Abstract
Keywords
Introduction
In the United States, Hispanic/Latino individuals are 1.4 times more likely to die from diabetes and 1.2 times more likely to be obese than non-Hispanic whites due to social determinants of health and systemic oppression due to allocation of power and resources (CDC, 2018, 2019a; Kapitan, 2016; Walker et al., 2016; Weinstein et al., 2017). Every year more than $300 billion are spent on diabetes medication and symptom management (ADA, 2018). According to NIH (2016), risk factors for developing type 2 diabetes mellitus (T2DM) include being overweight/obese, age 45 or older, Hispanic/Latino, having a family history of diabetes, high blood pressure, low levels of high-density lipoprotein cholesterol or high triglycerides, history of gestational diabetes, poor nutrition during pregnancy, being physically inactive, history of heart disease or stroke, depression, or polycystic ovary syndrome.
Previous studies have shown that culturally tailored interventions have high rates of sustainability, and participation in home meal preparation can improve self-efficacy and diet quality, while lowering adiposity (Hu et al., 2016; Mills et al., 2017; Wolfson et al., 2020; Wolfson & Bleich, 2014). In addition, studies have also shown that a whole food plant-based (WFPB) diet is sustainable, economical, and can potentially reverse T2DM, lower blood pressure and cholesterol, and help to promote insulin sensitivity by controlling blood sugar three times more effectively than a traditional diabetic diet that limits carbohydrates and calories (Alexander et al., 2017; Kahleova et al., 2018; McMacken & Shah, 2017; Sabaté & Soret, 2014).
Background
Hispanic/Latino Individuals and Diabetes
Hispanic/Latino individuals and their health are disproportionately impacted by various factors. These factors may include macroeconomics, privilege and/or discrimination (e.g., access to nutritious food, immigration status, structural and institutional racism), cultural values, income, education and literacy, occupation, and social support systems, including health services (Hobbs, 2018; Velasco-Mondragon et al., 2016). For example, an individual's educational and literacy level may impact their personal income, which may in turn impact their ability to access nutrition, food, and health services. Social determinants of health such as socioeconomic status, cultural background, employment, and foreign-born or unauthorized status place Hispanic/Latino individuals at greater risk for adverse social and health outcomes (Paz & Massey, 2016; Vega et al., 2009). Among working adults, 32% of Hispanic/Latino individuals are uninsured, which may also have a large impact on health care access (Levy & Sidel, 2013).
Hispanic/Latino adults need access to resources that may assist them in being proactive to prevent T2DM now. Among the overall U.S. population, estimates for 2018 reported that approximately 34.1 million adults (13%), aged 18 years or older, had diabetes (CDC, 2020). Without lifestyle modification, it has been predicted that there will be an annual rate of 5%–10% progression from prediabetes to diabetes (Levy & Sidel, 2013). In addition, studies have found that medication nonadherence and diabetes complications are higher when comparing Hispanic/Latino individuals to non-Hispanic white individuals (CDC, 2019b; Fernandez et al., 2017). By being proactive and making changes early on, individuals may possibly prevent or delay the onset of diabetes and potential complications, which could be physically and financially beneficial.
The Hispanic/Latino population in the United States is not a homologous/unified group (Beltrán, 2010). Subgroup differences in health outcomes may be related to age, gender, nativity, immigration status, skin color, living in a segregated neighborhood or low-income household, occupational status, health insurance status, or living in a county/state with high immigration enforcement and anti-immigrant/anti-Latinx sentiment (Martínez & Rhodes, 2020). Therefore, when studying Hispanic/Latino populations, if possible, it is best to specify any subgroups and how those differences are related to health behaviors and health outcomes. For example, low socioeconomic status is often linked to poor health status. Notwithstanding, Hispanic/Latino individuals often have a lower socioeconomic status and insured rates, when compared with other populations. However, Hispanic/Latino individuals are often found to have a longer life expectancy and better maternal child health outcomes when compared with non-Hispanic white individuals (Abraído-Lanza et al., 2005; Ruiz et al., 2013). The U.S. National Health and Nutrition Examination Survey, 2011–2016, showed the prevalence of total diabetes was highest, 24.6% (95% CI: 21.6%−27.6%), among the Mexican subgroup, 21.7% (95% CI: 14.6%−28.8%) among the Puerto Rican subgroup, and 20.5% (95% CI: 13.7%−27.3%) among the Cuban/Dominican subgroup (overall p <.001) (Cheng et al., 2019).
