Abstract
Introduction:
Bridges to Health Equity (BHE), a collaborative of community-based organizations (CBOs), insurers, hospitals, and an external evaluator was developed to forge partnerships that improve health in low-income neighborhoods in New York City. BHE developed an asthma program implemented by community health workers (CHWs) at participating CBOs in 2020 and 2021. Initially designed as an in-home intervention, the program shifted to remote delivery at the beginning of the study due to COVID-19.
Keywords
Introduction and Purpose
Housing quality, stability, cost, and location, as well as household composition, are important determinants of health, affecting levels of stress, management of disease, risk of injury, and access to needed services (Braveman et al., 2011; Taylor, 2018; World Health Organization, 2018). Poor housing maintenance (e.g., leaks, mold, pest infestations) is specifically associated with asthma progression, asthma exacerbations, and severity of disease (Conrad & Perzanowski, 2019; Taylor, 2018). Severe, poorly controlled asthma can lead to missed school and work, disrupted sleep, high rates of emergency department visits and hospitalizations, permanent lung damage, and death (Pate et al., 2021). In New York City (NYC), nearly one million homes had housing maintenance issues in 2017 (Spira-Cohen et al., 2021). Maintenance issues were more common in rental homes and in homes occupied by Black and Latine families, due primarily to historic disinvestment in communities of color (Spira-Cohen et al., 2021).
There is strong evidence that multi-component home-based interventions that reduce exposure to household asthma triggers, including mold and pest infestations, improve asthma management, particularly for children and adolescents (Crocker et al., 2011; The Community Preventive Services Task Force, 2013; US Department of Housing and Urban Development, 2018). These interventions, often staffed by Community Health Workers (CHWs), commonly include a home visit and assessment, education and supports to reduce triggers (e.g., integrated pest management), general asthma education, and connections to social services and supports (Crocker et al., 2011; The Community Preventive Services Task Force, 2013; US Department of Housing and Urban Development, 2018).
Similar to other CHW programming (Knowles et al., 2023; Malcarney et al., 2017; Peretz et al., 2020), CHW asthma interventions are currently implemented by healthcare provider organizations (Martin et al., 2021), health insurers, health departments (Elkugia et al., 2021), and community-based organizations (CBOs) (Sharp et al., 2019). Strengths of CBO-based CHW programs commonly include: close ties to the communities served, high levels of trust, and a broad array of services addressing social needs (Stout et al., 2019). Close community relationships and a wide range of services appear particularly important in low-income Latine communities, which may have specific service needs due to factors such as limited English language skills and limited access to public benefits (NYC Mayor's Office for Immigrant Affairs, 2021). Communities with high numbers of renters are also likely to benefit from the more comprehensive set of services offered by CBOs (Murphy & Sandel, 2011). CBOs may be particularly important for addressing home-based asthma triggers, such as mold and pest infestations, as their elimination may necessitate sensitive or contentious negotiations with landlords, which is likely to cause fear or discomfort among lower-income renters who have few options for alternative housing (Murphy & Sandel, 2011).
This paper describes quantitative findings from an evaluation of a multi-component asthma intervention implemented in low-income New York City Latine communities from 2020–2021, focusing on changes in asthma control and home-based asthma triggers among the enrolled children. Designed—and previously implemented—as an in-home intervention, the asthma program shifted to remote delivery at the beginning of the study period due to the COVID-19 pandemic. In describing outcomes from this remote intervention, we hope to continue to build the evidence on effective asthma interventions, including those that are delivered remotely, to address social and environmental challenges that impact health in communities with low incomes.
