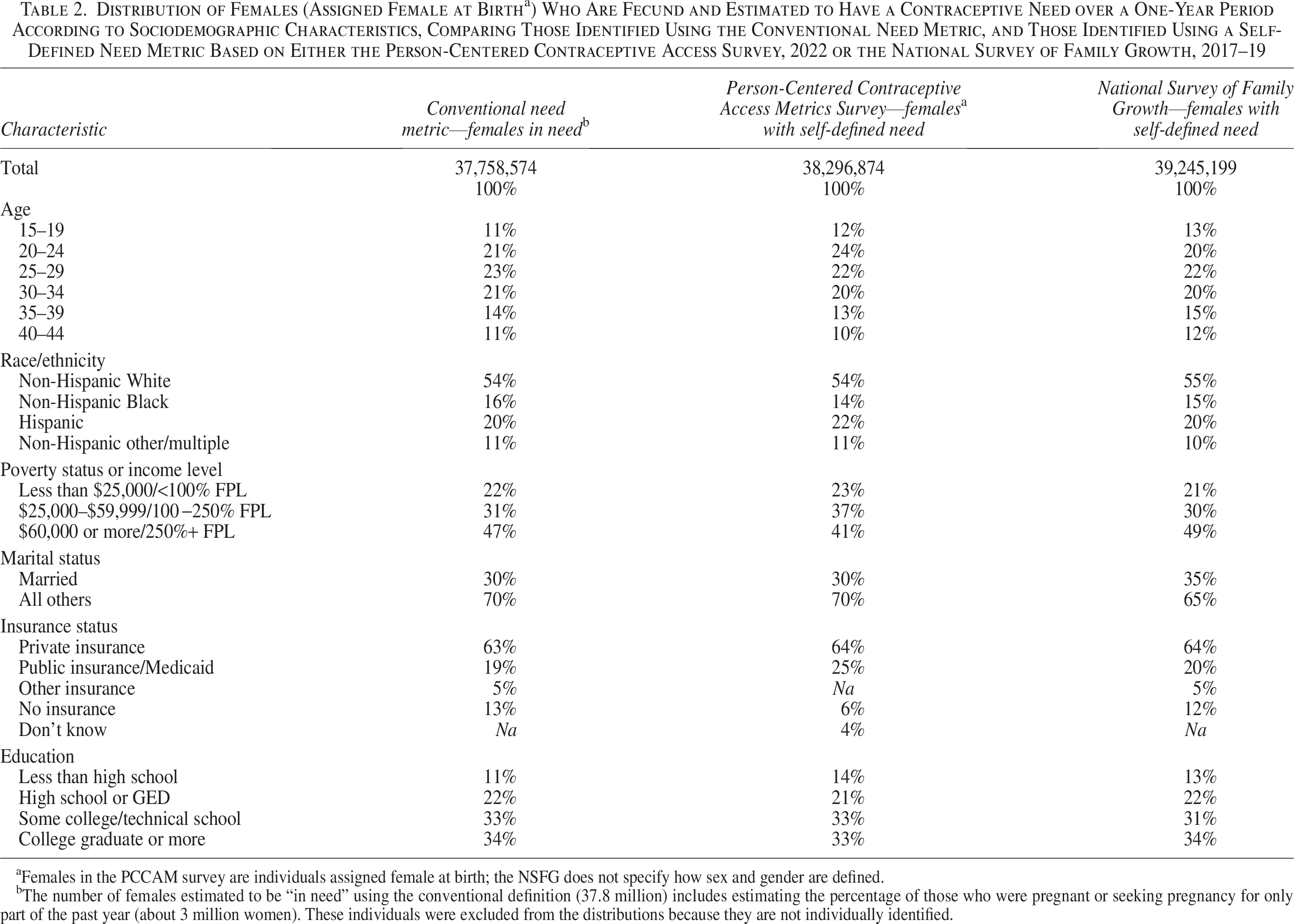
Females in the PCCAM survey are individuals assigned female at birth; the NSFG does not specify how sex and gender are defined.
The number of females estimated to be “in need” using the conventional definition (37.8 million) includes estimating the percentage of those who were pregnant or seeking pregnancy for only part of the past year (about 3 million women). These individuals were excluded from the distributions because they are not individually identified.