Hispanic/Latino Individuals and Nutrition
Although researchers continue to discover and identify connections between food and health outcomes, health care professionals may not always feel adequately trained on how to incorporate nutrition into their clinical practice when educating patients on lifestyle modification (Crowley et al., 2019). Nutrition in health care education should not be viewed as alternative medicine but should be included as a foundation for prevention and health promotion. Physical activity and a healthy, balanced diet have been found to be an integral part of T2DM prevention with previous studies showing successful management and reversal of T2DM through a WFPB diet (Al-Mrabeh et al., 2019; Barnard et al., 2009). This option often reduces sodium and fat, while increasing fiber through the consumption of fruits/vegetables without requiring special equipment. A WFPB diet includes whole, minimally processed foods and avoids animal products (e.g., meat, milk, eggs, and cheese), while focusing on plants (e.g., fruits/vegetables, whole grains, legumes, and nuts/seeds) (Campbell & Campbell, 2016, p. 237; Tuso, 2013). Refined foods (e.g., added sugars, salt, white flour, and processed oils) are limited/avoided, and locally sourced, organic food is used as much as possible. While Hispanic/Latino adults often report higher consumption of fruits/vegetables when compared with other ethnic groups, they also often report the highest intake of solid fats and added sugars (Hammons et al., 2019).
Knowledge Gaps
With the growing number of diabetes cases among Hispanic/Latino individuals and the associated costs, there is an urgent need for improved health care access with a focus on health promotion and disease prevention. While previous research and current nutritional/dietary interventions often focus on individuals already diagnosed with T2DM, little research has focused on reducing T2DM risk factors using a WFPB intervention in at-risk Hispanic/Latino adults (Ramal et al., 2018; Singh et al., 2019). To improve diabetes self-care in minoritized populations, culturally tailored interventions have been cited as being beneficial (Whittemore, 2007). Although Hispanic/Latino individuals are often described as a minority group, it should be noted that they are the second largest racial/ethnic group, after white non-Hispanic individuals (Noe-Bustamante et al., 2020).
Questions often surround the design of a culturally tailored intervention and implementation. While existing interventions provide education on healthy food choices, few interventions are culturally tailored to focus on reliable access to and hands-on preparation of healthy food, including food preferences and behaviors. Additionally, barriers such as needing childcare and transportation to facilitate participation in clinical and community-based interventions are not always addressed (Barajas et al., 2016; Doshi et al., 2020).
Aim
The purpose of this integrative review was to explore and analyze literature on culturally tailored nutrition interventions to identify how to best implement a plant-based diet using a WFPB culinary intervention to improve health outcomes for Hispanic/Latino adults at risk for developing or diagnosed with T2DM.
Methods
Data Sources and Search Criteria
For the purpose of this review, the key search terms were “Hispanic adults” or “Latino adults”, “culturally tailored” or “ethnic”, “diabetes”, “dietary” or “nutrition” and “intervention”, and/or “vegan”, or “plant based”. The term, “adults”, was used to exclude studies focused on children/adolescents. These key terms were used in full-text searches in PubMed, CINAHL Complete, PsycINFO, and Food Science and Technology Abstracts. Inclusion criteria included primary research articles in peer-reviewed journals, published in English, from January 2009 to January 2020 with key terms. The year 2009 was selected due to research conducted in the same year reporting that eggs are associated with an increased risk of T2DM (Djoussé et al., 2009). In the same year, Beyond Meat (2022), a Los Angeles-based producer of plant-based meat substitutes, was founded and the Poison-Free Poultry Act was introduced into Congress (2009). Inclusion criteria for studies consisted of adult participants, aged ≥18 years, at risk for or diagnosed with T2DM, with a culturally tailored intervention related to diet/nutrition. Unpublished manuscripts (e.g., abstracts and dissertations), as well as secondary sources, were excluded.