Methods
Program Description
Bridges to Health Equity (BHE), a multisector collaborative that included CBOs, managed care organizations (MCOs), hospital systems, and an external evaluator, was developed to forge community-healthcare partnerships that positively influence health and wellbeing in low-income NYC communities. Following an eighteen-month planning period, which involved focus groups with community members, research on effective programs working at the intersection of health and housing, and analyses of potential financing, BHE partners implemented an integrated community-based asthma CHW program at the three participating CBOs, one of which was currently implementing a similar program. The BHE program focused on children and adults with asthma living in low-income, primarily Latine neighborhoods and offered an individualized evidence-based asthma intervention from June 2020 to December 2021, which included:
home assessments conducted by phone and/or video conference by bilingual CHWs, which focused on identification and elimination of asthma triggers; tools and resources to eliminate asthma triggers in the home, including mattress and pillow covers and access to no-cost integrated pest management services provided through the NYC Department of Health and Mental Hygiene (DOHMH); education regarding common household items that trigger asthma, such as harsh cleaning products, and appropriate alternatives; supports for disease management, including medication spacers and instruction on the use and administration of controller and rescue medications; and referrals for healthcare and services to address the social determinants of health, including education, job training, nutritional programming, childcare, and facilitated enrollment into public benefit programs.
In addition to these evidence-based components, the asthma program offered linkages to legal and advocacy services as well as to tenants’ rights campaigns focused on addressing maintenance and other housing issues outside the control of the tenant (e.g., leaks, mold). BHE partners felt these services were particularly important in a city where most individuals rent their homes and rely on landlords to address structural issues.
Services were provided to each participant over the course of approximately six months and were tailored to identified needs and priorities. As home visits were not possible due to the COVID-19 pandemic, service provision—with the exception of the provision of certain supplies (e.g., mattress and pillow covers)—was remote (i.e., by phone and video chat).
Evaluation Design
Evaluators conducted a process and outcome evaluation of BHE to support quality improvement and to contribute to the evidence base regarding asthma interventions. This paper specifically focuses on quantitative findings related to program outcomes, assessed through baseline and follow-up surveys of enrolled children and caregivers—hereafter referred to as “children”—served by Make the Road New York (MRNY). MRNY builds the power of immigrant and working-class communities through an array of health, education, legal, and survival services, as well as community organizing and advocacy. This organization had a well-established CHW asthma program prior to the start of BHE with effective processes for recruitment and data collection and was therefore better suited to a robust analysis of outcomes than the other two participating CBOs. Prior to formal employment, all MRNY CHWs participate in a two-month classroom-based training focused on core competencies and specialized health knowledge, as well as a 135-hour internship. The larger evaluation of the BHE program was mixed methods and included qualitative interviews with program staff and partners (n = 10) that were focused on development and implementation of the BHE program model, as well as interviews with program participants (n = 10) that contextualized the quantitative findings. Qualitative findings are not included in this paper due to small sample size and a primary focus on implementation rather than outcomes.
The evaluation of BHE followed the six steps outlined in the CDC Framework for Program Evaluation in Public Health (Centers for Disease Control and Prevention, 2021b) and focused on the four standards for effective evaluation – it aimed to be useful to all stakeholders involved in the program and those using the evaluation findings; feasible with the available resources and mindful of the context in which the evaluation was taking place and the questions it sought to answer; ethical, guided by respect and regard for the wellbeing of all stakeholders involved; and accurate in its analysis, interpretation, and dissemination of information (Centers for Disease Control and Prevention, 2021a).
All evaluation protocols, consent materials, and data collection instruments were approved by the Institutional Review Board of The New York Academy of Medicine (protocol no. 062220) on June 24, 2020. All participants in the evaluation were informed of its purpose and procedures and provided verbal consent.
Participant Recruitment
Between June 2020 and December 2021, CHWs at MRNY enrolled 108 children living in low-income, primarily Latine neighborhoods in NYC in the asthma program and the evaluation. Individuals were eligible to participate in the program if they met at least one of the following criteria: no contact with a primary care provider in the last year; no contact with a pulmonologist or allergist in the last year; one or more hospitalization for asthma in the last year; one or more emergency room visits for asthma in the last year; an Asthma Medication Ratio less than .5; and/or uncontrolled or persistent asthma (Asthma Control Test score <=19). Criteria, developed by the BHE collaborative, were intentionally general in hopes of reaching a broad population with inadequate healthcare access. The majority of referrals to the program came from community health centers and partner MCOs. CHWs informed potential participants of the evaluation and its purpose and asked them if they were willing to participate. Those who consented were enrolled in the evaluation, in addition to the program.
