Abstract
Brachial plexus birth injuries (BPBIs) can affect children’s occupational participation. This review examined the efficacy of non-surgical interventions used by occupational therapy for increasing the range of motion (ROM) and improving motor skills of the affected upper extremities (UEs) of children with BPBIs. Non-surgical interventions are typically used as first-line treatment or in adjunct to surgery with the aim of optimizing recovery, decreasing risk of secondary impairment, and promoting occupational participation. Sources were Scopus, Cochrane Trials (CENTRAL), Ovid (Medline), and CINAHL. Data were abstracted following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. Inclusion criteria: Participants with BPBI, not older than 18 years, randomized controlled trials or comparative studies (cohort and case-control), sample size over 20, conservative management, published in a peer-reviewed journal, written in English. Strong evidence supported modified constraint-induced movement therapy, constraint-induced movement therapy, neuromuscular electrical stimulation, and virtual reality.
Plain Language Summary
Brachial plexus birth injuries (BPBIs) affect the nerve supply of a person’s arm and hand and can result in lifelong complications. This review examined studies of non-surgical treatments used by occupational therapy for increasing the range of movement and movement skills of the affected arms of children with BPBIs. Non-surgical treatments are typically used first or in combination with surgery to help with recovery, reduce additional problems and help the person be able to use that arm in regular activities.
Searches were completed using Scopus, Cochrane Trials (CENTRAL), Ovid (Medline), and CINAHL. Studies examined were those with participants who had BPBI, were not older than 18 years, were high to moderate level studies, had sample sizes over 20, did not include surgery, were published in a peer-reviewed journal, and were written in English.
Strong evidence supported modified constraint-induced movement therapy, constraint-induced movement therapy, neuromuscular electrical stimulation, and virtual reality as being successful for increasing the range of movement and movement skills of the affected arms of children with BPBIs. Plyometric training, dynamic orthoses and serial casting, and kinesiotaping were found to be successful when combined with regular therapy.
Literature Review
Brachial plexus birth injury (BPBI), also known as obstetrical brachial plexus palsy, Erb’s palsy, neonatal palsy, or obstetrical brachial plexus injury, is an injury affecting the nerve supply to the upper extremity (UE) called the brachial plexus. The incidence of BPBI varies from approximately 0.5 to 4.0 per 1,000 live births (Lalka et al., 2020). Most of these injuries result from shoulder dystocia, in which an infant’s shoulder becomes impacted behind the mother’s pelvis during birth. The mechanical traction or compression to the affected nerve roots can result in varying levels of paresis with a spectrum of clinical presentations. Lesions of the upper trunk of the brachial plexus (C5–C6), known as Erb’s palsy, constitute around 60% of cases and are associated with a “waiter’s tip” position due to unopposed shoulder internal rotation, elbow extension, and wrist flexion. Combined upper and lower trunk brachial plexus injuries (C5–C7), known as extended Erb’s palsy, represent the second most common injury. Global plexus lesions (C5–T1) represent up to 20% of cases and have the poorest rate of recovery. Isolated lower plexus injuries (C8–T1), known as Klumpke’s palsy, are relatively rare and affect the wrist flexors, long digital flexors, and intrinsic muscles of the involved UE (Lalka et al., 2020; Shah et al., 2021).
In many cases, the injury heals spontaneously; however, approximately 20% to 30% of infants with BPBI experience lifelong complications (Shah et al., 2021). Residual deficits most often include reduced limb strength, abnormal scapular morphology, glenohumeral displacement and subluxation, muscle weakness, and range of motion (ROM) limitations contributing to lifelong functional complications (Russo et al., 2016). Despite general advances in health care, the incidence of BPBI has remained relatively constant and was found to have increased within recent decades in some studies (DeFrancesco et al., 2025; Louden et al., 2018).
The sequelae of BPBI, including decreased strength, limited ROM, contractures, and scapular and glenohumeral malalignment, can significantly impair a child’s ability to perform age-appropriate activities (Russo et al., 2016; Shah et al., 2021). These functional limitations may lead to restrictions in occupational participation and overall quality of life throughout childhood and into adulthood (Dorich et al., 2024). Surgical intervention may be indicated for children with more severe nerve involvement. When the prognosis for spontaneous recovery is deemed poor, a decision typically made within the first 3 to 6 months of life, the child’s physician may consider procedures like nerve grafting or nerve transfers (Li et al., 2023).
Non-surgical conservative interventions remain essential in rehabilitation regardless of whether they are used as first-line treatment or post-operatively (O’Shea et al., 2025). Traditionally, these conservative approaches to treatment have included passive range of motion (PROM), active range of motion (AROM), active-assistive range of motion (AAROM), and progressive strengthening (Li et al., 2023). Many reviews have examined surgical interventions, but few have examined non-surgical interventions for children. A previous systematic review of non-surgical interventions examined CIMT (constraint-induced movement therapy) and splinting (dynamic and static), with second-tier techniques like joint manipulation, NMES (Neuromuscular Electrical Stimulation), early infant management education, and serial casting (Martínez-Carlón-Reina et al., 2024), finding positive outcomes from CIMT, splinting, NMES, joint manipulation and serial casting. Ho et al. (2019) found weak evidence that serial casting or elbow release surgery could reduce elbow contractures. With the emergence of studies examining the efficacy of less traditional rehabilitative technologies, a review of current literature is indicated to provide rehabilitation professionals with updated evidence to guide decision-making. Availability of up-to-date research is a tenant in evidence-based practice (EBP) in health care, incorporating also, clinical expertise and patient preference (Dusin et al., 2023). This systematic review aims to examine the efficacy of non-surgical interventions used by occupational therapy for increasing ROM and improving motor skills of the affected upper extremities (UEs) of children with BPBIs. For this review, motor skills will be defined as, “how effectively a person moves self or interacts with objects, including positioning the body, obtaining and hold objects, moving self and objects, and sustaining performance (American Occupational Therapy Association [AOTA], 2020b, p. 13). This is distinct from functional abilities, as it does not directly examine occupational performance or participation in daily activities, but rather performance at the level of body structures and functions.