Search Strategy
The search strategy resulted in an initial 1,474 articles for review. After duplicates were removed, 871 article titles and abstracts were scanned for relevance and ability to be retrieved, using the inclusion/exclusion criteria for the search (e.g., primary research, key terms, published in English). From there, 818 articles were excluded, and 53 full articles retained. The inclusion/exclusion criteria for the studies were then applied (e.g., ≥18 years, culturally tailored intervention related to diet/nutrition) and 25 articles were excluded after full text screen with an additional 13 articles being excluded after data extraction, resulting in a total of 15 articles (Figure 1). Articles included consisted of seven quantitative studies, five qualitative studies, and three mixed methods studies.
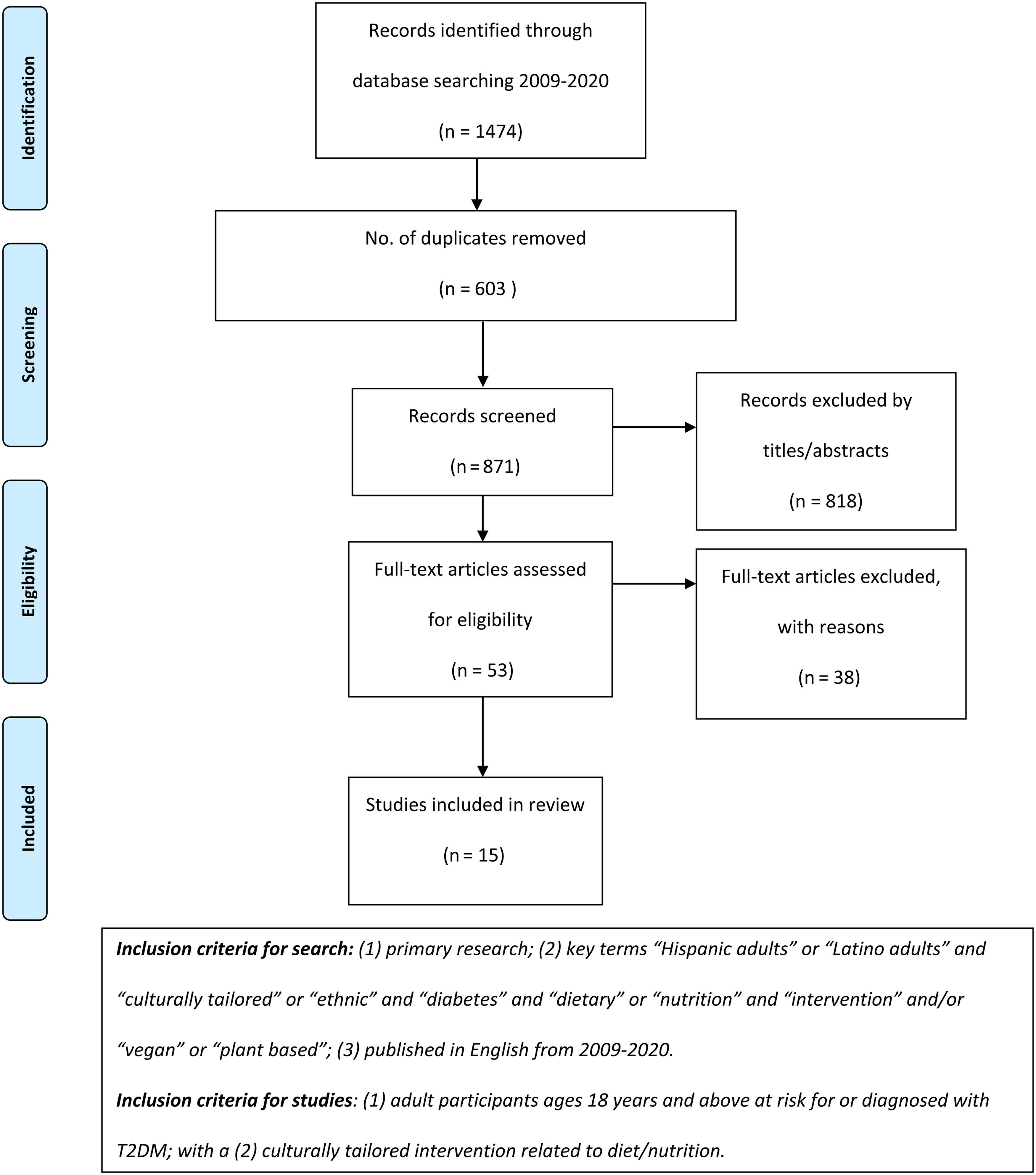
Adapted PRISMA flow diagram of search strategy and study report selection (Moher et al., 2009).