Instruments and Data Collection
CHWs administered baseline assessments at the time of program enrollment and follow-up assessments six months thereafter. Baseline assessments for the 108 children in the evaluation were completed by the children's caregivers in Spanish (n = 84) and English (n = 24), primarily via phone or video chat. Assessments supported both service delivery and the evaluation and included questions on sociodemographics (baseline assessment only), asthma severity and symptoms, asthma-related healthcare use (e.g., hospitalizations, emergency department visits), home-based triggers, and other needs related to the broader determinants of health. Assessments also included the two versions of the standardized Asthma Control Test (ACT)—one designed for children ages 4 to 11 and the other for those ages 12 and over. This standardized instrument is intended to be used by individuals with asthma and their healthcare providers to assess severity and to support better asthma management. For children ages 4 to 11, caregivers asked their children the questions and responded on their behalf. Children over age 12 completed the assessment on their own, with their caregiver present. Children ages 3 or under did not take the ACT as it is not designed for this age group.
The full assessment instruments were developed by the evaluators in collaboration with the other BHE partners. The evaluators met regularly with the CHWs to address data collection challenges and ensure consistent implementation of the assessment protocol. They also participated in larger collaborative meetings to remain up to date on progress and report preliminary evaluation findings.
Data Management and Analysis
Quantitative data from baseline and follow-up assessments were entered into QuestionPro, an online survey platform. Data were transferred to STATA SE (version 15; College Station, TX) for cleaning, management, and analysis by the evaluators. Descriptive statistics were generated for sociodemographic variables. Statistical significance for the baseline-follow up comparisons for the 73 children who completed both assessments was determined using the McNemar Bowker test for all categorical data and the Wilcoxon signed-rank test for asthma control test scores. Statistical significance was defined as p < .05.
Results