Method
Search Protocol, Search Terms, and Databases Searched
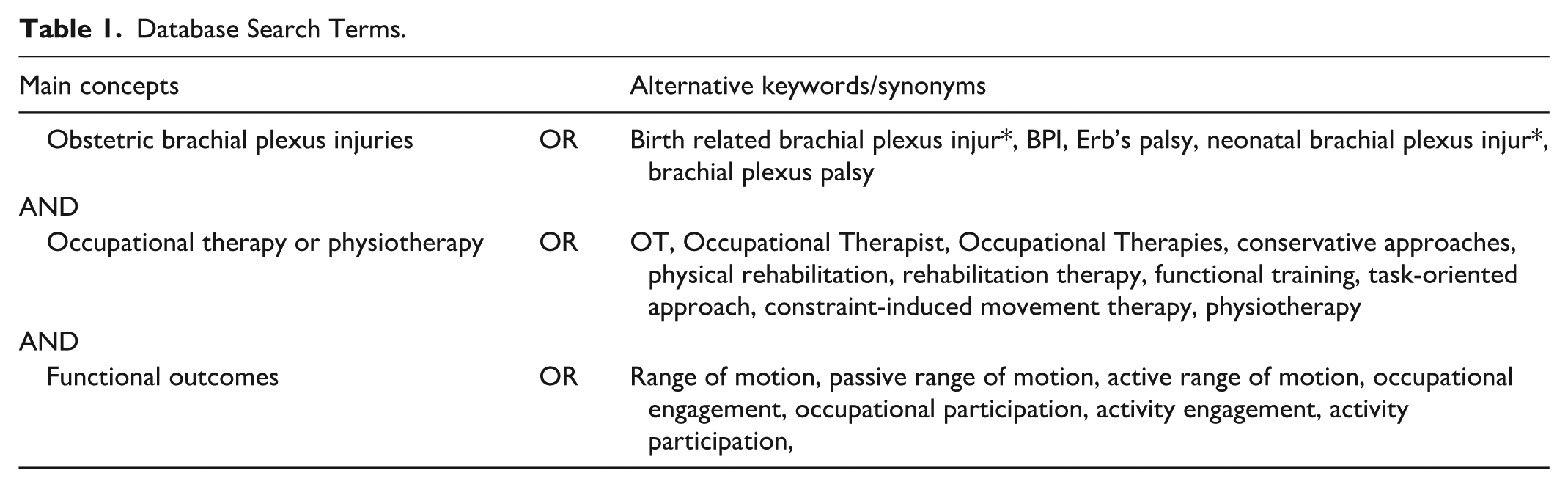
The search terms defined in Table 1 were determined by the authors. The initial search was conducted by the University of Texas Medical Branch research librarian and the following databases were used to identify relevant articles of interest for the systematic review: Scopus, Cochrane Trials (CENTRAL), Ovid (Medline), and CINAHL. The search was completed on July 5, 2024. Search term main concepts included obstetric brachial plexus injuries, occupational therapy, and functional outcomes. The title and abstract of each article were reviewed by at least two of the first five authors to determine eligibility based on the determined inclusion and exclusion criteria using Covidence software. The initial search yielded 1,248 studies, which were divided among the five reviewers for screening. Each article was screened by at least two reviewers. For disagreements, a third reviewer broke the tie. Following this, the full text of each selected article was reviewed by at least two additional authors to further determine eligibility. Final decisions about inclusion were discussed and unanimously agreed on by the five authors (Figure 1). This review was conducted in accordance with Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines. To broaden the scope of evidence encompassed in this review, physiotherapy was included as an alternative search term (See Table 1 for details). The search was limited to non-surgical, conservative inter-ventions.
Database Search Terms.
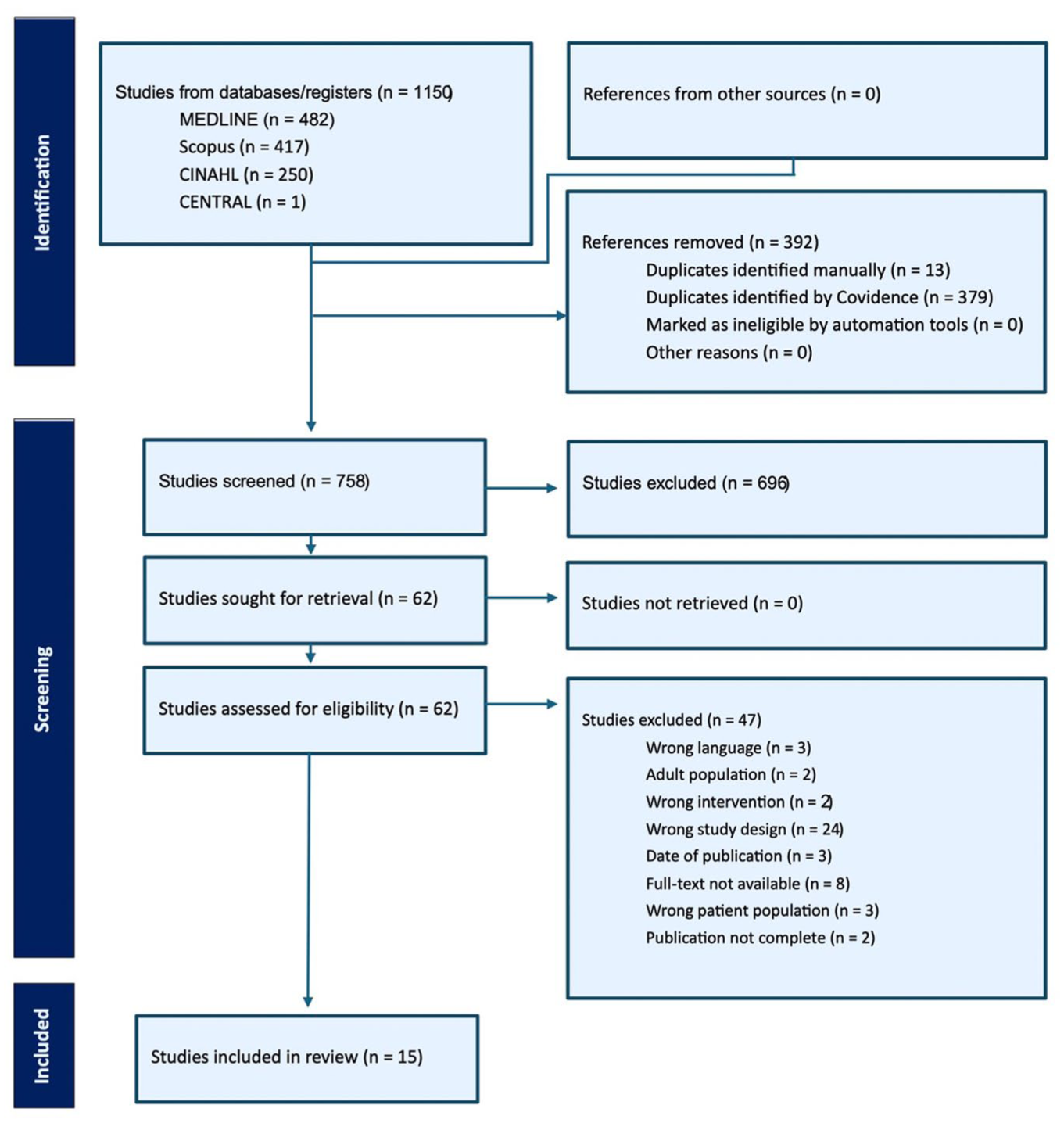
Flow Diagram of Search.