Discussion
We set out to develop a more person-centered method for estimating contraceptive need at the population level, comparing estimates made using the conventional approach and a new approach based on survey responses from two different sources. We found that the overall number of individuals aged 15–44 considered to have a need for contraceptive services at the population level is roughly similar when comparing the conventional estimation approach (37.8 million) to a more person-centered approach (38.3 million or 39.2 million, depending on the survey) and when excluding those who were sterile or who reported difficulty getting pregnant. The slight differences in these overall estimates of need can be attributed to a combination of shifts in the data inputs according to each approach, including consideration of individuals’ sexual activity, fecundity, and partner vasectomy. Importantly, however, these overall numbers represent different people according to each metric, with the more person-centered metrics reflecting numbers of individuals who have a self-defined need for contraception for any reason and the conventional metric reflecting numbers of individuals whose contraceptive need is based on being sexually experienced and presumed at risk for pregnancy, without consideration of their expressing a desire to use contraceptive services.
In addition to illustrating the differences between the conventional and more person-centered approaches to measuring need, our analysis highlights that measurement of self-defined contraceptive need is feasible, and we provide the methodological detail supporting this conclusion. The new metric is comparable to the conventional approach in terms of overall numbers and provides an important step toward shifting a key metric used to track and evaluate program success related to contraception in a more person-centered direction. Because of eligibility differences between the PCCAM and NSFG, we did not assess whether those who were contraceptively or non-contraceptively sterile would report a self-defined need for contraceptive services over the year. Going forward, we recommend doing so and would expect the total number of reproductive-aged individuals who report a self-defined need for contraceptive services to rise.
Our design process included a series of conversations with experts and stakeholders to understand the many ways that need metrics are used for program and policy decision-making and how a new metric might be used going forward. For some stakeholders, it was very important to maintain a metric focused specifically on contraception. Others highlighted the need for future work to examine how the need for broader SRH care can be defined and measured from a more person-centered perspective.
Looking forward, we propose that future population-level metrics of contraceptive need use the more person-centered approach represented by the PCCAM and NSFG metrics in this analysis and that future research should aim to collect better data that will improve metrics aiming to measure contraceptive need from a person-centered perspective. This approach prioritizes people’s own desires to use contraception, regardless of reason for use, and does not consider sexual activity or fecundity as relevant inputs for assessing need for contraceptive care. In addition, this approach considers an individual’s reliance on a partner method, like vasectomy, as an indication of a potential need for contraception in the same manner as reliance on any other contraceptive method. Using a metric that more accurately counts who has a need for contraceptive services would highlight how best to channel resources to ensure that care delivery is tailored to meet those needs and how those needs are distributed across population groups.
This analysis found close alignment between the PCCAM and NSFG when combining survey questions to measure self-defined contraceptive need, which suggests that ongoing calculation of this population-level metric on a regular basis is feasible. Using NSFG data to calculate self-defined contraceptive need will allow us to estimate contraceptive need at the national, state, and local levels by combining NSFG data with population data from the U.S. census and the American Community Survey. A forthcoming Guttmacher report will apply this new need metric to 2023 census data to estimate the numbers of females who have a self-defined need for contraceptive care, nationally and for each state and county.
We do note the limitations of our analysis. 13 First, given the design of the PCCAM survey that excluded some individuals from eligibility—specifically those who had indicated use of female sterilization/tubal ligation and who reported having difficulty becoming pregnant—we similarly excluded these groups from the self-defined contraceptive need metric using NFSG data. However, those who use permanent contraception or who consider themselves infecund may still have an expressed need for contraception beyond pregnancy prevention reasons and will be included in future calculations of self-defined contraceptive need. In future operationalization of self-defined contraceptive need, sterilized individuals should not be excluded but should be assessed as to whether they are current, recent, or potential users of contraception or contraceptive services. In fact, preliminary review of the full NSFG dataset suggests that about one-third of women who have undergone tubal ligation do report self-defined contraceptive service needs (data not shown).
Second, as described in the methods and in Figure 1, the survey questions available to measure recent and past or potential use of contraception (among those not currently using methods) differ between the PCCAM and NSFG. We relied on proxy questions in both datasets to capture recent and past contraceptive care and method use. In addition, both surveys asked a question on preferences to use contraception among those not using any method, but the wording differed. Neither survey included the recently recommend two-item series that includes both a hypothetical question regarding whether there was a method that the respondent would like to use and, if so, a follow-up question assessing the reasons for not using that method. In the short term, the current item on the NSFG is useful for informing estimates of potential contraceptive need. In the longer term, we encourage the NSFG to integrate the recommended two-item series into ongoing NSFG surveys.