The asthma program enrolled 108 child participants, most of whom (56%) were referred by an MCO partner (data not shown). Table 1 displays the demographic characteristics of all children enrolled in the program (n = 108) beside those in the subsample, which is limited to those children with both a baseline and a follow-up assessment (n = 73). Close to two-thirds (67%) of the children in the full sample were between the ages of 4 and 11, and slightly over half (54%) were male. The majority of children (85%) were Hispanic/Latinx. 1 Forty-four percent of caregivers of the enrolled children graduated from high school. The majority of children (80%) resided in rental apartments in privately-owned buildings. Eighty-six percent were covered by Medicaid, and all had a primary care provider (data not shown). There were no statistically significant differences at p < .05 between the characteristics of the children in the full sample and those in the subsample with follow-up assessments.
Participant Characteristics at Baseline.
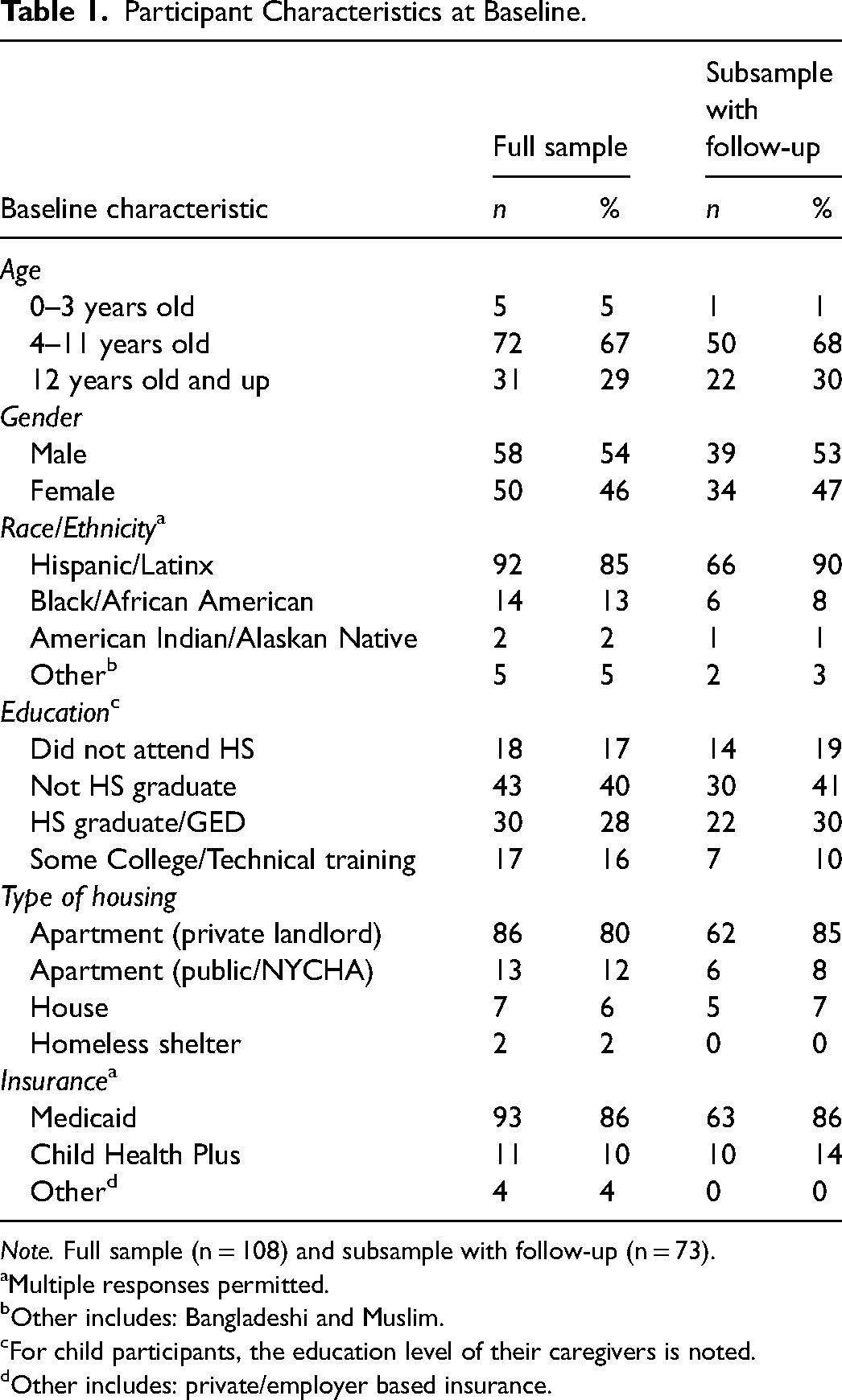
Note. Full sample (n = 108) and subsample with follow-up (n = 73).
Multiple responses permitted.
Other includes: Bangladeshi and Muslim.
For child participants, the education level of their caregivers is noted.
Other includes: private/employer based insurance.
Table 2 presents asthma-specific information at baseline and follow-up for the subsample with follow-up assessments. Participants reported statistically significant fewer asthma-related ED visits in the past six months at follow-up (5%) compared to baseline (15%). ACT scores were significantly higher after participation in the program (Mdn = 23, n = 72) compared to before (Mdn = 21, n = 72), Z = 4.78, p = <.001, r = .56. Ninety-two percent of children were considered “well controlled” at follow-up, compared to 61% at baseline.
Asthma Information for Subsample with Follow-up.

Note. N = 73.
Relevant only to children aged 4+ (n = 72).
The well controlled range for children 4–11 is 20–27, and the well controlled range for children 12 + is 20–25.
Table 3 shows information on participants’ housing, including home-based asthma triggers. Significantly fewer participants reported housing maintenance issues at follow up (30%) compared to baseline (45%). There was also a significant decrease in participants reporting the presence of at least one asthma trigger in the home (60% at follow-up compared to 86% at baseline). Specific triggers showing significant reductions included cockroaches (36% at follow-up vs 53% at baseline) and mice (12% at follow-up vs 33% at baseline).
Housing Information for Subsample with Follow-up.