Inclusion criteria were: (a) participants with diagnosis of BPBI, (b) pediatric population (not more than 18 years old), (c) randomized controlled trials (RCTs) or comparative studies (cohort and case-control), (d) sample size over 20, (e) study of conservative non-surgical management, (f) published in a peer-reviewed journal, and (g) written in English. Cohort and crossover study designs were included due to a limited availability of high-level evidence. Exclusion criteria were: (a) not intervention-based, (b) surgical intervention, (c) study of additional neurological conditions, (d) studies published before January 2009, (e) case studies or case series design, (f) adult population, and (g) full text not available. Studies that focused on Botulinum toxin injection in isolation were excluded due to the invasive nature of treatment; however, studies with participants who had received Botulinum toxin injection in the past were not excluded from this review. See Figure 1 for details.
Levels of evidence for included studies were derived from The Oxford Levels of Evidence (OxforCentrevidence-Based Medicine: Levels of Evidence Working Group, 2009) and Systematic Review Guidelines from the American Occupational Therapy Association (AOTA, 2020a).
Risk of bias was assessed for each of the included studies. Bias occurs when a continuous error is made during research that results in inaccurate measurements (Sterne et al., 2019). In this review, the risk of bias was evaluated to ensure inclusion of the most precise and reliable studies concerning interventions for BPBI. The Table Template 2 Risk-of-Bias Table for Randomized Controlled Trial (RCT) and Non-RCT (Sterne et al., 2019) was used to determine and document selection bias, performance bias, detection bias, attrition bias, reporting bias, and overall risk of bias for our included studies. We also used Table Template 3 Risk of Bias for Before–After (Pre–Post) Studies With No Control Group (National Heart Lung and Blood Institute, 2014) and its components to determine and document components of overall risk of bias for one of our included studies. The protocol was registered with the international prospective register of systematic reviews (PROSPERO) in accordance with PRISMA guidelines (PROSPERO CRD42024575565). Authors included two academic professors (one with extensive musculoskeletal expertise and one with substantial research experience), one research librarian with extensive experience in conducting systematic reviews, and five graduate students. The authors received no funding to support this review and report no conflicts of interest.
Results
Of the 15 included studies, nine were characterized as Level 1B, well-designed individual RCTs (Abdel-Kafy et al., 2013; Abdul-Rahman & El-Saeed, 2022; Alsakhawi & Atya, 2020; Al-Wahab et al., 2016; Çekmece et al., 2023; Elnaggar, 2016; Eren et al., 2020; Kuran et al., 2022; Sherief et al., 2021); four were Level 2B, three being low quality RCTs (Karas et al., 2021; Op De Coul et al., 2023; Sari et al., 2023) and one a randomized crossover trial (Werner et al., 2021); and two were Level 3B studies, one being a one-group nonrandomized pre-posttest study (Russo et al., 2016) and one a cross-sectional clinical measurement study (Russo et al., 2018). Six studies were conducted in Egypt, five in Turkey, three in the United States of America, and one in the Netherlands. Treatment provided in 10 studies was administered by physical therapists or physiotherapists, three by occupational therapists, and two by a combination of physical and occupational therapists (see Table 2). Participants were from 12 months to 18 years old. The number of participants ranged from 20 to 90, with 558 total.
Evidence Table of 15 Included Articles.
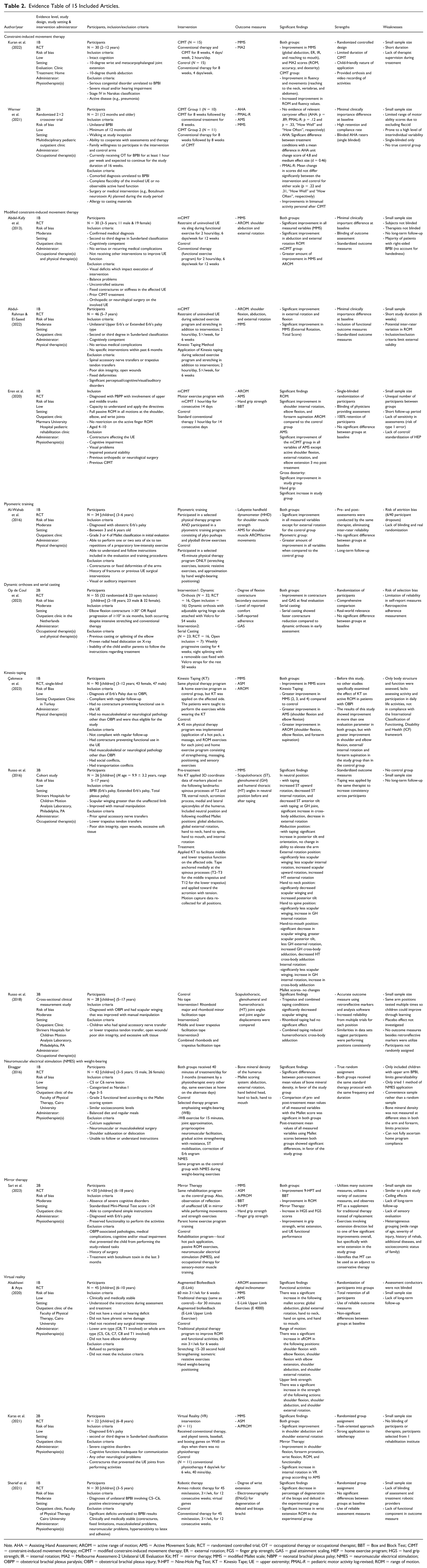
Note. AHA = Assisting Hand Assessment; AROM = active range of motion; AMS = Active Movement Scale; RCT = randomized controlled trial; OT = occupational therapy or occupational therapist; BBT = Box and Block Test; CIMT = constraint-induced movement therapy; mCIMT = modified constraint-induced movement therapy; ER = external rotation; FGS = finger grip strength; GAS = goal attainment scaling, HEP = home exercise program; HGS = hand grip strength; IR = internal rotation; MA2 = Melbourne Assessment-2 Unilateral UE Evaluation Kit; MT = mirror therapy; MMS = modified Mallet scale; NBPP = neonatal brachial plexus palsy; NMES = neuromuscular electrical stimulation; OBPP = obstetrical brachial plexus paralysis; OBPI = obstetrical brachial plexus injury; 9-HPT = Nine-Hole Peg Test; KT = Kinesio Tape; UE = upper extremity; PMAL-R = pediatric motor activity log-revised; ROM = range of motion.