Finally, self-defined contraceptive need metrics in this analysis draw on person-centered metrics of contraceptive preferences while not comprehensively reflecting person-centered metrics of the need for comprehensive contraceptive care (including, for example, contraceptive counseling). When applying Rothschild et al.’s definition of person-centered measurement to our updated metric, we find that the updated metric meets only one of the two criteria for being fully person-centered. 7 It draws on individuals’ own reports regarding their preferences for contraception, whereas it does not fully allow for individuals to self-define the value they place on needing or not needing contraception. Future work to refine this measure toward meeting both criteria for person-centered measurement should focus on integrating individuals’ perspectives regarding the extent to which they value contraceptive need as an important outcome in their own lives.
Our findings and recommendations are in line with a multitude of other efforts to move the measurement ecosystem that describes, tracks, measures, and evaluates the SRH of the United States population in a more person-centered and equitable direction. 14 We and other scholars have highlighted how a person-centered lens renders key metrics related to use of preferred contraception 15 where people want to obtain contraception,10,16 experience of contraceptive counseling, 17 and sexual and reproductive well-being 14 more accurate and reflective of people’s own experiences and lives and, thus, better metrics against which to measure whether systems are meeting the contraceptive access needs of all people in the United States.
Redefining the measurement of contraceptive need is only one aspect of the work necessary to move toward improved and more person-centered contraceptive access; future innovations are needed that focus on more holistic measurement in other aspects of access to care. For example, it is important to continue reorienting contraception in a more person-centered framework for metrics designed to monitor quality family planning care. Specifically, to most effectively monitor the quality of family planning care and support individuals who rely on that care, these and other person-centered metrics should be included in the nation’s Healthy People 2030 goals. 15
Policymakers also have a role to play in the uptake of these more person-centered metrics and in the allocation of resources toward contraceptive access programs; aligning these initiatives and the tracking of their progress with goals that prioritize the needs and preferences of the key stakeholders of these programs is an important step forward toward supporting people to achieve reproductive freedom. Centering people’s own perspectives in these metrics is both a necessary component of quality care and a step toward health equity.
Conclusion
To design and build health care systems that are responsive to the care that people need and want, we should base our metrics on data that identify individuals who have themselves reported a need for care and use that information to more accurately estimate the numbers and characteristics of people who will likely seek out such care. Understanding need for contraceptive services more accurately is also critical to being able to identify gaps in services and in identifying ways to fill gaps between what is currently available and the care that people need and want to fulfill their SRH goals. We developed a new, more person-centered metric for measuring contraceptive need and provided the methodological detail needed to support use of the new measure. Shifting to this new metric will better align measurement of contraceptive need according to what people want and will allow for improved estimates of potential demand for care and of how many individuals are likely to seek care.
Authors’ Contributions
J.J.F.: Conceptualization (lead); methodology (lead); and writing—original draft, review and editing (equal). M.L.K.: Conceptualization (supporting); methodology (supporting); and writing—original draft, review and editing (equal). A.D.-H.: Methodology (supporting); formal analysis (equal); and writing—review and editing (supporting). A.M.G.: Conceptualization (supporting); methodology (supporting); formal analysis (equal); and writing—original draft (supporting), review and editing (supporting).
Footnotes
Acknowledgments
This article was prepared by J.J.F., M.L.K., and A.D.-H., all of the Guttmacher Institute, and A.M.G., of University of California, Berkeley. The authors performed all data analyses and tabulations.
The authors thank the following Guttmacher colleagues: Audrey Maynard for research assistance and Kathryn Kost, Amy Friedrich-Karnik, and Emma Stoskoph-Ehrlich for reviewing drafts of this report. The authors also thank Sheila Desai of CECA for reviewing drafts of this paper and the staff at CECA for planning and facilitating a series of Technical Advisory Panel meetings and Lived Experience Panel meetings that contributed to the conceptualization of the new metric.
Author Disclosure Statement
None of the authors have anything to disclose.
Funding Information
This study was made possible by a grant to the Guttmacher Institute from the Office of Population Affairs (OPA) of the U.S. Department of Health and Human Services (Grant # FPRPA006074) as part of a financial assistance award totaling $2.25 million. The findings and conclusions in this study are those of the authors and do not necessarily reflect the positions and policies or the official views of, nor an endorsement by, OPA/OASH/HHS or the U.S. Government.