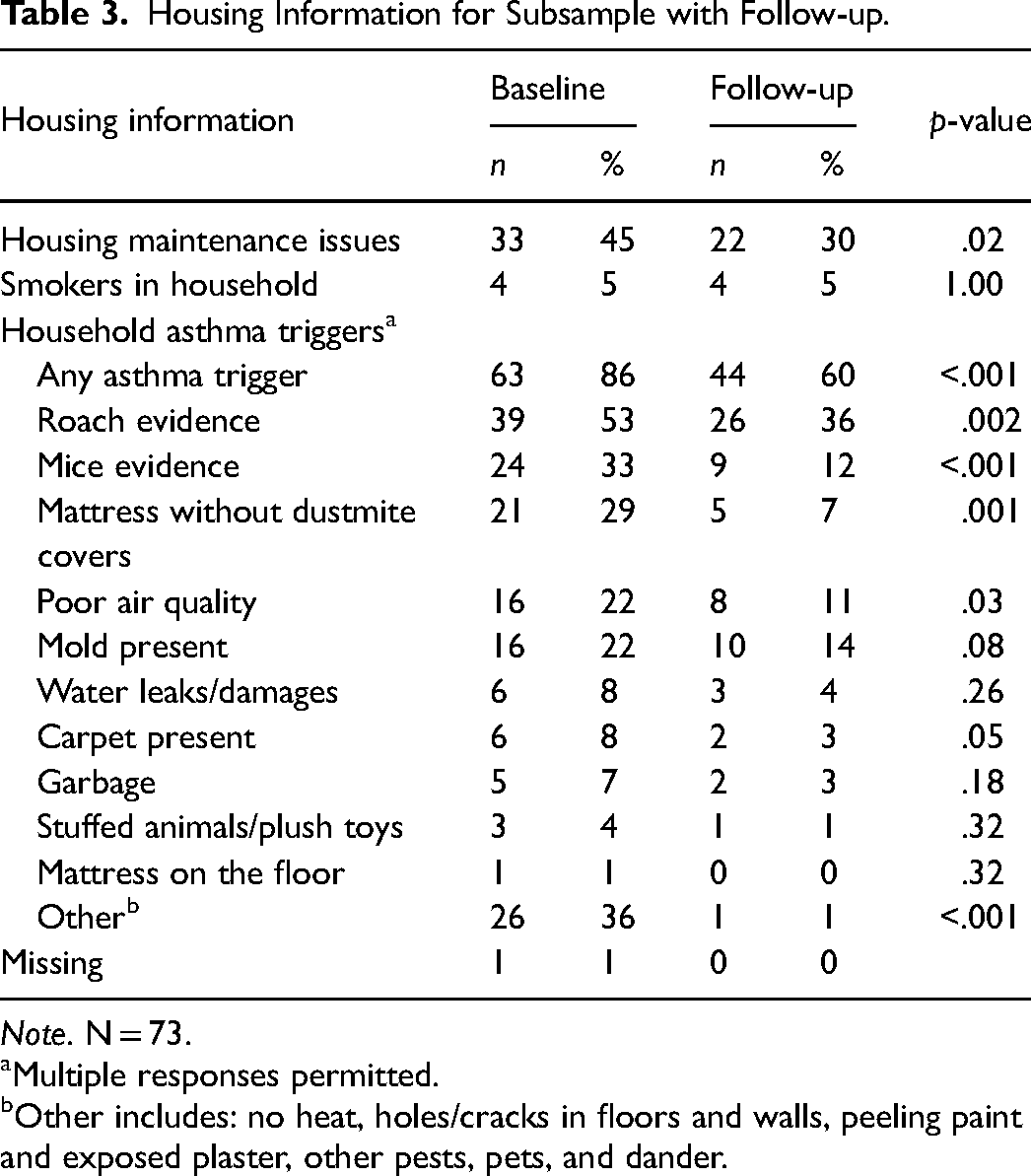
Note. N = 73.
Multiple responses permitted.
Other includes: no heat, holes/cracks in floors and walls, peeling paint and exposed plaster, other pests, pets, and dander.