Although some factors such as the lack of blinding of participants and the lack of blinding of objective outcome assessments increased the risk of bias, nine studies had a low risk of bias, and six had a moderate risk (see Tables 3 and 4). This low to moderate risk of bias was because the studies utilized components such as randomization processes, the complete reporting of outcome data, and non-selective reporting of results despite the magnitude of the findings. Overall, the majority of studies had a low risk of bias, which indicates high sample quality. All included articles had performance bias due to the inability to blind their participants and study personnel based on the treatment methods. Çekmece et al. (2023) was the only exception to the inability to blind their study personnel. Along with this bias risk, some of the included studies required adherence to protocol at home (e.g., CIMT and dynamic orthoses/serial casting), which meant the parents or caregivers of the children were enforcing the protocols instead of the researchers, which led to the inevitability of an uncontrolled environment.
Risk-of-Bias Table: Randomized Controlled Trial (RCT) and Non-RCT.
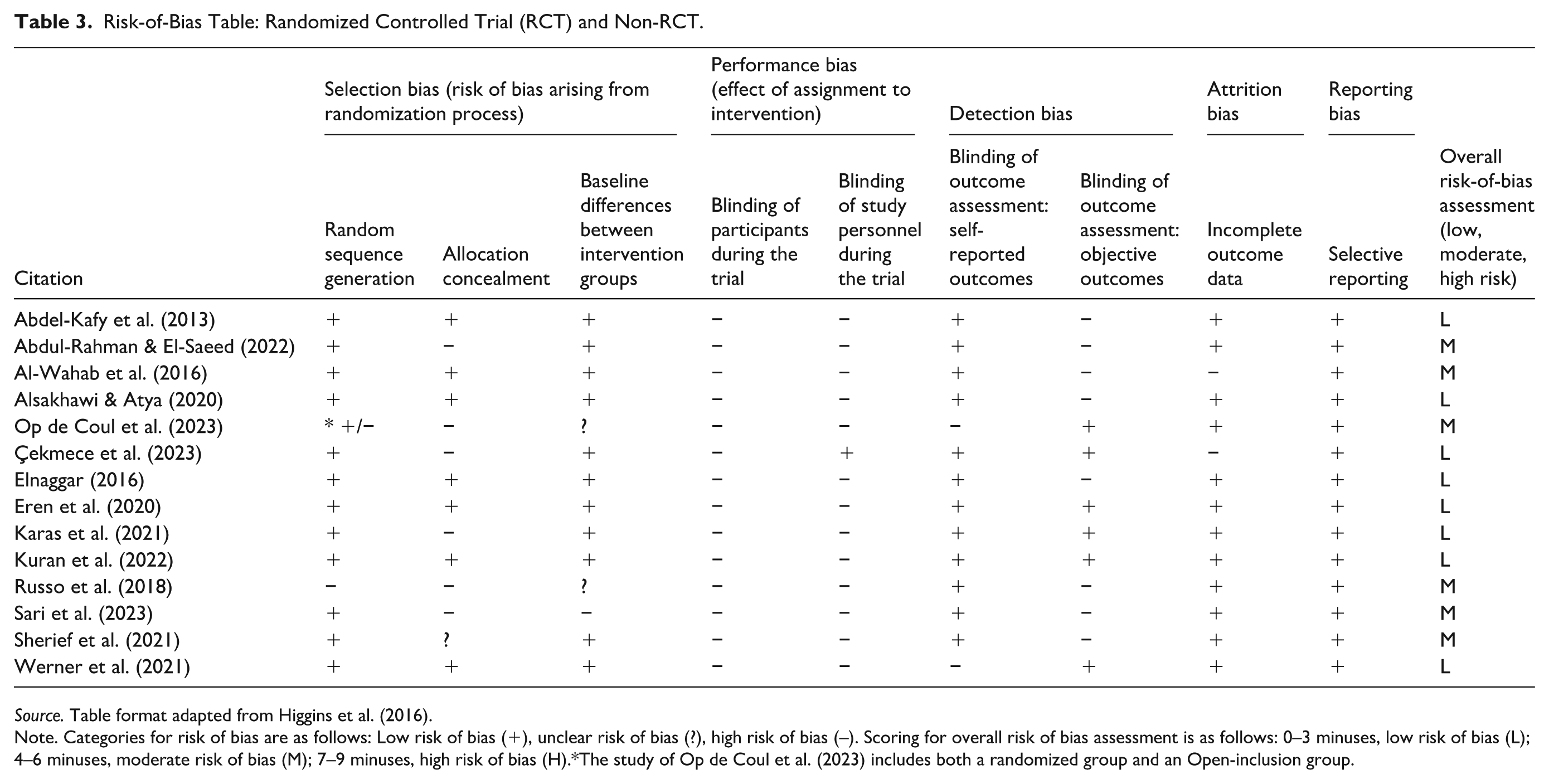
Source. Table format adapted from Higgins et al. (2016).
Note. Categories for risk of bias are as follows: Low risk of bias (+), unclear risk of bias (?), high risk of bias (–). Scoring for overall risk of bias assessment is as follows: 0–3 minuses, low risk of bias (L); 4–6 minuses, moderate risk of bias (M); 7–9 minuses, high risk of bias (H).*The study of Op de Coul et al. (2023) includes both a randomized group and an Open-inclusion group.
Risk of Bias for Before–After (Pre–Post) Studies With No Control Group.
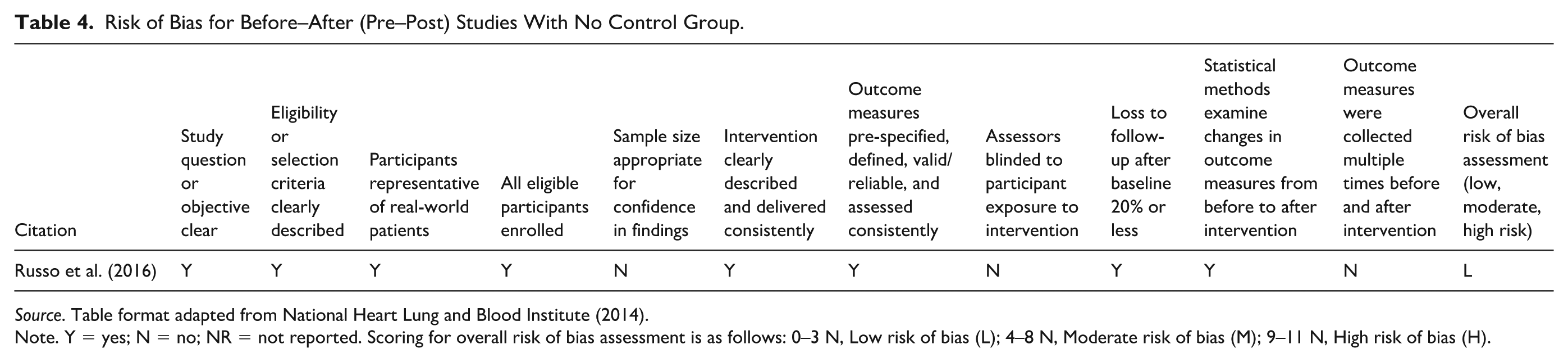
Source. Table format adapted from National Heart Lung and Blood Institute (2014).