The need for and importance of culturally tailored interventions for Hispanic/Latino adults in reducing T2DM risk factors was identified (Figure 1). From these articles, four main themes presented: participant interest, feasibility of intervention, the development and implementation of intervention, and the impact of intervention (Table 1). Database searches revealed systematic reviews for culturally tailored and culturally competent interventions for Hispanic/Latino individuals in relation to T2DM (McCurley et al., 2017; Whittemore, 2007), but did not reveal any integrative reviews.
Selected Studies for Review According to Theme.
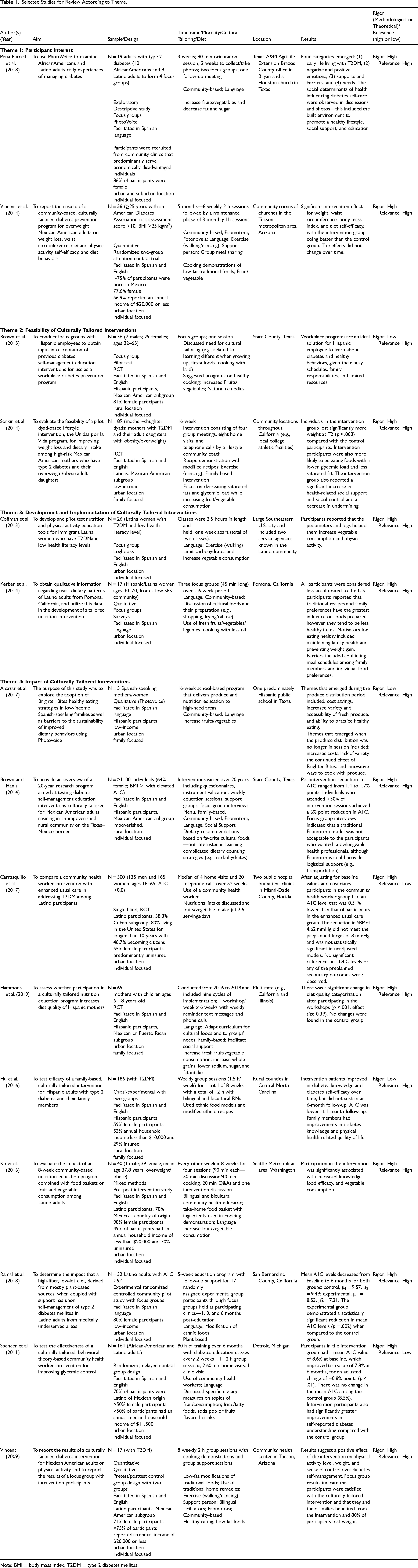
Note: BMI = body mass index; T2DM = type 2 diabetes mellitus.
Data Abstraction
Articles were then organized and compiled into a bibliography and database manager. Data from articles were extracted and prepared for data display and comparison. The data were entered into a matrix, organized, and analyzed for patterns, themes, and relationships, based on aim, design, and results (Whittemore & Knafl, 2005) (Table 1). The matrix provided a method for ordering, coding, categorizing, and summarizing the findings of the articles (Cooper, 1998). Articles with similar findings and themes were grouped together. Constant comparison was utilized to ensure that articles showed distinct relationships to the themes.