Discussion
The vital role of CBOs and CHWs in disease prevention and management, and in addressing the broader determinants of health, has been increasingly recognized (Griffin et al., 2018; Knowles et al., 2023; Peretz et al., 2020; Solomon & Kantor, 2018). CBO-based CHWs have been shown to effectively take on a variety of roles, including connecting community members to healthcare services and supporting social needs, health education, care coordination, and advocacy (Knowles et al., 2023). Findings from this evaluation provide additional evidence regarding CBO and CHW capacity to deliver programming with positive health impacts. At follow-up, child participants experienced statistically significant improvements in indicators of asthma control, including reductions in asthma-related ED visits and higher mean scores on the Asthma Control Test, indicating decreased severity of asthma. They also experienced statistically significant reductions in home-based asthma triggers, including reductions in evidence of pest infestations (i.e., mice, cockroaches).
The study also adds to the evidence base by demonstrating positive outcomes with remote delivery of a program model that was originally designed to be conducted in-person and in-home. While there is a substantial and growing body of literature on the implementation, outcomes, and acceptability of remote medical visits, information on remote delivery of programs addressing health-related needs that fall outside of traditional medical care (Murray et al., 2023; Peretz et al., 2020), such as multi-component asthma interventions, is more sparce. The asthma intervention described here transitioned to remote administration by necessity due to restrictions on home visits and in-person interactions at the start of the COVID-19 pandemic, but lessons learned have continued relevance. Given the generally lower cost and greater convenience of remote delivery, organizations implementing home-based asthma programs might consider the development of hybrid programs, with integration of remote services into their home-based models.
This study has several limitations. It is possible that improvements in asthma symptoms may have resulted from factors not examined in this study, including changes in prescribed medications (some of which may have stemmed from the COVID-19 pandemic). Seasonal variation may have also impacted asthma control for some children; however, rolling program enrollment should have reduced any seasonal effects on aggregated outcomes. We were unable to identify a control group—in part due to resource limitations and in part because it is standard practice in NYC for health providers, insurers, schools, and other agencies to refer children with poorly controlled asthma to asthma programs similar to BHE. Additionally, 35 children did not complete a follow-up assessment. Although we hoped for a higher response rate at follow-up, given the competing priorities during the COVID-19 pandemic we feel this is satisfactory—particularly since there were no statistically significant differences between the children in the full sample and those in the subsample with follow-up assessments. Although the hope was to triangulate findings from baseline and follow-up assessments with data from health plans, participating children were covered by several different MCOs making data access for the purpose of evaluation impractical. Participating CBOs also lacked access to health records from MCOs and providers. Multiple systems have been developed, including Unite Us (uniteus.com) and NowPow (nowpow.com), for data sharing to support cross-sector collaboration; however, these systems focus primarily on sharing information regarding social needs and social service supports, rather than healthcare use and health outcomes.
Conclusion and Implications for Practice
Despite the limitations described above, we feel the results of this evaluation make an important contribution to the literature and have implications for the development and implementation of asthma interventions. Findings from the present study suggest alternatives to the existing in-person program model that may reduce costs while producing positive outcomes. While there may be many programs—and program components—that should remain in-person, the successful shift to remote program delivery of a CHW asthma intervention for low-income, Latine populations in a large, urban area may offer alternatives or adaptations that can support program sustainability and expansion. Additional research, including research that expands upon findings described in this manuscript by including health record and cost data, should be carried out to inform program planning and implementation of similar interventions.
Footnotes
Acknowledgements
The authors would like to thank the asthma program participants for their time and generosity, as well as the community health workers who carried out the asthma program for their time and effort enrolling participants, collecting data, and sharing their expertise. The authors would also like to thank the members of the Bridges to Health Equity collaborative: in addition to Make the Road New York and The New York Academy of Medicine, this included the Local Initiatives Support Corporation (collaborative convener), RiseBoro Community Partnership, Fifth Avenue Committee, Empire BlueCross BlueShield HealthPlus, MetroPlusHealth, Healthfirst, NYU Langone Health, and NYC Health + Hospitals.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: The Bridges to Health Equity collaborative was supported by multiple funders, including the Altman Foundation, Deutsche Bank, the Empire BlueCross BlueShield Foundation, the Kresge Foundation, and State Farm. The evaluation described in this manuscript was supported by the Local Initiative Support Corporation (contract 45512-0005), with funding provided to them by the Altman Foundation.