Note. Y = yes; N = no; NR = not reported. Scoring for overall risk of bias assessment is as follows: 0–3 N, Low risk of bias (L); 4–8 N, Moderate risk of bias (M); 9–11 N, High risk of bias (H).
A wide range of interventions were included in this review, with CIMT, mCIMT, and VR being the most common. Three of the studies used mCIMT as an intervention (Abdel-Kafy et al., 2013; Abdul-Rahman & El-Saeed, 2022; Eren et al., 2020). Two studies examined CIMT (Kuran et al., 2022; Werner et al., 2021). Al-Wahab et al. (2016) investigated plyometric training and Op de Coul et al. (2023) observed outcomes of dynamic orthoses and serial casting. Çekmece et al. (2023), Russo et al. (2018), and Russo et al. (2016) examined the effects of KT. Elnaggar (2016) observed outcomes after NMES during weight-bearing, and Sari et al. (2023) used MT as an intervention. Finally, three studies investigated VR (Karas et al., 2021, with the Nintendo Wii®, Alsakhawi & Atya, 2020, with the E-Link Upper Limb Exerciser, and Sherief et al., 2021, with the Armeo® RT system). For the purposes of this review, PROM is represented in traditional treatment, typically seen within control group protocol and as an adjunct to additional treatment protocols (see Table 2 for details).
The outcome measures reviewed in this paper included scoring on a variety of items such as goniometry, electroneurography (ENoG), the Pediatric Motor Activity Log-Revised (PMAL-R), the Modified Mallet Scale (MMS), the Mallet Scoring System (MSS), the Active Movement Scale (AMS), dynamometry, pinch gauge, the Box and Block Test (BBT), the Nine-Hole Pegboard Test (9-HPT), the Melbourne Assessment 2 (MA2), the Assisting Hand Assessment (AHA), the Goal Attainment Scale (GAS), and self-reported adherence.
Constraint-Induced Movement Therapy
Constraint-Induced Movement Therapy (CIMT) is based on the theories of brain plasticity and cortical functional reorganization to address learned nonuse of the affected limb (Werner et al., 2021). Using massed and intensive practice with the affected limb, CIMT follows two principles that include placing a restraint on the unaffected UE for 90% of the time the individual is awake, with a simultaneous implementation of intensive repeated training for six or more hours a day on the affected limb (Hoare et al., 2019).
Two studies examined CIMT to improve UE functioning in children with BPBI (Kuran et al., 2022; Werner et al., 2021). Werner et al. (2021) conducted a randomized crossover trial using the AHA as a primary outcome measure to assess bimanual activity performance, and the caregiver-reported PMAL-R as a secondary outcome measure to assess caregiver-reported quality and frequency of UE use in their natural environment. CIMT was found to be more effective at improving bimanual activity performance than standard treatment based on an average increase of 7.1 AHA points, exceeding the 5 AHA unit threshold for establishing a minimal clinically important difference. Despite the apparent improvements in bimanual activity performance following CIMT therapy, there were no clinically significant differences in PMAL-R scores between the intervention and control groups.
Kuran et al. (2022) conducted an RCT, involving the treatment group (Group 1) receiving conventional exercise treatment in conjunction with CIMT and the control group (Group 2) receiving only conventional exercise treatment. Both groups experienced significant increases in their MMS scores and MA2 scale scores, though there was greater improvement in the group that received CIMT. The MA2 scores for ROM, accuracy, and dexterity significantly improved post-treatment for both groups, though fluency only improved after treatment in Group 1. In addition, both groups experienced significant improvements post-treatment in Mallet scores of global abduction, external rotation, internal rotation, and reaching the mouth, though the improvements seen in Group 2 were less significant than those seen in Group 1. Regarding Mallet system scores, there were significant differences seen pre- and posttest scores, and Group 1 experienced more significant improvements than Group 2.
Modified Constraint-Induced Movement Therapy
Modified Constraint-Induced Movement Therapy (mCIMT), similar to CIMT, is a therapy protocol that involves prolonged constraint of the non-affected extremity to encourage use of the affected side and facilitate cortical reorganization (Chamudot et al., 2018). As outlined by Brady and Garcia (2009), mCIMT “typically involves an alternative to casting for constraint, such as a mitt, splint, or sling, reduced hours per day using the constraint, reduced hours of shaping per day, reduced number of treatment days, provision of therapy in the home environment, and embedding therapy activities within the context of play” (p. 107). The treatment dosage varies in the literature. Wang et al. (2025) examined 10 studies in a meta-analysis, which were grouped by low dosage (<30 hours), moderate dosage (30–49 hours), and high dosage (≥60 hours). The analysis suggested that total training hours were not a significant moderator.
Three level 1B RCTs observed the effects of mCIMT on UE motor function. Both Abdel-Kafy et al. (2013) and Eren et al. (2020) concluded that mCIMT is effective in increasing functional UE use in children with BPBI. Both studies found significantly greater active range of motion (AROM) increase in the mCIMT group compared to the control group. The studies also observed improvement in standardized measurement scores for the treatment group only, with Abdel-Kafy et al. (2013) utilizing the Mallet scale system and Eren et al. (2020) using the dynamometer strength measurement. Eren et al. (2020) additionally saw significant improvement in BBT scores for both mCIMT and control groups, but only the mCIMT group saw a significant increase in transferred block numbers. The third group of researchers (Abdul-Rahman & El-Saeed, 2022) concluded that mCIMT was not superior to KT for improving functional outcomes in children with BPBI. Using the MMS and AROM measurements for shoulder flexion, abduction, and external rotation, no significant difference was seen between group means on all measured parameters. They did find significant improvement in both groups in external rotation ROM and forearm supination.
Plyometric Training
Plyometric training (Al-Wahab et al., 2016) emphasizes muscle loading during eccentric muscle action followed by quick rebound concentric action. Al-Wahab et al. (2016) in a Level 1B RCT found that plyometric training was an effective method for improving strength and active movement in children with BPBI, providing moderate strength of evidence for assessing the impact of plyometric training. Pre- and post-treatment evaluations measured isometric muscle strength of the shoulder flexors and external rotators using a Lafayette Handheld Dynamometer and active shoulder flexion and external rotation using the AMS. The results showed no significant difference between the control group and study group pre-treatment mean values in all measured variables, but significant improvement was seen when comparing pre- and post-treatment mean values in all measured variables for both groups, excluding active shoulder external rotation movement of the control group. No significant difference was seen between groups for the post-treatment mean values of all the measured variables, but post-treatment improvement was greater in the treatment group.