To score the quality of the articles, articles were evaluated based on methodological/theoretical rigor and data relevance with a possible “high” or “low” determination on a 2-point Likert scale (high = 2 or low = 1) (Whittemore & Knafl, 2005). A high rigor and relevance score had a greater contribution to the analytical process and required a clear description and appropriate use of the methodology, valid tools, and transparency regarding study limitations and potential threats to validity (Whittemore & Knafl, 2005) (Table 1).
Results
Development and implementation of culturally tailored interventions require specific planning prior to implementation, as well as measurement of the impact of the intervention, to determine the cultural impact, benefit, and outcome (Brown & Hanis, 2014; Carrasquillo et al., 2017; Hammons et al., 2019; Kerber et al., 2014). Studies were conducted across the United States, ranging from Washington to Florida, with the majority implemented in urban areas in California (4), Texas (3), and Arizona (2) (Table 1) with two studies including African American participants. Study designs mainly consisted of randomized controlled trials (7) and focus groups (6) conducted in English and Spanish. Additionally, the majority of studies focused on individual-level change and included primarily female participants. This may be due to cultural beliefs about nutrition or traditional gender roles. However, this also reveals a need for additional research on gender diversity and inclusion.
Theme 1: Participant Interest
When implementing culturally tailored interventions, two studies emphasized the importance of participant interest and feasible interventions with attainable outcomes to facilitate enrollment/retention (Peña-Purcell et al., 2018; Vincent et al., 2014). Participants’ interest levels should be assessed prior to an intervention, as well as their ability to participate (e.g., transportation, financial/time commitments, family/social responsibilities, support systems, and health literacy levels). This type of needs assessment can take place through focus groups, questionnaires, or informal conversations. Individuals may also need assistance with finances if participating in a dietary intervention, and childcare and/or transportation, depending on various commitments. Facilitators should make accommodations and efforts to remove potential barriers when planning interventions and develop community partnerships prior to the implementation of studies (Peña-Purcell et al., 2018; Vincent et al., 2014).
Theme 2: Feasibility of Intervention
Individuals may often verbalize that they wish to participate in diet/nutrition interventions. However, they may feel hesitant to make a change, if they feel that the change may potentially impact their family/social interactions in a negative way (e.g., meal planning for holidays/events) (Pilcher, 2015). Two studies reported that in Hispanic/Latino culture, participants may find it beneficial to include family members/support persons in education sessions/appointments to promote accountability and facilitate ongoing participation (Brown et al., 2015; Sorkin et al., 2014). Barriers to self-management and other cultural challenges (e.g., food preparation for self/others) should also be taken into consideration (Sorkin et al., 2014).
Regarding food preparation, previous studies in Latin America have shown that long-held cultural traditions of eating whole plant foods can potentially be an attractive target for high-impact interventions (Singh et al., 2019). In addition, many ancestral foods were actually plant-based and beef was only introduced to the Americas during colonization (Medina-Cadena, 2017).
Regarding time commitment and location, participants may express that due to time constraints, it is most effective for them to participate in interventions provided at community locations they already frequent on a regular basis (e.g., work, church) (Brown et al., 2015). Researchers reported interventions with timelines ranging from three weeks to more than a year, with one study analyzing results of a 20-year program (Brown & Hanis, 2014). However, regardless of length of intervention, participant burden should be taken into consideration.
Theme 3: Development and Implementation of Intervention
The third theme focused on the development and implementation of culturally tailored diet/nutrition interventions that included components such as the use of Spanish-speaking health care workers and improving health literacy, staff with a shared cultural identity, and how interventions were carried out to ensure sustainability. In two studies, researchers described essential design components that included the development and implementation of culturally tailored interventions which have the potential to make or break a study. Researchers confirmed that while participants may be eager and enthusiastic, as often as possible, education should be provided in the primary language and at a health literacy level that is appropriate to help promote understanding (Kerber et al., 2014). If education cannot be provided in a language that is understood, an interpreter must be made available.