Dynamic Orthoses and Serial Casting
Casting involves applying a series of casts to progressively stretch tight muscles and improve ROM in the joint. It is typically followed by night splinting with removable casts to maintain the joint in maximum extension while the individual sleeps. Dynamic orthoses include a dynamic spring hinge that allows for adjustable extension forces. Adjusting the spring provides a constant and mild stretch to the joint to increase extension (Op de Coul et al., 2023).
Op de Coul et al. (2023) found both dynamic orthoses and serial casting to be effective for improving elbow flexion contractures based on improvements in GAS score comparisons from initial evaluation to post-treatment evaluations at 54 weeks. The study had a unique group assignment structure, allowing participants an option to be randomly assigned or not. Participants who decided not to be randomly assigned could opt out of the intervention if it was not suitable for their condition (an open inclusion group). This is a Level 2B study due to mixed method group assignment with four evaluations: initial, after 8 weeks of treatment, after 20 weeks of treatment, and after 54 weeks of treatment. They measured elbow contracture, GAS, self-reported therapy comfort, and adherence to treatment. No significant differences were seen between the two groups in elbow flexion contractures and GAS scores after 54 weeks. However, serial casting showed a faster improvement in elbow contracture from the initial evaluation to week 8, remained constant from week 8 to week 24, and showed no difference between week 25 and week 54. The participants favored dynamic orthoses in therapy due to comfort, but showed no differences in adherence.
Kinesio taping
Kinesio taping (KT) involves applying tape to provide proprioceptive input to provide optimal alignment of joints through tension, which promotes functional use of the affected limb (Özüdoğru et al., 2023). Taping can be applied in various configurations to encourage proper alignment and support depending on specific impairments. Evidence from three studies supports the use of KT as an intervention for children with BPBI. One Level 1B RCT evaluated the effect of KT on MMS, AMS, and AROM scores (Çekmece et al., 2023). The study group demonstrated a significant improvement in MMS of Mallet 2, Mallet 3, Mallet 4, and total Mallet scores when compared to the control group receiving standard conservative treatment.
Shoulder and elbow flexion AMS assessments showed significant improvement in the treatment group. Remaining AMS and MMS components and AROM showed an increase in both groups without significant intergroup differences. In a Level 3B cohort study, Russo et al. (2016) examined the effect of therapeutic taping on stabilization of the scapulothoracic (ST), glenohumeral (GH), and humeral thoracic (HT) joint angles in neutral position, as well as modified Mallet positions. The study found a statistically significant increase in the GH joint with hand to spine, hand to mouth, and internal rotation positions, along with a decrease in scapular winging in all modified Mallet positions except abduction. No significant improvements were seen in the MMS score. Russo et al. (2018) in a Level 3B cross-sectional clinical measurement study found therapeutic taping for facilitation of trapezius and for combined facilitation of rhomboids and trapezius to significantly decrease scapular winging in all positions when compared to no tape. No significant difference was identified with taping for facilitation of the rhomboids alone.
Neuromuscular Electrical Stimulation With Weight-Bearing
Neuromuscular Electrical Stimulation (NMES) engages muscles through small electrical impulses delivered by electrodes placed on the skin to produce involuntary muscle contractions (Knutson et al., 2015). This stimulation improves muscle strength, ROM, and circulation to the engaged muscle(s). Evidence from Elnaggar (2016) in a Level 1B RCT suggested that NMES during weight-bearing exercises may improve shoulder function and total bone mineral density (BMD) of the humerus in children with BPBI. The pre- and post-treatment measurements included dual-energy x-ray absorptiometry to measure BMD and MSS to measure active shoulder function. The results showed significant post-treatment differences in both groups compared to the pre-treatment mean values of BMD and MSS for active shoulder flexion, with a greater difference in the intervention group.
Mirror Therapy
Mirror Therapy (MT) is a rehabilitation strategy based on the use of the mirror illusion and enables the neural network in the brain to reconfigure itself by creating a visual illusion (Sari et al., 2023). This allows for the substitution of reduced/missing proprioceptive input by “tricking” the brain into thinking the unaffected limb is the affected limb. One Level 2B RCT evaluated the effects of MT on UE function using assessments including the AMS, the MMS, the Hand Grip Strength (HGS) test, the Finger Grip Strength (FGS) Test, the BBT, 9-HPT, and ROM with goniometry (Sari et al., 2023). They found no statistically significant improvements in ROM, AMS, or MMS scores for treatment or control group, but a significant increase in HGS and FGS scores was seen in the treatment group when compared to the control. All other measures showed no significant difference between groups.
Virtual Reality
VR-based interventions use interactive, computer-generated simulations that represent real-world engagement within a controlled environment. VR systems typically provide real-time feedback, can be easily graded, and increase client motivation (Chen et al., 2022). For this systematic review, examples include the use of the Wii®, Armeo® robotic therapy (RT), and the E-Link Upper Limb Exerciser. Two Level 1B RCTs (Alsakhawi & Atya, 2020; Sherief et al., 2021) and one Level 2B study (Karas et al., 2021) investigated the effects of VR interventions, including the E-Link Upper Limb Exerciser, Nintendo Wii®, and Armeo® RT, all of which showed greater improvement than conventional therapy.
Alsakhawi and Atya (2020) evaluated an augmented biofeedback method of VR using the E-Link Upper Limb Exerciser and measured AROM using the MMS and the AMS. The MMS showed significant differences between the control physical therapy group and the E-Link group in global abduction, global external rotation, hand to neck, hand on spine, and hand to mouth. The E-Link group showed significant improvements in AROM in shoulder flexion with elbow flexion, shoulder flexion with elbow extension, shoulder abduction, and shoulder external rotation. In addition, upper limb strength showed significantly greater improvement in the E-Link group in shoulder flexion, shoulder abduction, and shoulder external rotation.
Karas et al. (2021) examined VR treatment using Nintendo Wii® systems and measured UE ROM using the AMS and the MSS. The VR treatment group showed significant improvements in shoulder flexion, forearm pronation, wrist flexion, ROM, and functionality, while the control group showed improvements in shoulder abduction and external rotation. The AMS results were significantly greater for the VR treatment group in shoulder internal rotation, but no significant differences were seen in MSS values.
Sherief et al. (2021) examined Armeo® RT, a type of VR, for inhibiting degeneration of arm and hand muscles and improving motor skills and ROM of upper limbs in children with Erb’s Palsy. The control group, Group A, received conventional therapy, while Group B practiced Armeo® therapy. Both groups experienced significant decreases in degeneration of the biceps brachii and deltoid muscles after treatment compared with pre-treatment, and significant increases in wrist extension ROM from pre- to post-testing. Though both groups demonstrated improvement in muscle degeneration and wrist extension ROM, Group B experienced significantly more improvement than Group A.
Discussion
The aim of this review was to examine the efficacy of non-surgical interventions used by occupational therapy for increasing the ROM and improving motor skills of the affected UE. This review includes new studies that add strength to some of the interventions previously reviewed and includes studies of interventions not previously reviewed (Ho et al., 2019; Martínez-Carlón-Reina et al., 2024). Overall, the findings suggest that several conservative interventions demonstrate significant benefits.
Task-based approaches, including CIMT, mCIMT, and VR demonstrated strong outcomes, particularly in the domains assessed by functional measures like the AHA, MA2, and PMAL-2. These interventions were found to be more effective than conventional therapy when administered to a population of children with sufficient active movement and cognitive capacity to perform the required tasks. More passive approaches, including serial casting, dynamic orthoses, and NMES, showed less significant improvements in motor skill, but increased in ROM. These interventions, notably, were found to be effective when used in conjunction with conventional therapy for younger children and/or children with more severe injury and presence, or high risk, of contracture development.
Constraint-Induced Movement Therapy
Kuran et al. (2022) and Werner et al. (2021) examined the effects of CIMT on functional outcomes. They are level 2B and 1B, respectively, providing moderate strength of evidence supporting CIMT for improving bimanual activity performance, UE strength, and ROM (AOTA, 2020a). Participants who received CIMT in addition to standard treatment experienced superior functional outcomes to those with standard treatment alone. It is important to note that studies utilizing CIMT will have some variability in the application of the intervention because participants will inevitably engage in slightly different daily activities and because the time-consuming nature of this intervention may limit feasibility for some families, particularly in outpatient settings. Overall, CIMT shows promise in improving motor skills and ROM for children 1 to 12 years of age with unilateral BPBI, adequate baseline movement, and without history of surgical repair of the affected extremity.
Modified Constraint-Induced Movement Therapy
Three Level 1B studies examined mCIMT as an intervention (Abdel-Kafy et al., 2013; Abdul-Rahman & El-Saeed, 2022; AOTA, 2020a; Eren et al., 2020). It is appropriate to conclude that mCIMT is an effective intervention for improving functional outcomes such as UE strength, ROM and hand dexterity in children between 3 and 10 years of age with BPBIs who are cognitively competent and have no serious medical complications. This approach may be more appropriate for patients or caregivers who have concerns about adhering to the more rigorous protocols involved in CIMT. In addition, mCIMT can be utilized with a slightly broader population, with less strict baseline requirements. Comparing mCIMT and KT, Abdul-Rahman and El-Saeed (2022) found no significant superiority of either approach, suggesting both may support functional gains, but indicating that more research is needed to reach meaningful conclusions. Overall, the evidence supports mCIMT as an effective intervention for children at least 3 years of age exhibiting nonuse who are capable of engaging in task-based therapy.
Plyometric Training
Plyometric training is a less common approach to treatment, investigated by Al-Wahab et al. (2016). This RCT had a moderate risk of bias due to a lack of blinding. Overall, this one study provides low-level evidence to support the effectiveness of plyometric training as a treatment for upper trunk BPBI in children three to six without a history of UE fracture or surgical intervention (AOTA, 2020a). The researchers found that plyometric training improved strength and active movements in study participants who had both conventional therapy and plyometric training. It can be concluded that plyometric training shows promise as being useful for improving strength and ROM for children with Erb’s palsy, between 3 and 6 years old, without the presence of fixed contractures. It is important to note that the outcome measures utilized were a hand dynamometer and the AMS for shoulder muscle AROM. Because functional outcome measures were not included, it cannot be concluded that plyometric training improves engagement in everyday activities. More research is indicated, as the narrow inclusion criteria and minimal availability of supporting evidence limit the ability to determine strong clinical relevance.
Dynamic Orthoses and Serial Casting
Dynamic orthoses and serial casting are both more specialized interventions for contracture management due to BPBI and were compared by Op de Coul et al. (2023). This study is Level 2B due to mixed method group assignment and provides low-level evidence to support the effectiveness of this intervention in contracture reduction for children aged two to 18 with BPBI (AOTA, 2020a). This is particularly indicated for children with the presence or risk of joint contractures, or during a period when active participation is limited by age, cognition, or severity of impairment. Both techniques were effective in reducing contractures, though serial casting saw faster improvement and dynamic orthoses were favored for comfort. Existing evidence is insufficient to draw a conclusion on the long-term effects of dynamic orthoses and serial casting on UE motor skills.
Kinesio Taping
Three studies observed the effects of KT methods on BPBI: Çekmece et al. (2023), Russo et al. (2016), and Russo et al. (2018). Çekmece et al. (2023) is a Level 1B study, and both Russo et al. (2016) and Russo et al. (2018) are Level 3B. One level 1B study and two level 3B studies provide moderate evidence of the effectiveness of KT, when combined with conventional treatment, for BPBI in children between 3 and 17 years of age without fixed deformity secondary to injury (AOTA, 2020a). Both Çekmece et al. (2023) and Russo et al. (2016) had a low risk of bias, and Russo et al. (2018) had a moderate risk of bias due to the lack of random sequence generation, allocation concealment, and blinding. All three studies utilized modified mallet positions and classifications to assess participants’ UE performance. The results of these studies suggest that KT, along with conventional treatment, can improve UE ROM and motor skills in a wide age range of children with BPBI who exhibit muscle imbalance or scapular instability but retain active movement. The non-restrictive and cost-effective nature of this intervention supports its use as an adjunct treatment to be combined with a developmentally appropriate occupation-based intervention.
Neuromuscular Electrical Stimulation With Weight-Bearing
The effects of NMES during weight-bearing exercises on shoulder functioning and BMD were examined by Elnaggar (2016) in a Level 1B RCT. The single level 1B study provides moderate evidence supporting NMES as an effective treatment for upper trunk BPBI in children aged 3 to 5 years of age with no surgical history (AOTA, 2020a). Though both the groups showed significant improvements in shoulder function and BMD from pre- to post-treatment, the NMES treatment group showed greater improvement than the control group suggesting that NMES combined with conventional treatment improves ROM, motor skill, and BMD in children with BPBI. This approach is particularly indicated for children with limited voluntary muscle activation. Narrow inclusion criteria of the reviewed study limits generalizability, indicating the need for further research.
Mirror Therapy
Sari et al. (2023) examined the efficacy of adding MT to traditional therapy for improving upper limb motor functioning. Though the study is set up as an RCT, it is a Level 2B because the sample size was small and it was similar to a pilot study. No significant difference between the treatment group and control group was found, and it is important to note that the study had small power and heterogeneity in demographics, such as age and severity of injury, and a noted ceiling effect, lack of long-term follow-up, and lack of sensory evaluations. Findings suggest no benefit from adding MT to traditional therapy when utilized as treatment for unilateral BPBI in children ages 6 to 18 years. Stronger studies may be indicated with greater power and specificity regarding participant selection.