In addition to primary language, cultural traditions surrounding identity and food should also be discussed to facilitate engagement and to remove/alleviate any potential barriers to achieve successful outcomes. According to Coffman et al. (2013), “Learning is best applied to daily life when it mimics life as it normally occurs” (p. 71). To assist participants with lifestyle changes, family and social network support may be utilized through small group gatherings and meals (Coffman et al., 2013).
Theme 4: Impact of Intervention
To validate the impact of culturally tailored interventions, nine studies reported changes in a variety of ways, including weight loss, serum lab values, diet quality, and food efficacy. While WFPB diets were not always specifically mentioned, studies specified increasing consumption of fruits/vegetables, as well as low-sodium, low-fat, and whole grains in interventions. Improvements were documented in record logs noting any changes in glycosylated hemoglobin tests (A1C), weight loss through body mass index (BMI), and other lab values, often compared to a control group. An article by Brown and Hanis (2014), provided an overview of a 20-year research program aimed at testing diabetes self-management education interventions culturally tailored for Mexican Americans residing in an impoverished rural community on the Texas–Mexico border.
A qualitative study by Alcazar et al. (2017), explored the adoption of healthy eating strategies in low-income Spanish-speaking families by distributing produce through a school-based program. Themes during the produce distribution period included cost savings, an increase in access and variety of fresh produce, as well as opportunities for healthy eating. However, once the distribution period ended, participants reported increased costs and loss of produce variety.
Successful results were measured through A1C ranging from a 1.4% to 1.7% overall decrease (Brown & Hanis, 2014). Mean baseline A1C levels were 12% and ranged from 6% to 18%, but individuals who attended at least half of the intervention sessions achieved a 6% point reduction (Brown & Hanis, 2014). Lessons learned included the impact of culture and the importance of family involvement. Cultural aspects included topics such as fatalism, folk remedies, language, religion, gender/family roles, social support, personal relationships, and also had an impact on recruitment/retention. Another study also utilizing a culturally tailored approach measured participants’ baseline mean A1C value at 8.6% at baseline, which improved after 6 months to 7.8% (p < .01) (Spencer et al., 2011).
Some studies used bilingual and bicultural community health workers in various capacities ranging from education to home visits and telephone calls to group activities (Carrasquillo et al., 2017; Ko et al., 2016). Results ranged from lowering A1C levels (52-week intervention) by 0.51% to providing food baskets (an 8-week intervention) with ingredients used in cooking demonstrations to encourage consumption of fruits/vegetables in Latino adults with financial constraints (Ko et al., 2016). The results from the food baskets showed a statistically significant change in knowledge (p < .01), food efficacy, and vegetable consumption (3.1 ± 2.0 vs. 3.9 ± 2.1; p < .05).
A study by Hammons et al. (2019) focused on culturally tailored nutrition education by focusing on the whole family and traditions and practices related to diet quality, family time, and physical activity in Hispanic mother–child dyads. Education sessions were two hours long, for six weeks, with a total of three hours dedicated to nutrition education. Participants received instruction on incorporating higher nutritional value foods and decreasing foods with lower nutritional value. Although this study was not directly focused on diabetes, the study was included as it described at-risk individuals using a culturally tailored intervention involving nutrition. The results indicate a significant change in diet quality categorization after participation in the workshops (p < .001, effect size 0.39). Workshop topics for changes in diet quality included activities, discussion, and hands-on demonstrations related to portion sizes and food labels, fruits/vegetables, whole grains/legumes, salt/sugar, fat, and protein. Participants were advised to start with small dietary changes and to eat foods with higher nutritional value while using traditional foods (e.g., beans as a plant-based source of protein/fiber) to strengthen family and cultural connections.
In a study by Vincent (2009), the use of a culturally tailored self-management approach with focus groups and physical activity resulted in a mean weight loss of 5 pounds at 4 weeks post-intervention. Through these combinations of culturally tailored interventions and lifestyle modifications (e.g., learning how to build social/familial support and use of culturally specific foods to improve diet quality), participants were able to make measurable improvements in their health.