Virtual Reality
Three VR treatment methods were observed: the E-Link Upper Limb Exerciser (Alsakhawi & Atya, 2020), Nintendo Wii® Sports (Karas et al., 2021), and Armeo® RT (Sherief et al., 2021). Considering the combined outcomes of these studies, strong evidence supports the broad category of VR as an intervention for unilateral BPBI in children without significant cognitive deficits, between the ages of 3 and 10 years (AOTA, 2020a). Significant improvements in functional movements, ROM, and UE strength were observed by Alsakhawi and Atya (2020) in a Level 1B RCT with a low risk of bias, testing the efficacy of the E-Link. The VR group in a level 2B RCT low risk of bias Wii® study by Karas et al. (2021) showed a significantly greater improvement in shoulder internal rotation, shoulder flexion, forearm pronation, and wrist flexion, but no significant differences were seen in MSS values. Sherief et al. (2021) conducted a Level 1B RCT with a moderate risk of bias, which examined the efficacy of RT using for inhibiting the degeneration of arm and hand muscles and improving the functioning of upper limbs in children with Erb’s Palsy. Armeo® RT (Sherief et al., 2021) found a significant increase in wrist extension and a significant decrease in the percentage of degeneration of the biceps brachii and deltoid muscles, showing promise for the use of Armeo® as superior to conventional therapy in the treatment of children with Erb’s Palsy. Considering the diversity of the VR interventions, the strength of the evidence is not as clear as with more equivalent interventions and more research on each type of VR is needed to strengthen the evidence for this type of intervention.
This approach is highly indicated for children with the developmental capacity to manipulate VR controls, typically school-aged and older, without contracture. VR can provide increased motivation and reduce the need for therapist or caregiver supervision. Cost represents a potential barrier to this approach, reinforcing the importance of collaborating with patients and caregivers when developing a plan of care.
Clinical Implications
Rehabilitation professionals, including occupational therapy practitioners, may use the findings of this review to guide the selection of appropriate conservative interventions based on the individual contexts of the child. For example, a clinician may find mCIMT and CIMT to be most appropriate for a client exhibiting learned nonuse. The child must, however, demonstrate adequate active movement and range of motion as outlined by specific protocols (Chamudot et al., 2018). Electrical stimulation may be a more appropriate intervention for children with limited motor activation (Knutson et al., 2015). Age and developmental factors should be considered in intervention planning. Task-based interventions, like those seen in mCIMT, CIMT, and VR, should be reserved for children with the developmental capacity to meaningfully engage in the treatment. For individuals in earlier stages of development, more passive interventions like serial casting and dynamic orthoses and NMES may be more appropriate. Additional research regarding changes in the efficacy of specific interventions across various stages of childhood would be beneficial to further support evidence-based practice of BPBI treatment. It is essential that the therapist to consider multiple factors—environmental, physical, and socioemotional—and collaborate with their client and care providers when determining a plan of treatment.
Limitations
Limitations of this review include the lack of a common functional outcome, creating difficulty in synthesizing results. Similarly, the articles were varied in injury severity, age, and duration of treatment, limiting the ability to draw conclusions on short-term and long-term effectiveness. Although the aforementioned client factors are necessary considerations in developing a plan of care, this review did not specifically evaluate these variations. A majority of the reviewed studies examined a narrow age range and lacked a shared outcome measure, study duration, participant age range, and severity of injury; Existing literature was insufficient to support meaningful comparison of outcomes within these subgroups.
Identifying outcome measures that would be most useful for determining if an intervention is effective for this population would have added to the findings of this review, but it was not yet appropriate for the current review and is a limitation. All studies, with the exception of one (Russo et al., 2016), were conducted within an outpatient rehabilitation setting, thus increasing subject homogeneity but limiting generalizability across the continuum of care. The variability of geographic locations of studies included in this review may also represent a limitation due to potential variations in service delivery models across cultures. This review did not include a cost-analysis treatment method, which may be an important factor to examine for real-world applicability.
Strengths
A strength of this systematic review was the use of comprehensive search strategies to identify all relevant evidence and minimize the risk of bias during the review process. Using Covidence, the following databases were searched: Scopus, Cochrane Trials (CENTRAL), Ovid (Medline) and CINAHL. To minimize bias, each article was reviewed by at least two of the five authors. Two additional strengths involve the inclusion of 15 studies from several countries including Egypt, Turkey, the Netherlands, and the United States, supporting the generalizability of the review and the inclusion of studies with sample sizes greater than 20 individuals. These study characteristics increased the generalizability of the findings for conservative non-surgical BPBI treatment methods.
Conclusion
Though many children with BPBI recover with minimal impact on functioning, 20% to 30% have lifelong effects that can hinder participation in all areas of occupation. The findings from this review revealed many potentially effective conservative treatment options for occupational therapists to consider when treating clients with BPBIs. The strongest findings supported CIMT, mCIMT, NMES, and VR. The treatments found to be effective when combined with conventional therapy were plyometric training, dynamic orthoses, and serial casting, and KT, each of which improved strength and ROM, contractures, and scapular stabilization. Occupational therapy practitioners should utilize clinical reasoning to guide treatment of BPBI. Findings from this review are intended to be used with consideration of client factors such as level of caregiver support, developmental age, client and family goals, and environmental support or barriers that may impact a child’s response to treatment and overall occupational performance. Although many of the included studies are high level and have low risks of bias, more studies are needed to meet the expectation of evidence-informed practice. Further research is needed to examine interventions for specific levels of impairment, specific ages, specific types of VR interventions, and to compare outcomes from different interventions. In addition, future studies are needed to examine specific functional and occupation-based outcomes.
Supplemental Material
sj-docx-1-otj-10.1177_15394492261426940 – Supplemental material for Systematic Review: Non-Surgical Rehabilitation Interventions for Children With Brachial Plexus Birth Injury
Supplemental material, sj-docx-1-otj-10.1177_15394492261426940 for Systematic Review: Non-Surgical Rehabilitation Interventions for Children With Brachial Plexus Birth Injury by Paige Koerner, Rosie Head, Cierra Beauvais, Leahana Haberman, Ye-Eun Oh, April Cowan, Alison DeVries Hansen, Riqiea Kitchens and Claudia Hilton in OTJR: Occupational Therapy Journal of Research
Footnotes
Ethical Considerations
No Institutional Review was needed because no human subjects were included in this review.
Consent Processes
Consent was not needed because the data consisted of manuscripts rather than human subjects.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Data Availability Statement
The search process is described in the manuscript and can be replicated.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