A study by Hu et al. (2016) tested the efficacy of a family-based, culturally tailored intervention using bilingual and bicultural registered nurses with team members for Hispanic individuals with T2DM and their family members. The intervention group received eight weeks of diabetes education presented in Spanish with data collection occurring at baseline, after intervention, and at 1- and 6-month follow-ups for the patients and their families. While the intervention appeared effective over time, the results did appear to be sustained at the 6-month follow-up (Hu et al., 2016). There were changes over time, with the most significant change occurring in A1C (p < .001) after adjustment for repeated measures and propensity score weighting with results based on mixed-effect models. Cultural tailoring in this study included use of a family-focused intervention in facilitating stress management, problem-solving, and confidence in diabetes self-management (Hu et al., 2016).
A study conducted by Ramal et al. (2018), was the only study that specifically mentioned the use of a diet obtained from mostly plant-based sources. In both the control and experimental groups, mean A1C levels decreased from baseline to six months (μ1 = 9.57, μ2 = 9.49; experimental, μ1 = 8.53, μ2 = 7.31). The experimental group also was found to have a statistically significant reduction in mean A1C levels (p = .002) when compared to the control group.
However, not all results were statistically significant. In a pilot study by Coffman et al. (2013), Latina women with T2DM and low health literacy levels took part in a self-management education class and focus groups to discuss diabetes concepts related to nutrition and physical activity. Participants kept nutrition logs and had access to pedometers. No statistical significance was found between the health literacy level and completion of the nutrition log (rs = .11; p = .58). The participants reported that the pedometers and logs helped to increase physical activity and improve the consumption of vegetables. Regarding cultural tailoring, the class materials and booklets were designed for individuals that speak Spanish and have low literacy levels, as well as having a research assistant who had experience working with a Latino population and was fluent in Spanish and English.
Discussion
As evidenced by the amount of research (n = 15) conducted from January 2009 to January 2020, there is an interest and need for culturally tailored nutrition interventions to prevent and reduce T2DM risk in Hispanic/Latino adults. Cultural tailoring was described as occurring through curriculum with culturally relevant themes and exercise, ethnic recipes, and language of delivery. Additional topics included stress management, religion, gender and family roles, and findings emphasized the value of bilingual and bicultural health care workers. Outcomes revealed an increased familiarity of fruits/vegetables and facilitation of family and community support.
Six of the studies resulted in significant reductions in weight, waist circumference, BMI, diet quality and self-efficacy, and A1C values, suggesting that culturally tailored nutrition interventions may be effective in reducing diabetes risk indicators. Some reported limitations included length/frequency of the interventions, inclusion of uncontrolled trials, generalizability, and sample sizes.
Conclusion and Clinical Implications
By utilizing culturally tailored methods (e.g., through curriculum, language, themes, food preparation, and eating), nurses and interdisciplinary teams can work together to design, implement, and evaluate innovative patient education while facilitating collaboration and open communication with Hispanic/Latino individuals and communities. In the study by Hu et al. (2016), using bilingual and bicultural registered nurses in their intervention, sustainable results were observed after six months. Nurses are in a strategic position to educate and assist in health promotion and disease prevention among Hispanic/Latino adults and their communities. Nurses compose 30% of the health care workforce and spend the most face-to-face time with patients; therefore, nurses are integral and should be prepared to advocate and support patients in the prevention of chronic diseases through health promotion, including nutrition (U.S. Bureau of Labor Statistics, 2020; Williams et al., 2018).
While policy changes, including those related to environmental and structural changes, are often beneficial for health outcomes, more research is needed in this area. Current studies show that individuals oftentimes experience greater success with individual and community-based or group health interventions than with policy change (Hillier-Brown et al., 2014). Therefore, research must be patient- and community-centered while focusing on sustainable health promotion, disease prevention, and self-management of chronic conditions. Through understanding of the sociocultural dimensions that influence decision-making processes and behavioral changes, nurses and health care providers can utilize culturally tailored nutrition interventions for equity, health promotion, and disease prevention.
Footnotes
Acknowledgments
The author would like to thank Dr. Kalpana Poudel-Tandukar and Dr. Rachel (Rae) Walker for their support during this review.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
